Abstract
Objective
To compare the efficacy and safety of robot-assisted laparoscopic ureteral reimplantation (RALUR) and open ureteral reimplantation (OUR) in treating primary pediatric vesicoureteral reflux (VUR) based on published literature.
Methods
A comprehensive literature search of PubMed, Embase, Cochrane Library, CBM, CNKI and VIP databases was conducted to identify studies comparing the outcomes of RALUR with OUR for treating primary pediatric VUR. The last search was in January 2017. Summarized mean differences (MDs) or odds ratios (ORs) with 95% confidence intervals (CIs) were used to assess the differences in outcomes between RALUR and OUR.
Results
A total of six studies containing 7122 children with primary VUR were included in this analysis. Significantly longer operation time was needed for RALUR than OUR (MD 66.69 min, 95% CI 41.71–91.67, P < 0.00001), while the RALUR group had significantly fewer days of hospital stay (MD − 17.80 h, 95% CI − 21.18 to − 14.42, P < 0.00001) and postoperative Foley placement (MD − 0.32 days, 95% CI − 0.57 to − 0.07, P = 0.01). No significant differences were found in estimated blood loss during operation, success rate, complications, and postoperative analgesia usage between the two groups. In subgroup analyses, a significantly higher rate of short-term postoperative complications in RALUR was found compared with OUR (OR 3.17, 95% CI 1.72–5.85, P = 0.0002).
Conclusions
Our study indicates that compared with OUR, RALUR is also an effective surgical approach for primary pediatric VUR and could help patients return to society more quickly; however, short-term postoperative complications of RALUR should be considered cautiously.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Vesicoureteral reflux (VUR) is a common health problem in pediatric urology, occurring in approximately 1% of children [1]. Impairment of renal function may be caused by VUR through recurrent urinary tract infection and pyelonephritis [2]. Ureteral reimplantation was the initial surgical correction method for pediatric VUR. Laparoscopic approach for VUR was introduced as early as 1993 [3], and robot-assisted laparoscopic approach followed about one decade later [4]. Although open ureteral reimplantation (OUR) is still the gold standard in surgical treatment of pediatric VUR [5, 6], the application of robot-assisted laparoscopic ureteral reimplantation (RALUR) has been growing in popularity [7, 8].
Although OUR offers a high and durable success rate for pediatric VUR [9], less invasive techniques have also been developed to minimize surgical damage. However, the conventional laparoscopic approach failed to achieve a similar success rate compared to OUR [10, 11]. With the development of robotic instrumentation, RALUR was applied in clinical practices and has been proven to relieve postoperative pain, shorten the recovery phase and have a shorter learning curve than the conventional laparoscopic approach [12,13,14].
With the increased use of RALUR, wide-ranging success rates have been reported [15,16,17,18], and the conclusive evaluation of RALUR seemed important. However, few available studies exist that investigated the efficacy of RALUR for treating pediatric VUR compared with traditional OUR, and most of these studies were limited by a small sample of cases based in a single institution. Additionally, both the current European Association of Urology (EAU) and American Urological Association (AUA) guidelines on VUR in children do not recommend RALUR as a routine procedure for surgical correction of pediatric VUR due to a lack of reports and evidence [6, 19]. Therefore, we conducted this systematic review and meta-analysis to assess the efficacy of RALUR for treating primary pediatric VUR compared with OUR, aiming to provide further evidence and guidelines for clinicians.
Materials and methods
The systematic review and meta-analysis were conducted in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) guidelines.
Search strategy
A comprehensive electronic literature search of PubMed, Embase, and Cochrane Library was conducted to obtain studies comparing the outcomes of RALUR and OUR for treating primary pediatric VUR. The search terms used were “‘robot-assisted laparoscopic’ or ‘robotic assisted laparoscopic’”, “‘open’ or ‘open surgery’ or ‘open approach’”, “‘ureteral reimplantation’ or ‘ureteral reimplant’ or ‘UR’”, and “‘vesicoureteral reflux’ or ‘VUR’”. References of all included studies were also checked for potential records. The last search was performed on January 2017, and no language restriction was applied.
Inclusion and exclusion criteria
Comparative studies concerning the efficacies or outcomes of RALUR versus OUR for the surgical correction of primary pediatric VUR were included in this analysis. Accordingly, convention abstracts, case reports, conference proceedings, reviews or repeated publications were excluded. Literature search and screening, including studies’ quality assessment and data extraction, were performed by two reviewers (TD and BL) independently, and discrepancies were resolved via open discussion.
Study quality assessment and data extraction
Criteria provided by the Oxford Centre for Evidence-based Medicine were applied to assess the level of evidence (LOE) for all included studies [20], and the quality of non-randomized controlled trials (non-RCTs) was also assessed by Newcastle–Ottawa Scale [21]. Literature with an assessment score reaching seven or more stars was considered to be of high quality.
Data of all eligible studies regarding the following factors were extracted: study design, country, period, successful outcome definition, participant information (number, age, VUR grade, follow-up time, and group matched characteristics), operation-related information (operative time, estimated blood loss, and intraoperative complications), and relevant outcomes (length of stay, success rate, postoperative complications, postoperative Foley placement, postoperative analgesia usage, and hospital cost). Mean values with standard deviation (SD) of continuous data were extracted, and event and total numbers of related classified data were also collected. We also contacted the original authors for complete data if necessary.
Study end points and statistics analysis
The aim of this analysis was to compare the outcomes of RALUR with OUR for primary pediatric VUR based on published articles. Thus, surgical outcomes available in original studies were regarded as end points of this analysis, including operative time, length of stay, success rate, intraoperative and postoperative complications, estimated blood loss in surgery, postoperative Foley placement, postoperative analgesia usage, and hospital cost. Additionally, the success of surgical correction was defined as postoperative resolution of VUR by voiding cystourethrogram and absence of postoperative febrile urinary tract infection.
In this analysis, RevMan analytical software package (Version 5.3, Cochrane Collaboration, Oxford, UK) was used to combine the extracted data of eligible studies. Summarized mean differences (MDs) with 95% confidence intervals (CIs) were applied to assess the differences of outcomes for continuous variables between RALUR and OUR. Pooled odds ratios (ORs) with 95% CIs of success and complication rates were calculated to evaluate the efficacy and safety. Heterogeneity of included studies was assessed using the Chi square test-based Q- and I2- statistics [22]. If no heterogeneity was found with P > 0.10 in the heterogeneity test, the fixed-effect model was used to calculate the combined MD or OR values. Otherwise, a random-effect model was used. Only a two-sided P < 0.05 demonstrated that the results in the analysis were significant. Subgroup analyses were also conducted according to study design (comparative or cohort study), data source (single center or multiple centers), VUR laterality (unilateral or bilateral reimplantation), surgical technique (extravesical or intravesical reimplantation), and follow-up time (≤ 1 or > 1 year). The publication bias of all included studies was assessed by visual inspection of the inverted funnel plot.
Results
Eligible studies and characteristics
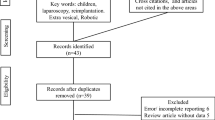
Six studies [8, 14, 15, 23,24,25] containing 7122 children with primary VUR were included in this systematic review and meta-analysis (Fig. 1). The characteristics of eligible studies are listed in Table 1. Included studies were performed between 2003 and 2014 and published between 2011 and 2016. All studies were conducted in the USA. In six included studies, four were designed as retrospective comparative studies [14, 15, 23, 24], and the remaining two were retrospective cohort studies [8, 25]. In all 7122 patients, 441 received RALUR and 6681 underwent OUR.
Quality assessment of eligible studies
As shown in Table 1, according to the LOE assessment, all included studies were rated Level 3. Under the Newcastle–Ottawa Scale, four studies [14, 15, 23, 24] with scores ≥ 7 stars were considered to be of high quality, and the other two studies [8, 25] scored 6 stars.
Operation time
Five studies [14, 15, 23,24,25] compared the operation time of RALUR with that of OUR. Meta-analysis by a random-effect model indicated that a longer operation time was needed for RALUR than OUR (MD 66.69 min, 95% CI 41.71–91.67, P < 0.00001) (Fig. 2). The results of subgroup analyses for operation time are shown in Table 2, and all revealed that significantly longer operation time was needed for RALUR compared with OUR.
Length of stay
The length of hospital stay between RALUR and OUR groups was compared in five studies [8, 14, 15, 23, 24]. Pooled data demonstrated that the RALUR group had a significantly shorter hospital stay time than the OUR group (MD − 17.80 h, 95% CI − 21.18 to − 14.42, P < 0.00001) without heterogeneity (I2 = 38%, P = 0.15) (Fig. 3). Table 3 demonstrates the subgroup analyses of length of hospital stay between these two groups, and all results indicated that significantly shorter time of hospital stay was needed by RALUR than OUR.
Success rate
The efficacy of RALUR versus OUR for surgical correction of pediatric VUR was evaluated in four comparative studies [14, 15, 23, 24], of which in all studies the mean follow-up time was longer than 1 year (range 14–22.5 months). The results of the meta-analysis demonstrated that no significant difference was found in the success rate between the two groups (OR 1.13, 95% CI 0.43–2.99, P = 0.80) without heterogeneity (I2 = 0%, P = 0.85) (Fig. 4). In subgroup analyses, none of the subgroups indicated a significant difference in the success rate (Table 4).
Postoperative complications
Five studies [14, 15, 23,24,25] compared the number of complications after RALUR with OUR. Significant heterogeneity (I2 = 71%, P = 0.004) existed, and no significant difference was found between RALUR and OUR in the number of postoperative complications (OR 0.77, 95% CI 0.28–2.15, P = 0.62) (Fig. 5). According to the sensitivity analysis, we found statistically significant heterogeneity in the study performed by Kurtz et al. [25], while in the other four studies [14, 15, 23, 24] no heterogeneity (I2 = 0%, P = 0.79) was found.
Kurtz et al. [25] conducted a retrospective cohort study from multiple centers. They found that the rate of postoperative complications in the RALUR group was significantly higher than in the OUR group (OR 3.17, 95% CI 1.72–5.85, P = 0.0002) after a 3-month follow-up (Table 5). The four other studies [14, 15, 23, 24] were retrospectively designed in a single center and had a follow-up time longer than 1 year. In this subgroup, no significant difference in the rate of postoperative complications was found between RALUR and OUR (OR 0.50, 95% CI 0.25–1.01, P = 0.05) (Table 5).
Other comparisons
Intraoperative complications from both groups were recorded in four studies [14, 15, 23, 24]; however, no cases were reported in all studies. In addition, the estimated blood loss, postoperative Foley placement, and postoperative analgesia usage were compared in only two studies. The results of the above comparisons are listed in Table 6. Significantly shorter days of postoperative Foley placement were found in RALUR than OUR. The hospital cost of RALUR and OUR was also compared in two studies [8, 25], of which both drew a conclusion that the cost of RALUR was significantly higher than that of OUR (median costs: $32409 vs. $22703, P < 0.001; median costs: $9128 vs. $7273, P = 0.049).
Publication bias
Through the inverted funnel plot, no publication bias was detected for all results in this meta-analysis.
Discussion
To the best of our knowledge, this is the first systematic review and meta-analysis comparing the efficacy and safety of RALUR and OUR for treating primary pediatric VUR. A total of six studies containing 7122 patients were included in this analysis. Our results indicated that patients receiving RALUR had a significantly longer operation time as well as shorter days of hospital stay and postoperative Foley placement than those receiving OUR. In addition, no significant differences were found in the estimated blood loss during operation, success rate, intraoperative and postoperative complications, and postoperative analgesia usage between the two groups. However, subgroup analyses in our study revealed that RALUR could induce more short-term postoperative complications. Therefore, compared with OUR, RALUR may also be considered as an effective surgical approach for primary pediatric VUR and could help patients shorten the time spent in the hospital to return to society more quickly; however, short-term postoperative complications of RALUR should be carefully considered.
Consistent with previous reports [14, 23, 24], our results indicated that RALUR was associated with longer operation time compared with OUR. It is reasonable and understandable that a surgical approach requiring dismembering and/or tapering lasts longer. Smith et al. [14] demonstrated that the operation time of RALUR was significantly longer, while the total operating room time did not demonstrate any differences. Schomburg et al. [23] also indicated that the bilateral procedure required a nearly twofold robotic console time than the unilateral procedure. Therefore, it is suggested that the bulk of time difference mainly resulted from the time in the operation itself and could not be attributed solely to robot setup time. Nevertheless, it has been shown that surgeons with adequate surgical experiences are more familiar with the RALUR technique, and thus less operation time is needed with increased robotic experience [26].
In this analysis, we found that RALUR was associated with shorter hospital stay and postoperative Foley placement than OUR. It is not surprising that as a minimally invasive approach, RALUR could accelerate the recovery of patients compared with an open approach. Postoperative analgesia usage of patients was compared in two studies [14, 23], and although the pooled results showed no significant difference, less analgesic usage in the RALUR group was reported in both studies. Therefore, a positive result in postoperative analgesia usage is also expected if the number of eligible studies is sufficient.
OUR has long been the gold standard of surgical correction for pediatric VUR with high success rates [27]. Our results showed that the success rate of RALUR was as high as that of OUR on the basis of a one-year follow-up. Four included studies in our analysis reported success rates of RALUR and OUR with a mean follow-up time ranging from 14 to 22.5 months, and the average success rates of the two groups were nearly identical (92.9% for RALUR and 91.9% for OUR). Herz et al. [28] also discovered a success rate of 85.2% for RALUR in a cohort with 54 children. Gundeti et al. [29] performed extravesical RALUR in 58 children and achieved a success rate of 87%. However, it is worth noting that some studies also reported wide-ranging success rates for RALUR [16,17,18]. Since no comparisons were conducted with open surgery, these studies were not eligible for our meta-analysis. As a result, although no significant difference in success rates between the two operation methods was found in our meta-analysis, the potentially unstable success rate of RALUR should also be considered.
Regarding postoperative complications, our results indicated that no significant difference existed between RALUR and OUR groups. Kurtz et al. [25] compared the 90-day complications between RALUR and OUR in a nationwide cohort of pediatric VUR patients, and they found that RALUR caused a significantly higher rate of 90-day complications than OUR. Although only one study compared the short-term postoperative complications between RALUR and OUR [25], the analyzed data were from multiple centers containing more than 1500 patients. Therefore, we should also focus on the short-term postoperative complications of RALUR. Furthermore, when the follow-up time was extended, the complication rate of RALUR was lower than half of that of OUR, with a P value of 0.05 in our analysis. In other words, although no significant difference has been identified yet, a significantly lower rate of postoperative complications in RALUR compared to OUR might be achieved if more eligible studies are included. Similar to our results, several previous studies also reported low complication rates of RALUR, ranging from 0 to 11% [16, 28,29,30]. Overall, RALUR has the advantage of fewer long-term postoperative complications compared with OUR.
In addition to the different operation methods, patients’ age and VUR grade could also impact the outcomes of VUR patients. Among the six included studies, the age of patients was similar, and there was no significant difference between RALUR and OUR groups in the two studies [14, 15], while significantly older age for the RALUR group was observed in the other four studies [8, 23,24,25] (P < 0.05). Additionally, Bowen et al. [8] revealed that age was an independent factor associated with the use of RALUR vs OUR (OR 1.12, 95% CI 1.02–1.08, P < 0.0001). Differences in age may lead to different features of VUR and certainly cause disparate outcomes after operations. Unfortunately, the original studies did not conduct stratified analyses based on a similar age of pediatric patients, and so related subgroup analyses were unable to be performed in our meta-analysis. Therefore, older patient age in RALUR group should be regarded as an important confounding factor. Regarding the VUR grade, since no significant differences existed between the RALUR and OUR groups in all included studies, it did not affect the outcomes of the two operation methods in this study.
Several limitations should be addressed regarding this analysis. First, all studies included were retrospective, and most were conducted in a single center, which could lead to some potential biases in the results, such as selective and detective biases. No RCTs on this topic were conducted or published as of yet, and further high-quality multicenter RCTs are necessary to confirm our results. Second, all included studies were conducted in the USA, which will likely influence the applicability of our results to other countries. Third, the number of eligible studies for some comparisons, including the estimated blood loss, postoperative Foley placement and postoperative analgesia usage, was relatively small. In addition, due to a lack of related stratified analyses in original studies, we could not perform the subgroup analyses according to some important factors, including age, VUR grade, detailed surgical technique, and single or duplicated systems, which may affect the outcomes and prognoses of pediatric VUR patients.
Conclusion
Our meta-analysis indicated that patients receiving RALUR had a significantly longer operation time, but fewer days of hospital stay and shorter postoperative Foley placement than those receiving OUR. No significant differences existed in the estimated blood loss during operation, success rate, intraoperative and postoperative complications, and postoperative analgesia usage between RALUR and OUR. Subgroup analyses in our study demonstrated that RALUR induced more short-term postoperative complications than OUR. Therefore, compared with OUR, RALUR should be considered as an effective surgical approach for primary pediatric VUR, since it has a similar success rate and could help patients shorten the time spent in the hospital to return to society sooner. However, pediatric urologists should pay more attention to the short-term postoperative complications of RALUR, and further high-quality multicenter RCTs are still needed to confirm our results.
References
Arant BS Jr (1991) Vesicoureteric reflux and renal injury. Am J Kidney Dis 17:491–511
Lich R, Howerton LW, Davis LA (1961) Recurrent urosepsis in children. J Urol 86:554–558
Atala A, Kavoussi LR, Goldstein DS, Retik AB, Peters CA (1993) Laparoscopic correction of vesicoureteral reflux. J Urol 150:748–751
Peters CA (2004) Laparoscopic and robotic approach to genitourinary anomalies in children. Urol Clin N Am 31:595–605
Elder JS (2000) Guidelines for consideration for surgical repair of vesicoureteral reflux. Curr Opin Urol 10:579
Tekgül S, Riedmiller H, Hoebeke P, Kočvara R, Nijman RJ, Radmayr C, Stein R, Dogan HS, European Association of Urology (2012) EAU guidelines on vesicoureteral reflux in children. Eur Urol 62:534–542
Weiss DA, Shukla AR (2015) The robotic-assisted ureteral reimplantation: the evolution to a new standard. Urol Clin N Am 42:99e109
Bowen DK, Faasse MA, Liu DB, Gong EM, Lindgren BW, Johnson EK (2016) Use of pediatric open, laparoscopic and robot-assisted laparoscopic ureteral reimplantation in the United States: 2000 to 2012. J Urol 196:207–212
Jodal U, Smellie JM, Lax H, Hoyer PF (2006) Ten-year results of randomized treatment of children with severe vesicoureteral reflux. Final report of the International Reflux Study in children. Pediatr Nephrol 21:785
Ehrlich RM, Gershman A, Fuchs G (1994) Laparoscopic vesicoureteroplasty in children: initial case reports. Urology 43:255
Janetschek G, Radmayr C, Bartsch G (1995) Laparoscopic ureteral anti-reflux plasty reimplantation. First clinical experience. Ann Urol 29:101
Peters CA (2004) Robotically assisted surgery in pediatric urology. Urol Clin N Am 31:743
Casale P (2009) Robotic pyeloplasty in the pediatric population. Curr Opin Urol 19:97
Smith RP, Oliver JL, Peters CA (2011) Pediatric robotic extravesical ureteral reimplantation: comparison with open surgery. J Urol 185:1876
Marchini GS, Hong YK, Minnillo BJ, Diamond DA, Houck CS, Meier PM, Passerotti CC, Kaplan JR, Retik AB, Nguyen HT (2011) Robotic assisted laparoscopic ureteral reimplantation in children: case matched comparative study with open surgical approach. J Urol 185:1870–1875
Akhavan A, Avery D, Lendvay TS (2014) Robot-assisted extravesical ureteral reimplantation: outcomes and conclusions from 78 ureters. J Pediatr Urol 10:864–868
Grimsby GM, Dwyer ME, Jacobs MA, Ost MC, Schneck FX, Cannon GM, Gargollo PC (2015) Multi-institutional review of outcomes of robot-assisted laparoscopic extravesical ureteral reimplantation. J Urol 193:1791–1795
Dangle PP, Shah A, Gundeti MS (2014) Robot-assisted laparoscopic ureteric reimplantation: extravesical technique. BJU Int 114:630–632
Peters CA, Skoog SJ, Arant BS Jr, Copp HL, Elder JS, Hudson RG, Khoury AE, Lorenzo AJ, Pohl HG, Shapiro E, Snodgrass WT, Diaz M (2010) Summary of the AUA guideline on management of primary vesicoureteral reflux in children. J Urol 184:1134
Phillips B, Ball C, Sackett D (2011) Oxford centre for evidence-based medicine 2011 levels of evidence. CEBM Available from: http://www.cebm.net/ocebm-levels-of-evidence/. Accessed 01 May 2016
Stang A (2010) Critical evaluation of the Newcastle–Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25:603–605
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ (Clin Res Ed) 327:557–560
Schomburg JL, Haberman K, Willihnganz-Lawson KH, Shukla AR (2014) Robot-assisted laparoscopic ureteral reimplantation: a single surgeon comparison to open surgery. J Pediatr Urol 10:875–879
Arlen AM, Broderick KM, Travers C, Smith EA, Elmore JM, Kirsch AJ (2016) Outcomes of complex robot-assisted extravesical ureteral reimplantation in the pediatric population. J Pediatr Urol 12:169.e1–169.e6
Kurtz MP, Leow JJ, Varda BK, Logvinenko T, Yu RN, Nelson CP, Chung BI, Chang SL (2016) Robotic versus open pediatric ureteral reimplantation: Costs and complications from a nationwide sample. J Pediatr Urol 12:408.e1–408.e6
Di Lorenzo N, Coscarella G, Faraci L, Konopacki D, Pietrantuono M, Gaspari AL (2005) Robotic systems and surgical education. JSLS 9:3–12
Sung J, Skoog J (2012) Surgical management of vesicoureteral reflux in children. Pediatr Nephrol 27:551–561
Herz D, Fuchs M, Todd A, McLeod D, Smith J (2016) Robot-assisted laparoscopic extravesical ureteral reimplant: a critical look at surgical outcomes. J Pediatr Urol 12:402.e1–402.e9
Gundeti MS, Boysen WR, Shah A (2016) Robot-assisted laparoscopic extravesical ureteral reimplantation: technique modifications contribute to optimized outcomes. Eur Urol 70:818–823
Hayashi Y, Mizuno K, Kurokawa S, Nakane A, Kamisawa H, Nishio H, Moritoki Y, Tozawa K, Kohri K, Kojima Y (2014) Extravesical robot-assisted laparoscopic ureteral reimplantation for vesicoureteral reflux: initial experience in Japan with the ureteral advancement technique. Int J Urol 21:1016–1021
Acknowledgements
This work was supported by the China Postdoctoral Science Foundation (Grant number 2017M612636), the National Natural Science Foundation of China (Grant numbers 81370804, 81670643), and the Guangzhou Science Technology and Innovation Commission (Grant numbers 201604020001, 201704020193).
Author information
Authors and Affiliations
Contributions
TD: project development, data collection, data analysis, and manuscript writing; BL: data collection, data analysis, and manuscript writing; LL: data collection and manuscript writing; XD: data collection; CC: data analysis; ZZ: manuscript editing; WZ: manuscript editing; WW: manuscript editing; GZ: project development and manuscript editing.
Corresponding author
Ethics declarations
Ethical approval
No ethical approval was necessary due to its exclusive use of secondary data.
Conflict of interest
The authors declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Deng, T., Liu, B., Luo, L. et al. Robot-assisted laparoscopic versus open ureteral reimplantation for pediatric vesicoureteral reflux: a systematic review and meta-analysis. World J Urol 36, 819–828 (2018). https://doi.org/10.1007/s00345-018-2194-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-018-2194-x