Abstract
Objectives
To prospectively evaluate the effect of hyoscine butylbromide (HBB) on visualisation of anatomical details and motion-related artefacts in mp-MRI of the prostate at 3.0 Tesla.
Methods
One hundred and three consecutive patients (65 ± 10 years) were included in this trial, powered to demonstrate an improvement of image quality after HBB administration, assessed on a 5-point scale by two blinded readers. All patients received high-spatial resolution axial T2-weighted TSE sequences at 3.0 T without spasmolytic agent, repeated after application of 40 mg HBB and followed by routine mp-MRI. Secondary endpoints were (1) susceptibility to side effects, (2) dependence of spasmolytic effect on patients´ weight, and (3) prostate volume.
Results
In 68% of patients, HBB significantly improved the anatomic score (mean 3.4 ± 0.9 before and 4.4 ± 0.7 after HBB for both readers, p = <0.001). In 67%, HBB significantly enhanced the artefact score (mean 3.2 ± 1 before and 4.2 ± 0.8 after HBB for reader 1, p = <0.001; 3.2 ± 1 and 4.1 ± 0.8 for reader 2, p = <0.001). Subgroup analysis revealed no statistically significant difference between patients with different bodyweight or prostate volume. Inter-reader agreement was excellent (k = 0.95–0.98).
Conclusions
Hyoscine butylbromide significantly improves image quality and reduces motion-related artefacts in mp-MRI of the prostate independent of bodyweight or prostate volume. No side effects were reported.
Key Points
• Hyoscine butylbromide (HBB) improved image quality in over 2/3 of patients.
• Severe artefacts were reduced after HBB in more than 20%.
• The number of non-diagnostic MRI was reduced to <1% after HBB.
• HBB effect was independent of bodyweight and prostate volume.
• No side effects of HBB were reported in this study population.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Multiparametric magnetic resonance imaging (mp-MRI) of the prostate has assumed a major role in detection, localisation and staging of prostate cancer [1,2,3,4]. Besides morphologic T2-weigthed sequences, at least two functional techniques are employed, which commonly include diffusion-weighted imaging (DWI) and dynamic contrast-enhanced (DCE) images [5,6,7]. In order to diminish motion-related artefacts, a majority of MRI studies of the prostate and other pelvic organs are performed with administration of an anti-peristaltic drug prior to the examination to reduce movement of prostate surrounding structures like the bladder, the rectum, and the small or large bowel, potentially impairing image quality and diagnostic performance [8, 9]. Therefore, usually hyoscine-N-butyl-bromide (hyoscine butylbromide, HBB, scopolamine butylbromide, butylscopolamine; trade name: Buscopan®) or glucagon are applied [10, 11].
Whereas administration of anti-peristaltic medication is recommended by several studies [8, 12] and considered to be potentially beneficial by the joint guidelines of the European Society of Urogenital Radiology (ESUR), the American College of Radiology (ACR) and the AdMeTech Foundation (PI-RADS Prostate Imaging – Reporting and Data System: 2015, Version 2; PI-RADS v2) [13], some studies did not find a significant effect on image quality [14, 15], putting into question the general necessity of these drugs for mp-MRI of the prostate. However, all available studies either examined two different cohorts with or without HBB or used endorectal coils, which largely immobilise the prostate in the lower pelvis but entail other disadvantages such as discomfort for the patient, anatomical distortion or even mechanical stimuli for intestinal peristalsis [14]. Since the extent of bowel movement-related artefacts varies considerably dependent on factors such as the filling, the amount of intraluminal gas, diet, and the individual anatomy, a comprehensive, intra-individual comparison of motion-related artefacts is still lacking.
Therefore, this prospective study evaluates the effect of hyoscine butylbromide on image quality of MRI of the prostate within the same patients without the use of an endorectal coil.
Material and methods
Study design
This prospective study was approved by the local institutional review board and written informed consent was obtained from all subjects. One hundred and three consecutive patients with elevated prostate-specific antigen (PSA) levels who underwent mp-MRI of the prostate were included over a period of 12 months. Exclusion criteria were glaucoma, cardiac arrhythmia and/or ischemic heart disease, myasthenia gravis, known allergy against hyoscine butylbromide (HBB), and active participation in public traffic (e.g. drivers) [16]. All patients first received high-spatial resolution T2-weighted turbo spin echo sequences in the transverse plane without a spasmolytic agent. Subsequently, 40 mg of HBB (Buscopan®; Boehringer, Ingelheim, Germany) were in-room administered intravenously according to the manufacturer’s protocol. Hereafter, all patients received routine mp-MRI including T1WI and T2WI sequences, DWI sequences, and DCE sequences according to the European Society of Urogenital Radiology (ESUR) guidelines, with conduction of the additional axial T2-weighted turbo spin echo sequence after HBB administration according to the pharmacokinetic profile with a plasma half-life of HBB (t½α = 4 min). To investigate if patients´ weight or prostate volume influence the HBB effect on image quality, the study population was separated into two groups, respectively. Patients with a bodyweight under 85 kg were compared to patients higher than or equal to 85 kg and patients with a prostate volume higher or equal to 50 ml to patients with prostate volumes under 50 ml. Subsequently, scores for anatomical details and motion-related artefacts of the respective groups were related and statistically analysed. Occurrence of side effects including nausea, constipation, visual changes, cardiovascular complaints, tiredness, dizziness, or abdominal pain was recorded 30 minutes after each examination.
Study endpoints
The primary endpoint of the study was to determine more than 10% improvement of the scores for visualisation of anatomical details and for motion-related artefacts after administration of HBB in axial T2WI based on a 5-point Likert scale. Secondary endpoints were (1) susceptibility to side effects of HBB, (2) dependence of spasmolytic effect on patients´ weight, and (2) prostate volume.
Imaging protocols
Multiparametric MR images were obtained using a 3 T MRI scanner (Magnetom Trio, Siemens Healthcare GmbH) with a body coil in accordance with the recommendations of a European Consensus Meeting [17]. Detailed imaging parameters have been published previously [18], containing T2-weighted turbo-spin echo (TSE) sequences in three planes [axial: voxel size 0.5 x 0.5 x 3.0 mm; field of view (FOV) 128 mm; acquisition time 8:21 min], axial T1-weighted TSE images, diffusion-weighted imaging (DWI), and DCE imaging. Apparent diffusion coefficient (ADC) parameter maps were calculated using the standard monoexponential model. The additional axial T2-weighted turbo spin echo sequence prior to HBB administration was conducted in the same way.
Imaging analysis
The acquired datasets were analysed by two radiologists (LS and TU) with 7 and 3 years of experience in reading prostate MR on a picture archiving and communication system (PACS; Sectra Imtec AB, IDS7, Linköping, Schweden). Both radiologists were blinded to administration of HBB and among themselves. Anatomical detail on T2WI was classified on a 5-point scale according to image criteria previously described by Wagner et al. [15]: (1) unacceptable: non-diagnostic, structures cannot be evaluated; (2) poor: poor visualisation; heavily blurred appearance of structures; (3) moderate: moderate visualisation, moderate blurring; (4) good: good delineation, slight blurring; and (5) excellent: excellent visualisation, sharp delineation. Criteria were visualisation of the capsule, apical and basal organ borders, the ejaculatory ducts and seminal vesicles, delineation between peripheral and transitional zone, distinction of nodules in the transitional zone, and depiction of the neurovascular bundle. Scores of 1 and 2 were considered as not sufficient for adequate diagnosis. Motion-related artefacts were similarly scored as (1) unacceptable: severely affected; (2) poor: considerable artefacts; (3) moderate: moderate artefacts; (4) good: few artefacts; (5) excellent: no artefacts. Prostate volume was measured on axial and sagittal T2WI (height x width x depth x 0.52). All mp-MRI datasets were independently assessed as part of the clinical routine according to the ESUR guidelines (PI-RADS).
Histopathology
After mp-MRI, 27 patients underwent either MRI-guided biopsy (MR-GB), transrectal ultrasound-guided biopsy (TRUS-GB), MRI-ultrasound fusion-guided biopsy (FUS-GB), or a combination of the latter two. All biopsy cores were histopathologically evaluated according to the recommendations of the International Society of Urological Pathology [19].
Sample size calculation and statistical analysis
This prospective study was powered at 80% to show a more than 10% improvement in image quality scores after HBB administration with a type 1 error rate of 0.05. One-hundred patients were planned to be enrolled. Statistical analysis was performed using IBM SPSS® Statistics (Version 21, IBM Deutschland GmbH, Ehningen, Germany). Data are expressed as mean ± SD and interquartile range (IQR), respectively. Non-parametric data were tested with the Mann–Whitney U test (MWU). Cohen´s kappa coefficient was calculated as a measure of random-corrected agreement. The inter-reader agreement for image quality was defined as excellent (κ > 0.81), good (κ = 0.61–0.80), moderate (κ = 0.41–0.60), fair (κ = 0.21–0.40), and poor (κ ≤ 0.20). Statistical significance was defined as a p value < 0.05.
Results
Patient population
Baseline characteristics of the 103 included patients are shown in Table 1. The group of patients with a bodyweight <85 kg consisted of 56 people with an average weight of 76 ± 6.1 kg (age 65 ± 9 y; PSA 7.5 ng/ml, IQR: 6.2–11.8 ng/ml). The group of patients weighing ≥85 kg consisted of 47 people with an average weight of 93 ± 10 kg (age 64 ± 10y, p value 0.6; PSA 7.6 ng/ml, IQR 6.4–12 ng/ml, p value 0.5). Fifty-six patients had a prostate volume ≤50 ml with a median of 38 ml (IQR: 28–45 ml; age 64 ± 11 y; PSA 7.4 ng/ml, IQR 6.1–12 ng/ml). Forty-seven patients’ prostate volume was >50 ml with a median of 67 ml (IQR 60–78 ml; age 66 ± 18 y, p value 0.8; PSA 7.6 ng/ml, IQR 6.5–12 ng/ml; p value 0.7). The respective groups showed no statistical difference regarding age or PSA levels. Twelve patients were in active surveillance with known low-grade prostate cancer during the study period. Twenty-seven patients received prostate biopsy with 24 patients positive for prostate cancer. Of these, 13 patients had higher grade cancer, defined as Gleason score ≥ 4 + 3 = 7b. The remaining 64 patients were either scheduled for follow-up MRI or were clinically followed up. No side effects of the given anti-peristaltic medication were reported.
Imaging analysis
Both readers (R1 and R2) gave significantly higher scores for visualisation of anatomic details after HBB administration with a mean score of 3.4 ± 0.9 before and 4.4 ± 0.7 after HBB (p = <0.001; Table 2; Fig 1). Artefacts were significantly reduced with mean scores of 3.2 ± 1 before and 4.2 ± 0.8 after HBB for R1 (p = <0.001) and 3.2 ± 1 and 4.1 ± 0.8 for R2 (p = <0.001), respectively (Table 2). Table 3 illustrates changes of scores before and after HBB administration on a patient level. The readers gave higher scores for visualisation of anatomic details in a mean of 70 patients (R1 = 71, R2 = 69; 68%) after HBB (Fig. 2). The number of patients with a score lower than 3, which was defined as non-diagnostic, was reduced from 12 (12%) before HBB to 1 (<1%) after HBB for both readers. The number of excellent scores (5) increased by 39 (38%) for R1 and by 35 (34%) for R2. Artefacts were reduced in 70 patients (68%) for R1 and 68 patients (66%) for R2. The numbers of patients with scores lower than 3 for motion-related artefacts were reduced from 26 before to 2 after HBB for R1 and from 27 to 2 for R2 (reduction from 25% to <2%). Higher scores before HBB administration were given to nine patients from R1 when assessing visualisation of anatomical details and to six patients when assessing motion-related artefacts and to nine and seven patients from R2, respectively. An example of image quality improvement is demonstrated in Fig. 3. Comparison of the groups with a bodyweight <85 kg vs. ≥85 kg and with a prostate volume ≤50 ml vs. >50 ml revealed no statistically significant difference regarding scores for anatomic details and artefacts. Scores for visualisation of anatomic details were significantly higher than scores for artefacts pre- and post-HBB for both readers (Table 2).
Anatomic scores (visualisation of anatomical details) and artefact scores (motion related artefacts) as assessed on a 5-point scale by two blinded readers (R1 and R2) before and after administration of hyoscine butylbromide (HBB). Anatomic scores are significantly better after HBB for both readers. Higher artefact scores represent significant reduction of artefacts for both readers after HBB. Note: Brighter columns: R1, darker columns: R2
Number of patients with higher scores before or after administration of hyoscine butylbromide (HBB) or with equal scores before and after HBB as assessed on a 5-point scale by two blinded readers (R1 and R2). More patients received higher scores for anatomical details after HBB from both readers. Higher scores of motion related artefacts after HBB represent reduction of artefacts. Note: Brighter columns: R1, darker columns: R2
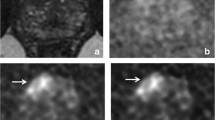
Example of image quality at 3.0 T before and after hyoscine butylbromide (HBB) administration: 52-year-old patient with elevated PSA level (9.1 ng/ml) and histologically proven high-grade prostate carcinoma (Gleason score 4 + 4 = 8) in the left anterior transitional and peripheral zone. a Shows the T2WI before and b illustrates T2WI after HBB administration with clearly improved visualisation of the capsule, the organ borders, and the tumor as well as enhanced delineation between peripheral and transitional zones.
Inter-reader analysis
The inter-reader agreement was excellent (κ > 0.81) for all criteria with κ = 0.97 for anatomical details before HBB, κ = 0.96 for anatomical details after HBB, κ = 0.98 for artefacts before HBB, and κ = 0.95 for artefacts after HBB.
Discussion
Anti-peristaltic agents like the parasympatholytic hyoscine-N-butyl-bromide (hyoscine butylbromide, HBB; butylscopolamine; trade name: Bucopan®) are commonly recommended and used in pelvic MRI studies to reduce motion-related artefacts despite the lack of clear evidence for improvement of image quality [8]. Our results demonstrate a significant improvement of visualisation of anatomic detail of the prostate and a clear reduction of motion-related artefacts after administration of HBB.
Good visualisation of the relevant anatomic structures is the basis for accurate diagnostics and facilitates tumour detection.
Our findings are in accordance with retrospective results reported by Johnson et al. [8] who revealed improved visualisation of the prostate in 40% of the patients after administration of HBB. Use of HBB is also considered to be potentially beneficial for prostate MRI by the joint guidelines of the European Society of Urogenital Radiology (ESUR), the American College of Radiology (ACR) and the AdMeTech Foundation (PI-RADS Prostate Imaging - Reporting and Data System: 2015, Version 2) [13]. In contrast, a previous study by Roethke et al. did not find a significant effect of HBB on image quality of prostate MRI [14]. However, their study was retrospectively designed and two different patient groups either with or without HBB were compared. Given the broad anatomic variety, the different amount of intraluminal gas and filling, an intra-individual comparison within one MRI examination in consecutive order is, in our opinion, a more reliable study design.
Another retrospective inter-individual comparison conducted by Wagner et al. reported a positive effect of HBB on the delineation of the bowel wall in PD-weighted images at 1.5 T [15]. The investigators, however, used an endorectal coil, which largely immobilises the prostate in the lower pelvis. According to the current guidelines, endorectal coils can be waived at both 3 T and at 1.5 T which allows higher patient comfort and reduces costs at comparable image quality and diagnostic accuracy [20,21,22]. Furthermore, the inflated endorectal coil can even constitute a mechanical stimulus for rectal movement. Nevertheless, our findings are in accordance to the results by Wagner et al. both, with respect to the number of artefacts and visualisation of anatomic details before and after HBB [15].
As stated above, gas or stool in the rectum can lead to considerable motion artefacts in the prostate through rectal peristalsis. In this study, motion-related artefacts could be reduced to a satisfactory minimum by administering HBB. In order to remove rectal gas, rectal enemas or rectal tubes can be used, but due to lack of data on this issue, the general inconvenience for the patient, and the extra amount of time being necessary, it is not generally recommended for clinical routine.
We exclusively injected HBB intravenously. Other groups conducted intramuscular injections of HBB and presume a longer duration of action [15]. Since the plasma half-life (t½α) of HBB is relatively short (4 minutes), we performed axial T2WI at the beginning of the examination when the HBB effect is maximal. This decision was made based on our experience that T2WI is the most susceptible to motion due to the long acquisition times. A direct comparison of the HBB effect when administered intravenously and intramuscularly might be of interest.
In favour of a uniform protocol, we used HBB for each examination. Other investigators reported good results with glucagon in MRI studies of the abdomen at 1.5 T [10]. Glucagon can be used as a substitute in patients with contraindications to HBB; however, higher costs and off-label use have to be considered. Potential hazards and side effects need to be taken into account and precautions must be taken when applying HBB [16]. Nevertheless, the known side effects are usually minor and self-limiting. Patients examined in this cohort did not complain about any HBB-related side effects.
There are some limitations of this study. We focused on image quality, but further studies should investigate differences and relevance for cancer detection rates with or without HBB. Patients might adjust to the supine position over the course of time, possibly in favour of a sharper image in later measurements. However, patients might also become restless after a certain time, possibly blurring later measurements. A randomised study design including a control group with, e.g. saline injection, might have further excluded a reduction of artefacts only as a result of time of simply lying on the table. Since both T2WI sequences were conducted immediately one after the other with HBB administration in the interim, the influence of patient and intestinal relaxing by time is assumably low. Also, the duration of HBB and the maximum and/or sustained effect on T2WI imaging are worth investigating in future studies. Furthermore, in this study, we focused on the effect of HBB on T2WI, since it is the most important sequence for anatomic evaluation. Finally, the study is limited by subjective evaluation of the image quality.
In conclusion, administration of HBB significantly improved visualisation of anatomic details and substantially reduced motion-related artefacts in mp-MRI of the prostate. In almost 70% of all patients, image quality was improved by application of HBB, artefacts were reduced about 20%, and non-diagnostic MRI could be reduced to less than 1%. No side effects of HBB were reported. Administration of HBB must, therefore, be recommended for mp-MRI.
Abbreviations
- mp-MRI:
-
Multiparametric magnetic resonance imaging
- HBB:
-
Hyoscine butylbromide; scopolamine butylbromide; butylscopolamine
- T2WI:
-
T2-weighted imaging
- DWI:
-
Diffusion-weighted imaging
- DCE:
-
Dynamic contrast-enhanced imaging
- PSA:
-
Prostate-specific antigen
- IQR:
-
Interquartile range
- ESUR:
-
European Society of Urogenital Radiology
- ACR:
-
American College of Radiology
- PI-RADS:
-
Prostate imaging reporting and data system, version 2
- PCA:
-
Prostate cancer
- MR-GB:
-
MRI-guided biopsy
References
Ahmed HU, El-Shater Bosaily A, Brown LC et al (2017) Diagnostic accuracy of multi-parametric MRI and TRUS biopsy in prostate cancer (PROMIS): a paired validating confirmatory study. Lancet 389:815–822
Murphy G, Haider M, Ghai S, Sreeharsha B (2013) The expanding role of MRI in prostate cancer. Am J Roentgenol 201:1229–1238
Schimmöller L, Quentin M, Arsov C et al (2014) Predictive power of the ESUR scoring system for prostate cancer diagnosis verified with targeted MR-guided in-bore biopsy. Eur J Radiol 12:2103–2108
Schoots IG, Roobol MJ, Nieboer D, Bangma CH, Steyerberg EW, Hunink MG (2015) Magnetic resonance imaging-targeted biopsy may enhance the diagnostic accuracy of significant prostate cancer detection compared to standard transrectal ultrasound-guided biopsy: a systematic review and meta-analysis. Eur Urol 68:438–450
Dias JL, Pina JM, Joao R et al (2015) Multiparametric resonance imaging. Acta Medica Port 28:240–249
De Visschere PJ, Briganti A, Fütterer JJ et al (2016) Role of multiparametric magnetic resonance imaging in early detection of prostate cancer. Insights Imaging 2:205–214
De Visschere PJ, Vral A, Perletti G et al (2017) Multiparametric magnetic resonance imaging characteristics of normal, benign and malignant conditions in the prostate. Eur Radiol 5:2095–2109
Johnson W, Taylor MB, Carrington BM, Bonington SC, Swindell R (2007) The value of hyoscine butylbromide in pelvic MRI. Clin Radiol 62:1087–1093
Park SH, Huh J, Park SH, Lee SS, Kim AY, Yang SK (2016) Diffusion-weighted MR enterography for evaluating Crohn's disease: effect of anti-peristaltic agent on the diagnosis of bowel inflammation. Eur Radiol. doi:10.1007/s00330-016-4609-8
Froehlich JM, Daenzer M, von Weymarn C, Erturk SM, Zollikofer CL, Patak MA (2009) Aperistaltic effect of hyoscine N-butylbromide versus glucagon on the small bowel assessed by magnetic resonance imaging. Eur Radiol 19:1387–1393
Marti-Bonmati L, Graells M, Ronchera-Oms CL (1996) Reduction of peristaltic artefacts on magnetic resonance imaging of the abdomen: a comparative evaluation of three drugs. Abdom Imaging 21:309–313
Dosdá R, Martí-Bonmatí L, Ronchera-Oms CL, Mollá E, Arana E (2002) Effect of subcutaneous butylscopolamine administration in the reduction of peristaltic artifacts in 1.5-T MR fast abdominal examinations. Eur Radiol 13:294–298
Weinreb JC, Barentsz JO, Choyke PL et al (2016) PI-RADS prostate imaging – reporting and data system: 2015, version 2. Eur Urol 69:16–40
Roethke MC, Kuru TH, Radbruch A, Hadaschik B, Schlemmer HP (2013) Prostate magnetic resonance imaging at 3 Tesla: is administration of hyoscine-N-butyl-bromide mandatory? World J Radiol 5:259–263
Wagner M, Rief M, Busch J et al (2010) Effect of butylscopolamine on image quality in MRI of the prostate. Clin Radiol 65:460–464
Dyde R, Chapman AH, Gale R, Mackintosh A, Tolan DJ (2008) Precautions to be taken by radiologists and radiographers when prescribing hyoscine-N-butylbromide. Clin Radiol 63:739–743
Barentsz JO, Richenberg J, Clements R et al (2012) ESUR prostate guidelines 2012. Eur Radiol 22:746–757
Schimmöller L, Quentin M, Arsov C et al (2014) MR-sequences for prostate cancer diagnostics: validation based on the PI-RADS scoring system and targeted MR-guided in-bore biopsy. Eur Radiol 24:2582–2589
Epstein JI, Allsbrook WC Jr, Amin MB, Egevad LL, Grading Committee ISUP (2005) The 2005 International Society of Urological Pathology (ISUP) consensus conference on Gleason grading of prostatic carcinoma. Am J Surg Pathol 29:1228–1242
Shah ZK, Elias SN, Abaza R et al (2015) Performance comparison of 1.5-T endorectal coil MRI with 3.0-T nonendorectal coil MRI in patients with prostate cancer. Acad Radiol 22:467–474
Schimmöller L, Blondin D, Arsov C et al (2016) MRI-guided in-bore biopsy: differences between prostate cancer detection and localisation in primary and secondary biopsy settings. AJR Am J Roentgenol 206:92–99
Ullrich T, Quentin M, Oelers C et al (2017) Magnetic resonance imaging of the prostate at 1.5 versus 3.0 Tesla: a prospective comparison study of image quality. Eur J Radiol. doi:10.1016/j.ejrad.2017.02.044
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Lars Schimmöller.
Conflict of interest
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Funding
The authors state that this work has not received any funding.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was obtained from all subjects (patients) in this study.
Ethical approval
Institutional review board approval was obtained.
Methodology
• prospective
• diagnostic or prognostic study
• performed at one institution
Rights and permissions
About this article
Cite this article
Ullrich, T., Quentin, M., Schmaltz, A.K. et al. Hyoscine butylbromide significantly decreases motion artefacts and allows better delineation of anatomic structures in mp-MRI of the prostate. Eur Radiol 28, 17–23 (2018). https://doi.org/10.1007/s00330-017-4940-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-017-4940-7