Abstract
Objective
To investigate the feasibility of highly efficient and controllable stem cell labelling for cellular MRI.
Methods
A new class of cationic, superparamagnetic iron oxide nanoparticle (SPION)-loaded nanovesicles was synthesised to label rat bone marrow mesenchymal stem cells without secondary transfection agents. The optimal labelling conditions and controllability were assessed, and the effect of labelling on cell viability, proliferation activity and multilineage differentiation was determined. In 18 rats, focal ischaemic cerebral injury was induced and the rats randomly injected with 1 × 106 cells labelled with 0-, 8- or 20-mV nanovesicles (n = 6 each). In vivo MRI was performed to follow grafted cells in contralateral striata, and results were correlated with histology.
Results
Optimal cell labelling conditions involved a concentration of 3.15 μg Fe/mL nanovesicles with 20-mV positive charge and 1-h incubation time. Labelling efficiency showed linear change with an increase in the electric potentials of nanovesicles. Labelling did not affect cell viability, proliferation activity or multilineage differentiation capacity. The distribution and migration of labelled cells could be detected by MRI. Histology confirmed that grafted cells retained the label and remained viable.
Conclusion
Stem cells can be effectively and safely labelled with cationic, SPION-loaded nanovesicles in a controllable way for cellular MRI.
Key Points
• Stem cells can be effectively labelled with cationic, SPION-loaded nanovesicles.
• Labelling did not affect cell viability, proliferation or differentiation.
• Cellular uptake of SPION could be controlled using cationic nanovesicles.
• Labelled cells could migrate along the corpus callosum towards cerebral infarction.
• The grafted, labelled cells retained the label and remained viable.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Stem cell therapy has brought revolutionary changes to regenerative medicine and cancer treatment [1] and has achieved gratifying results in various tissue, ischaemic, degenerative, and even immune and genetic diseases [2]. In vivo tracking of stem cells is very important for better understanding of their migrational dynamics, differentiation processes and regeneration potential [3, 4]. Cellular MRI upon cell labelling was a well-suited tool for monitoring the extent of transplanted cell survival and trafficking [5]. For cell labelling, superparamagnetic iron oxide nanoparticles (SPION) became the preferred contrast agents in terms of biocompatibility and higher sensitivity [6], whereas the non-modified form of SPION could not efficiently label stem cells [7, 8]. Various commercial transfection agents (TA) are usually needed to transfer SPION into cells [8]. Less frequently, chemical polymers or microbubble-enhanced ultrasound exposure has been used for non-specific intracellular magnetic labelling [9–11].
However, using TA for cell labelling has saturation effects, and high concentrations of TA are harmful to cells [8, 12]. Some TA can damage the cell membrane a few hours after transfection, and the labelling efficiency is not controllable [13]. The control of the amount of contrast agents transferred to cells is usually poorly determined. It is rather difficult to assess precisely the amount of contrast agents incorporated by a single cell [14]. Therefore, a highly efficient and controllable cell-labelling method that facilitates direct delivery of SPION into cells without use of a secondary TA would be highly desirable.
Polymeric nanoparticles have been extensively used in the transfer of genes and drugs, showing high transmission efficiency, less toxicity and active targeting effects [15, 16]. In this study, we synthesised novel cationic, polymeric nanovesicles with a unique hollow structure where SPION were loaded, and with positive charges on the surface to allow the quantity of charges to be adjusted for labelling bone marrow mesenchymal stem cells (MSC). Cellular MRI was performed to determine the feasibility of this efficient, controllable cell labelling through use of cationic SPION-loaded nanovesicles.
Materials and methods
Animals
The animals were obtained from the Animal Experiment Center of our university. All animals were housed in a standard animal facility and allowed standard food and water ad libitum. All procedures adhered to the guidelines for the care and use of laboratory animals and the ethics review process of our institution and were approved by the Institutional Animal Care Committee. Four adolescent Sprague-Dawley (SD) rats (aged 4–6 weeks) weighing 60–80 g were used as the donors of bone marrow MSC. Eighteen adult male SD rats weighing 250–280 g were used to establish focal ischaemic cerebral injury.
Cell preparation
Mesenchymal stem cells were isolated and expanded from the bone marrow of adolescent animals as described previously [17]. Cells were grown in a standard culture medium consisting of Dulbecco’s Modified Eagle Medium (DMEM, GiBco, NY, USA) supplemented with penicillin, streptomycin and glutamine (Sigma, St. Louis, MO, USA) and 10% fetal bovine serum (FBS, GiBco, NY, USA) at 37°C and 5% CO2, and were routinely passaged with a ratio of 1:2 to 1:3. MSC of three to five passages were used in the following experiments.
Synthesis and characterisation of copolymers
First, stearic acid–grafted polyethyleneimine copolymers (PEI-SA) were synthesised. Briefly, linear polyethyleneimine (lPEI, 423 Da, Sigma-Aldrich; 400 mg, 1 eq) and stearic acid (SA, Sigma-Aldrich; 800 mg, 3 eq) were transferred into the reaction flask and dried under vacuum at 70°C for 8 h. Chloroform (15 mL), dicyclohexylcarbodiimide (Sigma-Aldrich; 780 mg, 4 eq) and 4-dimethylaminopyridine (Sigma-Aldrich; 115 mg, 1 eq) were added under Ar protection. The mixture was stirred at room temperature for 24 h. The precipitated 1,3-dicyclohexylurea was removed by filtration, and the filtrate was added into excessive cold diethyl ether (Guangzhou Chemical Industry, China). Then stearic acid–grafted polyethyleneimine copolymers (PEI-SA) were collected by filtration and dried under vacuum at room temperature. Second, poly(ethylene glycol)-poly(L-glutamic acid) (PEG-PGA) was synthesised as described previously [18]. Briefly, poly(ethylene glycol)-poly(γ-benzyl-L-glutamate) (PEG-PBLG) (Mn = 9.3 kDa) was synthesised by ring-opening polymerisation of β-benzyl-L-aspartate N-carboxyanhydride using PEG-NH2 (Mn = 3.7 kDa) as a macroinitiator. PEG-PGA (Mn = 6.7 kDa) was obtained from PEG-PBLG by deprotection in HBr/HAc solution. 1H nuclear magnetic resonance (NMR) was carried out to confirm the synthesis of the designed copolymers by using a Varian 300-MHz NMR spectrometer in deuterated chloroform (CDCl3) at room temperature.
Synthesis of Fe3O4 nanoparticles
Fe3O4 nanoparticles (SPION) measuring 6 nm were synthesised according to a reported method [19].
Preparation of PEI-SA vesicles
The PEI-SA vesicles were prepared as follows: PEI-SA copolymer (10 mg) and SPION (0 or 1 mg) were dissolved in chloroform (2 mL), then 200 μL pure water was added dropwise under ultrasound agitation using a Type 60 Sonic Dismembrator (Fisher Scientific) at a power level of 30. Afterwards, the mixture was added dropwise into pure water (20 mL) under sonication. The organic solvent chloroform was then removed completely by vacuum distillation. The vesicle solution was concentrated and washed three times using a Millipore Centrifugal Filter Device (MW cut-off: 100,000 Da) to remove free SPION, and then filtered with a syringe filter (pore size: 0.22 μm).
PEG-PGA coating of PEI-SA vesicles
A predetermined amount of PEG-PGA was added to the prepared PEI-SA vesicle solution at different C/N ratios (the molar ratio of carboxyl groups of PEG-PGA to amino groups of PEI-SA) and kept at room temperature for 20 min to form various cationic PEG-PGA-coated nanovesicle solutions. The iron concentration of nanovesicles was measured by atomic absorption spectrophotometry (AAS), and r2 relaxivity was determined by in vitro MRI.
Optimal cell labelling conditions
A total of 5 × 105 MSC were cultured in 96-well plates with 200 μL culture medium per well. When cells grew to 80–90% confluence, the culture medium was replenished, and cationic nanovesicles were then directly added to the culture medium to label cells. To determine the optimal labelling concentration, 1, 2, 4, 6, 8, 10 and 12 μL of 20-mV nanovesicles were separately added to the cells in 12 wells each, with final iron concentrations of 0.525, 1.05, 2.1, 3.15, 4.2, 5.25 and 6.3 μg/mL respectively. The cells were incubated for 60 min under standard culture conditions (37°C, 5% CO2). To determine the optimal labelling duration, 6 μL of 20-mV nanovesicles was added and incubated with cells in 12 wells each for 5, 15, 30, 45, 60, 90 and 120 min under standard culture conditions. In the above two tests, 12 wells of untreated cells served as controls. After labelling, the medium was discarded, the cells were washed three times with phosphate-buffered saline (PBS) to eliminate residual nanovesicles, and the intracellular uptake of SPION was determined.
Controllability of labelling
As determined by the above optimal labelling condition, 6 μL charge-free (as controls) and equivalent 8, 14 and 20 mV nanovesicles were separately added to culture medium in 12 wells and incubated for 1 h under standard culture conditions to assess whether nanovesicles with different electric potentials could result in different intracellular uptake of SPION. After labelling, the cells were washed three times with PBS. The intracellular uptake of SPION was detected, and cell viability, proliferation activity and differentiation capability as well as the intracellular distribution of SPION were assessed.
Intracellular uptake of SPION
The intracellular uptake of SPION was evaluated by in vitro MRI, Prussian blue staining and AAS. The cells were resuspended in 200 μL 4% gelatin solution for MR imaging. For Prussian blue staining, the cells were incubated with Prussian blue solution containing 7% hydrochloride and 5% potassium ferrocyanide(II) trihydrate for 30 min at 37°C. For AAS, the cells were suspended in 1 M HCl solution to allow for polymer degradation and complete dissolution of SPION. Iron concentration was determined at the specific Fe absorption wavelength (248.3 nm) based on a pre-established calibration curve.
Cell viability, proliferation and differentiation and intracellular SPION distribution
Cell viability was determined by trypan blue exclusion assays, and cell proliferation activity was evaluated by 3-[4,5-dimethylthiazol-2-yl]-2,5-diphenyl tetrazolium bromide (MTT) assay on days 1, 2 and 3 after labelling, as described [20]. For differentiation capability, the labelled cells and untreated cells were treated with adipogenic, chondrogenic and osteogenic induction medium (Cyagen, Guangzhou, China) to test their differentiation capability as described [21]. Oil red O dye staining and Alizarin red dye staining were performed respectively to detect adipogenic differentiation after 14 days of treatment with adipogenic medium and osteogenic differentiation after 20 days of treatment with osteogenic medium. Toluidine blue staining (detection of proteoglycans) was used to reveal the presence of macromolecules diagnostic of chondrogenic differentiation after 21 days of micromass culture with serum-free medium and 10 ng/mL transforming growth factor-β3.
The intracellular distribution of SPION was determined by transmission electron microscopy (TEM). MSC were fixed in 3% glutaraldehyde-cacodylate buffer at 4°C overnight. After 1 h in 1% OsO4, they were dehydrated and embedded in artificial resin (Epon; Merck, Darmstadt, Germany). To prevent false-positive findings, thin sections of the cell probes were evaluated unstained (i.e. without double staining with uranyl acetate and lead citrate) using an electron microscope (CM-10, Philips) at 60–80 kV.
In vitro MRI
Magnetic resonance imaging was performed on a clinical 1.5-T system (Intera; Philips Medical Systems, Best, the Netherlands) with an 11-cm circular coil. Fast spin echo (FSE) T1- and T2-weighted images were acquired using the following parameters: TR/TE = 500/15 ms, number of signal acquisitions (NSA) = 2; TR/TE = 2,600/100 ms, NSA = 4. Fast field echo (FFE) T2*-weighted images were obtained using the following parameters: TR/TE = 200/14.7 ms, flip angle = 25°, NSA = 4. T2 relaxation data were acquired by using single-section multi-spin-echo sequences with the following parameters: TR = 2,000 ms, stepped echo time = 20–160 ms for eight steps; echo spacing = 20 ms. Other acquisition parameters for these sequences were FOV = 70–80 mm, matrix = 256 × 256 and section thickness = 1.5 mm. T2 maps were calculated from the T2 relaxation data by using the available software tools provided by the manufacturer, which are based on least-squares algorithms. A circular region of interest was selected in each sample, and the values of T2 relaxation times were derived. T2 relaxivity of nanovesicles was calculated from the slope of the linear plots of r2 relaxation rates (1/T) versus Fe concentration determined by linear least-squares regression analysis.
Animal surgery and cell transplantation
An intraluminal suture, middle cerebral artery occlusion was used to produce left cerebral acute ischaemic stroke as described previously [22]. Specifically, a nylon poly-l-lysine-coated 4-cm suture with a blunt head (model 2636; Sunbio Biotech, Beijing, China) was inserted 3.0 cm into the internal carotid artery via the proximal external carotid artery, and 120 min of occlusion was selected to establish the cerebral ischaemic model. Two days after surgery, 18 animals were randomly selected to receive stereotactic injection of 1 × 106 MSC pre-labelled by charge-free, 8 or 20 mV nanovesicles (n = 6 each) into the contralateral striatum (stereotaxic coordinates: 0.95 mm lateral to bregma, 0.02 mm rostral to bregma and 2.6 mm deep from the pial surface) using a 26s gauge needle attached to a 10-μL Hamilton syringe mounted on a microinjector. For injection, cells were suspended in 20 μL PBS, and cell viability was determined to be greater than 90%. The cell suspension was injected at a constant rate of 0.5 μL/min. After injection, the needle was left in place for an additional 5 min and then slowly withdrawn.
In vivo MRI
At 1, 3 and 7 days after injection, MRI was performed to detect the distribution and migration of the grafted cells on a clinical 1.5-T system (Intera; Philips Medical Systems) with a 50 × 69 mm linearly polarised birdcage radio frequency rat coil (Shanghai Chenguang Medical Technologies, China). Axial and coronal brain images were obtained by using FSE proton-weighted imaging (TR/TE = 1,500/30 ms; NSA = 2), T2-weighted imaging (TR/TE = 2,600/100 ms; NSA = 3) and FFE T2*-weighted images (TR/TE = 600/9.28 ms; flip angle = 90°; NSA = 3). Other parameters for these sequences were FOV = 70 mm, matrix = 256 × 256 and section thickness = 1.0 mm.
Histology
At 7 days after transplantation, animals were sacrificed after MRI by means of anaesthetic overdose and then transcardially perfused with saline followed by 4% paraformaldehyde in PBS. The brain was removed and cryoprotected in 20% sucrose solution. Contiguous coronal 10-μm thickness sections were prepared for Prussian blue staining and streptavidin-peroxidase immunohistochemical staining for CD11b (specific for macrophage-microglia) and CD29 (specific for MSC). For immunohistochemical staining, sections were blocked by goat serum for 30 min, followed by incubation with primary antibodies against CD11b (1:250, Chemicon, CA, USA) or CD29 (1:250, Chemicon) at 4°C overnight. After washing three times with PBS, sections were incubated with secondary antibodies (1:100, Chemicon) at room temperature in the dark for 2 h. Then, the sections were washed three times with PBS, and the immunoreactive signals were observed by 3,3’-diaminobenzidine (DAB) brown colour.
Statistical analysis
All data are expressed as means ± standard deviation, unless stated otherwise. Values for cell viability and proliferation in labelled and control cells are expressed as the percentage of the average value. Cell T2 value, Fe concentration, cell viability and proliferation activity were compared by using the analysis of variance (ANOVA), followed by the Bonferroni post-hoc test for multiple pairwise comparisons. Statistical calculations were performed using SPSS 12.0 software for Windows (Chicago, IL, USA). All P values of <0.05 were considered to indicate a statistically significant difference.
Results
Synthesis and characterisation of nanovesicles
1H NMR spectrum showed that the chemical shifts were consistent with the expected structures of the polymer (Fig. 1a). The graft density of PEI was 30%, as calculated from the 1H NMR spectrum by comparing the integral values of characteristic peaks of –NHCH2CH2– at 2.83 ppm and –(C=O)NCH2CH2– at 3.41 ppm. As electrostatic coating of PEG-PGA increased (i.e. as the C/N ratio increased), the zeta potential of the vesicles steadily declined, and the particle size was maintained at a higher value (Fig. 1b). Since the small size and positive charge are in favour of nanoparticle uptake by cells, vesicles prepared at a C/N ratio of 1/4 were selected for the following biological studies, where the measured size of the cationic vesicles was 150 ± 25 nm (Fig. 1c, d), the iron concentration was 105 μg/mL and the measured r2 relaxivity was 0.3431 × 106 M−1S−1 (Fig. 1e).
Synthesis and characteristics of nanovesicles. Graphs show the 1H nuclear magnetic resonance (NMR) spectrum of PEI-SA (a) and the particle size and zeta potential with or without electrostatic coating of poly(ethylene glycol)-poly(L-glutamic acid) (PEG-PGA) at various carbon/nitrogen (C/N) ratios (b). Transmission electron microscopy (TEM) image shows that the nanovesicles measured 150 nm (c), and the superparamagnetic iron oxide nanoparticles (SPION) were located inside the nanovesicles within the nanovesicle bilayer (d). Graphs show the r2 relaxivity of SPION-loaded nanovesicles (e)
Optimal labelling condition
T2 values and T2 signal intensity of labelled cells exhibited a non-linear change with an increase in both nanovesicle concentration and incubation time. AAS demonstrated that the optimal concentration was 3.15 μg Fe/mL, with a mean iron concentration of 51.12 pg in a single cell; and labelling was most efficient at 60 min incubation (P = 0.029), with a mean iron concentration of 50.02 pg in a single cell (Fig. 2). Greater nanovesicle concentration or longer exposure time (up to 2 h) did not improve the cellular SPION uptake.
Optimal labelling concentration. Graphs show that, with an increase in the concentration of nanovesicles (a, b) or incubation time (d, e), T2 values and cell iron content of labelled cells exhibited an exponential change as measured by atomic absorption spectrometry (AAS). This change was consistent with the signal intensity changes on T1-, T2- and T2*-weighted images and the T2 map (c, f)
Controllability of labelling
Under the optimal concentration and incubation time (i.e. 3.15 μg/mL and 1 h incubation time), T2 values and T2 signal intensity of cells showed a linear change with an increase in electric potential. The higher the electric potential with the nanovesicles, the higher the intracellular uptake of iron, as determined by AAS (P = 0.021) and Prussian blue staining. No SPION were detected in the cells labelled with charge-free nanovesicles (Fig. 3).
Controllability of labelling. Graphs show that with an increase in the electric potential of nanovesicles, the T2 value (a) and cell iron content measured by atomic absorption spectrometry (AAS) (b) exhibited a linear change. This was consistent with the signal intensity changes observed on T1-, T2- and T2*-weighted images and the T2 map (c) and cell uptake of iron particles revealed by Prussian blue staining (d)
Cell viability, proliferation and differentiation and intracellular SPION distribution
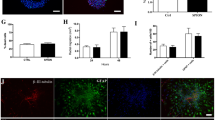
There was no decreased cell viability and cell proliferation capacity in labelled cells compared with controls (P = 0.241; 0.191) (Fig. 4). TEM demonstrated that SPION were present in the endosomes inside the cytoplasm. Occasionally some SPION particles were found to attach to the outer surface of the cell membrane (Fig. 5). The labelled cells showed a similar adipogenic, chondrogenic and osteogenic differentiation capacity as the untreated MSC under appropriate induction conditions (Fig. 6).
Cell differentiation. Under appropriate induction conditions, neutral lipid accumulation was observed as a result of adipogenic induction in unlabelled cells (a) and labelled cells (b). Alizarin red dye staining showed small calcium nodules in unlabelled (d) and labelled cells (d). Toluidine blue staining showed positive staining in the extracellular matrix for unlabelled (e) and labelled cells (f) following micromass culture. Arrows indicate typical SPION-loaded cells. The scale bar represents 100 μm
In vivo MRI
One day after injection, the grafted cells labelled with cationic nanovesicles were detected as strongly hypointense areas in the left striatum on T2- and T2*-weighted images. This signal intensity remained until 7 days after injection. Cells labelled with 20-mV nanovesicles showed greater hypointensity than those labelled with 8-mV nanovesicles. By 7 days after injection, a linear hypointense area was found in the corpus callosum on T2*-weighted images in animals grafted with 20-mV nanovesicle-labelled cells. No hypointense signal change was observed in animals that received 0-mV nanovesicle-labelled cell injection (Fig. 7).
In vivo MRI of the grafted cells. At 1 day after injection, coronal T2*-weighted images show hypointense area representing SPION-labelled mesenchymal stem cells (MSC) (arrows) in the right striatum in animals grafted with 8-mV (b) and 20-mV (c) nanovesicle-labelled cells. Cells labelled with 20-mV nanovesicles show larger hypointense areas than those labelled with 8-mV nanovesicles. No obvious developing signal was found during the entire study period in the animals grafted with charge-free nanovesicle-labelled cells (a). By 7 days after injection, linear hypointense signal was found in the corpus callosum in animals grafted with 20-mV nanovesicle-labelled cells (arrowheads)
Histology
At 7 days after injection, Prussian blue staining showed that there were positive cells in the striatum in animals injected with 8- or 20-mV nanovesicle-labelled cells. Immunohistochemistry demonstrated that most grafted cells remaining in the graft site showed positive CD29 staining but not overlapping CD11b staining in the animals receiving 0-, 8- or 10-mV nanovesicle-labelled cells, indicating the viability of grafted cells. In animals grafted with 8- and 10-mV nanovesicle-labelled cells, Prussian blue staining showed that there was a small number of positive cells in the corpus callosum, indicating cell migration along the corpus callosum towards the injured brain (Fig. 8). No double-labelled cells were found in the migrating cell population, making it unlikely that the observed migration was mainly caused by SPION-laden macrophages.
Histology of the grafted cells. At 7 days after injection, there is distinct punctuate Prussian blue staining in the graft site (arrows) and the corpus callosum (arrowheads) in animals treated with 8-mV (b) or 10-mV (c) nanovesicle-labelled cells. The distribution pattern of positive cells was matched with the hypointense signal observed on MRI. Immunohistochemical staining demonstrated that most of the cells remaining at the graft site in animals treated with 0-mV (a), 8-mV (b) or 10-mV (c) nanovesicle-labelled cells were positive for CD29 staining, but not overlapping CD11b staining. The scale bars represent 200 and 25 μm on Prussian blue staining and immunohistochemical staining micrographs respectively
Discussion
Our study suggested that SPION could be successfully transferred into MSC using cationic nanovesicles, and that controllable cell labelling could be achieved by regulating the electrical potential of the nanovesicles. The labelling did not alter cell viability, proliferation or differentiation. The distribution and migration of the grafted, labelled cells could be detected in vivo by MRI. The achieved labelling efficiency was comparable with that using dendrimers, PLL or lipofectamine [7]. Moreover, the variability in labelling efficiency with the different electric potentials of nanovesicles was reflected in the different extents of hypointense signal of labelled cells in the graft sites. Histology confirmed the label retention and viability of labelled cells at 7 days after transplantation.
Many molecules on the cell surface are negatively charged owing to the presence of sialic acids, which account for the bulk of the charge on the cell surface [23, 24]. The major class of TA and magnetodendrimers was used to ameliorate the electrostatic interaction between iron particles and cellular membrane, eliciting macropinocytosis for cell labelling [5]. In our study, the synthesised cationic nanovesicles have positive charges on their surface, through which SPION-loaded nanovesicles are thought to interact with the cell surface through electrostatic (van der Waals) bonds, resulting in a bending of the membrane that initiates endocytosis and/or macropinocytosis, whereby SPION were internalised into the cytoplasm or endosome. Unlike TA, the unique hollow structure of nanovesicles enables direct loading of SPION. The use of amphiphilic polymers in aqueous solution to form nanovesicles made the size relatively uniform and thus allowed a constant loading content of SPION. Moreover, the nanovesicles with the NH2 linked to the surface could carry different amounts of surface positive electric potentials through regulating the extent of NH2 amino protonation to achieve controllable labelling efficiency.
Our results showed that there was a saturation effect for nanovesicle internalisation in the tests of optimal labelling condition; that is, the most efficient labelling was achieved when using 3.15 μg Fe/mL nanovesicles with 20-mV positive charges and 1-h incubation time. The electrostatic interaction between nanovesicles and cell membranes gradually declined with the increase in the nanovesicle concentration or incubation time, and eventually reached a plateau where all the available negatively charged cell membranes were completely neutralised by the cationic nanovesicles. This phenomenon could also be observed with other cationic TA for cell labelling [25]. However, comparatively, using nanovesicles to label stem cells has a variety of advantages: the labelling procedure itself is simple and rapid; the nanovesicles consist of new materials with biocompatible and biodegradable characteristics, which have good biological safety and low toxicity; the nanovesicles can easily be chemically modified and linked with the specific ligands to achieve actively targeted imaging; the loading capacity of the nanoparticles is controlled, thus it can achieve high load and release loaded materials in a controlled way [26].
There were limitations in our study. Our study showed that the nanovesicle-labelled MSC had unaltered viability, proliferation activity and differentiation capability, and their distribution and migration following transplantation could be detected by MRI. However, the extensive use of this method might be limited with regard to the required synthetic fabrication of nanovesicles. Other than SPION labelling, a simple method of cell labelling with fluorine 18 [27] or 111In-oxine [28] has been reported for tracking injected MSC [27]. However, techniques dependent on radioactive isotopes in general are limited by the half-lives of the isotopes, and thus difficult to apply for longitudinal monitoring. With the advantages of non-invasiveness, non-radiation, superior resolution and simultaneous supplemental information about the surrounding tissue relevant to graft status, cellular MRI is entirely clinically translatable and is already being used in initial clinical applications [29].
In conclusion, our study demonstrated that highly efficient and controllable labelling of stem cells can be achieved by using cationic, SPION-loaded nanovesicles, whose in vivo distribution and migration of stem cells in the context of cerebral ischaemia injury can be tracked by MRI. The labelling does not affect the cell viability, proliferation activity or multilineage differentiation capability. The grafted cells can retain the label and remain viable. Without the need for a secondary transfection agent, our labelling appears to be an appealing, alternative cell labelling approach that could be used for further controllable cellular MRI in stem cell therapy.
References
Mimeault M, Hauke R, Batra SK (2007) Stem cells: a revolution in therapeutics—recent advances in stem cell biology and their therapeutic applications in regenerative medicine and cancer therapies. Clin Pharmacol Ther 82:252–264
Mimeault M, Batra SK (2006) Concise review: recent advances on the significance of stem cells in tissue regeneration and cancer therapies. Stem Cells 24:2319–2345
Lee Z, Dennis JE, Gerson SL (2008) Imaging stem cell implant for cellular-based therapies. Exp Biol Med (Maywood) 233:930–940
Walczak P, Bulte JW (2007) The role of noninvasive cellular imaging in developing cell-based therapies for neurodegenerative disorders. Neurodegener Dis 4:306–313
Bulte JW (2009) In vivo MRI cell tracking: clinical studies. AJR Am J Roentgenol 193:314–325
Kraitchman DL, Gilson WD, Lorenz CH (2008) Stem cell therapy: MRI guidance and monitoring. J Magn Reson Imaging 27:299–310
Frank JA, Miller BR, Arbab AS et al (2003) Clinically applicable labeling of mammalian and stem cells by combining superparamagnetic iron oxides and transfection agents. Radiology 228:480–487
Politi LS (2007) MR-based imaging of neural stem cells. Neuroradiology 49:523–534
Bulte JW, Douglas T, Witwer B et al (2001) Magnetodendrimers allow endosomal magnetic labeling and in vivo tracking of stem cells. Nat Biotechnol 19:1141–1147
Zhang C, Wangler B, Morgenstern B et al (2007) Silica- and alkoxysilane-coated ultrasmall superparamagnetic iron oxide particles: a promising tool to label cells for magnetic resonance imaging. Langmuir 23:1427–1434
Liu ZY, Wang Y, Liang CH et al (2009) In vitro labeling of mesenchymal stem cells with superparamagnetic iron oxide by means of microbubble-enhanced US exposure: initial experience. Radiology 253:153–159
Arbab AS, Yocum GT, Kalish H et al (2004) Efficient magnetic cell labeling with protamine sulfate complexed to ferumoxides for cellular MRI. Blood 104:1217–1223
Bauer M, Kristensen BW, Meyer M et al (2006) Toxic effects of lipid-mediated gene transfer in ventral mesencephalic explant cultures. Basic Clin Pharmacol Toxicol 98:395–400
Dousset V, Tourdias T, Brochet T et al (2008) How to trace stem cells for MRI evaluation? J Neurol Sci 265:122–126
Ozpolat B, Sood AK, Lopez-Berestein G (2010) Nanomedicine based approaches for the delivery of siRNA in cancer. J Intern Med 267:44–53
Cai W, Chen X (2007) Nanoplatforms for targeted molecular imaging in living subjects. Small 3:1840–1854
Nagaya N, Fujii T, Iwase T et al (2004) Intravenous administration of mesenchymal stem cells improves cardiac function in rats with acute myocardial infarction through angiogenesis and myogenesis. Am J Physiol Heart Circ Physiol 287:H2670–6
Cao N, Cheng D, Zou S et al (2011) The synergistic effect of hierarchical assemblies of siRNA and chemotherapeutic drugs co-delivered into hepatic cancer cells. Biomaterials 32:2222–2232
Sun S, Zeng H, Robinson D et al (2004) Monodisperse MFe2O4(M=Fe, Co, Mn) nanoparticles. J Am Chem Soc 126:273–279
Arbab AS, Bashaw LA, Miller BR et al (2003) Characterization of biophysical and metabolic properties of cells labeled with superparamagnetic iron oxide nanoparticles and transfection agent for cellular MR imaging. Radiology 229:838–846
Kostura L, Kraitchman DL, Mackay AM et al (2004) Feridex labeling of mesenchymal stem cells inhibits chondrogenesis but not adipogenesis or osteogenesis. NMR Biomed 17:513–517
Chen Y, Ito A, Takai K et al (2008) Blocking pterygopalatine arterial blood flow decreases infarct volume variability in a mouse model of intraluminal suture middle cerebral artery occlusion. J Neurosci Methods 174:18–24
Cook GM (1968) Glycoproteins in membranes. Biol Rev Camb Philos Soc 43:363–391
Angata T, Varki A (2002) Chemical diversity in the sialic acids and related alpha-keto acids: an evolutionary perspective. Chem Rev 102:439–469
Daldrup-Link HE, Rudelius M, Oostendorp RA et al (2003) Targeting of hematopoietic progenitor cells with MR contrast agents. Radiology 228:760–767
Marcucci F, Lefoulon F (2004) Active targeting with particulate drug carriers in tumor therapy: fundamentals and recent progress. Drug Discov Today 9:219–228
Ma B, Hankenson KD, Dennis JE, Caplan AI, Goldstein SA, Kilbourn MR (2005) A simple method for stem cell labeling with fluorine 18. Nucl Med Biol 32:701–705
Gildehaus FJ, Haasters F, Drosse I et al (2011) Impact of indium-111 oxine labelling on viability of human mesenchymal stem cells in vitro, and 3D cell-tracking using SPECT/CT in vivo. Mol Imaging Biol 13:1204–1214
De Vries IJ, Lesterhuis WJ, Barentsz JO et al (2005) Magnetic resonance tracking of dendritic cells in melanoma patients for monitoring of cellular therapy. Nat Biotechnol 23:1407–1413
Acknowledgements
This work is supported by the National Natural Science Foundation of China (grant number: 81071028, 50830107) and the Fundamental Research Funds for the Central Universities of China (grant number: 09ykpy04), and in part by the Guangdong Natural Science Foundation (grant number: 9151008901000001).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Guo, R.M., Cao, N., Zhang, F. et al. Controllable labelling of stem cells with a novel superparamagnetic iron oxide–loaded cationic nanovesicle for MR imaging. Eur Radiol 22, 2328–2337 (2012). https://doi.org/10.1007/s00330-012-2509-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-012-2509-z