Abstract
Foreign bodies (FBs) retained in the soft tissues are a common reason for medical consultation, and usually consist of wooden or metal splinters or glass shards. Failure to remove foreign bodies is likely to give rise to acute or late complications, such as allergies, inflammation or infection, that may be severe. The surgical removal of an FB is invasive, costly and technically challenging. The procedure may fail in some cases and carries the risk of complications. Our study describes a technique for the ultrasound-guided removal of an FB, devised from our experience, and demonstrates its advantages over the standard surgical procedure. Sixty-two patients (43 males and 19 females aged from 9 to 65 years, median age 31 years) presented at our institution between October 2005 and June 2008 with suspected foreign bodies retained in the soft tissues of various body districts. Radiographic and/or ultrasound diagnosis was established by a radiologist expert in musculoskeletal sonography. The same radiologist helped by a nurse subsequently undertook the ultrasound-guided removal in the outpatient’s clinic according to the technique described in the paper. ATL 5000 and PHILIPS iu22 ultrasound systems were used with high-frequency linear-array probes, sterile material, local anaesthetic (lidocaine 2%), scapels and surgical forceps. Antibiotic prophylaxis with amoxicillin and clavulanic acid were prescribed to all patients for 7 days after the procedure. Ninety-five FBs (39 glass, 35 metal, 17 vegetable, 2 plastic, 2 stone) were successfully removed under ultrasound guidance in all patients and the procedure took between 15 and 30 min. No complications arose either during or after the procedure. Seventy-five skin incisions were made and the wounds closed with Steri-Strips in 73/75 cases, whereas skin sutures were used in 2/75 cases. No complications arose either during or after the procedure. Ultrasound-guided removal of an FB retained in the soft tissues is a good alternative to surgery as is its relatively straightforward, inexpensive, repeatable and carries a low risk of complications. In addition, failure to remove an FB does not preclude traditional surgical removal. The advantages of this real-time procedure and the use of small instruments minimize bleeding time and avoid injury to surrounding structures. Patient compliance is enhanced by the fact that the procedure has little or no aesthetic impact. These encouraging results suggest ultrasound-guided removal as a first-choice procedure for the extraction of foreign bodies.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Foreign bodies (FBs) retained in the soft tissues are a common reason for medical consultation and this also applies in the emergency setting [1, 2]. An FB may result from accidents in the home or workplace [3] and usually consist of wooden or metal splinters or glass shards, causing pain and/or functional impairment.
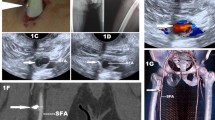
Failure to remove FBs is likely to give rise to acute or late complications, such as allergies, inflammation or infection, that may be severe [3, 4]. When FBs are located within or close to tendons, they may lead to irritative or septic, acute or chronic peritendinitis or tenosynovitis. In or near a nerve, an FB may give rise to acute lesions, post-traumatic neuromas (Fig. 1a) or neuropathies [5]. FBs may also migrate to deeper soft tissues, into the joints [6–10] or even into blood vessels with possible embolic complications [11, 12]. Long-term retention of FBs has also led to the onset of tumours [13].
FBs can seldom be identified and removed on the basis of clinical examination alone, and usually only when in a superficial location. Otherwise, imaging techniques are required to identify the FB and establish its exact location prior to surgical removal attempt. To identify and localize FBs other than by traditional radiography, which will usually display radiopaque FBs, echotomography has now proved irreplaceable, with high sensibility and specificity [1–4, 14–20].
The surgical removal of FBs is invasive, costly and technically challenging. The procedure may fail in some cases and carries the risk of complications.
Our study describes a technique for the ultrasound-guided removal of FBs devised from our experience and demonstrates its advantages over the standard surgical procedure.
Materials and methods
Sixty-two patients (43 males and 19 females aged from 9 to 65 years, median age 31 years) presented at our institution between October 2005 and June 2008. Of these, 28 had been referred by Casualty and 34 by an orthopaedic specialist with diagnosed or suspected FBs retained in the soft tissues of various body districts.
All patients had traditional radiograms and ultrasound investigation using ATL 5000 Philips or IU-22 Philips ultrasound systems with high-frequency linear-array probes 12-17 Mhz. Imaging confirmed the diagnosis identifying 95 FBs of various materials, measuring from less than 1 mm to 32 mm, located in different body districts (Table 1). Standard X-ray displayed FBs made of metal, glass and stone in 76/95 cases (Fig. 2a, b) but failed to detect vegetable and plastic FBs. Ultrasound displayed FBs in 94/95 cases. Radioscopy was required in the one remaining case to identify a thin-needle FB entrapped beneath the skin in the trochanteric region poorly distinguished from the surrounding tissues at ultrasound.
The same radiologist expert in musculoskeletal sonography who had performed the diagnostic tests, with the assistance of a nurse, subsequently removed the FB under ultrasound guidance in the outpatient’s clinic, according to the technique described below.
The removal procedure starts with a diagnostic ultrasound examination to establish the exact location of the FB, its morphology and its relations with nearby eloquent structures (vessels, nerves, tendons). This initial step is crucial for treatment planning to select the material to use, the appropriate ultrasound probe, and logistics (positioning of patient, operator, the ultrasound device and the material required).
After disinfecting the patient’s skin with Neomidil (Nuova Farmac, Verona, Italy) under sterile conditions (sterile probe cover, sterile gloves, mask), a 22- to 25-G needle (Becton Dickinson, Fraga-Huesca, Spain) is inserted to reach the FB and local anaesthetic with 2-3 ml of lidocaine chlorhydrate 2% (S.A.L.F., Bergamo, Italy) administered under ultrasound guidance (Fig. 3). In most cases, injection of the anaesthetic close to the FB will detach it from the surrounding tissues thereby facilitating subsequent removal. Anaesthetic continues to be injected while retracting the needle to anaesthetize the needle path to be used during removal.
Under constant ultrasound guidance, the skin is then incised, together with the underlying fascia if necessary, with a scapel (Xinda no. 11, WuXi Xinda Medical Device Co., Wuxi City, Jiangsu, China). The incision must be just large enough for the surgical forceps to be inserted, or in the case of a particularly large FB, wide enough for the FB to pass through. The tip of the scapel must reach the FB so as to create a complete linear passage between the skin and the FB (Fig. 4).
Under constant ultrasound guidance the skin is incised together with the underlying fascia if necessary. The tip of the scapel (empty white arrow) must reach the FB (full white arrow) located near the MCF joint of the third dorsal ray. MC head of metacarpal bone, asterix extensor tendon third finger
The operator then uses his/her dominant hand to insert the surgical forceps through the incision (Halsted-Mosquito Forceps, 12.8 cm, 18-2310) to reach the FB (Fig. 5), following its passage in real time on ultrasound longitudinal scans. The arms of the forceps are then opened slightly, displacing the tissues surrounding the FB, to grip the object (Fig. 6) (axial scanning planes are useful at this stage to facilitate prehension) and then remove it.
The procedure is terminated with skin disinfection and the skin flaps of the wound closed with Omnistrips (Paul Hartmann, Heidenheim, Germany) or sutures (3.5 EP, Ethicon black braided silk, Johnson-Johnson). Antibiotic prophylaxis with amoxicillin and clavulanic acid (Augmentin, 875 mg + 125 mg, Glaxo Smith Kline, Verona, Italy) (1 g every 12 h) is prescribed for 7 days after the removal procedure to prevent any iatrogenic septic complications or sequelae caused by mobilization of the FB. One patient was also given antitetanic serum (Gamma-TET P500, one 2-ml phial, 500 IU, ZLB Behring, Milan, Italy) as a precaution in case of lack of immunization cover.
Results
The following FBs were removed: 39 glass FBs from 12 patients, 35 metal FBs from 35 patients, 17 vegetable FBs from 12 patients, 2 plastic FBs from two patients and 2 stone FBs from one patient. The FBs were successfully removed from all patients under ultrasound guidance and the procedure took from 15 to 30 min.
The FB removal procedure was undertaken in three separate sessions in one patient with 20 glass-splinter shards from an explosion. Eight skin incisions were performed in this patient, with the procedure taking an average of 10 min to remove each shard. Numerous microgranules of glass dust, much smaller than a millimetre, were also extracted during these procedures. Three skin incisions were made during the same session in one patient with eight glass shards after a road accident. Two skin incisions were made in the same session to remove four vegetable fragments from another patient. Two glass shards and two stone FBs in two patients, respectively, were removed through one skin incision each.
Seventy-five skin incisions were made and the wounds closed with Omnistrips in 73/75 cases. The wound (sole of the foot) was closed by a suture in one patient because of the weight-bearing anatomic location. The FB in another patient (a bullet in the back) required a larger than normal incision, which required two sutures. No complications arose either during or after the procedure neither septic nor inflammatory.
Discussion
Clinical examination alone fails to identify an FB in a high percentage of cases (up to 38%) [14], due to pain, swelling and haematoma following injury. For this reason imaging techniques are essential to identify FBs and their exact location.
As traditional radiograms are widely available, simple to perform and inexpensive, X-ray is the reference examination [2] and will identify radiopaque FBs (glass, metal, stone) in around 80% of cases, but only displays 15% of non-radiopaque FBs (wood, plastic) [4, 14]. Radioscopy offers a more accurate topographic assessment and allows reference points to be marked on the skin to aid subsequent FB removal. However, radioscopy exposes patient and operator alike to relatively high doses of ionizing radiation. Computed tomography (CT) and magnetic resonance (MR) scans are very expensive and have very limited indications for FB detection as they have poor sensitivity and specificity [4].
Ultrasound is the first choice investigation in the diagnosis of an FB retained in the soft tissues, as it has a sensitivity and specificity of 90% and 96%, respectively [15, 16]. Thanks to its high spatial resolution, ultrasound will identify FBs smaller than a millimetre [17], be they wood, glass, metal or plastic [18]. The limitations of ultrasound are well known: it is an operator-dependent technique and will only display FBs retained in superficial tissues [18].
New-generation ultrasound devices fitted with high-frequency probes (7–17 MHz) will identify FBs with a thorough morphological and volumetric assessment and exact information on their three-dimensional spatial location [3]. FBs are usually displayed as hyperechoic areas with varying degrees of posterior acoustic shadowing or echo. Long after the traumatic event, the FB may be surrounded by a hypoechogenic halo caused by granulomatous inflammatory reaction [18]. In this case it is important to establish an accurate differential diagnosis between FB and any small air pockets, calcifications, skin scars, keratin deposits, haematomas or sesamoid bones [3].
Ultrasound examination will also establish the integrity of the surrounding ligaments, tendons, joint capsules and neurovascular structures (with the aid of colour Doppler) and accurately depict the relations between the FB and adjacent eloquent structures (tendons, nerves, vessels) to ensure the safe removal of the FB, avoiding iatrogenic lesions or complications [3, 18]. In view of its potential, ultrasound examination performed by expert doctors is the first choice investigation of FB providing essential information for therapeutic decision-making and accurate planning for possible surgical removal.
The ordinary management of patients referred to surgical consultation with diagnosed or suspected FBs retained in the soft tissues initially entails a distinction between open wounds and wounds with a small entry hole. Surgical exploration with an in-depth lesion assessment is essential in the case of open wounds. When there is documented evidence of associated lesions to neurovascular structures or tendons, surgical repair allows the concomitant search for an FB. When there are no associated lesions a wide surgical exposure should be made to search for the FB with careful dissection of adjacent eloquent structures.
In the case of a tiny FB with a small entry hole, surgical treatment is usually avoided because of the low risk of associated lesions and the objective difficulty of detecting a small FB in the operating field (due to both bleeding and the variable features of FB) and is only indicated when there is documented evidence of an associated lesion. In addition, the procedure can only make use of adjuvant radioscopy for a radiopaque FB, otherwise surgical planning must rely on an assessment of the entry hole and presumed transit path of the FB [21].
The drawbacks of surgery are also related to the need for a large skin and possibly fascial incision with isolation of neurovascular structures (Fig. 1a, b). In addition to possible iatrogenic lesions or surgical complications, these interventions entail an inevitable aesthetic impact to some degree.
In the case of a long-standing FB, surgery is indicated to deal with supervening complications requiring surgical repair.
Ultrasound-guided removal of an FB retained in the soft tissues is a good alternative to surgery as is its relatively straightforward, inexpensive, repeatable and carries a low risk of complications. In addition, failure to remove an FB does not preclude traditional surgical removal. Whereas surgical removal entails a significant loss of substance, ultrasound-guided removal of an FB is minimally invasive as its point entry is a simple skin incision of usually less than a centimetre and the small residual scar has little or no aesthetic impact.
The real-time features of the ultrasound-guided procedure minimize the amount of bleeding and avoid injury to structures surrounding the FB, while the sterile approach and antibiotic prophylaxis after the procedure reduces the risk of septic complications, and the use of small instruments minimizes any aesthetic impact, thereby enhancing patient compliance.
The ultrasound-guided technique requires experience and good manual skills on the part of the operator, who can be trained using biological models (e.g. turkey breast or ox tongue) [2].
A review of the latest literature failed to disclose studies on FB removal. Despite the small size of our cohort, the results of our study are encouraging and suggest ultrasound-guided removal as a first choice procedure for the extraction of FBs when there is no evidence of associated lesions requiring surgical intervention.
References
Blankstein A, Cohen I, Heiman Z et al (2001) Ultrasonography as a diagnostic modality and therapeutic adjuvant in the management of soft tissue foreign bodies in the lower extremities. Isr Med Assoc J 3(6):411–413
Shiels WE 2nd, Babcock DS, Wilson JL, Burch RA (1990) Localization and guided removal of soft-tissue foreign bodies with sonography. AJR Am J Roentgenol 155(6):1277–1281
Braham R, Said M, Jerbi Ommezine S, Gannouni A (2005) Foreign bodies in the soft tissues. The interest of sonography. Presse Med 34(3):256
Peterson JJ, Bancroft LW, Kransdorf MJ (2002) Wooden foreign bodies: imaging appearance. AJR Am J Roentgenol 178(3):557–562
Choudhari KA, Muthu T, Tan MH (2004) Progressive ulnar neuropathy caused by delayed migration of a foreign body. Scand J Plast Reconstr Surg Hand Surg 38(1):21–26
Devgan A, Mudgal KC (2002) An unusual case of foreign body knee that spontaneously migrated inside and out of the joint: arthroscopic removal. J Hand Surg [Am] 27(2):350–354
Pang KP, Pang YT (1994) A rare case of a foreign body migration from the upper digestive tract to the subcutaneous neck. Unfallchirurg 97(7):372–374
Gutierrez V, Radice F (1998) Late bullet migration into the knee joint. Neuroradiology 40(10):673–674
Ozsunar Y, Tali ET, Kilic K (2001) Unusual migration of a foreign body from the gut to a vertebral body. Br J Neurosurg 15(3):263–265
Combalia-Aleu A, Fuster-Obregon S (2003) Migration of a Kirschner wire from the sternum to the right ventricle. A case report. Eur J Cardiothorac Surg 24(2):301
Decker P, Hofler HR, Decker D et al (2003) Traumatic foreign body embolism from the basilic vein. Arthroscopy 19(3):E15
Gschwind CR (2002) The intravenous foreign body: a report of 2 cases. Ear Nose Throat J 81(10):730–732
Teltzrow T, Hallermann C, Muller S, Schwipper V (2006) Foreign body-induced angiosarcoma 60 years after a shell splinter injury. Mund Kiefer Gesichtschir 10(6):415–418
Anderson MA, Newmeyer WL 3rd, Kilgore ES (1982) Diagnosis and treatment of retained foreign bodies in the hand. Am J Surg 144:63–67
Jacobson JA, Powel A, Craig JG et al (1998) Wooden foreign bodies in soft tissue: detection at US. Radiology 206:45–48
Bray PW, Mahoney JL, Campbell JP (1995) Sensitivity and specificity of ultrasound in the diagnosis of foreign bodies in the hand. J Hand Surg [Am] 20(4):661–666
Ng SY, Songra AK, Bradley PF (2003) A new approach using intraoperative ultrasound imaging for localization and removal of multiple foreign bodies in the neck. Int J Oral Maxillofac Surg 32(4):433–436
Boyse TD, Fessell DP, Jacobson JA et al (2001) US of soft-tissue foreign bodies and associated complications with surgical correlation. Radiographics 21(5):1251–1256
Gibbs TS (2006) The use of sonography in the identification, localization and removal of soft tissue foreign bodies. J Diagnostic Medical Sonography 22(1):5–21
Cardinal É, Chhnem RK, Germain Beauregard C (1998) Ultrasound-guided interventional procedures in the musculoskeletal system. Rad Clin N Am 36(3):597–604
Tubiana R, McCullough CJ, Masquelet AC (1996) Atlante delle vie chirurgiche d’accesso all’arto superiore. Antonio Delfino Editore, Rome, pp 1–2
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Callegari, L., Leonardi, A., Bini, A. et al. Ultrasound-guided removal of foreign bodies: personal experience. Eur Radiol 19, 1273–1279 (2009). https://doi.org/10.1007/s00330-008-1266-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-008-1266-5