Abstract
The objectives of this study were to determine the usefulness of magnetic resonance (MR) imaging in the differentiation of various lesions causing an abnormality of the endometrial cavity by evaluating the imaging features on dynamic contrast-enhanced study and late contrast-enhanced T1-weighted images (T1WI). Contrast-enhanced MR imaging of 59 pathologically proven lesions that showed an abnormality of the endometrial cavity, including 32 endometrial cancers, five sarcomas, nine hyperplastic polyps, nine submucosal myomas, three hyperplasia, and one adenomyoma, were retrospectively reviewed. The enhancement degree and patterns on dynamic contrast-enhanced study and late contrast-enhanced T1WI were compared among different pathologies. On dynamic contrast-enhanced study, 72% (23/32) of endometrial cancers showed early peak enhancement to be reached within 1 min following intravenous administration of contrast material. On late-contrast-enhanced T1WI, lesions showed weak enhancement with gradual washout. Ninety-five percent (21/22) of benign lesions and 100% (5/5) of sarcomas showed late peak enhancement to be reached in 2–3 min following intravenous administration of contrast material. On late contrast-enhanced T1WI, both of these lesions showed persistent strong enhancement. Different enhancement patterns on dynamic contrast-enhanced MR imaging and late contrast-enhanced T1WI can provide a useful clue in the differentiation of various lesions causing an abnormality of the endometrial cavity.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
For evaluation of the various lesions causing endometrial abnormality, including endometrial carcinoma, polyp, hyperplasia, submucosal myoma, adenomyoma, and myometrial sarcoma, ultrasonography (US) and endometrial biopsy has been the mainstay for preoperative diagnosis. On US, however, these lesions often cannot be separated from the surrounding endometrium, and the whole endometrium is seen as diffuse thickening [1]. As endometrial thickening is a nonspecific US finding, it should be correlated with patient’s age, symptoms, and hormonal status. To make a specific diagnosis in these circumstances, endometrial curettage or biopsy should be performed. However, as these procedures are commonly performed in a blind manner, it is not always possible to obtain a definitive diagnosis.
Recently, the usefulness of magnetic resonance (MR) imaging in the differentiation of endometrial polyp and carcinoma has been reported [2]. In the study, the morphological features on T2-weighted images (WI) were reported to be helpful in distinguishing most polyps from carcinomas although biopsy was needed for the diagnostic confirmation [2]. Another study tried to differentiate endometrial lesions using T2WI and contrast-enhanced (CE) MR imaging [3]. Using the presence of myometrial invasion and less enhancement of the lesion on late CE T1WI than that of the myometrium as diagnostic criteria for malignancy, the authors reported a fairly high sensitivity, specificity, and accuracy of MR imaging [3]. To our knowledge, however, no study has investigated the usefulness of dynamic CE MR imaging in the differentiation of various endometrial lesions.
The purpose of this study was to determine the usefulness of dynamic CE MR imaging and late CE T1WI in differentiation of the various lesions causing an abnormality of the endometrial cavity by analyzing enhancement degree and patterns on these MR imaging sequences.
Materials and methods
Patients
This study was approved by our institutional review board. Of the patients who had gynecological MR examinations between September 1994 and May 2000 in our institution, 73 (age range 22–76; mean age, 44 years) who showed an abnormality of the endometrial cavity on MR imaging, including a mass or thickening of the endometrium and a central uterine mass with displacement or distortion of the endometrial cavity, were included in this study. Diffusely thickened endometrium was considered abnormal when its thickness exceeded 10 mm in premenopausal women and 5 mm in postmenopausal women. Seven patients were excluded because the endometrial lesions were less than 2.5 mm in diameter, thus making it difficult to measure signal intensity (SI) using a round cursor. Dynamic CE MR studies were available in 59 of the remaining 66 patients. Thirty-six patients were postmenopausal, and 30 were premenopausal. Out of 35 patients with endometrial cancer, 22 were postmenopausal.
Histopathological confirmation was made following hysterectomy in 57 patients, dilatation and curettage in two patients, and endometrial biopsy in remaining seven. Histopathological diagnoses were as follows: 35 patients with endometrial carcinomas, ten with hyperplastic polyps (without evidence of cellular atypia), 12 with submucosal leiomyomas, five with sarcomas (two stromal sarcomas and three malignant mixed mullerian tumors), three with endometrial hyperplasias, and one with adenomyoma. Lesion size ranged from 1.4 cm to 12 cm (3.6±2.4 cm) for endometrial carcinomas, from 3.5 to 12 cm (7.8±4.3 cm) for sarcomas, from 2.1 to 10 cm for submucosal myoma (5.2±2.4 cm), from 0.8 to 5 cm for hyperplatic polyp (7.8±4.3 cm), from 0.8 to 4 cm for endometrial hyperplasia (1.5±1.3 cm), and a 3.5 cm adenomyoma.
MR imaging was performed with a 1.5 T unit (Signa; GE Medical systems, Milwaukee, WI, USA). All subjects were examined using a pelvic or TORSO multicoil. Axial T1-weighted spin-echo images (TR/TE 450-700/10, matrix 256×192) and axial and sagittal fast spin-echo T2WI (TR/effective TE 3000-6000/85-104, matrix 512×256-512×192) were obtained. Field of view (FOV) was 22–26 cm, and section thickness was 5 mm with a 2 mm interscan gap.
Dynamic CE MR images using gradient echo techniques (multiplanar spoiled gradient recalled echo images; MPSPGR) were obtained in sagittal plane immediately and 1, 2, and 3 min following intravenous administration of gadopentetate dimeglumine (Magnevist; Schering, Germany; 0.1-0.15 mmol/kg). MPSPGR sequences were obtained using TR 40–60 ms, TE 3–5 ms, flip angle 60°, 256×192 matrix, and 5-mm section thickness. Late CE T1WI using parameters of TR/TE 450–700/10 ms, 256×192 matrix, and 5-mm section thickness was obtained in axial and sagittal planes about 5 min after contrast administration.
Image analysis
MR images were retrospectively evaluated by two radiologists who were unaware of histopathological diagnosis, and the differences were resolved by a consensus when there was a discrepancy in the interpretation. Sagittal images were used for analysis of three different MR imaging techniques: T2WI, dynamic CE studies, and late CE T1WI.
SI of uterine lesions were measured at the same area in the same level imaging plane as noncontrast and dynamic CE study performed immediately and 1, 2, and 3 min following contrast administration. SI ratio of lesions to that of noncontrast T1WI was plotted on a graph and compared among different pathologies. Time to peak enhancement and homogeneity of enhancement were recorded in each lesion and compared among different groups. On late CE T1WI, the enhancement degree of the lesions was classified into hypointense, isointense, and hyperintense relative to that of adjacent myometrium and compared between various lesions of different pathologies.
On T2WI, uterine lesions were analyzed as follows: (a) lesion SI, (b) SI homogeneity (homogeneous or heterogeneous), and (c) presence or absence of intratumoral cyst, fibrous core, and myometrial invasion. Lesion SI was compared with that of the outer myometrium and classified as hypointense, isointense, or hyperintense. On T2WI and CE MRI, an intratumoral cyst was defined as a discrete area of water SI within the lesion and the fibrous core as low SI structure at the myometrial junction. Myometrial invasion was defined when normal endometrial lining was disrupted by lesions.
For quantitative analysis, lesion SI on dynamic CE study and late CE T1WI were measured using the round cursor of the same size (>5 mm2) that includes only the solid portion of the lesion on a picture archiving and communication system (PACS) monitor (PathSpeed Workstation, GE Medical Systems, Milwaukee, WI, USA). If the lesion was homogeneous in SI, we put the cursor in the center of the lesion. If the lesion was heterogeneous, we avoided putting the region of interest (ROI) in the cystic or necrotic portions, which were seen as high signal intensity similar to water on T2WI or did not enhance on dynamic and delayed contrast-enhanced MR images. Results were plotted on a graph using ratios of the SI on each sequence of contrast-enhanced scans over those of precontrast scans (contrast-enhanced/precontrast).
Statistical analysis
SI ratios of the endometrial lesions were compared using one-way ANOVA. To compare the proportions of MR imaging features between various lesions, Fischer’s exact test was used. Statistical significance was considered when p value was less than 0.05.
Results
Dynamic CE study
Time to reach peak enhancement and enhancement patterns of various uterine lesions are summarized in Table 1. Endometrial carcinomas reached peak enhancement within 1 min following administration of contrast material in 23/32 (72%) patients whereas only one out of nine myomas showed peak enhancement within 1 min (Table 1). The remaining myomas and all polyps, hyperplasia, adenomyomas, and sarcomas showed maximal enhancement in 2 or 3 min after contrast administration. All five sarcomas showed peak enhancement in 2 or 3 min (Figs. 1, 2, 3, 4, and 5). Statistically, endometrial carcinomas showed significantly earlier peak enhancement than both benign uterine lesions and sarcomas (p<0.05). Endometrial carcinomas, polyps, and myomas showed homogeneous enhancement in 29/32 (91%), 6/9 (67%), and 6/9 (67%), respectively whereas sarcomas showed heterogeneous enhancement in 4/5 (80%). In quantitative analysis, endometrial carcinomas showed early mild enhancement and late gradual washout whereas sarcomas and benign uterine lesions demonstrated more intense and persistent enhancement.
Comparison of signal intensity (SI) ratios (contrast-enhanced/precontrast) of uterine lesions causing an abnormality of the endometrial cavity on dynamic contrast-enhanced MR imaging performed immediately and 1, 2, and 3 min after administration of contrast materia. Signal intensity ratios of these lesions were serially plotted. Endometrial cancers show early peak enhancement with gradual washout while leiomyomas, benign endometrial lesions, and sarcomas show late peak enhancement. EMCA endometrial carcinomas, MYOMA leiomyomas, BEL benign endometrial lesions, SARCOMA sarcomas
A 47-year-old woman with endometrial carcinoma (stage Ia). a Sagittal fast-spin-echo T2-weighted image (TR/effective TE: 4000/85) shows that the endometrial carcinoma (arrows) is polypoid-shaped and homogeneously hyperintense to the outer myometrium. b Sagittal dynamic contrastenhanced and late contrastenhanced MR images were obtained immediately and 1, 3, and 5 min (left to right) following intravenous administration of gadopentetate dimeglumine. The endometrial carcinoma (arrow) reaches peak enhancement immediately after administration of contrast material and then shows gradual washout. The last contrast-enhanced T1WI (TR/TE: 550/10) shows that the enhancement degree of the lesion is weaker than that of the outer myometrium
A 52-year-old woman with endometrial polyp. a Sagittal fast-spin-echo T2-weighted image (TR/effective TE: 6000/104) shows that the endometrial polyp (arrows) is oval shaped and heterogeneously hyperintense to the outer myometrium. b Sagittal dynamic contrast-enhanced MR images and late contrast-enhanced MR images were obtained immediately and 1, 3, and 5 min (left to right) following intravenous injection of gadopentetate dimeglumine. The endometrial polyp (arrow) shows late gradual and persistent enhancement. Time to peak enhancement of the lesion is at 3 min after administration of contrast material. The last contrast-enhanced T1-weighted image (TR/TE: 450/10) shows that the enhancement degree of the lesion is stronger than that of the outer myometrium
A 45-year-old woman with submucosal myoma. a Sagittal fast-spin-echo T2-weighted image (TR/effective TE: 4000/85). The submucosal myoma (arrows) is oval shaped and homogeneously hypointense to the outer myometrium. b Sagittal dynamic contrast-enhanced MR images and late contrast-enhanced MR images were obtained immediately and 1, 3, and 5 min (left to right) following intravenous injection of gadopentetate dimeglumine. The submucosal myoma (arrow) shows late peak enhancement at 3 min after administration of contrast material. The last contrast-enhanced T1-weighted image (TR/TE: 450/10) shows that the enhancement degree of the lesion is slightly weaker than that of the outer myometrium
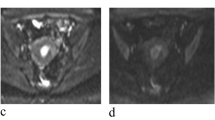
A 57-year-old woman with malignant mixed müllerian tumor. a Sagittal fast-spin-echo T2-weighted image (TR/effective TE: 4500/85) shows that the malignant mixed müllerian tumor (arrows) is an irregular shape and heterogeneously hyperintense to the outer myometrium. An intramural myoma (M) is incidentally detected. b Sagittal dynamic contrast-enhanced and late contrast-enhanced MR images were obtained immediately and 2, 3, and 5 min (left to right) following intravenous administration of gadopentetate dimeglumine. The polypoid endometrial lesion (arrow) demonstrates gradual and persistent enhancement. Time to peak enhancement of the lesion is at 2 min after administration of contrast material. Last contrast-enhanced T1-weighted image (TR/TE: 450/10) shows that the enhancement degree of the lesion is stronger than that of the outer myometrium
Late CE T1WI
On late CE T1WI, all endometrial carcinomas were seen as hypointense SI whereas sarcomas, polyps, myomas, hyperplasia, and the adenomyoma were all seen as hyperintense SI. Compared with dynamic studies, all carcinomas showed further gradual decrease in enhancement while sarcomas and all benign uterine lesions showed persistent enhancement (Figs. 2, 3, 4, and 5). Quantitative analysis demonstrated a significant difference in SIs between the carcinoma and the other groups, including all benign uterine lesions and sarcomas (p<0.05).
T2WI
Of 35 patients with endometrial carcinoma, these lesions showed homogeneous SI in 25 (71%) and heterogeneous SI in ten (29%) on T2WI (Fig. 2). Of ten patients with hyperplastic polyps, these showed homogeneous SI in three (30%) and heterogeneous SI in seven (70%) on T2WI (Fig. 3). Of 12 patients with submucosal myoma, these lesions showed homogeneous SI in three (25%) and heterogeneous SI in nine (75%) (Fig. 4). Of five patients with sarcoma, these showed homogeneous SI in one (25%) and heterogeneous SI in four (75%) (Fig. 5). As compared with sarcoma and benign uterine lesions, endometrial cancer more often demonstrates heterogeneous signal intensity on T2WI (p<0.05).
In 35 patients with endometrial carcinoma, these lesions were isointense to the outer myometrium in eight (23%) and hyperintense in 27 (77%) (Fig. 2). Nine of 12 (75%) submucosal myomas were hypointense to the outer myometrium (Fig. 4). Three (25%) submucosal myomas and two (20%) polyps were isointense to the outer myometrium. Hyperintense SI lesions compared to the outer myometrium were seen in eight (80%) hyperplastic polyps, three (100%) hyperplasias, one (100%) adenomyoma, and five (100%) sarcomas (Figs. 3 and 5). As compared with other uterine lesions, submucosal myomas more often demonstrated low SI relative to myometrium on T2WI (p<0.05). However, there was no significant SI difference on T2WI among endometrial carcinoma, sarcoma, and other benign uterine lesions (p>0.05).
Of 35 patients with endometrial cancer, intratumoral cyst was seen in two (6%) and fibrous core was seen in three (9%). Among the benign uterine lesions, intratumoral cyst was seen in two hyperplastic polyps, three submucosal myomas, and one adenomyoma. Fibrous core was seen in three endometrial cancers, four hyperplastic polyps, one endometrial hyperplasia, and one adenomyoma. However, the incidence of intratumoral cyst and fibrous core was not significantly different between endometrial carcinoma and benign uterine lesions (p>0.05). Myometrial invasion was seen in 80% (28/35) of endometrial carcinomas and 20% (1/5) of sarcomas. No myometrial invasion was seen in the benign lesions. Myometrial invasion was more frequently seen in endometrial carcinoma than in sarcoma (p<0.05).
Discussion
In daily clinical practice, it is often difficult to differentiate various lesions causing an abnormality of endometrial cavity, including endometrial polyp, pedunculated submucosal myoma, endometrial hyperplasia, and carcinoma. Imaging studies are frequently indicated in this situation. Transvaginal US is the primary modality for evaluation of the endometrium [1], and hysterosonography [4] and MR imaging [2, 3, 5–9] can be used for further investigation. Hulka et al. reported that transvaginal US could be useful for differentiation of endometrial lesions [1]. However, even with US, differentiation may be difficult because findings are often nonspecific (e.g., diffuse thickening of the endometrium), and it is not always possible to delineate individual endometrial lesions [1].
MR imaging may be helpful in differentiation of various lesions of the endometrium [2, 3, 5–8] and in assessment of myometrial invasion of endometrial carcinoma [9–15]. Grasel et al. reported that MR imaging could distinguish most endometrial polyps from carcinomas on the basis of morphologic features on T2WI [2]. They also reported that a central core and an intratumoral cyst were more often seen in endometrial polyps than in carcinomas, and myometrial invasion and necrosis was highly predictive for carcinomas [2].
In our study, SI of lesions on T2WI was not useful to differentiate various endometrial lesions except submucosal myoma. Submucosal myoma showed typical low SI, as was described in a previous report [16], and could be differentiated by SI from other endometrial pathologies. An intratumoral cyst or a fibrous core was less frequently seen in our study than reported in Grasel’s study [2]. As they were seen in similar frequency in polyps and carcinomas, the presence or absence of these findings was not very helpful in differentiation of these lesions in our series.
As with other tumors outside the uterus, including hepatocellular carcinoma, renal cell carcinoma, and bladder cancer, endometrial carcinoma typically demonstrates early enhancement. On dynamic study in our series, endometrial carcinomas showed different enhancement patterns compared with other endometrial pathologies. Most endometrial carcinomas showed early maximal enhancement and late gradual washout, which has been described in previous literature [9]. In contrast, benign lesions and sarcomas showed delayed persistent enhancement pattern. The cause of these differences are not known but may be related to the differences in vascular permeability of contrast material between carcinomas and other pathologies.
On late CE T1WI, endometrial carcinomas most frequently showed lower SI than the myometrium, and other uterine lesions, including endometrial sarcoma, polyp, and myoma, tended to show higher SI than the myometrium. These findings correlate well with the result of Imaoka’s work [3]. Ueda et al. reported that heterogeneous SI on T2WI and persistent strong enhancement of endometrial sarcoma on dynamic studies and late CE T1WI were helpful in differentiating them from endometrial carcinomas in spite of limited numbers of the lesions. The relatively large size of sarcomas with enlarged endometrial cavity also might be useful in differentiating these lesions from benign endometrial lesions [17].
Ohguri et al. reported differential features between endometrial carcinoma and malignant mixed mesodermal tumors using gadolinium-enhanced dynamic MR studies [18]. Unlike the results of our study, they described that endometrial cancer shows early peak enhancement only in one out of 11 cases, and most are poorly enhanced. There are a few limitations in their study: endometrial cancers are small in number and are qualitatively analyzed by two radiologists. However, endometrial cancers (n=32) in our study are relatively large in number as compared with their study and are analyzed in a qualitative and quantitative way. Although they shows figures of endometrial cancer of homogeneous but poor enhancement, this lesion seems to reach peak enhancement within 1 min and reveals gradual washout of contrast material on 3-min delayed enhanced MR image similar to the result of our study.
The limitations of our study included the relatively small number of benign lesions and sarcomas compared with the large number of carcinomas. Most endometrial cancers in our study invaded the myometrium. It is ideal to include only early carcinomas without myometrial invasion when they are compared with other tumors on dynamic and delayed CE MR imaging. Further study with a larger population is needed to overcome this limitation. Secondly, we used relatively longer scanning intervals for dynamic CE MR imaging. With relatively longer intervals, we may have missed the detailed enhancement patterns. However, we believe it was enough to evaluate overall enhancement patterns of various uterine lesions. Thirdly, even with advanced imaging techniques, the use of MR imaging in the differentiation of endometrial pathologies may be limited because most often, these lesions are ultimately diagnosed by pathologic examination following endometrial curettage or biopsy. With those invasive procedures, however, it is not uncommon to miss hidden endometrial malignancy. Therefore, being familiar with MR imaging findings of various uterine lesions may be helpful in differentiation of these lesions, particularly when the diagnosis is inconclusive or the patient cannot undergo more invasive procedures.
In conclusion, dynamic CE MR imaging and late CE T1WI may have a potential to differentiate various lesions causing an abnormality of the endometrial cavity. On dynamic contrast-enhanced study, endometrial cancers often showed early weak enhancement whereas most uterine sarcomas and benign uterine lesions, such as myomas and polyps, demonstrated later stronger enhancement. Signal characteristics of uterine lesions on T2WI were not very helpful in differentiation except for low the SI of uterine myoma.
References
Hulka CA, Hall DA, McCarthy K, Simeone JF (1994) Endometrial polyps, hyperplasia, and carcinoma in postmenopausal women: differentiation with endovaginal sonography. Radiology 191:755–758
Hulka CA, Hall DA, McCarthy K, Simeone JF (1994) Endometrial polyps, hyperplasia, and carcinoma in postmenopausal women: differentiation with endovaginal sonography. Radiology 191:755–758
Imaoka I, Sugimura K, Masui T, Takehara Y, Ichijo K, Naito M (1999) Abnormal uterine cavity: differential diagnosis with MR imaging. Magn Reson Imaging 17:1445–1455
Parsons AK, Lense JJ (1993) Sonohysterography for endometrial abnormalities: preliminary results. J Clin Ultrasound 21:87–95
Ascher SM, Johnson JC, Barnes WA, Bae CJ, Patt RH, Zeman RK (1996) MR imaging appearance of the uterus in postmenopausal women receiving tamoxifen therapy for breast cancer: histopathologic correlation. Radiology 200:105–110
Koyama T, Togashi K, Konishi I, Kobayashi H, Ueda H, Kataoka ML, Itoh T, Higuchi T, Fujii S, Konishi J (1999) MR imaging of endometrial stromal sarcoma: correlation with pathologic findings. AJR Am J Roentgenol 173:767–772
Shapeero LG, Hricak H (1989) Mixed müllerian sarcoma of the uterus: MR imaging findings. AJR Am J Roentgenol 153:317–319
Brown JJ, Thurnher S, Hricak H (1990) MR imaging of the uterus: low-signal-intensity abnormalities of the endometrium and endometrial cavity. Magn Reson Imaging 8:309–313
Seki H, Kimura M, Sakai K (1997) Myometrial invasion of endometrial carcinoma: assessment with dynamic MR and contrast-enhanced T1-weighted images. Clin Radiol 52:18–23
Sironi S, Colombo E, Villa G, Taccagni G, Belloni C, Garancini P, DelMaschio A (1992) Myometrial invasion by endometrial carcinoma: assessment with plain and gadolinium-enhanced MR imaging. Radiology 185:207–212
Yamashita Y, Mizutani H, Torashima M, Takahashi M, Miyazaki K, Okamura H, Ushijima H, Ohtake H, Tokunaga T (1993) Assessment of myometrial invasion by endometrial carcinoma: transvaginal sonography vs contrast-enhanced MR imaging. AJR Am J Roentgenol 161:595–599
Kim SH, Kim HD, Song YS, Kang SB, Lee HP (1995) Detection of deep myometrial invasion in endometrial carcinoma: comparison of transvaginal ultrasound, CT, and MRI. J Comput Assist Tomogr 19:766–772
Kim SH, Kim HD, Song YS, Kang SB, Lee HP (1995) Detection of deep myometrial invasion in endometrial carcinoma: comparison of transvaginal ultrasound, CT, and MRI. J Comput Assist Tomogr 19:766–772
Takahashi S, Murakami T, Narumi Y, Kurachi H, Tsuda K, Kim T, Enomoto T, Tomoda K, Miyake A, Murata Y, Nakamura H (1998) Preoperative staging of endometrial carcinoma: diagnostic effect of T2-weighted fast spin-echo MR imaging. Radiology 206:539–547
Seki H, Takano T, Sakai K (2000) Value of dynamic MR imaging in assessing endometrial carcinoma involvement of the cervix. AJR Am J Roentgenol 175:171–176
Murase E, Siegelman ES, Outwater EK, Perez–Jaffe LA, Tureck RW (1999) Uterine leiomyomas: histopathologic features, MR imaging findings, differential diagnosis, and treatment. Radiographics 19:1179–1197
Ueda M, Otsuka M, Hatakenaka M, Sakai S, Ono M, Yoshimitsu K, Honda H, Torii Y (2001) MR imaging findings of uterine endometrial stromal sarcoma: differentiation from endometrial carcinoma. Eur Radiol 11:28–33
Ohguri T, Aoki T, Watanabe H, Nakamura K, Nakata H, Matsuura Y, Kashimura M (2002) MRI findings including gadolinium-enhanced dynamic studies of malignant, mixed mesodermal tumors of the uterus: differentiation from endometrial carcinomas. Eur Radiol 12:2737–2742
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Park, B.K., Kim, B., Park, J.M. et al. Differentiation of the various lesions causing an abnormality of the endometrial cavity using MR imaging: emphasis on enhancement patterns on dynamic studies and late contrast-enhanced T1-weighted images. Eur Radiol 16, 1591–1598 (2006). https://doi.org/10.1007/s00330-005-0085-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-005-0085-1