Abstract
Osteonecrosis (ON) or avascular necrosis (AVN) is a common bone metabolic disorder, mostly affecting femoral head. Although many biological, biophysical, and surgical methods have been tested to preserve the femoral head with ON, none has been proven fully satisfactory. It lacks consensus on an optimal approach for treatment. This is due, at least in part, to the lack of ability to systematically compare treatment efficacy using an ideal animal model that mimics full-range osteonecrosis of femoral head (ONFH) in humans with high incidence of joint collapse accompanied by reparative reaction adjacent to the necrotic bone in a reproducible and accessible way. A number of preclinical animal ON models have been established for testing potential efficacy of various modalities developed for prevention and treatment of ON before introduction into clinics for potential applications. This paper describes a number of different methods for creating animal experimental ON models. Advantages and disadvantages of such models are also discussed as reference for future research in battle against this important medical condition.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Osteonecrosis (ON) or avascular necrosis (AVN), especially at hip joint, i.e., osteonecrosis of the femoral head (ONFH), is a common orthopedic disorder, with an incidence between 10,000 and 20,000 per year reported in the United States. ONFH usually occurs in patients in their late 30s and early 40s. Left untreated, ON generally progresses to femoral head collapse with subsequent secondary osteoarthritis (OA) [1, 2]. Most available treatments for ONFH aim to forestall collapse of the subchondral bone, either by direct reduction in mechanical stresses in vulnerable repairing bone, e.g., through decrease in weight bearing, rotational osteotomies, and vascularized bone grafting, or by enhancing natural structural repair processes by core decompression, electromagnetic stimulation, and bone grafting techniques [3]. With the limited effectiveness of precollapse treatment and higher failure rate of arthroplasties in patients with ONFH, there is great need in recognizing effective treatments that can be reliably applied for preventing femoral head collapse [4]. This controversy is due, in part, to lack of ability to systematically compare treatment efficacy in an animal model whose natural history and its progression mimicking joint collapse in patients of ONFH [5]. Although technically it is rather easier to create early-stage [6, 7] (Tables 1, 2) ON at femoral head in animals using various approaches, it is difficult to develop an animal model that mimics full-range ONFH, from the earlier radiographic and histological changes to the end stage of the problem with structural collapse of the femoral head [3].
In order to test potential protocols for effective ON treatment and study potential underlying mechanism(s) of ON and subsequent ONFH, the ideal experiment animal model should be able to mimic full-range ONFH similar to that occurring in our clinical patients with high incidence of joint collapse accompanied by reparative reaction or bone repair adjacent to the necrotic lesions in a reproducible and accessible way. In addition, the animals used include quadruped, such as rat, rabbits, pig, goats, and dogs, and biped, including chicken and emus, for ideal ONFH model. The animals should be skeletal mature and suitable for testing modalities developed for potential effective prevention and treatment of ON relevant to ON patients with different etiologies, including trauma, disease associated with intravascular coagulation, use of corticosteroid, and alcoholism [8–10] (Fig. 1). This paper categorizes ON into traumatic and non-traumatic ON based on their underlying mechanisms and reviews various methods developed for establishing relevant experimental animal models with ONFH for potential adaptation and/or modification for future basic and clinical research in rheumatology and orthopedics.
Experimental ONFH animal models resulted from trauma
Trauma-induced ON can be subcategorized into following three major forms, i.e., surgical vascular deprivation, physical and chemical insult–induced traumatic ON, with potentials to progress to joint collapse.
ONFH models induced by surgically vascular deprivation
The trauma-induced ON is closely related to the damage of vascularity and blood circulation around the femoral head [11]. Nishino et al. [12] established an adult dog model of ONFH by dislocating the hip joint and ligating the medial and lateral circumflex femoral arteries and veins. At 2 and 4 weeks, 80% of the animals showed widespread necrosis and the necrotic zones were detectable by MRI, yet this study only demonstrated early-stage ON, in part attributed to rather short follow-up time.
Hofstaetter et al. [13] established an adult rabbit model of traumatic ONFH. They achieved this by complete surgical removal of the hip joint capsule, including cauterizing circumferentially the periosteum and blood vessels covering the femoral neck to interrupt the blood supply to the femoral head. The ligamentum teres was also ligated with a non-resorbable suture. A 3-mm drill hole was made through the posterior femoral neck into the marrow cavity, which was then cauterized to interrupt the intramedullary blood supply to the femoral head. They evaluated the femoral head using micro-computerized tomography (micro-CT) and histology and alleged that at 6 months after surgery, no collapse was seen, while at 12 months 2 out of 15 (13.3%) ONFH collapsed. However, the authors of the present review paper carefully reassessed their published findings and found that the study only demonstrated the subchondral fractures with bone resorption while the contour of femoral head did not change significantly according to their micro-CT images. We are of the opinion that the observation time at 1 year after ON induction might be too long. As ON could be reversible, especially in quadrupedal animals [14], and observation with a 6-month interval might be also too long to show both temporal and spatial changes of ONFH and its collapse in spite of good evidence of advanced ON stages reported in this model study.
Levin et al. [15], Peled et al. [16], and many other scientists [17–20] reported a surgical ON model using smaller animal rats. During the operation, the femoral head was dislocated temporarily and the ligamentum teres was cut, the periosteum at the base of the neck of the femoral head was incised together with the reflected capsular fibers twice by circumferentially sweeping the edge of the knife at a 1-mm interval around the bone. Levin et al. observed ON till 42 days after surgery, accompanied with new bone formation in trabecular bone, yet without resulting in joint collapse. As rats grow throughout their life (growth plates remain unclosed), it should be only regarded an early-stage Legg-Calve-Perthes disease (LCPD) model when rats were used as ON model. Differently, after 42 days, Peled et al. found the femoral head distorted while there was no necrotic trabecular bone found histologically. The authors of this review are of the opinion that such structural changes could be explained by the surgery that traumatized small rat hip so as the subsequent instability of hip joint that might result in long-term joint dislocation. Based on bone deformity and less weight bearing on the affected joints, we believe that such distortion might also lead to osteoporosis and osteoarthritis around the rat hip joints. In fact, this phenomenon was indeed by an earlier work of Bejar et al. [21].
Another popular surgical vascular deprivation ON model is a piglet model [22–25], which was induced by placing a ligature tightly around the femoral neck and transecting the ligamentum teres. Hofstaetter et al. [25] found that gross, radiographic, microscopic, and backscattered electron imaging examination revealed typical changes resembling LCPD, such as growth arrest of the epiphysis at 4 weeks and severe flattening due to structural failure of the epiphysis at 8 weeks in all animals following the induction of ischemia. This model would be useful for elucidating the pathogenesis of LCPD as well as for developing preventive and therapeutic strategies.
Swiontkowski et al. [26] developed another ON model in swine by introducing femoral neck fracture and subsequent internal fixation, whose etiology was close to that of clinical patients. Histologically, all femoral heads showed certain degree of necrosis of trabeculae with microstructural deterioration, increase in marrow fat, and neovascularization, with severe cases proceeding to mechanical collapse (7 out of 10 while 5 had closed upper femoral epiphysis and 5 did not) after 8 weeks. Later, Seiler et al. [27] reported similar ONFH model in 12 skeletally mature miniature swine using the same induction protocol reported in Swiontkowski’s paper. Differently, they found only one animal with external changes of cartilage softening and early collapse after 8 weeks, suggesting less reproducible in results.
Physical insult–induced ONFH
Cryogenic and thermal insults have been increasingly adopted as laboratory vehicles for inducing ON. Although not among the causes of naturally occurring ON, they are useful as a research vehicle because the main aspects of the resulting repair response reasonably replicate those of naturally occurring ON lesions [3, 28–30]. In cryosurgery, the freezing process causes direct cellular and vascular injury. With hyperthermia treatment between 43 and 45°C, the tissue temperature mildly raised for a certain period of time is expected to induce cell death by affecting membrane fluidity, cytoskeleton, protein and nuclear structure, and disruption of DNA replication [31].
Malizos et al. [32] described a quadrupedal canine ON model induced by a process of deep freezing, accompanied by stripping of the soft tissue attachments from the femoral neck and intertrochanteric area. This model created ONFH and induced a reparative process that incompletely healed the defect without hip joint collapse. Although it did not fully simulate the human ON, but did provide a basis for further experiment that the freezing could be utilized to establish an ON model. Conzemius et al. [3] proposed an animal model of ONFH in bipedal emus, which is achieved by cryogenic insult with a direct stream of liquid nitrogen delivered into the trabecular bone of the femoral head through a foramen located near the head–neck junction combined with vascular ligation. They found consistently the affected bone region progressed to human-like structural collapse of hip joint. This study also reported an inspiring result on functional disturbance where the animals showed cripple gait patterns in 16 of 19 birds: juxta-articular fragmentation, and collapse with loss of contour of the articular surface were grossly evident in 13 out 19 animals, with 6 exhibiting a crescent sign. Subcapital fracture developed through an area of massive trabecular resorption in 4 of the birds that developed lameness. Emu is a bipedal and sizeable animal with hip joint biomechanics similar to that of humans [5, 33]. This implied that bipedal emu model might be an optimal traumatic ONFH model for testing treatment strategies for the preservation of necrotic hip joints. However, this model should be improved to less subcapital fractures due to the freeze insult, smaller lesion size when compared with more segmental type lesions in ONFH patients, and able to control liquid nitrogen administration and intracephalic temperature [3, 28]. In order to be able to control the key necrotic lesion parameters, a cryo-insult instrument with internal closed circulation of liquid nitrogen was developed [28]. Besides precluding direct contact of liquid nitrogen with the tissue bed, closed circulation has the important advantage of avoiding spurious occlusion of the liquid nitrogen flow stream because of tissue fluid ice formation [28]. The instrument successfully produced segmental lesions in the emu, but without resulting in femoral head collapse. Velez et al. [34] described a similar model that was achieved by means of a cryoprobe and vascular ligation in sheep. Histological findings at 6 and 12 weeks showed progression to advanced stage of ON, but no collapse either. Nevertheless, these two approaches could at least be used as a useful preclinical ONFH model.
Li et al. [30] established an ONFH animal model in rabbits induced by microwave heating, with a good collapse rate in a short term. The femoral heads were heated at 55°C for 10 min, the treated region showed low density and cystic changes in X-ray photographs, and ON and repair occurred simultaneously at 4 and 8 weeks as confirmed histologically, with 69% femoral heads collapsed at 12 weeks. Histological examination showed that the cartilage was damaged as well, and the collapse was exhibited flattening pattern at radiography while the subchondral bone of acetabulum reduced obviously, so authors of this review suspected that the flattening pattern might be a sign of OA.
Many reports revealed that ON could be induced by radiofrequency [35–39]. Martel et al. [35] described that percutaneous radiofrequency ablation in dog long bone and found ON and reparative reaction in trabecular bone with cortical bone and articular cartilage intact. It seemed that the radiofrequency might be an effective biophysical means in creating experimental ONFH model.
Chemical insult–induced ONFH
Manggold et al. [40] established an animal ONFH model in sheep induced by direct intraosseous injection of pure ethanol. Partial necrosis was documented over a period of 12 weeks in all animals with macro-texture, macro-circulation, and joint cartilage intact while 1 out of 10 died during the injection of ethanol due to a massive pulmonary embolism, and another one subcapital fracture occurred 6 weeks postoperatively. They used ethanol as a toxic agent because of its concentration-dependent toxicity and its complete enzymatic degradation. This model showed a high ON incidence, but only early-stage ON with a medium complication incidence, with 2 out of 10 sheep.
Experimental ONFH animal models induced by non-traumatic agents
Non-traumatic ONFH can be categorized into spontaneous, steroid-induced or steroid-associated, lipopolysaccharide-induced or their combination-induced, horse serum-induced, alcohol-induced, and dysbaric ON etc.
Spontaneous ONFH
ON is frequently found in spontaneously hypersensitive rats [41–44]. Hirano et al. [45] suggested that ON in the femoral head of spontaneously hypersensitive male rats was attributed to abnormality of the cartilage in the epiphysis and metaphyseal growth plate and subsequent enchondral ossification. Mihara et al. [46] found when these rats were placed in cages in which they had to stand for eating as they used to be. There was a significantly higher ON incidence of 40% when the rats were forced to stand. This implied that weight bearing could increase ON incidence. Because rats grow throughout their life, this and other rat models might be best regarded as models of a LCPD [47].
Steroid-induced ONFH
Corticosteroid medication is a pivotal risk factor in ON development [48], but a causal relationship is not always directly found [8]. Many scientists described steroid-induced ONFH model in rabbit by administering methylprednisolone (MPS) intramuscularly. Iwakiri et al. [49] described a rabbit model by 20 mg/kg MPS administered once intramuscularly, with 83% incidence of ON in proximal metaphysis histologically 3 weeks after induction. Kuribayashi et al. [50] described a same model with 70% ON incidence at the distal one-third and proximal one-third femur histologically at 4 weeks, yet 20% rabbits died after the MPS induction. Takao et al. [51] also used the same model, but only found bone marrow necrosis located in the proximal metaphysis or diaphysis, yet without ON when continuously monitored at 1, 3, 6, and 9 postinduction weeks. From the results of this same rabbit model, we might argue that this model was not a repeatable one. Wang et al. [52] and Ichiseki et al. [53] described a similar rabbit model induced by a single intramuscular injection of 4 mg/kg MPS. ON was judged based on the presence of necrosis of the medullary haematopoietic cells or fat cells or empty lacunae or condensed nuclei in osteocytes in either of the isolated femora. We think the rule to verify ON might not be rigorous, as most scientists defined ON as the diffuse presence of empty lacunae or pyknotic nuclei of osteocytes in the trabecular bone, accompanied by surrounding bone marrow cell necrosis [54], so the structural definition on ON incidence in both models might not be credible to some extent. Kabata [55] administered 4 mg/kg MPS per injection intramuscularly for 1, 2, 4, or 8 times, respectively, and ON was found concentrated on the medial side of the metaphyseal region and shaft region 1 week after induction with an ON incidence of 47, 60,73, and 67%, respectively. The size or number of necrotic foci within the proximal femur was not significantly different between the groups. In steroid-induced ON in rabbits, ON lesion was not concentrated on femoral head, and there was only ON sign in its early stage, implying that these models were not ideal models for studying ONFH.
Han et al. [56] described a steroid-induced ON model in rats, where the rats received subcutaneous injections of 21 mg/kg/day MPS for 4 weeks with an incidence of ONFH up to 80%. But they defined early ON as a condition in which the marrow cells had disappeared or had degenerated and bone marrow spaces had been filled with adipocytes, though trabecular osteocytes were still alive. This model was not a typical ONFH model but also an early-stage LCPD model.
Yang et al. [57] established a steroid-induced ON model in mice for the first time by oral dexamethasone for up to 12 weeks either by continuous dosing or by intermittent dosing, the frequency of ON trended lower after intermittent compared with the continuous dosing for 12 weeks (8% vs. 45%), consistent with the possible benefits of a “steroid holiday” seen in clinical settings [58]. But ON was identified histologically only in the distal femora and only at early stage without resulting in a high ON incidence.
Wang et al. [59] established a bipedal chicken model induced by intramuscular injections of 3 mg/kg MPS weekly. ON evidence including subchondral bone death and resorption, fat cell proliferation and new bone formation were seen at 24 weeks in 4 out of 12 chickens while 48% animals died at the experiment period. With low ON incidence and high mortality, this model was not as good as the quadrupedal rabbit model, but it was at least the first successful try to establish ON model in bipedal animals.
Lipopolysaccharide-induced ON
Irisa et al. [60] developed ON model in rabbits induced by Shwartzman reaction with a single low-dose (10 μg/kg) lipopolysaccharide (LPS) intravenous injection that showed a multifocal ON in 77% of the treated rabbits after 4 weeks where 4 out of 35 rabbits died after injection. Organized thrombi in the intraosseous small-sized arteries and arterioles were frequently seen in and around the necrotic tissues. Although ON was seen at femoral epiphysis in only 9% of the treated rabbits, only early-stage ON was induced. This model would be useful for elucidating the pathogenesis of non-steroid non-traumatic ON in patients especially with inflammatory hypercoagulability and also a useful model for testing strategies developed for ON prevention and therapy.
Immune reaction–induced ON
Tsuji et al. [61, 62] described a rabbit serum sickness ON model induced by immune reaction induced by an intravenous injection of 10 ml/kg of sterile heat–inactivated horse serum at room temperature, administered twice with a 3-week interval, similar to the immune complex deposition that was seen in patients with systemic lupus erythematosus (SLE). At 72 h, no ON incidence was found, but already 86% after 1 week, yet back to 64% after 3 weeks. There was only early-stage ON, and no ON was seen at femoral head.
ON induced by steroid in combination with other non-traumatic factors
ON induced by steroid in combination with LPS
Yamamoto T et al. [63] were the first to use a combination of the Shwartzman reaction and corticoid injections in rabbits to develop an animal ON model in 1995. This model showed a significantly higher incidence (85%) and wider area of ON in the femur and humerus than that found in rabbits with either Shwartzman reaction or steroid injection alone, however, accompanied with high mortality (50%) of experimental animals. Now many scientist utilized Qin’s protocol [14] to establish steroid-associated ON model in rabbit induced by a single low-dose LPS (10 μg/kg) intravenous injection and subsequently three intramuscular injections of high-dose MPS (20 mg/kg) at a time interval of 24 h for testing strategies developed for the prevention of ON [64–67]. In Qin’s work, 6 weeks after induction, 93% of the rabbits developed ON, with 29% in the proximal epiphysis and no rabbits died throughout the experiment period. Both high ON incidence and no mortality in rabbits treated with this inductive protocol suggested its effectiveness for the evaluation of therapeutic efficacy of interventions developed for prevention of steroid-associated ON. Similarly, Wu et al. [68] described a rabbit model induced by two low-dose LPS (10 μg/kg) intravenous injections and subsequently three intramuscular injections of high-dose MPS (20 mg/kg) at a time interval of 24 h with a slightly lower incidence of ON lesion (90%) and higher mortality (6.2%) compared with Qin and coworkers’ protocol. Later, Guan et al. [69] also described a rabbit model induced by steroid and LPS, with two injections of lipopolysaccharide (40 μg/kg) at an interval of 24 h and was then immediately given one injection of prednisolone acetate (20 mg/kg). This model showed a significant higher incidence of ON at femoral head(36.2% vs. 30.0%)when compared with steroid injection alone after 3 weeks, and no rabbits died throughout the experiment period. Kawamoto et al. [70] reported that there was a high mortality in rabbit with LPS dose more than 15 μg/kg, but no animal died with the high LPS dose as 49 μg/kg at this model; the high incidence (30.0%) of ON of femoral head in group of steroid injection only also was never seen in similar models [49–51], and this may imply that this model might not be reproducible. Okazaki et al. [71] described a non-traumatic ON model in male Wistar rats induced by twice 2 mg/kg LPS intravenously and three 20 mg/kg MPS intramuscularly with a 24-h interval at each injection. The animals were killed 1, 2, 3, and 4 weeks after the last injection and found an ON incidence at proximal femur of 33, 33, 67, and 33%, respectively. But this study only had 3 animals in most groups (3 out of 4), suggesting that large sample size was essential to repeat the study before compared with other models.
ON induced by steroid in combination with horse serum
Matsui et al. [72] described a rabbit ON model induced by employing a combined protocol of hypersensitivity vasculitis caused by horse serum and administration of high-dose corticosteroids. Fourteen of 20 specimens (70%) showed histological evidence of ON in the femoral metaphysic. Among them, 7 showed marrow necrosis and seven marrow and trabecular necrosis while no ON was observed at the other two groups induced by horse serum or steroid alone. But compared with models of other scientists [49, 61], the incidence was not higher than that induced by steroid alone induced. Later, Wen et al. [73] established a rabbit early-stage ON model induced by hypersensitivity vasculitis with injection of horse serum intravenous (first dose of 10 ml/kg and second dose of 5 ml/kg with a time interval of 2 days) twice and 2 weeks later administration of 7.5 mg/kg of prednisolone acetate intraperitoneal twice a week for 2 weeks. As they did not provide ON incidence in the published study, we could not compare this model with that induced by steroid or horse serum alone. In another words, we could not verify whether this combinational ON induction protocol was superior to other reported ones induced by steroid alone or to other steroid-associated ON models.
Alcohol-induced ON
Alcohol consumption is popular in Asia, especially in China, which frequently resulted in ONFH [48]. In order to understand its underlying pathophysiology, Wang et al. [74] tested an ON induction protocol in mice by spirits (20 ml/kg body weight) containing 46% ethanol and administered intragastrically. After 6 months, ON was seen in the subchondral region of the femoral head. Although this was still early-stage ON feature, but the etiology was parallel to that often seen in ONFH patients. This model would be therefore useful for elucidating the pathogenesis of alcohol-related ONFH in humans as well as for evaluating different therapeutic protocols.
Dysbaric ON
In 1981, Chryssanthou [75] described a dysbaric ON model in C57BL/6 J mice subjected to 75 psig (516.75 kpa) air pressure for 2–3 h followed by stage decompression. Histological evidences of ON showed similarities to human dysbaric ON after a latent period of more than 2 months. Later in 1997, Lehner et al. [76] established a dysbaric ON in adult sheep after 12–13, 24 h exposures to compressed air (2.6–2.9 atm absolute) during a 2-month period. At 7 months, juxta-articular regions of some long bones showed histological evidences of apoptosis of osteocytes and fatty marrow fibrosis; although as in human caisson disease most lesions were diaphyseal. This animal model seems a suitable one for investigating the pathogenesis, diagnosis, and treatment of dysbaric ON.
Chemically induced ON
Bone injury occurs in human hemolytic disorders associated with thrombosis, such as betathalassemia and sickle-cell disease [77]. Metabolic activation of 2-butoxyethanol (BE) to form butoxyacetic acid (BAA) is a prerequisite for the development of hematotoxicity. Shabat et al. [77] reported a new rat model for ON induced by four daily doses of 250 mg BE/5 ml water/kg of body weight for four consecutive days. At 24 days after induction, ON in femur was seen histologically in 1 of 8 animals while changes in the femurs were confined to the diaphysis. This model is therefore useful for studying ON induced by sickle-cell disease and other hemoglobinopathies.
Experimental ONFH animal model induced by steroid combined with surgical vascular deprivation
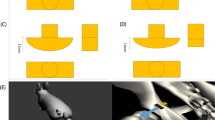
Recently, Kuroda et al. [78] described a new ONFH animal model in adult rabbit induced by once intramuscular injection with 40 mg/kg methylprednisolone and vascular occlusion of the capital femoral epiphysis by electrocoagulation. The rabbits started to develop ONFH around 4 weeks and with confirmed ONFH within 8 weeks. At 12 weeks, collapse of the femoral head was observed in 2 out of 5 animals. At 24 weeks after the surgery, all specimens showed OA changes. This result was better than that of rabbit ONFH model induced by similar surgical vascular deprivation [13] or steroid alone [49–51]. However, by judging the micro-CT images used for defining the collapse by Kuroda et al., only irregular subchondral bone deformity without typical collapse was present. The reparative reaction to necrotic bone showed as appositional bone formation on the surface of necrotic trabeculae histologically, which was, however, defined as limited repair [14] instead of a destructive repair that was often seen in collapsed femoral head of ONFH patients [79], suggesting a structural collapse in bipedal emus that found in authors’ own research (Fig. 2).
Representative images of the collapsed femoral Head of emu (Pointed with red arrows). a 3-D reconstruction of the proximal femur region. b Sagittal, horizontal and coronal sections of the collapsed femoral head. c Destructive repair: granulation tissue creep (pointed with thin arrows) linked to necrotic bone resorption (pointed with arrow) and limited new bone formation (pointed with arrowhead) (H&E staining, × 40). d Gross coronal section obtained from the same femoral head with A. Typical signs of segmental osteonecrosis (Pointed with black arrows) and segmental collapse (Pointed with red arrows)
Concluding remarks
Over the past decades, efforts have been made to establish animal models mimicking the etiology and pathophysiology of ON and also simulating structural collapse of the hip joint. Based on our systemic review, we might conclude that the ideal animal model(s) with ONFH has not been established using either traumatic or non-traumatic intervention (Fig. 3). There were always some disadvantages should be improved further. In traumatic models, one of the advantages is that the necrotic lesions concentrated in femoral head and a big range of ON stages could be achieved, especially up to the end stage of ONFH in bipedal emu model. The bipedal emu with body size and hip joint similar to human has great advantages to be utilized in an ideal ONFH model in future, especially in orthopedic research for testing efficacy treatment protocols. Except lower morbidity and smaller necrotic lesion, cryogenic insult used in the Conzemius’s emu model did not parallel to the etiologies of ONFH patients, and it would be better if we could established a full-range non-traumatic ONFH emu model, from the earliest histological changes to end-stage structural and mechanical collapse of the femoral head. Non-traumatic ON models had an advantage with etiology similar to ON patients but also with disadvantages of only early-stage ON and necrotic lesions mostly in metaphysis instead of concentrating in femoral head, partially due to the difference in blood supply, metabolism, and associated pathophysiology. A combination induction protocol with steroid and surgical vascular deprivation may achieve higher ON incidence than either method alone. However, we should also have to realize possible compensation of other advantages of traumatic or non-traumatic models, as the etiology did not parallel to humans and necrotic lesions might not confine to femoral head.
Compared with adult animals, the piglet seemed more sensitive to surgical vascular deprivation and progressed to severe flattening after ON induction. It surely was a good LCPD model, but the pathophysiology, natural history and treatments were differ between LCPD and the adult form of ONFH [80]. What is observed in the immature femoral head could not be extrapolated directly to the adult femoral head [25].
Compared with quadrupedal animals, the bipedal emu had the great advantage of being a sizeable animal with hip joint biomechanics similar to that of humans [5, 33]. For the loading onto the osteonecrotic zone also contributes to the femoral head collapse [79], the differences in hip joint biomechanics between biped and quadruped could be the crucial factor resulting or not resulting in joint collapse. As steroid-induced ON model in chicken did not show advantages, it seemed that bipedal birds might not be sensitive to steroid as mammalian.
Since there is no ideal ONFH animal model(s) available, the authors of this review paper made commented on advantages and limitations of various ON models. Kim and coworkers introduced a surgical vascular deprivation ON model in piglet induced by placing a ligature tightly around the femoral neck and transecting the ligamentum teres. This approach would be more useful for elucidating the pathogenesis of LCPD as well as for developing preventive and therapeutic strategies. Qin and coworkers’ protocol in rabbit induced by a single low-dose LPS intravenous injection and subsequently three intramuscular injections of high-dose MPS would be more effective for the evaluation of therapeutic efficacy of interventions developed for prevention of steroid-associated ON. To test the potential protocols for treatment of ONFH, especially in treatment to forestall collapse, Conzemius and coworkers’ emu model induced by cryogenic insult combined with vascular ligation would be better. Authors of this review paper are of the view point that the bipedal emu model would be the more ideal model ONFH model up to date.
Taken together, ONFH animal models have been utilized in research for many years that did improve our understandings about this common orthopedic disorder. However, much work is still ahead of us, including establishing ideal model(s).
References
Lavernia CJ, Sierra RJ, Grieco FR (1999) Osteonecrosis of the femoral head. J Am Acad Orthop Surg 7(4):250–261
Mont MA, Jones LC, Einhorn TA, Hungerford DS, Reddi AH (1998) Osteonecrosis of the femoral head. Potential treatment with growth and differentiation factors. Clin Orthop Relat Res (355 Suppl): S314–335
Conzemius MG, Brown TD, Zhang Y, Robinson RA (2002) A new animal model of femoral head osteonecrosis: one that progresses to human-like mechanical failure. J Orthop Res 20(2):303–309. doi:10.1016/S0736-0266(01)00108-5
McGrory BJ, York SC, Iorio R, Macaulay W, Pelker RR, Parsley BS, Teeny SM (2007) Current practices of aahks members in the treatment of adult osteonecrosis of the femoral head. J Bone Joint Surg Am 89(6):1194–1204. doi:89/6/1194[pii]10.2106/JBJS.F.00302
Troy KL, Brown TD, Conzemius MG (2009) Contact stress distributions on the femoral head of the emu (dromaius novaehollandiae). J Biomech 42(15):2495–2500. doi:S0021-9290(09)00419-9[pii]10.1016/j.jbiomech.2009.07.017
Ficat RP (1985) Idiopathic bone necrosis of the femoral head. Early diagnosis and treatment. J Bone Joint Surg Br 67(1):3–9
Steinberg ME, Hayken GD, Steinberg DR (1995) A quantitative system for staging avascular necrosis. J Bone Joint Surg Br 77(1):34–41
Assouline-Dayan Y, Chang C, Greenspan A, Shoenfeld Y, Gershwin ME (2002) Pathogenesis and natural history of osteonecrosis. Semin Arthritis Rheum 32(2):94–124. doi:S0049017202000586[pii]
Aaron RK (1998) Osteonecrosis: etiology, pathophysiology and diagnosis. In: Callaghan JJ, Rosenberg AG, Rubash HE (eds) The adult hip. Lippincott-Ravin, Philadelphia, pp 451–466
Parsons SJ, Steele N (2007) Osteonecrosis of the femoral head: part 1—aetiology, pathogenesis, investigation, classification. Current Orthopaedics 21(6):457–463. doi:10.1016/j.cuor.2007.11.004
Malizos KN, Karantanas AH, Varitimidis SE, Dailiana ZH, Bargiotas K, Maris T (2007) Osteonecrosis of the femoral head: etiology, imaging and treatment. Eur J Radiol 63(1):16–28. doi:S0720-048X(07)00159-3[pii]10.1016/j.ejrad.2007.03.019
Nishino M, Matsumoto T, Nakamura T, Tomita K (1997) Pathological and hemodynamic study in a new model of femoral head necrosis following traumatic dislocation. Arch Orthop Trauma Surg 116(5):259–262
Hofstaetter JG, Wang J, Yan J, Glimcher MJ (2009) The effects of alendronate in the treatment of experimental osteonecrosis of the hip in adult rabbits. Osteoarthritis Cartilage 17(3):362–370. doi:S1063-4584(08)00248-3[pii]10.1016/j.joca.2008.07.013
Qin L, Zhang G, Sheng H, Yeung KW, Yeung HY, Chan CW, Cheung WH, Griffith J, Chiu KH, Leung KS (2006) Multiple bio-imaging modalities in evaluation of an experimental osteonecrosis induced by a combination of lipopolysaccharide and methylprednisolone. Bone 39(4):863–871. doi:S8756-3282(06)00419-4[pii]10.1016/j.bone.2006.04.018
Levin D, Norman D, Zinman C, Rubinstein L, Sabo E, Misselevich I, Reis D, Boss JH (1999) Treatment of experimental avascular necrosis of the femoral head with hyperbaric oxygen in rats: histological evaluation of the femoral heads during the early phase of the reparative process. Exp Mol Pathol 67(2):99–108. doi:10.1006/exmp.1999.2273S0014-4800(99)92273-6[pii]
Peled E, Bejar J, Zinman C, Boss JH, Reis DN, Norman D (2009) Prevention of distortion of vascular deprivation-induced osteonecrosis of the rat femoral head by treatment with alendronate. Arch Orthop Trauma Surg 129(2):275–279. doi:10.1007/s00402-008-0656-0
Vadasz Z, Misselevich I, Norman D, Peled E, Boss JH (2004) Localization of vascular endothelial growth factor during the early reparative phase of the rats’ vessels deprivation-induced osteonecrosis of the femoral heads. Exp Mol Pathol 77(2):145–148. doi:10.1016/j.yexmp.2004.06.002S0014-4800(04)00062-0[pii]
Levin D, Norman D, Zinman C, Misselevich I, Reis DN, Boss JH (1999) Osteoarthritis-like disorder in rats with vascular deprivation-induced necrosis of the femoral head. Pathol Res Pract 195(9):637–647
Norman D, Reis D, Zinman C, Misselevich I, Boss JH (1998) Vascular deprivation-induced necrosis of the femoral head of the rat. An experimental model of avascular osteonecrosis in the skeletally immature individual or legg-perthes disease. Int J Exp Pathol 79(3):173–181
Peskin B, Shupak A, Misselevich I, Zinman C, Levin D, Jacob Z, Reis DN, Boss JH (2001) Transphyseal osseous bridges in experimental osteonecrosis of the femoral head of the rat. Histologic study of the bony bridges connecting the epiphyseal with the metaphyseal bony trabeculae through gaps in the physeal cartilage. J Pediatr Orthop B 10(3):214–218
Bejar J, Peled E, Boss JH (2005) Vasculature deprivation–induced osteonecrosis of the rat femoral head as a model for therapeutic trials. Theor Biol Med Model 2:24. doi:1742-4682-2-24[pii]10.1186/1742-4682-2-24
Kim HK, Su PH, Qiu YS (2001) Histopathologic changes in growth-plate cartilage following ischemic necrosis of the capital femoral epiphysis. An experimental investigation in immature pigs. J Bone Joint Surg Am 83(5):688–697
Koob TJ, Pringle D, Gedbaw E, Meredith J, Berrios R, Kim HK (2007) Biomechanical properties of bone and cartilage in growing femoral head following ischemic osteonecrosis. J Orthop Res 25(6):750–757. doi:10.1002/jor.20350
Kim HK, Sanders M, Athavale S, Bian H, Bauss F (2006) Local bioavailability and distribution of systemically (parenterally) administered ibandronate in the infarcted femoral head. Bone 39(1):205–212. doi:S8756-3282(05)00605-8[pii]10.1016/j.bone.2005.12.019
Hofstaetter JG, Roschger P, Klaushofer K, Kim HK (2010) Increased matrix mineralization in the immature femoral head following ischemic osteonecrosis. Bone 46(2):379–385. doi:S8756-3282(09)01972-3[pii]10.1016/j.bone.2009.10.006
Swiontkowski MF, Tepic S, Rahn BA, Cordey J, Perren SM (1993) The effect of fracture on femoral head blood flow Osteonecrosis and revascularization studied in miniature swine. Acta Orthop Scand 64(2):196–202
Seiler JG, Kregor PJ, Conrad EU, Swiontkowski MF (1996) Posttraumatic osteonecrosis in a swine model—correlation of blood cell flux, mri and histology. Acta Orthopaedica Scandinavica 67(3):249–254
Reed KL, Brown TD, Conzemius MG (2003) Focal cryogen insults for inducing segmental osteonecrosis: computational and experimental assessments of thermal fields. J Biomech 36(9):1317–1326. doi:S0021929003001544[pii]
Mont MA, Einhorn TA, Sponseller PD, Hungerford DS (1998) The trapdoor procedure using autogenous cortical and cancellous bone grafts for osteonecrosis of the femoral head. J Bone Joint Surg Br 80(1):56–62
Li Y, Han R, Geng C, Wang Y, Wei L (2009) A new osteonecrosis animal model of the femoral head induced by microwave heating and repaired with tissue engineered bone. Int Orthop 33(2):573–580. doi:10.1007/s00264-008-0672-2
Hamazoe R, Maeta M, Murakami A, Yamashiro H, Kaibara N (1991) Heating efficiency of radiofrequency capacitive hyperthermia for treatment of deep-seated tumors in the peritoneal cavity. J Surg Oncol 48(3):176–179
Malizos KN, Quarles LD, Seaber AV, Rizk WS, Urbaniak JR (1993) An experimental canine model of osteonecrosis: characterization of the repair process. J Orthop Res 11(3):350–357. doi:10.1002/jor.1100110306
Troy KL, Lundberg HJ, Conzemius MG, Brown TD (2007) Habitual hip joint activity level of the penned emu (dromaius novaehollandie). Iowa Orthop J 27:17–23
Velez R, Soldado F, Hernandez A, Barber I, Aguirre M A new preclinical femoral head osteonecrosis model in sheep. Arch Orthop Trauma Surg. doi:10.1007/s00402-010-1084-5
Martel J, Bueno A, Dominguez MP, Llorens P, Quiros J, Delgado C (2008) Percutaneous radiofrequency ablation: relationship between different probe types and procedure time on length and extent of osteonecrosis in dog long bones. Skeletal Radiol 37(2):147–152. doi:10.1007/s00256-007-0416-1
Le TX, Andrews RT (2008) Thermal osteonecrosis of the rib after radiofrequency ablation in the thorax. J Vasc Interv Radiol 19(6):940–944. doi:S1051-0443(08)00229-7[pii]10.1016/j.jvir.2008.02.017
Encalada I, Richmond JC (2004) Osteonecrosis after arthroscopic meniscectomy using radiofrequency. Arthroscopy 20(6):632–636. doi:S0749806304005559[pii]
Cetik O, Cift H, Comert B, Cirpar M (2009) Risk of osteonecrosis of the femoral condyle after arthroscopic chondroplasty using radiofrequency: a prospective clinical series. Knee Surg Sports Traumatol Arthrosc 17(1):24–29. doi:10.1007/s00167-008-0604-0
Bonutti PM, Seyler TM, Delanois RE, McMahon M, McCarthy JC, Mont MA (2006) Osteonecrosis of the knee after laser or radiofrequency-assisted arthroscopy: treatment with minimally invasive knee arthroplasty. J Bone Joint Surg Am 88(Suppl 3):69–75. doi:88/suppl_3/69[pii]10.2106/JBJS.F.00533
Manggold J, Sergi C, Becker K, Lukoschek M, Simank HG (2002) A new animal model of femoral head necrosis induced by intraosseous injection of ethanol. Lab Anim 36(2):173–180
Shibahara M, Nishida K, Asahara H, Yoshikawa T, Mitani S, Kondo Y, Inoue H (2000) Increased osteocyte apoptosis during the development of femoral head osteonecrosis in spontaneously hypertensive rats. Acta Med Okayama 54(2):67–74
Wada M, Kumagai K, Murata M, SY Y, Shindo H (2004) Warfarin reduces the incidence of osteonecrosis of the femoral head in spontaneously hypertensive rats. J Orthop Sci 9(6):585–590. doi:10.1007/s00776-004-0829-9
Suzuki M, Kumagai K, Osaki M, Murata M, Tomita M, Miyata N, Hozumi A, Niwa M (2008) Osteonecrosis of femoral head in the stroke-prone spontaneously hypertensive rats, especially old rats. Clin Exp Hypertens 30(7):689–697. doi:904100434[pii]10.1080/10641960802251883
Kataoka Y, Hasegawa Y, Iwata H, Matsuda T, Genda E, Miura T, Takahashi H (1992) Effect of hyperbaric oxygenation on femoral head osteonecrosis in spontaneously hypertensive rats. Acta Orthop Scand 63(5):527–530
Hirano T, Iwasaki K, Yamane Y (1988) Osteonecrosis of the femoral head of growing, spontaneously hypertensive rats. Acta Orthop Scand 59(5):530–535
Mihara K, Hirano T (1998) Standing is a causative factor in osteonecrosis of the femoral head in growing rats. J Pediatr Orthop 18(5):665–669
Catterall A (1981) Legg-calve-perthes syndrome. Clin Orthop Relat Res (158): 41–52
Mont MA, Jones LC, Hungerford DS (2006) Nontraumatic osteonecrosis of the femoral head: ten years later. J Bone Joint Surg Am 88(5):1117–1132. doi:88/5/1117[pii]10.2106/JBJS.E.01041
Iwakiri K, Oda Y, Kaneshiro Y, Iwaki H, Masada T, Kobayashi A, Asada A, Takaoka K (2008) Effect of simvastatin on steroid-induced osteonecrosis evidenced by the serum lipid level and hepatic cytochrome p4503a in a rabbit model. J Orthop Sci 13(5):463–468. doi:10.1007/s00776-008-1257-z
Kuribayashi M, Fujioka M, Takahashi KA, Arai Y, Ishida M, Goto T, Kubo T Vitamin e prevents steroid-induced osteonecrosis in rabbits. Acta Orthop 81(1):154–160. doi:10.3109/17453671003628772
Takao M, Sugano N, Nishii T, Sakai T, Nakamura N, Yoshikawa H (2009) Different magnetic resonance imaging features in two types of nontraumatic rabbit osteonecrosis models. Magn Reson Imaging 27(2):233–239. doi:S0730-725X(08)00210-5[pii]10.1016/j.mri.2008.07.001
Wang L, Wang N, Li M, Wang K To investigate the role of the nervous system of bone in steroid-induced osteonecrosis in rabbits. Osteoporos Int. doi:10.1007/s00198-009-1159-8
Ichiseki T, Matsumoto T, Nishino M, Kaneuji A, Katsuda S (2004) Oxidative stress and vascular permeability in steroid-induced osteonecrosis model. J Orthop Sci 9(5):509–515. doi:10.1007/s00776-004-0816-1
Sugano N, Kubo T, Takaoka K, Ohzono K, Hotokebuchi T, Matsumoto T, Igarashi H, Ninomiya S (1999) Diagnostic criteria for non-traumatic osteonecrosis of the femoral head. A multicentre study. J Bone Joint Surg Br 81(4):590–595
Kabata T, Kubo T, Matsumoto T, Hirata T, Fujioka M, Takahashi KA, Yagishita S, Kobayashi M, Tomita K (2005) Onset of steroid-induced osteonecrosis in rabbits and its relationship to hyperlipaemia and increased free fatty acids. Rheumatology (Oxford) 44(10):1233–1237. doi:keh721[pii]10.1093/rheumatology/keh721
Zhang X, Liu Y, Ren K, Liu J, Zhu B, Sun Z [secondary total hip arthroplasty for osteonecrosis of femoral head after failed internal fixation of femoral neck fracture]. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi 24(3):257–261
Yang L, Boyd K, Kaste SC, Kamdem Kamdem L, Rahija RJ, Relling MV (2009) A mouse model for glucocorticoid-induced osteonecrosis: effect of a steroid holiday. J Orthop Res 27(2):169–175. doi:10.1002/jor.20733
Frediani B, Falsetti P, Bisogno S, Baldi F, Acciai C, Filippou G, Bacarelli MR, Filipponi P, Galeazzi M, Marcolongo R (2004) Effects of high dose methylprednisolone pulse therapy on bone mass and biochemical markers of bone metabolism in patients with active rheumatoid arthritis: a 12 months randomized prospective controlled study. J Rheumatol 31(6):1083–1087. doi:0315162X-31-1083[pii]
Cui Q, Wang GJ, Su CC, Balian G (1997) The otto aufranc award. Lovastatin prevents steroid induced adipogenesis and osteonecrosis. Clin Orthop Relat Res (344):8–19
Irisa T, Yamamoto T, Miyanishi K, Yamashita A, Iwamoto Y, Sugioka Y, Sueishi K (2001) Osteonecrosis induced by a single administration of low-dose lipopolysaccharide in rabbits. Bone 28(6):641–649. doi:S8756328201004604[pii]
Tsuji T, Sugano N, Sakai T, Yoshikawa H (2003) Evaluation of femoral perfusion in a non-traumatic rabbit osteonecrosis model with t2*-weighted dynamic mri. J Orthop Res 21(2):341–351. doi:S0736026602001444[pii]10.1016/S0736-0266(02)00144-4
Sakaia T, Sugano N, Tsuji T, Nishii T, Yoshikawa H, Ohzono K (2000) Serial magnetic resonance imaging in a non-traumatic rabbit osteonecrosis model: an experimental longitudinal study. Magn Reson Imaging 18(7):897–905. doi:S0730-725X(00)00175-2[pii]
Yamamoto T, Hirano K, Tsutsui H, Sugioka Y, Sueishi K (1995) Corticosteroid enhances the experimental induction of osteonecrosis in rabbits with shwartzman reaction. Clin Orthop Relat Res (316):235–243
Zhang G, Sheng H, He YX, Xie XH, Wang YX, Lee KM, Yeung KW, Li ZR, He W, Griffith JF, Leung KS, Qin L (2009) Continuous occurrence of both insufficient neovascularization and elevated vascular permeability in rabbit proximal femur during inadequate repair of steroid-associated osteonecrotic lesions. Arthritis Rheumatism 60(10):2966–2977. doi:10.1002/Art.24847
Sheng HH, Zhang GG, Cheung WH, Chan CW, Wang YX, Lee KM, Wang HF, Leung KS, Qin LL (2007) Elevated adipogenesis of marrow mesenchymal stem cells during early steroid-associated osteonecrosis development. J Orthop Surg Res 2:15. doi:1749-799X-2-15[pii]10.1186/1749-799X-2-15
Zhang G, Qin L, Sheng H, Yeung KW, Yeung HY, Cheung WH, Griffith J, Chan CW, Lee KM, Leung KS (2007) Epimedium-derived phytoestrogen exert beneficial effect on preventing steroid-associated osteonecrosis in rabbits with inhibition of both thrombosis and lipid-deposition. Bone 40(3):685–692. doi:S8756-3282(06)00803-9[pii]10.1016/j.bone.2006.10.026
Sun Y, Feng Y, Zhang C (2009) The effect of bone marrow mononuclear cells on vascularization and bone regeneration in steroid-induced osteonecrosis of the femoral head. Joint Bone Spine 76(6):685–690. doi:S1297-319X(09)00101-8[pii]10.1016/j.jbspin.2009.04.002
Wu X, Yang S, Duan D, Zhang Y, Wang J (2008) Experimental osteonecrosis induced by a combination of low-dose lipopolysaccharide and high-dose methylprednisolone in rabbits. Joint Bone Spine 75(5):573–578. doi:S1297-319X(08)00089-4[pii]10.1016/j.jbspin.2007.11.004
Guan XY, Han D Role of hypercoagulability in steroid-induced femoral head necrosis in rabbits. J Orthop Sci 15(3):365–370. doi:10.1007/s00776-010-1452-6
Kawamoto S, Shirai N, Strandberg JD, Boxerman JL, Bluemke DA (2000) Nontraumatic osteonecrosis: Mr perfusion imaging evaluation in an experimental model. Acad Radiol 7(2):83–93
Okazaki S, Nishitani Y, Nagoya S, Kaya M, Yamashita T, Matsumoto H (2009) Femoral head osteonecrosis can be caused by disruption of the systemic immune response via the toll-like receptor 4 signalling pathway. Rheumatology (Oxford) 48(3):227–232. doi:ken462[pii]10.1093/rheumatology/ken462
Matsui M, Saito S, Ohzono K, Sugano N, Saito M, Takaoka K, Ono K (1992) Experimental steroid-induced osteonecrosis in adult rabbits with hypersensitivity vasculitis. Clin Orthop Relat Res (277):61–72
Wen Q, Ma L, Chen YP, Yang L, Luo W, Wang XN (2008) A rabbit model of hormone-induced early avascular necrosis of the femoral head. Biomed Environ Sci 21(5):398–403. doi:S0895-3988(08)60060-4[pii]10.1016/S0895-3988(08)60060-4
Wang Y, Yin L, Li Y, Liu P, Cui Q (2008) Preventive effects of puerarin on alcohol-induced osteonecrosis. Clin Orthop Relat Res 466(5):1059–1067. doi:10.1007/s11999-008-0178-7
Chryssanthou C (1981) Animal model of human disease: Dysbaric osteonecrosis. Am J Pathol 103(2):334–336
Lehner CE, Adams WM, Dubielzig RR, Palta M, Lanphier EH (1997) Dysbaric osteonecrosis in divers and caisson workers. An animal model. Clin Orthop Relat Res (344):320–332
Shabat S, Nyska A, Long PH, Goelman G, Abramovitch R, Ezov N, Levin-Harrus T, Peddada S, Redlich M, Yedgar S, Nyska M (2004) Osteonecrosis in a chemically induced rat model of human hemolytic disorders associated with thrombosis–a new model for avascular necrosis of bone. Calcif Tissue Int 74(3):220–228. doi:10.1007/s00223-003-0068-7
Kuroda Y, Akiyama H, Kawanabe K, Tabata Y, Nakamura T Treatment of experimental osteonecrosis of the hip in adult rabbits with a single local injection of recombinant human fgf-2 microspheres. J Bone Miner Metab. doi:10.1007/s00774-010-0172-5
Plenk H, Jr., Gstettner M, Grossschmidt K, Breitenseher M, Urban M, Hofmann S (2001) Magnetic resonance imaging and histology of repair in femoral head osteonecrosis. Clin Orthop Relat Res (386):42–53
Kim HK (2007) Introduction to osteonecrosis of the femoral head (ofh) and osteonecrosis of the jaw (onj). J Musculoskelet Neuronal Interact 7(4):350–353
Author information
Authors and Affiliations
Corresponding authors
Additional information
The authors Meng Fan and Jiang Peng are contributed equally to this work.
Rights and permissions
About this article
Cite this article
Fan, M., Peng, J., Qin, L. et al. Experimental animal models of osteonecrosis. Rheumatol Int 31, 983–994 (2011). https://doi.org/10.1007/s00296-011-1819-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-011-1819-9