Abstract
Recent researches suggest that imbalance in apoptotic process may lead to susceptibility to systemic lupus erythematosus (SLE). Production of pro-inflammatory cytokines, such as IL-18, has important role in autoimmune process in lupus. There are cumulative data on the pro-apoptotic role of IL-18, in the Fas-mediated apoptosis. Soluble Fas (Apo/1-CD95) is a marker of apoptosis that appears to increase in serum of SLE patients. Previous studies demonstrated increasing serum concentrations of soluble Fas (sFas) and IL-18 in SLE. To assess the correlation between serum concentrations of sFas and IL-18 in SLE patients, 114 SLE patients were selected randomly at the different stages of disease activity according to SLEDAI2K. IL-18 and sFas serum concentrations were compared in patients and fifty randomly selected healthy volunteers. The correlations of IL-18 and sFas serum concentrations with SLEDAI2K and with each other were evaluated in patients. There were a significant difference between serum concentrations of sFas and IL-18 in the case and control groups (P = 0.001). There was a significant correlation between serum concentrations of sFAS and IL-18 in SLE patients (P < 0.0001, r = 0.411). The elevations of IL-18 and sFas(Apo/1-CD95) serum concentrations in SLE patients are significantly correlated.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
There are cumulative data about the role of impaired apoptosis pathways, in development of autoimmune diseases like SLE [1]. Fas(Apo/1-CD95) and Fas ligand are essential factors in the activated induced cell death, and any dysfunction in this system will lead to a breakdown in peripheral tolerance and induction of an autoimmune phenomenon [2]. Increased serum concentrations of soluble Fas ligand and/or soluble Fas antigen (sFas) are quite often a remarkable peculiarity observed in lupus erythematosus disease [2–4]. With the assumption of suppressive effects of sFas on Fas-mediated apoptosis, it was proposed that sFas helps autoreactive thymocytes escaping the negative selection by bearing transmembrane Fas antigen on their surface. Oligomeric form of sFas may have pro-apoptotic effects and causes cytotoxicity in lymphocyte primary culture and in transformed cells [5–7].
On the other hand, IL-18, a member of the IL-1 family, can induce TNFα production, an effect which links this cytokine to the pathogenesis of several autoimmune diseases [8, 9]. The role of IL-18 in pathogenesis of SLE, its correlation with organ-specific damages like nephropathy and its correlation with disease activity index (SLEDAI) have been shown [10, 11]. The important proposed question is whether a correlation or association between sFAS and IL-18 serum concentration exists. Several lines of evidence for induction of FasL expression and TNFα by IL-18 and its pro-apoptotic role have been provided [12–14]. Dao et al. [15] in their study proposed that “IL-18 might play a potential role in immunoregulation or in inflammation by augmenting the functional activity of FasL on Th1 cells.” Chen et al. [16] showed that the percentage of peripheral blood apoptotic lymphocytes after a 24 h of incubation with recombinant human IL-18 was significantly higher compared to the percentage at time zero of incubation in adult onset still’s disease (AOSD), SLE and healthy participants. There are a few studies reporting the correlation between sFas and IL-18 in hepatic diseases [17, 18] and pulmonary complications in tuberculosis [19]. To explore the existence of the correlation between sFas, an apoptotic marker, and IL-18, a pro-apoptotic cytokine, serum concentration in SLE, this study was designed in a large group of lupus patients in different stages of disease activity.
Materials and methods
Patient and control groups
In this case–control study, 114 SLE patients, who were being followed in the Rheumatic Diseases Research Center in Mashhad University of Medical Sciences, registered from May 2007 to June 2008. These patients were diagnosed according to the American College of Rheumatology criteria [20]. Based on SLE Disease Activity Index (SLEDAI2K) score, these patients were at different stages of disease activity. Possible scores in SLEDAI2K system vary from 0 to 105. We excluded all pregnant or postpartum patients, those with past or concurrent history of malignancy, concurrent infection, smoking or addiction, overlap syndromes, chronic renal failure, history of hepatitis or liver disease. All patients with creatinine level more than 2 mg/dl were excluded [21]. As the control group, 50 healthy matched volunteer were selected. This study was approved by the ethics committee of Mashhad University of Medical Science.
Methods
Briefly, 10 ml sample of venous blood was obtained and used for the following tests; complete blood count, ANA (immuneflorescence), anti dsDNA (ELISA), C3, C4 (nephelometry), C-reactive protein (CRP) (Latex) and ESR (1st hour). A random urine analysis and the measurement of protein and creatinine on a 24 h urine collection were also preformed. An aliquot of serum samples was stored in −70°C for analysis of sFas and IL-18. sFas concentrations were determined using a sAPO-1/FAS BMS245 ELISA kit (Bender MedsystemsTM, Austria) according to the manufacturer's instructions. The overall intra- and interassay coefficients of variation in this study were 4.5 and 3.1%, respectively. IL-18 concentrations were measured with BMS267 ELISA kit (Bender MedsystemsTM, Austria) according to the manufacturer's instructions. The overall intra- and interassay coefficients of variation were 6.5 and 8.1%, respectively.
Statistical analysis
The statistical analysis was performed using the SPSS 11.5 program (SPSS Inc., Chicago, IL, USA). Values are reported as mean ± SD for normally distributed variables and median with inter-quartile range (IQR) for others. To determine not normally distributed variables, we used “Kolomogrove-Smirnov” test, and differences among these groups were determined by “Kruskal–Wallis” test for nonparametric analysis of variance and “Mann–Whitney” test. Baseline demographics and clinical characteristics were compared between groups using “t student test” for continuous and “chi-square test” for categorical variables. Since sFas and IL-18 serum concentrations were not normally distributed, the correlation coefficient was obtained by nonparametric Spearman’s rank correlation test.
Results
Demographics
This study was performed on 164 participants (114 patients and 50 healthy controls). The mean age of patients was 30 ± 9 years (range 13–62). The mean age of controls was 29 ± 7 years (range 20–50). Nine patients and four controls were men. The mean duration of disease among the patients was 4 years. Patients were at different stages of disease activity with or without major organ involvements. The mean SLEDAI2K score for the patients was 11.97 ± 10.07.
sFas
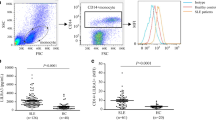
The median (IQR) sFas serum concentrations in patients was 245.00 (158.75–470.00)pg/ml and in controls was 141.50 (119.50–200.00)pg/ml. We found a significant difference between the sFas serum concentrations in these two groups (P = 0.001) (Fig. 1). There was a significant correlation between sFas serum concentrations and SLEDAI score, (P = 0.001 and r = 0.494). The cut-off point for sFas serum concentrations in patients and controls in this study was 87.5 pg/ml.
IL-18
The median (IQR) IL-18 serum concentration in the controls was 75.50 (64.25–115.00)pg/ml and in the patients was 445.50 (120.50–652.25)pg/ml. There was a significant difference between these two groups (P = 0.001) (Fig. 1). The correlation coefficient between serum concentration of IL-18 and SLEDAI score was (P = 0.05 and r = 0.17). The cut-off point for IL-18 serum concentrations in patients and controls in this study was 21.5 pg/ml.
sFas, IL-18 and other laboratory parameters
Table 1 shows the statistical difference between sFas and IL-18 concentrations in patients with normal and abnormal quantitative laboratory parameters. It also shows the correlation between the median levels of sFas, IL-18 and the ESR 1st hour, C3, C4 and anti-dsDNA. There was a significant difference between sFas serum levels in 63% of SLE patients with negative and 37% with positive CRP tests (P = 0.027), but we could not find statistical difference between IL-18 serum levels in these groups (P = 0.2).
sFas, IL-18 and drug history
Among 114 patients, 82.5% were treated with prednisolone and 41% were under immunosuppressive therapy. The difference between sFas concentrations (P = 0.16) and IL-18 concentrations (P = 0.6) in patients who were taking prednisolone was not significant. Treatment with cytotoxic drugs did not make any significant difference on sFas serum concentrations (P = 0.8); on the other hand, the IL-18 serum levels were significantly different (P = 0.03).
Correlation between sFas and IL-18 serum concentrations
This study showed a significant positive correlation between sFas and IL-18 in serum of all patient and control groups (P = 0.0001 r = 0.4). This correlation was also significant in patients (P = 0.005 r = 0.26) (Fig. 2). We determined the cut-off points for IL-18 and sFas serum levels in patients and controls. IL-18 concentrations were not significantly different (P = 0.15) in above and below sFas cut-off point groups (87.5 pg/ml). When we divided the patients into above and below cut-off point groups based on IL-18 levels (21.5 pg/ml), the concentrations of sFas showed significant difference (P = 0.018).
Discussion
The main result of this study is finding a significant positive correlation between serum concentrations of sFas, an apoptotic marker, and IL-18 an important pro-inflammatory and pro-apoptotic cytokine in lupus patients. We could also find a positive correlation between sFas and IL-18 serum levels with SLEDAI2K. The role of sFas-mediated apoptosis in immunity, SLE and elimination of autoreactive lymphocytes is clear [5–7].
On the other hand, it is obvious that IL-18 has a critical role in lupus [8–11]. More recent studies showed the pro-apoptotic role of IL-18 through Fas/Fas ligand pathway [12, 13, 15]. Our results supported the earlier studies that revealed significant increase in serum levels of IL-18 [8–11] or sFas [5–7, 22] in lupus patients in comparison with controls; however, there are still controversies on this issue, Sahin M et al. [2] reported decreased serum levels of sFas in lupus patients; however, they have also referred to other studies reporting normal or high levels of sFas in lupus patients. These controversies may be due to sampling sizes or inclusion criteria for patients and the stages of disease activities. We found a positive correlation between sFas, IL-18 and disease activity according to SLEDAI2K. These results were in line with several previous studies [6, 10, 11, 20, 22, 23]. This finding supports the results of Chen DY and coworkers study; in which, the effect of IL-18 on the apoptosis of peripheral blood lymphocytes through up-regulation of FasL and p53 transcripts was shown. In their study, significantly higher percentage of spontaneous apoptotic lymphocytes were observed in patients with active untreated Adult Onset Still’s Disease and SLE. They also showed increasing amounts of activation induced lymphocyte death by incubation of these cells with recombinant human IL-18. They found that the percentage of both groups of apoptotic lymphocytes and serum IL-18 levels correlates positively with SLEDAI [16]. In our study, among the measured laboratory parameters, only ESR 1st hour correlated with IL-18 and sFas serum levels. This finding supports the importance of IL-18 and sFas in active inflammation in lupus pathogenesis.
In another study, the researchers found a correlation between IL-18 and sFas and interferon gamma levels in pulmonary tuberculosis and concluded that this correlation could be a pathognomonic marker suggesting pulmonary tuberculosis particularly in complicated cases [19]. Hashimoto W et al. [24] in their study concluded that the IL-18 antitumor effects are exerted by FasL-induced cross-linking of Fas and subsequent tumor apoptosis. Marı′n-Serrano and coworkers reported the positive correlation between sFas and IL-18 in patients with chronic hepatitis C infection. They suggested that in response to therapy, IL-18 concentrations and sFas serum levels return to normal [17]. In another study, the association between sFas and IL-18 with severity of multiple organ dysfunctions in sepsis was established, and both of these markers had higher levels in poor outcome patients [25]. Marino et al. [26] in their study showed that the pro-apoptotic role of IL-18 on liver endothelial cells is not related to Fas-mediated apoptosis, and the cell death is mediated via TNFRI. Nakae H et al. [18] showed the raising serum levels of IL-18 and sFas in patients with postoperative hepatic failure. They suggested that IL-18 has both pro-apoptotic and anti-apoptotic effects. It is also known that sFas may be increased in liver injuries, renal failure, sepsis and malignancies. In the current study, we excluded all patients with these conditions. Therefore, it seems that the correlation between sFas and IL-18 in a large number of lupus patients in the current study solely is due to an autoimmune process.
We could not establish any correlation between sFas and IL-18 levels and medications. This can be explained by inactive disease state in some patients who were taking maintenance immunomodulatory drugs due to major organ involvement. These results support Sahin et al. [2] study that reports no significant difference between serum sFas levels in patients on glucocorticoid or immunomodulatory therapies in different autoimmune diseases and the patients who were not treated with these drugs. In other words, these drugs may reduce serum levels of sFas and IL-18 via apoptosis and cytokine release modulation before decreasing the disease activity. Designing a follow-up study may further reveal the role of sFas and IL-18 serum levels as independent markers in determination of disease activity.
In summary, we demonstrated that sFas and IL-18 serum levels are higher in lupus patients comparing with matched normal individuals. We also showed the existence of a positive correlation of sFas and IL-18 serum levels with disease activity and ESR. The association of sFas and IL-18 should be evaluated in future studies. This will provide a better understanding of disease pathogenesis.
References
Munoz LE, van Bavel C, Franz S, Berden J, Herrmann M, van der Vlag J (2008) Apoptosis in the pathogenesis of systemic lupus erythematosus. Lupus 17:371–375
Sahin M, Aydıntug O, Tunc SE, Tutkak H, Nazıroğlu M (2007) Serum soluble Fas levels in patients with autoimmune rheumatic diseases. Clin Biochem 40:6–10
Nozawa K, Kayagaki N, Tokano Y, Yagita H, Okumura K, Hasimoto H (1997) Soluble Fas (APO-1, CD95) and soluble Fas ligand in rheumatic diseases. Arthritis Rheum 40:1126–1129
Hao JH, Ye DQ, Zhang GQ, Liu HH, Dai H, Huang F, Pan FM, Su H, Dong MX, Chen H, Wang Q, Zhang XJ (2006) Elevated levels of serum soluble Fas are associated with organ and tissue damage in systemic lupus erythematosus among Chinese. Arch Dermatol Res 297(7):329–332
Alecu M, Coman G, Alecu S (2000–2001) Serological levels of apoptotic bodies, sFAS and TNF in lupus erythematosus. Rom J Intern Med 38–39:83–88
Courteny PA, Crockard AD, Williamson K, McConnell J, Kennedy RJ, Bell AL (1999) Lymphocyte apoptosis in systemic lupus erythematosus, relationship with Fas expression, serum soluble FAS and diease activity. Lupus 8:508–513
Silvestris F, Grinello D, Tucci M, Cafforio P, Dammacco F (2003) Enhancement of T cell apoptosis correlates with increased serum levels of soluble Fas (CD95/Apo-1) in active lupus. Lupus 12:8–14
Carroll HP, Paunovic V, Gadina M (2008) Crossed signals: the role of interlukin-15 and -18 in autoimmunity. Rheumatology 47:1269–1277
Boraschi D, Dinarello CA (2006) IL-18 in autoimmunity: review. Eur Cytokine Netw 17(4):224–252
Calvani N, Richards HB, Tucci M, Pannarale G, Silvester F (2004) Upregulation of IL-18 and predominance of Th1 immune response is a hallmark of lupus nephritis. Clin Xp Immunol 138:171–178
Park MC, Park YB, Lee SK (2004) Elevated interlukin- 18 levels correlated with disease activity in systemic lupus erythematosus. Clin Rheumatol 23:225–229
Ohtsuki T, Micallef MJ, Kohno K, Tanimoto T, Ikeda M, Kurimoto M (1997) Interleukin 18 enhances Fas ligand expression and induces apoptosis in Fas-expressing human myelomonocytic KG-1 cells. Anticancer Res 17:3253–3258
Kitaura H, Tatamiya M, Nagata N, Fujimura Y, Eguchi T, Yoshida N, Nakayama K (2006) IL-18 induces apoptosis of adherent bone marrow cells in TNF- α mediated osteoclast formation in synergy with IL-12. Immunol Lett 107:22–31
Reddy P (2004) Interleukin-18: recent advances. Curr Opin Hematol 11:405–410
Dao T, Ohashi K, Kayano T, Kurimoto M, Okamura H (1996) Interferon-gamma-inducing factor, a novel cytokine, enhances Fas ligand-mediated cytotoxicity of murine T helper 1 cells. Cell Immunol 173:230–235
Chen DY, Hsieh TY, Hsieh CW, Lin FJ, Lan JN (2007) Increased apoptosis of peripheral blood lymphocytes and its association with interleukin-18 in patients with active untreated adult-onset still’s disease. Arthritis Rheum (Arthritis Care Res) 57:1530–1538
Marín-Serrano E, Rodríguez-Ramos C, Díaz F, Martín-Herrera L, Girón-González JA (2006) Modulation of the anti-inflammatory interleukin 10 and of proapoptotic IL-18 in patients with chronic hepatitis C treated with interferon alpha and ribavirin. J Viral Hepat. 13:230–234
Nakae H, Zheng YJ, Wada H, Tajimi K, Endo S (2003) Involvement of IL-18 and soluble fas in patients with postoperative hepatic failure. Eur Surg Res 35:61–66
El-Masry S, Lotfy M, Nasif WA, El-Kady IM, Al-Badrawy M (2007) Elevated serum level of interleukin (IL)-18, interferon (IFN)-gamma and soluble Fas in patients with pulmonary complications in tuberculosis. Acta Microbiol Immunol Hung 54:65–77
Hochberg MC (1997) Updating the American College of Rheumatology revised criteria for the classification of systemic lupus erythematosus [letter]. Arthritis Rheum 40:1725
Dalboni MA, Sardenberg C, Andreoli MC, Watanabe R, Canziani ME, Santos BF, Liangos O, Jaber BL, Draibe S, Cendoroglo M (2003) Soluble FAS a novel marker of inflammation in uremia. Artif Organs 27:678–691
Sahebari M, hatef, Rezaiyeyazdi Z, Abbasi M, Abbasi B, Mahmoudi M (2010) Correlation between serum levels of soluble Fas (CD95/Apo-1) with disease activity in systemic lupus erythematosus patients in khorasan. Iran. Arch Iran Med 13:135–142
Tinazzi E, Puccetti A, Gerli R, Rigo A, Migliorini P, Simeoni S, Beri R, Dolcino M, Martinelli N, Corrocher R, Lunardi C (2009) Serum DNase I, soluble Fas/FasL levels and cell surface Fas expression in patients with SLE: a possible explanation for the lack of efficacy of hrDNase I treatment. Int Immunol. doi:10.1093/intimm/dxn142
Hashimoto W, Osaki T, Okamura H, Robbins PD, Kurimoto M, Nagata S, Lotze MT, Tahara H (1999) Differential anti tumor effects of administration of recombinant IL-18 or recombinant IL-12 are mediated primarily by Fas-Fas ligand- and perforin-induced tumor apoptosis, respectively. J Immunol 163:583–589
Satoko I, Nobuhiro S, Yoshihiro I, Shigeatsu E (2005) A study of interleukin 18 and sFas in septic multiple organ dysfunction syndrome. J Iwate Med A 5:497–503
Mariño E, Cardier JE (2003) Differential effect of IL-18 on endothelial cell apoptosis mediated by TNF-a and Fas (CD95). Cytokine 22:142–148
Acknowledgment
This research was financially supported by a grant provided by the Chancellor for Research of Mashhad University of Medical Science, Mashhad, Iran. We are grateful to all patients & healthy volunteers for their kind participation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sahebari, M., Rezaieyazdi, Z., Nakhjavani, M.J. et al. Correlation between serum concentrations of soluble Fas (CD95/Apo-1) and IL-18 in patients with systemic lupus erythematosus. Rheumatol Int 32, 601–606 (2012). https://doi.org/10.1007/s00296-010-1633-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-010-1633-9