Abstract
CD147 expressed by monocytes, macrophages, and synoviocytes cells can stimulate the production of matrix metalloproteinases (MMPs) associated with the development of rheumatoid arthritis (RA). We investigated the effects of Sinomenine (SIN) on invasion and migration ability and gene expression of CD147, MMP-2, MMP-9 of fibroblast-like synoviocytes cells (FLS) co-cultured with activated human monocytic THP-1 cells (A-THP-1) in vitro. SIN is a pure alkaloid extracted from the Chinese medical plant Sinomenium acutum. FLS cells were co-cultured with THP-1 cells which were induced to differentiate into macrophages with phorbol 12-myristate 13-acetate (PMA). Cells were treated with different concentrations of SIN. Invasion and migration ability of cells was tested by transwell assays. Western blot analysis and zymographic analysis were adopted to detect the expression of CD147 and MMPs, respectively. RT–PCR was used to determine the expression of mRNA of CD147, MMP-2, and MMP-9. The invasion and migration ability of the co-cultured cells was significantly inhibited by SIN in a concentration-dependent fashion, and at the same time, the levels of CD147, MMP-2, MMP-9 were markedly down-regulated. This inhibitory effect was most notable at concentrations of 0.25 and 1.00 mM (P < 0.01). Our results point to a possible mechanism of SIN on treatment of RA is the inhibitory effect of SIN on cell invasion and migration ability, which strongly correlates with repressing the expression of CD147, MMP-2, and MMP-9.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Sinomenine(SIN,7,8-didehydro-4-hydroxy-3,7-dimethoxy-17-methylmorphinan-6-one, C19H23NO4) (Fig. 1) is a bioactive alkaloid derived from the Chinese medicinal plant, Sinomenium acutum Rehder & E.H. Wilson (Family Menispermaceae). Chinese and Japanese doctors have utilized this plant to treat rheumatic and arthritic diseases for over 1000 years. Clinical trials completed in China demonstrated that the pure alkaloid Sinomenine had significant therapeutic effect for the patients who suffered from rheumatoid arthritis [1, 2]. Previous pharmacological studies showed that Sinomenine had a wide range of actions including anti-inflammation, immunosuppression, arthritis amelioration, and protection against hepatitis induced by lipid polysaccharides [3].
Rheumatoid arthritis (RA) is a complex chronic inflammatory disease dependent on multiple interacting environmental and genetic factors, characterized by chronic inflammation of the synovium in joint cavities [4]. This inflammation is characterized by the presence of macrophages, lymphocytes, and fibroblast-like synoviocytes cells (FLS), which leads to enhanced migration and invasion of peripheral macrophages and FLS cells, contribute to the progressive destruction of articular cartilage, ligament, and bone. Therefore, the regulation of cell migration and invasion is a critical process throughout the development of RA.
The number of FLS cells and macrophages in the joint greatly increases in both the lining and sublining areas of RA synovium, produce various cell factors and matrix metalloproteinases (MMPs), infiltrate into neighboring tissue, cause persistent inflammation, and lead to joint destruction [5, 6]. Cartilage destruction is due to proteolysis by MMPs in remodeling of the extracellular matrix. Gelatinase A (also called matrix metalloproteinase-2, MMP-2) and Gelatinase B (also called matrix metalloproteinase-9, MMP-9) are critical for the progression of RA [7].
The degree of MMPs increases well correlates with extracellular matrix metalloproteinase inducer (EMMPRIN, CD147), which is enriched on the surface of macrophages, and is associated with differentiation of human monocytic THP-1 cells when treated with phorbol 12-myristate 13-acetate (PMA). This protein stimulates the production of MMPs.
Although many in vivo studies have demonstrated that SIN can significantly improve RA [8–11], the molecular mechanism of SIN has not as yet been completely worked out. The purpose of this study was to investigate the effects of SIN on the co-culture system of human FLS cells and A-THP-1 cells and to evaluate its mechanism.
Materials and methods
Reagents
SIN was donated for use by Hunan Zheng Qing Pharmaceutical Co., Ltd (Huaihua zhengqin road NO.288, Hunan Province). Human monocytic THP-1 cells were purchased from the Cell Bank of Peking Union Medical College. All reagents used for cell culture containing penicillin/streptomycin, pyruvate, FCS (fetal calf serum), DMEM, and RPMI 1640 medium were purchased from Gibco BRL (Grand Island, NY). Phorbol 12-myristate 13-acetate (PMA) was purchased from Sigma Chemical Co. (St. Louis, MO). Restriction enzymes and Taq polymerase was obtained from Takara, and all antibodies used in western blot assay were purchased from the Santa cruz (CA, USA).
Cells culture and stimulation
Rheumatoid synoviocytes were isolated from knee at the time of total joint replacement surgery in patients with rheumatoid arthritis. All patients fulfilled the 1987 American College of Rheumatology revised criteria for rheumatoid arthritis. Synovia membranes were minced and digested with a mixture of 1 mg/ml collagenase in serum-free DMEM overnight at 37°C in 5% CO2. After centrifugation and washing, the cells were resuspended in DMEM supplemented with 10% fetal bovine serum, 100 U/ml penicillin, and 100 U/ml streptomycin. Non-adherent cells were removed. Adherent cells were cultured in complete medium, trypsinized with trypsin/EDTA at confluence, and plated in culture flask. To obtain a homogeneous population of synoviocytes, confluent cultures from passages 3–7 were used.
Human monocytic THP-1 cells were cultured in RPMI 1640 medium supplemented with 10% heat-inactivated fetal bovine serum, containing 2 mM, l-glutamine, 5 mM sodium pyruvate, and antibiotics (100 U/ml penicillin, 100 U/ml streptomycin) in culture flasks and were maintained at 37°C in a humidified 5% CO2 atmosphere. Experiments were routinely carried out using cells in the log phase of growth. PMA was dissolved in DMSO to obtain a 1 mM stock solution and was further diluted with PBS before use. For all experiments, THP-1 cells were cultured at an initial density of 5 × 105 cells/ml and treated with PMA at a final concentration of 50 μg/l for 24 h [12]. FLS cells and A-THP-1 cells were co-cultured at a ratio of 1:1 of a suitable density and left to recover and adhere for 24 h [13]. The media was replaced by 0.1-ml DMEM with the addition of SIN (0, 0.01, 0.05, 0.25, 1.00 mM) incubated for 48 h at 37°C, 5% CO2.
Experimental grouping is as follows:
-
Group 1: co-cultured cells treated by 1.00 mM SIN;
-
Group 2: co-cultured cells treated by 0.25 mM SIN;
-
Group 3: co-cultured cells treated by 0.05 mM SIN;
-
Group 4: co-cultured cells treated by 0.01 mM SIN;
-
Group 5: Control (co-cultured cells not treated with SIN;
-
Group 6: A-THP-1 cells not treated with SIN;
-
Group 7: FLS cells not treated with SIN.
In vitro cell invasion and migration assays
In vitro cell invasion assay, which was determined in the ECM-based assay as described previously [13], performed in transwell plates (Millipore) with 10 mm diameter, 8-μm pore polycarbonate filters. The upper and lower compartment of the transwells were separated by the filter coated with 25 μg of matrigel (Peking University Health Science Center), which formed a reconstituted basement membrane at 37°C. Cells (5 × 105 cells in 100 μl DMEM), after treatment with SIN (0, 0.01, 0.05, 0.25, 1.00 mM) for 48 h, were seeded into the upper well of the chamber, while the lower well was filled up to the top (500 μl) with DMEM with 10% FCS as a chemoattractant [14]. After incubation for 24 h at 37°C in the presence of 5% CO2, the cells were fixed for 30 min in 4% formaldehyde and stained for 15 min with crystal violet. The non-migrating cells were then carefully removed from the upper surface (inside) of the transwell with a wet cotton swab. Cells that had migrated or invaded to the bottom surface of the filter were counted. Six evenly spaced fields of cells were counted in each well, using an inverted phase-contrast microscope.
There was no matrigel precoated on membranes of the upper surface in in vitro migration assays. The other conditions were all the same as the invasion assays.
Isolation of total RNA and RT–PCR
RNA extraction from treated cells and cDNA synthesis was conducted as described. Primers were designed according to published sequences [13, 15]. The PCR products were visualized by electrophoresis in 1.5% agarose gel stained with 0.2 μg/ml ethidium bromide. The intensities of the each band were normalized relative to the internal control gene GAPDH. Images of the RT–PCR ethidium bromide-stained agarose gels were acquired with a digital Kodak camera (Eastman Kodak Company, Rochester, NY, USA). Quantification of the bands was analyzed by imaging analysis software from Kodak (Table 1).
Western blot analysis for CD147 expression
Protein concentrations were measured by Bradford protein assay. Protein samples (20 lg) were separated by 10% SDS–PAGE and transferred onto PVDF membranes (Millipore, MA). Non-specific reactivity was blocked by 5% non-fat dry milk in TBST (10 mM Tris–HCl, 150 mM NaCl, 0.05% Tween 20, pH 7.5) for 1 h at room temperature, followed by probing with primary antibodies for rabbit anti-human-EMMPRIN diluted to 1: 1000 (Santa Cruz, CA, USA) and then by goat anti-rabbit HRP-conjugated secondary antibody (Santa Cruz, CA, USA) at 1:3,000 dilution. The reactions were visualized with ECL detection system (Applygen, Peking). Anti-b-actin antibody at 1: 10000 dilution (Santa Cruz, CA, USA) was used to ensure equal loading of each sample. Densitometric analysis was again performed by using the Quantity One (Bio-Rad) to scan the signals [16, 17].
Zymographic analysis
Cells were harvested at the exponential growth phase, the supernatants were collected. Gelatinolytic activities were carried out in 7.5% SDS–PAGE containing 0.1% gelatin type I. Without prior boiling, 20 μl of samples mixed with 10 μl of loading buffer were run under non-reducing conditions. Then, gels were washed two times with 2.5% Triton X-100 to remove SDS and allow proteins to renature and were then immersed in buffer (50 mM Tris, pH 7.5, 5 mM CaCl2, 1 μmol/l ZnCl2, and 0.01% NaN3) for 18 h at 37°C. Gels were stained with 0.2% Coomassie (0.25% brilliant blue, 40% methanol, 7.5% acetic acid) for 4 h at room temperature followed by treatment with destaining buffer (30% methanol, 10% acetic acid) until the desired contrast was achieved. A clear white band showing proteolytic activity was detected against a blue background of undigested gelatin. Gels were documented using an Epi ChemII darkroom (UVP Inc., Upland, CA) documentation system, and the intensity of the bands was quantified by imaging analysis software from Kodak [18].
Statistical analysis
Data were expressed as means ±SD. With the use of the SPSS 10.0 software, a comparison of the difference of means was done through the one-way ANOVA. Statistical significance was defined as P < 0.05. All experiments were performed at least three times.
Results
Inhibition of invasion and migration ability by SIN in FLS and A-THP-1 cells co-culture system in vitro
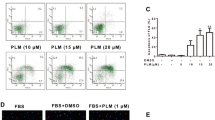
Cell invasion through the matrigel basement membrane in the cell invasion assay and cell migration directly through the membrane in the cell migration assay were analyzed in a modified transwell, as described in Section “Materials and methods.” Cells that invaded to the lower surface of the membrane in these assays were fixed and stained (Fig. 2). The percentage of migration and invasion of co-cultured cells was significantly lower when the cells were incubated with SIN for 24 h.
Cell migration and invasion assay in SIN-(0, 0.01, 0.05, 0.25, 1.00 mM) treated FLS and A-THP-1 cells co-culture system. Cells (5 × 105 cells/ml) were treated with various concentrations of SIN for 48 h: (1) SIN 1.00 mM, (2) SIN 0.25 mM, (3) SIN 0.05 mM, (4) SIN 0.01 mM, (5) Control, (6) A-THP-1 cells, (7) FLS cells. Mean cell counts from 6 random fields and data represent the mean ± SD of three independent experiments. a P > 0.05 vs. control. b P < 0.05 vs. control. c P < 0.01 vs. control
Effects of SIN on CD147, MMP-2, and MMP-9 gene expressions in FLS and A-THP-1 cells co-culture system in vitro
In order to study the effect of SIN on CD147, MMP-2, and MMP-9 production at the transcriptional level, co-cultured cells were maintained in culture in the presence of SIN for 48 h and the total RNA of cells were isolated and RT–PCR was performed as described under methods section. As shown in Fig. 3, the levels of CD147, MMP-2, and MMP-9 mRNA were down-regulated efficiently by SIN dose-dependently.
SIN repressed the mRNA expression of CD147, MMP-2, and MMP-9 as tested by RT–PCR. a FLS and A-THP-1 cells co-culture system (5 × 105 cells/ml) was treated with various concentrations of SIN for 48 h, 1 (SIN 1.00 mM), 2 (SIN 0.25 mM), 3 (SIN 0.05 mM), 4 (SIN 0.01 mM), 5 (Control), 6 (A-THP-1 cells), 7 (FLS cells) are representative of the effects of SIN expression on genes CD147, MMP-2, and MMP-9. The data are representative of three independent experiments. b Quantification of RT–PCR data. Values correspond to the mean ± SD of three independent experiments. a P > 0.05 vs. control. b P < 0.05 vs. control. c P < 0.01 vs. control
SIN causes effective down-regulation of CD147 expression in FLS and A-THP-1 cells co-culture system in vitro
FLS cells co-cultured with A-THP-1 cells were treated with various concentrations of SIN for 48 h. SIN-mediated inhibition of CD147 release was dose-dependent with maximal effects being obtained at 0.25 and 1.00 mM (Fig. 4). The data indicated that SIN inhibited CD147 protein level as a result of down-regulated CD147 mRNA level.
a Western blot assay of the effect of SIN on the expression of CD147 in the co-culture system. FLS and A-THP-1 cells (5 × 105 cells/ml) were incubated with SIN for 48 h. Panel 1 (SIN 1.00 mM), 2 (SIN 0.25 mM), 3 (SIN 0.05 mM), 4 (SIN 0.01 mM), 5 (Control), 6 (A-THP-1 cells), 7 (FLS cells) are representative of the effects of SIN on the expression of CD147. b Quantification of western blot assay data. Values correspond to the mean ± SD of three independent experiments. aP > 0.05 vs. control. bP < 0.05 vs. control. cP < 0.01 vs. control
Effects of SIN on levels of MMP-2 and MMP-9 in FLS and A-THP-1 cells co-culture system in vitro
Gelatinolytic activities of MMP-2 and MMP-9 in conditioned media were detected by electrophoresis of soluble protein on a gelatin containing 7.5% polyacrylamide gel. These experiments show that the suppression of enzyme activity of MMP-2 and MMP-9 in the groups treated with SIN was more pronounced when compared with that of the control group (Fig. 5).
Gelatin zymography for the determination of MMP-2 and MMP-9 activities in SIN-treated co-cultured cells. a Co-cultured cells (5 × 105 cells/ml) were treated with various concentrations of SIN (0, 0.01, 0.05, 0.25, 1.00 mM) for 48 h, and activities of MMP-2 and MMP-9 in conditioned media were evaluated by electrophoresis of soluble protein on a gelatin containing 7.5% polyacrylamide gel. 1 (SIN 1.00 mM), 2 (SIN 0.25 mM), 3 (SIN 0.05 mM), 4 (SIN 0.01 mM), 5 (Control), 6 (A-THP-1 cells), 7 (FLS cells). b Areas and relative intensities of gelatin digested bands by MMP-2 and MMP-9 were quantified by densitometry and expressed as relative activity compared to that of the RPMI 1640 control group. Values correspond to the mean ± SD of three independent experiments. a P > 0.05 vs. control. b P < 0.05 vs. control. c P < 0.01 vs. control
Discussion
RA is a chronic autoimmune disease of unknown origin that primarily affects the joints and ultimately leads to their destruction. The involvement of immune cells is a general hallmark of autoimmune-related disorders. In this regard, macrophages and their respective cytokines play a pivotal role in RA. Recently, it has been understood that resident FLS cells also contribute significantly to the perpetuation of disease and that they may even play a role in its initiation. FLS cells constitute a quite unique cell type that distinguishes RA from other inflammatory conditions of the joints. A number of studies have demonstrated that FLS show alterations in morphology and behavior, including molecular changes and in the expression of adhesion molecules as well as matrix-degrading enzymes. These changes appear to reflect a stable activation of RASFs, which occurs independently of continuous exogenous stimulation. As a consequence, RASFs are no longer considered passive bystanders but active players in the complex intercellular network of RA [19].
There are some direct consequences of the activation of RASFs: the up-regulation of CD147, enabling the strong interaction of fibroblasts with the extracellular matrix, which culminates in the destruction of cartilage and bone. The attachment of RASFs to the articular cartilage is the first step of synovial invasion and mediated by the up-regulation of CD147 on the surface of RASFs. CD147 are responsible for the anchoring of fibroblasts to the extracellular matrix of the articular cartilage, namely MMPs.
All these processes have a common underlying mechanism, namely the degradation of extracellular matrix, which is mediated by MMPs [20]. MMPs are a family of Zn2+-containing enzymes that cleave most of the components of extracellular matrix (ECM). Degradation of ECM components by MMPs is critical for cell invasion and metastasis. Since disruption of the basement membrane is a crucial step for RA progression, MMP-2 and MMP-9 have been noted because of their activities to degrade type IV collagen. By cleaving many of the ECM structural proteins, MMPs have been reported to play a role in the migration and invasion of FLS cells and macrophage–monocyte cells through the intima under pathological settings [21].
Regulation of gene expression of most MMPs correlates with CD147 which is one of the factors involved in the production and activation of MMPs [22]. EMMPRIN (also known as CD147, basigin, and tumor cell-derived collagenase stimulatory factor), a member of the immunoglobulin superfamily [23], is initially identified on the surface of cells and shown to stimulate adjacent stromal cells to produce several MMPs. EMMPRIN, belongs to immunoglobulin super family, is a highly glycosylated transmembrane protein with two extracellular domains and a short cytoplasmic domain [24–26].
It was detected that the expression of CD147, MMP-2, and MMP-9 was increased in synovial fluid of patients with RA [27]. And we have previously found that CD147 was expressed in human monocyte-derived macrophages, and the level of CD147 was significantly related with levels of MM-2 and MMP-9. The results of our research suggest that a possible mechanism of the inhibitory effect of SIN on cell invasion and migration ability is repression of the expression of MMP-2 and MMP-9, which strongly correlates with inhibition of CD147 activity. For the close relationship between macrophages and FLS cells, and their pivotal roles in RA, in order to further advance our knowledge of the mechanism of SIN’s effect on RA, through the establishment of A-THP-1 and FLS cells co-culture model in vitro, we investigated the effects of SIN on the invasion and migration abilities of these cells, and the expression of CD147 and MMPs, to provide further experimental basis of the molecular mechanisms of SIN’s effect on RA. Invasion and migration ability of cells was tested by in vitro transwell assays, which was inhibited by SIN particularly at concentrations of 0.05 and 0.25 mM (P < 0.05), 1.00 mM (P < 0.01). The expression of CD147, MMP-2, and MMP-9 mRNA, as measured by RT–PCR, was down-regulated by SIN at concentrations of 0.25 and 1.00 mM (P < 0.05). The protein level of CD147, as tested by western blot, was decreased by SIN at concentrations of 0.05 mM (P < 0.05), 0.25, and 1.00 mM (P < 0.01). The enzyme activity of MMP-2 and MMP-9, as measured by Zymographic analysis, was suppressed by SIN at concentrations of 0.05 mM (P < 0.05), 0.25, and 1.00 mM (P < 0.01). These data demonstrated that SIN can significantly repress the invasion and migration ability of the co-cultured cells in a dose-dependent manner, and this repression is strongly correlated with inhibition of CD147, MMP-2, and MMP-9 activity by SIN.
Taking these data together, our study showed that SIN could repress A-THP-1 and FLS cells expressing MMP-2, MMP-9 through down-regulating the CD147 activity, therefore, the invasion and migration ability of cells was inhibited, this maybe the possible mechanism by which SIN exerts its function in RA.
References
Ke XY, Xiu MX (1986) Treatment of rheumatoid arthritis by sinomenine. Beijing Yixue 3:186–187
Shi PM, Ma ZX, Zhang WZ (1985) History of Chinese medicine. Xien Yi Xue 3:292–293
Liu ZQ, Kelvin C, Zhou H, Jiang ZH, Wong WF (2005) The pharmacokinetics and tissue distribution of sinomenine in rats and its protein binding ability in vitro. Life Sci 77:3197–3209
Noriaki N, Takashi F, Yoshimasa I, Shigeyuki U, Kazuyuki H (2009) Preventive effect of co-administration of water containing magnesium ion on indomethacin induced lesions of gastric mucosa in adjuvant-induced arthritis rat. Biol Pharm Bull 32:116–120
Li XJ, Patrick YK, Ha WY, Daisy YL, Mandy MY, Wang PX (2006) Effect of sinomenine on gene expression of the IL-1β-activated human synovial sarcoma. Life Sci 79:665–673
Yamasaki H (1976) Pharmacology of sinomenine, an anti-rheumatic alkaloid from Sinomenium acutum. Acta Med Okayama 30:1–20
Li F, Li XF, Hu XF (2005) The serum matrix metalloproteinase- 9 level and it′s significance in rheumatoid arthritis. Chin J Rheumatol 9:9–11
Eric EG, Thanh HX, Alain M, Suzanne M (2005) EMMPRIN/CD147, an MMP modulator in cancer, development and tissue repair. Biochimie 87:361–368
Liu JH, Li WD, Teng HL, Lin ZB (2005) Immunopharmacological action of sinomenine, an alkaloid isolated from Sinomenium acutum, and its mechanism of action in treating rheumatoid arthritis. Acta Pharmaceu Sin 40:127–131
Liu L, Buchner E, Beitze D, Schmidt CB, Kaever V, Emmrich F (1996) Amelioration of rat experimental arthritides by treatment with the alkaloid sinomenine. Int Immunopharmacol 18:529–543
Kok TW, Yue PY, Mak NK, Fan TP, Liu L, Wong RN (2005) The anti-angiogenic effect of sinomenine. Angiogenesis 8:3–12
Wu ZB, Zhu P, Lu N, Shi ZG, Fan CM, Wang YH (2005) Enhanced production of MMP-2, MMP-9 by fibroblast cells from rheumatoid arthritis patients when co-cultured with monocytes of high CD147 expression. Chin J Rheumatol 5:26–27
Ou YQ, Chen LH, Li XJ, Lin ZB (2009) Sinomenine influences invasion and migration ability by inhibiting the expression of MMP-2, MMP-9, CD147 in activated human monocytic THP-1 cells. Acta Pharmacol Sin 30:435–441
Tae H, Kim KW, Suh SJ, Kwak CG, Kima JK, Kimb CH (2007) Inhibitory effect of Uncaria sinensis on human aortic smooth muscle cell migration is based on matrix metalloproteinase-9 inhibitory. Environ Toxicol Phar 24:218–222
Jin MH, Yang JH, Lee E, Lu Y, Kwon S, Son KH, Son JK, Chang HW (2009) Antiasthmatic activity of luteolin-7-O-glucoside from Ailanthus altissima through the downregulation of T helper 2 cytokine expression and inhibition of prostaglandin E2 production in an ovalbumin-induced asthma model. Biol Pharm Bull 32:1500–1503
Kuang YH, Chen X, Su J, Wu LS, Liao LQ, Li D, Chen ZS, Takuro K (2008) RNA interference targeting the CD147 induces apoptosis of multi-drug resistant cancer cells related to XIAP depletion. Cancer letter 10:10–16
Sun X, Zhang XD, Hu H, Lu Y, Chen J, Yasuda K, Wang H (2009) Berberine inhibits hepatic stellate cell proliferation and prevents experimental liver fibrosis. Biol Pharm Bull 32:1533–1537
Kataoka H, DeCastro R, Zucker S, Biswas C (1993) Tumor cell-derived collagenase -stimulatory factor increases expression of interstitial collagenase, stromelysin, and 72-kDa gelatinase. Cancer Res 53:3154–3158
Huber LC, Distler O, Tarner I, Gay RE, Gay S, Pap T (2006) Synovial fibroblasts: key players in rheumatoid arthritis. Rheumatology 45:669–675
Pap T, Gay S, Schett G (2002) Matrix metalloproteinases. In: Smolen J, Lipsky J, Dunitz M (eds)Targeted therapies in rheumatology, pp 483–497
Amorino GP, Hoover RL (1998) Interactions of monocytic cells with human endothelial cells stimulate monocytic metalloproteinase production. Am J Pathol 152:199–207
Guo H, Zucker S, Gordon MK, Toole BP, Biswas C (1997) Stimulation of matrix metalloproteinase production by recombinant extracellular matrix metalloproteinase inducer from transfected Chinese hamster ovary cells. J Biol Chem 272:24–27
Sun J, Hemler ME (2001) Regulation of MMP-1 and MMP-2 production through CD147/extracellular matrix metalloproteinase inducer interactions. Cancer Res 61:2276–2281
Biswas C, Zhang Y, DeCastro R, Guo H, Nakamura T, Kataoka H, Nabeshima K (1995) The human tumor cell-derived collagenase stimulatory factor (renamed EMMPRIN) is a member of the immunoglobulin superfamily. Cancer Res 55:434–439
Guo H, Majmudar G, Jensen TC, Biswas C, Toole BP, Gordon MK (1998) Characterization of the gene for human EMMPRIN, a tumor cell surface inducer of matrix metalloproteinases. Gene 220:99–108
Liang L, Terry M, Thomas B (2002) Characterization of the promoter of human extracellular matrix metalloproteinase inducer (EMMPRIN). Gene 282:75–86
Dong WJ, Zhu P, Fan CM, Wang YH, Xiao LB (2004) Expression of CD147 and matrix metalloproteinases in rheumatoid synovium. Chin J Rheumatol 8:135–138
Acknowledgments
The authors are very grateful to Dr. Michael A. McNutt and Dr. xiaoling-ZHU for revising this paper.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ou, Y., Li, W., Li, X. et al. Sinomenine reduces invasion and migration ability in fibroblast-like synoviocytes cells co-cultured with activated human monocytic THP-1 cells by inhibiting the expression of MMP-2, MMP-9, CD147. Rheumatol Int 31, 1479–1485 (2011). https://doi.org/10.1007/s00296-010-1506-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-010-1506-2