Abstract
Although it has been reported that the MHC class I molecule, HLA-B51, is a risk factor for Behçet’s disease (BD), contribution of the tumor necrosis factor (TNF) genes, which are located in the vicinity of the HLA-B locus, to the genetic susceptibility for BD has yet to be elucidated. The purpose of this study was to analyze the effect of TNF-α promoter polymorphisms at positions −308, −238 and −376 on the susceptibility, severity and clinical features of BD. The TNF-α gene sequences from 107 patients with BD and 102 healthy subjects were amplified by the polymerase chain reaction. Sequence analysis of the TNF-α gene locus, which contains promoter polymorphisms at positions −376, −308, and −238, was performed with a DNA sequencing kit on automated sequencer. The patients were classified according to disease severity and clinical features. Serum TNF-α level in the study groups was measured by sandwich enzyme immunoassay. In patients with BD the frequencies of TNF-α −308 (19.4% vs 18.4%), −238 (3.7% vs 5.9%), and −376 (0.9% vs 2.9%) gene polymorphisms were not found to be significantly different from those in healthy subjects. The TNF-α gene polymorphisms did not show any association with disease severity or clinical features. Serum TNF-α level was significantly higher in patients with BD than in healthy controls (3.10±1.45 pg/ml vs 2.43±1.94 pg/ml, P < 0.01). Serum TNF-α level was not found to be significantly associated with disease severity, activity, clinical findings and TNF-α genotypes. The results of this study suggest that the TNF-α gene polymorphisms are unlikely to play an important role in the pathogenesis and severity of BD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Behçet’s disease (BD) is a multi-systemic inflammatory disorder classified among the vasculitidies. It was first described as a triad of recurrent oral and genital ulcers and uveitis with hypopion. Various other ophthalmic and cutaneous lesions, as well as musculoskeletal, vascular, gastrointestinal, neurological, pulmonary, and cardiac involvement, are other well-known features of BD.
The etiopathogenesis of BD is not clearly established. However, immune dysfunction, characterized by activation in neutrophils and T cells and release of Th1-type proinflammatory cytokines such as tumor necrosis factor-alpha (TNF-α), has been considered as the major pathogenetic factor of the disease [1–6]. The TNF-α produced by activated macrophages and T lymphocytes is a cytokine showing a potent immunomodulator activity [7]. TNF-α expression is induced by bacterial lipopolysaccharide, mitogens, and viruses, and it is regulated both transcriptionally and post-transcriptionally [8, 9]. It has been demonstrated that peripheral blood mononuclear cells from patients with BD have increased TNF-α gene expression and synthesis [4–6]). When one considers the arranging effects of TNF-α on acute phase response, vascular adhesion, progenitor differentiation in bone marrow, and apoptosis [10], this cytokine may play a role in the pathogenesis of BD. It is also suggested that TNF-α may be directly responsible from activation of T cells and neutrophils, main pathogenetic changes in BD [2, 3].
Genetic factors can assist in the development of BD with effecting response of inflammatory cells to antigenic stimuli, inflammatory cell functions and release of various cytokines [1–3]. Contribution of the MHC class I molecule HLA-B51 to the genetic susceptibility for BD is well documented [11]; however, it is still unknown whether HLA-B51 directly participates in the pathogenesis of BD or is only associated with it because of linkage disequilibrium with another predisposition gene [12]. Therefore, investigation of other polymorphic loci of the MHC region in BD patients is of interest.
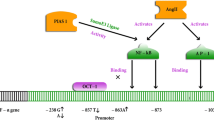
The TNF genes, which are located centromeric to HLA-B in the class III region [13], encode closely related cytokines, which play an important role in the regulation of the immune response as part of the cytokine network [14]. In view of the localization of the TNF genes and the biological properties of these cytokines, it has been postulated that polymorphic TNF genes might play a role in the various HLA-associated diseases [15]. Accordingly, polymorphisms, a G→A substitution at position −308, a G→A substitution at position –238, and a G→A substitution at position −376, have been described in the proximal promoter of the TNF-α gene [16–20]. While there is evidence for transcriptional regulation of TNF-α gene expression [8, 9], these polymorphisms may be important for TNF-α gene expression and protein production. Previous studies have demonstrated a role of TNF gene polymorphisms in MHC-associated diseases such as systemic lupus erythematosus, rheumatoid arthritis, and ankylosing spondylitis [16, 21–23]. Recently, TNF genes attracted research as possible candidates for BD susceptibility. The results of previous studies of the association of the TNF gene polymorphisms with BD are contradictory [24–28]. Therefore, we investigate the association of TNF-α promoter polymorphisms at positions −308, −238 and −376 with susceptibility to BD and clinical features of BD.
Patients and methods
One hundred-seven patients, 65 male and 42 female, fulfilling the International Study Group Criteria for the diagnosis of BD [29], were included in the study. Our patients were adults of Turkish origin living in Turkey. Mean age was 35.0±9.5 years, and median disease duration was 60 months (range 1–276 months) in the patients’ group. One hundred-two healthy blood donors of the same ethnic origin, 61 male and 41 female, were examined as the healthy control group. Mean age was 33.7±8.8 years in control group. The study was approved by the Committee on Medical Ethics of the Ankara University Faculty of Medicine, and written informed consent was obtained from all subjects after an explanation of the purpose of the study.
The detailed clinical characteristics were recorded for each patient. Behçet’s disease with vascular involvement described patients with venous and arterial thromboses and/or aneurysm. The diagnosis of vascular involvement was made on clinical grounds, color Doppler ultrasonography and/or angiography using computed tomographic techniques where appropriate. The patients were classified according to disease severity as mild, moderate or severe [30]. Patients with BD, who had two or more active clinical features related to BD at the time of the study, were considered to have active BD, and patients who had had no symptoms apart from recurrent oral ulcers for at least 1 month prior to the study were considered to have inactive BD.
DNA preparation
Genomic DNA was extracted from EDTA anti-coagulated blood by a conventional salting-out procedure of the cellular proteins, followed by dehydration and precipitation of the DNA by a saturated sodium chloride solution [31]. The DNA was dissolved in water by mixing overnight and stored at −20°C until required.
Polymerase chain reaction
TNF-α gene sequences from all individuals included in this study were amplified by the polymerase chain reaction (PCR). PCR was performed in 50 μl reactions containing 2.5 μl purified genomic DNA, 50 pmol of each primer and 1 U of Taq DNA polymerase. The temperature cycles were 0.5 min at 94°C and 1 min at 56°C for 30 cycles in a thermal cycler (MJR PTC200, USA). An elongation time of 7 min at 68°C was used in the final cycle. Primers used in the PCR reaction were as follows: primer (forward), 5′-TGCCAACAACTGCCTTTA-3′ and primer (reverse), 5′-GAGTCTCCGGGTCAGAATGA-3′ [17]. PCR products, 10 μl, were electrophorized on a 1.5% agarose gel and visualized after ethidium bromide and orange G gel staining under ultraviolet transillumination. The band-amplified 671 bp was searched for and then analyzed. The results were photographed under a red filter with Polaroid film or image editor. Sequence analysis of the TNF-α gene locus that contained promoter polymorphisms at positions −376, −308, and −238 was performed with the 7-Deaza-dGTP Cy5/5.5 Dye Primer Cycle DNA sequencing kit (Visible Genetics, Canada) on a Visible Genetics automated sequencer [22].
Serum TNF-α level was measured by sandwich enzyme immunoassay (QuantikineHS, R&D Systems, Wiesbaden, Germany), sensitive from 0.06 pg/ml to 32 pg/ml.
Statistical analysis
Continuous data are expressed as mean ± SD, and categorical data are expressed as percentages. Comparison of percentages was made with the chi-squared test with Yates’ correction or Fisher’s exact test, as appropriate. A Bonferroni correction was applied for multiple comparisons with all novel associations, with a correction factor derived from the number of alleles tested. Pc indicates where the Bonferroni correction was applied. The associations between TNF-α gene polymorphisms and BD or disease severity indicators are expressed as odds ratio (OR) with 95% confidence intervals (CI). Comparison of means was carried out with the unpaired Student’s t-test. A P<0.05 was considered statistically significant.
Results
The cumulative clinical characteristics of patients with BD are shown in Table 1. Thirty-three patients had vascular involvement. According to the index of Krause et al. 41 patients were classified as having mild disease, 36 patients as moderate, and 30 patients as having severe disease. The disease was active in 57 patients and inactive in 50 patients during the study.
The TNF-α −308, −238, and −376 genotype and allele frequencies in patients with BD and healthy subjects are shown in Table 2. TNF-α −308 G/A heterozygous polymorphism was detected in 21 BD patients (19.6%) and in 16 healthy subjects (15.7%). Two subjects in the control group demonstrated −308 A/A genotype, while no homozygous mutation was observed in patients with BD. The TNF-α −238 G/A polymorphism was present in four patients with BD (3.7%) and in six healthy controls (5.9%). The frequency of TNF-α −376 G/A polymorphism was 0.9% in the patients’ group and 2.9% in the control group. In patients with BD the frequencies of TNF-α −308, −238 and −376 polymorphisms were not found to be significantly different from those in healthy subjects (P>0.05).
The associations between the frequencies of TNF-α −308 and –238 G/A genotypes and clinical findings of BD are shown in Table 3. The TNF-α −308 polymorphism did not show any association with clinical findings. Although the frequency of TNF-α −238 G/A genotype in patients with vascular involvement (9.1%) was higher than that in the patients without vascular involvement (1.4%), the difference was not found to be statistically significant (OR=7.30; 95% CI=0.73–73.0; P>0.05).
The distribution of TNF-α −308 and –238 G/A genotypes in BD patients according to disease severity are shown in Table 4. Although, in patients with severe disease, the frequency of TNF-α −308 G/A genotype was lower, and the frequency of TNF-α −238 G/A genotype was higher, than those of the patients with mild or moderate disease, differences did not reach statistically significant levels (P>0.05).
Serum TNF-α level was significantly higher in patients with BD than in the control group (3.10±1.45 pg/ml vs 2.43±1.94 pg/ml, respectively; P<0.01). Mean serum TNF-α levels were not significantly different among the patients with mild (3.13±1.55 pg/ml), moderate (3.21±1.70 pg/ml), or severe (2.92±0.91 pg/ml) disease (P>0.05). Serum TNF-α level was also found to be similar between the patients with active or inactive disease (3.09±1.37 pg/ml vs 3.11±0.55 pg/ml, respectively; P>0.05). There was no significant difference in serum TNF-α level between the patients with or without vascular involvement (3.07±1.49 pg/ml vs 3.11±1.44 pg/ml, respectively; P>0.05). Serum TNF-α level was not found to be significantly associated with TNF-α genotypes in either patients or control groups (Table 5).
Discussion
Although familial aggregation of BD patients [32] and association of HLA-B51 with BD [11] strongly support the contribution of genetic factors to the pathogenesis of BD, a disease-susceptible gene has not yet been determined. It has long been investigated whether HLA-B51 has a direct role in the pathogenesis, or whether this association reflects linkage disequilibrium with a putative susceptibility gene for BD located close to the HLA-B locus. TNF is encoded in the class III region of the HLA complex, adjacent to HLA-B, implicating it as both a functional and positional candidate gene in the pathogenesis of BD. A number of polymorphisms in the TNF promoter have been identified. However, the role of TNF gene polymorphisms in the pathogenesis of BD has not been researched enough.
In the present study no significant difference was observed in the TNF-α −308 G/A heterozygous polymorphism between BD patients and healthy controls. In other studies in the Turkish population the −308 gene polymorphism was also not found to be significantly associated with BD [25, 26]. Similarly, Verity et al. [24], Ahmad et al. [27] and Lee et al. [28] did not find a significant difference in the TNF-α −308A allele frequency between the BD patients and healthy controls. In the studies examining the association between TNF-β gene polymorphisms and BD [24, 28, 33], the TNF-β1 and β2 allele frequencies in BD patients were not found to be different from the control group, except for the BD patients with ocular involvement [24].
We have not found significant associations between the TNF-α −308 polymorphism and disease severity and clinical parameters, including the vascular and ocular involvement in BD patients. The −308 polymorphism was also not found to be significantly associated with the manifestations or severity of BD in the studies of Duymaz-Tozkir et al. [26] and Lee et al. [28]. These findings suggest that TNF-α −308 gene polymorphism does not have a significant effect on the development and clinical status of BD.
In our study, TNF-α −238 gene heterozygous polymorphism was observed in only four patients with BD (3.7%), and frequency of this polymorphism was not different from that in healthy subjects. Thus, this polymorphism appears to be not responsible for the development of BD in our patient population. Ahmad et al. [27] studied 133 UK white Caucasoid patients with BD and 354 healthy controls, and they found that the frequencies of TNF-α -1031C and −238A alleles were significantly higher in BD patients than in controls. In this study, 18.0% of BD patients had the −238A allele. The reason(s) for the difference in the frequency of −238 gene polymorphism between the present study and the study of Ahmad et al. is not clear; however, the ethnic variability might be responsible for these discordant results. In our study, the frequency of –238 G/A genotype in patients with vascular involvement was higher than that in the patients without vascular involvement; however, the difference did not reach a statistically significant level. Further studies are required to reach a certain conclusion about the association between −238 polymorphism and vascular involvement in BD patients.
The TNF-α −376 polymorphism in BD patients has also been examined in our study, and heterozygous mutation was observed in only one patient. Duymaz-Tozkir et al. [26] also reported that three of 99 patients with BD had a heterozygous mutation on TNF-α gene at position −376.
It has been shown that TNF-α levels are increased in both the peripheral blood mononuclear cell culture supernatants and serum samples from the patients with BD [4–6, 34). We also found a higher serum TNF-α level in BD patients than in healthy subjects. However, serum TNF-α level was not associated with disease activity, severity or clinical features. Our findings suggest that serum TNF-α level may not be a useful marker of disease activity and severity. The reason why a relationship between the serum TNF-α level and disease activity and severity could not be established could be that the serum level of this cytokine does not sufficiently reflect its local tissue concentration. Previous studies have shown an increase in TNF-α gene expression in the peripheral blood mononuclear cells of the patients with active BD [35]. Moreover, clinical remission is achieved following the TNF-α monoclonal antibody therapy in BD patients [36]. As a result, cellular TNF-α synthesis may have key role in the disease pathogenesis and its activity.
TNF-α production displays significant inter-individual variations. These differences can be related to the polymorphisms in the TNF-α gene [17–19]. However, the results regarding the functional role of TNF-α −308 and −238 polymorphisms are contradictory. In vitro studies have shown that the –308 A allele is a more powerful transcriptional activator than the –308G allele [37–39]. Louis et al. [38] and Brinkman et al. [39] found that the peripheral blood mononuclear cells of the individuals having –308 A/A genotype synthesized more TNF-α than the individuals having G/G genotype. However, no significant effect of 308 G/A genotype on TNF-α gene transcription has been observed [39–41]. Allen [42] suggested that TNF-α gene transcription and synthesis are increased in the individuals carrying –308A allele as homozygous. No significant effect of −238 polymorphism on TNF-α gene transcription and synthesis has been observed in previous studies [40, 43].
We did not observe a significant difference in serum TNF-α levels between the individuals having –308 G/A and G/G genotypes in either the patient group or the controls. The serum levels of the cytokines do not sufficiently reflect the synthesis rates and their local concentrations in the tissues. Thus, an increase in cellular TNF-α synthesis caused by the heterozygous –308 G/A polymorphism, which is a less powerful transcriptional activator than that of A/A genotype, would not be reflect the serum TNF-α level. This opinion is supported by the study of Hamzaoui et al. [34], in which they have shown a greater in vitro TNF-α synthesis in the peripheral blood mononuclear cells obtained from the patients with BD than in that of healthy subjects, despite both groups having the same serum TNF-α levels. In our study, serum TNF-α levels were higher in subjects having –238 G/A genotype than in those having –238 G/G genotype, in both the patients and control groups, but the differences were not found to be statistically significant. As the number of the individuals having this mutation is very low, however, it is not possible to make a definite comment.
This study has several limitations. First, its low statistical power can make it difficult to determine small differences between genotype frequencies. Second, we demonstrated that the TNF-α −238A and –376A alleles are rare in the Turkish population, which prevented meaningful analysis with a sample size of 107. Third, we investigated three single nucleotide polymorphic sites. TNF-α has three other promoter polymorphisms (−1031, −863 and −857). Therefore, it will be possible for us to find a difference in genetic polymorphisms at other genetic loci as well as Ahmad et al. [27].
In conclusion, the etiopathogenesis of BD remains unknown. Although the previous studies had provided the role of TNF-α polymorphisms in HLA-accompanying diseases, we did not find any associations between the polymorphisms on the TNF-α gene at −308, −238 and −376 positions and susceptibility to BD and its clinical course in Turkish patients. Considering the pathogenic role of TNF-α cytokine, we suggest that the role of TNF gene polymorphism in the etiopathogenesis of BD is not determined, but it can be functionally explained. However, in order to reach a definite conclusion on this subject, we need to wait for the results of further studies.
References
Lehner T (1999) Immunopathogenesis of Behçet’s disease. Ann Med Interne (Paris) 150:483–487
Gül A (2001) Behçet’s disease: an update on the pathogenesis. Clin Exp Rheumatol 19 [Suppl 24]:S6–S12
Direskeneli H (2001) Behçet’s disease: infectious aetiology, new autoantigens, and HLA-B51. Ann Rheum Dis 60:996–1002
Mege JL, Dilsen N, Sanguedolce V, Gül A, Bongrand P, Roux H, Ocal L, Inanc M, Capo C (1993) Overproduction of monocyte derived tumor necrosis factor α, interleukin (IL) 6, IL-8 and increased neutrophil superoxide generation in Behçet’s disease. A comparative study with familial Mediterranean fever and healthy subjects. J Rheumatol 20:1544–1549
Yamashita N, Kaneoka H, Kaneko S, Takeno M, Oneda K, Koizumi H, Kogure M, Inaba G, Sakane T (1997) Role of γδ T lymphocytes in the development of Behçet’s disease. Clin Exp Immunol 107:241–247
Kaneko S, Suzuki N, Yamashita N, Nagafuchi H, Nakajima T, Wakisaka S, Yamamoto S, Sakane T (1997) Characterization of T cells specific for an epitope of human 60-kD heat shock protein (hsp) in patients with Behçet’s disease (BD) in Japan. Clin Exp Immunol 108:204–212
Beutler B, Cerami A (1989) The biology of cachectin/TNF-α primary mediator of the host response. Annu Rev Immunol 7:625–655
Golfeld AE, Doyle C, Maniatis T (1990) Human tumor necrosis factor α gene regulation by virus and lipopolysaccharide. Proc Natl Acad Sci U S A 87:9769–9773
Han J, Brown T, Beutler B (1990) Endotoxin-responsive sequences control cachectin/tumor necrosis factor biosynthesis at the translational level. J Exp Med 171:465–475
Beutler B (1995) TNF, immunity and inflammatory disease: lessons of the past decade. J Invest Med 43:227–235
Verity DH, Marr JE, Ohno S, Wallace GR, Stanford MR (1999) Behçet’s disease, the silk road and HLA-B51: historical and geographical perspectives. Tissue Antigens 54:213–220
Mizuki N, Ohno S, Sato T, Ishihara M, Miyata S, Nakamura S, Naruse T, Mizuki H, Tsuji K, Inoko H (1995) Microsatellite polymorphism between the tumor necrosis factor and HLA-B genes in Behçet’s disease. Hum Immunol 43:129–135
Campbell RD, Trowsdale J (1993) Map of the human MHC. Immunol Today 14:349–352
Beutler B, Cerami A (1988) Tumor necrosis, cachexia, shock and inflammation: a common mediator. Ann Rev Biochem 57:505–518
Verjans GM, Messer G, Weiss EH, van der Linden SM, Kijlstra A (1992) Polymorphism of the tumor necrosis factor region in relation to disease: an overview. Rheum Dis Clin North Am 18:177–185
Jacob CO, Fronek Z, Lewis GD, Koo M, Hansen JA, McDewitt HO (1990) Heritable major histocompatibility complex class II-associated differences in production of tumor necrosis factor α: relevance to genetic predisposition to systemic lupus erythematosus. Proc Natl Acad Sci U S A 87:1233–1237
Wilson AG, di Giovine FS, Blakemore AI, Duff GW (1992) Single base polymorphism in the human tumour necrosis factor α (TNF-α) gene detectable by NcoI restriction of PCR product. Hum Mol Genet 1:353–359
D’Alfonso S, Richiardi PM (1994) A polymorphic variation in a putative regulation box of the TNFA promoter region. Immunogenetics 39:150–154
Pociot F, Briant L, Jongeneel CV, Molvig J, Worsaae H, Abbal M, Thomsen M, Nerup J, Cambon-Thomsen A (1993) Association of tumor necrosis factor (TNF) and class II major histocompatibility complex alleles with the secretion of TNF-α and TNF-β by human mononuclear cells: a possible link to insulin-dependent diabetes mellitus. Eur J Immunol 23:224–231
Hamann A, Mantzoros C, Vidal-Puig A, Flier JS (1995) Genetic variability in the TNF-α promoter is not associated with type II diabetes mellitus (NIDDM). Biochem Biophys Res Commun 211:833–839
Rood MJ, van Krugten MV, Zanelli E, van der Linden MW, Keijsers V, Schreuder GMT, Verduyn W, Westendorp RG, de Vries RR, Breedveld FC, Verweij CL, Huizinga TW (2000) TNF−308A and HLA-DR3 alleles contribute independently to susceptibility to systemic lupus erythematosus. Arthritis Rheum 43:129–134
Brinkman BMN, Huizinga TWJ, Kurban SS, van der Velde EA, Schreuder GMT, Hazes JMW, Breedveld FC, Verweij CL (1997) Tumour necrosis factor α gene polymorphisms in rheumatoid arthritis: association with susceptibility to, or severity of, disease? Br J Rheumatol 36:516–521
Höhler T, Schaper T, Schneider PM, Meyer zum Buschenfelde KH, Marker-Hermann E (1998) Association of different tumor necrosis factor α promoter alleles frequencies with ankylosing spondylitis in HLA-B27 positive individuals. Arthritis Rheum 41:1489–1492
Verity DH, Wallace GR, Vaughan RW, Kondeatis E, Madanat W, Zureikat H, Fayyad F, Marr JE, Kanawati CA, Stanford MR (1999) HLA and tumour necrosis factor (TNF) polymorphisms in ocular Behçet’s disease. Tissue Antigens 54:264–272
Öz D, Karslı F, Atalay A, Şahin Ş (2000) TNF-alpha gene polymorphisms in Behçet’s disease. In: Bang D, Lee ES, Lee S (eds). Proceedings of the 9th international conference on Behçet’s disease 2000, May 27–29. Design Mecca Publishing, Seoul, pp161–165
Duymaz-Tozkir J, Gül A, Uyar FA, Özbek U, Saruhan-Direskeneli G (2003) Tumour necrosis factor-alpha gene promoter region −308 and –376 G→A polymorphisms in Behçet’s disease. Clin Exp Rheumatol 21:15–18
Ahmad T, Wallace GR, James T, Neville M, Bunce M, Mulcahy-Hawes K, Armuzzi A, Crawshaw J, Fortune F, Walton R, Stanford MR, Welsh KI, Marshall SE, Jewell DP (2003) Mapping the HLA association in Behçet’s disease. A role for tumor necrosis factor polymorphisms? Arthritis Rheum 48:807–813
Lee EB, Kim JY, Lee YJ, Park MH, Song YW (2003) TNF and TNF receptor polymorphisms in Korean Behçet’s disease patients. Hum Immunol 64:614–620
International Study Group for Behçet’s Disease (1990) Criteria for diagnosis of Behçet’s disease. Lancet 335:1078–1080
Krause I, Rosen Y, Kaplan I, Milo G, Guedj D, Molad Y, Weinberger A (1999) Recurrent aphthous stomatitis in Behçet’s disease: clinical features and correlation with systemic disease expression and severity. J Oral Pathol Med 28:193–196
Miller SA, Dykes DD, Polesky HT (1988) A simple salting out procedure for extracting DNA from human nucleated cells. Nucl Acids Res 16:1215
Gül A, İnanç M, Öcal L, Aral O, Koniçe M (2000) Familial aggregation of Behçet’s disease in Turkey. Ann Rheum Dis 59:622–625
Mizuki N, Ohno S, Tanaka H, Sugimura K, Seki T, Mizuki N, Kera J, Inaba G, Tsuji K, Inoko H (1992) Association of HLA-B51 and lack of association of class II alleles with Behçet’s disease. Tissue Antigens 40:22–30
Hamzaoui K, Hamza M, Ayed K (1990) Production of TNF-alpha and IL-1 in active Behçet’s disease. J Rheumatol 17:1428–1429
Yamakawa Y, Sugita Y, Takahashi Y, Yamakawa T, Tanaka S, Nakamura S, Fukushima J, Kawamoto S, Ohno S, Okuda K, et al (1993) Gene expression of tumour necrosis factor-α (TNF-α) and heat-shock protein (HSP) 70 in patients with Behçet’s disease. Arch Dermatol Res 285:505–508
Goossens PH, Verburg RJ, Breedveld FC (2001) Remission of Behçet’s syndrome with tumour necrosis factor α blocking therapy. Ann Rheum Dis 60:637
Wilson AG, Symons JA, McDowell TL, McDevitt HO, Duff GW (1997) Effects of a polymorphism in the human tumour necrosis factor α promoter on transcriptional activation. Proc Natl Acad Sci U S A 94:3195–3199
Louis E, Franchimont D, Piron A, Gevaert Y, Schaaf-Lafontaine N, Roland S, Mahieu P, Malaise M, De Groote D, Louis R, Belaiche J (1998) Tumour necrosis factor (TNF) gene polymorphism influences TNF-α production in lipopolysaccharide (LPS)-stimulated whole blood cell culture in healthy humans. Clin Exp Immunol 113:401–406
Brinkman BMN, Zuijdgeest D, Kaijzel EL, Breedveld FC, Verweij CL (1996) Relevance of the tumor necrosis factor alpha (TNFα) −308 promoter polymorphism in TNF-α gene regulation. J Inflamm 46:32–41
Uglialoro AM, Turbay D, Pesavento PA, Delgado JC, McKenzie FE, Gribben JG, Hartl D, Yunis EJ, Goldfeld AE (1998) Identification of three new single nucleotide polymorphisms in the human tumor necrosis factor-α gene promoter. Tissue Antigens 52:359–367
Skoog T, Van’t Hooft FM, Kallin B, Jovinge S, Boquist S, Nilsson J, Eriksson P, Hamsten A (1999) A common functional polymorphism (C→A substitution at position -863) in the promoter region of the tumour necrosis factor-α (TNF-α) gene associated with reduced circulating levels of TNF-α. Hum Mol Genet 8:1443–1449
Allen RD (1999) Polymorphism of the human TNF-α promoter—random variation or functional diversity? Mol Immunol 36:1017–1027
Pociot F, D’Alfonso S, Compasso S, Scorza R, Richiardi PM (1995) Functional analysis of a new polymorphism in the human TNF alpha gene promoter. Scand J Immunol 42:501–504
Acknowledgments
This study is supported in part by Ankara University Research Foundation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ateş, A., Kinikli, G., Düzgün, N. et al. Lack of association of tumor necrosis factor-alpha gene polymorphisms with disease susceptibility and severity in Behçet’s disease. Rheumatol Int 26, 348–353 (2006). https://doi.org/10.1007/s00296-005-0610-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-005-0610-1