Abstract
Microbial-derived natural products have functional and structural diversity and complexity. For several decades, they have provided the basic foundation for most drugs available to modern medicine. Microbial-derived natural products have wide-ranging applications, especially as chemotherapeutics for various diseases and disorders. By exploring distinct microorganisms in different environments, small novel bioactive molecules with unique functionalities and biological or biomedical significance can be identified. Aquatic environments, such as oceans or seas, are considered to be sources of abundant novel bioactive compounds. Studies on marine microorganisms have revealed that several bioactive compounds extracted from marine algae and invertebrates are eventually generated by their associated bacteria. These findings have prompted intense research interest in discovering novel compounds from marine microorganisms. Natural products derived from Dermacoccus exhibit antibacterial, antitumor, antifungal, antioxidant, antiviral, antiparasitic, and eventually immunosuppressive bioactivities. In this review, we discussed the diversity of secondary metabolites generated by genus Dermacoccus with respect to their chemical structure, biological activity, and origin. This brief review highlights and showcases the pivotal importance of Dermacoccus-derived natural products and sheds light on the potential venues of discovery of new bioactive compounds from marine microorganisms.
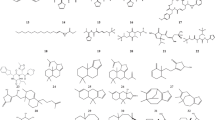
Graphical Abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Marine microbes have a special significance to everyday life. There is a possibility that marine microorganisms could be the closest relatives of initial life forms, as life is believed to have started in the oceans. They are capable of carrying out numerous stages in biochemical sequences that are impossible for other organisms as a result of their metabolic abilities and diversities, and they are also employed for several biochemical uses, such as the production of industrial goods [63, 65, 92]. In specific members of the order Actinomycetales, marine microbes are excellent sources of new metabolites with potential pharmaceutical application [7, 24]. More than 140 actinomycete genera have been reported, and a few of them have been identified to be major sources of known essential compounds [7, 42, 77]. Furthermore, other actinomycetes like Saccharopolyspora, Amycolatopsis, Micromonospora, and Actinoplanes also generate small bioactive metabolic molecules. Actinomycete strains may be present in different habitats: Many are usually present in terrestrial soils, although others have also been isolated from marine sediments and sponges [23, 75]. Actinomycetes provide the foundation for the synthesis of useful natural products with biological, biomedical, and pharmaceutical importance. For a long time, actinomycetes have been the most popular and known for their application as antibiotics. Moreover, their previously documented use as an antifungal agent is responsible for their popularity with antibiotic research today. Actinomycetes include a substantially large group of species with a wide range of applications in food, biomedical, and pharmaceutical industries [98].
In 1995, Stackebrandt et al. [94] suggested that the monospecific genus Dermacoccus should be classified under actinomycetes [94]. Based on 16S rDNA gene sequence comparison, the genus Dermacoccus is classified under the Dermacoccaceae family [96], which includes other genera such as Demetria [33] and Kytococcus [94]. Previous studies have identified and characterized several species of this family, such as D. nishinomiyaensis, D. abyssi, D. barathri, D. sedentarius, and D. profundi [72, 94].
One member of this group, D. Nishinomiyaensis, is often distinguished by its terrestrial environmental contexts like soil, salt, and partially preserved meat items [15, 19, 69, 89]. Furthermore, within Chinese residential homes, D. profundi has been traced [22], and D. barathri has been detected from soil and water [89].
D. Nishinomiyaensis was previously known as Micrococcus nishinomiyaensis. More than 100 years ago, the genus Micrococcus was first reported and initially characterized, and since then the initial description has been revised multiple times. It has been revealed that D. Nishinomiyaensis, which phenotypically belongs to the large group of Gram-positive and catalase-positive cocci, is phylogenetically considered as a member of the actinomycete group [95]. Several features that characterize this genus include the spherically shaped cells (diameter range from 0.9 to 1.6 pm) and their occurrence in pairs, tetrads, or irregular clusters of tetrads. Their colonies grow up to 2 mm in diameter, and are circular in shape, slightly convex with glistening smooth surfaces, and bright orange in color. D. nishinomiyaensis can grow well in up to 5% NaCI, but no growth occurs in the presence of 7% NaCl. Optimum growth temperature was reported to be in the range of 25 to 37 °C [94].
D. abyssi is detailed as non-acid-alcohol-fast, non-motile actinomycete. Its cells are coccoid-shaped with diameters between 0.8 and 1.5 µm, appearing in uneven groups. Smooth, shiny colonies that are colored pale-yellow to cream, which are circular, entire, or convex, are created on agar from glucose yeast extract at 28 °C for 5 days. D. abyssi develops swiftly on tryptic soy agar, although not as well on inorganic nitrogen agar. Development takes place from 10 to 37 °C, with optimum development at about 28 °C. Degradation of hypoxanthine, cellulose, uric acid, starch, and casein take place. Development happens with the availability of 7.5% NaCl. Glucose yeast extract broth promotes satisfactory development of D. abyssi at 40 MPa [72]. In the present work, we discuss the medical applications of secondary metabolites isolated from D. nishinomiyaensis and D. abyssi, as well as highlight their molecular mode of activities and potential medical applications.
Dermacoccus spp Role in Bacterial Community
Many reports have established the function of Dermacoccus within the bacterial community. Phylogenetic evaluations of the culturable proportion of the bacterial community separated from the marine sponge Erylus deficiens disclosed the availability of Dermacoccus. Numerous Erylus isolates were seen to show antibacterial and high antifungal bioactivities against pathogenic and environmental strains. Polyketide synthases (PKS) and Novel non-ribosomal peptide synthetase (NRPS) genes may also have relation to a few Erylus isolates. As a result, the raised bioactivity levels and the fact that there could be some related genes hint that Erylus deficiens bacteria may be the origin of new marine bioactive mixtures [30]. Scrutiny of gastrointestinal GI tract communities of Panaque nigrolineatus produced by anaerobic microcrystalline cellulose enhancement cultures through 16S rRNA gene examination showed phylotypes having a common high sequence likeness to recognized cellulolytic bacteria such as Dermacoccus nishinomiyaensis, Clostridium xylanolyticum, Cellulomonas chitinilytica, Bacteroides xylanolyticus, Eubacterium contortum, and Aeromonas spp. For this reason, the P. nigrolineatus GI tract is a better environment for cellulose degrading, and these communities might have to deal with the availability of assimilable carbon in the case of difficult dietary conditions [104]. Paenibacillus sp., Leifsonia sp. and Bacillus sp. had the greatest numbers in the rhizosphere linked to ‘Belgisch Rood’(BR) willow clone, at 22.04, 20.81, and 21.27%, respectively, for the individual strains. The other proportion of the isolated BR-related rhizosphere bacteria was made up of Streptomyces sp. (13.29%), Dermacoccus sp. (7.97%), Luteibacter sp. (7.97%), and Caulobacter sp [106]. Wittebolle et al. [107] outlined that the performance of a bacterial community with greater diversity has greater resistance to stress from the environment than that of a bacterial community with reduced diversity. Being aware of this, endophytic bacterial diversity seen in ‘Tora’ (TO) clone could bring about improved performance for the endophytic TO-related bacterial community with the current metal stress, which could assist improved maturity and growth of the host plant [107]. Analysis of the upper buttock showed a strong gender effect with males displaying relatively high proportions of Corynebacterium, Dermacoccus, Streptococcus, and Finegoldia, while females exhibited greater levels of Lactobacillus, Propionibacterium, Staphylococcus, and Enhydrobacter [110]. Bacterial colonization on human skin begins at birth and carries on all through the early years of life. The microbial communities later stabilize and assist in the formation of cutaneous homeostasis and control of inherent human responses [9]. The brief or long-term availability of these microbes on the skin is reliant on the topographical areas of the body which have varying particular conditions (such as pH, moisture, and sebum content), factors specific to the host (such as age and gender), and environmental aspects particular to the individual (such as geographical location, occupation, lifestyle, use of antibiotics, use of cosmetics, and soaps) [32]. Remarkably, the microbiome of the deeper stratum corneum layers remarkably has an important function in the skin’s microbial recolonization procedure following injury. Additionally, microbiome dynamics of the human epidermis after disruption of the skin barrier displayed great interpersonal variation, and significant differences due to gender [110]. Pang et al. [68] reported that three out of four bacterial isolates taken from a reverse osmosis (RO) membrane treating potable water (Dermacoccus RO12, Microbacterium RO18, and Rhodopseudomonas RO3) were reported as not displaying swimming motility, which suggested that they could be conveyed to the surface of the membrane by means of other structures including convective permeate flow [68].
Dermacoccus Nishinomiyaensis
D. nishinomiyaensis has demonstrated the capability to produce monensins A and B using a soya bean medium [80], within flat-bottomed flasks of volume 500 mL at 34 °C for 10 days on a rotary shaker (162 rpm) with the origin of carbon being lactose or fructose [79]. Monensins are oligomers with C2–C4 units comprising acetate, propionate, and butyrate [18]. The salts from this group of compounds exhibit significant medical importance. For instance, the compound monensin sodium is a known polyether ionophore antibiotic that can control and counteract specific viral infections [49].
Biosynthetic Trajectory of Monensin A
Monensin, which has several homologues such as monensin A, B, and C, was isolated for the first time in 1967. Monensin sodium salt has been biosynthesized in the culture of S. cinnamonensis [18, 48, 86]. Monensin A, which is oxidized to the corresponding polyepoxide, is produced in a classic polyketide pathway from seven propionate, one butyrate, and five acetate units [8]. According to Bhatt et al. [5], activation of oxidative cyclization does not precede production of the full-length chain, while a linear enzyme-bound (E,E,E)-triene known as “premonensin” is the original PKS product [5]. The tri-epoxide 3 is produced as a result of the catalysis of three stereospecific epoxidations by the flavin-dependent epoxidase MonCI and is subsequently subjected to a cascade of ring opening/closing. The unusual epoxide hydrolases MonBI and MonBII then act together to catalyze this cascade and generate the supposed protein-bound intermediate dehydroxydemethylmonensin [61]. The following stages involve hydroxylation at C-26 with cytochrome P450 hydroxylase MonD acting as catalyst and hydroxy group O-methylation at C-3 with the catalyst methyltransferase MonE [37]. In Fig. 1, methylation is demonstrated to take place following hydroxylation, although in actuality no regulation has been enforced concerning the sequence of these procedures. The generation of mature monensins A and B from MonACPX, with the irregular thioesterase MonCII functioning as a catalyst, comprises the final biosynthesis phase [40].
The suggested model through which monensin can be biosynthesized in the case of Streptomyces cinnamonensis (Reproduced with permission of author [39])
Clinical Applications of Monensin
In the current large-scale industries, exposure to heavy metals, such as lead, presents a major health problem faced by both developed and developing countries [25, 31, 67, 73]. Lead exposure has various negative effects on the function of different organs, such as the spleen, liver, kidneys, and brain [25]. Notably, the nervous system is the most sensitive to lead-induced toxicity [13, 16, 64, 90]. Furthermore, lead was reported to destroy the function of hematopoietic system cells [78]. Despite its cellular toxicity, the biochemical activity of this toxic metal was shown to resemble that of other divalent metal ions, such as calcium [51]. Intoxicated male mice exposed to lead salts showed significant accumulation of lead in all studied organs compared with the untreated control animals [41]. The results from this study revealed that the bio-distribution of lead occurred in the following order: kidneys > spleen > liver > brain. Interestingly, the treatment of the lead-intoxicated animals with tetraethylammonium salts of monensin significantly mitigated the accumulation of the toxic metal, compared to the toxic control animals. The previously observed effect varied from 38% (for kidneys) to 52% (for brain) compared to the toxic control group (lead). Therefore, monensin is considered to be a potential chelating agent for the treatment of lead poisoning [41]. Through monensin treatment, the expression of Penk mRNA was down-regulated, whereas that of Ceacam10 was increased without affecting the Gapdh gene in DRG neurons obtained from wild-type mice. These results indicated that monensin could serve as a second messenger in sensory neurons for the regulation of gene expression [62]. It has been reported that monensin exhibits antiviral, antifungal, antiparasitic, antimalarial, anti-inflammatory, and tumor cell cytotoxic activity [10, 35, 45, 81]. Recently, the anti-neoplastic activity of polyether ionophores was substantially supported by the finding that these compounds may be able to kill cancer stem cells and mitigate the growth of breast cancer, and metastasis in mice [34, 109]. Such effects partly resulted from the alteration of the intracellular pH by ionophores [55]. The tumor growth has been suppressed in the APC+/Min mice after the treatment by monensin. While the average number of tumors has remained unchanged in the treated animals, the size of neoplastic lesions was reduced. These findings indicated that monensin plays a role in tumor progression inhibition instead of the tumor initiation process [100].
Several studies have demonstrated that monensins exhibit antiproliferative activity against several cancer cell lines and their models, such as human colon cancer, lymphoma, and myeloma. Specifically, it was revealed that monensin induces G1 and/or G2-M arrest during the cell cycle of these cells. The potent cytotoxic effect of this ionophore and its crucial function in counteracting the multi-drug resistance of cancer cells has been also demonstrated previously. Only four compounds, including monensin, of 4910 tested compounds show a specific inhibition on the proliferation and growth of prostate cancer cells at a small concentration scale such as nanomolar concentrations [14, 21, 44, 52, 53, 66, 105].
The major mechanism of monensin as a cation carrier is the electrically silent exchange of sodium (or potassium) cations for protons across the membrane. Monensin can perform non-electrogenic exchange of potassium (sodium) ions for protons and serve as electrogenic potassium ion carriers similar to valinomycin [81, 105]. The functional activity observed on artificial membranes and mitochondria can explain the function of monensin and its derivatives in living systems related to ionophorous properties and the action on the oxidative phosphorylation. This work is particularly important in the study of the antitumor activity of monensin and similar polyether ionophores, especially as apoptotic cell death is frequently associated with the perturbation of mitochondria through the induction of oxidative stress, activation of pro-apoptotic proteins localized in the mitochondria, and release of cytochrome C. Thus, the swelling of the mitochondria can be assumed to trigger the process of mitochondrial perturbation [2].
The synergistic effect of monensin with EGFR inhibitors and oxaliplatin has been demonstrated through the inhibition of cell proliferation and induced apoptosis of ovarian cancer cells. Xenograft studies showed that tumor growth was effectively inhibited by repressing cell proliferation, by targeting EGFR signaling. Therefore, monensin could be used as a therapeutic agent for ovarian cancer treatment, although future investigations are required [20]. Moreover, an interaction between monensin and silybin considerably reduced the cytotoxicity within cell line cultures of HepG2, LMH, and L6. These findings confirmed that the action of monensin mainly focused on the metabolism of HepG2 and LMH cells, leading to their severe impairment [17]. However, the disintegration of the cell membrane in the rat myoblasts covered by monensin appeared as a prevalent mechanism of cytotoxicity [83, 84]. Therefore, these results might represent a useful approach for the applicability of monensin in human therapy [17]. The clinical applications of monensin are summarized in Fig. 2.
Due to it exhibiting such high biological activity, monensin is considered as an attractive molecule for biomedical and biological investigations. As a result, several chemical modifications have been performed on this compound to improve its bioactivity and its bioavailability. Depending on the nature and site of modification, the resulting derivatives may differ in their activities, toxicities, and selectivity of cation complexity compared to that of the parental compound [53]. Various modifications on the COOH group of monensin have been performed frequently to generate a series of secondary amide and ester derivatives that can exhibit biological activity against various Gram-positive bacterial species; for instance, these effects have been demonstrated against strains obtained from hospitals, such as methicillin-sensitive and methicillin-resistant Staphylococcus aureus strains [54]. This resistance suggested the need for chemically improved versions of monensin that can exhibit higher efficacy. Indeed, new tertiary amide derivatives of polyether ionophore monensin A were synthesized, and their anti-neoplastic activity against human cancer cell lines was studied. Monensin A showed very high activity (IC50 = 0.09 µM) and selectivity (SI = 232) toward human biphenotypic myelomonocytic leukemia cell line (MV4-11). Thus, the generated derivatives of monensin demonstrated remarkable anti-neoplastic activity, high selectivity, and the ability to bypass the drug resistance of some cancer cell lines [39].
Dermacoccus Abyssi
Two strains of D. abyssi (MT1.1 and MT1.2) have been isolated from Mariana sediments at a depth of approximately 10 898 m. The MT1.1 D. abyssi strain was developed in baffled shake flasks of volume 250 mL, comprising 70 mL yeast extract-malt extract broth [91] with the availability of HP20 resin over 7 days at a temperature of 28 ◦C, following first-phase seeding in 10 mL glucose yeast extract [29]. The MT 1.2 D. abyssi strain was grown in a multifarious medium within 500-mL Erlenmeyer flasks comprising one baffle due to its intense foaming features which appeared in stirred-tank fermenters with aeration [1]. The process of fermentation using complex media resulted in the production of seven new oxidized and reduced phenazine-type pigments, dermacozines A–G (1–7), as well as the well-known phenazine-1-carboxylic acid (PCA) (8) and phenazine-1,6-dicarboxylic acid (9) [1] (Fig. 3).
Biogenetic Pathway of Dermacozines
Like the majority of natural phenazine products, dermacozines are thought to be originated through the shikimic acid pathway, as highlighted in Fig. 4, with chorismic acid comprising the most likely branch point intermediate. Shikimic acid is changed to chorismic acid within acknowledged alterations which comprise elements of the aromatic amino acid biosynthetic trajectory [50, 58, 76, 88]. The conversion from chorismic acid into the phenazine precursors is catalyzed by a sequence of phenazine synthesis-particular enzyme-managed stages to provide trans-2,3-dihydro-3-hydroxyanthranilic acid (DHHA) [60, 70, 71]. Two DHHA molecules can condense themselves to create phenazine-1,6- dicarboxylic acid (9) [6, 27, 57, 60, 101]. An optional trajectory would progress through aminodehyroquinic acid to 5-amino-5-deoxyshikimic acid, which during self-condensation, dehydration, and oxidation, could result in the creation of phenazine-1,6-dicarboxylic acid or its decreased state, which comprise the key precursors for additionally intricate phenazine metabolites [46, 101].
Proposed biogenetic pathway for the dermacozines (Reproduced with permission of author [76])
At some point, phenazine-1,6-dicarboxylic acid would experience N-methylation and single or double amide bond creation, producing a dermacozine A-type biogenetic intermediate [11]. This would pair with a C6–C1 or C6–C2 building block to produce dermacozine B/C compounds or dermacozine D-G congeners. Within this setting, it is remarkable to observe that phenylacetic acid as well as its amide was traced within the culture medium [1]. Ghanta et al. [26] have reported that Dermacozines A, B, and C were synthesized from a commercially available methyl 2-bromo-3-nitrobenzoate and methyl 3-amino-2-chlorobenzoate. The key carbon–carbon and carbon–nitrogen bond-forming reactions include inter- and intra-molecular palladium Pd (0)-catalyzed N-arylations and regioselective Friedel–Crafts benzoylation, respectively. Nitrile group, which is considered as a masked carboxylic group, has been used to functionalize two carboxylic acids to produce Dermacozine C [26].
Biological Activities of Phenazines
Phenazines are extracted as secondary metabolite molecules from Streptomyces, Pseudomonas, and other bacterial strains from diverse habitats including soil and marine. Phenazines have antimicrobial, antiparasitic, and anti-neoplastic activities [12, 50, 56, 59, 82]. PCA, generated by the fluorescent pseudomonads, comprised a significant component of the new antifungal pesticide Shenqinmycin [108], which is described as a potent and broad-spectrum antifungal metabolic molecule [36, 38, 85, 99]. PCA, known as tubermycin B with potent antibiotic activity against Mycobacterium tuberculosis, is one of the simplest molecules of the phenazine group [50]. Moreover, PCA has been shown to facilitate bacterial biofilm formation via ferrous iron sequestering. While it has become clear that iron is required for the growth of organisms, it is well known that the biofilm formation required an amount of iron in excess of this need [3, 4, 74, 87, 93]. Thus, the PCA present in infected cells can alter the kinetics of the redox equilibrium between Fe(III) and Fe(II), and thereby make iron ions relatively more bioavailable [103]. The highest activity of 4 μg/mL by PCA has been recorded against Trichophyton rubrum, a human pathogen that causes athlete’s foot, jock itch, ringworm, and fingernail fungal infections, followed by the potency of PCA against Candida albicans and C. tropicalis [28]. Interestingly, 5-methyl phenazine-1-carboxylic acid betaine (MPCAB) has a potent specific cytotoxicity toward various human cell lines, including lung and breast cancer cell lines, in a dose-dependent manner with IC50 values of 488.7 ± 2.52 and 458.6 ± 2.48 nM, respectively [43]. Furthermore, the cytotoxicity of MPCAB may stem from several molecular effects, including the inhibition of cell viability, inhibition of DNA synthesis, induction of G1 cell cycle arrest, and induction of apoptosis in cancer cells [47, 97]. Docking and interaction studies further solidified and confirmed the binding potential of MPCAB with antiapoptotic proteins, such as Bcl-2, Bcl-xL, and Bcl-w proteins. These results significantly suggest that treatment with MPCAB induced apoptotic cell death in cancer cells through the intrinsic mitochondrial pathway via the activation pro-apoptotic proteases, particularly caspase-3, and the down-regulation of antiapoptotic Bcl-2 protein [43].
As discussed beforehand, the dermacozines are phenazine alkaloids, and the phenazines are naturally created by cells which have ceased dividing and slowly metabolizing. There is no apparent role of phenazine metabolites in cell development, i.e., no significance as origins of energy or reserve materials of any sort. The absence of apparent phenazine metabolic roles has resulted in a number of theories on their physiological function in nature. The fact that phenazine-generating organisms endure longer in their natural settings as contrasted to non-phenazine-generating species has been illustrated [50]. Thus, it is feasible that the phenazines signify a bacterial protective element, resulting from their obvious antibiotic activity, which functions to safeguard the producing organism and its environment against alternative microbial rivals and microorganisms, and therefore enhances the living circumstances of the host organism [50]. Alternative acknowledged biological operations comprise antimalarial, antitumour, antiparasitic, and antioxidant. The likely mode of operation comprises the limitation or control of DNA (groove binding or intercalation), protein and RNA synthesis in addition to disturbance of metabolic procedures that necessitate energy [50].
Dermacozines F (6) and G (7) have a significant cytotoxic activity against chronic myeloid leukemia cell line K562 with IC50 values of 9 and 7 µM, respectively. Furthermore, the maximum radical scavenger activity was noted for dermacozine C (3), with an IC50 value of 8.4 µM [1].
Furthermore, the dermacozines H–J (Fig. 5) extracted from D. abyssi have demonstrated radical scavenging activity; the highest activity was observed for dermacozine H (1), with an IC50 value of 18.8 μM [102]. The efficacy of dermacozines A–G and PCA toward various diseases are shown in Fig. 6.
Conclusion and Future Prospects
Small, secondary metabolic molecules derived from microbes have become a wealthy source of compounds with unique chemical structures and broad biomedical functions. During microbial fermentation, numerous structurally diverse molecules are generated. These natural products have been shown to exhibit various biological activities, such as antibacterial, anticancer, antifungal, immunosuppressive, antioxidant, antiviral, antiparasitic, enzyme-inhibiting, and neuroprotective. Studying the original structures of parent bioactive molecules may prompt the development of unique candidates for novel and potent therapeutics. There is the fact that several secondary metabolic molecules with antibacterial activity led to the broad usage of these molecules and their derived compounds in the treatment of infectious diseases. A large number of bioactive compounds were originally isolated from the soil, which is an easily accessible environment. Current investigations study new strains from less accessible places, such as seas and oceans. The recent emergence of multi-drug resistant strains and the urgent need for improved tumor treatment support the efforts for a continuous study of novel natural bioactive metabolites. In summary, microbial organisms like bacteria represent a rich source of diverse and unique bioactive molecules with potent biological activity, and this area of research still needs to be investigated in the future.
In sum, we suggest that future research should focus on (i) investigating the cytotoxic effect of monensin in vivo; (ii) examining D. abyssi-derived PCA and phenazine-1,6-dicarboxylic acid as bioactive products against diverse types of diseases; (iii) investigating the optimal growth conditions for D. abyssi and D. Nishinomiyaensis to optimize the high-yield production of PCA and monensin; and (v) identifying and examining the novel compounds and enzymes from D. profundi or D. barathri, which could exhibit biotechnological properties for biomedical, pharmaceutical, and industrial applications.
References
Abdel-Mageed WM, Milne BF, Wagner M, Schumacher M, Sandor P, Pathom-Are W, Goodfellow M, Bull AT, Horikoshi K, Ebel R, Diederich M, Fiedler HP, Jaspars M (2010) Dermacozines, a new phenazine family from deep-sea dermacocci isolated from a mariana trench sediment. Org Biomol Chem 8:2352–2362
Antonenko YN, Rokitskaya TI, Huczyński A (2015) Electrogenic and nonelectrogenic ion fluxes across lipid and mitochondrial membranes mediated by monensin and monensin ethyl ester. Biochim Biophys Acta 1848:995–1004
Banin E, Vasil ML, Greenberg EP (2005) Iron and Pseudomonas aeruginosa biofilm formation. Proc Natl Acad Sci USA 102:11076–11081
Berlutti F, Morea C, Battistoni A, Sarli S, Cipriani P, Superti F, Ammendolia MG, Valenti P (2005) Iron availability influences aggregation, biofilm, adhesion and invasion of Pseudomonas aeruginosa and Burkholderia cenocepacia. Int J Immunopathol Pharmacol 18:661–670
Bhatt A, Stark CB, Harvey BM, Gallimore AR, Demydchuk YA, Spencer JB, Staunton J, Leadlay PF (2005) Accumulation of an E, E, E-triene by the monensin-producing polyketide synthase when oxidative cyclization is blocked. Angew Chem Int Edit 44:7075–7078
Buckland PR, Gulliford SP, Herbert RB, Holliman FG (1981) The biosynthesis of lomofungin via phenazine-l,6-dicarboxylic acid. J Chem Res Synop 362
Bull AT, Stach JE (2007) Marine actinobacteria: new opportunities for natural product search and discovery. Trends Microbiol 15:491–499
Cane DE, Celmer WD, Westley JW (1983) Unified stereochemical model of polyether antibiotic structure and biogenesis. J Am Chem Soc 105:3594–3600
Capone KA, Dowd SE, Stamatas GN, Nikolovski J (2011) Diversity of the human skin microbiome early in life. J Invest Dermatol 131:2026–2032
Chapman H, Jeffers T, Williams R (2010) Forty years of monensin for the control of coccidiosis in poultry. Poult Sci 89:1788–1801
Chin-A-Woeng TFC, Thomas-Oates JE, Lugtenberg BJJ, Bloemberg GV (2001) Introduction of the phzH gene of Pseudomonas chlororaphis PCL1391 extends the range of biocontrol ability of phenazine-1-carboxylic acid-producing Pseudomonas spp. strains. Mol Plant Microbe Interact 14:1006–1015
Cimmino A, Evidente A, Mathieu V, Andolf A, Lefranc F, Kornienko A, Kiss R (2012) Phenazines and Cancer. Nat Prod Rep 29:487–501
Cleveland LM, Minter ML, Cobb KA, Scott AA, German VF (2008) Lead hazards for pregnant women and children: part 1: immigrants and the poor shoulder most of the burden of lead exposure in this country. Part 1 of a two-part article details how exposure happens, whom it affects, and the harm it can do. Am J Nurs 108:40–49
Colombatti M, Dell’arciprete L, Chignola R, Tridente G (1990) Carrier protein-monensin conjugates: enhancement of immunotoxin cytotoxicity and potential in tumor treatment. Cancer Res 50:1385–1391
Cordero MR, Zumalaca´rregui JM (2000) Characterization of Micrococcaceae isolated from salt used for spanish dry-cured ham. Lett Appl Microbiol 31:303–306
Cory-Slechta DA (1996) Legacy of lead exposure: consequences for the central nervous system. Otolaryngol Head Neck Surg 114:224–226
Cybulski W, Radko L, Rzeski W (2015) Cytotoxicity of monensin, narasin and salinomycin and their interaction with silybin in hepg2, lmh and l6 cell cultures. Toxicol In Vitro 29:337–344
Day L, Chamberlin J, Gordee E, Chen S, Gorman M, Hamill RL, Ness T, Weeks RE, Stroshane R (1973) Biosynthesis of monensin. Antimicrob Agents Chemother 4:410–414
De la Rosa MC, Mohino MR, Mohino M, Mosso MA (1990) Characteristics of micrococci and staphylococci isolated from semipreserved meat products. Food Microbiol 7:207–215
Deng Y, Zhang J, Wang Z, Yan Z, Qiao M, Ye J, Wei Q, Wang J, Wang X, Zhao L, Lu S, Tang S, Mohammed MK, Liu H, Fan J, Zhang F, Zou Y, Liao J, Qi H, Haydon RC, Luu HH, He TC, Tang L (2015) Antibiotic monensin synergizes with EGFR inhibitors and oxaliplatin to suppress the proliferation of human ovarian cancer cells. Sci Rep 5:17523
Derbyshire EJ, Henry RV, Stahel RA, Wawrzynczak EJ (1992) Potent cytotoxic action of the immunotoxin swa11-ricin a chain against human small cell lung cancer cell lines. Br J Cancer 66:444–451
Fang Z, Gong C, Ouyang Z, Liu P, Sun L, Wang X (2014) Characteristic and concentration distribution of culturable airborne bacteria in residential environments in Beijing, China. Aerosol Air Qual Res 14:943–953
Fenical W, Jensen PR (2006) Developing a new resource for drug discovery: marine actinomycete bacteria. Nat Chem Biol 2:666–673
Fiedler HP, Bruntner C, Bull AT, Ward AC, Goodfellow M, Potterat O, Puder C, Mihm G (2005) Marine actinomycetes as a source of novel secondary metabolites. Ant van Leeuwenhoek 87:37–42
Flora G, Gupta D, Tiwari A (2012) Toxicity of lead: a review with recent updates. Interdiscip Toxicol. 5:47–58
Ghanta VR, Pasula A, Soma L, Raman B (2016) Synthetic studies on dermacozines: first synthesis of dermacozines a, b and c. Chem PubSoc Europe 6:1296–1299
Giddens SR, FengY Mahanty HK (2002) Characterization of a novel phenazine antibiotic gene cluster in Erwinia herbicola Eh1087. Mol Microbiol 45:769–783
Gorantla JN, Kumar NS, Nisha GV, Sumandu AS, Dileep C, Sudaresan A, Kumar MM, Lankalapalli RS, Kumar BS (2014) Purification and characterization of antifungal phenazines from a fluorescent pseudomonas strain fpo4 against medically important fungi. J Mycol Med 24:185–192
Gordon RE, Mihm JM (1962) The type species of the genus Nocardia. Acad Sci 98:628–636
Graça AP, Viana F, Bondoso J, Correia MI, Gomes LAGR, Humanes M, Reis A, Xavier J, Gaspar H, Lage O (2015) The antimicrobial activity of heterotrophic bacteria isolated from the marine sponge Erylus deficiens (Astrophorida, Geodiidae). Front Microbiol 6:1–14
Grant LD (2008) Lead and compounds, in environmental toxicants: human exposures and their health effects, 3rd edn. John Wiley & Sons Inc., USA
Grice EA, Segre JA (2011) The skin microbiome. Nat Rev Microbiol 9:244–253
Groth I, Schumann P, Rainey F, Martin K, Schuetze B, Augsten K (1997) Demetria terragena gen. nov., sp. nov., a new genus of actinomycetes isolated from compost soil. Int J Syst Bacteriol 47:1129–1133
Gupta PB, Onder TT, Jiang G, Tao K, Kuperwasser C, Weinberg RA, Lander ES (2009) Identification of selective inhibitors of cancer stem cells by high-throughput screening. Cell 138:645–659
Gupta RC (2012) Veterinary toxicology: basic and clinical principles, 2nd edn. Academic Press, Boston
Haas D, Défago G (2005) Biological control of soil-borne pathogens by fluorescent pseudomonads. Nat Rev Microbiol 3:307–319
Harvey BM, Mironenko T, Sun Y, Hong H, Deng Z, Leadlay PF, Weissman KJ, Haydock SF (2007) Insights into polyether biosynthesis from analysis of the nigericin biosynthetic gene cluster in Streptomyces sp. DSM4137. Chem Biol 14:703–714
Haynes WC, Stodola FH, Locke JM, Pridham TG, Conway HF, Sohns VE, Jackson RW (1956) Pseudomonas aureofaciens kluyver and phenazine α-carboxylic acid, its characteristic pigment. J Bacteriol 72:412–417
Huczyński A, Klejborowska G, Antoszczak M, Maj E, Wietrzyk J (2015) Anti-proliferative activity of monensin and its tertiary amide derivatives. Bioorg Med Chem Lett 15:4539–4543
Hüttel W, Spencer JB, Leadlay PF (2014) Intermediates in monensin biosynthesis: a late step in biosynthesis of the polyether ionophore monensin is crucial for the integrity of cation binding. Beilstein J Org Chem 10:361–368
Ivanova J, Gluhcheva Y, Dimova D, Pavlova E, Arpadjan S (2016) Comparative assessment of the effects of salinomycin and monensin on the biodistribution of lead and some essential metal ions in mice, subjected to subacute lead intoxication. J Trace Elem Med Bio 33:31–36
Jensen PR, Mincer TJ, Williams PG, Fenical W (2005) Marine actinomycete diversity and natural product discovery. Ant van Leeuwenhoek 87:43–48
Kennedy RK, Naik PR, Veena V, Lakshmi B, Lakshmi P, Krishna R, Sakthivel N (2015) 5-Methyl Phenazine-1-Carboxylic Acid: a novel bioactive metabolite by a rhizosphere soil bacterium that exhibits potent antimicrobial and anticancer activities. Chem Biol Interact 231:71–82
Ketola K, Vainio P, Fey V, Kallioniemi O, Iljin K (2010) Monensin is a potent inducer of oxidative stress and inhibitor of androgen signaling leading to apoptosis in prostate cancer cells. Mol Cancer Ther 9:3175–3185
Kevin-Ii DA, Meujo DA, Hamann MT (2009) Polyether ionophores: broad-spectrum and promising biologically active molecules for the control of drug-resistant bacteria and parasites. Expert Opin Drug Discov 4:109–146
Kim CG, Kirsching A, Bergon P, AhnY Wang JJ, Shibuya M, Floss HG (1992) Formation of 3-amino-5-hydroxybenzoic acid, the precursor of mC7 N units in ansamycin antibiotics, by a new variant of the shikimate pathway. J Am Chem Soc 114:4941–4943
Kondratyuk TP, Park EJ, Yu R, van Breemen RB, Asolkar RN, Murphy BT, Fenical W, Pezzuto JM (2012) Novel marine phenazines as potential cancer chemopreventive and anti-inflammatory agents. Mar Drugs 10:451–464
Kralovcova E, Krumphanzl V, Vanek Z (1984) Improving the production of monensin by Streptomyces cinnamonensis. Folia Microbiol 29:35–42
Kyriakis SC, Lemmas JC, Mavromatis JC, Tsinas AC, Lekkas SG, Tsangaris TA (1993) The effect of monensin in the control of transmissible gastroenteritis (TGE) of pigs. J Swine Health Prod 1:15–18
Laursen JB, Nielsen J (2004) Phenazine natural products: biosynthesis, synthetic analogues, and biological activity. Chem Rev 104:1663–1686
Lidsky TI, Schneider JS (2003) Lead neurotoxicity in children: basic mechanisms and clinical correlates. Brain 126:5–19
Ling Y, Priebe W, Perezsoler R (1993) Intrinsic cytotoxicity and reversal of multidrug-resistance by monensin in kb parent and mdr cells. Int J Oncol 3:971–977
Łowicki D, Huczyński A (2013) Structure and antimicrobial properties of monensin a and its derivatives: summary of the achievements. BioMed Re Int 2013:1–14
Łowicki D, Huczyński A, Stefańska J, Brzezinski B (2010) Structural characterization and antibacterial activity against clinical isolates of Staphylococcus of N-phenylamide of monensin A and its 1:1 complexes with monovalent cations. Eur J Med Chem 45:4050–4057
Margolis LB, Novikova YU, Rozovskaya IA, Skulachev VP (1989) K +/H + -antiporter nigericin arrests DNA synthesis in ehrlich ascites carcinoma cells. Proc Natl Acad Sci 86:6626–6629
Mavrodi DV, Blankenfeldt W, Thomashow LS (2006) Phenazine compounds in fluorescent pseudomonas spp. biosynthesis and regulation. Annu Rev Phytopathol 44:417–445
Mavrodi DV, Bonsall RF, Delaney SM, Soule MJ, Phillips G, Thomashow LS (2001) Functional analysis of genes for biosynthesis of pyocyanin and phenazine-1-carboxamide from Pseudomonas aeruginosa PAO1. J Bacteriol 183:6454–6465
Mavrodi DV, Ksenzenko VN, Bonsall RF, Cook RJ, Boronin AM, Thomashow LS (1998) A seven-gene locus for synthesis of phenazine-1-carboxylic acid by Pseudomonas fluorescens2-79. J Bacteriol 180:2541–2548
Mavrodi DV, Peever TL, Mavrodi OV, Parejko JA, Raaijmakers JM, Lemanceau P, Mazurier S, Heide L, Blankenfeldt W, Weller DM, Thomashow LS (2010) Diversity and evolution of the phenazine biosynthesis pathway. Appl Environ Microbiol 76:866–879
McDonald M, Mavrodi DV, Thomashow LS, Floss HG (2001) Phenazine biosynthesis in Pseudomonas fluorescens: branchpoint from the primary shikimate biosynthetic pathway and role of phenazine-1,6-dicarboxylic acid. J Am Chem Soc 123:9459–9460
Minami A, Ose T, Sato K, Oikawa A, Kuroki K, Maenaka K, Oguri H, Oikawa H (2014) Allosteric regulation of epoxide opening cascades by a pair of epoxide hydrolases in monensin biosynthesis. ACS Chem Biol 9:562–569
Minett MS, Pereira V, Sikandar S, Matsuyama A, Lolignier S, Kanellopoulos AH, Mancini F, Iannetti GD, Bogdanov YD, Santana-Varela S, Millet Q, Baskozos G, MacAllister R, Cox JJ, Zhao J, Wood JN (2015) Endogenous opioids contribute to insensitivity to pain in humans and mice lacking sodium channel Nav1. 7. Nat Commun 6:8967
Molinski TF, Dalisay DS, Lievens SL, Saludes JP (2009) Drug development from marine natural products. Nat Rev Drug Discovery 8:69–85
Needleman H (2004) Lead poisoning. Annu Rev Med 55:209–222
Newman DJ, Cragg GM (2004) Marine natural products and related compounds in clinical and advanced preclinical trials. J Nat Prod 67:1216–1238
Newton DL, Hansen HJ, Mikulski SM, Goldenberg DM, Rybak SM (2001) Potent and specific antitumor effects of an anti-cd22–targeted cytotoxic ribonuclease: potential for the treatment of non-hodgkin lymphoma. Blood 97:528–535
Pachauri V, Dubey M, Yadav A, Kushwaha P, Flora S (2012) Monensin potentiates lead chelation efficacy of MiADMSA in rat brain post chronic lead exposure. Food Chem Toxicol 50:4449–4460
Pang MC, Hong H, Guo H, Liu WT (2005) Biofilm formation characteristics of bacterial isolates retrieved from a reverse osmosis membrane. Environ Sci Technol 39:7541–7550
Papamanoli E, Kotzekidou P, Tzanetakis N, Litopoulou-Tzanetaki E (2002) Characterization of Micrococcaceae isolated from dry fermented sausage. Food Microbiol 19:441–449
Parsons JF, Calabrese K, Eisenstein E, Ladner JE (2003) Structure and mechanism of Pseudomonas aeruginosa phzd, an isochorismatase from the phenazine biosynthetic pathway. Biochemistry 42:5684–5693
Parsons JF, Calabrese K, Eisenstein E, Ladner JE (2004) Structure of the phenazine biosynthesis enzyme PhzG. Acta Crystallogr D Biol Crystallogr 60:2110–2113
Pathom-Aree W, Nogi Y, Ward AC, Horikoshi K, Bull AT, Goodfellow M (2006) Dermacoccus barathri sp. nov. and Dermacoccus profundi sp. nov., novel actinomycetes isolated from deep-sea mud of the mariana trench. Int J Syst Evol Microbiol 56:2303–2307
Patrick L (2006) Lead toxicity part II: the role of free radical damage and the use of antioxidants in the pathology and treatment of lead toxicity. Altern Med Rev 11:114–127
Patriquin GM, Banin E, Gilmour C, Tuchman R, Greenberg EP, Poole K (2008) Influence of quorum sensing and iron on twitching motility and biofilm formation in Pseudomonas aeruginosa. J Bacteriol 190:662–671
Penesyan A, Kjelleberg S, Egan S (2010) Development of novel drugs from marine surface associated microorganisms. Mar Drugs 8:438–459
Pierson LS, Thomashow LS (1992) Cloning and heterologous expression of the phenazine biosynthetic locus from Pseudomonas aureofaciens 30-84. Mol Plant-Microbe Interact 5:330–339
Pimentel-Elardo SM, Kozytska S, Bugni TS, Ireland CM, Moll H, Hentschel U (2010) Anti-parasitic compounds from Streptomyces sp. strains isolated from mediterranean sponges. Mar Drugs 8:373–380
Piomelli S (2002) Childhood lead poisoning. Pediatr Clin North Am 49:1285–1304
Pospisil S, Benada O, Kofronova O, Petricek M, Janda L, Havlicek V (1998) Kytococcus sedentarius (formerly Micrococcus sedentarius) and Dermacoccus nishinomiyaensis (formerly Micrococcus nishinomiyaensis) produce monensins, typical Streptomyces cinnamonensis metabolites. Can J Microbiol 44:1007–1011
Pospíšil S, Sedmera P, Havlícek V, Tax J (1994) Production of 26-deoxymonensins A and B by Streptomyces cinnamonensis in the presence of metyrapone. Appl Environ Microbiol 60:1561–1564
Pressman BC, Deguzman NT (1975) Biological applications of ionophores. Annu Rev Biochem 264:373–386
Price-Whelan A, Dietrich LE, Newman DK (2006) Rethinking ‘secondary’ metabolism: physiological roles for phenazine antibiotics. Nat Chem Biol 2:71–78
Radko L, Cybulski W, Rzeski W (2013) Cytoprotective effect of silybin against lasalocid-induced toxicity in HepG2 cells. Pol J Vet Sci 16:275–282
Radko L, Cybulski W, Rzeski W (2013) The protective effect of silybin against lasalocid cytotoxic exposure on chicken and rat cell lines. BioMed Res Int 2013:1–8
Ranjbariyan A, Shams-Ghahfarokhi M, Razzaghi-Abyaneh M (2014) Antifungal activity of a soil isolate of Pseudomonas chlororaphis against medically important dermatophytes and identification of a phenazine-like compound as its bioactive metabolite. J Mycol Med 24:E57–E64
Rezanka T, Klanova K, Podojil M, Vanek Z (1984) Fatty acids of Streptomyces cinnamonensis, producer of monensin. Folia Microbiol 29:217–221
Rogan MP, Taggart CC, Greene CM, Murphy PG, O’Neill SJ, McElvaney NG (2004) Loss of microbicidal activity and increased formation of biofilm due to decreased lactoferrin activity in patients with cystic fibrosis. J Infect Dis 190:1245–1253
Romer A, Herbert RB (1982) Further observations on the source of nitrogen in phenazine biosynthesis. Z Naturforsch C Bio Sci 37:1070
Ruckmani A, Chakrabarti T (2011) Analysis of bacterial community composition of a spring water from the Western Ghats, India using culture dependent and molecular approaches. Curr Microbiol 62:7–15
Sanders T, Liu Y, Buchner V, Tchounwou PB (2009) Neurotoxic effects and biomarkers of lead exposure: a Review. Rev Environ Health 24:15–46
Shirling EB, Gottlieb D (1966) Methods for characterization of Streptomyces species. Int J Syst Bacteriol 16:313–340
Simmons T, Andrianasolo E, McPhail K, Flatt P, Gerwick WH (2005) Marine natural products as anticancer drugs. Mol Cancer Ther 4:333–342
Singh PK, Parsek MR, Greenberg EP, Welsh MJ (2002) A component of innate immunity prevents bacterial biofilm development. Nature 417:552–555
Stackebrandt E, Koch C, Gvozdiak O, Schumann P (1995) Taxonomic dissection of the genus Micrococcus: Kocuria gen. nov., Nesterenkonia gen. nov., Kytococcus gen. nov., Dermacoccus gen. nov., and Micrococcus Cohn 1872 gen. emend. Int J Syst Bacteriol 45:682–692
Stackebrandt E, Lewis B, Woese C (1980) The phylogenetic structure of the coryneform group of bacteria. Zentralbl Bakteriol 1:137–149
Stackebrandt E, Schumann P (2000) Description of Bogoriellaceae fam. nov., dermacoccaceae fam. nov., rarobacteraceae fam. nov. and sanguibacteraceae fam. nov. and emendation of some families of the suborder Micrococcineae. Int J Syst Evol Microbiol 50:1279–1285
Stewart ZA, Westfall M, Pietenpol JA (2003) Cell cycle dysregulation and anticancer therapy. Trends Pharmacol Sci 24:139–145
Subramani R, Aalbersberg W (2012) Marine actinomycetes: an ongoing source of novel bioactive metabolites. Microbiol Res 167:571–580
Thomashow LS, Weller DM (1988) Role of a phenazine antibiotic from Pseudomonas fluorescens in biological control of Gaeumannomyces graminis var. tritici. J Bacteriol 170:3499–3508
Tumova L, Pombinho AR, Vojtechova M, Stancikova J, Gradl D, Krausova M, Sloncova E, Horazna M, Kriz V, Machonova O (2014) Monensin inhibits canonical Wnt signaling in human colorectal cancer cells and suppresses tumor growth in multiple intestinal neoplasia mice. Mol Cancer Ther 13:812–822
Van’t Land CW, Mocek U, Floss HG (1993) Biosynthesis of the phenazine antibiotics, the saphenamycins and esmeraldins, in Streptomyces antibioticus. J Org Chem 58:6576–6582
Wagner M, Abdel-Mageed WM, Ebel R, Bull AT, Goodfellow M, Fiedler HP, Jaspars M (2014) Dermacozines H-J isolated from a deep-sea strain of Dermacoccus abyssi from Mariana Trench sediments. J Nat Prod 77:416–420
Wang Y, Wilks JC, Danhorn T, Ramos I, Croal L, Newman DK (2011) Phenazine-1-carboxylic acid promotes bacterial biofilm development via ferrous iron acquisition. J Bacteriol 193:3606–3617
Watts JE, Mcdonald R, Daniel R, Schreier HJ (2013) Examination of a culturable microbial population from the gastrointestinal tract of the wood-eating loricariid catfish Panaque nigrolineatus. Diversity 5:641–656
Westley JW (1982) Polyether antibiotics: naturally occurring acid ionophores. Marcel Dekker, New York, pp 1–20
Weyens N, Beckers B, Schellingen K, Ceulemans R, Croes S, Janssen J, Haenen S, Witters N, Vangronsveld J (2013) Plant-associated bacteria and their role in the success or failure of metal phytoextraction projects: first observations of a field-related experiment. Microb Biotechnol 6:288–299
Wittebolle L, Marzorati M, Clement L, Balloi A, Daffonchio D, Heylen K, De Vos P, Verstraete W, Boon N (2009) Initial community evenness favours functionality under selective stress. Nature 458:623–626
Xu Y (2013) Genomic features and regulation of phenazine biosynthesis in the rhizosphere strain Pseudomonas aeruginosa M18. In: Chincholkar S, Thomashow L (eds) Microbial Phenazines. Springer, Heidelberg, pp 177–198
Yoon MJ, Kang YJ, Kim IY, Kim EH, Lee JA, Lim JH, Kwon TK, Choi KS (2013) Monensin, a polyether ionophore antibiotic, overcomes TRAIL resistance in glioma cells via endoplasmic reticulum stress, DR5 upregulation and c-FLIP down regulation. Carcinogenesis 34:1918–1928
Zeeuwen P, Boekhorst J, Van Den Bogaard EH, De Koning HD, Van De Kerkhof P, Saulnier DM, Van Swam II, Van Hijum S, Kleerebezem M, Schalkwijk J (2012) Microbiome dynamics of human epidermis following skin barrier disruption. Genome Biol 13:R101
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors confirm that this article content has no conflict of interest.
Rights and permissions
About this article
Cite this article
AlMatar, M., Eldeeb, M., Makky, E.A. et al. Are There Any Other Compounds Isolated From Dermacoccus spp at All?. Curr Microbiol 74, 132–144 (2017). https://doi.org/10.1007/s00284-016-1152-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00284-016-1152-3