Abstract
B cells and B cell-derived autoantibodies play a central role in the pathogenesis of many autoimmune diseases. Thus, depletion of B cells via monoclonal antibodies such as Rituximab is an obvious therapeutic intervention and has been used successfully in many instances. More recently, novel therapeutic options targeting either the autoantibody itself or resetting the threshold for B cell activation have become available and show promising immunomodulatory and anti-inflammatory effects in a variety of animal models. The aim of this review is to summarize these results and to provide an insight into the underlying molecular and cellular pathways of these novel therapeutic interventions targeting autoantibodies and B cells and to discuss their value for human therapy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Loss of humoral tolerance is a hallmark of autoimmune diseases such as immunothrombocytopenia (ITP), autoimmune hemolytic anemia (AIHA), rheumatoid arthritis (RA), systemic lupus erythematosus (SLE), skin blistering diseases, and acute and chronic inflammation of the peripheral nervous system [1–3]. Research over the last years has established that the production of self-reactive antibodies (autoantibodies) in these diseases may not represent a mere bystander effect useful for therapeutic purposes but that B cells and autoantibodies actively contribute to the inflammatory process and tissue destruction. Moreover, it has become clear that B cells and autoantibodies may also be critical for the development of autoimmune diseases in which T cells were thought to be the dominant factor driving tissue destruction and inflammation such as multiple sclerosis and type 2 diabetes [4]. Thus, in the absence of B cells and pathogenic IgG antibodies, diabetes induced by a high-fat diet was strongly ameliorated, suggesting that class-switched IgG-positive B cells, which accumulate in fat tissue, play a crucial role for the disease. Quite interestingly, a transfer of IgG antibodies from mice with diabetes was sufficient to induce higher glucose levels in B cell-deficient mice, which are resistant to diet-induced obesity and diabetes, suggesting that IgG molecules are also involved in the disease process. Supporting the relevance of these observations for therapy, depletion of B cells with a monoclonal antibody diminished diabetes development in this mouse model system [4]. With respect to multiple sclerosis, several reports were able to show that depletion of B cells greatly impacts disease severity [5–7]. Besides autoantibody production, B cells may act as antigen-presenting cells to stimulate autoreactive T helper cell responses, which in turn may be critical for the generation of high-affinity class-switched autoantibodies or may enhance or maintain autoimmune inflammation by secreting pro-inflammatory cytokines such as IL6 [8]. Moreover, IL10-producing B cells may have an active role in dampening autoimmune disease and hence have been referred to as regulatory B cells [9–11]. Thus, a simple depletion of B cells may not only diminish harmful B cell populations but also this highly regulatory B cell subset. Moreover, the major (auto) antibody-producing B cell population, namely, plasma cells in the bone marrow, may not be easily targeted via cytotoxic antibodies due to the downregulation of many common B cell lineage markers. Thus, alternative strategies aiming at inactivation of the autoantibodies itself or targeting B cells and plasma cells via other approaches will be necessary. One example of such a strategy which shows great preclinical success is the use of the proteasome inhibitor bortezomib [12–15]. Plasma cells, which produce thousands of antibody molecules per second, seem to be especially sensitive to proteasome blockade resulting in cell death and reduction of autoantibody levels. In this review, we will take one step back and summarize preclinical information about two enzymes targeting IgG activity and discuss how they may become useful in the therapy of human autoimmune disease. Moreover, we will provide some insights into novel immunomodulating activities of intravenous immunoglobulins on B cells and how this may interfere with chronic autoantibody production.
Targeting autoantibody-dependent effector functions in autoimmunity
A variety of studies have addressed the molecular and cellular pathways by which autoantibodies especially of the IgG subclass may mediate tissue inflammation and in the worst case organ destruction. The common theme of these results is that activating cellular Fcγ receptors (FcγR) expressed on a wide variety of innate immune effector cells are critical for autoantibody-induced tissue pathology [16–18]. In contrast, autoimmune disease was enhanced in mice deficient in the inhibitory FcγRIIB, suggesting that the integration of positive and negative signals triggered via the binding of immune complexes to both types of FcγR expressed on the same cell may set a threshold for activation [19–23]. The complement system further enhanced autoantibody activity in diseases such as AIHA in an IgG subclass-specific manner [24]. Although the details of the exact pathway remain to be established, it was demonstrated by several groups that an FcγR-dependent release of C5 or C5a independent of early components of the classical complement pathway may have a great impact on tissue inflammation in autoimmune diseases such as inflammatory arthritis and skin blistering diseases [25–30]. In these diseases, FcγR and C5 deficiency protect from autoimmune disease development. As the anaphylatoxin C5a not only recruits innate immune effector cells to the site of inflammation but also upregulates activating FcγR expression; this may represent a positive feedback loop fueling inflammation. In humans, allelic variants of activating FcγRIIA and FcγRIIIA were associated with the development and severity of RA and SLE, and infusion of a FcγRIIIA blocking antibody or inhibitors of Syk activation, which is a crucial component of the signaling pathway of activating FcγR, were able to interfere with platelet depletion in ITP patients [16, 31–33]. Therefore, blocking or interfering with the interaction of autoantibodies with cellular FcγR represents an attractive therapeutic target. Indeed, targeting this Achilles heel of most antibody-dependent effector functions has shown very promising results in experimental model systems and has been achieved by treating animals with two enzymes derived from Streptococcus pyogenes (S. pyogenes) called endoglycosidase S (EndoS) and the IgG-degrading enzyme of S. pyogenes (IdeS). Both proteins selectively inactivate the IgG molecule, albeit through entirely different mechanisms. Whereas EndoS targets the sugar moiety attached to the IgG Fc-fragment, IdeS hydrolyzes the IgG backbone beyond the disulfide bonds in the hinge region, generating a F(ab)2 fragment and two single Fc fragments (Fig. 1) [34–36]. The therapeutic success of these enzymes underscores the critical role of the IgG Fc fragment in mediating the effector functions which are ultimately responsible for tissue inflammation and destruction during autoimmunity. Of note, an interesting species-specific variability of IdeS activity has been noted. Whereas all human and rabbit IgG subclasses are efficiently hydrolyzed, in mice, a selective specificity for the IgG2a/c subclass has been noted, which limits the availability of murine experimental in vivo models of autoimmune diseases [37]. Where possible, however, an impressive suppression of autoantibody-mediated autoimmune disease was noted. Thus, injection of IdeS into rabbits resulted in a very rapid removal of serum IgG within 4–6 h and lasted for about 1 week [38]. In mice, the arthritis incidence induced by the injection of collagen type II-specific IgG2a antibodies was diminished from over 80 % to about 20 % [37]. In active models induced by immunizing mice with collagen type II, a reduction in the severity of arthritis was achieved, and the strength and incidence of chronic relapses usually observed in this model system were reduced. In mouse models of immunothrombocytopenia, induced by the injection of platelet-specific rabbit polyclonal IgG into mice, IdeS injection rescued mice from lethal bleeding and restored platelet counts [38]. In a similar manner, IdeS injection prevented kidney damage in a passive model system in which rabbit antibodies directed against the glomerular basement membrane (GBM) were injected into mice [39]. In mice and humans, anti-GBM antibodies are responsible for Goodpasture’s disease, which is characterized by a ribbon-like deposition of IgG molecules in the glomeruli of the kidney and the lung causing organ inflammation, fibrosis, lung hemorrhage, and ultimately total organ failure if no treatment is initiated [40]. More recently, IdeS was used to inactivate aquaporin-4 (AQP-4)-specific autoantibodies, which are considered to be causative for neuromyelitis optica, an autoimmune disease in which inflammation and demyelination occurs predominantly in the spinal cord and the optical nerve [41, 42]. Consistent with the important role of IgG-Fc-dependent effector mechanisms involved in nerve inflammation and demyelination, IdeS-pretreated AQP-4-specific antibodies were no longer able to demyelinate nerve cells in a mouse model in vivo [42]. Similar results were obtained by injection of IdeS post injection of AQP-4-specific antibodies, suggesting that IdeS may have therapeutic value (Table 1).
Effects of EndoS and IdeS on the IgG molecule. Shown is a schematic view depicting the effect of EndoS and IdeS on the IgG molecule. Whereas EndoS treatment removes the largest part of the sugar moiety, leaving only one residual N-acetylglucosamine residue and one branching fucose residue, incubation with IdeS generates a F(ab)2 fragment and two single Fc fragments as IdeS cleaves the IgG molecule beyond the disulfide bond connecting the two heavy chains
Besides in vivo cleavage of the IgG molecule, the removal of the sugar domain attached to the asparagine 297 residue of each IgG Fc fragment has proven to be quite efficacious in ameliorating a number of autoimmune diseases in in vivo model systems. The general requirement of this sugar domain for IgG activity has been demonstrated by several previous studies using either IgG molecules in which the N297 residue is exchanged for another amino acid, PNGase F-treated antibodies, or by incubating IgG-producing hybridoma cells with tunicamycin, which blocks protein glycosylation [17, 43, 44]. In all of these instances, this resulted in an abrogation of IgG activity in vivo. On a molecular basis, crystal structural analysis of aglycosylated IgG demonstrated that the open conformation of the IgG Fc fragment collapses, which may explain the loss of binding to cellular Fcγ receptors and the complement component C1q [45–50]. In contrast to PNGase F, EndoS removes the sugar moiety not entirely, but spares one N-acteylglucosamine residue with or without a branching fucose residue (Fig. 1) [35]. Unlike IdeS, EndoS is active on all human, mouse, and rabbit IgG subclasses and efficiently cleaves the sugar moiety in vitro and upon EndoS injection into mice and rabbits in vivo. Accordingly, ITP induced by injection of rabbit-derived platelet-specific antibodies into mice was efficiently prevented by EndoS injection under preventive and therapeutic treatment conditions [35]. A similar efficacy of EndoS was noted in a rabbit IgG-mediated model of acute glomerulonephritis in mice, where one injection of EndoS was sufficient to protect the animals from kidney inflammation and organ failure [39]. Further confirming these results, autoantibody-dependent induction of skin blistering diseases such as epidermolysis bullosa acquisita (EBA), which is induced by injection of rabbit anti-collagen type VII antibodies, was abolished by therapeutic EndoS administration [51].
A quite interesting IgG subclass-specific effect of EndoS treatment on the activity of mouse IgG1, IgG2a, and IgG2b switch variants of a platelet-specific antibody was noted in a mouse model of ITP. Whereas both IgG1 and IgG2b subclasses pretreated with EndoS lost their platelet depleting activity in vivo, antibodies of the IgG2a subclass remained fully active [52]. These results were confirmed by others in an independent model of autoantibody-induced hemolytic anemia (AIHA), in which IgG1 but not IgG2a induced red blood cell depletion was ameliorated by EndoS injection [53]. Most interestingly, EndoS treatment not only reduced autoantibody binding to cellular FcγR but also inhibited complement activation and deposition in this model system. With respect to human IgG subclasses, a similar effect was noted for human IgG2 binding to FcγRIIA and FcγRIIB which was either not affected or even enhanced, whereas IgG1, IgG3, and IgG4 binding to FcγR were all strongly reduced in vitro [54]. Consistent with the inactivation of mouse IgG1 and IgG2b subclasses, EndoS treatment was able to ameliorate joint swelling in a passive model of inflammatory arthritis in which IgG1 autoantibodies and FcγRIII play a dominant role [55]. The remaining disease activity in this model may be explained by the concomitant presence of IgG2a autoantibodies, which mediate their activity via FcγRIV and are not inactivated by EndoS treatment [56, 57]. In a similar manner, the SLE-like autoimmune disease, which spontaneously develops in BXSB mice and is dominated by autoantibodies of the IgG2b subclass, responded very well to EndoS therapy as demonstrated by an improved survival despite the presence of high autoantibody levels [52] (Table 1). Quite interestingly, autoantibody specificity seemed to change over time in EndoS-treated mice shifting from a predominant nuclear to a more cytoplasmic staining in some of the long-term surviving animals [52]. This may suggest that the autoantibody response seems to be variable and change over time or that EndoS impacted autoantibody production by B cells. Further studies will be necessary to fully understand these effects on a molecular and cellular level.
Apart from acting on the disease-inducing autoantibody directly, another immunomodulatory activity of EndoS-treated antibodies was noted more recently. Injection of EndoS treated antibodies specific for collagen type II together with untreated CII-specific antibodies prevented the development of inflammatory arthritis [58]. Quite surprisingly, other non-collagen-specific antibodies of different mouse IgG subclasses were also able to suppress arthritis development if they were pretreated with EndoS, arguing against a simple competition mechanism of EndoS-treated and EndoS-untreated antibodies for the target antigen. Indeed, small amounts of EndoS-treated antibodies at a dose 36-fold lower than the untreated disease inducing antibodies were sufficient to block disease development. Moreover, this effect was only observed in a narrow time frame from 3 h before until 3 h after injection of collagen type II-specific antibodies, suggesting that EndoS-treated antibodies may interfere with the phase of autoantibody deposition or immune complex formation in joints [58]. Consistent with this interpretation, less complement activation and C3b deposition was noted in animals receiving EndoS-treated therapeutic antibodies. As we will discuss later, this mechanism is entirely different from the suppression of autoimmune inflammation by polyclonal human IgG preparations (IVIg) injected intravenously at high doses. Here, IgG deglycosylation via PNGase F abrogates the anti-inflammatory activity in vivo.
One obvious question with respect to the potential of these enzymes for treatment of human patients may be their immunogenicity. Indeed, EndoS- and IdeS-specific antibodies were detected in human and rabbit serum [35, 38]. Interestingly, however, this did not result in a loss of activity, indicating that the catalytic site of the respective enzymes is not bound by these antibodies and remains functional. In a similar manner, multiple injections of EndoS into rabbits resulted in an increased level of EndoS-specific antibodies, which again did not result in impaired EndoS activity [35]. Moreover, streptokinase, another enzyme derived from Streptococci is used in the clinic since years to remove blot clots and to prevent or treat acute heart attacks and strokes [59]. Whether a long-term treatment will be possible remains to be established, but at the least, a treatment of acute autoimmune inflammation seems a viable option. Combining IgG inactivation with the depletion of B cells or other target cells involved in tissue damage during autoimmune disease with therapeutic antibodies may be another potentially new therapeutic avenue. This could be either achieved by using therapeutic IgG subclasses which are not inactivated by EndoS, such as IgG2 for example, or by using therapeutic antibodies produced in organisms adding high mannose sugar structures instead of the biantennary sugar moiety found in mammalian cells. Whereas EndoS removes biantennary sugar moieties, it cannot hydrolyze high-mannose structures efficiently, which would enable the parallel use of EndoS and a therapeutic antibody targeting B cells for example [60].
With respect to the transferability of the animal data to human disease and most forward with respect to the potential efficacy of EndoS treatment, two other potential issues should be considered. First, autoantibody responses are rarely restricted to one IgG subclass. Thus, in SLE patients, DNA-specific antibodies of various IgG subclasses have been detected including IgG2, which is not inactivated by EndoS treatment. Taking this into account, one may expect to achieve no complete suppression of autoantibody-mediated inflammation, but rather a reduction as observed in the BXSB model system, which would be a major achievement, nonetheless [52]. Second, a recent study suggests that EndoS-mediated inactivation of human IgG activity may be influenced not only by the IgG subclass, but also by the size of the IgG containing immune complex and the individual FcγR [61]. Previous studies showing that EndoS treatment results in loss of IgG binding investigated the interaction of monomeric IgG with recombinant FcγR. During autoimmune diseases such as SLE for example, rather immune complexes consisting of multiple IgG molecules bound to their target antigen than single IgG molecules are responsible for the pro-inflammatory and tissue destructive activity. By generating different immune complex sizes with human IgG subclasses, it was demonstrated that the size of the immune complex did impact binding to cellular FcγR, with larger complexes showing a better binding and a higher level of pro-inflammatory cytokine release [61]. Of note, even IgG4 immune complexes, supposed to have a very low or even absent binding to human FcγR, were able to bind if present in a large complex. More interestingly, EndoS-treated immune complexes showed a similar behavior. Thus, IgG1, IgG2, and IgG3 immune complexes binding to FcγRIIA were virtually absent in a small complex, but clearly detectable if present in a larger immune complex. Moreover, a FcγR allele-specific contribution was noted in this study, suggesting that the FcγRIIA-131H and FcγRIIIA-158V allele, both shown to be associated with the incidence and severity of autoimmune diseases, may retain their capacity to bind to EndoS-treated IgG1 and IgG3 immune complexes [33, 61]. This potential problem could be easily overcome by a careful selection of patients based on their activating FcγR alleles and by using IdeS in these instances instead. Taken together, both EndoS and IdeS have shown promising therapeutic effects in passively induced and spontaneous complex animal models of autoimmune disease and thus may represent a viable option for the use in human therapy in the future.
Targeting immune homeostasis via polyclonal IgG preparations
The other nondepleting IgG-based therapeutic strategy to treat autoimmune diseases we will discuss is the use of polyclonal IgG preparations pooled from tens of thousands of donors which are infused at high doses intravenously (intravenous IgG therapy or IVIg therapy). This type of therapy is used for autoimmune diseases such as ITP, Kawasaki disease, Guillain-Barre syndrome, chronic inflammatory demyelinating polyneuropathy, and more recently for autoantibody-mediated skin blistering diseases such as epidermolysis bullosa acquisita (EBA) [49, 62–64]. Its off-label use for a variety of autoimmune and inflammatory diseases is quite substantial, and mirroring this widespread use of IVIg preparations are the proposed mechanisms underlying this immunomodulatory activity [65, 66]. We will not be able to cover all these pathways in detail and the interested reader is directed to several excellent recent reviews covering this topic in greater depth [49, 63, 65, 67–69]. Instead, we will exclusively focus on results from human clinical trials [70] and mouse in vivo model systems of autoimmune diseases such as ITP, nephrotoxic nephritis, transfusion-related acute lung injury (TRALI), and inflammatory arthritis, which all suggest that the IgG-Fc fragment is sufficient for the anti-inflammatory and immunomodulatory activity of IVIg [71–75] (Fig. 2). Similar to what we have discussed before with respect to the important function of the N297-attached sugar moiety for pro-inflammatory IgG-dependent effector functions, deglycosylation of IVIg also results in a loss of the anti-inflammatory activity in vivo [73, 76]. More specifically, terminal sialic acid residues were critical for the modulation of FcγR-dependent effector functions in model systems of ITP and inflammatory arthritis [73, 76, 77], whereas IgG glycoforms rich in galactose residues present in immune complexes were able to interfere with complement-dependent tissue inflammation [78]. With respect to the cellular pathway underlying the immunomodulatory activity of IVIg and sialic acid-rich glycoforms within this IgG preparation, myeloid effector and more recently B cells were shown to respond to IVIg infusion in mice and humans in vivo. The majority of studies concentrated on the effect of IVIg on myeloid effector cells, elucidating a quite complex molecular and cellular pathway. In brief, a general outcome of IVIg infusion seems to be an upregulation of the inhibitory FcγRIIB on innate immune effector cells resulting in a higher threshold for activation via immune complexes [71–74, 79]. A series of elegant studies in a model of inflammatory arthritis suggest that mouse splenic macrophages and human myeloid or dendritic cells have the capacity to directly recognize sialic acid-rich IgG glycoforms via SIGNR1 (mice) or DC-SIGN (humans) [77, 80, 81]. This results in the release of IL33, which induces IL4 secretion via basophils, ultimately resulting in an upregulation of FcγRIIB on innate immune effector cells [77, 80–82]. A similar requirement for SIGNR1 was noted in a model of IVIg-mediated amelioration of ITP, although the impact of IL4 and IL33 was less dominant under these rather non-inflammatory conditions [76, 83].
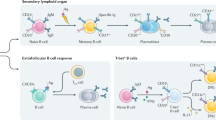
Effects of intravenous immunoglobulins on B cells and innate immune effector cells. Overview of the effects of IVIg infusion on B cells and myeloid innate immune effector cells. In mice and humans, IVIg infusion results in an upregulation of FcγRIIB on B cells and myeloid effector cells. On B cells, this may result in a release of anti-inflammatory cytokines and a lower level of autoantibody production, whereas plasma cells or plasma blasts may become more susceptible for apoptosis induction via immune complexes. On innate immune effector cells, the threshold for cell activation is increased. See text for further details
As this immunodulatory pathway has been covered extensively by recent reviews, we will focus our attention on the recent observation that IVIg infusion may have a direct impact on B cells via upregulation of FcγRIIB [79, 84]. To do so, we first have to provide some background about the physiological role of this inhibitory FcγR on B cells. In contrast to cells of the innate immune system, B cells solely express the FcγRIIB, which counterbalances activating signals transduced via the B cell receptor. Lack of FcγRIIB expression or function results in loss of humoral tolerance in mice and to a SLE-like autoimmune disease on susceptible genetic backgrounds in mice and humans [17, 21, 85–89]. Autoimmune-prone mouse strains including NOD, BXSB, and NZBW are characterized by a polymorphism in the FcγRIIB promoter, resulting in a lower level of expression on B cells and innate immune effector cells, the loss of humoral tolerance, and an increased level of plasma blasts and plasma cells [90, 91]. Restoring FcγRIIB expression either ubiquitously or selectively on B cells restored humoral tolerance in these mouse strains and ameliorated the autoimmune phenotype, arguing for a major gatekeeper function of FcγRIIB to prevent the production of autoantibodies and the initiation of autoimmune disease [92, 93]. In a similar manner, human SLE and CIDP patients were demonstrated to express lower levels of FcγRIIB on B cells and myeloid cells [79, 94, 95]. More interestingly, a failure of FcγRIIB upregulation was noted on memory B cells, which together with plasma cells and plasma blasts normally show an increased level of FcγRIIB expression compared to mature B cells. Further along these lines, either FCGR2B promoter polymorphisms or allelic variants of the receptor in which an isoleucine at position 232 in the transmembrane domain is exchanged for a threonine residue (FcγRIIB-I232T variant) were shown to be associated with the development or severity of autoimmune diseases including SLE and rheumatoid arthritis [89, 95–97]. The exchange of the isoleucine residue for threonine results in a defective association of the receptor with lipid rafts and a diminished signaling function. Indeed, a recent study using a humanized mouse model, in which immunodeficient mouse strains were reconstituted with human hematopoietic stem cells derived from donors carrying the functionally defect FcγRIIB-I232T allele, could demonstrate that the human immune system developing in these animals was affected by the presence of this allelic variant [98]. For example, animals carrying the FcγRIIB-232T variant in a homozygous fashion had a higher amount of memory B cells and plasma cells, consistent with earlier studies in mouse model systems. Moreover, these animals produced autoantibodies directed against double-stranded DNA and citrullinated proteins, strongly arguing for an important function of FcγRIIB as a gatekeeper of humoral tolerance in mice and humans.
Apart from this negative regulation of signals delivered via the BCR, FcγRIIB was also suggested to be involved in plasma cell survival, providing a possible explanation for the increased level of plasma cells, which was noted in autoimmune-prone mouse strains [99]. A potential mechanism underlying this phenomenon was provided by several studies showing that isolated triggering of FcγRIIB on B cells in the absence of a concomitant activating signal provided by the B cell receptor induced apoptosis. On plasma cells and plasma blasts, the B cell receptor is expressed either at very low levels or not at all, whereas FcγRIIB is becoming even upregulated. Thus, immune complexes, which are present at enhanced levels during an infection (or an active autoimmune disease) may feedback on the antibody-producing plasma cell by inducing apoptosis. This mechanism has been suggested to be at least one explanation for the establishment of a broad variety of plasma cells producing antibodies for a wide variety of pathogens, by opening up survival niches for newly generated plasma cells. With respect to the lower level of FcγRIIB expression on memory B cells and plasma cells in mice and humans with autoimmune diseases, this may indicate that these autoantibody-producing cells escape this feedback loop, allowing a long-term survival of these cells once they have reached their niches either in the bone marrow or, as described by several groups for autoimmune diseases such as SLE or arthritis, in peripheral tissues such as the joint or the kidney.
Taken together these results suggest that restoring FcγRIIB expression levels may be of therapeutic value. Quite interestingly, it was noted that infusion of IVIg into mice and humans not only upregulates FcγRIIB on innate immune effector cells, thereby raising their threshold for activation by immune complexes, but also on B cells [79, 84]. Taking into account the important role of FcγRIIB for B cell activation and plasma cell survival, this may restore a balanced B cell response, reduce the production of autoantibodies and allow the removal of autoantibody-producing plasma cells by circulating immune complexes. As neither SIGNR1 nor DC-SIGN are expressed on B cells and sialic acid-rich IgG glycoforms have a reduced affinity for FcγRIIB, two non-mutually exclusive mechanisms seem possible. First, FcγRIIB upregulation on B cells may be induced indirectly via cytokines, for example. As IL4, however, while upregulating FcγRIIB on myeloid cells, rather results in a downmodulation of this receptor on B cells it seems unlikely that the recently described Th2 pathway is involved in modulating FcγR expression on B cells. Second, IVIg may directly bind to cell surface molecules on B cells. Evidence for the latter scenario was obtained by two recent studies showing that IVIg can indeed bind to human and mouse B cells [100, 101]. More interestingly, also sialic acid-enriched IVIg glycovariants bound to human B cells, suggesting that a receptor for this IgG glycovariant is indeed present on B cells. An obvious candidate molecule which may have this capacity is CD22, which belongs to the family of Siglec proteins and has been shown to be able to recognize sialic acid containing sugar moieties [102]. Consistently, a co-staining of bound sialic acid-rich IVIg showed significant overlaps with the localization of CD22 on the surface of B cells and CD22 co-immunoprecipitated with IVIg [101]. Further functional studies performed with human tonsillar B cells in vitro revealed that either the intact IVIg molecule or the sialic acid-rich glycovariants, but not the IVIg F(ab)2 fragment or the sialic acid-depleted IVIg fraction, were able to reduce B cell survival and to modulate B cell receptor signaling. Thus, compared to triggering BCR signaling alone, phosphorylation of CD19, Lyn, BLNK, and PLCγ were all reduced by co-incubation with IVIg or sialic acid-rich IVIg, but not if the sialic acid-negative IVIg fraction was used. A conceptual concern remaining with these results is that CD22 usually is occupied by sialic acid residues abundantly present on other molecules expressed on the B cells (most notably CD22 itself and the B cell receptor) [103]. Thus, normally, a neuraminidase treatment is required first to remove these ligands before CD22 can bind to exogenous sialic acid containing sugar residues. Indeed, a study performed with CD22-deficient mice demonstrated that IVIg is still able to bind to B cells [100].
More recently, yet another cell surface molecule expressed on B cells, known as the low-affinity receptor for IgE or CD23, was identified to have the capacity to bind to sialic acid-rich IgG [82]. CD23 belongs to the family of calcium-dependent C-type lectins and has been shown to have an important role for the negative feedback regulation of IgE on B cells [104]. The crystal structure of IgE in complex with CD23 suggests that upon binding of two CD23 molecules to the IgE Cε3Cε4 domain, the rather flexible conformation of the Cε3 domain acquires a closed structure preventing a further interaction with the high-affinity FcεRI [105]. Despite being a C-type lectin, the binding of CD23 to IgE seemed not to involve IgE glycosylation sites and solely represented a protein-protein interaction. A similar mode of binding was proposed to be relevant for the interaction of sialic acid-rich IgG to SIGNR1, where sialic acid was essential for SIGNR1 binding to IgG. Importantly, SIGNR1 would not interact directly with the sugar residue but rather with the IgG amino acid backbone. Indeed, biophysical data suggest that sialic acid-rich IgG may have an altered structure, although a recent crystal structure obtained with sialic acid-rich IgG did not show major structural alterations [106]. Regardless of these open questions concerning the impact of sialic acid on IgG structure, it was demonstrated that sialic acid-rich IgG glycovariants acquire the capacity to bind to CD23 expressed on CHO cells. Thus, sialic acid-rich IgG binding to CD23 on B cells may be involved in modulating the B cell response. It would be especially interesting to study if CD23 is involved in the upregulation of the inhibitory FcγRIIB, which has been observed in mouse and human B cells as discussed before.
Apart from modulating the humoral immune response, IVIg binding to B cells may also have an indirect effect on autoantibody activity. Given the potency of B cells to downmodulate autoimmune diseases such as EAE via secretion of IL10, one could envisage a scenario where the B cell-dependent release of anti-inflammatory cytokines may be responsible for the changes in activating and inhibitory FcγR expression observed in several models of autoimmune disease. Arguing against this scenario, two studies performed in B cell-deficient mice showed that IVIg was still able to ameliorate ITP and inflammatory arthritis [71, 100]. Although more experiments in other model systems may be necessary to fully exclude a function of B cells, the current data suggest that B cells or B cell-derived cytokines may not be involved in the immediate anti-inflammatory and immunomodulatory activity of IVIg acting on innate immune effector cells.
Conclusions and outlook
Work over the last 10 years has provided convincing evidence that B cells and autoantibodies of the IgG isotype play a very active role in autoimmune diseases including SLE, MS, RA, CIDP, ITP, AIHA, and IPEX. It seems quite likely that further autoimmune diseases will be added to this list in the future, emphasizing that B cells and antibodies represent important therapeutic targets. Apart from simply depleting B cells via monoclonal antibodies, other more selective and less immunosuppressive therapeutic options have become available. This includes enzymes such as EndoS and IdeS, which leave the B cell compartment intact but inactivate IgG function via deglycosylating or cleaving the IgG-Fc fragment. More recently, an impact of IVIg on B cells was noted which may allow achieving long-term effects by resetting the threshold for B cell activation and thereby halting the production of cross-reactive and/or autoreactive antibodies. As a continuous treatment with bacterial enzymes will result in an antibody response of the host, which may at some point prevent a further use, a combination therapy of EndoS or IdeS as first-line treatments to stop the destructive activity of autoantibodies, followed by the use of intravenous immunoglobulins to achieve a reduction in autoantibody production or B cell depletion via cytotoxic antibodies, may be promising therapeutic avenues. Taken together, the armament of therapeutic options to interfere with autoimmune inflammation is increasing and hopefully will lead to a better management of these devastating diseases in the near future.
References
Wahren-Herlenius M, Dorner T (2013) Immunopathogenic mechanisms of systemic autoimmune disease. Lancet 382(9894):819–831
Wardemann H, Nussenzweig MC (2007) B-cell self-tolerance in humans. Adv Immunol 95:83–110
Anolik JH (2013) B cell biology: implications for treatment of systemic lupus erythematosus. Lupus 22(4):342–349
Winer DA, Winer S, Shen L, Wadia PP, Yantha J, Paltser G et al (2011) B cells promote insulin resistance through modulation of T cells and production of pathogenic IgG antibodies. Nat Med 17(5):610–617
Bar-Or A, Calabresi PA, Arnold D, Markowitz C, Shafer S, Kasper LH et al (2008) Rituximab in relapsing-remitting multiple sclerosis: a 72-week, open-label, phase I trial. Ann Neurol 63(3):395–400
Hauser SL, Waubant E, Arnold DL, Vollmer T, Antel J, Fox RJ et al (2008) B-cell depletion with rituximab in relapsing-remitting multiple sclerosis. N Engl J Med 358(7):676–688
Matsushita T, Yanaba K, Bouaziz JD, Fujimoto M, Tedder TF (2008) Regulatory B cells inhibit EAE initiation in mice while other B cells promote disease progression. J Clin Invest 118(10):3420–3430
Barr TA, Shen P, Brown S, Lampropoulou V, Roch T, Lawrie S et al (2012) B cell depletion therapy ameliorates autoimmune disease through ablation of IL-6-producing B cells. J Exp Med 209(5):1001–1010
Fillatreau S, Gray D, Anderton SM (2008) Not always the bad guys: B cells as regulators of autoimmune pathology. Nat Rev Immunol 8(5):391–397
Mauri C, Bosma A (2012) Immune regulatory function of B cells. Annu Rev Immunol 30:221–241
DiLillo DJ, Matsushita T, Tedder TF (2010) B10 cells and regulatory B cells balance immune responses during inflammation, autoimmunity, and cancer. Ann N Y Acad Sci 1183:38–57
Hainz N, Thomas S, Neubert K, Meister S, Benz K, Rauh M et al (2012) The proteasome inhibitor bortezomib prevents lupus nephritis in the NZB/W F1 mouse model by preservation of glomerular and tubulointerstitial architecture. Nephron Exp Nephrol 120(2):e47–e58
Maseda D, Meister S, Neubert K, Herrmann M, Voll RE (2008) Proteasome inhibition drastically but reversibly impairs murine lymphocyte development. Cell Death Differ 15(3):600–612
Neubert K, Meister S, Moser K, Weisel F, Maseda D, Amann K et al (2008) The proteasome inhibitor bortezomib depletes plasma cells and protects mice with lupus-like disease from nephritis. Nat Med 14(7):748–755
Gomez AM, Willcox N, Molenaar PC, Buurman W, Martinez-Martinez P, De Baets MH et al (2012) Targeting plasma cells with proteasome inhibitors: possible roles in treating myasthenia gravis? Ann N Y Acad Sci 1274:48–59
Hogarth PM (2002) Fc receptors are major mediators of antibody based inflammation in autoimmunity. Curr Opin Immunol 14(6):798–802
Nimmerjahn F, Ravetch JV (2008) Fc gamma receptors as regulators of immune responses. Nat Rev Immunol 8(1):34–47
Takai T (2002) Roles of Fc receptors in autoimmunity. Nat Rev Immunol 2(8):580–592
Baerenwaldt A, Nimmerjahn F (2008) Immune regulation—Fc gamma RIIB—regulating the balance between protective and autoreactive immune responses. Immunol Cell Biol 86(6):482–484
Bolland S, Ravetch JV (1999) Inhibitory pathways triggered by ITIM-containing receptors. Adv Immunol 72:149–177
Bolland S, Yim YS, Tus K, Wakeland EK, Ravetch JV (2002) Genetic modifiers of systemic lupus erythematosus in FcgammaRIIB(−/−) mice. J Exp Med 195(9):1167–1174
Daeron M, Lesourne R (2006) Negative signaling in Fc receptor complexes. Adv Immunol 89:39–86
Nimmerjahn F, Ravetch JV (2010) Antibody-mediated modulation of immune responses. Immunol Rev 236:265–275
Azeredo da Silveira S, Kikuchi S, Fossati-Jimack L, Moll T, Saito T, Verbeek JS et al (2002) Complement activation selectively potentiates the pathogenicity of the IgG2b and IgG3 isotypes of a high affinity anti-erythrocyte autoantibody. J Exp Med 195(6):665–672
Mihai S, Nimmerjahn F (2013) The role of Fc receptors and complement in autoimmunity. Autoimmun Rev 12(6):657–660
Banda NK, Hyatt S, Antonioli AH, White JT, Glogowska M, Takahashi K et al (2012) Role of C3a receptors, C5a receptors, and complement protein C6 deficiency in collagen antibody-induced arthritis in mice. J Immunol 188(3):1469–1478
Baumann U, Kohl J, Tschernig T, Schwerter-Strumpf K, Verbeek JS, Schmidt RE et al (2000) A codominant role of Fc gamma RI/III and C5aR in the reverse Arthus reaction. J Immunol 164(2):1065–1070
Shushakova N, Skokowa J, Schulman J, Baumann U, Zwirner J, Schmidt RE et al (2002) C5a anaphylatoxin is a major regulator of activating versus inhibitory FcgammaRs in immune complex-induced lung disease. J Clin Invest 110(12):1823–1830
Skokowa J, Ali SR, Felda O, Kumar V, Konrad S, Shushakova N et al (2005) Macrophages induce the inflammatory response in the pulmonary Arthus reaction through G alpha i2 activation that controls C5aR and Fc receptor cooperation. J Immunol 174(5):3041–3050
Syed SN, Konrad S, Wiege K, Nieswandt B, Nimmerjahn F, Schmidt RE et al (2009) Both FcgammaRIV and FcgammaRIII are essential receptors mediating type II and type III autoimmune responses via FcRgamma-LAT-dependent generation of C5a. Eur J Immunol 39(12):3343–3356
Podolanczuk A, Lazarus AH, Crow AR, Grossbard E, Bussel JB (2009) Of mice and men: an open-label pilot study for treatment of immune thrombocytopenic purpura by an inhibitor of Syk. Blood 113(14):3154–3160
Clarkson SB, Kimberly RP, Valinsky JE, Witmer MD, Bussel JB, Nachman RL et al (1986) Blockade of clearance of immune complexes by an anti-Fc gamma receptor monoclonal antibody. J Exp Med 164(2):474–489
Nimmerjahn F (2006) Activating and inhibitory FcgammaRs in autoimmune disorders. Springer Semin Immunopathol 28(4):305–319
Ryan MH, Petrone D, Nemeth JF, Barnathan E, Bjorck L, Jordan RE (2008) Proteolysis of purified IgGs by human and bacterial enzymes in vitro and the detection of specific proteolytic fragments of endogenous IgG in rheumatoid synovial fluid. Mol Immunol 45(7):1837–1846
Collin M, Shannon O, Bjorck L (2008) IgG glycan hydrolysis by a bacterial enzyme as a therapy against autoimmune conditions. Proc Natl Acad Sci USA 105(11):4265–4270
Collin M, Olsen A (2001) EndoS, a novel secreted protein from Streptococcus pyogenes with endoglycosidase activity on human IgG. EMBO J 20(12):3046–3055
Nandakumar KS, Johansson BP, Bjorck L, Holmdahl R (2007) Blocking of experimental arthritis by cleavage of IgG antibodies in vivo. Arthritis Rheum 56(10):3253–3260
Johansson BP, Shannon O, Bjorck L (2008) IdeS: a bacterial proteolytic enzyme with therapeutic potential. PLoS One 3(2):e1692
Yang R, Otten MA, Hellmark T, Collin M, Bjorck L, Zhao MH et al (2010) Successful treatment of experimental glomerulonephritis with IdeS and EndoS, IgG-degrading streptococcal enzymes. Nephrol Dial Transplant 25(8):2479–2486
Salama AD, Levy JB, Lightstone L, Pusey CD (2001) Goodpasture’s disease. Lancet 358(9285):917–920
Wingerchuk DM, Lennon VA, Lucchinetti CF, Pittock SJ, Weinshenker BG (2007) The spectrum of neuromyelitis optica. Lancet Neurol 6(9):805–815
Tradtrantip L, Asavapanumas N, Verkman AS (2013) Therapeutic cleavage of anti-aquaporin-4 autoantibody in neuromyelitis optica by an IgG-selective proteinase. Mol Pharmacol 83(6):1268–1275
Arnold JN, Wormald MR, Sim RB, Rudd PM, Dwek RA (2007) The impact of glycosylation on the biological function and structure of human immunoglobulins. Annu Rev Immunol 25:21–50
Nose M, Wigzell H (1983) Biological significance of carbohydrate chains on monoclonal antibodies. Proc Natl Acad Sci USA 80(21):6632–6636
Feige MJ, Nath S, Catharino SR, Weinfurtner D, Steinbacher S, Buchner J (2009) Structure of the murine unglycosylated IgG1 Fc fragment. J Mol Biol 391(3):599–608
Ghirlando R, Lund J, Goodall M, Jefferis R (1999) Glycosylation of human IgG-Fc: influences on structure revealed by differential scanning micro-calorimetry. Immunol Lett 68(1):47–52
Sondermann P, Huber R, Oosthuizen V, Jacob U (2000) The 3.2-A crystal structure of the human IgG1 Fc fragment-Fc gammaRIII complex. Nature 406(6793):267–273
Radaev S, Motyka S, Fridman WH, Sautes-Fridman C, Sun PD (2001) The structure of a human type III Fcgamma receptor in complex with Fc. J Biol Chem 276(19):16469–16477
Schwab I, Nimmerjahn F (2013) Intravenous immunoglobulin therapy: how does IgG modulate the immune system? Nat Rev Immunol 13(3):176–189
Leatherbarrow RJ, Rademacher TW, Dwek RA, Woof JM, Clark A, Burton DR et al (1985) Effector functions of a monoclonal aglycosylated mouse IgG2a: binding and activation of complement component C1 and interaction with human monocyte Fc receptor. Mol Immunol 22(4):407–415
Hirose M, Vafia K, Kalies K, Groth S, Westermann J, Zillikens D et al (2012) Enzymatic autoantibody glycan hydrolysis alleviates autoimmunity against type VII collagen. J Autoimmun 39(4):304–314
Albert H, Collin M, Dudziak D, Ravetch JV, Nimmerjahn F (2008) In vivo enzymatic modulation of IgG glycosylation inhibits autoimmune disease in an IgG subclass-dependent manner. Proc Natl Acad Sci USA 105(39):15005–15009
Allhorn M, Briceno JG, Baudino L, Lood C, Olsson ML, Izui S et al (2010) The IgG-specific endoglycosidase EndoS inhibits both cellular and complement-mediated autoimmune hemolysis. Blood 115(24):5080–5088
Allhorn M, Olin AI, Nimmerjahn F, Collin M (2008) Human IgG/Fc gamma R interactions are modulated by streptococcal IgG glycan hydrolysis. PLoS One 3(1):e1413
Ji H, Ohmura K, Mahmood U, Lee DM, Hofhuis FM, Boackle SA et al (2002) Arthritis critically dependent on innate immune system players. Immunity 16(2):157–168
Nimmerjahn F, Lux A, Albert H, Woigk M, Lehmann C, Dudziak D et al (2010) FcgammaRIV deletion reveals its central role for IgG2a and IgG2b activity in vivo. Proc Natl Acad Sci USA 107(45):19396–19401
Seeling M, Hillenhoff U, David JP, Schett G, Tuckermann J, Lux A et al (2013) Inflammatory monocytes and Fcgamma receptor IV on osteoclasts are critical for bone destruction during inflammatory arthritis in mice. Proc Natl Acad Sci USA 110(26):10729–10734
Nandakumar KS, Collin M, Happonen KE, Croxford AM, Lundstrom SL, Zubarev RA et al (2013) Dominant suppression of inflammation by glycan-hydrolyzed IgG. Proc Natl Acad Sci USA 110(25):10252–10257
Lippi G, Mattiuzzi C, Favaloro EJ (2013) Novel and emerging therapies: thrombus-targeted fibrinolysis. Semin Thromb Hemost 39(1):48–58
Baruah K, Bowden TA, Krishna BA, Dwek RA, Crispin M, Scanlan CN (2012) Selective deactivation of serum IgG: a general strategy for the enhancement of monoclonal antibody receptor interactions. J Mol Biol 420(1–2):1–7
Lux A, Yu X, Scanlan CN, Nimmerjahn F (2013) Impact of immune complex size and glycosylation on IgG binding to human FcgammaRs. J Immunol 190(8):4315–4323
Ballow M (2011) The IgG molecule as a biological immune response modifier: mechanisms of action of intravenous immune serum globulin in autoimmune and inflammatory disorders. J Allergy Clin Immunol 127(2):315–323, quiz 24–5
Bayry J, Negi VS, Kaveri SV (2011) Intravenous immunoglobulin therapy in rheumatic diseases. Nat Rev Rheumatol 7(6):349–359
Imbach P (2012) Treatment of immune thrombocytopenia with intravenous immunoglobulin and insights for other diseases. A historical review. Swiss Med Wkly 142:w13593
Negi VS, Elluru S, Siberil S, Graff-Dubois S, Mouthon L, Kazatchkine MD et al (2007) Intravenous immunoglobulin: an update on the clinical use and mechanisms of action. J Clin Immunol 27(3):233–245
Nimmerjahn F, Ravetch JV (2008) Anti-inflammatory actions of intravenous immunoglobulin. Annu Rev Immunol 26:513–533
Crow AR, Brinc D, Lazarus AH (2009) New insight into the mechanism of action of IVIg: the role of dendritic cells. J Thromb Haemost 7(Suppl 1):245–248
Crow AR, Song S, Siragam V, Lazarus AH (2006) Mechanisms of action of intravenous immunoglobulin in the treatment of immune thrombocytopenia. Pediatr Blood Cancer 47(5 Suppl):710–713
Kazatchkine MD, Kaveri SV (2001) Immunomodulation of autoimmune and inflammatory diseases with intravenous immune globulin. N Engl J Med 345(10):747–755
Debre M, Bonnet MC, Fridman WH, Carosella E, Philippe N, Reinert P et al (1993) Infusion of Fc gamma fragments for treatment of children with acute immune thrombocytopenic purpura. Lancet 342(8877):945–949
Bruhns P, Samuelsson A, Pollard JW, Ravetch JV (2003) Colony-stimulating factor-1-dependent macrophages are responsible for IVIG protection in antibody-induced autoimmune disease. Immunity 18(4):573–581
Kaneko Y, Nimmerjahn F, Madaio MP, Ravetch JV (2006) Pathology and protection in nephrotoxic nephritis is determined by selective engagement of specific Fc receptors. J Exp Med 203(3):789–797, Epub 2006 Mar 6
Kaneko Y, Nimmerjahn F, Ravetch JV (2006) Anti-inflammatory activity of immunoglobulin G resulting from Fc sialylation. Science 313(5787):670–673
Samuelsson A, Towers TL, Ravetch JV (2001) Anti-inflammatory activity of IVIG mediated through the inhibitory Fc receptor. Science 291(5503):484–486
Semple JW, Kim M, Hou J, McVey M, Lee YJ, Tabuchi A et al (2012) Intravenous immunoglobulin prevents murine antibody-mediated acute lung injury at the level of neutrophil reactive oxygen species (ROS) production. PLoS One 7(2):e31357
Schwab I, Biburger M, Kronke G, Schett G, Nimmerjahn F (2012) IVIg-mediated amelioration of ITP in mice is dependent on sialic acid and SIGNR1. Eur J Immunol 42(4):826–830
Anthony RM, Nimmerjahn F, Ashline DJ, Reinhold VN, Paulson JC, Ravetch JV (2008) Recapitulation of IVIG anti-inflammatory activity with a recombinant IgG Fc. Science 320(5874):373–376
Karsten CM, Pandey MK, Figge J, Kilchenstein R, Taylor PR, Rosas M et al (2012) Anti-inflammatory activity of IgG1 mediated by Fc galactosylation and association of FcgammaRIIB and dectin-1. Nat Med 18(9):1401–1406
Tackenberg B, Jelcic I, Baerenwaldt A, Oertel WH, Sommer N, Nimmerjahn F et al (2009) Impaired inhibitory Fcgamma receptor IIB expression on B cells in chronic inflammatory demyelinating polyneuropathy. Proc Natl Acad Sci USA 106(12):4788–4792
Anthony RM, Kobayashi T, Wermeling F, Ravetch JV (2011) Intravenous gammaglobulin suppresses inflammation through a novel T(H)2 pathway. Nature 475(7354):110–113
Anthony RM, Wermeling F, Karlsson MC, Ravetch JV (2008) Identification of a receptor required for the anti-inflammatory activity of IVIG. Proc Natl Acad Sci USA 105(50):19571–19578
Sondermann P, Pincetic A, Maamary J, Lammens K, Ravetch JV (2013) General mechanism for modulating immunoglobulin effector function. Proc Natl Acad Sci USA 110(24):9868–9872
Crow AR, Song S, Semple JW, Freedman J, Lazarus AH (2007) A role for IL-1 receptor antagonist or other cytokines in the acute therapeutic effects of IVIg? Blood 109(1):155–158
Nikolova KA, Tchorbanov AI, Djoumerska-Alexieva IK, Nikolova M, Vassilev TL (2009) Intravenous immunoglobulin up-regulates the expression of the inhibitory FcgammaIIB receptor on B cells. Immunol Cell Biol 87(7):529–533
Bolland S, Ravetch JV (2000) Spontaneous autoimmune disease in Fc(gamma)RIIB-deficient mice results from strain-specific epistasis. Immunity 13(2):277–285
Boross P, Arandhara VL, Martin-Ramirez J, Santiago-Raber ML, Carlucci F, Flierman R et al (2011) The inhibiting Fc receptor for IgG, FcgammaRIIB, is a modifier of autoimmune susceptibility. J Immunol 187(3):1304–1313
Takai T, Ono M, Hikida M, Ohmori H, Ravetch JV (1996) Augmented humoral and anaphylactic responses in Fc gamma RII-deficient mice. Nature 379(6563):346–349
Willcocks LC, Smith KG, Clatworthy MR (2009) Low-affinity Fcgamma receptors, autoimmunity and infection. Expert Rev Mol Med 11:e24
Willcocks LC, Carr EJ, Niederer HA, Rayner TF, Williams TN, Yang W et al (2010) A defunctioning polymorphism in FCGR2B is associated with protection against malaria but susceptibility to systemic lupus erythematosus. Proc Natl Acad Sci USA 107(17):7881–7885
Espeli M, Clatworthy MR, Bokers S, Lawlor KE, Cutler AJ, Kontgen F, et al. (2012) Analysis of a wild mouse promoter variant reveals a novel role for FcgammaRIIb in the control of the germinal center and autoimmunity. J Exp Med 209(12):2307–2319
Pritchard NR, Cutler AJ, Uribe S, Chadban SJ, Morley BJ, Smith KG (2000) Autoimmune-prone mice share a promoter haplotype associated with reduced expression and function of the Fc receptor FcgammaRII. Curr Biol 10(4):227–230
McGaha TL, Sorrentino B, Ravetch JV (2005) Restoration of tolerance in lupus by targeted inhibitory receptor expression. Science 307(5709):590–593
Brownlie RJ, Lawlor KE, Niederer HA, Cutler AJ, Xiang Z, Clatworthy MR et al (2008) Distinct cell-specific control of autoimmunity and infection by FcgammaRIIb. J Exp Med 205(4):883–895
Mackay M, Stanevsky A, Wang T, Aranow C, Li M, Koenig S et al (2006) Selective dysregulation of the FcgammaIIB receptor on memory B cells in SLE. J Exp Med 203(9):2157–2164
Clatworthy MR, Willcocks L, Urban B, Langhorne J, Williams TN, Peshu N et al (2007) Systemic lupus erythematosus-associated defects in the inhibitory receptor FcgammaRIIb reduce susceptibility to malaria. Proc Natl Acad Sci USA 104(17):7169–7174
Kono H, Kyogoku C, Suzuki T, Tsuchiya N, Honda H, Yamamoto K et al (2005) FcgammaRIIB Ile232Thr transmembrane polymorphism associated with human systemic lupus erythematosus decreases affinity to lipid rafts and attenuates inhibitory effects on B cell receptor signaling. Hum Mol Genet 14(19):2881–2892, Epub 005 Aug 22
Waisberg M, Tarasenko T, Vickers BK, Scott BL, Willcocks LC, Molina-Cruz A et al (2011) Genetic susceptibility to systemic lupus erythematosus protects against cerebral malaria in mice. Proc Natl Acad Sci USA 108(3):1122–1127
Baerenwaldt A, Lux A, Danzer H, Spriewald BM, Ullrich E, Heidkamp G, et al. (2011) Fcgamma receptor IIB (FcgammaRIIB) maintains humoral tolerance in the human immune system in vivo. Proc Natl Acad Sci USA 108(46):18772–18777
Xiang Z, Cutler AJ, Brownlie RJ, Fairfax K, Lawlor KE, Severinson E et al (2007) FcgammaRIIb controls bone marrow plasma cell persistence and apoptosis. Nat Immunol 8(4):419–429
Schwab I, Seeling M, Biburger M, Aschermann S, Nitschke L, Nimmerjahn F (2012) B-cells and CD22 are dispensable for the immediate antiinflammatory activity of intravenous immunoglobulins in vivo. Eur J Immunol 42(12):3302–3309
Seite JF, Cornec D, Renaudineau Y, Youinou P, Mageed RA, Hillion S (2010) IVIg modulates BCR signaling through CD22 and promotes apoptosis in mature human B lymphocytes. Blood 116(10):1698–1704
Nitschke L (2009) CD22 and Siglec-G: B-cell inhibitory receptors with distinct functions. Immunol Rev 230(1):128–143
Nitschke L (2005) The role of CD22 and other inhibitory co-receptors in B-cell activation. Curr Opin Immunol 17(3):290–297
Heyman B (2000) Regulation of antibody responses via antibodies, complement, and Fc receptors. Annu Rev Immunol 18:709–737
Dhaliwal B, Yuan D, Pang MO, Henry AJ, Cain K, Oxbrow A et al (2012) Crystal structure of IgE bound to its B-cell receptor CD23 reveals a mechanism of reciprocal allosteric inhibition with high affinity receptor FcepsilonRI. Proc Natl Acad Sci USA 109(31):12686–12691
Crispin M, Yu X, Bowden TA (2013) Crystal structure of sialylated IgG Fc: Implications for the mechanism of intravenous immunoglobulin therapy. Proc Natl Acad Sci USA 110(38):E3544–E3546
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is a contribution to the special issue on B cell-mediated autoimmune diseases - Guest Editors: Thomas Winkler and Reinhard Voll
Rights and permissions
About this article
Cite this article
Kao, D., Lux, A., Schwab, I. et al. Targeting B cells and autoantibodies in the therapy of autoimmune diseases. Semin Immunopathol 36, 289–299 (2014). https://doi.org/10.1007/s00281-014-0427-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00281-014-0427-7