Abstract
Recent studies have renewed the interest on the potential role that neutrophils play in the development of systemic lupus erythematosus (SLE) and other autoimmune conditions. A distinct subset of proinflammatory, low-density granulocytes (LDGs) isolated from the peripheral blood mononuclear cell fractions of patients with SLE has been described. While the origin and role of LDGs needs to be fully characterized, there is evidence that these cells may contribute to lupus pathogenesis and to the development of end-organ damage through heightened proinflammatory responses, altered phagocytic capacity, enhanced ability to synthesize type I interferons, and to kill endothelial cells. Furthermore, these cells readily form neutrophil extracellular traps, a phenomenon that may promote autoantigen externalization and organ damage. This review examines the biology and potential origin of LDGs, describes the ultrastructural characteristics of these cells, and discusses their putative pathogenic role in systemic autoimmune diseases.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
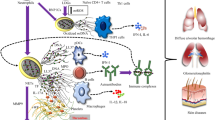
Neutrophils and the pathogenesis of systemic lupus erythematosus
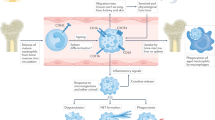
Neutrophils, the most abundant white blood cells in humans, play crucial roles as sentinels and first line of defense against pathogens. Neutrophils are short-lived non-mitotic cells that produce a variety of proinflammatory molecules that are important for the initiation and amplification of inflammatory reactions; their deployment is, therefore, tightly controlled to minimize organ damage [1]. Neutrophils mature in the bone marrow and are released into the bloodstream when terminally differentiated [2].
While aberrant neutrophil responses have been described in a variety of chronic inflammatory and autoimmune conditions, the role that neutrophils play in systemic lupus erythematosus (SLE) was, until recently, less clear. Classically, SLE is described as a systemic autoimmune syndrome characterized by the production of immune complexes and autoantibodies to various nuclear antigens [3]. Lupus follows a chronic course where subclinical autoimmunity precedes the development of overt clinical manifestations secondary to immune-mediated tissue damage [4]. Accelerated atherosclerosis is also a prominent feature in SLE and represents a common cause of morbidity and mortality [5]. SLE has typically been considered a disease of abnormal adaptive immunity, where clearly both B and T lymphocytes play prominent pathogenic roles [6, 7]. However, evidence over the last few decades has also clearly implicated abnormal innate immune responses (particularly a prominent role for type I interferons (IFNs)) in the development of autoimmunity and organ damage in this disease [8–11]. More recently, several groups have proposed novel roles for neutrophil responses in the development of loss of tolerance and organ damage in SLE.
Lupus neutrophils have been reported to have altered functional properties, including diminished phagocytic capabilities, increased aggregation, and intravascular activation [12–16]. Furthermore, depletion of neutrophils can protect against antibody-mediated glomerulonephritis, which supports a role for these cells in the progression of autoimmune responses and organ damage in SLE [17]. However, previous studies did not systematically analyze neutrophil subsets with regards to differences in pathogenicity or function.
Isolation and characterization of low-density granulocytes in lupus
In 1986, Hacbarth and Kajdacsy-Balla were the first to describe the presence of what they called “low-buoyant-density granulocytes,” which were detected in peripheral blood mononuclear cell (PBMC) preparations obtained from adult SLE patients [18]. The presence of this low buoyancy subset correlated with disease activity, and this group proposed that humoral factors present in the plasma of lupus patients may be responsible for this phenotype [18]. In 2003, Bennett et al. performed microarray analysis of blood mononuclear cells isolated by density gradient from pediatric lupus patients and identified high expression of neutrophil-specific genes. They proposed that this signature was the result of immature neutrophils present in the PBMC fractions of these patients [10]. These observations were followed by a publication by Nakou et al., which demonstrated that gene arrays performed in bone marrows from adult SLE patients also revealed upregulation of granulopoiesis-related genes associated with disease activity. Compellingly, several of the upregulated genes were those found in early stages of neutrophil development [19]. We developed a negative selection technique to highly purify these low-density neutrophils, which we termed “low-density granulocytes” (LDGs), from the PBMC fractions of lupus patients [9]. Using this approach, we confirmed that all adult SLE patients examined displayed LDGs in their PBMC fractions, with those patients with higher numbers of these cells in the periphery developing enhanced prevalence of skin involvement and/or vasculitis [9].
Several distinct features were identified in LDGs and are further discussed in this review. Compared with control neutrophils or with autologous, normal-density lupus neutrophils, LDGs show enhanced capacity to synthesize type I IFNs upon specific types of stimulation (including granulocyte-colony stimulation factor (G-CSF) or polyinosinic/polycytidylic acid (poly I/C). Furthermore, LDGs display decreased ability to phagocytose bacteria, but they have a strikingly enhanced capacity to form neutrophil extracellular traps (NETs) [9, 20]. NETs are characterized as chromatin fibers associated to granular proteins that are released to the extracellular space in order to immobilize and kill invading microbes during a process of cell death termed “NETosis” [21, 22]. In addition to their antimicrobial role, recent evidence suggests that NETs can induce endothelial damage and expose potent immunostimulatory molecules [20, 23]. Due to the potential role of netting neutrophils in externalizing autoantigens and activating the adaptive immune system, we have proposed that LDGs, at least in part through a NET-associated effect, may play an important role in the pathogenesis of SLE and its associated organ damage. This is explored in more detail later in this review.
Morphology and function of lupus LDGs
Phenotypically, a neutrophil can be distinguished by two distinctive morphological characteristics: its unique polymorphous nucleus and the content of its granules. Furthermore, classification of neutrophils and their precursors is based on their stage of maturation in the bone marrow. Myelopoiesis is a tightly controlled process whereby precursor cells divide and differentiate from pluripotent hematopoietic stem cells and proceed to committed stem cells that provide lineage-restricted progenies. During maturation, neutrophils acquire their granule products, and variations in the timing of synthesis of various proteins present in granules lead to the formation of granule subsets with distinct peptide content depending on the specific stage of differentiation. It is considered that the elevated heterogeneity of neutrophil granules arises from continuous formation of granules from the myeloblast to the segmented stages. Under normal conditions, neutrophils are released from the bone marrow when terminally differentiated [24].
The developmental stage of LDGs and the mechanisms driving their synthesis in SLE remains unclear. While mature neutrophils typically sediment with the red-blood cell fraction in a Ficoll-density gradient, LDGs co-purify in the PMBC fraction. Examination of nuclear morphology of LDGs by differential staining has revealed a mixed population of segmented, band, or myelocyte-like cells [9, 10]. In order to establish whether the low density of these cells is the result of degranulation due to activation or the result of a more immature phenotype, we have performed transmission electron microscopy of purified lupus LDG fractions and compared their ultrastructural characteristics to those of normal-density neutrophils. Using this approach, we have observed that LDGs have less segmented nuclei compared with normal-density granulocytes, with their hetero- (dense) and euchromatin (decondensed) clearly delineated, and with various types of granules identified in their cytoplasm. The nuclear morphology by ultrastructural analysis may suggest a more immature stage, such as band/juvenile forms. These observations support the notion that LDGs do not represent a subset of activated neutrophils that have undergone granule release. Furthermore, the cytoplasm of LDGs shows no evidence of vacuolization or apoptosis (Fig. 1).
Analysis of lupus low-density granulocyte morphology by electron microscopy. Transmission electron microscopy of a normal- (a–c) and of a low-density granulocyte (d–f) isolated from a patient with SLE display various types of granules in their cytoplasm. Heterochromatic (dark) and euchromatic (lighter) areas are clearly defined in both cells. Nuclear lobes are clearly defined in normal-density granulocytes while LDGs demonstrate less lobulated nuclei
Gene array analysis of LDGs
As an additional tool to assess whether LDGs represent a distinct pool of neutrophils, gene expression profiling of purified neutrophil fractions of lupus LDGs, autologous lupus neutrophils, and control neutrophils was determined using Affymetrix genechip microarrays. While no genes were significantly differentially regulated when comparing normal-density lupus neutrophils with healthy control neutrophils, several genes were differentially expressed in LDGs relative to the other neutrophil groups. Indeed, 302 genes were differentially expressed in lupus LDGs when compared with control neutrophils, and 281 genes were found to be altered using pairwise comparison of each patient’s LDGs to their autologous lupus neutrophils. Furthermore, 224 genes were upregulated in both comparisons. In addition, 57 genes were selectively regulated in lupus LDGs, compared with autologous lupus neutrophils, and 78 genes were restricted to LDGs alone when compared with control neutrophils. Identification of canonical pathways identified actin cytoskeleton, macropinocytosis, clathrin-mediated endocytosis, and integrin signaling pathways among the most significantly regulated in lupus LDGs compared with normal-density neutrophils. Interestingly, the top upregulated genes in lupus LDGs included various serine proteases, bactericidal proteins, and other molecules present in azurophilic granules and involved in neutrophil regulation of inflammatory responses [20]. These findings once again suggest a more immature phenotype of the LDGs, as levels of expression of the mRNAs that encode neutrophil serine proteases are greatest at the promyelocytic stage of neutrophil differentiation and are downregulated as neutrophils mature [25]. In support of the gene array analysis, high levels of calprotectin (S100A8/S100A9) were recently reported in a proteomic analysis of SLE PBMCs, in direct correlation with the presence of LDGs. These observations suggest a proteomic signature for circulating LDGs in lupus patients that requires further investigation [26]. Overall, based on the gene expression profile and the ultrastructural analysis of LDGs, it is possible that they represent a more immature granulocyte subset prematurely released from the marrow due to yet uncharacterized stimuli. These observations are in agreement with the studies from Bennett et al. in pediatric lupus patients, as mentioned above [10]. Various cytokines abundant in SLE could potentially enhance mobilization of neutrophil precursors from the bone marrow or interfere with their differentiation capacity. Among the putative stimuli, granulocyte-macrophage colony-stimulating factor (GM-CSF) and type I IFNs should be considered, as levels of these cytokines are reported elevated in SLE and may drive marrow mobilization and/or impair differentiation, respectively [27, 28]. However, since the LDG microarray analysis did not reveal evidence of enhanced expression of type I IFN inducible genes [20, 29], it does not appear that LDGs represent a subset preferentially exposed to higher levels of these cytokines.
LDG surface markers and activation status
The exact characterization of the origin and differentiation status of LDGs has been problematic, in part due to discrepancies found between the nuclear morphology/gene expression studies and the cell surface molecule characterization. Indeed, while nuclear morphology and gene expression studies suggest an immature phenotype, cell surface marker analysis of LDGs using flow cytometry (FACS) is indicative of a mature granulocyte [9] (Table 1). LDGs can be distinguished from monocytes by FACS by their high expression of CD15 and their low expression of CD14. In contrast, monocytes are CD14 high and CD15 low [9]. With regards to other markers, LDGs express CD10 and CD16, both characteristic of mature granulocytes. CD33, a marker expressed on developing or immature granulocytes is only very weakly expressed, with no detection of other early progenitor markers, such as CD34 and Flt-3. In addition, LDGs express CD31, CD11c, G-CSFR, and GM-CSFR. Relative to healthy control neutrophils, LDGs and autologous lupus neutrophils have an activated phenotype based on the surface molecule expression of CD66b and CD11b, but they do not differ with regard to l-selectin expression and shedding before and after exogenous stimulation [9]. How to reconcile the cell surface marker analysis with the nuclear morphology analysis remains unclear. We cannot exclude the possibility that LDGs are a heterogeneous population of neutrophils that does not exclusively comprise of mature activated or immature cells. In order to have a deep insight into the nature of LDGs, it is essential to perform more comprehensive analyses verifying the status of other granular resident proteins. Additionally, epigenetic heterochromatin markers can also be used to assess whether LDGs display an incomplete/aberrant development and/or arrest [30, 31].
Proinflammatory phenotype of lupus LDGs
In addition to protease release through degranulation and/or NETosis, neutrophils can synthesize pro-inflammatory cytokines and eicosanoids when recruited to sites of infection [1]. Activated neutrophils have the capacity to synthesize TNF-α mRNA [32], and we have reported that LDGs secrete higher levels of this cytokine than normal-density neutrophils [9]. As overexpression of TNF-α has been documented in lupus nephritis [33–35] and may play an important role in kidney damage in this disease [36], it is possible that these cells may represent one of the sources of this cytokine in this disease. Levels of synthesis of IL-8 and IL-6 were also found to be higher in LDGs, when compared with autologous lupus and control neutrophils [9] and this may contribute to the amplification of inflammatory responses and tissue damage in SLE.
Type I IFNs have been reported to be secreted by neutrophils [37, 38] upon specific types of stimulation. As mentioned above, we have found that LDGs have enhanced capacity to synthesize these cytokines when compared with healthy control neutrophils or with autologous lupus neutrophils. Indeed, LDGs synthesize sufficient amounts of type I IFNs in culture to interfere with the capacity of endothelial progenitor cells to differentiate into mature endothelial cells [9], a phenomenon implicated in the development of premature atherosclerosis that significantly affects patients with lupus [8, 39]. In contrast, depletion of plasmacytoid dendritic cells, the cells synthesizing the highest concentrations of IFN-α in human and murine systems, did not have an effect of endothelial cell differentiation. This observation suggests that LDGs may play prominent roles in disrupting endothelial health in SLE, at least in part through a type I IFN effect. The pathways leading to enhanced type I IFN synthesis by LDGs (TLR dependent and/or independent) remain to be fully characterized. Furthermore, the specific type I IFNs that are synthesized at higher levels by LDGs both at the mRNA and protein level remain to be determined.
LDGs and NETosis
Beside phagocytosis and degranulation, neutrophils possess another antimicrobial mechanism to immobilize and kill invading pathogens named NETosis [21]. During NETosis, large strands of DNA are extruded from neutrophils, carrying specific proteins from the cytosol and granules (Fig. 2) [21, 40]. NETs can be produced upon activation by PMA, bacteria, fungi, virus, microbial products, and activated platelets and various cytokines [21, 29, 41–50]. Our group and others have reported that neutrophils isolated from SLE patients are primed to make NETs [20, 48, 49]. In particular, LDGs have a striking enhancement in their capacity to generate NETs [9, 20]. Various stimuli have been proposed to induce enhanced NETosis in SLE, including immune complexes, type I IFNs, and autoAbs [20, 48, 49]. Importantly, netting neutrophils have been proposed as strong inducers of IFN-α synthesis by pDCs [20, 49], thereby supporting additional contributions to lupus pathogenesis. Furthermore, type I IFNs can potentiate production of NETs by mature neutrophils [46], and this may lead to a self-perpetuating cycle where cytokines activate granulocytes to die by NETosis, which in turn leads to more type I IFN synthesis by pDCs. In addition, sera from SLE patients can bind to NETs (Fig. 3), suggesting that autoantibodies to NETs components are generated in this disease. In addition, NETs generated by LDGs have the capacity to stimulate the NLRP3 inflammasome machinery at augmented levels in lupus macrophages, with potential to establish vicious inflammatory cycles [50].
Detection of neutrophil granular proteins in NETs. Immunofluorescence microphotographs of control neutrophils activated with LPS in vitro, releasing NETs, characterized as long strands of DNA (blue) decorated with the antimicrobial peptide LL-37 (green) and neutrophil elastase (red). Original magnification, ×40
Autoantibodies present in SLE, but not control, sera react with molecules present in LDG NETs. NETs generated by LPS stimulation of control neutrophils, or spontaneously released by lupus LDGs were incubated with 10 % healthy control serum (upper) or 10 % SLE serum (lower). Bound IgGs were detected using a secondary antibody conjugated with a red fluorochrome. Blue represents nuclear material, as quantified by Hoechst. Original magnification, ×40
Additionally, Hakkim and colleagues demonstrated that approximately one third of serum samples obtained from a cohort of SLE have impaired capacity to degrade NETs. They have implicated molecules present in SLE sera that interfere with DNase I activity. They identified a link between SLE patients with poor DNase I activity and high titers of anti-dsDNA antibodies, while impaired NET clearance was associated to the presence of nephritis [51]. Impairment of DNAse I activity in SLE patients can be caused by genetic factors [52, 53] or by the presence of DNAse 1 inhibitors in sera [51, 54]. Dysregulation in NET clearance may play a role in lupus pathogenesis and also impact the formation of thrombosis in SLE patients [22]. Thus, presence of LDGs that have enhanced netting capabilities, combined with impairments in NET clearance might result in the prolonged exposure of antigenic material and further induction of proinflammatory cytokines that can perpetuate a vicious cycle leading to prolonged autoimmunity in predisposed individuals.
It remains to be determined whether the externalization of proteins through NET formation plays prominent roles in the loss of self-tolerance, the activation of adaptive immune responses and the development of autoimmunity. While in a recent study purified NETs failed to exacerbate autoimmune phenotype in some mouse models of lupus [55], the roles of second signals or additional stimuli need to be considered to more clearly identify how NETs may promote aberrant immune responses. It is also unclear if the protein cargo of the LDG NETs is different than the one elicited by other NET-inducing stimuli.
LDGs and the development of organ damage in SLE
LDGs have been associated with endothelial damage as well as with induction of abnormal endothelial differentiation, with potential implications in the development of premature atherosclerosis that affects patients with various autoimmune diseases [9, 20]. In vitro experiments conducted in our laboratory demonstrate restoration of the capacity of endothelial progenitors to differentiate into a mature endothelium when LDGs are depleted from cultures [9]. Furthermore, the cytotoxic effect of LDGs on endothelial cells appears to be related to their capacity to synthesize NETs, as abrogation of vascular cell death was observed in the presence of a nuclease that disrupts the NETs [20]. The mechanisms by which NETs damage the endothelium remain to be fully determined, although histones present in these structures may play prominent roles [56].
The exact role that LDGs may play in other lupus complications, including nephritis and skin disease, remains to be determined. As mentioned above, higher numbers of LDGs correlated with skin involvement and vasculitis in our original observations [9]. Furthermore, netting neutrophils were observed infiltrating skin and kidneys from lupus patients with dermatologic and renal complications [20]. However, whether these cells represent LDGs or normal-density neutrophils remains unclear, as no distinctive cell markers have been identified that can distinguish between these two types of neutrophils at the tissue level.
LDGs in other diseases
Neutrophils with low-density features have been documented in conditions such as cancer, HIV infection, sepsis, psoriasis, and, recently, in the pristane-induced arthritis (PIA) rat model [57–61]. On the other hand, it is unclear if these cells represent a distinct phenotype (as described in SLE), or merely degranulated cells. For example, septic patients display increased numbers of low-density neutrophils with diminished chemotactic responses and minimal β-glucuronidase activity. However, the morphology and cell surface analyses of these cells indicate that they represent mature degranulated neutrophils with vacuolized cytoplasm [57].
LDGs have been also reported in other vertebrates. Density gradient separation of blood from pigs infected with classical swine flu (CSF) virus display the presence of SWC3-positive granulocytes, a pan-myeloid marker, in their PBMC preparation [62]. Morphological analyses revealed that SSC+ SWC+ were immature granulocytes, mainly myelocyte and band neutrophils [62].
As mentioned above, we have documented LDGs in the peripheral blood of patients with psoriasis [60]. Similar to SLE, we found that psoriasis LDGs are more primed to form NETs that externalize IL-17, a proinflammatory cytokine linked to the pathogenesis of psoriasis and other autoimmune diseases such as rheumatoid arthritis (RA) [63]. Low buoyancy neutrophils were also initially described in RA [18] and, recently, a PIA rat model demonstrated increased percentage of cells expressing His48+, a rat granulocyte marker, co-purifying with PBMCs [61]. The expression of the rCRAMP, rat analog of the cathelicidin LL-37, was higher in PIA compared with naïve rats. Such expression was mostly apparent in His48+ cells, supporting the presence of granulocytes. Although the origin of these granulocytes is unknown, the authors proposed an early release from the bone marrow due to accelerated turnover of mature neutrophils. To our knowledge, this is the first report of a putative LDG subset in an animal model of autoimmunity. Whether similar cells can be found in murine models of lupus remains to be determined.
Conclusions
As mentioned above, it is possible that cytokines, autoAbs, and/or immune complexes present in lupus patients can alter the bone marrow niche or promote the release of immature granulocytes (Fig. 4). It is unclear, however, whether the exposure of marrow granulocytes to cytokines and/or immune complexes may alter their morphology and/or gene expression. Conversely, and given the cell surface marker profile consistent with mature cells, LDGs could represent a subpopulation of activated neutrophils similar to the ones reported in the marginal zone of the spleen in humans [64]. In this case, splenic neutrophils were found to have a distinct phenotype compared with circulating neutrophils, and to elicit specific adaptive immune in marginal zone B cells through NET-like structures [64]. This finding supports the notion that subsets of neutrophils present in different tissues can have distinct phenotypes and function and that this be further evaluated in the case of LDGs. Studies in animal models of autoimmunity are imperative to further clarify the origin, maturation status and pathogenicity of LDGs. This would also allow us the opportunity to test potential pharmacologic approaches in this specific cell subset. Future characterization and establishment of specific LDG markers may prove very useful in assessing their putative roles in tissue damage in lupus and other diseases.
Schematic representation of the possible origins of LDGs in SLE. 1, High levels of cytokines, immune complexes, autoantibodies, and/or other yet unidentified molecules can affect neutrophil development in the bone marrow and promote altered gene expression and nuclear morphology. 2, Alternatively, mature neutrophils exposed to high levels of the aforementioned molecules alter their gene expression, homing capabilities, and phenotype, generating an aberrant pathogenic subpopulation
Nevertheless, the findings summarized in this review support the existence of a distinct subset of aberrant neutrophils in SLE patients. Longitudinal studies are needed to systematically assess if LDGs can be used as biomarkers or predictors of tissue damage, disease activity and specific complications in SLE. Furthermore, it is important to explore whether low-buoyancy PMNs detected in other autoimmune disease play similar pathogenic roles as in SLE, with regards to cytokine synthesis, capacity to generate NETs, etc.
The factors driving the abnormal phenotype and function of lupus LDGs need to be determined and may include specific cytokines that could arrest neutrophil maturation. Whether NETs generated by LDGs have different immunostimulatory capabilities and protein cargo to those generated by conventional neutrophils in response to microbes is unclear. Finally, the interactions between LDGs and the adaptive immune system should be the focus of future investigations. By clarifying the origin and pathogenicity of LDGs, we may be able to devise novel therapeutic strategies in lupus and other autoimmune diseases. We may also be able to better understand the link between infections and the development of autoimmune responses and disease flares.
References
Weiss SJ, Young J, LoBuglio AF, Slivka A, Nimeh NF (1981) Role of hydrogen peroxide in neutrophil-mediated destruction of cultured endothelial cells. J Clin Invest 68:714–721
Bainton DF, Ullyot JL, Farquhar MG (1971) The development of neutrophilic polymorphonuclear leukocytes in human bone marrow. J Exp Med 134:907–934
Kyttaris VC, Juang YT, Tsokos GC (2005) Immune cells and cytokines in systemic lupus erythematosus: an update. Curr Opin Rheumatol 17:518–522
Camussi G, Cappio FC, Messina M, Coppo R, Stratta P, Vercellone A (1980) The polymorphonuclear neutrophil (PMN) immunohistological technique: detection of immune complexes bound to the PMN membrane in acute poststreptococcal and lupus nephritis. Clin Nephrol 14:280–287
Ward MM (1999) Premature morbidity from cardiovascular and cerebrovascular diseases in women with systemic lupus erythematosus. Arthritis Rheum 42:338–346
Crispin JC, Kyttaris VC, Terhorst C, Tsokos GC (2010) T cells as therapeutic targets in SLE. Nat Rev Rheumatol 6:317–325
Dorner T, Jacobi AM, Lee J, Lipsky PE (2011) Abnormalities of B cell subsets in patients with systemic lupus erythematosus. J Immunol Methods 363:187–197
Denny MF, Chandaroy P, Killen PD, Caricchio R, Lewis EE, Richardson BC, Lee KD, Gavalchin J, Kaplan MJ (2006) Accelerated macrophage apoptosis induces autoantibody formation and organ damage in systemic lupus erythematosus. J Immunol 176:2095–2104
Denny MF, Yalavarthi S, Zhao W, Thacker SG, Anderson M, Sandy AR, McCune WJ, Kaplan MJ (2010) A distinct subset of proinflammatory neutrophils isolated from patients with systemic lupus erythematosus induces vascular damage and synthesizes type I IFNs. J Immunol 184:3284–3297
Bennett L, Palucka AK, Arce E, Cantrell V, Borvak J, Banchereau J, Pascual V (2003) Interferon and granulopoiesis signatures in systemic lupus erythematosus blood. J Exp Med 197:711–723
Banchereau J, Pascual V (2006) Type I interferon in systemic lupus erythematosus and other autoimmune diseases. Immunity 25:383–392
Brandt L, Hedberg H (1969) Impaired phagocytosis by peripheral blood granulocytes in systemic lupus erythematosus. Scand J Haematol 6:348–353
Courtney PA, Crockard AD, Williamson K, Irvine AE, Kennedy RJ, Bell AL (1999) Increased apoptotic peripheral blood neutrophils in systemic lupus erythematosus: relations with disease activity, antibodies to double stranded DNA, and neutropenia. Ann Rheum Dis 58:309–314
Hashimoto Y, Ziff M, Hurd ER (1982) Increased endothelial cell adherence, aggregation, and superoxide generation by neutrophils incubated in systemic lupus erythematosus and Felty’s syndrome sera. Arthritis Rheum 25:1409–1418
Abramson SB, Given WP, Edelson HS, Weissmann G (1983) Neutrophil aggregation induced by sera from patients with active systemic lupus erythematosus. Arthritis Rheum 26:630–636
Molad Y, Buyon J, Anderson DC, Abramson SB, Cronstein BN (1994) Intravascular neutrophil activation in systemic lupus erythematosus (SLE): dissociation between increased expression of CD11b/CD18 and diminished expression of L-selectin on neutrophils from patients with active SLE. Clin Immunol Immunopathol 71:281–286
Cochrane CG, Unanue ER, Dixon FJ (1965) A Role of Polymorphonuclear Leukocytes and Complement in Nephrotoxic Nephritis. J Exp Med 122:99–116
Hacbarth E, Kajdacsy-Balla A (1986) Low density neutrophils in patients with systemic lupus erythematosus, rheumatoid arthritis, and acute rheumatic fever. Arthritis Rheum 29:1334–1342
Nakou M, Knowlton N, Frank MB, Bertsias G, Osban J, Sandel CE, Papadaki H, Raptopoulou A, Sidiropoulos P, Kritikos I et al (2008) Gene expression in systemic lupus erythematosus: bone marrow analysis differentiates active from inactive disease and reveals apoptosis and granulopoiesis signatures. Arthritis Rheum 58:3541–3549
Villanueva E, Yalavarthi S, Berthier CC, Hodgin JB, Khandpur R, Lin AM, Rubin CJ, Zhao W, Olsen SH, Klinker M et al (2011) Netting neutrophils induce endothelial damage, infiltrate tissues, and expose immunostimulatory molecules in systemic lupus erythematosus. J Immunol 187:538–552
Brinkmann V, Reichard U, Goosmann C, Fauler B, Uhlemann Y, Weiss DS, Weinrauch Y, Zychlinsky A (2004) Neutrophil extracellular traps kill bacteria. Science 303:1532–1535
Fuchs TA, Abed U, Goosmann C, Hurwitz R, Schulze I, Wahn V, Weinrauch Y, Brinkmann V, Zychlinsky A (2007) Novel cell death program leads to neutrophil extracellular traps. J Cell Biol 176:231–241
Saffarzadeh M, Juenemann C, Queisser MA, Lochnit G, Barreto G, Galuska SP, Lohmeyer J, Preissner KT (2012) Neutrophil extracellular traps directly induce epithelial and endothelial cell death: a predominant role of histones. PLoS One 7:e32366
Mollinedo F, Borregaard N, Boxer LA (1999) Novel trends in neutrophil structure, function and development. Immunol Today 20:535–537
Cowland JB, Borregaard N (1999) The individual regulation of granule protein mRNA levels during neutrophil maturation explains the heterogeneity of neutrophil granules. J Leukoc Biol 66:989–995
Pavon EJ, Garcia-Rodriguez S, Zumaquero E, Perandres-Lopez R, Rosal-Vela A, Lario A, Longobardo V, Carrascal M, Abian J, Callejas-Rubio JL et al (2012) Increased expression and phosphorylation of the two S100A9 isoforms in mononuclear cells from patients with systemic lupus erythematosus: a proteomic signature for circulating low-density granulocytes. J Proteomics 75:1778–1791
Fiehn C, Wermann M, Pezzutto A, Hufner M, Heilig B (1992) Plasma GM-CSF concentrations in rheumatoid arthritis, systemic lupus erythematosus and spondyloarthropathy. Z Rheumatol 51:121–126
Willeke P, Schluter B, Schotte H, Erren M, Mickholz E, Domschke W, Gaubitz M (2004) Increased frequency of GM-CSF secreting PBMC in patients with active systemic lupus erythematosus can be reduced by immunoadsorption. Lupus 13:257–262
Ramos-Kichik V, Mondragon-Flores R, Mondragon-Castelan M, Gonzalez-Pozos S, Muniz-Hernandez S, Rojas-Espinosa O, Chacon-Salinas R, Estrada-Parra S, Estrada-Garcia I (2009) Neutrophil extracellular traps are induced by Mycobacterium tuberculosis. Tuberculosis (Edinb) 89:29–37
Popova EY, Claxton DF, Lukasova E, Bird PI, Grigoryev SA (2006) Epigenetic heterochromatin markers distinguish terminally differentiated leukocytes from incompletely differentiated leukemia cells in human blood. Exp Hematol 34:453–462
Lukasova E, Koristek Z, Falk M, Kozubek S, Grigoryev S, Kozubek M, Ondrej V, Kroupova I (2005) Methylation of histones in myeloid leukemias as a potential marker of granulocyte abnormalities. J Leukoc Biol 77:100–111
Lindemann A, Riedel D, Oster W, Ziegler-Heitbrock HW, Mertelsmann R, Herrmann F (1989) Granulocyte-macrophage colony-stimulating factor induces cytokine secretion by human polymorphonuclear leukocytes. J Clin Invest 83:1308–1312
Studnicka-Benke A, Steiner G, Petera P, Smolen JS (1996) Tumour necrosis factor alpha and its soluble receptors parallel clinical disease and autoimmune activity in systemic lupus erythematosus. Br J Rheumatol 35:1067–1074
Gabay C, Cakir N, Moral F, Roux-Lombard P, Meyer O, Dayer JM, Vischer T, Yazici H, Guerne PA (1997) Circulating levels of tumor necrosis factor soluble receptors in systemic lupus erythematosus are significantly higher than in other rheumatic diseases and correlate with disease activity. J Rheumatol 24:303–308
Malide D, Russo P, Bendayan M (1995) Presence of tumor necrosis factor alpha and interleukin-6 in renal mesangial cells of lupus nephritis patients. Hum Pathol 26:558–564
Edwards CK 3rd, Zhou T, Zhang J, Baker TJ, De M, Long RE, Borcherding DR, Bowlin TL, Bluethmann H, Mountz JD (1996) Inhibition of superantigen-induced proinflammatory cytokine production and inflammatory arthritis in MRL-lpr/lpr mice by a transcriptional inhibitor of TNF-alpha. J Immunol 157:1758–1772
Shirafuji N, Matsuda S, Ogura H, Tani K, Kodo H, Ozawa K, Nagata S, Asano S, Takaku F (1990) Granulocyte colony-stimulating factor stimulates human mature neutrophilic granulocytes to produce interferon-alpha. Blood 75:17–19
Tamassia N, Le Moigne V, Rossato M, Donini M, McCartney S, Calzetti F, Colonna M, Bazzoni F, Cassatella MA (2008) Activation of an immunoregulatory and antiviral gene expression program in poly(I:C)-transfected human neutrophils. J Immunol 181:6563–6573
Kaplan MJ, Salmon JE (2011) How does interferon-α insult the vasculature? Let me count the ways. Arthritis Rheum 63:334–336
Urban CF, Ermert D, Schmid M, Abu-Abed U, Goosmann C, Nacken W, Brinkmann V, Jungblut PR, Zychlinsky A (2009) Neutrophil extracellular traps contain calprotectin, a cytosolic protein complex involved in host defense against Candida albicans. PLoS Pathog 5:e1000639
Urban CF, Reichard U, Brinkmann V, Zychlinsky A (2006) Neutrophil extracellular traps capture and kill Candida albicans yeast and hyphal forms. Cell Microbiol 8:668–676
Cogen AL, Yamasaki K, Muto J, Sanchez KM, Crotty Alexander L, Tanios J, Lai Y, Kim JE, Nizet V, Gallo RL (2010) Staphylococcus epidermidis antimicrobial delta-toxin (phenol-soluble modulin-gamma) cooperates with host antimicrobial peptides to kill group A Streptococcus. PLoS One 5:e8557
Clark SR, Ma AC, Tavener SA, McDonald B, Goodarzi Z, Kelly MM, Patel KD, Chakrabarti S, McAvoy E, Sinclair GD et al (2007) Platelet TLR4 activates neutrophil extracellular traps to ensnare bacteria in septic blood. Nat Med 13:463–469
Juneau RA, Pang B, Weimer KE, Armbruster CE, Swords WE (2011) Nontypeable Haemophilus influenzae initiates formation of neutrophil extracellular traps. Infect Immun 79:431–438
Pilsczek FH, Salina D, Poon KK, Fahey C, Yipp BG, Sibley CD, Robbins SM, Green FH, Surette MG, Sugai M et al (2010) A novel mechanism of rapid nuclear neutrophil extracellular trap formation in response to Staphylococcus aureus. J Immunol 185:7413–7425
Martinelli S, Urosevic M, Daryadel A, Oberholzer PA, Baumann C, Fey MF, Dummer R, Simon HU, Yousefi S (2004) Induction of genes mediating interferon-dependent extracellular trap formation during neutrophil differentiation. J Biol Chem 279:44123–44132
Gupta AK, Hasler P, Holzgreve W, Gebhardt S, Hahn S (2005) Induction of neutrophil extracellular DNA lattices by placental microparticles and IL-8 and their presence in preeclampsia. Hum Immunol 66:1146–1154
Garcia-Romo GS, Caielli S, Vega B, Connolly J, Allantaz F, Xu Z, Punaro M, Baisch J, Guiducci C, Coffman RL et al (2011) Netting neutrophils are major inducers of type I IFN production in pediatric systemic lupus erythematosus. Sci Transl Med 3:73ra20
Lande R, Ganguly D, Facchinetti V, Frasca L, Conrad C, Gregorio J, Meller S, Chamilos G, Sebasigari R, Riccieri V et al (2011) Neutrophils activate plasmacytoid dendritic cells by releasing self-DNA-peptide complexes in systemic lupus erythematosus. Sci Transl Med 3:73ra19
Kahlenberg JM, Carmona-Rivera C, Smith CK, Kaplan MJ (2013) Neutrophil extracellular trap-associated protein activation of the NLRP3 inflammasome is enhanced in lupus macrophages. J Immunol 190:1217–1226
Hakkim A, Furnrohr BG, Amann K, Laube B, Abed UA, Brinkmann V, Herrmann M, Voll RE, Zychlinsky A (2010) Impairment of neutrophil extracellular trap degradation is associated with lupus nephritis. Proc Natl Acad Sci U S A 107:9813–9818
Yasutomo K, Horiuchi T, Kagami S, Tsukamoto H, Hashimura C, Urushihara M, Kuroda Y (2001) Mutation of DNASE1 in people with systemic lupus erythematosus. Nat Genet 28:313–314
Shin HD, Park BL, Kim LH, Lee HS, Kim TY, Bae SC (2004) Common DNase I polymorphism associated with autoantibody production among systemic lupus erythematosus patients. Hum Mol Genet 13:2343–2350
Leffler J, Martin M, Gullstrand B, Tyden H, Lood C, Truedsson L, Bengtsson AA, Blom AM (2012) Neutrophil extracellular traps that are not degraded in systemic lupus erythematosus activate complement exacerbating the disease. J Immunol 188:3522–3531
Liu CL, Tangsombatvisit S, Rosenberg JM, Mandelbaum G, Gillespie EC, Gozani OP, Alizadeh AA, Utz PJ (2012) Specific post-translational histone modifications of neutrophil extracellular traps as immunogens and potential targets of lupus autoantibodies. Arthritis Res Ther 14:R25
Caudrillier A, Kessenbrock K, Gilliss BM, Nguyen JX, Marques MB, Monestier M, Toy P, Werb Z, Looney MR (2012) Platelets induce neutrophil extracellular traps in transfusion-related acute lung injury. J Clin Invest 122:2661–2671
Morisaki T, Goya T, Ishimitsu T, Torisu M (1992) The increase of low density subpopulations and CD10 (CALLA) negative neutrophils in severely infected patients. Surg Today 22:322–327
Rodriguez PC, Ernstoff MS, Hernandez C, Atkins M, Zabaleta J, Sierra R, Ochoa AC (2009) Arginase I-producing myeloid-derived suppressor cells in renal cell carcinoma are a subpopulation of activated granulocytes. Cancer Res 69:1553–1560
Cloke T, Munder M, Taylor G, Muller I, Kropf P (2012) Characterization of a novel population of low-density granulocytes associated with disease severity in HIV-1 infection. PLoS One 7:e48939
Lin AM, Rubin CJ, Khandpur R, Wang JY, Riblett M, Yalavarthi S, Villanueva EC, Shah P, Kaplan MJ, Bruce AT (2011) Mast cells and neutrophils release IL-17 through extracellular trap formation in psoriasis. J Immunol 187:490–500
Hoffmann MH, Bruns H, Backdahl L, Neregard P, Niederreiter B, Herrmann M, Catrina AI, Agerberth B, Holmdahl R (2013) The cathelicidins LL-37 and rCRAMP are associated with pathogenic events of arthritis in humans and rats. Ann Rheum Dis (in press)
Porntrakulpipat S, Depner KR, Moennig V (2001) Are low-density granulocytes the major target cells of classical swine fever virus in the peripheral blood? J Vet Med B Infect Dis Vet Public Health 48:593–602
Wilson NJ, Boniface K, Chan JR, McKenzie BS, Blumenschein WM, Mattson JD, Basham B, Smith K, Chen T, Morel F et al (2007) Development, cytokine profile and function of human interleukin 17-producing helper T cells. Nat Immunol 8:950–957
Puga I, Cols M, Barra CM, He B, Cassis L, Gentile M, Comerma L, Chorny A, Shan M, Xu W et al (2012) B cell-helper neutrophils stimulate the diversification and production of immunoglobulin in the marginal zone of the spleen. Nat Immunol 13:170–180
Acknowledgments
This study is supported by the NIH through PHS grants AR007080 and HL088419.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is a contribution to the special issue on Neutrophils - Guest Editors: Paul Hasler and Sinuhe Hahn
Rights and permissions
About this article
Cite this article
Carmona-Rivera, C., Kaplan, M.J. Low-density granulocytes: a distinct class of neutrophils in systemic autoimmunity. Semin Immunopathol 35, 455–463 (2013). https://doi.org/10.1007/s00281-013-0375-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00281-013-0375-7