Abstract
Purpose
This study aimed to investigate the predictive and prognostic roles of circulating exosomal miRNAs in breast cancer treated with trastuzumab-based chemotherapy.
Methods
Circulating exosomal miRNAs from trastuzumab-resistant (n = 4) and -sensitive (n = 4) patients were profiled using miRNA microarray. The predictive and prognostic roles of filtered miRNAs were validated in 107 early-stage and 68 metastatic patients treated with trastuzumab-based chemotherapy through receiver-operating characteristic (ROC) curve analysis, logistic regression and Cox proportional hazards regression analysis, and Kaplan–Meier survival analysis.
Results
MiRNA microarray analysis revealed miR-1246 and miR-155 were the most up-regulated miRs in trastuzumab-resistant HER2-positive breast cancer patients, which were further validated in trastuzumab-resistant patient samples (n = 32) compared with trastuzumab sensitive ones (n = 36). MiR-1246 showed a ROC curve area of 0.750 with 78.1% sensitivity and 75% specificity in discriminating resistant from sensitive patients (p < 0.001), while miR-155 showed a ROC curve area of 0.877 with 68.8% sensitivity and 97.2% specificity (p < 0.001). Predictive factors and multivariate analysis showed that high levels of miR-1246 and miR-155 strongly predicted poor event-free survival (EFS) for early-stage patients, and poor progression-free survival (PFS) for metastatic patients. However, both miRNAs were revealed not to be associated with overall survival (OS). In addition, Kaplan–Meier survival analysis demonstrated that early-stage and metastatic patients with high expression of miR-1246 and miR-155 had poorer EFS or PFS, respectively, than those with decreased expression of both miRs.
Conclusions
This study demonstrated the valuable roles of circulating exosomal miR-1246 and miR-155 in distinguishing trastuzumab resistant from sensitive patients.
Similar content being viewed by others

Avoid common mistakes on your manuscript.
Introduction
Breast cancer (BC) occurs with high incidence and is the second leading cause for women deaths [1]. The human epidermal growth factor receptor-2 (HER2) is frequently overexpressed in approximately 20% BC patients [2], which usually indicates poorer overall survival and shorter time to relapse [3]. Trastuzumab, a kind of humanized monoclonal antibody, is specifically designed to target extracellular domain of HER2, and has proved remarkable therapeutic effects, when being used either alone or in combination with chemotherapeutics to treat HER2-positive BC patients [4, 5]. However, due to de novo or primary resistance, no less than 20% of early-stage HER2-positive breast cancer patients become resistant to trastuzumab-based chemotherapy, which makes the therapeutic strategy turn out ineffective. Furthermore, over 70% of HER2-positive metastatic breast tumors are initially responsive to trastuzumab, but eventually experience disease progression within 1 year of exposure to the drug for acquisition of trastuzumab resistance [6, 7]. Therefore, it is essential to predict the potential of trastuzumab resistance, which will help to make specific therapeutic strategies for patients with BC.
The exosomes form in the manner of fusion of intracellular multivesicular bodies with the plasma membrane, and present as the circulating vesicles with a diameter between 30 and 150 nm [8]. The most critical function of exosomes is to facilitate cell–cell communication by transmitting various types of molecules, including lipids, nucleotide acids, and proteins, to neighboring or distant cells [9]. Circulating exosome components have been increasingly reported to be related with diagnosis and prognosis of patients with BC. For example, gold nanoflare probe-mediated detection of biomarkers for BC diagnosis revealed plasma exosomal miR-1246 robustly differentiate BC patients from healthy individuals [10]; microRNA-profiling analysis disclosed that several exosomal miRNAs are effective biomarkers for predicting recurrence of BC patients [11]; and GSTP1-containing exosomes have been explored to predict chemo-resistance in BC patients treated with anthracycline/taxane-based chemotherapy [12]. Although a few studies have also uncovered the mechanisms for exosome-mediated trastuzumab resistance in BC patients [13, 14], little is known about the diagnostic roles of exosomes in predicting trastuzumab resistance, and thus prognosis of HER2-positive BC treated with trastuzumab-based therapy.
Growing evidences have indicated that microRNA profiling revealed differentially expressed miRNAs are reliable biomarkers for diagnosis, therapeutic effective, and prognosis in various type of cancer patients, including breast cancer [15,16,17]. MiRNAs in tumor cells can be packed into exosomes and released into circulation via active secretion of shedding microvesicles [18, 19]. In addition, it is noteworthy that miRNAs packed in the exosome of plasma are remarkably stable, because of the protection from endogenous RNase activity by the exosomes membrane [20, 21]. Recently, it has been reported that circulating exosomal miRNAs are of diagnostic and prognostic values for various cancers such as esophageal cancer, head and neck tumors, and gastric cancer [22,23,24]. However, the predictive roles of circulating exosomal miRNAs for trastuzumab resistance in HER2-positive BC patients remain to be further investigated.
A predictive factor refers to a measurable variable associated with response to a given therapy, while a prognostic factor is defined as a measurable variable that correlates with the natural history of the disease. In this study, we performed logistic regression and Cox proportional hazards regression independently to determine the predictive and prognostic roles of circulating exosomal miRNAs involved in trastuzumab resistance in breast cancer. Our work abided by the recommendations for tumor marker prognostic studies (REMARK) [25, 26], and proved that particular miRNAs packed in circulating exosomes could provide substantial trastuzumab resistance detection.
Methods
Study populations
The inclusion criteria for patients of this rule-based retrospective study were female, 18–70 years old, histologically confirmed HER2-positive, with early-stage or metastatic breast cancer diagnosed in Shandong Provincial Hospital between March 2013 and March 2019, and treated with trastuzumab at a loading dose of 8 mg/kg followed 6 mg/kg per 3 weeks for duration of 1 year for early-stage patients, and with trastuzumab at a loading dose of 4 mg/kg followed by 2 mg/kg per week until diseased progression for the metastatic patients. The following information have been acquired for early-stage patients: age, menopausal status, clinical T stage, clinical N stage, Ki67 score, histologic subtype, Bloom–Richardson histologic grade, and hormone receptor (HR) status (including estrogen receptor and progesterone receptor status), relative expression of circulating exosomal miR-1246 and miR-155. For metastatic patients, acquired data included age, menopausal status, metastatic sites, histologic grade, Ki67 score, HR status, and relative expression of circulating exosomal miR-1246 and miR-155. All metastatic patients should have bi-dimensionally measurable disease with clearly defined margins and radiologically (CT and/or ultrasound and/or MRI) documented tumor progression. Patients with central nervous system (CNS) lesions as the only site of measurable metastatic disease were excluded.
In this study, resistance to trastuzumab treatment in metastatic patients were defined as progressed or stable disease occurred, and sensitive to trastuzumab refers to partial or complete response to treatment. For survival analyses, the end point was event-free survival (EFS) for early-stage patients and progression-free survival (PFS) for metastatic patients. We defined EFS as the interval from initial diagnosis to distant metastasis, locoregional recurrence, or death from any cause, and PFS as the length of time from the start of trastuzumab-based treatment to disease progression or death, respectively. Overall survival (OS) was defined as the length of time from initial diagnosis to death from any cause for early-stage patients, and the length of time from the start of trastuzumab-based treatment to death from any cause for metastatic patients. Beside, pathological complete response (PCR) was defined as absence of residual invasive tumor cells in breast or nodes (ypT0/is + ypN0).
Blood processing and serum exosome isolation
Total exosomes were separated from peripheral blood using ExoQuick (BioCat, Heidelberg, Germany) in accordance with the manufacturer’s protocol. Briefly, 550 μl of plasma, isolated from debris and cells by two centrifugation procedures at 3000× g for 15 min, was incubated with 120 μl ExoQuick exosome precipitation solution at 4 °C for 30 min. After centrifugation at 1500× g for 30 min, the precipitated exosomes were then resuspended in 50 μl of phosphate-buffered saline (PBS) buffer.
Transmission electron microscopy (TEM) and nanoparticle tracking analysis (NTA)
Isolated exosomes were confirmed by TEM and NTA. The samples were managed in 2% glutaraldehyde at 4 °C for 2 h. After being washed four times with PBS, exosomes were fixed in 1% osmium tetroxide for 2 h, and then washed two times with distilled H2O. Next, the exosomes were dehydrated with acetone and gradient ethanol, fixed with 2% glutaraldehyde at 4 °C for 2 h, and washed with PBS for 4 times. Finally, exosomes were immersed, embedded and polymerized with ethoxyline resin to prepare slices with thickness of 0.5 mm. After being stained with uranium acetate and lead citron citrate, the prepared exosomes were observed under TEM instrument. The mean size of the prepared exosomes was measured by NTA applying the NanoSight NS300 instrument.
Western blotting (WB) analysis
Total exosomal proteins were extracted using the Total Exosome Protein Isolation Kit (Invitrogen, Shanghai, China) according to the manufacturer’s instruction manual. Protein concentration was analyzed by a BCA Protein Assay Kit (Beyotime, Shanghai, China). A total of 60 μg extracted protein was electrophoretically separated on 10–12% SDS-PAGE and then blotted onto to a polyvinylidene fluoride membrane (Millipore, Billerica, USA), which was subsequently blocked on and incubated with rabbit polyclonal antibody specific for CD81 (1:1000; Invitrogen, Darmstadt, Germany) and CD63 (1:1000; ABGENT, San Diego, CA, USA) overnight. After washing with Tris-buffered saline containing 0.1% Tween-20 (TBST) three times, the membrane was incubated with horseradish peroxidase-conjugated goat anti-rabbit IgG at room temperature for 1 h. A chemiluminescence kit (Thermo Fisher, Waltham, MA, USA) was applied for development of color, and a gel imager was applied to take photos.
Extraction of miRNA and conversion in cDNA
MiRNA were extracted from 50 μl exosomes resuspended in 150 μl of lysis buffer applying the TaqMan miRNA ABC Purification Kit (Thermo Fisher Scientific, Darmstadt, Germany) according to the manufacturer’s protocol. Reverse transcription was performed using the TaqMan MicroRNA Reverse Transcription Kit (Life Technologies, Carlsbad, CA, USA) immediately after miRNA extraction. The reverse transcription reaction (10 μl) contained 4 μl RNA, nuclease-free water, 2 μl TaqMan RT Primer, 0.13 μl RNase Inhibitor, 1 μl Reverse Transcription Buffer, 0.66 μl MultiScribe Reverse Transcriptase, and 0.1 μl dNTPs. The reaction progressed at 16 °C for 30 min, 42 °C for 30 min, and 85 °C for 5 min on a MJ Research PTC-200 Peltier Thermal Cycler (Global Medical Instrumentation, Ramsey, MN, USA). The cDNA samples were stored at − 20 °C for further use.
MiRNA microarray analysis
The miRNA expression profiles of circulating exosomes were analyzed by a 3D-Gene Human miRNA Oligo chip version 20 (TORAY, Tokyo, Japan) according to the manufacturer’s recommendations. Fluorescence signals were scanned and analyzed applying the 3D-Gene Scanner (TORAY, Tokyo, Japan). This chip contained a total number of 2168 genes. Data of miRNA expression were scaled by global normalization and the hybridization intensity data were normalized to 1000 total signal intensities of each array, then the differential expression was investigated. Welch’s t test was applied to analyze significant correlation.
Quantitative real-time polymerase chain reaction (QRT-PCR) for miRNAs of circulating exosomes
MiRNA expression of circulating exosomes was assayed using QRT-PCR. Derived from the above miRNA microarray, miR-1246 and miR-155 were most significantly upregulated in trastuzumab-resistant patients compared with sensitive patients. Relative expression of miRNAs was detected by a real-time PCR instrument (Eppendorf Mastercycler ep realplex, Eppendorf, Hamburg, Germany) using miScript SYBR Green PCR Kit (Qiagen, Hilden, Germany) following the manufacture’s recommendations. The sequence of forward primer for miR-155 we used was ACGCTCAGTTAATGCTAATCGTGATA and for miR-1246 was TTCGACGTGAATGGATTTTTG, the reverse primer for miR-155 was TATGGTTTTGACGACTGTGTGAT and for miR-1246 was TATCGTTGTACTCCAGACCAAGAC. The PCR system was as follows (25 μl): 0.5 μl ROX Dye, 9 μl ddH2O, 2 μl template DNA, 0.5 μl forward primer, 0.5 μl reverse primer, and 12.5 μl SYBR Advantage Premix. The amplification protocol included an initial denaturation step at 95 °C for 10 min, followed by 40 cycles at 95 °C for 15 s and annealing at 60 °C for 60 s. MiR-16a was used as an internal control as reference miRNA in the literature [27]. The experiment was repeated three times. Relative quantification of miRNA expression was calculated using the 2−∆∆CT method. ∆CT was calculated by subtracting the CT values for miRNA-16a from the CT values for miRNA-1246 and miRNA-155. ∆∆CT was determined by subtracting average ∆CT of the control from ∆CT of cases. The data were presented as mean ± SD.
Statistical analysis
Statistical analysis was performed using the SPSS 18.0 software (SPSS Inc., Chicago, IL, USA). The significant differences of circulating exosomal miRNAs expression between trastuzumab-resistant and -sensitive patients were analyzed applying the Mann–Whitney U test. The association between expression of miRNA and clinicopathological features were analyzed applying the one-way analysis of variance (ANOVA), Chi-square test, and Student’s t test. The EFS, PFS, and OS curves were analyzed applying the method of Kaplan–Meier survival curve, and the difference was investigated applying log-rank tests. We used Cox proportional hazards regression to analyze univariate and multivariate hazard ratios (HR) for OS, EFS and PFS. Receiver-operating characteristic (ROC) curves and the area under the ROC curve (AUC) were applied to analyze the sensitivity and specificity of the miRNAs in the prediction of trastuzumab resistance in the patients. The optimal cutoff threshold value for diagnosis was calculated by Youden’s Index (specificity + sensitivity-1). Univariate analysis was performed for each factor, while multivariate analysis was applied for factors that demonstrated significance in univariate analysis. All p values are 2-sided, and a p value < 0.05 was considered statistically significant. The graphs were generated using GraphPad Prism 6.0 (GraphPad Software, San Diego, CA, USA) and SPSS 18.0 (SPSS Inc., Chicago, IL, USA).
Results
Patient characteristics
109 consecutive early-stage breast cancer patients and 71 metastatic patients met the inclusion criteria, two early-stage patients and three metastatic patients were lost from follow-up; therefore, a total of 107 early-stage breast cancer patients and 68 metastatic patients were included in this study. Treatment and baseline characteristics of the entire patients are summarized in Tables 1 and 2, and the parameter data listed in inclusion criteria were all available for investigation. Of the early-stage patients, 48 cases received trastuzumab-contained neoadjuvant treatment for at least four cycles, then accepted surgical therapy with postoperative evaluation of pathological response, and 13 patients achieved PCR (Table 3). As for clinical outcomes, the early-stage patients were followed up for a median observation period of 44 months (range from 4 to 72 months), 23 patients had local recurrence or distant metastasis, and five deaths had occurred, all of which were attributed to disease progression. The metastatic patients were followed up for a median observation period of 39 months (range from 5 to 71 months), and 12 deaths had occurred which were also attributed to disease progression.
Characterization of the isolated circulating exosomes by TEM, NTA and WB analysis
We applied TEM, NTA and the WB test to verify the accuracy and efficacy of the circulating exosome extraction method (Online Resource 1). Microvesicle clusters in circulation represented round vesicular membranes and the greatest dimension measured 50–200 nm. The extraction of exosomes was also analyzed using WB test applying antibodies specific for the exosomes biomarkers CD81 and CD63, which are members of tetraspanin family that localizes to the internal vesicles of exosomes [28]. As the 29 and 45 kDa bands visible, CD81 and CD63 specific antibodies distinguished the exosomes in the pellet, respectively, but did not find any exosomes in the supernatant.
Different circulating exosomal miRNA signatures in trastuzumab-resistant and -sensitive patients
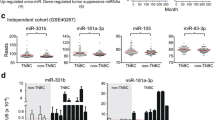
Following qualitative analysis of circulating exosomes, we investigated the expression of miRNA profiles in circulating exosomes derive from serum of four metastatic HER2-positive breast cancer patients who progressed within 1 year of trastuzumab-contained therapy (trastuzumab resistance) and four patients with partial or complete response (trastuzumab sensitive). We aimed to pick up the exosomal miRNAs which are most differentially expressed between the two groups from the panel of 2168 miRNAs. Result shows that 16 exosomal miRNAs were demonstrated to be markedly differentially expressed (p < 0.005) between the trastuzumab-resistant and -sensitive patients, including miR-1246, miR-155, miR-376c, miR-660, miR-99b, miR-665, miR-195, miR-223-3p, miR-30c-5p, miR-6238, miR-222, miR-7040, miR-122, miR-215, miR-885-5p, and miR-3663-3p (Online Resource 2). Among these microRNAs, miR-1246 and miR-155 showed the highest fold-change (23.45 and 21.39, respectively). We selected circulating exosomal miR-1246 and miR-155 as potential markers for predicting trastuzumab resistance in breast cancer patients in further investigation.
Relationship between selected circulating exosomal miRNAs and trastuzumab resistance in metastatic breast cancer patients
In 68 metastatic patients, the median level of miR-1246 was 1.858 (range from 0.125 to 6.003, SD = 1.564) in the entire cases, 2.747 (range from 0.125 to 6.003, SD = 1.559) in the trastuzumab-resistant patients (n = 32), and 1.168 (range from 0.288 to 5.221, SD = 1.311) in the sensitive patients (n = 36). The miR-1246 expression level was significantly upregulated in the trastuzumab resistant compared with the sensitive patients (p < 0.001) (Fig. 1a). Besides, the median level of miR-155 was 2.954 (range from 0.147 to 10.123, SD = 2.208) in the entire cases, 3.569 (range from 0.202 to 10.123, SD = 2.541) in the trastuzumab-resistant patients, and 2.099 (range from 0.147 to 7.066, SD = 1.708) in the sensitive patients. The expression of miR-155 was significantly upregulated in the trastuzumab resistant compared with the sensitive patients (p < 0.001) (Fig. 1b).
We performed ROC curve analysis in 68 metastatic patients to discuss the threshold of miR-1246 level that best discriminated trastuzumab resistant from sensitive patients (Fig. 2a). The area under the ROC curve was 0.750 (95% CI 0.626–0.875; P < 0.001) and the optimal cutoff value of 1.85750 could best discriminated the resistant from sensitive patients. The Youden’s Index, specificity, and sensitivity of the 1.85750 threshold were 0.531, 75, and 78.1%, respectively. We also performed ROC curve analysis to discuss the threshold of miR-155 level (Fig. 2b). The area under the ROC curve was 0.877 (95% CI 0.794–0.961; P < 0.001) and the cutoff value was 3.966. The Youden’s Index, specificity, and sensitivity of the 3.966 threshold were 0.66, 97.2, and 68.8%, respectively. The relative expression of circulating exosomal miR-1246 or miR-155 greater than or equal to the cutoff value derived from the ROC curve analysis was deemed as high level.
The ROC curve analysis further proved the role of miR-1246 and miR-155 in stratifying resistant and sensitive patients, separately. To improve the discrimination, the concentrations of exosomal miR-1246 and miR-155 were combined by logistic regression. The combined scores of these exosomal miRNAs could discriminate between resistant and sensitive patients with the area under the ROC curve was 0.898 (95% CI 0.822–0.975; P < 0.001) (Fig. 2c). These demonstrated the combination of the two miRNAs exhibited better predictive power compared the any individual miRNA and would be relevant for a robust biomarker.
Relationship between clinicopathological factors and selected circulating exosomal miRNAs
The association between the circulating exosomal miRNAs expression and key clinicopathological features was analyzed and results are shown in Table 4. Among the 107 early-stage patients, the exosomal expression of miR-1246 was significantly higher in the clinical T3-4 tumor patients compared to T1-2 tumor patients (p = 0.026).
Predictive value of selected circulating exosomal miRNAs
In early-stage patients treated with trastuzumab-contained therapy, we performed logistic regression analysis to discuss the predictive value of circulating exosomal miR-1246 and miR-155 along with key clinicopathological features. Clinical lymph nodal status (P < 0.001), miR-1246 (P < 0.001), and miR-155 (P = 0.001) were significantly correlated with EFS in univariate analysis. In addition, multivariate analysis indicated that clinical lymph node status (p = 0.001), high level of miR-1246 (p = 0.001) and high level of miR-155 (p = 0.005) were independent predictors of poor EFS (Table 5).
In early-stage patients, 48 cases accepted trastuzumab-contained neoadjuvant treatment. Logistic regression analysis revealed clinical tumor size (p = 0.020), lymph node status (p = 0.003), and miR-1246 (p = 0.020) were significantly correlated with PCR in univariate analysis. However, multivariate analysis demonstrated that no factor acted as independent predictor of PCR (Table 6).
In metastatic patients treated with trastuzumab-contained therapy, we performed logistic regression analysis to discuss the predictive value of miR-1246 and miR-155 along with key clinicopathological features. HR status (p = 0.005), miR-1246 (P < 0.001), and miR-155 (p < 0.001) were significantly associated with PFS in univariate. Multivariate analysis indicated that high level of miR-1246 (p = 0.006), and high level of miR-155 (p < 0.001) were independent predictors of poor PFS (Online Resource 3).
Prognostic value of selected circulating exosomal miRNAs
In early-stage patients treated with trastuzumab-contained therapy, Cox proportional hazards regression was performed to discuss the prognostic value of circulating exosomal miR-1246 and miR-155 along with key clinicopathological features. Lymph node status (P = 0.005), miR-1246 level (P = 0.002), and miR-155 level (P = 0.003) were significantly correlated with EFS in univariate analysis. Multivariate analysis indicated that clinical lymph node status (p = 0.008), high level of miR-1246 (P = 0.002) and high level of miR-155 (p = 0.014) were independent predictors of poor EFS (Online Resource 4). Besides, univariate analysis demonstrated no factors were significantly correlated with OS (Online Resource 5).
In metastatic patients treated with trastuzumab-contained therapy, univariate analysis demonstrated that PFS was correlated with HR status (P = 0.006), miR-1246 (P < 0.001), and miR-155 (P < 0.001). Multivariate analysis for PFS revealed that HR status (p = 0.018), high level of miR-1246 (p = 0.008) and high level of miR-155 (p < 0.001) were independent predictors of poor PFS (Online Resource 6). Besides, univariate analysis showed age of patients (p = 0.033) was significantly correlated with OS (Online Resource 7).
Kaplan–Meier survival analysis demonstrated early-stage patients with high level of circulating exosomal miR-1246 had poor EFS compared to those with low level (log-rank test, p = 0.001) (Fig. 3a), and patients with high level of circulating exosomal miR-155 also had poor EFS (log-rank test, p = 0.001) (Fig. 3b). But early-stage patients with high or low level of these two miRNAs had no significant difference in OS (Fig. 3c, d). Besides, metastatic patients with high level of circulating exosomal miR-1246 had poor PFS compared to those with low level (log-rank test, p < 0.001) (Fig. 3e), patients with high level of circulating exosomal miR-155 also had poor PFS (log-rank test, p < 0.001) (Fig. 3f). Concerning OS, metastatic patients with high or low level of these two miRNAs still had no significant difference (Fig. 3g, h).
Survival curves of patients with high-level versus low-level relative expression of selected miRNAs. a EFS curves of early-stage patients with high-level versus low-level miR-1246. b EFS curves of early-stage patients with high-level versus low-level miR-155. c OS curves of early-stage patients with high-level versus low-level miR-1246. d OS curves of early-stage patients with high-level versus low-level miR-155. e PFS curves of metastatic patients with high-level versus low-level miR-1246. f PFS curves of metastatic patients with high-level versus low-level miR-155. g OS curves of metastatic patients with high-level versus low-level miR-1246. h OS curves of metastatic patients with high-level versus low-level miR-155
Discussion
The present research used microarray profiling of exosomal miRNAs and identified miR-1246 and miR-155 as the most significantly changed miRNAs in trastuzumab-resistant breast cancer patients compared to sensitive patients. Next, we investigated the selected miRNAs value based on ROC curve methodology and the results revealed miR-1246 and miR-155 were significantly associated with trastuzumab effect in metastatic patients. Then, our research revealed that upregulated expression of miR-1246 and miR-155 was predictive factors for poor trastuzumab reaction in early-stage and metastatic patients. In prognostic analysis, the data also suggested high expression of miR-1246 and miR-155 patients might have poor EFS in early-stage patients and poor DFS in metastatic patients, but OS was not significantly associated with either selected miRNAs. As we know, this is the first research to evaluate the predictive and prognostic role of exosomal miRNAs selected from microarray profiling in trastuzumab resistance in HER2-positive early-stage and metastatic breast cancer patients.
Breast cancer is a molecularly heterogeneous disease, exhibiting variations in gene expression signatures, clinical outcome and response to therapeutic options. HER2-positive breast cancers tend to be more aggressive than other types and they are associated with worse prognosis. Although HER2-positive breast cancer shows a decrease in the response to chemotherapy and hormonal treatments, development of HER2-targeted therapies has significantly increased clinical benefit in adjuvant and metastatic settings. Despite the major advances made in the field of anti-HER2 immunotherapy, many tumors treated with trastuzumab are either insensitive even before treatment with trastuzumab-based therapy begins (innate resistance to trastuzumab) or may eventually develop resistance to therapy during the course of treatment (acquired resistance to trastuzumab). Among other aspects, cellular and molecular heterogeneity in breast tumors may increase the selection of tumor subpopulations containing molecular alterations that can lead to the development of different cellular phenotypes and behaviors, such as drug resistance. We wish to explore reliable and feasible factors which could distinguish between trastuzumab resistance patients and -sensitive patients.
Testing of non-invasive biomarker which could allow improved monitoring, and the early identification of metastatic breast cancer is of greater clinical value. Traditional circulating biomarkers included CA15-3, CA 125 and CEA, increasing expression level of these circulating biomarkers in breast cancer patients’ plasma have been proved to forecast the development of recurrence and metastases [29, 30]. Nevertheless, these traditional circulating biomarkers still lack sufficient specificity and sensitivity to facilitate identification of therapeutic resistance and early detection of cancer metastasis. Quantification of circulating tumor cells (CTCs) was proved to be an independent prognostic factor of cancer relapse [31, 32]. However, CTCs are not appropriate method for monitoring therapeutic response because accurately detection tumor cells from the blood circulation requires relatively large sample [33]. In addition, detection of CTCs demands expression of known and sometimes variable markers with high quality antibodies needed for the profiling [34]. Our study demonstrated that peculiar circulating exosomal miRNAs could serve as credible, easy-available, predictive and prognostic biomarkers for treatment resistance.
There are several circulating microRNAs that have been reported to identify patients with differential responses to HER2-targeted therapy. Increased expression of circulating miR-21, miR-150-5p, and miR-4734 showed association with poor clinical outcomes in HER2-positive non-metastatic BC patients, which have been treated with neoadjuvant therapy or adjuvant therapy with or without trastuzumab [27, 35]. Although miR-210 was initially shown to be a predictive factor of response to trastuzumab, it was later revealed to be linked with decreased EFS [36]. Besides, circulating miR-140-5p levels after 2 weeks of receiving trastuzumab appeared to be associated with EFS in BC patients [37]. In this study, we reported that circulating exosomal miR-1246 and miR-155 could individually or in combination serve as predictive and prognostic factors for trastuzumab-based therapy resistance in HER2-positive breast cancer. Exosomal miR-1246 has been previously reported with higher expression in BC patients than healthy controls [38], and shown to facilitate cell proliferation, invasion and drug resistance by CCNG2 targeting [39]. Exosomal miR-155 secreted by breast cancer cell were revealed to be likely responsible for triggering metastasis by inducing cancer-associated cachexia through metabolistic reprogramming of adipocytes and muscle cells [40]. However, the function and mechanism for miR-1246 and miR-155 in trastuzumab responsive regulation of HER2 BC patients remain worth study to shed light on their potential therapeutic applications.
Our study has limitations. This trial included a relatively small number of patients and short follow-up. Besides, this trial was designed to assess role of selected miRNAs for trastuzumab resistance. With usage of pertuzumab, ado-trastuzumab emtansine, and neratinib more popular, exploration resistance mechanism and predictive factors for these anti-HER2 monoclonal antibodies in breast cancer patients are necessary. The results of our study manifested miR-1246 and miR-155 could be predictive and prognostic factors in trastuzumab resistance, but their directly targets which were prove oncogenic feature were not evaluated in tumor specimen. In future study, target genes and proteins expression of selected miRNAs need assess to inquire into the mechanism of miR-1246 and miR-155-induced trastuzumab resistance.
This study also has several strengths and implications. As far as we known, this work confirmed the hypothesis for the first time that circulating exosomal miR-1246 and miR-155 predict clinical prognosis of breast cancer patients treated with trastuzumab-based therapy. Given the hypothesis-generating value of these findings, additional research is warranted to intensively study the mechanism of miR-1246 and miR-155-induced trastuzumab resistance, by which it is possible to develop new agents to reverse trastuzumab resistance and enhance trastuzumab curative effect in HER2-positive breast cancer treatment.
References
Scott LC, Mobley LR, Kuo TM, Il’yasova D (2019) Update on triple-negative breast cancer disparities for the United States: a population-based study from the United States Cancer Statistics database, 2010 through 2014. Cancer 125(19):3412–3417. https://doi.org/10.1002/cncr.32207
Ziaeemehr A, Shahidsales S, Ghosi Z, Avan A, Aldavood AS, Anvari K, Makhdoomi Y, Asadi M (2019) Association of the involvement of axillary lymph nodes in HER-2/neu overexpression in patients with breast cancer. Breast J 25(3):537–538. https://doi.org/10.1111/tbj.13282
Giannone G, Milani A, Geuna E, Galizia D, Biello F, Montemurro F (2019) What is the best pharmacotherapeutic strategy for HER-2 positive breast cancer? Expert Opin Pharmacother 20(1):5–9. https://doi.org/10.1080/14656566.2018.1543406
Tolaney SM, Guo H, Pernas S, Barry WT, Dillon DA, Ritterhouse L, Schneider BP, Shen F, Fuhrman K, Baltay M, Dang CT, Yardley DA, Moy B, Marcom PK, Albain KS, Rugo HS, Ellis MJ, Shapira I, Wolff AC, Carey LA, Overmoyer B, Partridge AH, Hudis CA, Krop IE, Burstein HJ, Winer EP (2019) Seven-year follow-up analysis of adjuvant paclitaxel and trastuzumab trial for node-negative, human epidermal growth factor receptor 2-positive breast cancer. J Clin Oncol 37(22):1868–1875. https://doi.org/10.1200/JCO.19.00066
Daniels B, Kiely BE, Lord SJ, Houssami N, Lu CY, Ward RL, Pearson SA (2018) Long-term survival in trastuzumab-treated patients with HER2-positive metastatic breast cancer: real-world outcomes and treatment patterns in a whole-of-population Australian cohort (2001–2016). Breast Cancer Res Treat 171(1):151–159. https://doi.org/10.1007/s10549-018-4804-0
Watanabe S, Yonesaka K, Tanizaki J, Nonagase Y, Takegawa N, Haratani K, Kawakami H, Hayashi H, Takeda M, Tsurutani J, Nakagawa K (2019) Targeting of the HER2/HER3 signaling axis overcomes ligand-mediated resistance to trastuzumab in HER2-positive breast cancer. Cancer Med 8(3):1258–1268. https://doi.org/10.1002/cam4.1995
Masuda N, Ohtani S, Takano T, Inoue K, Suzuki E, Nakamura R, Bando H, Ito Y, Ishida K, Yamanaka T, Kuroi K, Yasojima H, Kasai H, Takasuka T, Sakurai T, Kataoka TR, Morita S, Ohno S, Toi M (2020) A randomized, 3-arm, neoadjuvant, phase 2 study comparing docetaxel + carboplatin + trastuzumab + pertuzumab (TCbHP), TCbHP followed by trastuzumab emtansine and pertuzumab (T-DM1+P), and T-DM1+P in HER2-positive primary breast cancer. Breast Cancer Res Treat 180(1):135–146. https://doi.org/10.1007/s10549-020-05524-6
Zhu C, Li L, Wang Z, Irfan M, Qu F (2020) Recent advances of aptasensors for exosomes detection. Biosens Bioelectron 160:112213. https://doi.org/10.1016/j.bios.2020.112213
Sun D, Zhuang X, Zhang S, Deng ZB, Grizzle W, Miller D, Zhang HG (2013) Exosomes are endogenous nanoparticles that can deliver biological information between cells. Adv Drug Deliv Rev 65(3):342–347. https://doi.org/10.1016/j.addr.2012.07.002
Zhai LY, Li MX, Pan WL, Chen Y, Li MM, Pang JX, Zheng L, Chen JX, Duan WJ (2018) In situ detection of plasma exosomal microRNA-1246 for breast cancer diagnostics by a Au nanoflare probe. ACS Appl Mater Interfaces 10(46):39478–39486. https://doi.org/10.1021/acsami.8b12725
Sueta A, Yamamoto Y, Tomiguchi M, Takeshita T, Yamamoto-Ibusuki M, Iwase H (2017) Differential expression of exosomal miRNAs between breast cancer patients with and without recurrence. Oncotarget 8(41):69934–69944. https://doi.org/10.18632/oncotarget.19482
Yang SJ, Wang DD, Li J, Xu HZ, Shen HY, Chen X, Zhou SY, Zhong SL, Zhao JH, Tang JH (2017) Predictive role of GSTP1-containing exosomes in chemotherapy-resistant breast cancer. Gene 623:5–14. https://doi.org/10.1016/j.gene.2017.04.031
Dong H, Wang W, Chen R, Zhang Y, Zou K, Ye M, He X, Zhang F, Han J (2018) Exosome-mediated transfer of lncRNASNHG14 promotes trastuzumab chemoresistance in breast cancer. Int J Oncol 53(3):1013–1026. https://doi.org/10.3892/ijo.2018.4467
Han M, Hu J, Lu P, Cao H, Yu C, Li X, Qian X, Yang X, Yang Y, Han N, Dou D, Zhang F, Ye M, Yang C, Gu Y, Dong H (2020) Exosome-transmitted miR-567 reverses trastuzumab resistance by inhibiting ATG5 in breast cancer. Cell Death Dis 11(1):43. https://doi.org/10.1038/s41419-020-2250-5
Hosseinahli N, Aghapour M, Duijf PHG, Baradaran B (2018) Treating cancer with microRNA replacement therapy: a literature review. J Cell Physiol 233(8):5574–5588. https://doi.org/10.1002/jcp.26514
Quan J, Liu S, Dai K, Jin L, He T, Pan X, Lai Y (2018) MicroRNA-23a/24–2/27a as a potential diagnostic biomarker for cancer: a systematic review and meta-analysis. Mol Clin Oncol 8(1):159–169. https://doi.org/10.3892/mco.2017.1492
Zhang Z, Zhang L, Wang B, Wei R, Wang Y, Wan J, Zhang C, Zhao L, Zhu X, Zhang Y, Chu C, Guo Q, Yin X, Li X (2020) MiR-337–3p suppresses proliferation of epithelial ovarian cancer by targeting PIK3CA and PIK3CB. Cancer Lett 469:54–67. https://doi.org/10.1016/j.canlet.2019.10.021
Shah MY, Calin GA (2013) The mix of two worlds: non-coding RNAs and hormones. Nucleic Acid Ther 23(1):2–8. https://doi.org/10.1089/nat.2012.0375
Hu Y, Qi C, Liu X, Zhang C, Gao J, Wu Y, Yang J, Zhao Q, Li J, Wang X, Shen L (2019) Malignant ascites-derived exosomes promote peritoneal tumor cell dissemination and reveal a distinct miRNA signature in advanced gastric cancer. Cancer Lett 457:142–150. https://doi.org/10.1016/j.canlet.2019.04.034
Alfonsi R, Grassi L, Signore M, Bonci D (2018) The double face of exosome-carried microRNAs in cancer immunomodulation. Int J Mol Sci. https://doi.org/10.3390/ijms19041183
Yoshikawa M, Iinuma H, Umemoto Y, Yanagisawa T, Matsumoto A, Jinno H (2018) Exosome-encapsulated microRNA-223–3p as a minimally invasive biomarker for the early detection of invasive breast cancer. Oncol Lett 15(6):9584–9592. https://doi.org/10.3892/ol.2018.8457
Guraya S (2018) Prognostic significance of circulating microRNA-21 expression in esophageal, pancreatic and colorectal cancers; a systematic review and meta-analysis. Int J Surg 60:41–47. https://doi.org/10.1016/j.ijsu.2018.10.030
Jinling W, Sijing S, Jie Z, Guinian W (2017) Prognostic value of circulating microRNA-21 for breast cancer: a systematic review and meta-analysis. Artif Cells Nanomed Biotechnol 45(6):1–6. https://doi.org/10.1080/21691401.2016.1216856
Jiang Z, Ma J, Wang Q, Wu F, Ping J, Ming L (2017) Circulating microRNA expression and their target genes in deep vein thrombosis: a systematic review and bioinformatics analysis. Medicine (Baltimore) 96(50):e9330. https://doi.org/10.1097/MD.0000000000009330
McShane LM, Altman DG, Sauerbrei W, Taube SE, Gion M, Clark GM, Statistics Subcommittee of the NCIEWGoCD (2005a) REporting recommendations for tumour MARKer prognostic studies (REMARK). Br J Cancer 93(4):387–391. https://doi.org/10.1038/sj.bjc.6602678
McShane LM, Altman DG, Sauerbrei W, Taube SE, Gion M, Clark GM, Statistics Subcommittee of the NCIEWGoCD (2005b) Reporting recommendations for tumor MARKer prognostic studies (REMARK). Nat Clin Pract Urol 2(8):416–422
Muller V, Gade S, Steinbach B, Loibl S, von Minckwitz G, Untch M, Schwedler K, Lubbe K, Schem C, Fasching PA, Mau C, Pantel K, Schwarzenbach H (2014) Changes in serum levels of miR-21, miR-210, and miR-373 in HER2-positive breast cancer patients undergoing neoadjuvant therapy: a translational research project within the Geparquinto trial. Breast Cancer Res Treat 147(1):61–68
Stevic I, Muller V, Weber K, Fasching PA, Karn T, Marme F, Schem C, Stickeler E, Denkert C, van Mackelenbergh M, Salat C, Schneeweiss A, Pantel K, Loibl S, Untch M, Schwarzenbach H (2018) Specific microRNA signatures in exosomes of triple-negative and HER2-positive breast cancer patients undergoing neoadjuvant therapy within the GeparSixto trial. BMC Med 16(1):179. https://doi.org/10.1186/s12916-018-1163-y
Di Gioia D, Stieber P, Schmidt GP, Nagel D, Heinemann V, Baur-Melnyk A (2015) Early detection of metastatic disease in asymptomatic breast cancer patients with whole-body imaging and defined tumour marker increase. Br J Cancer 112(5):809–818. https://doi.org/10.1038/bjc.2015.8
Nicolini A, Carpi A, Ferrari P, Morganti R, Mazzotti V, Barak V, Duffy MJ (2018) An individual reference limit of the serum CEA-TPA-CA 15–3 tumor marker panel in the surveillance of asymptomatic women following surgery for primary breast cancer. Cancer Manag Res 10:6879–6886. https://doi.org/10.2147/CMAR.S177522
Tsoutsou PG, Vozenin MC (2019) Circulating tumor cells and radiotherapy benefit in early breast cancer. JAMA Oncol 5(1):111–112. https://doi.org/10.1001/jamaoncol.2018.5077
Gao C, Xiao G, Piersigilli A, Gou J, Ogunwobi O, Bargonetti J (2019) Context-dependent roles of MDMX (MDM4) and MDM2 in breast cancer proliferation and circulating tumor cells. Breast Cancer Res 21(1):5. https://doi.org/10.1186/s13058-018-1094-8
van Schaijik B, Wickremesekera AC, Mantamadiotis T, Kaye AH, Tan ST, Stylli SS, Itinteang T (2019) Circulating tumor stem cells and glioblastoma: a review. J Clin Neurosci 61:5–9. https://doi.org/10.1016/j.jocn.2018.12.019
Vafaei S, Fattahi F, Ebrahimi M, Janani L, Shariftabrizi A, Madjd Z (2019) Common molecular markers between circulating tumor cells and blood exosomes in colorectal cancer: a systematic and analytical review. Cancer Manag Res 11:8669–8698. https://doi.org/10.2147/CMAR.S219699
Du F, Yuan P, Zhao ZT, Yang Z, Wang T, Zhao JD, Luo Y, Ma F, Wang JY, Fan Y, Cai RG, Zhang P, Li Q, Song YM, Xu BH (2016) A miRNA-based signature predicts development of disease recurrence in HER2 positive breast cancer after adjuvant trastuzumab-based treatment. Sci Rep 6:33825. https://doi.org/10.1038/srep33825
Jung EJ, Santarpia L, Kim J, Esteva FJ, Moretti E, Buzdar AU, Di Leo A, Le XF, Bast RC Jr, Park ST, Pusztai L, Calin GA (2012) Plasma microRNA 210 levels correlate with sensitivity to trastuzumab and tumor presence in breast cancer patients. Cancer 118(10):2603–2614. https://doi.org/10.1002/cncr.26565
Di Cosimo S, Appierto V, Pizzamiglio S, Tiberio P, Iorio MV, Hilbers F, de Azambuja E, de la Pena L, Izquierdo M, Huober J, Baselga J, Piccart M, de Braud FG, Apolone G, Verderio P, Daidone MG (2019) Plasma miRNA levels for predicting therapeutic response to neoadjuvant treatment in HER2-positive breast cancer: results from the NeoALTTO trial. Clin Cancer Res 25(13):3887–3895. https://doi.org/10.1158/1078-0432.CCR-18-2507
Wang M, Ji S, Shao G, Zhang J, Zhao K, Wang Z, Wu A (2018) Effect of exosome biomarkers for diagnosis and prognosis of breast cancer patients. Clin Transl Oncol 20(7):906–911. https://doi.org/10.1007/s12094-017-1805-0
Li XJ, Ren ZJ, Tang JH, Yu Q (2017) Exosomal MicroRNA MiR-1246 promotes cell proliferation, invasion and drug resistance by targeting CCNG2 in breast cancer. Cell Physiol Biochem 44(5):1741–1748. https://doi.org/10.1159/000485780
Wu Q, Sun S, Li Z, Yang Q, Li B, Zhu S, Wang L, Wu J, Yuan J, Yang C, Li J, Sun S (2018) Tumour-originated exosomal miR-155 triggers cancer-associated cachexia to promote tumour progression. Mol Cancer 17(1):155. https://doi.org/10.1186/s12943-018-0899-5
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All the authors declare no conflicts of interest.
Ethical approval
All the procedures performed in studies involving human participants were in accordance with the ethical standards of Shandong Provincial Hospital, and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
280_2020_4168_MOESM1_ESM.docx
Supplementary file1 Online Resource. 1 Verification and quantification of circulating exosomes. (A) Circulating exosomes were observed under a transmission electron microscope and showed round-shaped vesicles of different sizes (scale bars=100nm). (B) The size distribution of the circulating exosomes. (C) Exosomal specific biomarker CD63 and CD81 were detected by western blotting in sample 1 (trastuzumab resistant patients) and sample 2 (trastuzumab sensitive patients) (TIF 1348 kb)
Rights and permissions
About this article
Cite this article
Zhang, Z., Zhang, L., Yu, G. et al. Exosomal miR-1246 and miR-155 as predictive and prognostic biomarkers for trastuzumab-based therapy resistance in HER2-positive breast cancer. Cancer Chemother Pharmacol 86, 761–772 (2020). https://doi.org/10.1007/s00280-020-04168-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00280-020-04168-z