Abstract
Purpose
Ibrutinib is an orally administered, irreversible Bruton’s tyrosine kinase inhibitor for treatment of B-cell malignancy. This study evaluated the effects of single-dose ibrutinib at therapeutic and supratherapeutic exposures on cardiac repolarization in healthy subjects.
Methods
Part 1 used an open-label, two-period sequential design to assess the safety and pharmacokinetics of single doses of ibrutinib 840 and 1680 mg in eight subjects. Part 2 was a randomized, placebo- and positive (moxifloxacin)-controlled, double-blind, single dose, four-way cross-over study to assess the effect of ibrutinib (840 and 1680 mg) on QT/QTc interval. 64 healthy subjects were planned to be enrolled. Baseline-adjusted QT (QTc) intervals for ibrutinib and moxifloxacin (assay sensitivity) were compared to placebo using linear mixed-effect model. A concentration-QTc analysis was also conducted.
Results
No clinically relevant safety observations were noted in Part 1. During Part 2, one subject experienced Grade 4 ALT/AST elevations with ibrutinib 1680 mg, leading to study termination and limiting the enrollment to 20 subjects. Ibrutinib demonstrated dose-dependent increases in exposure. The upper bounds of the 90% CIs for the mean difference in change from baseline in QTc between ibrutinib and placebo were < 10 ms at all timepoints and at supratherapeutic C max. Moxifloxacin showed the anticipated QTc effect, confirming assay sensitivity despite the early study termination. Ibrutinib caused a concentration-dependent mild shortening of QTc and mild PR prolongation, but these effects were not considered clinically meaningful.
Conclusions
Therapeutic and supratherapeutic concentrations of ibrutinib do not prolong the QTc interval.
Clinicaltrials.gov
NCT02271438.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Ibrutinib (IMBRUVICA®), is a first-in-class, potent, orally administered, covalently binding inhibitor of Bruton’s tyrosine kinase [1, 2]. It is approved in the US, EU, and other regions for the treatment of patients with mantle cell lymphoma (MCL; 560 mg per day) who have received at least 1 prior therapy, patients with chronic lymphocytic leukemia (CLL; 420 mg per day) or small lymphocytic lymphoma (SLL; 420 mg per day), and patients with CLL/SLL with 17p deletion, and patients with Waldenström’s macroglobulinemia (WM; 420 mg per day) [3]. In the US, it is now also approved for the treatment of patients with marginal zone lymphoma (MZL; 560 mg per day) who require systemic therapy and have received at least one prior anti-CD20-based therapy [3].
Preclinical cardiovascular safety of ibrutinib has been assessed in in vitro and in vivo studies. In vitro radioligand binding studies and human ether-à-go-go-related gene (hERG) ion channel studies identified no specific risks to human cardiac safety [4]. In vivo safety pharmacology assessments performed in telemetry monitored dogs identified increased PR interval, lowered heart rate, and shortened heart rate-corrected QT (QTc) interval [4].
The positive benefit/risk ratio of ibrutinib has been established in multiple Phase 3 settings [5,6,7] and does not indicate any clinically meaningful QTc changes in a predominately elderly population many of whom have known cardiovascular disease at baseline. Electrocardiogram (ECG) monitoring performed in two open-label Phase 1b/2 single-agent ibrutinib studies (NCT01105247; NCT00849654) has shown no evidence of ECG morphological changes and QTc prolongation (> 500-ms absolute value or > 60-ms shift from baseline) in subjects treated with ibrutinib administered at doses ranging from 420-mg once-daily to 840-mg once-daily [8]. In the Phase 1b/2 study in patients with CLL/SLL, ibrutinib treatment was associated with a tendency for mild QTc shortening, mild heart rate slowing, and mild PR prolongation [8].
As prolongation of QTc can be a clinically significant adverse event of some non-antiarrhythmic drugs, a rigorous characterization of a drug’s ability to prolong QTc is required [9, 10].
This study was designed as two parts: first, confirm that ibrutinib 840- and 1680-mg single doses were well tolerated in Part 1 of the study, followed by a placebo- and positive-controlled, four-way crossover, blinded, thorough QT/QTc study in Part 2 to evaluate the effect of single doses of therapeutic and supratherapeutic ibrutinib exposure on cardiac repolarization in healthy adults. The study design and the doses selected (840-mg single dose, ensuring exposures in line with those observed at steady-state after the highest therapeutic dose of 560 mg/day, and 1680-mg dose level to obtain the supratherapeutic exposure) were suggested and approved by the Interdisciplinary Review Team (IRT) at the FDA. Exposures were further enhanced by dosing under non-fasted condition after a high-fat breakfast [11].
Materials and methods
This study (NCT02271438) was conducted at the Phase 1 Clinical Pharmacology Unit of Janssen R & D in Belgium from 27 October 2014 to 04 May 2015. Protocol and amendments(s) were reviewed and approved by an Independent Ethics Committee. The study was conducted in accordance with the ethical principles communicated in the Declaration of Helsinki and in accordance with the International Conference on Harmonization (ICH) Good Clinical Practice guidelines, applicable regulatory requirements and in compliance with the protocol. Study subjects provided written informed consent prior to study participation. The design of Part 2 of this study followed the general design principles outlined in the ICH E14 guidance for the clinical evaluation of the QT/QTc interval with non-antiarrhythmic drugs [9].
Study population
Healthy men and healthy women of non-child bearing potential, aged between 18 and 55 years (inclusive), with a body mass index (BMI) between 18.0 and 30.0 kg/m2 (inclusive) and weighing not less than 50 kg were eligible for enrollment in this study. Subjects were non-smokers with normal 12-lead ECG recordings demonstrating normal cardiac rhythm and conduction and normal blood pressure at screening. Subjects with QTc interval between 350 and 430 ms (men) or 450 ms (women), QRS interval of ≤ 110 ms, and PR interval of ≤ 200 ms were eligible for enrollment in the study. Subjects with a history of long or short QT syndrome, clinically relevant heart rhythm disturbances (atrial, junctional, re-entry, and ventricular tachycardias), heart blocks, unusual T-wave morphology likely to interfere with QT interval measurement, electrolyte abnormalities (≥ Grade 2 hypokalemia, hypocalcemia, hypomagnesemia), or clinically significant medical illness were excluded from the study.
Concomitant medications
The use of required doses of acetaminophen/paracetamol and hormone replacement therapy was permitted. Prescription medications and over-the-counter medications including homeopathic medications, dietary supplements, or herbal medications were prohibited within 14 days before participation and during the study.
Study design and treatments
This was a single-center, two-part, study in healthy subjects. In the open-label, two-period sequential Part 1, subjects were administered a single dose of ibrutinib 840 mg (6 × 140-mg capsules; therapeutic exposure) and six placebo capsules in period 1 and ibrutinib 1680 mg (12 × 140-mg capsules; supratherapeutic exposure) in period 2. The two treatment periods were separated by a washout period of minimally 7 days. The objective of Part 1 of the study was to assess the safety, tolerability, and pharmacokinetics of a single dose of ibrutinib at therapeutic and supratherapeutic exposures. Together with the screening period (20 days) and the follow-up visit 10 days after the last dose, the total planned study duration for each subject was 42 days.
Part 2, a four-way cross-over, randomized, single-dose, double-blind, placebo- and positive (moxifloxacin) controlled study, was initiated after confirmation of adequate tolerability and adequate ibrutinib exposure with the supratherapeutic dose in Part 1. In Part 2, subjects were randomized to receive single doses of ibrutinib 840 mg, ibrutinib 1680 mg, and placebo and moxifloxacin 400 mg after a high-fat breakfast. Treatments were randomly assigned to one of the four treatment sequences with a minimum 7-day washout between treatment periods. Ibrutinib was supplied as 140-mg hard gelatin capsules and moxifloxacin as 400-mg capsules. Placebo was supplied as capsules that matched ibrutinib or moxifloxacin capsules in appearance. Together with the post-treatment visit (day 4 of period 4 or at early withdrawal) and a follow-up visit 10 days after the last dose, the total planned study duration for each subject was 58–76 days.
The primary objective of Part 2 of this study was to assess the effects of a single dose of therapeutic and supratherapeutic ibrutinib exposure on QT/QTc intervals and ECG morphology in healthy adults. The secondary objectives included evaluation of the effects of ibrutinib on ECG parameters (HR, RR, PR, and QRS intervals), pharmacokinetics of ibrutinib and its metabolite PCI-45227, the potential relationship between the plasma concentrations of ibrutinib and PCI-45227 and QT/QTc changes, and the safety and tolerability of ibrutinib in healthy subjects.
Determination of the population sample size for Part 2
Approximately 64 healthy subjects were planned to be recruited to the thorough QT study to ensure that at least 52 subjects completed all required assessments. A sample size of 52 subjects was required to achieve an 80% power for obtaining 90% CIs for the difference in mean ΔQTc between each dose of ibrutinib and placebo (ΔΔQTc) at a single timepoint to fall below 10 ms. These assumptions were based on an intra-subject standard deviation (SD) for ΔQTc of 10 ms and a true difference in means between each dose of ibrutinib and placebo of 5 ms.
Pharmacokinetics
Blood samples (2.5 mL each) were collected before dosing and up to 72 h after each dose in Part 1 of the study. During Part 2, blood samples were collected before dose administration and within 5 min after each postdose 12-lead ECG recording (up to 72-h postdose). Validated liquid chromatography coupled to tandem mass spectrometry methods was used to assay plasma concentrations of ibrutinib and its metabolite PCI-45227 [12], and moxifloxacin (data on file) at Frontage Laboratories, Exton, PA, USA. Pharmacokinetic parameters included maximum plasma concentration (C max), time to C max (t max), area under the plasma concentration–time curve (AUC) from time 0–24 h (AUC24) and time of the last quantifiable concentrations (AUClast), elimination half-life (t 1/2), apparent volume of distribution (V z/F), oral clearance (CL/F, parent only), and metabolite-to-parent ratio (MPR, metabolite only). PK parameters were summarized using descriptive statistics.
Electrocardiogram and QTc analyses
In Part 2, serial 12-lead ECGs were recorded in triplicate at three timepoints before dosing (− 1 h, − 30 min, and − 10 min), at nine timepoints on the day of dosing (30 min and 1, 1.5, 2, 3, 4, 6, 8, and 12 h) and at 24, 36, 48, and 72 h postdose. ECG interval duration was measured by trained professionals using a high-resolution, semi-automatic (computer-assisted) on-screen caliper method on the “global” presentation of superimposed median PQRST complexes from all leads. The final ECG interval measurement was confirmed by a cardiologist who also performed a diagnostic assessment (e.g., normal, abnormal, myocardial infarction, ST segment elevation, etc) of the ECG at the central laboratory (Quintiles Data Processing Centre, Mumbai, India). The cardiologist also evaluated the T- and U-wave morphology. Heart rate (HR), PR, RR, QRS, and QT intervals were measured in triplicate from the 12-lead ECG. Both ECG readers and cardiologists were blinded to treatment group, treatment period, dosing day within period, timepoint within day, and subject identifiers.
QT interval data were corrected for heart rate using the Bazett formula (QTcB), Fridericia formula (QTcF), and a study-specific power model (QTcP). The baseline QTc intervals were the average of the three sets of triplicate QTc values recorded at 1 h, 30 min, and 10 min prior to dosing on day 1 of the period. The changes from baseline in QTc (ΔQTc), and the difference in ΔQTc between each treatment and placebo (ΔΔQTc), were calculated.
Primary correction method
As the slope of the effect of heart rate was still significant with QTcF, a study-specific population correction (QTcP) was computed using the estimated slope from a linear mixed effects model of log (QT) over log (RR) at baseline. QTcP was used as the primary correction method [13]. The QTcP was calculated using the formula below with the estimated population estimate of power (b):
QTc analyses were performed using the standards set by ICH E14.
QTc assay sensitivity
The assay sensitivity was assessed by evaluating the difference in mean ∆QTc between moxifloxacin and placebo (∆∆QTc) over the four pre-selected timepoints (2-, 3-, 4-, and 6-h postdose). A linear mixed effect model was applied to construct the point estimate of the mean difference in ∆QTc and the associated 90% CI. The lower limits of the 90% CI over the four pre-selected timepoints were compared to the regulatory defined threshold of 5 ms. The multiplicity corrected CI using Bonferroni procedure was not considered in assessing assay sensitivity due to the significantly reduced sample size and statistical power.
Pharmacodynamics and pharmacokinetics/pharmacodynamics analysis
All ECG variables, the corresponding change from baseline variables, and ΔΔQTc were summarized using descriptive statistics (mean, SD, and two-sided 95% CI) for each treatment and timepoint. Linear regression analysis of QT/QTc over RR at baseline was performed. A linear mixed-effects model was used with concentration as a predictor and subject as a random effect (random intercept and random slope model) to describe the relationship between ibrutinib plasma concentration and ΔΔQTc. If the intercept term was not significant, the model was refit with a zero intercept term. The analysis was also conducted with PCI-45227 plasma concentration.
Safety
Safety and tolerability were monitored throughout the study. The safety analysis was based on all subjects who received at least one dose of study drug (Part 1) or all subjects who were randomized to a treatment sequence and received at least one dose of the study drug (Part 2). Safety assessments included treatment-emergent adverse events (TEAEs), clinical laboratory tests, ECG, vital signs, and physical examination, and were summarized using descriptive statistics.
Results
Demography and participation
In Part 1, eight healthy subjects were enrolled and completed the two-period sequential treatment. The majority were women (62.5%), the median age of the subjects was 51 years (range 34–55 years), median weight was 71.4 kg (range 53.7–86.2 kg), and median body mass index (BMI) was 24.1 kg/m2 (range 20.2–27.8 kg/m2). All subjects were white. In Part 2, a total of 20 subjects of the planned 64 were randomized. Majority of the subjects were men (80.0%) and white (85.0%). The median age of the subjects was 43.5 years (range 28–54 years), median weight was 74.7 kg (range 51.4–94.0 kg), and the median BMI was 25.15 kg/m2 (range 18.2–28.5 kg/m2). Part 2 of the study was terminated early due to a safety observation in one subject; no subject received all four study treatments in the four-way crossover before termination of the study. Sixteen (80.0%) subjects had received three of the four study treatments, two (10.0%) subjects had received two study treatments, and two (10.0%) subjects had received one study treatment. Of the 16 subjects who received three of the four treatments, nine received ibrutinib (either 840 or 1680 mg or both), the negative control (placebo), and/or the positive control (moxifloxacin). Overall, 13 subjects received placebo, 14 received moxifloxacin, 13 received ibrutinib 840 mg, and 14 subjects received ibrutinib 1680 mg. Other than termination of the study by the sponsor (20 subjects), the reasons for early discontinuation from the study were adverse events (Part 2: 2 subjects), noncompliance with prohibited medications (Part 2: 1 subject), and withdrawn consent (1 subject).
Pharmacokinetics
In both Part 1 (8 subjects) and Part 2 (14 subjects) of the study, exposure to ibrutinib (AUC) increased slightly greater than dose-proportionally when the dose was increased from 840 to 1680 mg, whereas exposure to PCI-45227 increased in a dose-proportional manner. C max for ibrutinib increased in a dose-proportional manner when the dose was increased from 840 to 1680 mg and less than dose-proportional for PCI-45227. Accordingly, metabolite-to-parent ratios were lower following the 1680-mg dose compared with the 840-mg dose. With t max of approximately 4 h, absorption was slightly delayed after the ibrutinib 1680-mg dose compared to ibrutinib 840 mg, whereas terminal half-lives were similar for the two dose levels (Table 1; Fig. 1).
Of the 20 subjects enrolled in Part 2, 14 subjects received a single dose of moxifloxacin 400 mg. Maximum concentrations of moxifloxacin in plasma ranged from 148 to 3100 ng/mL, with a mean C max of 1720 ng/mL (CV = 56.1%) reached at a median t max of 3 h.
QT correction
Three different QT corrections, QTcP, QTcB, and QTcF, were applied. A power of 0.2052 was derived to compensate for the relationship between QT and RR for QTcP. Slopes (95% CI) were 0 (− 0.0393; 0.0393) for QTcP, − 0.2947 (− 0.3334; − 0.2559) for QTcB, and − 0.1284 (− 0.1676; − 0.0892) for QTcF.
QTc assay sensitivity
Assay sensitivity was assessed using moxifloxacin as the positive control. A linear mixed-effects model demonstrated that the lower limits of the 90% CIs for ∆∆QTc exceeded 5 ms following dose administration at one or more of the four timepoints across all three correction methods (at 3 h for QTcP, at 3, 4, 8, and 24 h for QTcB, and at 3, 4, 6, 8, and 24 h for QTcF). The result suggested an acceptable assay sensitivity, consistent with the overall moxifloxacin time/ QTc curve based on the past studies [8, 14,15,16].
Primary endpoint determined using QTcP
At most postdose timepoints, mean decreases from baseline in QTcP interval were observed in subjects administered with ibrutinib and placebo with changes from baseline ranging from − 10.3 to − 0.2 ms for ibrutinib 840 mg, − 6.7 to 2.1 ms for ibrutinib 1680 mg, and − 8.7 to 7.0 ms for placebo. In contrast, moxifloxacin resulted in mean changes from baseline (− 6.8 to 13.9 ms) at most postdose timepoints (Fig. 2a). Following the administration of moxifloxacin 400 mg, one subject had > 30 ms increase from baseline in QTcP; no increase of > 30 ms was observed for ibrutinib or placebo. No subject of any treatment group had a QTcP value > 450 ms or an increase from baseline > 60 ms at any timepoint during the study.
The mean QTcP values were lower with ibrutinib 840 mg than with placebo at most timepoints with the largest ∆∆QTcP being − 7.3 ms. After administration of ibrutinib 1680 mg, the largest mean ∆∆QTcP was − 4.6 ms. In contrast, the mean ∆∆QTcP values were higher with moxifloxacin than with placebo at all timepoints and ranged from 0.1 to 8.8 ms (Fig. 2b). Results from the mixed-effects model for pairwise comparisons of the exposures with ibrutinib 840-mg doses and supratherapeutic ibrutinib exposures and placebo showed that the upper bounds of the 90% CIs for mean ΔΔQTcP were < 10 ms, indicating no QTc interval prolongation with ibrutinib (Table 2). The lower limit of the 90% CI was not greater than 0 ms at any timepoint for the ibrutinib treatments.
The change in QTcF and QTcB intervals over time followed the same pattern as that for QTcP.
Heart rate
The mean values for HR were generally lower after administration of ibrutinib than at baseline across all treatment groups. There was a trend for decreasing mean values during the first 4 h after dose administration in the ibrutinib 840 mg, ibrutinib 1680 mg, and placebo groups. In contrast, the mean values were stable during the first 4 h after administration of moxifloxacin. HR > 100 bpm was not observed in any patient of any treatment group. HR < 50 bpm was observed in 13 dosing occasions (ibrutinib 840 mg: 3 [23.1%], ibrutinib 1680 mg: 5 [35.7%], placebo: 3 [23.1%], and moxifloxacin: 2 [14.3%]). All the low values for HR occurred during the first 8 h after dose administration, except for four occasions (placebo: 1 [7.7%] and ibrutinib 1680 mg: 3 [21.4%]), where low HR values occurred 24 h after dose administration.
Other ECG parameters
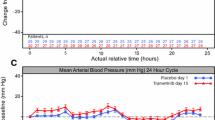
Across treatment groups, mean increases from baseline in PR interval were observed at most postdose timepoints. The mean changes from baseline ranged from − 0.4 to 3.5 ms for ibrutinib 840 mg, 0.7 to 8.2 ms for ibrutinib 1680 mg, − 2.8 to 7.1 ms for placebo, and − 0.8 to 6.3 ms for moxifloxacin 400 mg. For both doses of ibrutinib, the mean changes were larger than those for placebo between 3 and 12 h after dosing. For moxifloxacin, the mean changes were generally similar to, or lower than, those for placebo.
Mean changes in QRS interval over time were small and similar across the four treatments, with no time-related trends. The changes from baseline remained within 2 ms for all treatments.
Most subjects had normal T-waves and U-wave was absent in all subjects. One subject had an abnormal T-wave morphology on three ECGs recorded 72 h after receiving placebo and on all ECGs recorded 1, 2, and 36 h after receiving moxifloxacin 400 mg. Another subject had a known, long-standing deviation described as “flat T wave/mild inversion in the inferior lead of the ECG” which was not considered clinically significant by the investigator.
Pharmacokinetics/pharmacodynamics analysis
The PK/PD results suggested a negative relationship between plasma concentrations of ibrutinib or PCI-45227 and change in QTc. At the mean C max for ibrutinib following the administration of ibrutinib 840 mg and ibrutinib 1680 mg, the estimated ∆∆ QTcP (90% CI) was − 1.92 ms (−4.23, 0.39) and − 5.27 ms (− 9.41, − 1.13), respectively. The upper bound of the 90% CI at ibrutinib 1680 mg C max was < 10 ms. The results suggest a decrease of 0.72 and 0.76 ms in ∆∆QTcP with each 100 ng/mL increase in plasma concentration of ibrutinib (Fig. 3 ) and PCI-45277, respectively. Converted to QTcP at the therapeutic ibrutinib dose of 560 mg daily (C max = 164 ng/mL), the predicted effect is − 0.78 ms (− 2.82, 1.26). Conversely, a positive relationship between plasma concentrations of ibrutinib or PCI-45227 and change in PR interval was observed. At the mean C max for ibrutinib following the administration of ibrutinib 840 mg and ibrutinib 1680 mg, the estimated ∆∆ PR (90% CI) was 2.63 (− 0.01, 5.27) and 5.94 (1.29, 10.58), respectively.
Safety
Data for all 28 enrolled subjects were included in the safety analysis. In Part 1 of the study, a total of nine TEAEs were reported by three (37.5%) subjects, and all events were reported recovered or resolved by the end of Part 1. Single doses of ibrutinib of 840 and 1680 mg resulted in an acceptable safety profile that was well tolerated in Part 1 and the adverse event profile was similar to what has been reported in other single dose studies with ibrutinib in healthy subjects [11, 17, 18]. There were no clinically significant abnormalities in laboratory safety, vital signs, or ECGs.
In Part 2, safety data were based on the 20 subjects who received at least one dose of study medication. The most frequently occurring TEAEs (> 10% of subjects) were diarrhea (35.0%), upper abdominal pain (30.0%), nausea (20.0%), and headache (15.0%) (Table 3). The overall percentage of TEAEs was similar for all the four treatment groups (moxifloxacin 400 mg [50.0%], ibrutinib 840 mg [46.2%], ibrutinib 1680 mg [50.0%], and placebo [38.5%]). One subject in the ibrutinib 1680 mg group discontinued the study due to three SAEs: Grade 4 alanine transaminase (ALT)/aspartate transaminase (AST) increases in combination with Grade 2 myalgia and Grade 2 abdominal upper pain. Grade 2 gastroenteritis led to study discontinuation of one subject in the moxifloxacin 400 mg group which was not considered related to the study drug.
As mentioned above, one subject had Grade 4 elevations of AST (926 U/L) and ALT (3312 U/L) that began 1 day after completing period 2. The subject had received ibrutinib 840 mg 11 days earlier in period 1 and ibrutinib 1680 mg 4 days earlier in period 2. The subject was withdrawn from the study due to Grade 4 SAE (hepatic enzyme increased) and Grade 2 SAEs (myalgia and abdominal pain upper) and was hospitalized for hepatic function monitoring. Maximal elevations of ALT and AST occurred 8 days after the last ibrutinib dose and reached normal ranges after 26 days. Bilirubin remained within normal range at all timepoints. No alternative causes for the ALT/AST elevations were identified based on further investigations including viral serology, autoimmune testing, and abdominal ultrasound. The events of Grade 4 ALT/AST increase, and Grade 2 abdominal pain and Grade 2 myalgia were considered possibly drug related by the Investigator. Systemic exposure of ibrutinib and the PCI-45227 metabolite, as well as four other documented metabolites was at the lower end of the range observed in the study. Since a causal relationship of the liver function abnormalities to ibrutinib could not be ruled out, further dosing was stopped and the study was subsequently terminated by the sponsor. No clinically relevant changes in any other laboratory safety parameters or in vital signs were observed in Part 2 of the study.
Discussion
In this study, we evaluated the effects of ibrutinib on cardiac repolarization in healthy subjects as per the recommendation in the ICH14 guideline. Although the test dose of 840 mg in this study is higher than the currently approved doses of 420 and 560 mg, the higher dose was selected to better represent the therapeutic exposures in patients at steady state who are taking multiple doses of ibrutinib under typical dosing conditions (i.e., non-fasted and after steady-state dosing) [11]. Based on the current labeling, the two-fold higher dose of 1680 mg was selected to reflect the potential supratherapeutic exposure scenarios in patients at steady state. A previous study demonstrated that ibrutinib exposure is reduced to approximately 60% when administered under fasted conditions [11]. Ibrutinib is approved for administration regardless of food intake [3, 11]. It should be noted that the ibrutinib mean C max achieved at the 840 and 1680 mg doses exceeded the documented mean C max at the 560 mg dose, i.e., 164 ng/mL, by a factor of 1.9 and 4.4, respectively, thus amply covering the target range of exposures including those that could occur when ibrutinib is taken at the reduced dose of 140 mg, either in combination with moderate or strong CYP3A inhibitors, or when taken by patients with mild or moderate liver impairment. The results of this study indicate that ibrutinib had no clinically significant effects on the QTc interval at both 840- and 1680-mg dose levels. The upper bounds of the 90% CIs for the placebo-corrected ∆∆QTc at all timepoints for subjects receiving ibrutinib were below 10 ms for all three QT correction methods (QTcP, QTcF, and QTcB) and below the threshold of regulatory concern [9].
In the current study, ibrutinib and placebo were associated with mean decreases in QTcP from baseline at most timepoints observed, whereas the positive control moxifloxacin was associated with a mean increase in QTc from baseline at most timepoints, in line with expectations.
Results from the non-linear mixed effects PK/PD model suggest a negative relationship between the plasma concentrations of ibrutinib and change in QTc, and a positive relationship between plasma concentrations of ibrutinib and change in PR interval. Similar relationships were noted with PCI-45227, ibrutinib metabolite, as parent and metabolite concentrations are highly correlated. However, the magnitude of the shortening of QTc interval and prolongation of PR interval were not considered clinically significant [19,20,21].
The results of this study are consistent to those from the Phase 1b/2 Study 1102 [22] which did not report prolongation of QTc interval as a concern. Designed to determine the safety, preliminary efficacy, PK and PD of a fixed-dose daily regimen of ibrutinib 420 mg and ibrutinib 840 mg in patients with CLL/SLL, QTcF intervals were not prolonged by ibrutinib at either dose in Study 1102. In the current study, consistent with the previous results, ibrutinib was also associated with subclinical reductions in mean heart rate, but without bradycardia (HR < 60 bpm). In addition, mild increases in the PR interval were noted, but none above 200 ms. Ibrutinib at both dose levels did not affect QRS duration.
The PK profile of ibrutinib exhibited a dose-dependent exposure (AUC) and C max. The oral volume distribution and half-lives were comparable between the two doses, the oral clearance and the metabolite-to-parent ratios were approximately 25–35% lower after ibrutinib 1680 mg than ibrutinib 840 mg.
Overall, ibrutinib 840 mg had an acceptable safety profile, similar to earlier studies with lower doses in healthy subjects and larger trial populations [5, 23, 24]. No clinically important treatment-emergent adverse events or changes in clinical chemistry were observed. An event of reversible Grade 4 hepatic enzymes increase (ALT and AST) was observed following single dose administration of ibrutinib 1680 mg. These elevations normalized over the course of 1 month.
Although the study included a smaller-than-intended sample size as based on statistical assumptions, the positive control moxifloxacin behaved as expected on the ECG parameters. The maximum mean and upper bound of the 90% CIs for moxifloxacin were 8.6 and 12.1 ms at 3-h post-dose confirming the sensitivity and validity of the test. In addition, the QTcF evaluation parameters were met and this further supports the acceptability of the assay sensitivity [25]. Mining of QTc data obtained in first-in-human studies provided further evidence that exposure–response relationships can provide a reliable prediction of a QT liability despite small sample sizes [26, 27].
Despite the smaller-than-intended sample size due to the early termination of the study, the data support the conclusion that single therapeutic and supratherapeutic doses of ibrutinib are not associated with QTc interval prolongation in healthy subjects. Ibrutinib at the approved maximum therapeutic dose of 560 mg per day is unlikely to have a clinically relevant effect on cardiac repolarization in patients.
Change history
06 December 2017
The author would like to correct the affiliations and conflict of interest in the publication of the original article. The corrected details are given below for your reading.
References
Honigberg LA, Smith AM, Sirisawad M, Verner E, Loury D, Chang B, Li S, Pan Z, Thamm DH, Miller RA, Buggy JJ (2010) The Bruton tyrosine kinase inhibitor PCI-32765 blocks B-cell activation and is efficacious in models of autoimmune disease and B-cell malignancy. Proc Natl Acad Sci USA 107(29):13075–13080. doi:10.1073/pnas.1004594107
Davids MS, Brown JR (2014) Ibrutinib: a first in class covalent inhibitor of Bruton’s tyrosine kinase. Future Oncol 10(6):957–967. doi:10.2217/fon.14.51
Janssen Biotech IH (2017) Ibrutinib Prescribing Information
CHMP (2014) CHMP assessment report. European Medicines Agency
Dreyling M, Jurczak W, Jerkeman M, Silva RS, Rusconi C, Trneny M, Offner F, Caballero D, Joao C, Witzens-Harig M, Hess G, Bence-Bruckler I, Cho SG, Bothos J, Goldberg JD, Enny C, Traina S, Balasubramanian S, Bandyopadhyay N, Sun S, Vermeulen J, Rizo A, Rule S (2016) Ibrutinib versus temsirolimus in patients with relapsed or refractory mantle-cell lymphoma: an international, randomised, open-label, phase 3 study. Lancet 387(10020):770–778. doi:10.1016/S0140-6736(15)00667-4
Chanan-Khan A, Cramer P, Demirkan F, Fraser G, Silva RS, Grosicki S, Pristupa A, Janssens A, Mayer J, Bartlett NL, Dilhuydy MS, Pylypenko H, Loscertales J, Avigdor A, Rule S, Villa D, Samoilova O, Panagiotidis P, Goy A, Mato A, Pavlovsky MA, Karlsson C, Mahler M, Salman M, Sun S, Phelps C, Balasubramanian S, Howes A, Hallek M, investigators H (2016) Ibrutinib combined with bendamustine and rituximab compared with placebo, bendamustine, and rituximab for previously treated chronic lymphocytic leukaemia or small lymphocytic lymphoma (HELIOS): a randomised, double-blind, phase 3 study. Lancet Oncol 17(2):200–211. doi:10.1016/S1470-2045(15)00465-9
Burger JA, Tedeschi A, Barr PM, Robak T, Owen C, Ghia P, Bairey O, Hillmen P, Bartlett NL, Li J, Simpson D, Grosicki S, Devereux S, McCarthy H, Coutre S, Quach H, Gaidano G, Maslyak Z, Stevens DA, Janssens A, Offner F, Mayer J, O’Dwyer M, Hellmann A, Schuh A, Siddiqi T, Polliack A, Tam CS, Suri D, Cheng M, Clow F, Styles L, James DF, Kipps TJ, Investigators R (2015) Ibrutinib as Initial Therapy for Patients with Chronic Lymphocytic Leukemia. N Engl J Med 373 (25):2425–2437. doi:10.1056/NEJMoa1509388
Darpo B (2010) The thorough QT/QTc study 4 years after the implementation of the ICH E14 guidance. Br J Pharmacol 159(1):49–57. doi:10.1111/j.1476-5381.2009.00487.x
ICH (2005) ICH E14 guidance: the clinical evaluation of QT/QTc interval prolongation and proarrhythmic potential for non-arrhythmic drugs
Curigliano G, Spitaleri G, de Braud F, Cardinale D, Cipolla C, Civelli M, Colombo N, Colombo A, Locatelli M, Goldhirsch A (2009) QTc prolongation assessment in anticancer drug development: clinical and methodological issues. Ecancermedicalscience 3:130. doi:10.3332/ecancer.2009.130
de Jong J, Sukbuntherng J, Skee D, Murphy J, O’Brien S, Byrd JC, James D, Hellemans P, Loury DJ, Jiao J, Chauhan V, Mannaert E (2015) The effect of food on the pharmacokinetics of oral ibrutinib in healthy participants and patients with chronic lymphocytic leukemia. Cancer Chemother Pharmacol 75(5):907–916. doi:10.1007/s00280-015-2708-9
de Vries R, Huang M, Bode N, Jejurkar P, Jong J, Sukbuntherng J, Sips L, Weng N, Timmerman P, Verhaeghe T (2015) Bioanalysis of ibrutinib and its active metabolite in human plasma: selectivity issue, impact assessment and resolution. Bioanalysis 7(20):2713–2724. doi:10.4155/bio.15.159
Tabo M, Nakamura M, Kimura K, Ito S (2006) QT-RR relationships and suitable QT correction formulas for halothane-anesthetized dogs. J Toxicol Sci 31(4):381–390
Culley CM, Lacy MK, Klutman N, Edwards B (2001) Moxifloxacin: clinical efficacy and safety. Am J Health Syst Pharm 58(5):379–388
Hug B, Abbas R, Leister C, Burns J, Sonnichsen D (2010) A single-dose, crossover, placebo- and moxifloxacin-controlled study to assess the effects of neratinib (HKI-272) on cardiac repolarization in healthy adult subjects. Clin Cancer Res 16(15):4016–4023. doi:10.1158/1078-0432.CCR-10-0280
Demolis JL, Kubitza D, Tenneze L, Funck-Brentano C (2000) Effect of a single oral dose of moxifloxacin (400 mg and 800 mg) on ventricular repolarization in healthy subjects. Clin Pharmacol Ther 68(6):658–666. doi:10.1067/mcp.2000.111482
Scheers E, Leclercq L, de Jong J, Bode N, Bockx M, Laenen A, Cuyckens F, Skee D, Murphy J, Sukbuntherng J, Mannens G (2015) Absorption, metabolism, and excretion of oral (1)(4)C radiolabeled ibrutinib: an open-label, phase I, single-dose study in healthy men. Drug Metab Dispos 43(2):289–297. doi:10.1124/dmd.114.060061
de Jong J, Skee D, Murphy J, Sukbuntherng J, Hellemans P, Smit J, de Vries R, Jiao JJ, Snoeys J, Mannaert E (2015) Effect of CYP3A perpetrators on ibrutinib exposure in healthy participants. Pharmacol Res Perspect 3(4):e00156. doi:10.1002/prp2.156
Gallagher MM, Magliano G, Yap YG, Padula M, Morgia V, Postorino C, Di Liberato F, Leo R, Borzi M, Romeo F (2006) Distribution and prognostic significance of QT intervals in the lowest half centile in 12,012 apparently healthy persons. Am J Cardiol 98(7):933–935. doi:10.1016/j.amjcard.2006.04.035
Anttonen O, Junttila MJ, Rissanen H, Reunanen A, Viitasalo M, Huikuri HV (2007) Prevalence and prognostic significance of short QT interval in a middle-aged Finnish population. Circulation 116(7):714–720. doi:10.1161/CIRCULATIONAHA.106.676551
Aro AL, Anttonen O, Kerola T, Junttila MJ, Tikkanen JT, Rissanen HA, Reunanen A, Huikuri HV (2014) Prognostic significance of prolonged PR interval in the general population. Eur Heart J 35(2):123–129. doi:10.1093/eurheartj/eht176
Loury DJ, Clow JS, F., James D, Kunkel L (2013) Open-label evaluation of ECG in patients with chronic lymphocytic leukemia (CLL) receiving ibrutinib monotherapy. Paper presented at the American Society of Clinical Oncology Annual Meeting
Byrd JC, O’Brien S, James DF (2013) Ibrutinib in relapsed chronic lymphocytic leukemia. N Engl J Med 369(13):1278–1279. doi:10.1056/NEJMc1309710
Advani RH, Buggy JJ, Sharman JP, Smith SM, Boyd TE, Grant B, Kolibaba KS, Furman RR, Rodriguez S, Chang BY, Sukbuntherng J, Izumi R, Hamdy A, Hedrick E, Fowler NH (2013) Bruton tyrosine kinase inhibitor ibrutinib (PCI-32765) has significant activity in patients with relapsed/refractory B-cell malignancies. J Clin Oncol 31(1):88–94. doi:10.1200/JCO.2012.42.7906
Bloomfield DM, Kost JT, Ghosh K, Hreniuk D, Hickey LA, Guitierrez MJ, Gottesdiener K, Wagner JA (2008) The effect of moxifloxacin on QTc and implications for the design of thorough QT studies. Clin Pharmacol Ther 84(4):475–480
Darpo B, Benson C, Dota C, Ferber G, Garnett C, Green CL, Jarugula V, Johannesen L, Keirns J, Krudys K, Liu J, Ortemann-Renon C, Riley S, Sarapa N, Smith B, Stoltz RR, Zhou M, Stockbridge N (2015) Results from the IQ-CSRC prospective study support replacement of the thorough QT study by QT assessment in the early clinical phase. Clin Pharmacol Ther 97(4):326–335. doi:10.1002/cpt.60
Darpo B, Garnett C, Keirns J, Stockbridge N (2015) Implications of the IQ-CSRC Prospective Study: Time to Revise ICH E14. Drug Saf 38(9):773–780. doi:10.1007/s40264-015-0325-5
Acknowledgements
The authors thank the study subjects who volunteered to participate in this study; the sponsor staff involved in data collection and analyses; Donna Skee and Dr Qingtao Huang (formerly from Janssen Research & Development, LLC) for data analysis and bioanalysis, respectively; Dr. Shivangi Gupta and Dr. Rishabh Pandey (SIRO Clinpharm Pvt. Ltd.) for providing writing assistance and Dr. Namit Ghildyal (Janssen Research & Development, LLC) for additional editorial support for the development of this manuscript. The writing assistance was funded by Janssen Research & Development, LLC.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The study was sponsored by Janssen Research & Development LLC and Pharmacyclics LLC, an AbbVie company.
Conflict of interest
J Jong, P Hellemans, JJ Jiao, Y Hunag, S Mesens, and D Ouellet are employees of Janssen Research & Development, LLC. J Sukbuntherng is an employee of Pharmacyclics LLC, an AbbVie company.
Ethical approval
All procedures performed were in accordance with the ethical standards of the institutional research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Informed consent
Written informed consent was obtained from all study participants.
Additional information
A correction to this article is available online at https://doi.org/10.1007/s00280-017-3490-7.
Rights and permissions
About this article
Cite this article
de Jong, J., Hellemans, P., Jiao, J.J. et al. Ibrutinib does not prolong the corrected QT interval in healthy subjects: results from a thorough QT study. Cancer Chemother Pharmacol 80, 1227–1237 (2017). https://doi.org/10.1007/s00280-017-3471-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00280-017-3471-x