Abstract
Purpose
Sorafenib and S-1 (one mixed formulation containing 5-FU prodrug and dihydropyrimidine dehydrogenase inhibitor) were two effective agents against hepatocellular carcinoma (HCC), but whether they had synergistic effects remained unclear. The present study aimed at evaluating their synergistic effects against HCC and its mechanisms.
Methods
Inhibitory effects of sorafenib, 5-FU and their combination on HCC cells PLC/PRF/5 and SK-HEP-1 were evaluated. Expressions of transcription factor E2F-1 and its downstream thymidylate synthetase (TS) in the treated cells were determined using real-time PCR and Western blot. In vivo anti-tumoral efficacy of S-1 plus sorafenib on HCC was evaluated in NOD/SCID mice. E2F-1 and TS expressions in tumors were determined by immunohistochemical staining.
Results
Sorafenib inhibited growth of HCC cells in dose-dependent manner, with IC50 of 5.4 ± 0.3 μmol/L for PLC/PRF/5 and 5.3 ± 0.5 μmol/L for SK-HEP-1. Sorafenib (1 μmol/L) enhanced inhibitory efficacy of 5-FU on HCC cells in vitro, dropping IC50 of 5-FU from 167.7 ± 12.1 to 105.4 ± 8.4 μmol/L for PLC/PRF/5 and 115 ± 10.2 to 82 ± 7.4 μmol/L for SK-HEP-1 (both p < 0.01). Sorafenib downregulated E2F-1 and TS expressions on HCC cells, and its combination with 5-FU yielded a synergistic downregulation of TS expression on HCC cells. In NOD/SCID mice with subcutaneously inoculated HCC, sorafenib combined with S-1 yielded greater inhibition on tumor growth and remarkable TS suppression when compared with sorafenib or S-1 alone (all p < 0.05).
Conclusions
Sorafenib enhanced therapeutic efficacy of 5-FU/S-1 against HCC through downregulation of E2F-1 and TS expressions. Sorafenib combined with S-1 might represent as valuable therapeutic regimen against HCC.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Sorafenib, a recently developed multi-kinases inhibitor (i.e., molecular-target drug), could suppress tumor angiogenesis via blockage of vascular endothelial growth factor receptor (VEGFR) and platelet-derived growth factor receptor (PDGFR) [1]. Moreover, it had anti-proliferative effect on hepatocellular carcinoma (HCC) cells by inhibiting the receptor tyrosine kinases KIT and FLT-3 and the serine/threonine kinases in Raf/MEK/ERK pathway [1]. Its efficacy in treating advanced HCC has been proven in two large-scale randomized control trials, with a prolongation of median survival time of around 3 months compared with placebo [2, 3]. Provided sorafenib has been used as a standard medical therapy for advanced HCC, its efficacy alone is still far from satisfaction. Identification of its synergistic drugs may help to improve its efficacy.
5-FU, an anti-metabolic chemotherapeutic agent, has been widely used for various malignancies for decades. However, it had little efficacy in treating HCC mainly due to high level of dihydropyrimidine dehydrogenase (DPD) in tumor cells [4, 5], which rapidly degraded 5-FU and weakened its anti-tumoral efficacy. S-1 was one mixed formulation composed of tegafur (FT, one 5-FU prodrug), 5-chloro-2,4-dihydroxypyridine (CDHP, one DPD inhibitor) and potassium oxonate (Oxo). FT was transformed into 5-FU in the liver, CDHP competitively inhibited DPD and helped to maintain an effective concentration of 5-FU in tumor cells for an extended time [6]. Oxo helped to alleviate the gastrointestinal adverse effects through the reduction in 5-FU phosphorylation in gastrointestinal tract [7]. Its anti-tumoral efficacy has been validated in gastric cancer [8], colorectal carcinoma [9], non-small lung cancer [10], head and neck cancer [11], pancreatic cancer [12], cholangiocarcinoma [13] and renal cancer [14, 15]. Some pilot studies indicated that S-1 was effective in treating HCC [16].
Combination of molecular-targeted drugs and chemotherapeutic agents in treating malignancies has some advantages. With different anti-tumoral mechanisms, molecular-targeted drugs and chemotherapeutic agents may have additive and even synergistic efficacy. On the other hand, they have different spectrum of adverse effects, the combination will not compromise the patients’ tolerance. Whether sorafenib and S-1 have synergistic effects against HCC still remains unclear. The present study aimed at investigating the synergistic effect and mechanisms of 5-FU/S-1 and sorafenib against HCC in vitro and in vivo.
Materials and methods
Cell culture, reagents and antibodies
Human HCC cell lines PLC/PRF/5 and SK-HEP-1 were purchased from the Cell Resources Bank of Laboratory Animal Center, Sun Yat-sen University (Guangzhou, China) and cultured in RPMI-1640 medium (Gibco BRL, USA) supplemented with 10 % fetal bovine serum (Gibco BRL, USA). Sorafenib and S-1 were kindly provided by Bayer Pharmaceutical (Germany) and Taiho Pharmaceutical (Tokyo, Japan), respectively. Sorafenib was dissolved in DMSO in a concentration of 10 mM. 5-FU was purchased from Sigma (USA). Mouse anti-human monoclonal TS antibody and mouse anti-human monoclonal E2F-1 antibody were obtained from Millipore (MA, USA). Mouse anti-human monoclonal β-actin antibody was from Boaosen (Beijing, China).
Cytotoxicity of sorafenib and 5-FU on HCC cells
S-1 is the prodrug of 5-FU, and it needs to be metabolized into 5-FU in the liver to play tumoricidal roles. Hence, in vitro cytotoxicity study 5-FU is directly adopted for replacement of S-1.
PLC/PRF/5 or SK-HEP-1 cells were seeded into 96-well plate (2 × 103/well), respectively. Twenty-four hours after seeding, cells were incubated with various concentrations of sorafenib alone, 5-FU alone or 5-FU combined with 1 μmol/L sorafenib for 72 h. Cells cultured in medium with DMSO (a concentration of 0.01 %) were used as negative control and wells containing only medium served as blank control. At the end of incubation, 10ul of CCK-8 solution (Donjido, Japan) was added into each well. Absorbance at 450 nm (A450) was measured in a microplate reader (Thermo Scientific, USA). Growth inhibition rate (%) = 1 − [(A450 of treated group-A450 of blank control group)/(A450 of negative control group-A450 of blank control group)] × 100 %. Wells were sextuplicated and assay was repeated for 3 times. IC50 (half-maximal inhibitory concentration) was then calculated from growth inhibition rates. The Chou and Talalay’s combination index (CI) was calculated to assess the interaction of sorafenib and 5-FU. CI values of <1, 1 and >1 indicated synergistic, additive and antagonistic effects, respectively [17].
Quantitative real-time PCR
Total RNA was extracted by using RNAiso Plus (TaKaRa, Japan). cDNA was reverse synthesized by using PrimeScript® RT reagent (Perfect Real Time) Kit (TaKaRa, Japan). The subsequent real-time PCRs of TS and E2F-1 were performed using TaKaRa SYBR® Premix Ex TaqTM (Perfect Real Time) Kit (TaKaRa, Japan). GAPDH expression was used as the internal control. Primers were synthesized by TaKaRa (China), and their sequences were listed as follows: forward primer of TS: 5′-TACCTGAATCACATCGAGCCACT-3′; reverse primer of TS: 5′-GAAGAATCCTGAGCTTTGGGAAA-3′; forward primer of E2F-1: 5′-GAAGCTTCTAGCTGGGGTCTG-3′; reverse primer of E2F-1: 5′-CACACACACATGCTCACACACAT-3′; forward primer of GAPDH: 5′-ACACCCACTCCTCCACCTTT-3′; reverse primer of GAPDH: 5′-TTACTCCTTGGAGGCCATGT-3′.
Western blot
Total protein was extracted from treated PLC/PRF/5 and SK-HEP-1 cells with KeyGEN Total Protein Extraction Kit (KeyGEN Biotech, Nanjing, China) following the manufacturer’s instructions. Protein was then separated by polyacrylamide gel electrophoresis and then transferred to polyvinylidene difluoride (PVDF) membranes (Millipore, MA, USA), which were subsequently blocked in 5 % skim milk for 1 h and then incubated with primary antibodies (anti-TS and anti-E2F-1 antibodies) at 1:500 dilution at 4 °C overnight. The membranes were re-warmed at room temperature, and washed with phosphate buffered saline Tween-20 (PBST) for three times and then incubated with secondary goat anti-mouse antibody at 1:2,500 dilution for 1 h at room temperature. Following application of ECL Western blotting kit (KeyGEN, Nanjing, China) on the membrane, the signals were detected by Kodak X-OMAT film. The membranes were then subjected to a 15 min stripping with Western blot stripping buffer (KeyGEN, Nanjing, China), three times of 10 min wash with PBST, and then detected for β-actin expression.
Immunohistochemical staining
Tissues were fixed in 4 % paraformaldehyde, embedded in paraffin and cut into 4-μm sections. Sections were deparaffinized in xylene, rehydrated in ethanol and then incubated in 3 % H2O2 to block endogenous peroxidase activity. Antigen retrieval was achieved by treating the tissues with citrate buffer in a pressure cooker. The sections were subsequently incubated with mouse anti-human E2F-1 antibody (dilution 1:100, Millipore) or TS antibody (dilution 1:100, Millipore) at 4 °C overnight. A mouse IgG (Biosynthesis, China) was utilized as a negative control. Staining was detected by adding biotinylated secondary antibodies (Maxin-Bio, Fuzhou, China), avidin–biotin complex (Maxin-Bio), and diaminobenzidine (Maxin-Bio). Sections were then counterstained with hematoxylin.
The intensity and distribution of E2F-1 and TS staining were evaluated under microscopy, respectively. The intensity of staining (score A) was estimated as follows: colorless (0); buff (1); brownly yellow (2) and darkly brown (3). The distribution of staining (score B) was marked as follows: no positive cells (0); <10 % positive cells (1); 10–50 % positive cells (2); 50–75 % positive cells (3) and >75 % positive cells (4). Multiplication of score A and score B was defined as immunohistochemical staining level. For each sample, 10 visual fields (×400) were evaluated.
Tumoricidal efficacy of sorafenib and S-1 against HCC in animal model
Male NOD/SCID mice (5–6 weeks old) were purchased from Experimental Animal Center of Sun Yat-sen University (Guangzhou, China) and kept in a SPF environment. The mice were exposed to a 12:12-h light–dark cycle and fed with food and water ad libitum in a barrier facility.
NOD/SCID mice were inoculated subcutaneously at right flank with PLC/PRF/5 or SK-HEP-1 cells (1 × 107 cells/mouse). Mice were randomized into four groups (6 mice per group) when tumors reached up to a volume of 120–150 mm3. Treatment for 4 groups was as follows: daily oral gavage of 10 mg/kg of S-1 alone (S-1 group); 10 mg/kg of sorafenib alone (sorafenib group); combination of S-1 and sorafenib (both 10 mg/kg) (combined group); 0.2 ml normal saline (control group). Tumor length (L) and width (W) were measured with a caliper twice per week, and tumor volume was calculated according to the formula 0.52 × L × W 2. Body weight of mice was measured simultaneously.
Statistic analysis
Data are presented as mean ± standard deviation. Statistical analysis was performed on personal computer using SPSS software package version 13.0. Student’s t test was used to compare inter-group differences in continuous variables, and Mann–Whitney test was adopted to compare the inter-group differences in the immunohistochemical staining of E2F-1 and TS. The differences in cell viability and tumor volume between groups were analyzed with repeated measures analysis of variance. A two-tailed p value less than 0.05 was considered as statistical significance.
Results
Sorafenib enhances the cytotoxicity of 5-FU on PLC/PRF/5 and SK-HEP-1 cells
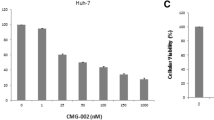
Sorafenib inhibited the growth of both PLC/PRF/5 and SK-HEP-1 cells in a dose-dependent manner (Fig. 1a, b). IC50 of sorafenib was 5.4 ± 0.3 μmol/L for PLC/PRF/5 and 5.3 ± 0.5 μmol/L for SK-HEP-1. 5-FU also suppressed the growth of both cell lines in a dose-dependent manner (Fig. 1c, d). IC50 of 5-FU was 167.7 ± 12.1 μmol/L for PLC/PRF/5 and 115 ± 10.2 μmol/L for SK-HEP-1.
Synergistic cytotoxicity of sorafenib and 5-FU on HCC cells in vitro. PLC/PRF/5 and SK-HEP-1 cells were incubated with various agents for 72 h in 96-well plates, and cell growth inhibition rates were evaluated. a, b showed that sorafenib inhibited the growth of both PLC/PRF/5 and SK-HEP-1 cells in dose-dependent manner, respectively. c, d illustrated that 5-FU had cytotoxicity on both PLC/PRF/5 and SK-HEP-1 cells in dose-dependent manner, and its cytotoxicity on both cell lines was markedly augmented in the presence of 1 μM sorafenib. All values were representative of three independent experiments
Interestingly, various concentrations of 5-FU combined with 1 μmol/L sorafenib resulted in greater growth inhibition on both PLC/PRF/5 and SK-HEP-1 cells in comparison with 5-FU alone. In the presence of 1 μmol/L of sorafenib, IC50 of 5-FU markedly dropped to 105.4 ± 8.4 μmol/L for PLC/PRF/5 cells and 82 ± 7.4 μmol/L for SK-HEP-1 cells (both p < 0.01, Fig. 1c, d). At 50 % growth inhibition for PLC/PRF/5 and SK-HEP-1 cells, CI of sorafenib and 5-FU was 0.91 and 0.96, respectively. The results demonstrated that sorafenib and 5-FU had a synergistic cytotoxic effect on both cell lines.
Sorafenib downregulated the expressions of E2F-1 and TS gene in vitro
To investigate the mechanisms of synergistic effects of sorafenib and 5-FU on HCC cells, the expressions of TS and its upstream transcription factor E2F-1 genes were evaluated in PLC/PRF/5 and SK-HEP-1 cells at 24, 48, 72 h after sorafenib treatment. Quantitative real-time PCR showed that sorafenib downregulated mRNA expressions of E2F-1 and TS genes in both PLC/PRF/5 and SK-HEP-1 cells in a time-dependent manner (Fig. 2a, b). Consistently, Western blot illustrated that sorafenib inhibited protein expressions of E2F-1 and TS in both cell lines in time-dependent manner (Fig. 2c, d).
Effects of sorafenib on the expressions of E2F-1 and TS in HCC cells. In HCC cells treated with 1 μM sorafenib for 24, 48 and 72 h, mRNA levels of E2F-1 and TS were downregulated in both PLC/PRF/5 and SK-HEP-1 cell lines in time-dependent manner (a, b). Consistently, protein expressions of E2F-1 and TS were downregulated in both cell lines treated with l μM sorafenib in time-dependent manner (c, d). In PLC/PRF/5 and SK-HEP-1 cells treated with various concentrations of 5-FU alone or combined with 1 μM sorafenib for 72 h, mRNA expression of TS was suppressed by 5-FU in both PLC/PRF/5 and SK-HEP-1 cell lines in dose-dependent manner (e, f), and 1 μM sorafenib markedly augmented TS suppression induced by 5-FU in both HCC cell lines (e, f). Western blot confirmed that sorafenib markedly enhanced TS suppression induced by 5-FU in both HCC cell lines at protein level (g, h)
In the parallel experiments of 5-FU treatment alone or in combination with 1 μmol/L sorafenib on PLC/PRF/5 and SK-HEP-1 cells for 72 h, 25 μmol/L 5-FU alone had no inhibitory effect on mRNA expression (Fig. 2e, f) and protein expression (Fig. 2g, h) of TS on both cell lines, and 100 and 200 μmol/L 5-FU alone significantly downregulated mRNA expression (Fig. 2e, f) and protein expression (Fig. 2g, h) of TS on both cell lines. In presence of 1 μmol/L sorafenib, TS expression in all three concentrations of 5-FU was more prominently downregulated on both cell lines (all p < 0.05, Fig. 2e–h). It suggested that sorafenib augmented the cytotoxicity of 5-FU on HCC cells via downregulating E2F-1 gene expression and its downstream TS gene expression.
Synergistic anti-tumoral effects of sorafenib and S-1 in vivo
Treatment of subcutaneous PLC/PRF/5 and SK-HEP-1 tumors on NOD/SCID mice demonstrated that sorafenib combined with S-1 had a greater inhibitory efficacy on tumor growth compared with sorafenib alone, S-1 alone and control groups (all p < 0.01, Fig. 3).
Synergistic anti-tumoral efficacy of sorafenib and S-1 in vivo. PLC/PRF/5 or SK-HEP-1 cells were implanted subcutaneously at the right flank of male NOD/SCID mice. Tumor-bearing mice were randomized and treated by oral gavage of various agents for 28 consecutive days. Tumor volume of sorafenib group and S-1 group in both cell lines was significantly smaller than that of control group (both p < 0.05, a, b). Tumor volume of sorafenib + S-1 group was significantly smaller than that of sorafenib alone, S-1 alone and control groups (all p < 0.05, a, b)
Immunohistochemical staining illustrated that E2F-1 expression in HCC tissues was not influenced by S-1 treatment (Fig. 4a, b, f, g, k), but its expression was markedly downregulated by sorafenib alone or combined with S-1 treatment (all p < 0.05, Fig. 4c, d, h, i, k). On the other hand, both S-1 and sorafenib treatments could suppress TS expression in HCC tissues (Fig. 5a–c, f–h, k), and combined treatment of sorafenib and S-1 could more profoundly downregulate TS expression in HCC tissues when compared with either sorafenib or S-1 alone treatment (Fig. 5a–k). These in vivo findings were consistent with the in vitro results of cytotoxicity of sorafenib and 5-FU on HCC cells. It implied that sorafenib exerted synergistic effects with S-1 on HCC via suppressing E2F-1 gene expression and its downstream TS expression.
Immunohistochemical staining of E2F-1 in HCC tissues. Compared with control group, S-1 treatment had no impact on E2F-1 expression in both PLC/PRF/5 and SK-HEP-1 tumors (a, b, f, g, k). Sorafenib or sorafenib + S-1 treatment markedly downregulated E2F-1 expression in both PLC/PRF/5 and SK-HEP-1 tumors (c, d, h, i, k)
Immunohistochemical staining of TS in HCC tissues. Compared with control group, S-1 or sorafenib alone treatment suppressed TS expression in both PLC/PRF/5 and SK-HEP-1 tumors (a–c, f–h, k). Combination of sorafenib and S-1 treatment more profoundly inhibited TS expression in both PLC/PRF/5 and SK-HEP-1 tumors (d, i, k)
Safety of combined sorafenib and S-1 in treating tumor-bearing mice
The body weight of tumor-bearing mice was monitored during the treatment for evaluating the therapy safety. S-1 treatment alone was well tolerated with no significant differences in body weight when compared with control group (Fig. 6, p = 0.161 for PLC/PRF/5; p = 0.282 for SK-HEP-1). Sorafenib treatment alone resulted in a moderate weight loss in mice when compared with control group and S-1 (Fig. 6, p = 0.032, 0.046, respectively, for PLC/PRF/5; p = 0.037, 0.052, respectively, for SK-HEP-1). Combined sorafenib and S-1 did not aggravate weight loss of mice when compared with sorafenib (Fig. 6, p = 0.341 for PLC/PRF/5; p = 0.482 for SK-HEP-1). It suggested that a combination of sorafenib and S-1 was a safe and tolerable therapeutic regimen.
Body weight changes in tumor-bearing mice. Compared with control group, S-1 treatment had no influences on the body weight of mice bearing either PLC/PRF/5 or SK-HEP-1 tumors. Sorafenib treatment inhibited body weight of mice bearing either PLC/PRF/5 or SK-HEP-1 tumors when compared with control group, but there was no significant difference in body weight of mice between sorafenib group and sorafenib + S-1 group
Discussion
Though curative resection was the treatment of choice for HCC, it was only feasible in less than one-third of patients. Non-surgical therapies, including medical treatment, played important roles in management of HCC [1, 16].
Sorafenib is one molecule-targeted agent which has been proven to be effective against HCC and prolong patients’ survival in advanced HCC [2, 3]. However, there is still room for improving its efficacy [9–15]. One potential approach is its combination with chemotherapeutic agents. Since they have different tumoricidal mechanisms and different spectrum of adverse effects, their combinations may produce a synergistic anti-tumoral efficacy and not compromise patients’ tolerance. The key is to identify an effective and synergistic chemotherapeutic agent against HCC.
S-1 is a novel oral prodrug of 5-FU containing DPD inhibitor and gastrointestinal toxicity protector. Its efficacy and tolerability has been proven in many solid malignancies. Some pilot studies showed that S-1 was effective in treating HCC. Whether sorafenib and S-1 exist a synergistic efficacy against HCC still remains unknown.
In the present study, in vitro cytotoxicity assay revealed that 1 μmol/L sorafenib markedly enhanced the cytotoxicity of 5-FU on HCC cells, with an IC50 of 5-FU dropping down from 167.7 ± 12.1 to 105.4 ± 8.4 μmol/L for PLC/PRF/5 cells and from 115 ± 10.2 to 82 ± 7.4 μmol/L for SK-HEP-1 cells. Furthermore, in the murine subcutaneous HCC model, a combination of S-1 and sorafenib resulted in a greater inhibition on tumor growth when compared with sorafenib alone, S-1 alone and control group. These results demonstrated that sorafenib and S-1 had a synergistic efficacy against HCC.
For investigating the mechanisms of synergistic efficacy of sorafenib and S-1 against HCC, TS in HCC cells was evaluated in vitro and in vivo after treatment. TS is the key enzyme for the synthesis of deoxythymidine monophosphate (dTMP), a requisite precursor for the synthesis of DNA [18]. 5-FU and its prodrugs, including S-1, inhibit cell proliferation and tumor growth through TS inhibition and subsequent DNA synthesis. TS expression in tumor tissue is a determinant to the anti-tumor effect of 5-FU. A high level of TS expression in tumors has been considered as one of the reasons for fluorouracil resistance [19–23]. On the contrary, downregulation of TS expression in tumors enhances the anti-tumoral efficacy of 5-FU [24], and sustaining inhibition of TS promotes apoptosis of tumor cells via destroying DNA synthesis and repair [25, 26]. In the present study, 100 and 200 μmol/L of 5-FU treatment alone achieved significant TS suppression in HCC cells, and a further decrease in TS expression was observed in the presence of 1 μmol/L sorafenib. Even in low concentration of 5-FU (25 μmol/L), which had no inhibition on TS expression, 1 μmol/L sorafenib demonstrated an inhibitory effect on TS expression. These results suggested that sorafenib enhanced the cytotoxicity of 5-FU by downregulation of TS expression.
With respect to the influence of 5-FU on TS expression, our results were inconsistent with some previous studies, in which 5-FU treatment in multi-drug resistant breast and colon cancer cells was shown to up-regulate TS expression [27]. The reasons for the inconsistency were probably related to the different biological behaviors in different cancer cells. The mechanisms for TS downregulation by high-dose 5-FU (100 and 200 μmol/L) in HCC cells still remained unclear, since the expression of E2F-1, the regulating factor of TS [28], was not influenced by 5-FU [29–31]. Possibly, it was related to RNA misincorporation of 5-FU, which eventually led to disruption of RNA synthesis and processing [23].
For further investigating the mechanism for inhibitory effect of sorafenib on TS expression, E2F-1 expression in HCC cells was evaluated. Some molecular-targeted drugs have been shown to suppress the expression of E2F-1 and subsequent expression of TS. Tanizaki and Komoto reported a synergistic anti-tumoral efficacy of lapatinib and 5-FU against gastric and pancreatic carcinoma, and showed that the inhibition of E2F-1 and TS expression by lapatinib led to the augmentation of 5-FU cytotoxicity [32, 33]. Studies in non-small cell lung cancer revealed the suppression of E2F-1 and TS expression by gefitinib was a potential mechanism for the synergistic anti-tumoral efficacy of gefitinib and 5-FU [34, 35]. Recently, Takeuchi et al. [36] showed a synergistic anti-tumoral efficacy of sorafenib and S-1 against renal cell carcinoma via downregulating E2F-1 and TS expression. Lee and his associates treated 20 patients with advanced HCC using sorafenib and S-1 and achieved a median progression-free survival of 3.9 months and median overall survival of 10.4 months [37]. Our study showed that sorafenib could inhibit E2F-1 expression and consequently downregulate TS expression in a time-dependent manner in HCC in vitro and in vivo, which might be the mechanism for synergistic efficacy of sorafenib and 5-FU against HCC. The combination of sorafenib and S-1 might represent as a reasonable and applicable therapeutic regimen for HCC.
References
Liu L, Cao Y, Chen C, Zhang X, McNabola A, Wilkie D, Wilhelm S, Lynch M, Carter C (2006) Sorafenib blocks the RAF/MEK/ERK pathway, inhibits tumor angiogenesis, and induces tumor cell apoptosis in hepatocellular carcinoma model PLC/PRF/5. Cancer Res 66:11851–11858
Llovet JM, Ricci S, Mazzaferro V, Hilgard P, Gane E, Blanc JF, de Oliveira AC, Santoro A, Raoul JL, Forner A, Schwartz M, Porta C, Zeuzem S, Bolondi L, Greten TF, Galle PR, Seitz JF, Borbath I, Häussinger D, Giannaris T, Shan M, Moscovici M, Voliotis D, Bruix J, SHARP Investigators Study Group (2008) Sorafenib in advanced hepatocellular carcinoma. N Engl J Med 359:378–390
Cheng AL, Kang YK, Chen Z, Tsao CJ, Qin S, Kim JS, Luo R, Feng J, Ye S, Yang TS, Xu J, Sun Y, Liang H, Liu J, Wang J, Tak WY, Pan H, Burock K, Zou J, Voliotis D, Guan Z (2009) Efficacy and safety of sorafenib in patients in the Asia-Pacific region with advanced hepatocellular carcinoma: a phase III randomised, double-blind, placebo-controlled trial. Lancet Oncol 10:25–34
Ichikawa W, Uetake H, Shirota Y, Yamada H, Nishi N, Nihei Z, Sugihara K, Hirayama R (2003) Combination of dihydropyrimidine dehydrogenase and thymidylate synthase gene expressions in primary tumors as predictive parameters for the efficacy of fluoropyrimidine-based chemotherapy for metastatic colorectal cancer. Clin Cancer Res 9:786–791
Milano G, McLeod HL (2000) Can dihydropyrimidine dehydrogenase impact 5-fluorouracil-based treatment? Eur J Cancer 36:37–42
Shirasaka T, Shimamato Y, Ohshimo H, Yamaguchi M, Kato T, Yonekura K, Fukushima M (1996) Development of a novel form of an oral 5-fluorouracil derivative (S-1) directed to the potentiation of the tumor selective cytotoxicity of 5-fluorouracil by two biochemical modulators. Anticancer Drugs 7:548–557
Shirasaka T, Shimamoto Y, Fukushima M (1993) Inhibition by oxonic acid of gastrointestinal toxicity of 5-fluorouracil without loss of its antitumor activity in rats. Cancer Res 53:4004–4009
Koizumi W, Kurihara M, Nakano S, Hasegawa K (2000) Phase II study of S-1, a novel oral derivative of 5-fluorouracil, in advanced gastric cancer. For the S-1 Cooperative Gastric Cancer Study Group. Oncology 58:191–197
Shirao K, Ohtsu A, Takada H, Mitachi Y, Hirakawa K, Horikoshi N, Okamura T, Hirata K, Saitoh S, Isomoto H, Satoh A (2004) Phase II study of oral S-1 for treatment of metastatic colorectal carcinoma. Cancer 100:2355–2361
Kawahara M, Furuse K, Segawa Y, Yoshimori K, Matsui K, Kudoh S, Hasegawa K, Niitani H (2001) S-1 Cooperative Study Group (Lung Cancer Working Group), Phase II study of S-1, a novel oral fluorouracil, in advanced non-small-cell lung cancer. Br J Cancer 85:939–943
Inuyama Y, Kida A, Tsukuda M, Kohno N, Satake B (2001) Late phase II study of S-1 in patients with advanced head and neck cancer. Gan To Kagaku Ryoho 28:1381–1390
Okusaka T, Funakoshi A, Furuse J, Boku N, Yamao K, Ohkawa S, Saito H (2008) A late phase II study of S-1 for metastatic pancreatic cancer. Cancer Chemother Pharmacol 61:615–621
Furuse J, Okusaka T, Boku N, Ohkawa S, Sawaki A, Masumoto T, Funakoshi A (2008) S-1 monotherapy as first-line treatment in patients with advanced biliary tract cancer: a multicenter phase II study. Cancer Chemother Pharmacol 62:849–855
Naito S, Tsukamoto T, Usami M, Fujimoto H, Akaza H (2010) An early phase II trial of S-1 in Japanese patients with cytokine-refractory metastatic renal cell carcinoma. Cancer Chemother Pharmacol 66:1065–1070
Naito S, Eto M, Shinohara N, Tomita Y, Fujisawa M, Namiki M, Nishikido M, Usami M, Tsukamoto T, Akaza H (2010) Multicenter phase II trial of S-1 in patients with cytokine-refractory metastatic renal cell carcinoma. J Clin Oncol 28:5022–5029
Furuse J, Okusaka T, Kaneko S, Kudo M, Nakachi K, Ueno H, Yamashita T, Ueshima K (2010) Phase I/II study of the pharmacokinetics, safety and efficacy of S-1 in patients with advanced hepatocellular carcinoma. Cancer Sci 101:2606–2611
ChouTC Talalay P (1984) Quantitative analysis of dose-effect relationships: the combined effects of multiple drugs or enzyme inhibitors. Adv Enzyme Regul 22:27–55
Rustum YM (2004) Thymidylate synthase: a critical target in cancer therapy? Front Biosci 9:2467–2473
Copur S, Aiba K, Drake JC, Allegra CJ, Chu E (1995) Thymidylate synthase gene amplification in human colon cancer cell lines resistant to 5-fluorouracil. Biochem Pharmacol 49:1419–1426
Chu E, Voeller DM, Jones KL, Takechi T, Maley GF, Maley F, Segal S, Allegra CJ (1994) Identification of a thymidylate synthase ribonucleoprotein complex in human colon cancer cells. Mol Cell Biol 14:207–213
Chu E, Koeller DM, Johnston PG, Zinn S, Allegra CJ (1993) Regulation of thymidylate synthase in human colon cancer cells treated with 5-fluorouracil and interferon-gamma. Mol Pharmacol 43:527–533
Johnston PG, Drake JC, Trepel J, Allegra CJ (1992) Immunological quantitation of thymidylate synthase using the monoclonal antibody TS 106 in 5-fluorouracil-sensitive and -resistant human cancer cell lines. Cancer Res 52:4306–4312
Longley DB, Harkin DP, Johnston PG (2003) 5-fluorouracil: mechanisms of action and clinical strategies. Nat Rev Cancer 3:330–338
Ferguson PJ, Collins O, Dean NM, DeMoor J, Li CS, Vincent MD, Koropatnick J (1999) Antisense down-regulation of thymidylate synthase to suppress growth and enhance cytotoxicity of 5-FUdR, 5-FU and tomudex in HeLa cells. Br J Pharmacol 127:1777–1786
Yoshioka A, Tanaka S, Hiraoka O, Koyama Y, Hirota Y, Ayusawa D, Seno T, Garrett C, Wataya Y (1987) Deoxyribonucleoside triphosphate imbalance. 5-Fluorodeoxyuridine-induced DNA double strand breaks in mouse FM3A cells and the mechanism of cell death. J Biol Chem 262:8235–8241
Ayusawa D, Shimizu K, Koyama H, Takeishi K, Seno T (1983) Accumulation of DNA strand breaks during thymineless death in thymidylate synthase-negative mutants of mouse FM3A cells. J Biol Chem 258:12448–12454
Chu E, Drake JC, Koeller DM, Zinn S, Jamis-Dow CA, Yeh GC, Allegra CJ (1991) Induction of thymidylate synthase associated with multidrug resistance in human breast and colon cancer cell lines. Mol Pharmacol 39:136–143
DeGregori J, Kowalik T, Nevins JR (1995) Cellular targets for activation by the E2F1 transcription factor include DNA synthesis- and G1/S-regulatory genes. Mol Cell Biol 15:4215–4224
Lin WC, Lin FT, Nevins JR (2001) Selective induction of E2F1 in response to DNA damage, mediated by ATM-dependent phosphorylation. Genes Dev 15:1833–1844
Chellappan SP, Hiebert S, Mudryj M, Horowitz JM, Nevins JR (1991) The E2F transcription factor is a cellular target for the RB protein. Cell 65:1053–1061
Drago-Ferrante R, Santulli A, Di Fiore R, Giuliano M, Calvaruso G, Tesoriere G, Vento R (2008) Low doses of paclitaxel potently induce apoptosis in human retinoblastoma Y79 cells by up-regulating E2F1. Int J Oncol 33:677–687
Komoto M, Nakata B, Nishii T, Kawajiri H, Shinto O, Amano R, Yamada N, Yashiro M, Hirakawa K (2010) In vitro and in vivo evidence that a combination of lapatinib plus S-1 is a promising treatment for pancreatic cancer. Cancer Sci 101:468–473
Tanizaki J, Okamoto I, Takezawa K, Tsukioka S, Uchida J, Kiniwa M, Fukuoka M, Nakagawa K (2010) Synergistic antitumor effect of S-1 and HER2-targeting agents in gastric cancer with HER2 amplification. Mol Cancer Ther 9:1198–1207
Okabe T, Okamoto I, Tsukioka S, Uchida J, Iwasa T, Yoshida T, Hatashita E, Yamada Y, Satoh T, Tamura K, Fukuoka M, Nakagawa K (2008) Synergistic antitumor effect of S-1 and the epidermal growth factor receptor inhibitor gefitinib in non-small cell lung cancer cell lines: role of gefitinib-induced down-regulation of thymidylate synthase. Mol Cancer Ther 7:599–606
Okabe T, Okamoto I, Tsukioka S, Uchida J, Hatashita E, Yamada Y, Yoshida T, Nishio K, Fukuoka M, Jänne PA, Nakagawa K (2009) Addition of S-1 to the epidermal growth factor receptor inhibitor gefitinib overcomes gefitinib resistance in non-small cell lung cancer cell lines with MET amplification. Clin Cancer Res 15:907–913
Takeuchi A, Shiota M, Tatsugami K, Yokomizo A, Eto M, Inokuchi J, Kuroiwa K, Kiyoshima K, Naito S (2011) Sorafenib augments cytotoxic effect of S-1 in vitro and in vivo through TS suppression. Cancer Chemother Pharmacol 68:1557–1564
Lee SJ, Lee J, Park SH, Park JO, Park YS, Kang WK, Lee J, Yim DS, Lim HY (2012) Phase I trial of S-1 in combination with sorafenib for patients with advanced hepatocellular carcinoma. Invest New Drugs 30:1540–1547
Acknowledgments
This work was supported by grants from National Natural Science Foundation of China (No. 30672051), Chinese Society of Clinical Oncology foundation (2010).
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhai, JM., Yin, XY., Lai, YR. et al. Sorafenib enhances the chemotherapeutic efficacy of S-1 against hepatocellular carcinoma through downregulation of transcription factor E2F-1. Cancer Chemother Pharmacol 71, 1255–1264 (2013). https://doi.org/10.1007/s00280-013-2120-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00280-013-2120-2