Abstract
Nrf2 is a key transcription factor, which induces a cytoprotective gene array. Nrf2 is regulated at the posttranslational level through proteasomal degradation through an interaction with the adapter protein Keap1. High levels of Nrf2, resulting from a loss of function mutation in Keap1, were reported in chemoresistant non-small cell lung cancer. We observed very low levels of Nrf2 and of Nrf2-regulated detoxification proteins as a frequent phenotype in the more chemosensitive breast cancer, and when engineering increased Nrf2 levels, we found resistance to both doxorubicin and paclitaxel. We here show that basal Nrf2 levels in different cell lines correlate with their respective sensitivity to a common cytotoxic chemotherapy. Nrf2 and its regulated genes and proteins are the targets of a major strategy in cancer prevention. Molecules that interfere with the Nrf2–Keap1–Cul3 protein–protein interactions result in higher levels of Nrf2. Both naturally occurring and synthetic molecules with this effect have been suggested as clinical chemopreventive agents, including molecules derived from cruciferous vegetables such as the isothiocyanate sulforaphane and even green tea polyphenols. Here, we determine the impact of these putative chemopreventive agents on the sensitivity of established cancer cell lines to chemotherapy. We confirmed that these molecules do increase Nrf2 and detoxification enzyme levels in breast cancer cell lines with very low basal Nrf2 levels, and this is associated with significant chemoresistance to cytotoxic drugs. Both effects are less in another breast cancer cell line with intermediate Nrf2, and in lung cancer cells with high Nrf2, these same molecules have no effect on Nrf2 but do actually enhance chemoresitance. While the details of dose and schedule of these agents require further study in in vivo models, these data sound a cautionary note for the use of these agents in patients with established cancers who are undergoing chemotherapy treatment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The comprehensive system that detoxifies a range of environmental and endogenous toxins, mutagens, and potential carcinogens is composed of multiple antioxidant and detoxifying enzymes and drug transporters [1–4]. Nrf2 is a master transcriptional regulator of phase II antioxidant and detoxifying enzymes, which binds to the cis-acting ARE (antioxidant response element) present in the promoters of multiple phase II detoxifying genes in a heterodimeric complex with a small Maf protein. The Nrf2-regulated battery of carcinogen-detoxifying enzymes includes glutathione S-transferase (GST), γ-glutamylcysteine synthetase (γGCS), NADP (H): quinone oxidoreductase1 (NQO1), aldo–keto reductase family 1, member C1 (AKR1C1) and UDP: glucuronosyl transferase (UGT) and the ABCC1 transporter [5–7].
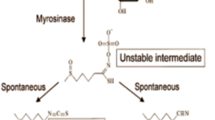
An important mechanism for the regulation of stability and cellular localization of Nrf2 and therefore its activity is controlled at the posttranslational level. Under basal redox conditions, the redox-sensitive protein Keap1 tightly binds to Nrf2 and anchors it in the cytoplasm. Keap1 serves as an adaptor protein for the Cullin 3 ubiquitin E3 ligase (Cul3), which then specifically targets Nrf2 for degradation by the ubiquitin–proteasome pathway [8–10]. With oxidative stress, Keap1 undergoes conformational changes that disrupt its interaction with Nrf2, freeing it for interaction with promoter sequences of the target genes. The Cullins assemble into multiple E3 ligases by interacting with a protein motif present in multiple proteins [9]. The interaction between Nrf2, Keap1, and Cul3 represents a target for the development of molecules that interfere with Nrf2 ubiquination and thus result in increased Nrf2 and Nrf2-regulated proteins. Such molecules are developed as putative chemopreventive agents [11, 12]. For example, the isothiocyanate sulforaphane, derived from glucoraphanin present in cruciferous vegetables, is known to interact with Keap1 and thereby disrupt Nrf2 proteasomal degradation [13].
The present study was aimed to determine if chemicals used to raise Nrf2-regulated cell detoxification systems with chemoprevention in mind, and also result in resistance to treatment in established cancer cells. These chemicals come from various sources. For example, coffee drinking has been associated with reduced incidence of some experimental cancers, potentially due to modification of the metabolism of dietary heterocyclic amine carcinogens by the coffee constituents kahweol (KAW) and cafestol (CAF) diterpenes. The chemopreventive effect of coffee has also been suggested in population-based studies [17–19]. These molecules act at least in part by increasing Nrf2 for transcriptional activation function. Others, such as the isothiocyanate sulforaphane (SFP), [5-(2-pyrazinyl)-4-methyl-1,2-dithiole-3-thione] (oltipraz) or green tea polyphenols, such as epigallocatechin gallate (EGCG) have also been examined in experimental models and are chemoprotective and do activate the Nrf2-regulated pathways [13, 20–23].
Recent studies have shown a link between Nrf2 expression and chemoresistance. Mutations in Keap1 have been identified in non-small-cell lung cancer clinical specimens and cell lines, which functionally disrupt the Cul3-dependent Nrf2 degradation, increase Nrf2 levels and activity, which in turn activate the transcription of antioxidant, xenobiotic metabolism, drug efflux pumps, and intrinsic chemoresistance [14, 15]. On the other hand, we have shown that many breast cancer cell lines and clinical specimens have decreased Nrf2 levels, due to increased Cul3 expression and consequent proteasomal degradation. This is of interest because breast cancer is generally more chemosensitive than in lung cancer. We reversed this phenotype in Cul3-silenced cells, which resulted in high levels of Nrf2 and Nrf2-regulated detoxification mechanisms and significant resistance to chemotherapeutic drugs [16].
Materials and methods
Chemicals and antibodies
Oltipraz was provided by the National Cancer Institute of the United States. D3T was kindly provided by Dr. Thomas Kensler (John Hopkins University) MG132 was purchased from Sigma-Aldrich (St. Louis, MO). Sulforafane (SFP) was purchased from LKT Labs (St. Paul, MN). Kahweol (KAW) and cafestol (CAF) palmitates were purchased from Nestle Research Center (Lausanne, Switzerland). The green tea phenol EGCG was purchased from Sigma Chemical Co. (St Louis, MO, USA). The antibody against Nrf2 was from Santa Cruz Biotechnology Co. (Santa Cruz, CA). The rabbit polyclonal antibodies against the GSTA1/2, GSTP1, γGCS, and NQO1 were generously provided by Dr. John D. Hayes (University of Dundee, Scotland, UK).
Cell culture
The MCF-7 and MDA-231 breast cancer cell lines and the A549 non-small cell lung cancer cell line were all obtained from ATCC (Manassas, VA) and maintained in RPMI 1640 with 10% FBS.
Western blotting
The nuclear extract was prepared as previously described [24]. Thirty microgram of nuclear extract or 60 μg of cytoplasmic extract was resolved by SDS-PAGE, transferred onto nitro-cellulose membranes. The membranes were blocked with 5% fat-free milk solution and then sequentially incubated with primary antibodies and the enzyme-conjugated secondary antibody. The results were documented on X-ray films with ECL detection. Antibodies against Nrf2 and the detoxification enzymes studied were used to detect their respective protein levels. We have previously confirmed the use of these antibodies and the correct size position of Nrf2 using Nrf2 over-expressing cell extracts [16].
Gene expression analysis by RT-PCR
Total RNA was isolated from the MCF7 cells with the Trizol reagent, according to the manufacturer’s protocol (Invitrogen). The mRNA amplification was performed with the One-Step RT-PCR kit (QIAGEN) according to the manufacturer’s instructions. Each RT-PCR reaction contained 20 ng of total RNA, 250 μM dNTPs, 50 pmol of each primer, and 10 unit of enzyme in a final volume of 25 μl. The RT-PCR profile was 50°C for 30 min, 95°C for 15 min, followed by 32 cycles of 94°C for 40 s, 55°C for 30 s and 72°C for 1 min, and a final 10 min extension at 72°C. RT-PCR products were analyzed on 1.0% agarose gels. Sequences of the primers were generated for each of the detoxification enzyme encoding genes studied, using previously available sequence data for γGCS, AKR1C1, GSTP1, and UGDP.
Cytotoxicity assays
Cytotoxicity assays were performed in all three cell lines, examining their relative sensitivity to doxorubicin and to paclitaxel. To study the effects of pre-and concurrent exposure to putative chemopreventive agents, cells were seeded in 96 well plates at a density of 2,000 cells/well. After 24 h, the cells were treated with SFP or EGCG for 24 h, after which either doxorubicin or paclitaxel was added for an additional 48 h, as indicated in the specific experiments, at the indicated concentrations. The cells were incubated for 5 days before the cell survival being measured by MTT assay. The absorbance was determined at 570 nm with a microplate reader (Bio-Rad, model 450). Cell survival was evaluated 5 days post-addition of doxorubicin or paclitaxel using the MTT assay. Cell survival is expressed as percentage of cell growth in comparison with or without the “chemopreventive” agent (SFP, KAW, CEF, or EGCG). The unpaired Student’s t test was used to compare between the treated and the untreated cells (*P < 0.05).
Results
Baseline levels of nuclear Nrf2 in the three cell lines, and chemosensitivity to doxorubicin
Figure 1a shows the results of Western blotting of nuclear protein extracts from each of the three human cancer cell lines studied, with antibodies to Nrf2. Actin is immunoblotted as a loading control. There is a significant gradient of levels of Nrf2 protein, with A549 > MDA231 > MCF7 cells. Figure 1b shows the survival curves for each of the cell lines to doxorubicin. The sensitivity of the cells to this cytotoxic drug also form a gradient, in inverse order to Nrf2 levels, with MCF7 > MDA231 > A549.
The effects of putative chemopreventive molecules on Nrf2 and its regulated genes’ expression in an established human breast cancer cell line
We examined these effects of various putative chemoprotective agents in MCF7 cells, to confirm that the effects shown in a variety of models and cells are also true of an established human cancer cell line. Figure 2 shows the results of Western blotting of MCF7 cells after exposure to chemopreventive molecules known to increase Nrf2 and its transcriptional function. After 24-h exposure to oltipraz, 1,2-dithiole-3-thione (D3T) (D3T) and EGCG at the respective highest non-toxic doses, Nrf2 protein in these cells is increased. This is associated with increased mRNA levels for some of the genes which encode detoxification enzymes, which are known to be Nrf2 regulated, including γGCS, AKR1C1, GSTP1, and UGDP (Fig. 3a). Indeed, the protein levels of these transcriptional-activated genes are increased, as shown for some of these and others, including NQO1, in Fig. 3b.
Nrf2 protein level can be increased by exposing the cells with the putative chemopreventive agents including oltipraz, D3T, KAW, and EGCG. The results showed that oltipraz and D3T could potently upregulate Nrf2 expression, while KAW and EGCG could moderately induce Nrf2 expression. Nrf2 is measured in whole cell lysates, with GAPDH as the loading control
The effects of putative chemopreventive molecules on Nrf2 protein levels in three human cancer cell lines
We then returned to the three human cell lines in which we found differences in Nrf2 levels and in sensitivity to doxorubicin-induced cytotoxicity, using Western immunoblottong. Figure 4 shows that in MCF7 cells exposed to sub-toxic doses of SFP and EGCG for 24 h, Nrf2 levels are increased in a dose-dependent fashion to both. In MDA231 cells treated in exactly the same way, adjusting for differences in protein loading, there is a small effect of EGCG, while Nrf2 was significantly increased to the same degree at both doses of sulforaphane. In contrast, the A549 cells exposed to the same agents under the same conditions showed no change or even decreased Nrf2 levels in response to the two higher doses of EGCG, and no change in response to sulforaphane exposure.
The effect of Nrf2-inducing putative chemoprotective molecules on the cytotoxicity of doxorubicin and paclitaxel in the three human cell lines tested
We selected a synthetic (SFP) and naturally occurring molecule (EGCG) to explore the potential implications of the results above. Cells were exposed to the putative chemopreventive agents EGCG and SFP, at their respective highest non-toxic doses, for 24 h, and then the medium was changed and the same molecule was added plus either doxorubicin or paclitaxel. Just as there is a gradient of Nrf2 nuclear protein content across these three cell lines, there is also a significant different in the effects of these molecules on cytotoxicity. Figure 5 demonstrates that EGCG and SFP confer significant resistance in MCF7 cells, to both doxorubicin (three- to sixfold, respectively, in a dose-dependnt manner) and to paclitaxel (3- to >100-fold, respectively).
The cytotoxic effect of either doxorubicin or paclitaxel in MCF7, MDA231 or A549 cell lines, respectively. Pretreatment with sub-toxic doses of EGCG or SFP confers varying degrees of resistance to the cytotoxic drug-induced cell death. Cell survival is expressed in comparison to cells treated with solvent alone. Values represent the mean ± SEM of three independent measurements. Statistical analysis (Student’s t test) was performed by comparison of D3T- or SFP-treated and untreated cells (*P < 0.05)
MDA-231 cells are less sensitive to doxorubicin and to paclitaxel, as seen previously. Exposure to EGCG results in approximately threefold resistance to doxorubicin, but SFP has no effect on doxorubicin sensitivity. On the other hand, ECGC at the highest dose results in threefold resistance to doxorubicin, while SFP causes 5- to 100-fold resistance to paclitaxel.
In A549 cells, which are even more resistant to doxorubicin, though not to paclitaxel at baseline, exposure to EGCG has no effect on doxorubicin sensitivity, but sulforaphane appears to significantly enhance doxorubicin cytotoxicity. EGCG has no effect on paclitaxel sensitivity, but there is as high as threefold resistance in cells exposed to sulforaphane.
Discussion
We looked to the chemoprevention literature, where uncoupling Nrf2 from its degradative pathway is a desirable target, and a number of molecules have been discovered or designed to do precisely that. Sulforaphane and green tea polyphenols both fit this description, and some are already encouraged as cancer preventive strategies, and also has been examined in clinical trials looking at its potent impact on inflammatory lung disease [25]. ECGC the major flavonoid in green tea has also been studied in humans, examining its impact on serum lipids and inflammatory markers [26]. The relationship between the Nrf2–Keap1–Cul3 protein interactions and chemotherapy sensitivity has only recently been shown in non-small cell lung cancer, where loss of function Keap1 mutations result in dysregulation of Nrf2 turnover, accumulation of Nrf2 and the detoxification batteries of enzymes it regulates, and hence the frequent intrinsic resistance to chemotherapy in this tumor type [14, 15]. We have demonstrated that the decrease in detoxification enzymes we had previously observed in breast cancer specimens is at least in large part related to diminished Nrf2 protein in breast cancer [16]. The consequence is sensitivity to chemotherapy typical of most breast cancers. The present data disclose that greater complexity is involved. While there appears to be a relationship between Nrf2 protein levels and cellular sensitivity to doxorubicin across these three cell lines, such is not the case for sensitivity to paclitaxel. Hints of the importance of the specific cytotoxic drug involved were observed in our previous work, in which SiRNA silencing of Cul3, that led to increased Nf2 protein, resulted in substantial (50-fold) resistance to doxorubicin, but only modest (<5-fold) resistance to paclitaxel.
Our data in this study also suggest, not surprisingly, that these “Nrf2-inducing agents” have significant off-target effects. This is particularly true for sulforaphane, where we see dramatic resistance induced to paclitaxel, even in cells with no change in Nrf2 protein levels, such as the A549 NSCLC cell line. Sulforaphane is known to have multiple other actions, including interaction with tubulin proteins, which has actually been demonstrated in A549 cells, and our experiments suggest that these may be operative in the A549 cells with very high levels of Nrf2 [27]. The fact that suforphane can result in significant resistance to paclitaxel requires further examination, because this could be clinically significant for lung cancer patients. Another study recently demonstrated the essential role of Nrf2 in cisplatin resistance in lung cancer cell lines, using SiRNA silencing of Nrf2. The effect of increasing Nrf2 above baseline using chemical agents was not examined [28]. The modest chemosensitization to doxorubicin we observed in the A549 cells is of interest, but since this is not a commonly used class of agents in this disease, the clinical significance may be less. EGCG does not appear to have significant impact on chemosensitivity to either drug in A549 cells, perhaps because it is a less potent Nrf2 inducer, or less potent effector, in general.
While our data are very preliminary, the notion expressed in some of the popularly read non-peer reviewed “prevention/nutrition literature” that there is a convergence between anti-cancer treatment and cancer prevention, and that they should both be approached in the same manner, is potentially risky. It is often recommended in those media that some of these molecules can be helpful in “detoxifying” a cancer patient of the carcinogenic factors.
We do indeed find that these molecules both increase Nrf2 and also activate detoxification pathways in some established cancer cells, and that in some contexts this results in significant resistance to standard cytotoxic drugs. The Nrf2 data in this report is not intended to necessarily prove that this is the sole mechanism of the chemoresistance that we observe to be induced. Rather, we are demonstrating that these molecules can indeed induce the cellular detoxification regulatory pathway, as intended in the chemoprevention scenario, and at that dose there is an associated chemoresistance in established tumor cell lines. For some cells, the basal level of Nrf2 may determine the effect of some of these agents. Additional studies are ongoing to fully assign mechanism.
We may even have underestimated the full spectrum of these effects, since, for example, green tea polyphenols have been shown to internalize the EGF receptor of cells, which could render then insensitive to the kinase inhibitors currently in use in various forms of cancer which specifically target EGFr [29]. One study did find that sulforaphane sensitized non-transformed mouse fibroblasts in vitro to doxorubicin, although the sulforaphane dose was in a low cytotoxic range [30]. This raises the possibility of a scenario in which chemopreventive molecules are sensitive to non-malignant cells while rendering cancer cells resistant to cytotoxic chemotherapy.
The specific enzymes we have found increased in response to increasing available Nrf2 have interesting and relevant effects on cellular resistance, e.g., AKR expression affects cellular resistance to methotrexate [31], and a polymorphism of NOQ1 is noted to be a strong predictive factor in breast cancer [32].
Our findings provide a cautionary note with regards to the use of these putative chemopreventive agents during anti-cancer therapy. While more work is required to determine dose and schedule of these putative chemopreventive agents’s effect on Nrf2 and on chemoresistance, at least in the case of the green tea catechin EGCG, an in vivo model has already demonstrated an effect on intestinal Nrf2 that is related to resistance to radiation-induced damage.
References
Hayes JD, McMahon M (2001) Molecular basis for the contribution of the antioxidant responsive element to cancer chemoprevention. Cancer Lett 174(2):103–113
Kwak MK, Egner PA, Dolan PM, Ramos-Gomez M, Groopman JD, Itoh K et al (2001) Role of phase 2 enzyme induction in chemoprotection by dithiolethiones. Mutat Res 480–481:305–315
Rushmore TH, Kong AN (2002) Pharmacogenomics, regulation and signaling pathways of phase I and II drug metabolizing enzymes. Curr Drug Metab 3(5):481–490
Nakata K, Tanaka Y, Nakano T, Adachi T, Tanaka H, Kaminuma T et al (2006) Nuclear receptor-mediated transcriptional regulation in Phase I, II, and III xenobiotic metabolizing systems. Drug Metab Pharmacokinet 21(6):437–457
McMahon M, Itoh K, Yamamoto M, Chanas SA, Henderson CJ, McLellan LI et al (2001) The Cap’n’Collar basic leucine zipper transcription factor Nrf2 (NF-E2 p45-related factor 2) controls both constitutive and inducible expression of intestinal detoxification and glutathione biosynthetic enzymes. Cancer Res 61(8):3299–3307
Ramos-Gomez M, Kwak MK, Dolan PM, Itoh K, Yamamoto M, Talalay P et al (2001) Sensitivity to carcinogenesis is increased and chemoprotective efficacy of enzyme inducers is lost in nrf2 transcription factor-deficient mice. Proc Natl Acad Sci USA 98(6):3410–3415
Maher JM, Dieter MZ, Aleksunes LM, Slitt AL, Guo G, Tanaka Y, Scheffer GL, Chan JY, Manautou JE, Chen Y, Dalton TP, Yamamoto M, Klaassen CD (2007) Oxidative and electrophilic stress induces multidrug resistance-associated protein transporters via the nuclear factor-E2-related factor-2 transcriptional pathway. Hepatology 46(5):1597–1610
Cullinan SB, Gordan JD, Jin J, Harper JW, Diehl JA (2004) The Keap1-BTB protein is an adaptor that bridges Nrf2 to a Cul3-based E3 ligase: oxidative stress sensing by a Cul3-Keap1 ligase. Mol Cell Biol 24(19):8477–8486
Furukawa M, Xiong Y (2005) BTB protein Keap1 targets antioxidant transcription factor Nrf2 for ubiquitination by the Cullin 3-Roc1 ligase. Mol Cell Biol 25(1):162–171
Zhang DD, Lo SC, Cross JV, Templeton DJ, Hannink M (2004) Keap1 is a redox-regulated substrate adaptor protein for a Cul3-dependent ubiquitin ligase complex. Mol Cell Biol 24(24):10941–10953
Giudice A, Montella M (2006) Activation of the Nrf2-ARE signaling pathway: a promising strategy in cancer prevention. Bioessays 28(2):169–181
Surh YJ (2003) Cancer chemoprevention with dietary phytochemicals. Nat Rev Cancer 3(10):768–780
Tan XL, Spivack SD (2009) Dietary chemoprevention strategies for induction of phase II xenobiotic-metabolizing enzymes in lung carcinogenesis: a review. Lung Cancer 65(2):129–137
Singh A, Misra V, Thimmulappa RK, Lee H, Ames S, Hoque MO et al (2006) Dysfunctional KEAP1-NRF2 interaction in non-small-cell lung cancer. PLoS Med 3(10):e420
Ohta T, Lijima K, Miyamoto K, Nakahara I, Tanaka H, Ohtsuji M, Suzuki T, Kobayashi A, Yokota J, Sakiyama T, Shibata T, Yamamoto M, Hirohashi S (2008) Loss of Keap 1 function activates Nrf2 and provides advantages for lung cancer cell growth. Cancer Res 1;68(5):1303–1309
Loignon M, Miao W, Hu L, Bier A, Tarek A, Bismar P, Scrivens J, Mann K, Basik M, Fiset P, Batist Z, Batist G (2009) Cul3 overexpression depletes Nrf2 in breast cancer and is associated with sensitivity to carcinogens oxidative stress and to chemotherapy. Mol Cancer Ther 8(8):2432–2440
Steinkellner H (2005) Coffee consumption induces GSTP in plasma and protects lymphocytes against (±)-anti-benzo[a]pyrene-7,8-dihydrodiol-9,10-epoxide induced DNA-damage: results of controlled human intervention trials. Mutat Res 11;591(1–2):264–275
Higgins YLG (2008) Induction of cancer chemopreventive enzymes by coffee is mediated by transcription factor Nrf2. Evidence that the coffee-specific diterpenes cafestol and kahweol confer protection against acrolein. Toxicol Appl Pharmacol 226(3):328–337
Huber WW (2004) Potential chemoprotective effects of the coffee components kahweol and cafestol palmitates via modification of hepatic N-acetyltransferase and glutathione S-transferase activities. Environ Mol Mutagen 44(4):265–276
Yuan JH (2008) Protective effects of epigallocatechin gallate on colon preneoplastic lesion induced by 2-amino-3-methylimidazo [4, 5-f] quinoline in mice. Mol Med 28:414–416
Hu L (2008) Modification of gamma-radiation response in mice by green tea polyphenols. Phytother Res 22:1380–1383
Yuan J-H, Li Y-Q, Yang X-Y (2008) Protective effects of epigallocatechin gallate on colon preneoplastic lesion induced by 2-amino-3-methylimidazo [4, 5-f] quinoline in mice. Mol Med 14:590–598
Miao W, Hu L, Kandouz M, Batist G (2003) Oltipraz is a bifunctional inducer activating both phase I and phase II drug-metabolizing enzymes via the xenobiotic responsive element. Mol Pharmacol 64(2):346–354
Dignam JD, Lebovitz RM, Roeder RG (1983) Accurate transcription initiation by RNA polymerase II in a soluble extract from isolated mammalian nuclei. Nucleic Acids Res 11(5):1475–1489
Riedl MA, Saxon A, Diaz-Sanchez D (2009) Oral sulforaphane increases phase II antioxidant enzymes in the human upper airway. Clin Immunol. 130(3):244–251
Nakagawa K, Nakayama K, Nakamura M, Sookwong P, Tsuduki T, Niino H, Kimura F, Miyazawa T (2009) Effects of co-administration of tea epigallocatechin-3-gallate (EGCG) and caffeine on absorption and metabolism of EGCG in humans. Biosci Biotechnol Biochem 73(9):2014–2017
Mi L, Gan N, Cheema A, Dakshanamurthy S, Wang X, Yang DC, Chung FL (2009) Cancer preventive isothiocyanates induce selective degradation of cellular α- and β-tubulins by proteasomes. J Biol Chem 284(25):17039–17051
Homma S, Ishii Y, Morishima Y, Yamadori T, Matsuno Y, Haraguchi N, Kikuchi N, Satoh H, Sakamoto T, Hizawa N, Itoh K, Yamamoto M (2009) Nrf2 enhances cell proliferation and resistance to anticancer drugs in human lung cancer. Clin Cancer Res 15(10):3423–3432
Adachi N (2008) (−)-Epigallocatechin gallate causes internalization of the epidermal growth factor receptor in human colon cancer cells. Carcinogenesis 29:1986–1993
Fimognari C, Nusse M, Lenzi M, Sciuscio D, Cantelli-Forti G, Hrelia P (2006) Sulforaphane increases the efficacy of doxorubicin in mouse fibroblasts characterized by p53 mutations. Mutation Res. 601:92–101
Selga E, Noé V, Ciudad CJ (2008) Transcriptional regulation of aldo-keto reductase 1C1 in HT29 human colon cancer cells resistant to methotrexate: role in the cell cycle and apoptosis. Biochem Pharmacol 75(2):414–426
Fagerholm R, Hofstetter B, Tommiska J, Aaltonen K, Vrtel R, Syrjäkoski K, Kallioniemi A, Kilpivaara O, Mannermaa A, Kosma VM, Uusitupa M, Eskelinen M, Kataja V, Aittomäki K, von Smitten K, Heikkilä P, Lukas J, Holli K, Bartkova J, Blomqvist C, Bartek J, Nevanlinna H (2008) NAD(P)H:quinone oxidoreductase 1 NQO1*2 genotype (P187S) is a strong prognostic and predictive factor in breast cancer. Nat Genet 40(7):844–853
Acknowledgments
We wish to thank Drs. Mark Hannink and Moulay Alaoui-Jamali for insightful discussions; Dr. Voker Blank for providing recombinant Nrf2 reagents; Dr. Lesley Alpert for providing clinical breast cancer specimens; Dr. John D. Haynes for providing the antibodies against GSTA1/2, GSTP1, γGCS and NQO1; Dr. Andrew Stolz for providing the antibody against the AKR1C. This work was supported by the grants from the Canadian Institute of Health Research, the Cancer Research Society and a US army breast cancer research concept award (BC033714), and the Fonds de la recherche en santé du Québec.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hu, L., Miao, W., Loignon, M. et al. Putative chemopreventive molecules can increase Nrf2-regulated cell defense in some human cancer cell lines, resulting in resistance to common cytotoxic therapies. Cancer Chemother Pharmacol 66, 467–474 (2010). https://doi.org/10.1007/s00280-009-1182-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00280-009-1182-7