Abstract
Purpose
Histone deacetylase inhibitors (HDACi) inhibit the growth of cancer cells, and combinations of HDACi with established chemotherapeutics can lead to synergistic effects. We have investigated effects of PXD101 (HDACi in phase II clinical trials) in combination with 5-fluorouracil, on tumour cell proliferation and apoptosis both in vitro and in vivo.
Experimental design
HCT116 cells were studied using proliferation and clonogenic assays. Synergistic inhibition of proliferation and clonogenicity was determined by incubation with PXD101 and 5-fluorouracil, and analysis using CalcuSyn™ software. The effect of combining PXD101 and 5-fluorouracil on apoptosis was examined in vitro using PARP-cleavage and TUNEL. Finally, the effectiveness of combining PXD101 and 5-fluorouracil in vivo was tested using both HT-29 and HCT116 xenograft models.
Results
Synergistic inhibition of proliferation and clonogenicity was obtained when HCT116 cells were incubated with PXD101 and 5-fluorouracil. 5-fluorouracil combined with PXD101 also increased DNA fragmentation and PARP cleavage in HCT116 cells. Incubation with PXD101 down regulated thymidylate synthase expression in HCT116 cells. In vivo studies, using mouse HT29 and HCT116 xenograft models, showed improved reductions in tumour volume compared to single compound, when PXD101 and 5-fluorouracil were combined.
Conclusions
PXD101 and 5-fluorouracil synergistically combine in their anti-tumour effects against colon cancer cells in vitro and show enhanced activity when combined in vivo. Based on the results presented herein, a rationale for the use of PXD101 and 5-fluorouracil in combination in the clinic has been demonstrated.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Even after four decades of use, 5-fluorouracil (5-FU) remains the cornerstone of current colorectal cancer (CRC) treatments even though resistance to the drug is a common clinical problem. 5-FU is a well-characterised fluoropyrimidine compound whose active metabolite, fluorodeoxyuridine monophosphate (FdUMP) inhibits vital biosynthetic pathways, including the enzyme thymidylate synthase (TS). TS converts deoxyuridine monophosphate (dUMP) to deoxythymidine monophosphate (dTMP), a substrate that is vital for DNA replication and repair. FdUMP competes for the nucleotide-binding site of TS forming a complex with 5,10-methylene tetrahydrofolate and blocking the ability of the natural substrate, dUMP, to bind [1, 2].
In vitro studies have established that in 5-FU resistant cell lines, the levels of TS rise dramatically and this is a major contributing factor towards the mechanism of resistance [3, 4]. Elevated levels of tumour TS have also been repeatedly demonstrated to be a major contributor towards resistance to 5-FU, with high levels of TS being predictive of a poor response [5].
Gene expression is controlled in part by a class of enzymes known as histone deacetylases (HDACs). HDACs are zinc-dependent hydrolases that control remodelling of chromatin by deactylation of specific lysine residues on histone tails [6–8]. The deacetylase action of HDACs has the effect of condensing chromatin and therefore restricting access to the DNA for nuclear proteins such as transcription factors, leading to alterations in gene expression.
Histone deacetylase inhibitors (HDACi) are currently being developed as anti-tumour agents and have been shown to inhibit the growth and induce apoptosis of hyper-proliferating cancer cells. Expression profiling of cells treated with HDACi in vitro showed that under these conditions genes are both up- and down-regulated, at least at the mRNA level [9, 10]. Up to 5% of the total genome has been shown to be regulated by HDACi using microarrays, although the exact figure appears to be dependent on the HDACi and cell line used in the study [9–12]. Altered genes included those required for cellular proliferation, signal transduction, metabolism and metastasis, as well as others. This data has encouraged the investigation of combining HDACi and compounds that have their molecular target(s) regulated by HDACi. Indeed, it has been demonstrated that combinations of HDACi with well-established chemotherapeutics can synergise with their anti-tumour effects [13–15].
We have examined in detail the effects of PXD101 in combination with 5-FU on colorectal tumour cell proliferation and apoptosis, both in vitro and in vivo. PXD101 is an HDACi that shows nM and sub-μM potency in HDAC biochemical and anti-proliferative in vitro assays respectively [16].
PXD101 (hydroxamic acid type HDACi) is currently undergoing phase I/II clinical evaluation for the treatment of multiple cancers types including T-cell lymphoma, multiple myeloma, ovarian and colorectal. Data provided here establishes a rationale for the use of HDACi and 5-FU combinations for the treatment of colorectal cancer.
Materials and methods
Chemicals and antibodies
PXD101 was synthesised to a purity of >98% (determined by HPLC) by the Latvian Institute of Organic Chemistry (Riga, Latvia). The structure of PXD101 (confirmed by NMR) is given in ref. [16]. All other standard reagents and 5-FU were supplied by Sigma-Aldrich (Poole, UK). Primary antibodies used were anti-TS (Abcam Ltd; Cambrige, UK), anti-actin (Sigma; Poole, UK) and anti-poly-ADP-ribose polymerase (R&D Systems; Abingdon, UK).
Cell culture
The colorectal carcinoma cell lines, HCT116 and HT29, were purchased from the American Type Culture Collection (ATCC; Virginia, USA) and European Collection of Cell Cultures (ECACC; Salisbury, UK) respectively. Culture medium (HCT116 – RPMI 1640 and HT29 – McCoy’s 5A) was supplemented with 10% (v/v) FCS and penicillin (100 U/ml), streptomycin (0.1 mg/ml) and cells incubated at 37°C in an atmosphere containing 5% CO2.
WST-1 proliferation assays
Cells were seeded in 96-well plates at 3 × 103 cells/well in 50 μl of culture medium. The following day compound was serially diluted in culture medium at a 2 × concentration and 50 μl of each dilution added per well in triplicate. Plates were incubated for the designated time at 37°C in a 5% CO2 atmosphere and the number of viable cells assessed using cell proliferation reagent WST-1 (Roche, Mannheim, Germany). 10 μl of reagent were added to each well and after a 1 h incubation period, absorbance was measured at 450 nm subtracting absorbance at 690 nm as a reference. Data were analysed using GraphPad Prism (GraphPad Software, CA, USA) and Calcusyn (Biosoft, Cambridge, UK) as appropriate. Using Calcusyn, synergy or antagonism is reported using an output value known as the combination index (CI). A full description of how the CI mathematical equation is derived and CI values are calculated can be found in ref. [17]. Table 1 outlines the descriptive meanings that the range of reported CI values represent.
Clonogenic assays
In vitro colony forming assays were performed essentially to the same protocol as outlined in ref. [18]. Briefly, HCT116 cells were cultured with compounds for the indicated times and seeded onto 35 mm dishes in 3% (w/v) agar containing a sheep erythrocyte feeder layer. Agar plates were cultured for 14–21 days at 37°C and colonies counted using a digital colony counter and Sorcerer image analysis software (Perceptive Instruments Ltd, Suffolk, UK). Data were analysed using GraphPad Prism (GraphPad Software, CA, USA) and Calcusyn (Biosoft, Cambridge, UK) as appropriate.
Western blotting
Sub-confluent HCT116 cells were exposed to compounds as required and incubated for up to 24 h, then harvested by trypsinisation and washed twice in ice cold PBS. The cells were re-suspended in two volumes of buffer (60 mM Tris–HCl pH 7.4, 30% (v/v) glycerol, 450 mM NaCl) and lysed by three freeze-thaw cycles (dry ice/30°C). Cell debris was removed by centrifugation at 20,000 g and the supernatant stored at −20°C.
Forty micrograms of proteins were electrophoresed on SDS-PAGE gels and transferred to nitrocellulose membranes then blocked in phosphate-buffered saline (137 mM NaCl, 2.7 mM KCl, 8.1 mM Na2HPO4, 1.5 mM KH2PO4) containing 0.05% (v/v) Tween 20 (PBST) and 5% (w/v) non-fat milk for 1 h at room temperature. Blots were incubated overnight at 4°C in primary antibodies diluted in PBST, washed and incubated with a suitable secondary antibody diluted in PBST with 5% (w/v) non-fat milk for 1 h at room temperature. Antibody binding was detected using ECL reagent and X-ray film.
Apoptosis analysis
An evaluation of apoptosis was performed using an In Situ Cell Death Detection Kit (Roche Diagnostics Ltd, East Sussex, UK) that employs the principle of the TdT (terminal deoxynucleotidyl transferase)-mediated dUTP nick end labelling (TUNEL) reaction, as follows.
375 × 103 HCT116 cells were plated onto a 75 cm2 flask and cultured overnight. Compounds were added to the cells and incubated at 37°C in an atmosphere with 5% CO2. After incubation, medium was removed and cells harvested, washed and resuspended in 4% (w/v) paraformaldehyde. Cells were fixed at room temperature for 30 min then washed twice. Fixed cells were resuspended in 0.5 ml of 0.1% (v/v) Triton X100, incubated on ice to permeabilise the cells, and washed. TUNEL reaction mixture was prepared according to the kit instructions, and each cell pellet was resuspended in 50 μl. Cells were incubated at 37°C for 1 h, washed and resuspended in FACS FLOW solution for FACS analysis using a FACScan system (BD, Oxford, UK).
In vivo xenograft studies
Experiments were conducted at EPO-GmbH, Berlin-Buch, Germany and approved by the Institutional Animal Care and Use Committee at EPO. These standards are equivalent to the UKCCCR guidelines for the welfare of animals in experimental neoplasia (Br J Cancer 58: 109–113, 1988).
Female Ncr:nu/nu mice (Charles River Laboratories, NCI-Frederick, USA) were injected sub-cutaneously with 107 HCT116 cells, and treatment began at day 6 when tumour size reached around 100 mm3. At this stage, animals were randomised into groups of ten for experiments. PXD101 was formulated in l-arginine/isotonic sterile saline (pH ≈ 9.4) to give a final concentration sufficient for a dose of 100 mg/ml. 5-FU for clinical use was diluted with isotonic sterile saline and used at a sufficient concentration for a dose of 15 mg/ml. PXD101 was administered for 5 days each week for 2 weeks in the morning followed by 5-FU in the afternoon as appropriate. Tumour diameters were measured at 3-day intervals using calliper measurements and estimated assuming spherical geometry according to the formula: (Width2 × Length)/2, until day 31 when the study was terminated. Relative tumour volumes compared to pre-treatment are also shown to account for variations in starting tumour volumes.
Following on from the HCT116 xenograft experiments, a further study was performed using HT−29 cells and an increased dose of 5-FU (30 mg/kg) and PXD101 at either 60 or 100 mg/kg. Study treatment began on positive tumour take (day 7), at which point, animals were randomised into groups of 8 and continued until day 35. The 5-FU treatment was stopped after the first 5 day cycle due to weight loss and diarrhoea. Two toxic deaths occurred in the 100/30 mg/kg PXD101/5-FU combination group and the data is not presented here. Mice were therefore administered 60 mg/kg PXD101 for 5 days each week in the morning followed by 30 mg/kg 5-FU in the afternoon during the first week only. Tumour volumes were calculated and are presented as above.
Results
PXD101 and 5-FU are potent inhibitors of HCT116 cell proliferation in vitro
The WST−1 assay tests the viability and/or proliferation of cells by measuring mitochondrial activity by cleavage of a tetrazolium salt to formazan dye by the electron coupling reaction. Using this assay, PXD101 and 5-FU titration curves were produced and gave EC50 values of 0.28 and 7.46 μM for incubations over 48 h, respectively (Fig. 1a, b).
a PXD101 and b 5-FU WST−1 proliferation assays were generated using HCT116 cells incubated with compound for 48 h. EC50 values of 0.28 and 7.46 μM for PXD101 and 5-FU were obtained, respectively. Error bars are masked by data points in Fig. 1a
Effect of PXD101 on TS expression in vitro
As it has been previously reported that HDACi can down-regulate TS [11] we therefore investigated the effects of treatment of HCT116 cells with PXD101. HCT116 cells were incubated with 0.9 μM PXD101 for up to 24 h and immunoblotting of whole cell lysates performed. PXD101 down-regulated TS protein levels after 6 h incubation, with no expression being detectable after 24 h (Fig. 2). Treatment of HCT116 cells with 0.9 μM PXD101 for 24 h also significantly diminished expression of TS at the mRNA level measured by quantitative PCR (data not shown).
Synergistic anti-proliferative effects of PXD101 and 5-FU in vitro
In order to determine if there was any benefit to combining PXD101 with 5-FU on inhibition of proliferation, a constant ratio combination design based on each compound’s EC50 value was used. The maximum concentrations of PXD101 and 5-FU were determined by multiplying their EC50 values by 5.0625, followed by constructing a titration curve using 1.5-fold dilutions. This ensured that all concentrations used were on the linear range of their individual titration curves.
Co-incubation of PXD101 and 5-FU for 48 h produced synergy over a wide range of concentrations with only one combination point being slightly antagonistic (Fig. 3a). Furthermore, the synergistic effects were improved by pre-incubation with PXD101 for 24 h followed by 5-FU for 48 h alone (Fig. 3b). Strong synergy could be produced with this schedule, using adjusted PXD101 concentrations to take into account the shorter exposure time. Again, only one combination point showed some mild antagonism.
a 48 h PXD101/5-FU co-incubation and b 24 h PXD101 followed by 48 h 5-FU alone Calcusyn™ analysis of combination WST−1 data produced using HCT116 cells. For full key to combination values, see Table 1. Values below 0.7 represent synergism
Synergistic anti-clonogenic effects of PXD101 and 5-FU in vitro
The effects of PXD101 and 5-FU alone and in combination on the clonogenicity potential of HCT116 cells were tested in vitro. Both PXD101 and 5-FU proved to be effective inhibitors of colony formation with EC50 values of 13 and 45 μM after 24 h incubation, respectively (Fig. 4a, b).
a PXD101 and b 5-FU clonogenic assays using HCT116 cells incubated with compound for 24 h. EC50 values of 13 and 45 μM for PXD101 and 5-FU were obtained, respectively. c 24 h PXD101/5-FU co-incubation and d 24 h PXD101 followed by 24 h 5-FU alone Calcusyn™ analysis of combination clonogenic assay data. For full key to combination values, see Table 1. Values below 0.7 represent synergism
For combination studies, the maximum concentration of PXD101 was determined by multiplying its EC50 values by 8, followed by constructing a titration curve using twofold dilutions (a rounded concentration of 100 μM was used). The maximum concentration of 5-FU was determined by multiplying its EC50 value by 3, followed by construction of a titration curve using 1.5-fold dilutions. Again, this ensured that all concentrations used were on the linear range of their individual titration curves.
Co-incubation of PXD101 and 5-FU for 24 h produced synergy to strong synergy over a wide range of concentrations (Fig. 4c). Additionally, the synergistic effects were slightly improved by pre-incubation with PXD101 for 24 h followed by 5-FU for 24 h alone (Fig. 4d), with one combination point showing very strong synergism.
Incubation with PXD101 and 5-FU produces enhanced apoptosis over single agent incubations in vitro
HCT116 cells were incubated with PXD101 and 5-FU either alone or in combination for 48 h and whole cell lysates prepared. Western blots were then produced using these lysates and probed with antibodies that detect PARP-cleavage. Cleavage of PARP by Caspase−3 occurs early in the apoptotic response [19]. Incubation of HCT116 cells with either PXD101 (0.7 μM) or 5-FU (17 μM) alone for 48 h produced low levels of PARP cleavage while co-incubation enhanced this effect substantially (Fig. 5a). In contrast, incubating in PXD101 (0.9 μM) for 24 h followed by a further 48 h in 5-FU (11 μM) alone did not lead to enhanced cleavage over either compound alone (data not shown).
The effects of either compound alone on the TUNEL assay in HCT116 cells were enhanced when PXD101 and 5-FU were combined. TUNEL detects apoptosis-induced DNA nicks, which is also one of the hallmarks of apoptosis [20]. Cells were treated with 0.9 μM PXD101 for 24 h followed by a further 48 h in 11 μM 5-FU alone, and the TUNEL assay was performed. PXD101 and 5-FU produced 1.4 and 1.8-fold shifts in the TUNEL positive population, respectively, whereas a 3.4-fold shift was produced when they were combined (Fig. 5b). In contrast to the PARP cleavage experiments a co-incubation schedule only produced a minor shift in TUNEL positive population of around 1.6-fold compared to 1.3-fold using single compound (data not shown). This in line with the data demonstrating that incubation with PXD101, followed by 5-FU, achieved a greater degree of synergy in their anti-proliferative effects.
Enhanced effects of PXD101 and 5-FU combinations in HCT116 and HT29 tumour xenografts
HCT116 tumour bearing mice were treated as described in the methods section with PXD101 (100 mg/kg) and 5-FU (15 mg/kg). At these concentrations each compound alone produced reductions in tumour volume over the measured period (Fig. 6a, b). When PXD101 and 5-FU were administered together there was a further inhibition of tumour growth, with a significant reduction in volume at days 28 and 31 compared to the single compound treated groups (Figs. 6a, b). At day 24, there was a significant reduction in tumour growth with co-administration compared to 5-FU alone only. No significant effect on body weight was observed for any of the treated groups (Fig. 6c).
Effect of PXD101 and 5-FU treatment on a absolute, b relative tumour growth and c body weight in a HCT116 subcutaneous xenograft established in NCR:nu/nu mice. Effect of PXD101 and 5-FU treatment on d absolute, e relative tumour growth and f body weight in a HT29 subcutaneous xenograft established in NCR:nu/nu mice. Statistical analysis for effect on tumour growth was performed using Mann–Whitney U test; *P < 0.05
In a subsequent xenograft experiment, using HT−29 cells, the dose of 5-FU was increased to 30 mg/kg in an attempt to achieve an enhanced effect over that found using 15 mg/kg 5-FU in the HCT116 study. Only one cycle, however, of 5-FU treatment was administered at this level due to toxicity. The combination of 100 mg/kg PXD101 with 30 mg/kg produced four mice with toxic weight loss, two of which subsequently died. This group was, therefore, excluded from subsequent study.
Some tumour inhibition was observed in the 60 mg/kg PXD101 and 30 mg/kg 5-FU single treatment groups, with increased tumour growth inhibition in the PXD101/5-FU (60/30 mg/kg) group (Figs. 6d, e). The effect of the combination is larger when data is normalised to the pre-treatment tumour volume (Fig. 6e), with the tumour reduction by the combination significantly greater than the control and 5-FU alone groups at days 24, 28, 31 and 35. Statistical significance was not achieved compared to the PXD101 alone group at any measurement time.
It should be noted that toxic weight loss was observed in mice from both the 5-FU alone and in the group treated with the combination (Fig. 6f). Owing to this, the 5-FU treatment was halted after only the first weekly cycle allowing body weight recovery, even though they were treated with the second cycle of PXD101.
Discussion
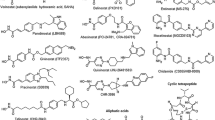
The finding that treatment of cell lines with HDACi in vitro, as demonstrated by others [9–12, 21–23], only appears to regulate a relatively small subset of genes is surprising given the lack of HDAC isoform selectivity that most HDACi demonstrate [24, 25]—see ref. [26] for an overview of the classical HDAC family). Commonly included in the subset of genes that are regulated by HDACi is TS. It has been previously demonstrated that HDACi, including trichostatin A (TSA), suberoylanilide hydroxamic acid (SAHA), MS−275, FK228 and BL1521, can down-regulate the expression of TS in vitro [11, 22, 23, 27]. Down-regulation of TS is likely to be a fundamental response to histone acetylation induced by HDACi treatment since it was not found to be species or cell line/type specific (human breast, prostate, renal, neuroblastoma and rat retinoblastoma were included in these different studies). As discussed in the introduction, over-expression of TS in colorectal cancer in vitro is implicated in the mechanism of resistance to 5-FU [3, 4] and is a marker of poor prognosis clinically [5, 28, 29]. Therefore any reduction in TS levels in patient colorectal tumours may translate into a clinical advantage.
It has been demonstrated here that PXD101, in common with other HDACi, can down-regulate TS expression both at the mRNA and protein level. Similar to other HDACi, it is likely that PXD101 regulates TS levels via effects on histone acetylation [16] and downstream transcription. This led to the hypothesis that combining HDACi, in this case PXD101, with 5-FU should lead to synergism in their anti-proliferative effects. The HCT116 colorectal cancer cell line was employed, which is commonly used as a model for colorectal tumours, to examine this in some detail. Both PXD101 and 5-FU were found to be potent inhibitors of HCT116 cellular proliferation in vitro, in both WST−1 and clonogenic assays, and when combined their effects on proliferation were synergistic. It is plausible that the down-regulation of TS by PXD101 is required for optimal synergy to occur since pre-incubation with PXD101 for 24 h, followed by 48 h with 5-FU, was more effective than the 48 h co-incubation (Fig. 3). In addition to the affect of PXD101 on thymidylate synthase expression, other HDACi have been shown to effect additional molecular pathways involved in colon cancer carcinogensis and growth. These include down-regulation of Cyclin B1 in a p21WAF−1 and transcriptional dependent manner [30], suppression of Cox−2 activation [31] and repression of Src family kinase members [32]. PXD101 may also regulate each of these pathways via its action as an HDACi. It is therefore conceivable that other molecular mechanisms of HDAC inhibition (aside from down-regulation of TS) may be implicated in the synergy of anti-proliferative actions of PXD101 and 5-FU.
In addition to the synergistic effects on proliferation, co-incubation of PXD101 and 5-FU enhanced apoptosis compared with single compound treatment. The PARP-cleavage experiment, however, showed no increased cleavage over single compound alone when the PXD101 pre-incubation followed by 5-FU schedule was used. This is in line with the fact that PARP-cleavage is an early stage event in apoptosis [19]. Owing to this, it is likely to be difficult to distinguish any differences in cleavage between single compound and combinations at such an extended period post compound treatment outset.
To our knowledge, no in vivo data using HDACi/5-FU combinations have been previously described. In line with our in vitro data, results presented here show that both enhanced survival and tumour reduction in vivo over and above single compound treatment can be achieved using PXD101/5-FU combination. It should be noted however, that there was evidence of increased toxicity when doses of 30 mg/kg 5-FU (and above) alone in combination with PXD101 in vivo, in a preliminary toxicology study using B6D2F1 mice (cross between female C57BL/6 and male DBA/2 mice - unpublished data). Due to these observations, a sub-therapeutic concentration of 5-FU (15 mg/kg) was tested and tolerated in the nude mouse HCT116 xenograft when combined with PXD101. Even at this lower concentration, significant beneficial responses were observed when compared to each monotherapy. These data indicate that PXD101 significantly enhances the anti-tumour efficacy of 5-FU in vivo. After the success of the HCT116 study, a second xenograft model using HT29 cells was then established to examine this combination using an elevated dose of 5-FU in an attempt to enhance the effect of the combination. Two toxic deaths were observed, however, when a dose of 100 mg/kg PXD101 was combined with 30 mg/kg 5-FU. After reduction of PXD101 to 60 mg/kg no toxic deaths occurred, although weight loss was observed which could be attributed to the elevated dose of 5-FU since the mice recovered after cessation of the 5-FU treatment. This is in agreement with the preliminary toxicology study performed using B6D2F1 mice, suggesting that the toxicity produced by daily treatments of 30 mg/kg 5-FU and above is not strain specific. Furthermore, even though the combined treatment did not produce a statistically significant effect on tumour growth over PXD101 alone, there was an observable benefit to this combination over single compound treatment (Fig. 6e).
It has been previously demonstrated that the combination of the HDACi SAHA with 5-FU and irinotecan, in hepatoma cell lines, enhanced their anti-proliferative and apoptotic effects in a triple combination [33]. Dual compound incubations, on the other hand, did not produce any superior responses over single compound alone. In a second study, SAHA was also combined with 5-FU using both pre- and post-HDACi incubation schedules in a breast cancer cell line [34]. These authors found no enhanced anti-clonogenic activity over single agent alone, and concluded that only reagents that target DNA, such as Topoisomerase inhibitors, are likely to produce synergy with HDACi. This is based on the finding that treatment with HDACi creates hyper-acetylated histones leading to the relaxation of DNA around chromatin [35–37], allowing increased access to the DNA. It has become clear that this is a simplified view since many of the cellular consequences of HDACi treatment are non-histone related [38, 39] and does not take into account the effects of HDAC inhibition on transcription (see above). Differences between these previously published studies and the data shown here could be due to a number of factors including differences in cell type, scheduling, assay format and the HDACi that was used. Indeed, it is probable that differences in the 5-FU metabolism pathways between breast, hepatoma and colorectal cancer cell lines [40] are a major contributor towards this discrepancy.
In summary, synergy was produced by the combination of PXD101 and 5-FU in vitro, with enhanced anti-tumour effects in vivo in multiple models, as predicted. This data provides validation for the use of HDACi and 5-FU combinations in cancer treatment. Based on this solid biological basis, the rationale for combination therapy using PXD101 and 5-FU has been established. A Phase Ib dose escalation proof-of-concept clinical trial evaluating PXD101 combination therapy with 5-FU for advanced solid tumours and colorectal cancer has been initiated.
References
Santi DV, Brewer CF (1973) Model studies of thymidylate synthetase Intramolecular catalysis of 5-hydrogen exchange and 5-hydroxymethylation of 1-substituted uracils. Biochemistry 12:2416–2424
Santi DV, McHenry CS, Sommer H (1974) Mechanism of interaction of thymidylate synthase with 5-Fluorodeoxyuridylate. Biochemistry 13:471–481
Copur S, Keisuke A, Drake JC, Allegra CJ, Chu E (1995) Thymidylate synthase gene amplification in human colon cancer cell lines resistant to 5-fluorouracil. Biochem Pharmacol 49:1419–1426
De Angelis PM, Fjell B, Kravik KL, Haug T, Tunheim SH, Reichelt W, Beigi M, Clausen OP, Galteland E, Stokke Trond (2004) Molecular characteristics of derivatives of HCT116 colorectal cancer cells that are resistant to the chemotherapeutic reagent 5-fluorouracil. Int J Oncol 24:1279–1288
Longley DB, Harkin DP, Johnston PG (2003) 5-Fluorouracil: Mechanisms of action and clinical strategies. Nat Rev Cancer 3:330–338
McLaughlin F, La Thangue NB (2004) Histone deacetylase inhibitors open new doors in cancer therapy. Biochem Pharmacol 68:1139–1144
Grozinger CM, Schrieber SL (2002) Deacetylase enzymes: biological functions and the use of small-molecule inhibitors. Chem Biol 9:3–16
Hess-Strumpp H (2005) Histone deacetylase inhibitors and cancer: from cell biology to the clinic. Eur J Cell Biol 84:109–121
Joseph J, Mudduluru G, Anthony S, Vashistha S, Ajitkumar P, Somasundaram K (2004) Expression profiling of sodium butyrate (NaB)-treated cells: identification of regulation of genes related to cytokine signalling and cancer metastasis by NaB. Oncogne 23:6304–6315
Chiba T, Yokosuka O, Fukai K, Kojima H, Tada M, Arai M, Imazeki F, Saisho H (2004) Cell growth inhibition and gene expression induced by the histone deacetylase inhibitor trichostatin A, on human hepatoma cells. Oncology 66:481–491
Glaser KB, Staver MJ, Waring JF, Stender J, Ulrich RG, Davidsen SK (2003) Gene expression profiling of multiple histone deacetylase (HDAC) inhibitors: defining a common gene set produced by hdac inhibition in T24 and MDA carcinoma cell lines. Mol Cancer Ther 2:151–163
Lee H, Lee S, Baek M, Kim HY, Jeoung D-I (2002) Expression profile analysis of trichostatin A in human gastric cells. Biotech Lett 24:377–381
Kim MS, Blake M, Baek JH, Kohlhagen G, Pommier Y, Carrier F (2003) Inhibition of histone deacetylase increases cytotoxicity to anti-cancer drugs targeting DNA. Cancer Res 63:7291–7300
Jang ER, Lim S, Lee ES, Jeong G, Kim T-Y, Bang Y-J, Lee J-S (2003) The histone deacetylase inhibitor trichostatin A sensitises estrogen receptor α-negative breast cancer cells to tamoxifen. Oncogene 23:1–13
Marchion DC, Bicaku E, Daud AI, Richon V, Sullivan DM, Munster PN (2004) Sequence-specific potentiation of topoisomerase II inhibitors by the histone deacetylase inhibitor suberoylanilide hyroxamic acid. J Cell Biochem 92:223–237
Plumb JA, Finn PW, Williams RJ, Bandara M, Romero R, Watkins CJ, La Thangue NB, Brown R (2003) Pharmacodynamic response and inhibition of growth of human tumour xenografts by the novel histone deacetylase inhibitor PXD101. Mol Cancer Ther 2:721–728
Chou TC (1991) e median-effect principle and the combination index for the quantitation of synergism and antagonism. In: Chou TC, Rideout DC (eds) Synergism and antagonism in chemotherapy. Academic, San Diego, pp 61–102
Roed H, Christensen IJ, Vindeloev LL, Spang-Thomsen M, Hansen HH (1987) Inter-experiment variation and dependence on culture conditions in assaying the chemosensitivity of human small cell lung cancer cell lines. Eur J Cancer Clin Oncol 23:177–186
Duriez PJ, Shah GM (1997) Cleavage of poly(ADP-ribose) polymerase: a sensitive parameter to study cell death. Biochem Cell Biol 75(4):337–349
Allen RT, Hunter III WJ, Agrawal DK (1997) Morphological and biochemical characterization and analysis of apoptosis. J Pharmacol Toxicol Methods 37:215–228
Chiba T, Yokosuka O, Arai M, Tada M, Fukai K, Imazeki F, Kato M, Seki N, Saisho H (2004) Identification of genes up-regulated by histone deacetylase inhibition with cDNA microarray and exploration of epigenetic alterations on hepatoma cells. J Hepatology 41:436–445
Sasakawa Y, Naoe Y, Sogo N, Inoue T, Sasakawa T, Matsuo M, Manda T, Mutoh S (2005) Marker genes to predict sensitivity to FK228, a histone deacetylase inhibitor. Biochem Pharmacol 69:603–616
Ruijter AJM, Meinsma RJ, Bosma P, Kemp S, Caron HN, Kuilenburg ABP (2005) Gene expression profiling in response to the histone deacetylase inhibitor BL1521 in neuroblastoma. Exp Cell Res 309:451–467
Suzuki T, Miyata N (2005) Non-hydroxymate histone deacetylase inhibitors. Curr Med Chem 12:2867–2880
Kelly WK, Marks PA (2005) Drug insight: histone deacetylase inhibitors – development of the new targeted anticancer agent suberoylanilide hydroxamic acid. Nat Clin Pract Oncol 2:150–157
De Ruijter AJM, Van Gennip AH, Caron HN, Kemp S, Van Kuilenburg ABP (2003) Histone deacetylases (HDACs): characterization of the classical HDAC family. Biochem J 370:737–749
Siddiqui H, Solomon DA, Gunawardena RW, Wang Y, Knudsen ES (2003) Histone deacetylation of RB-responsive promoters: requisite for specific gene repression but dispensible for cell cycle inhibition. Mol Cell Biol 23:7719–7731
Chu E, Callender MA, Farrell MP, Schmitz JC (2003) Thymidylate synthase inhibitors as anticancer agents: from bench to bedside. Can Chem Pharmacol 52:S80–S89
Allen WL, Johnston PG (2005) Role of genomic markers in colorectal cancer treatment. J Clin Oncol 23:4545–4552
Archer SY, Johnson J, Kim HJ, Ma Q, Mou H, Daesety V, Meng S, Hodin RA (2005) The histone deacetylase inhibitor butyrate downregulates cylcin B1 expression via a p21/WAF−1-dependent mechanism in human colon caner cells. Am J Physiol Gastrointest Liver Physiol 289:G696–G703
Tong X, Yin L, Giardina C (2004) Butyrate suppresses Cox−2 activation in colon cancer cells through HDAC inhibition. Biochem Biophys Res Commun 317:463–471
Hirsch CL, Smith-Windsor EL, Bonham K (2006) Src family kinase members have a common response to histone deacetylase inhibitors in human colon cancer cells. Int J Cancer 118:547–554
Ocker M, Alajati A, Ganslmayer M, Zopf S, Lüders M, Neureiter D, Hahn EG, Schuppan D, Herold C (2005) The histone-deacetylase inhibitor SAHA potentiates proapoptotic effects of 5-fluorouracil and irinotecan in hepatoma cells. J Cancer Re Clin Oncol 131:385–394
Kim MS, Blake M, Baek JH, Kohlhagen G, Pommier Y, Carrier F (2003) Inhibition of histone deacetylase increases cytotoxicity to anticancer drugs targeting DNA. Cancer Res 63:7291–7300
Davie JR (1998) Covalent modifications of histones: expression from chromatin templates. Curr Opin Genet Dev 8:173–178
Marks PA, Richon VM, Rifkind RA (2000) Histone deactetylase inhibitors: Inducers of differentiation or apoptosis of transformed cells. J Natl Cancer Inst 15:1210–1216
Grant PA (2001) A tale of histone modifications. Genome Biol 2:reviews0003.1–0003.6
Hu J, Colburn NH (2005) Histone deacetylase inhibition down-regulates cyclin D1 transcription by inhibiting nuclear factor-κB/p65 DNA binding. Mol Cancer Res 3:100–109
Lin HY, Chen CS, Lin SP, Weng JR, Chen CS (2006) Targeting histone deacetylase in cancer therapy. Med Res Rev 26:397–413
Kamoshida S, Shiogama K, Shimomura R, Inada K, Sakurai Y, Ochiai M, Matuoka H, Maeda K, Tsutsumi Y (2005) Immunohistochemical demonstration of fluoropyrimidine-metabolizing enzymes in various types of cancer. Oncol Rep 14:1223–1230
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tumber, A., Collins, L.S., Petersen, K.D. et al. The histone deacetylase inhibitor PXD101 synergises with 5-fluorouracil to inhibit colon cancer cell growth in vitro and in vivo. Cancer Chemother Pharmacol 60, 275–283 (2007). https://doi.org/10.1007/s00280-006-0374-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00280-006-0374-7