Abstract
The peritoneal surface remains an important failure site for patients with colorectal cancer. We have recently shown that albendazole (ABZ), a safe and effective anthelmintic drug, has profound antitumor activity in hepatocellular cancer. Furthermore, albendazole also possesses unique physiochemical and pharmacokinetic properties probably making it a potential drug for use in the regional treatment of peritoneal carcinomatosis (PC). The current study was therefore designed to investigate this concept under both in vitro and in vivo conditions using human colorectal cancer cells HT-29. In cell culture, studies were conducted to investigate the effect of ABZ and its major metabolites, albendazole sulfoxide (ABZ-SO) and albendazole sulfone (ABZ-SO2) on the growth of human colorectal cell line HT-29. We also investigated the effects of ABZ on the cell cycle and the possible induction of apoptosis in these cells. Male nude mice inoculated intraperitoneally (i.p.) with HT-29 cells were treated with various schedules of ABZ given i.p. or orally for 6 weeks. Response was evaluated as the number of peritoneal tumor nodules present in animals at the end of the treatment period. In vitro, ABZ treatment of cells for 5 days led to profound inhibition of growth. 3H-Thymidine assay and trypan blue viable cell counts confirmed the dose- and time-dependency of the ABZ effect, while recovery experiments revealed the reversible nature of this inhibition. ABZ-SO and ABZ-SO2 were also evaluated in cell culture studies and compared with the parent drug. In HT-29 cells, the IC50 values were calculated to be 0.12 μM for ABZ and 2.35 μM for ABZ-SO. The other metabolite, ABZ-SO2, was completely inactive. Studies on the mechanism of ABZ action, revealed arrest of HT-29 cells at the G2/M phase of the cell cycle, while TUNEL, DNA laddering and caspase-3 activity all confirmed ABZ induced apoptosis. In nude mice with peritoneal HT-29 xenografts, ABZ profoundly inhibited peritoneal tumor growth. While alternate i.p. dosing (ABZ, 150 mg/kg) led to the highest degree of tumor growth suppression (P<0.001), schedules such as once-weekly dosing and even a single dose for the entire course of treatment (6 weeks) were also effective in reducing peritoneal tumor growth. However, no such activity was observed when ABZ was administered orally. This study shows for the first time the potent effect of regionally administered ABZ in suppressing the growth of peritoneal tumors of human colorectal origin. The effect is thought to be brought about by arresting tumor cells at the G2/M phase of the cycle and apoptosis. These findings provide evidence for potential value of ABZ in the treatment of regional PC arising from colorectal cell lines.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Colorectal carcinoma accounts for 10–20% of all cancers. The major anatomical sites for dissemination of colorectal cancer include lymph nodes, liver, and peritoneal surfaces. Because of the dismal results of conventional drugs, peritoneal carcinomatosis (PC) from colon cancer represents an ideal target for the development of new treatments [1, 2]. The use of systemic chemotherapy has not been shown to be effective in the management of PC, due to poor penetration of the cytotoxic agents into the peritoneal cavity [3].
There has been long-standing interest in the local delivery of drugs into the peritoneum, providing high drug concentrations at the site of tumor for a longer period of time leading to higher efficacy and lower toxicity [4]. However, most cytotoxic agents currently employed in the treatment of PC, are well absorbed from the peritoneum leading to rapid decline of drug concentrations in the peritoneum on the one hand and the presence of the drug in the systemic circulation and toxicity on the other. Therefore to achieve therapeutic goals in this setting, an antiproliferative agent that is retained within the abdominal cavity at a sufficiently high concentration for a long period of time is needed. In pursuit of this target, we have been studying the benzimidazole carbamate (BZ) group of compounds in general, and ABZ in particular, as potential drugs for the treatment of PC. The major application of BZs including ABZ to date has been the treatment of veterinary and human helminthiasis, in which they have demonstrated remarkable efficacy and safety [5]. Our interest in ABZ dates back to the 1980s when the drug was tested for hydatid disease [6, 7].
The elucidation in recent years of the cellular effects of these compounds and especially their binding to tubulin in parasites rekindled our interest in BZs, only this time these compounds were investigated as antitumor agents. Through these studies, we were able to show that in cell culture, ABZ is a highly potent inhibitor of cancer cell proliferation. ABZ inhibits proliferation of a wide variety of cancer cells including a range of hepatocellular cancer cells [8], colorectal cells, ovarian cells, pancreatic cells, and a variety of other malignant human cell lines (unpublished data). We subsequently reported a pilot study in which some patients with colorectal cancer and liver metastases showed a decline or stabilization of tumor markers (CEA) after treatment with oral ABZ [9]. Recently other investigators have provided exciting evidence on the antitumor activity of another BZ anthelmintic drug, mebendazole, in lung cancer cells both in vitro and in nude mice [10, 11].
In addition to the described antitumor effect, ABZ has some important pharmacokinetic properties such as limited aqueous solubility leading to slow absorption and also extensive first-pass metabolism leading to non-detectable plasma concentrations [5, 12, 13]. It was therefore hypothesized that these favorable pharmacological features would make intraperitoneally (i.p.) administered ABZ a potential agent for the regional treatment of PC. Accordingly, the present study was undertaken to investigate the antitumor efficacy of i.p. administered ABZ, using human colorectal cancer cells HT-29 in a nude mouse i.p. xenograft model of PC.
Materials and methods
Chemicals
Metabolites of ABZ, albendazole sulfoxide (ABZ-SO) and albendazole sulfone (ABZ-SO2), were kindly donated by GSK (Australian subsidiary). ABZ and all other agents, solvents or vehicles were obtained from Sigma Chemicals (Australian subsidiary, Sydney). For in vitro work and when used alone, ABZ was dissolved in ethanol with a final cell culture ethanol concentration of 1%. However, when used for comparative studies alongside ABZ-SO and ABZ-SO2, all agents were dissolved in DMSO. This is because at the concentrations required, the metabolites were not sufficiently soluble in ethanol. For in vivo studies, ABZ was suspended in 0.5% carboxymethyl cellulose (CMC).
In vitro cell culture and proliferation assays
HT-29 used in this study was originally obtained from the American Type Culture Collection and maintained according to the supplier’s instructions.
Inhibition of cell proliferation
3H-Thymidine incorporation was used to study the effect of ABZ on cell proliferation in vitro. Cells (2500 per well) plated in 24-well Corning tissue culture dishes were treated with cell culture medium (RPMI plus 5% fetal calf serum) containing various concentrations of ABZ (final concentrations 0.01–10.0 μM). ABZ was originally made up in absolute ethanol and subsequently diluted with medium to give the desired drug concentrations with a final ethanol concentration of 1%. Cells were kept in an incubator at 37°C under a humidified atmosphere containing 5% CO2. The treatment medium was replaced on alternate days. At the end of the treatment period (5 days), cells were assayed for thymidine incorporation by the addition of 0.5 μCi of 3H-thymidine to each well for the last 4 h of culture. The amount of radioactivity incorporated into the cells was determined using a β-scintillation counter [14]. In all experiments, controls for ABZ-treated cells were included, which consisted of cells treated with the medium containing 1% ethanol. Counts were obtained from quadruplicate wells and each experiment was repeated at least twice. Results are presented as means ± SE of actual counts per minute plotted against the concentration of drug used.
Cell viability assay
HT-29 cells seeded in six-well plates were treated with various concentrations of ABZ (0.01–1 μM) on alternate days for 1, 3 or 5 days. At the end of the treatment period, viable cells present in each well of the tissue culture plate were counted using the Trypan blue exclusion method [15].
Recovery from inhibition
This was conducted to find out if the ABZ effect was reversible and if so how rapidly cells would recover from the growth-inhibitory effect. To do this, cells were initially treated with ABZ (0.01–1 μM) once in the culture medium for 3 days. Following this, the medium was replaced and cells were then incubated with drug-free medium for the next 3 days. At the end of treatment period, cell proliferation was measured using the 3H-thymidine assay.
Cell cycle kinetics
HT-29 cells (5×104) were treated with a single 1 μM dose of ABZ for 24, 48 or 72 h. At the end of the treatment period, cells were collected, washed twice with PBS and treated with ribonuclease, Triton X-100 and propidium iodide. The percentage of cells in the G1, S, and G2/M phases of the cell cycle were determined using a FACScan flow cytometer (Becton Dickinson, FACSort) and Multifit cell cycle analysis software (Verity Software) [16].
Apoptosis
TUNEL (TdT-mediated dUTP-biotin nick end labeling), DNA laddering and caspase-3 activity were used to check for the induction of apoptosis by ABZ in these cells.
TUNEL
which characterizes an important biochemical feature of apoptosis, was used to detect apoptosis both in cells treated in vitro with ABZ and also later in tumors excised from nude mice treated with the drug. For this, the TdT-FragEL DNA fragmentation detection kit (Oncogene Research Products, Boston, Mass.) was employed. The kit was used according to the manufacturer’s instructions. In vitro, after treating HT-29 cells with 1 μM ABZ for 5 days, cells were fixed using 4% formalin and later treated with proteinase K and endogenous peroxidases inactivated with 3% H2O2. Then samples were incubated with TdT enzyme for 1.5 h at 37°C and terminated with stop buffer. This was followed by the streptavidin-biotin peroxidase method. Apoptotic cells were visualized after diaminobenzidine color development. The sections were counterstained with 0.3% methyl green. A dark brown staining indicated apoptosis. In vivo, peritoneal nodules were embedded in paraffin blocks and 5.0-μm thick sections were cut. After treatment with xylene and graded ethanol, samples were taken through the same procedure as described above. At least 500 tumor cells were counted for each sample and the apoptotic index (AI) was determined as the percentage of apoptotic cells [17].
DNA fragmentation assay
HT-29 cells were treated with ABZ (1 μM) for 48 h. Both adherent and floating cells were collected for DNA fragmentation analysis. This was carried out according to the method described by Herrmann et al. [18]. Briefly, 1–2 million cells were lysed in lysis buffer (1% triton-X in 20 mM EDTA, 50 mM Tris-HCl, pH 7.5) and after centrifugation the supernatant was extracted again with lysis buffer. Both supernatant and pellet were treated with 1% SDS and 5 μg/μl RNase for 2 h at 56°C. This was followed by further digestion with 5 μg/μl proteinase K for at least 2 h at 37°C. DNA was precipitated and dissolved in Tris-acetate-EDTA. Samples were run on 1% agarose gel and DNA ladders were documented by photography.
Caspase-3 activity
Caspase-3 colorimetric assay kit (Bioscientific, R&D Systems, Gymea, NSW, Australia) was used according to the manufacturer’s instructions. After treatment of cells with 1 μM ABZ for 8, 24 or 48 h, cells were harvested, centrifuged at 250 g for 10 min and the cell pellet lysed by the addition of the lysis buffer. The cell lysate was incubated on ice for 10 min followed by centrifugation at 10,000 g for 5 min. The supernatant was used to start the enzymatic reaction in 96 well plates with each well containing 50 μl cell lysate, 50 μl reaction buffer and 5 μl caspase-3 colorimetric substrate (DEVD-pNA). After incubation of the plate at 37°C for 2 h, the optical density was read at a wavelength of 405 nm. Recombinant caspase-3 enzyme was used as positive control and no cell lysate was used as additional control [19].
In vivo antitumor activity
Male BALB/c nu/nu nude mice at 6 weeks of age purchased form Biological Research Centre of the University of New south Wales (Sydney, Australia) were kept under specific-pathogen-free conditions with free access to autoclaved food and water. All mice were injected i.p. with one million HT-29 cells grown in RPMI 10% FCS. Drug treatment was initiated 24 h after tumor cell inoculation. Mice were randomized to one of five treatment groups (n=10 per treatment). Except for one group which was treated orally (0.1 ml/10 g body weight) on alternate days for 6 weeks, all other groups were treated i.p. (1 ml per injection). The dose administered was 150 mg/kg based on pilot studies. The administered dose was given as: (a) one single dose, (b) once-weekly dose, or (c) alternate-day dose for 6 weeks. The 150 mg/kg three-times-weekly dose was selected as the most active schedule administrable for a prolonged period with no signs of toxicity. A control group receiving 1 ml of the vehicle (0.5% CMC) i.p. on alternate days was also included. At the end of the treatment period (6 weeks), animals were killed, and peritoneal and liver nodules were dissected out, counted and preserved for further examination.
Statistical analysis
All statistical analyses were done using Statistical Software version 3.0 (GraphPad Software, San Diego, Calif.), with P values <0.05 considered to be statistically significant. In vitro screening assays were tested using Student’s paired t-test. Tumor-associated parameters were tested for statistical significance using Student’s t-test or the Mann-Whitney U-test (non-parametric).
Results
Reversible inhibition of HT-29 cells by ABZ
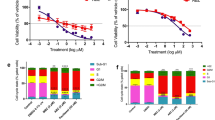
In vitro alternate-day treatment of HT-29 cells at various concentrations of ABZ led to dose-dependent inhibition of growth as measured by 3H-thymidine incorporation. The inhibitory effect of ABZ was highly significant (P=0.001) at the higher drug concentrations (Fig. 1a). Proliferation of cells treated with 1 and 10.0 μM concentrations of ABZ were over 90% inhibited. This shows the profound inhibitory effect of ABZ on HT-29 cell proliferation. Treatment of cells with medium containing various concentrations (0.01–10.0 μM) of ABZ-SO or ABZ-SO2, revealed that while ABZ-SO retains some of the parent antiproliferative activity, the sulfone metabolite was totally inactive. From these data, the IC50 value for ABZ-SO was calculated to be 2.35 μM compared to that of 0.12 μM for ABZ.
Dose-dependent growth inhibition of HT-29 cells in vitro by ABZ. a After treating cells in culture for 5 days with various concentrations of ABZ (0.001–10 μM), cell proliferation was measured by 3H-thymidine incorporation and the results are expressed as mean ± SEM counts per minute. Each concentration was tested in quadruplicate and each experiment was repeated at least twice. b Number of viable cells remaining 1, 3, or 5 days after treatment with ABZ (0.01–10 μM). Viable cells remaining were counted using the Trypan blue exclusion method. Values are the means ± SEM of cell numbers from two experiments. All counts were obtained in triplicate. c Resumption of cell proliferation following removal of the drug from the medium. Cells were initially treated for 3 days with various concentrations of ABZ (0–1 μM) followed by 3 days in drug-free medium
Similarly, in vitro treatment of HT-29 cells with various concentrations of ABZ revealed that inhibition of proliferation leading to a reduction in cell number was both time- and concentration-dependent (Fig. 1b). At the end of the treatment period, the 0.5 and 1 μM concentrations of ABZ had led to a significant reduction in the number of cells from the number originally seeded (P=0.001). These data confirm the time and dose dependency of the ABZ effect.
Cells treated with ABZ (single dose, 3 days) followed by medium alone (another 3 days) were able to overcome the inhibition and started to proliferate. As shown in Fig. 1c, cells exposed to various concentrations of ABZ were able to recover once the drug was removed from the medium. The recovery was almost complete in cells exposed to lower drug concentrations, whereas cells exposed to the higher ABZ concentrations, despite some recovery, were still highly suppressed at the end of the recovery period. These results indicate that the profound antiproliferative effect of ABZ is reversible.
ABZ induced cell cycle arrest
Flow cytometric analysis of ABZ-treated HT-29 cells revealed cell cycle arrest at the G2/M phase (Table 1 and Fig. 2). During the first 24 h, the percentage of cells in the G0/G1 phase declined from 81.1±0.5% to a mere 3.2±0.1%, while at the same time cells in the G2/M phase increased from 1.3±0.3% to 88.1±0.9%. Accompanying these changes was also a reduction in the percentage of cells residing in the S phase which was halved during the first 24 h of ABZ treatment. Also of interest were the apoptotic nuclei displaying decreased DNA content below the G1 peak paralleled by an increase in the side-scatter subdiploid cells indicative of cell death after mitotic arrest (Fig. 2). These observations in a human colorectal cancer cell line are consistent with early reports suggesting that the anthelmintic effect of BZs is mediated through interference with spindle formation leading to cell death after mitotic arrest [20, 21]. We now know that this effect results from arrest of cells in the G2/M phase of the cell cycle.
ABZ induced apoptosis
To confirm that the cell death was brought about by apoptosis, TUNEL, DNA laddering and caspase-3 activity assays were performed on ABZ-treated cells. As shown in Fig. 3, induction of apoptosis brought about by ABZ treatment was evident in the staining of cells by TUNEL (Fig. 3a–b), by the activation of endonucleases leading to the fragmentation (laddering) of the DNA (Fig. 3c) and by upregulation of caspase-3 (Fig. 3d), an intracellular cysteine protease mediator of apoptosis [22]. Consistent with induction of apoptosis, we observed an increase in the ability of cell lysates to cleave the caspase-3 substrate, when prepared from cells treated for 8, 24 or 48 h with ABZ. Caspase-3 has been shown to play an important role in triggering the apoptotic process [19].
Induction of apoptosis in HT-29 cells following treatment with 1 μM ABZ. a, b The TUNEL assay showed the presence of apoptotic (brown-stained) cells among cells treated for 5 days with vehicle (a) or ABZ (b). Cells were visualized after diaminobenzidine color development and counter-staining with methyl green. c Agarose gel electrophoresis demonstrates the ladder effect indicating DNA fragmentation following treatment with ABZ for 48 h (lane 1 molecular weight marker, lane 2 DNA from cells treated with medium only, lane 3 DNA from cells treated with ABZ). d Caspase-3 activity of HT-29 cells following 8, 24 or 48 h of treatment with vehicle only or ABZ (blank columns vehicle only treatment, filled columns ABZ treatment)
Inhibition of peritoneal tumor growth in nude mice
Following the in vitro results, ABZ was tested against HT-29 colorectal cells grown in the peritoneum of nude mice. One of the main targets of the study was to determine the effect of frequency of dosing upon response. Animals were dosed at a predetermined dose of 150 mg/kg, which was worked out from pilot studies. As shown in Fig. 4, at this dose level ABZ was highly effective (P=0.0005) in reducing tumor burden when given on alternate days, and effective as weekly or even as a single-dose treatment (P=0.0028 and P=0.0125, respectively). Inevitably, while the alternate-day dosing proved to be the most effective dosing schedule, results from the once-weekly and single-dose regimens were also quite impressive in reducing peritoneal tumor growth. The large intra-animal variation in the number of liver nodules seen in animals receiving the single-dose treatment schedule, resulted in it being not significantly different from control values (P=0.435). Interestingly, oral alternate-day treatment of animals for the entire period of experimentation (6 weeks) did not lead to significant prevention or reduction of peritoneal tumor growth (P=0.556). At least in the case of ABZ, this observation confirms the value of peritoneal over oral drug treatment in PC. Moreover, monitoring of nude mice under treatment with ABZ for 6 weeks showed no side effects arising from this treatment schedule.
Suppression of tumor growth by ABZ in nude mice bearing tumors. Animals inoculated with 106 HT-29 cells (i.p.) were treated with various schedules of ABZ (150 mg/kg, i.p.) ranging from a single dose, to weekly dosing and alternate-day dosing for 6 weeks. Another group was treated with ABZ at 150 mg/kg on alternate days orally for 6 weeks. The control group was treated with the vehicle (0.5% CMC) every other day. The upper graph shows the number of peritoneal tumor nodules and the lower graph the number of liver tumor nodules present in mice at the end of the treatment period. Ten mice were assigned to each group and the difference between treatment groups was tested using Student’s t-test and the Mann-Whitney U-test
Discussion
ABZ and other BZs were synthesized and marketed as anthelmintic drugs with a broad spectrum of activity and good safety profiles. The major focus in the development of these drugs has been solubility as these compounds are not easily dissolved in either aqueous or oily media. More than three decades after their first approval, BZs are still indicated and widely used for the treatment of helminths in humans and animals. In 1985 Lacey and Watson reported the activity of BZs against mouse L1210 leukemia cells [23]. Later in 1989, Rolin et al. [24] reported the metabolism of ABZ by human liver cancer cells HepG2 and its inhibitory effect on the growth of these cells. It was not until 1998 when, following running a thorough check of BZs as antiproliferative agents, we described the profound antitumor effect of ABZ [8, 9].
The intracavitary administration of high concentrations of anticancer agents to treat PC is backed by sound pharmacokinetic principles. Pharmacokinetic studies of the i.p. route of administration of anticancer agents demonstrate a protracted local concentration as compared to systemic levels [25]. In the distribution model proposed by Dedrick et al. [26, 27], delayed systemic distribution is predictable and dependent on drug diffusivity within the adjacent tissues within the peritoneal cavity and the rate of drug removal from tissue by capillary blood. This results in increased drug concentration in the vicinity of tumors, a longer duration of exposure of tumor cells to the drug which also facilitates the binding and uptake of the drug by these cells [28, 29]. However, there are major problems associated with the cytotoxic agents in current use. These agents are available as aqueous solutions, and are consequently easily absorbed through capillaries below the large serosal surface leading to rapid decline in peritoneal drug concentration, availability of drug in the systemic circulation and hence systemic toxicity.
Based on the pharmacokinetic principles, an ideal agent for use in the i.p. treatment of PC would therefore be one with a low absorption rate and high hepatic clearance, as low systemic drug concentrations are maintained by a rapid systemic metabolism or excretion [30, 31]. Consequently, prolonged exposure of tumor cells to the drug and low systemic bioavailability should ensure maximum antitumor effect with minimal or no systemic toxicity. With a low aqueous and lipid solubility together with high first-pass metabolism, ABZ fulfils both these criteria [32, 33]. Once absorbed, ABZ is very rapidly oxidized by liver microsomal flavin-containing monooxygenases (MFMO) and cytochrome P450 isozymes to sulfoxide, sulfone and a number of other metabolites with only trace amounts of the parent drug being detectable in all species studied [33–38]. The major metabolite formed, ABZ-SO has been recognized as an active metabolite contributing to the anthelmintic properties of the treatment [6, 39–43]. Our cell culture data revealed a comparatively weak antiproliferative effect for ABZ-SO. Preliminary results from our ongoing pharmacokinetic studies in the rabbit have shown that the systemic levels of ABZ-SO are several times higher in animals treated orally than in those receiving the drug at the same dose as an i.p. injection. This ties up very well with the data from nude mice where unlike the i.p. schedule, despite alternate-day dosing for 6 weeks, the oral schedule was totally ineffective in suppressing peritoneal tumor growth.
A profound reduction of tumor burden in animals receiving only a single dose of ABZ or the group being treated once weekly is a further indication of the prolonged residence of the drug within the peritoneum, leading to sustained concentrations and antitumor activity. Furthermore, cell culture proliferation studies revealed that the ABZ effect is a reversible one in that, the cells start to proliferate once the drug is removed from the cell culture medium. This shows that the mechanism by which ABZ inhibits tumor growth is a concentration-dependent reversible mechanism.
In general, BZs produce many biochemical changes. However, the primary mode of action of these drugs in susceptible nematodes has been described as the inhibition of microtubule polymerization by binding to β-tubulin [21, 44–46]. However, the tubulin-binding site of BZs is distinctly different from that of other microtubule-disrupting (vinca alkaloids, colchicine analogs) or stabilizing agents (taxanes). As yet there is no clear indication of the binding region for the BZs [47].
In addition to their involvement in a number of cellular functions, microtubules also play a key role in the formation of the mitotic spindles, disruption of which would lead to cell death.
Induction of apoptosis by ABZ, as confirmed by caspase-3 activation (an important executor of apoptosis), DNA laddering and TUNEL assay, was also clearly visible under the microscope in ABZ-treated cells prior to cytolysis. The mechanism by which apoptosis is induced by microtubule-disrupting agents is yet to be completely understood, consequently, involvement of other mechanisms cannot be ruled out. In fact, Sasaki et al. together with Mukhopadhyay et al. have recently confirmed mitotic arrest, mitochondrial cytochrome c release and inhibition of angiogenesis by mebendazole, another commonly used BZ anthelmintic drug [10, 11]. In summary, together these results provide strong support for the profound antitumor activity of some of the BZs. However, what the current study revealed for the first time, is evidence for the potential use of ABZ in the regional treatment of PC. Further pharmacological studies with ABZ (and perhaps other BZs) in the regional treatment of PC are warranted.
References
Jayne DG, Fook S, Loi C, Seow-Choen F (2002) Peritoneal carcinomatosis from colorectal cancer. Br J Surg 89:1545–1550
Sugarbaker PH, Graves T, DeBruijn EA, Cunliffe WJ, Mullins RE, Hull WE, Oliff L, Schlag P (1990) Early postoperative intraperitoneal chemotherapy as an adjuvant therapy to surgery for peritoneal carcinomatosis from gastrointestinal cancer: pharmacological studies. Cancer Res 50:5790–5794
Sticca RPMDF (2003) Peritoneal carcinomatosis: a final frontier (editorial). Ann Surg Oncol 10(5):484–485
Mohamed F, Stuart OA, Sugarbaker PH (2003) Pharmacokinetics and tissue distribution of intraperitoneal docetaxel with different carrier solutions. J Surg Res 113:114–120
De Silva N, Guyatt H, Bundy D (1997) Anthelmintics. A comparative review of their clinical pharmacology. Drugs 53:769–788
Morris DL, Dykes PW, Dickson B, Marriner SE, Bogan JA, Burrows FG (1983) Albendazole in hydatid disease. Br Med J Clin Res Ed 286:103–104
Morris DL (1983) Chemotherapy of hydatid disease. J Antimicrob Chemother 11:494–496
Pourgholami MH, Woon L, Almajd R, Akhter J, Bowery P, Morris DL (2001) In vitro and in vivo suppression of growth of hepatocellular carcinoma cells by albendazole. Cancer Lett 165:43–49
Morris DL, Jourdan JL, Pourgholami MH (2001) Pilot study of albendazole in patients with advanced malignancy. Effect on serum tumor markers/high incidence of neutropenia. Oncology 61:42–46
Mukhopadhyay T, Sasaki J, Ramesh R, Roth JA (2002) Mebendazole elicits a potent anti-tumor effect on human cancer cell lines both in vitro and in vivo. Clin Cancer Res 8:2963–2969
Sasaki J, Ramesh R, Chada S, Gomyo Y, Roth JA, Mukhopadhyay T (2002) The anthelmintic drug mebendazole induces mitotic arrest and apoptosis by depolymerizing tubulin in non-small cell lung cancer cells. Mol Cancer Ther 1:1201–1209
Marriner SE, Morris DL, Dickson B, Bogan JA (1986) Pharmacokinetics of albendazole in man. Eur J Clin Pharmacol 30:705–708
Edwards G, Breckenridge AM (1988) Clinical pharmacokinetics of anthelmintic drugs. Clin Pharmacokinet 15:67–93
Labarca C, Paigen K (1980) A simple, rapid, and sensitive DNA assay procedure. Anal Biochem 102:344–352
Macario AJ, Dugan C, Perez-Lloret IL, Conway de Macario E (1981) Purification of erythroblastic nests. Blood 57:922–927
Taylor IW (1980) A rapid single step staining technique for DNA analysis by flow microfluorimetry. J Histochem Cytochem 28:1021–1024
Gavrieli Y, Sherman Y, Ben-Sasson SA (1992) Identification of programmed cell death in situ via specific labeling of nuclear DNA fragmentation. J Cell Biol 119:493–501
Herrmann M, Lorenz HM, Voll R, Grunke M, Woith W, Kalden JR (1994) A rapid and simple method for the isolation of apoptotic DNA fragments. Nucleic Acids Res 22:5506–5507
Jung MY, Kwon SK, Moon A (2001) Chemopreventive allylthiopyridazine derivatives induce apoptosis in SK-Hep-1 hepatocarcinoma cells through a caspase-3-dependent mechanism. Eur J Cancer 37:2104–2110
Lacey E (1989) The role of the cytoskeletal protein, tubulin, in the mode of action and mechanism of drug resistance to benzimidazoles (erratum appears in Int J Parasitol, May; 19(3):359). Int J Parasitol 18:885–936
Lacey E (1990) Mode of action of benzimidazoles. Parasitol Today 6:112–115
Cohen GM (1997) Caspases: the executioners of apoptosis. Biochem J 326:1–16
Lacey E, Watson TR (1985) Activity of benzimidazole carbamates against L1210 mouse leukaemia cells: correlation with in vitro tubulin polymerization assay. Biochem Pharmacol 34:3603–3605
Rolin S, Souhaili-el Amri H, Batt AM, Levy M, Bagrel D, Siest G (1989) Study of the in vitro bioactivation of albendazole in human liver microsomes and hepatoma cell lines. Cell Biol Toxicol 5:1–14
De Lima Vazquez V, Stuart OA, Mohamed F, Sugarbaker PH (2003) Extent of parietal peritonectomy does not change intraperitoneal chemotherapy pharmacokinetics. Cancer Chemother Pharmacol 52:108–112
Flessner MF, Dedrick RL, Schultz JS (1984) A distributed model of peritoneal-plasma transport: theoretical considerations. Am J Physiol 246:R597–R607
Dedrick RL, Myers CE, Bungay PM, DeVita VT Jr (1978) Pharmacokinetic rationale for peritoneal drug administration in the treatment of ovarian cancer. Cancer Treat Rep 62:1–11
de Bree E, Witkamp AJ, Zoetmulder FA (2002) Intraperitoneal chemotherapy for colorectal cancer. J Surg Oncol 79:46–61
Markman M (2001) Intraperitoneal chemotherapy in the management of malignant disease. Expert Rev Anticancer Ther 1:142–148
Jacquet P, Sugarbaker PH (1996) Peritoneal-plasma barrier. Cancer Treat Res 82:53–63
Sugarbaker PH, Stuart OA, Vidal-Jove J, Pessagno AM, DeBruijn EA (1996) Pharmacokinetics of the peritoneal-plasma barrier after systemic mitomycin C administration. Cancer Treat Res 82:41–52
Theodorides VJ, Gyurik RJ, Kingsbury WD, Parish RC (1976) Anthelmintic activity of albendazole against liver flukes, tapeworms, lung and gastrointestinal roundworms. Experientia 32:702–703
Gottschall DW (1990) The metabolism of benzimidazole anthelmintics. Parasitol Today 6:115–124
Bogan JA, Marriner S (1980) Analysis of benzimidazoles in body fluids by high-performance liquid chromatography. J Pharm Sci 69:422–423
Marriner SE, Bogan JA (1980) Pharmacokinetics of albendazole in sheep. Am J Vet Res 41:1126–1129
Souhaili-El Amri H, Mothe O, Totis M, Masson C, Batt AM, Delatour P, Siest G (1988) Albendazole sulfonation by rat liver cytochrome P-450c. J Pharmacol Exp Ther 246:758–764
el Amri HS, Fargetton X, Delatour P, Batt AM (1987) Sulphoxidation of albendazole by the FAD-containing and cytochrome P-450 dependent mono-oxygenases from pig liver microsomes. Xenobiotica 17:1159–1168
Rossignol JF, Maisonneuve H (1984) Albendazole: a new concept in the control of intestinal helminthiasis. Gastroenterol Clin Biol 8:569–576
McCormick D, Chong H, Hobbs C, Datta C, Hall PA (1993) Detection of the Ki-67 antigen in fixed and wax-embedded sections with the monoclonal antibody MIB1. Histopathology 22:355–360
Morris DL, Chinnery JB, Ubhi C (1987) A comparison of the effects of albendazole, its sulphone metabolite, and mebendazole on the viability of protoscoleces of Echinococcus granulosus in an in vitro culture system. Trans R Soc Trop Med Hyg 81:804–806
Morris DL, Taylor D (1986) Sensitivity to albendazole sulphoxide of Echinococcus granulosus scoleces in man. Lancet 2:1035
Chinnery JB, Morris DL (1986) Effect of albendazole sulphoxide on viability of hydatid protoscoleces in vitro. Trans R Soc Trop Med Hyg 80:815–817
Souhaili-El Amri H, Fargetton X, Delatour P, Batt AM (1987) Sulphoxidation of albendazole by the FAD-containing and cytochrome P-450 dependent mono-oxygenases from pig liver microsomes. Xenobiotica 17:1159–1168
Barrowman MM, Marriner SE, Bogan JA (1984) The binding and subsequent inhibition of tubulin polymerization in Ascaris suum (in vitro) by benzimidazole anthelmintics. Biochem Pharmacol 33:3037–3040
Lacey E, Watson TR (1985) Structure-activity relationships of benzimidazole carbamates as inhibitors of mammalian tubulin, in vitro. Biochem Pharmacol 34:1073–1077
Martin RJ (1997) Modes of action of anthelmintic drugs (comment). Vet J 154:11–34
Downing KH (2000) Structural basis for the interaction of tubulin with proteins and drugs that affect microtubule dynamics. Annu Rev Cell Dev Biol 16:89–111
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pourgholami, M.H., Akhter, J., Wang, L. et al. Antitumor activity of albendazole against the human colorectal cancer cell line HT-29: in vitro and in a xenograft model of peritoneal carcinomatosis. Cancer Chemother Pharmacol 55, 425–432 (2005). https://doi.org/10.1007/s00280-004-0927-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00280-004-0927-6