Abstract
Acute promyelocytic leukemia (APL) cells constitutively express a large amount of tissue factor (TF) antigen, most of which is present in the cytoplasm. Coagulopathy may persist after induction therapy. We evaluated the overall role of circulating microparticles (MPs) in coagulation activation in APL-associated coagulopathy before and during induction therapy. Eleven adult patients with ≥ World Health Organization’s (WHO) grade 2 bleeding events and 11 sex- and age-matched healthy controls were selected. All patients received arsenic trioxide alone as induction therapy. MP-associated TF (MP-TF) activity and MP procoagulant activity (MP-PCA) and 12 coagulation- and anticoagulation-associated indexes were measured before, during, and after induction therapy. Correlation between MP-associated indexes and the other 12 indexes was analyzed in patients. The MP-TF activity was negligible in controls, whereas it markedly increased in patients, dropped rapidly after treatment, and returned to normal at the end of induction therapy. The MP-PCA was similar between patients and controls. The correlation analysis revealed that TF-bearing MPs in patients mainly originated from APL cells. Partially differentiated APL cells could also release TF-bearing MPs, and the higher the degree of APL cell differentiation, the lower the ability of APL cells to release TF-bearing MPs. MP-TF was the main source of active TF in plasma and an important contributor for the coagulation activation in APL-associated coagulopathy. It was MPs released by APL cells/partially differentiated APL cells that served as the vehicle to transfer the large amount of TF to plasma to activate coagulation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Catastrophic hemorrhage remains the leading cause of early death in acute promyelocytic leukemia (APL) and is the major cause of APL treatment failure. Remission induction therapy with all-trans retinoic acid (ATRA) and/or arsenic trioxide (ATO) has been accompanied by rapid resolution of clinical bleeding, but elevated plasma levels of sensitive markers of clotting activation may persist beyond the cessation of clinical bleeding [1].
The pathophysiology of APL-associated coagulopathy is a complex process and remains unclear in many aspects [2, 3]. It is currently believed that primary hyperfibrinolysis is probably the most important mechanism behind the APL-associated coagulopathy, which may be induced by abnormal expression and/or activity of urokinase and tissue plasminogen activator (uPA and tPA), their inhibitors plasminogen activator inhibitor 1 (PAI-1) and plasminogen activator inhibitor 2 (PAI-2), or their receptors such as urokinase plasminogen activator receptor (u-PAR) and annexin II [4,5,6]. Another main mechanism behind the disease is tissue factor (TF)–induced disseminated intravascular coagulation (DIC) [7, 8]. Other factors include the endothelial activation and damage induced by proteases and cytokines released by APL cells which convert the endothelium to a procoagulant state [9,10,11,12]. Additionally, an interesting mechanism involved in APL-associated coagulopathy is ETosis, which, releasing extracellular chromatin into the extracellular space, induces activation of coagulation, hyperfibrinolysis, and endothelium damage [13]. More recently, the podoplanin gene was found to be highly expressed on APL cells leading to aberrant platelet binding, activation, and aggregation [14].
A number of studies showed that APL cells constitutively express a large amount of TF antigen [15,16,17], which is the trigger of the extrinsic coagulation cascade. Most TF expressed by APL cells is present in the cytoplasm [16] and needs to be transferred to plasma to activate coagulation. Because having innate phosphatidylserine (PS) procoagulant activity and being capable of carrying active TF on its surface, microparticle (MP) has been widely described in the setting of thromboembolic diseases. Increased levels of TF-bearing microparticles have been described in patients with APL [18]. However, to our knowledge, only two studies have explored the role of MPs in the pathogenesis of APL-associated coagulopathy. In one study, relevant tests were performed only on cell lines [19], while in the other study, only preliminary tests were performed on circulating APL cells [20]. It remains unknown how much roles MPs, especially TF-carrying MPs (TF-MPs), play in coagulation activation in APL-associated coagulopathy.
In this study, after detecting related coagulation parameters and using the statistical method of correlation analysis, we evaluated the overall role of circulating MPs in coagulation activation in APL-associated coagulopathy before and during induction therapy.
Materials and methods
Patients and controls
This is a prospective study on patients with APL-associated coagulopathy who were admitted to our hospital between June 2016 and May 2017. All patients were more than 18 years old; had ≥World Health Organization’s (WHO) grade 2 bleeding events [21] at the time of diagnosis; did not receive any APL-related treatment prior to admission; and were treated with ATO alone as remission induction. Patients were excluded if they died during induction therapy.
Totally 11 patients were selected (10 with newly diagnosed APL and one in the first hematological relapse; 6 men and 5 women; median age 42 years, range 28 to 64 years). The diagnosis was confirmed by the presence of t(15;17) and/or the PML/RARα fusion gene. The total daily dose of ATO (0.16 mg/kg/day for a maximum of 10 mg/day) was infused until visible leukemic blasts and promyelocytes were eliminated from the bone marrow and the blast and promyelocyte counts were no more than 5% of marrow mononuclear cells. For the management of coagulopathy, fresh frozen plasma, platelet (PLT) concentrates, cryoprecipitate, or/and fibrinogen (FIB) were transfused to replenish coagulation factors, maintain target PLT counts >30×109/L, and target FIB levels >1.5 g/L.
Eleven sex- and age-matched healthy volunteers were selected as controls. All healthy controls should have no liver diseases, cardiovascular diseases, or diabetes and for at least 1 month have not taken antiplatelet agents, anticoagulants, and non-steroidal anti-inflammatory drugs (NSAIDs) which could affect the PLT function and coagulation.
The study protocol was reviewed and approved by the hospital’s Medical Ethics Committee, and all patients and controls gave written informed consent. This trial was registered at www.clinicaltrials.gov as#NCT02991066.
Blood collection and processing
Fasting venous blood was collected from each patient at time points of baseline (T0); days 7 (T1), 14 (T2), and 21 (T3) of ATO treatment; at the end of induction therapy (EIT or T4); and 4 weeks after EIT (EIT+4w or T5). At 2–3 of the 6 time points, blood samples were simultaneously drawn from the pair-matched healthy control. The collected blood samples were mixed 9:1 (v/v) with 3.2% sodium citrate. An aliquot of 2 ml of blood samples collected at each time was directly sent to the clinical laboratory for routine coagulation tests, and the remainders were processed as follows within 1 h. Blood samples were centrifuged for 15 min at 1500 × g, 20°C, to obtain platelet-poor plasma and then centrifuged for 2 min at 13,000 × g, 20°C, to obtain platelet-free plasma (PFP). The PFP was aliquoted and frozen at −80°C until used.
To prepare normal human platelet-free plasma (NHP), blood was collected from a healthy volunteer after informed consent was obtained. The NHP was aliquoted and stored at −80°C until used in the MP procoagulant activity (MP-PCA) assay.
Routine coagulation tests
Using fresh blood samples, prothrombin time (PT), activated partial thromboplastin time (APTT), FIB levels, FIB/fibrin degradation product (FDP), D-dimer (DD), and anti-thrombin 3 (AT3) activity level (all kits from Siemens, Germany) were measured on a Sysmex CA7000 analyzer (Sysmex, Japan).
Enzyme-linked immunosorbent assay (ELISA)
All the ELISA tests were performed using frozen-thawed PFP. The PFP samples were 6-fold diluted for measuring thrombomodulin (TM) level and were 100-fold diluted for detecting free tissue factor pathway inhibitor (TFPI) (both kits from R&D Systems, USA). The PFP samples were directly used to detect thrombin-antithrombin (TAT) (Dade Behring, Germany) and TF antigen levels (R&D Systems, USA). The experiments were done according to the manufacturer’s instructions.
Isolation of plasma MPs
All deionized water used as solvent to prepare a solution in MP-associated experiments was filtered through a 0.1-μm-pore size filter (SLVV033RS, EMD Millipore, Billerica, MA). Frozen-thawed PFP samples were diluted in phosphate-buffered saline (PBS, pH 7.40) and centrifuged for 90 min at 20,000 × g, 4°C. The MP pellets were then washed once with PBS. The resultant MP pellets were used for the following experiments.
Detection of MPs by laser scanning confocal microscopy
MP suspensions were spotted on poly-L-lysine (Sigma, USA)-coated glass slides overnight at 4°C. Glass slides were washed three times with 50 μl of binding buffer. MPs were simultaneously stained with CD142-AF488 (US Biological, USA) and annexin V-Cy3 (Sigma, USA) in 50 μl of binding buffer (Sigma, USA) for 20 min at room temperature in the dark. Glass slides were washed three times with 50 μl of binding buffer. Then, MPs were visualized using a Zeiss LSM 510 Meta confocal microscope (Carl Zeiss, Germany).
Circulating MP-associated TF (MP-TF) activity assay
The MP-TF activity was evaluated by TF-dependent FXa generation assay. MPs were isolated from stored PFP as described above except that samples were washed with HBSA (137-mM NaCl, 5.38-mM KCl, 5.55-mM glucose, 10-mM HEPES, 0.1% BSA, pH 7.50) instead of PBS. The MP-TF activity was measured with a chromogenic assay that quantifies the MP-TF-dependent FXa generation. The MP pellets were re-suspended in HBSA by thoroughly vortexing. Fifty μl of MP suspension pelleted from 100 μl of PFP was incubated with 8 μl of either a mouse against human CD142 monoclonal antibody (anti-HTF1, final concentration, 10 μg/ml; BD, USA) or an isotype-matched control antibody (mouse IgG; BD, USA) for 20 min at 25°C. A previously described two-stage chromogenic assay [22] was employed with the following modifications: (1) 50-μl aliquots were incubated for 2 h with 50 μl of mixture containing 10 μl of 50 nM FVIIa, 20 μl of 750 nM FX, and 20 μl of 25 mM CaCl2; (2) absorbance measurements were made every 20 s for 120 min after adding 25 μl of 25-mM EDTA and 25 μl of 4-mM chromogenic substrate S-2765 (Chromogenix, Italy). To convert the slope of resulting absorbance curve to the amount of FXa generation, a reference curve was prepared using purified human FXa (all human coagulation factors purchased from Enzyme Research Laboratories, USA). The amount of TF-dependent FXa generation (nM), which represents the MP-TF activity, was determined by subtracting the amount of FXa generated in the presence of anti-HTF1 from the amount of FXa generated in the presence of the control antibody.
Circulating MP-PCA assay
The MP-PCA in the intrinsic coagulation system was measured by plasma recalcification time (RT) assay. Briefly, 50 μl of MP suspension pelleted from 50 μl of PFP was mixed with 30 μl of NHP at 37°C, and the assay was initiated by adding 40 μl of 50-mM CaCl2 solution. Plasma fibrin polymerization was monitored by the change in turbidity at 405 nm (A405) every 20 s, for at least 1.5 h at 37°C using a SpectraMax M5 microplate reader (Molecular Devices, USA). RT was the time to the inflection point prior to the turbidity increase.
MP-PCA inhibition assays with anti-TF antibody were also performed. Forty-five μl of MP suspension pelleted from 50 μl of PFP was incubated with 5 μl of either anti-HTF1 (final concentration of 50 μg/ml; BD, USA) or an isotype-matched control antibody (mouse IgG; BD, USA) for 20 min at 25°C. Then, the MP-PCA was measured.
Statistical analysis
For each healthy control, data were from two or three different time points, and means were used to decrease within-group variation. Data are presented as median (range). At each time point, the difference in each index between the patients and controls was analyzed using the Wilcoxon signed rank test. In patients, relationships between indexes were analyzed by Spearman’s correlation test on baseline data (T0 data) and on all data from T0 to T5 (6T data), respectively. The correlation coefficients (ρ) indicate the relative reliability and are interpreted using the following criteria: ρ≥0.7 specifies a high correlation, 0.7>ρ≥0.4 represents moderate correlation, and ρ<0.4 is a low correlation.
The SPSS 19.0 software was used. A P value less than 0.05 was considered statistically significant except for the correlation test on 6T data, where relationship between indexes also included correlation between repeated measures, i.e., within-individual association; thus a P value less than 0.01 was arbitrarily considered statistically significant.
Results
Hemorrhagic manifestations and treatment effects in patients
In 11 patients, mucocutaneous hemorrhage (100%), including petechiae, ecchymoses, and bleeding gums, was the most frequently observed hemorrhagic manifestation, and hemorrhage at the trauma site (e.g., vein puncture site) was also common. One patient presented with hematuria at diagnosis, three patients exhibited retinal hemorrhage or sclera hemorrhage, and one patient showed a small amount of cerebral hemorrhage during treatment. No thrombotic complications were noted in any patient. In all patients, the hemorrhagic symptoms were most severe in the first week of treatment and then obviously improved; the hemorrhagic symptoms disappeared within the first, second, third, and fourth week of treatment in four cases, three cases, three cases, and one case, respectively. In one patient, active bleeding had stopped within the first week of treatment, whereas bleeding symptoms reappeared during the third week.
The median duration of induction therapy in the 11 patients was 30 days (24–35 days).
Coagulation profile in patients
The location of the coagulation parameters, tested in this study, in coagulation-fibrinolysis pathways and the test results are shown in Figs. 1 and 2. The white blood cell (WBC) count was markedly reduced in 7 patients whereas notably increased in 4 cases at admission (median, 2.04×109/L; range, 0.65–68.99×109/L) with a median APL cell count of 0.37×109/L (0–60.71×109/L). Upon ATO induction, the WBC count increased, reaching a peak at T2 (significantly higher than normal level). Thereafter, the WBC count decreased rapidly, reaching a minimum at EIT (significantly lower than normal level), and was restored to normal only in some patients at EIT+4w (Fig. 2a). The PLT count was remarkably reduced at admission and gradually recovered with treatment, returning to normal at EIT (Fig. 2b).
The profile of abnormal activation of coagulation-fibrinolysis pathways in acute promyelocytic leukemia (APL)–associated coagulopathy. Red indicates extrinsic coagulation pathway and relevant parameters detected in this study; green indicates intrinsic coagulation pathway and relevant parameters detected in this study; gray indicates anticoagulant system and relevant parameters detected in this study; purple indicates fibrinolytic system and relevant parameters detected in this study. ↑ increased, ↓ decreased, ↔ no change. It can be seen that the extrinsic coagulation, anticoagulant, and fibrinolytic systems are all activated except the intrinsic coagulation system
The changing trends in routine laboratory tests and plasma levels of anticoagulants during induction therapy in patients with acute promyelocytic leukemia, a white blood cell (WBC) count, b platelet (PLT) count, c prothrombin time (PT), d activated partial thromboplastin time (APTT), e fibrinogen (FIB), f D-dimer (DD), g FIB/fibrin degradation product (FDP), h thrombin-antithrombin (TAT), i anti-thrombin 3 (AT3), j thrombomodulin (TM), k tissue factor pathway inhibitor (TFPI), l tissue factor (TF). Data plotted are the results from 11 patients and matched healthy controls and are displayed as median with interquartile range. The horizontal gray lines represent the normal reference ranges. * denotes P<0.05 when compared with healthy controls
PT was significantly longer before and during treatment (Fig. 2c), whereas APTT was not longer before treatment and only slightly longer after treatment in patients than in controls, with the longest time at T3 (P=0.013 vs. control, Fig. 2d). Plasma FIB levels decreased significantly at admission (P=0.006 vs. control), returned to normal at T1, and exceeded the levels in controls at T3 and EIT (P=0.037 and 0.016, respectively) (Fig. 2e). The plasma levels of DD, FDP, and TAT in APL patients were dramatically increased at admission and notably decreased after treatment but remained significantly higher than in controls at EIT, as shown in Fig. 2f, g, and h.
TAT is a sensitive marker of thrombin formation, and DD levels reflect fibrinolysis, while FDP reflects not only fibrinolysis but also fibrinogenolysis (Fig. 1). None of PT, APTT, DD, FDP, and TAT levels returned to normal until EIT+4w. DD, FDP, and TAT levels all improved rapidly after a week of treatment except for PT, which almost did not improve during induction therapy.
Although plasma TAT levels in APL patients were significantly increased, AT3 levels showed no substantial decrease before and during ATO induction (Fig. 2i). TM and TFPI levels were abnormally increased in APL patients upon admission but were restored to normal at T2 and EIT, respectively (Fig. 2j and k).
Compared with controls, PFP-TF levels in patients (Fig. 2l) were abnormally elevated at admission and T1 (P=0.008 and 0.016, respectively) and restored to normal thereafter.
MP-TF activity was markedly increased in patients
TF-MPs were observed via laser scanning confocal microscopy. At T0 and T1, a large amount of TF-MPs was present in the plasma of patients (Fig. 3a, b, c), while TF-MPs were absent in the plasma of healthy controls.
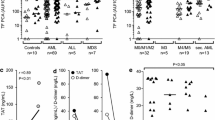
The changing trends in circulating microparticle (MP)-associated tissue factor (TF) activity (MP-TF activity) and MP-procoagulant activity (MP-PCA) during induction therapy in patients with acute promyelocytic leukemia. a–c Representative confocal microscopy images of circulating MPs obtained from patients before treatment. MPs were observed using an oil objective (×100). The scale bar is 1 μm in size. a Circulating MPs were captured using Cy3-labeled annexin V; b Circulating MPs were detected using AF488-labeled anti-TF antibody; c the pictures of MPs and TF were merged. d The MP-TF activity was measured with a chromogenic assay that quantifies the MP-TF-dependent FXa generation. e The MP-PCA was measured with plasma recalcification time (RT) assay. MP suspension pelleted from platelet-free plasma (PFP) was mixed with normal human platelet-free plasma (NHP), and then plasma RT assay was performed. The horizontal gray line represents the average value for the negative controls where phosphate-buffered saline (PBS) was mixed with NHP for the plasma RT assay. d, e Data plotted are the results from 11 patients and matched healthy controls and are displayed as median with interquartile range. * denotes P<0.05 when compared with healthy controls
The MP-TF activity assay (Fig. 3d) indicated that there was negligible MP-TF activity in controls (0.117±0.105 nM). The MP-TF activity of APL patients was markedly increased at admission (median, 2.08 nM; range, 0–24 nM, P=0.008 vs. control). Upon ATO induction, the MP-TF activity dropped rapidly but remained significantly higher than that of controls at T1–T3 (P=0.012, 0.006, and 0.013, respectively) and returned to normal at EIT (P>0.05 vs. control).
No significant changes were observed in MP-PCA in the intrinsic coagulation system in patients
RT method was used to measure MP-PCA in the intrinsic coagulation system. MP-RT did not significantly differ between patients and controls except at T3 (longer in patients than in controls, P=0.011; Fig. 3e).
MP-PCA inhibition assays were performed with anti-TF antibody in 5 patients with relatively high MP-TF activity. The results showed that anti-TF antibody remarkably prolonged the MP-plasma RT in patients, and the effect was the most at T0 (P=0.043), followed by T1 (P=0.043), and the effect was no longer obvious thereafter. Anti-TF antibody had no effect on the MP-plasma RT in healthy controls. It indicated that MP-TF (active TF) also had an effect on MP-plasma RT.
Correlation analyses revealed that TF-MPs played a key role in linking APL cells with coagulation activation
Correlation between MP-associated indexes and other indexes in patients was analyzed on the T0 and 6T data, respectively (see supplementary Table S1). A significant correlation only indicates that two indexes are correlated but does not mean causality. But based on the information provided by Fig. 1, causality was inferred between some of the significant correlations. To visually show the relationship between indexes, we extracted the significant correlations from the T0 and 6T data, respectively, and assigned causality to some pairs of correlated indexes and then got the T0 and 6T MP regulatory networks (Fig. 4) associated with coagulation activation in APL-associated coagulopathy.
Microparticle (MP)-associated regulatory networks linked to acute promyelocytic leukemia (APL)-associated coagulopathy. MP-associated indexes, including MP-procoagulant activity (MP-PCA) and MP-associated tissue factor activity and 12 coagulation- and anticoagulation-associated indexes were tested before (T0), during (4 time points), and after (one time point) induction therapy in patients with APL. Correlation between two kinds of indexes was analyzed in patients on the T0 and 6T (all time points) data, respectively. Then causality between significant correlations was inferred based on the information provided by Fig. 1. Significant correlations were extracted, and inferred causality was assigned to them; then the MP regulatory networks were constructed, named network T0 (A) and network 6T (B), respectively. The T0 network reveals regulatory relationships that are more directly related to the occurrence of disease, while the 6T network could reveal some regulatory relationships that are not apparent in the T0 network because at T0; evident changes occurred in both coagulation and anticoagulation systems. Simultaneous changes in numerous influencing factors may mask some correlations between indexes. In the T0 data, a P value less than 0.05 was considered statistically significant. In the 6T data, relationship between indexes also included correlation between repeated measures, i.e., within-individual association; thus a P value less than 0.01 was arbitrarily considered statistically significant. Figures were produced using Cytoscape 3.6.1; boxes indicate MP-associated indexes; circles indicate coagulation- and anticoagulation-associated indexes; solid lines indicate positive correlations; dotted lines indicate negative correlations, and single-headed arrows indicate causality
In the T0 time point, MP-TF activity was highly positively correlated with APL cell count (ρ=0.855, P=0.001), but not with lymphocyte count and monocyte count (both P>0.05). MP-TF activity was highly positively correlated with WBC count at T1, T2, and T3 (ρ=0.714, P=0.047; ρ=0.709, P=0.015; and ρ=0.764, P=0.006, respectively) and was not correlated at T4 and T5.
In the T0 network, PT was moderately correlated with MP-TF activity (ρ=0.656, P=0.028), suggesting that MP-TF was an important contributor for the activation of the extrinsic coagulation pathway in APL. TAT level was significantly correlated with MP-TF activity (T0, ρ=0.645, P=0.032; 6T, ρ=0.645, P<0.001, respectively), suggesting that MP-TF was always an important contributor for thrombin formation before and during induction therapy. In the 6T network, DD and FDP levels (ρ=0.597, P<0.001, and ρ=0.566, P<0.001, respectively) were moderately correlated with MP-TF activity, suggesting that MP-TF was an important contributor to fibrinolysis in APL. However, in the T0 network, DD/FDP level was not correlated with MP-TF activity. This may be because intense primary fibrinolytic activity at T0 masked the correlations between DD/FDP and MP-TF activity.
TM level was significantly correlated with MP-TF activity (T0, ρ=0.764, P=0.006; 6T, ρ=0.493, P<0.001), suggesting that MP-TF could promote the release of TM from endothelial cells. In the 6T network, PLT count (ρ=−0.360, P=0.004), FIB level (ρ=−0.363, P=0.004), and TFPI level (ρ=0.391, P=0.002) were significantly correlated with MP-TF activity, indicating that the MP-TF could promote the consumption of platelets and FIB and the release of TFPI from endothelial cells. But these correlations were not found in the T0 network.
In APL, MP-PCA was positively correlated with PFP-TF levels (T0, ρ=0.733, P=0.010; 6T, ρ=0.337, P=0.006). PFP-TF levels mainly reflect the levels of soluble TF in plasma, most of which had no activity of initiating coagulation. It was inferred that soluble TF could affect the PCA of MPs; its level could have a direct or indirect effect on PS expression or binding of coagulation factors to the surface of MPs. MP-PCA was negatively correlated with FIB levels (T0, ρ=−0.687, P=0.020; 6T, ρ=−0.581, P<0.001), whereas the causal relationship could not be inferred.
Totally, it can be seen from Fig. 4 that MP-TF played far greater roles than MP-PCA in coagulation activation in APL-associated coagulopathy.
Discussion
In this study, we used a new research strategy to explore the overall role of circulating MPs in coagulation activation in APL-associated coagulopathy. First, we tested MP-associated indexes and as many coagulation- and anticoagulation-associated indexes as possible in patients. Then, we analyzed correlations between the two types of indexes. Finally, based on these results and background knowledge on coagulation-fibrinolysis pathways, we constructed MP regulatory networks associated with coagulation activation in APL-related coagulopathy. The regulatory relationships among some indexes are seldom shown up in healthy controls due to the small variations in these indexes, whereas in specific diseases or during specific therapeutic processes, significant changes occurred in specific indexes. Then, disease- or therapeutic process–specific regulatory relationships can be displayed due to the increased variation in these specific indexes. For studying the role of circulating MPs before and during induction therapy, analysis of correlation between indexes was performed on both the T0 and 6T data sets. The T0 network could reveal regulatory relationships that were more directly related to the occurrence of disease, while the 6T network could reveal some regulatory relationships during induction therapy.
Totally 12 coagulation- and anticoagulation-associated indexes, involving blood cell counts, routine coagulation tests, and plasma levels of natural anticoagulants (Fig. 1), were monitored in APL patients before, during, and after ATO induction treatment. Consistent with obvious bleeding manifestations, large amounts of thrombin were generated (as shown by TAT levels) via the extrinsic pathway (PT was prolonged whereas APTT was not) in patients upon admission (Fig. 1); after treatment, the clinical bleeding resolved quickly coincident with a rapid decrease in thrombin formation in patients; but there is still generated a small amount of thrombin at EIT. Patients were in persistent hypocoagulable state (PT prolongation) throughout the course of treatment, which did not match with the changes in severity of clinical bleeding and in level of coagulation activation (shown by TAT level) during induction therapy. Coagulation factor activities were also measured in patients (data are not shown), and the results indicated that the changing trend in PT was highly consistent with that in FVII activities, which also significantly decreased throughout the induction period. The results suggested that the continuous prolongation of PT may be due to slow synthesis of FVII in the liver instead of constant existence of large amounts of active TF. A new discovery is that the intrinsic pathway was mildly activated after treatment, which may be due to the release of chromatin from APL cells undergoing ETosis after treatment [13]. The changes in levels of natural anticoagulants, TM and TFPI, in APL patients suggested that the anticoagulation system was also activated following the activation of coagulation system (Fig. 1).
In addition, to express PCA mediated by MP-TF under some pathological conditions, MPs also express PCA mediated by PS exposed on their surface and maybe also by some other coagulation factors binding on their surface, at both pathological and physiological conditions. This study explored the roles of both the MP-TF activity in activating the extrinsic coagulation cascade and MP-PCA in the intrinsic coagulation system in APL-associated coagulopathy. The MP-TF activity was significantly increased in patients. The plasma RT assay, which is usually a measure of the intrinsic coagulation function, was selected to measure MP-PCA in the intrinsic coagulation system, and the results revealed that there was no significant difference in MP-PCA between patients and controls. Plasma RT mainly reflects intrinsic coagulation function, whereas the MP-PCA inhibition assay indicated that MP-TF also had a small effect on MP-plasma RT.
Finally, the overall roles of MP-TF activity in coagulation activation in APL-associated coagulopathy before and during induction therapy were analyzed by correlation method in the patients. The results indicated that MP-TF activity was highly positively correlated with APL cell count, but not with lymphocyte count and monocyte count, suggesting that TF-MPs mainly originated from APL cells. With the ATO treatment, APL cells were induced to differentiate. It is unknown whether partially differentiated APL cells can release TF-MPs. To find the answer, we first evaluated the share of partially differentiated APL cells in WBCs in the peripheral blood by fluorescence in situ hybridization (FISH) assay, and the results revealed that cells bearing PML/RARα fusion gene accounted for more than 80% of total WBCs from T1 to T3, and there remained many at EIT (data are not shown). So from T1 to T3 time points, WBC count could well reflect partially differentiated APL cell count in the peripheral blood. In addition, APL cells with different differentiation degrees may have different abilities to release TF-MPs. We assessed the differentiation degrees of cells by peripheral blood smear examination, and the results indicated that the differentiation degrees of APL cells were gradually increased from T0 to T4 (data are not shown). So, the correlation analyses between MP-TF activity and WBC count were carried out on data at each time point rather than 6T data. The results indicated that MP-TF activity was highly positively correlated with WBC count at T1 and T2 time points, suggesting that partially differentiated APL cells were also capable of releasing TF-MPs. From T0 to T2, WBC count increased rapidly, whereas MP-TF activity decreased quickly, suggesting higher degrees of APL cell differentiation corresponded to a weaker ability to release TF-MPs. At T3, MP-TF activity already dropped to very low levels, whereas it remained highly correlated with WBC count, suggesting that the partially differentiated APL cells were still capable of releasing a small number of TF-MPs at this time point. MP-TF activity was not correlated with WBC count at T4 and T5 time points, when cells bearing PML/RARα fusion gene accounted for only a small proportion of WBCs, or even disappeared from peripheral blood, and MP-TF activity also dropped to an extreme low level.
From the T0 and 6T MP regulatory networks (Fig. 4), it could be seen that MP-TF activity rather than MP-PCA played a key role in linking APL cells with coagulation activation in APL-associated coagulopathy before and during induction therapy. The roles of TF-MPs played in APL-associated coagulopathy are shown in Fig. 5. The circulating TF-MPs in APL patients mainly originated from APL cells. Partially differentiated APL cells could also release TF-MPs, but as the degree of differentiation of APL cells increased, their ability to release TF-MPs decreased. The MP-TF derived from APL cells/partially differentiated APL cells was the main source of active TF in plasma, although it was probably not the only source. Apoptotic APL cell/partially differentiated APL cell should be another source of active TF. Although the procoagulant activity of TF on the cell surface is mostly dormant, the exteriorization of PS during apoptosis enables its activation [23]. As the main source of active TF in plasma, MP-TF was an important contributor for coagulation activation in APL-associated coagulopathy. So, it was MPs released by APL cells/partially differentiated APL cells that served as the vehicle to transfer the large amount of TF inside cells to plasma to activate coagulation, ultimately causing the occurrence of coagulopathy. The correlation analysis also found that the increased MP-TF activity stimulated the release of anticoagulants, TM and TFPI, into the blood and resulted in an increase in fibrinolytic degradation products. Obviously, these effects were indirect rather than direct (Fig. 1).
The simplified schema of the roles of tissue factor (TF)–bearing microparticles (MP) played in acute promyelocytic leukemia (APL)–associated coagulopathy. APL cells constitutively express a large amount of TF antigen, most of which is present in the cytoplasm. Both APL cells and partially differentiated APL cells can release TF-bearing MPs, but the ability of APL cells to release TF-bearing MPs decreases with the increase of the differentiation degree of APL cells. The MP-associated TF derived from APL cells/partially differentiated APL cells is the main source of active TF, although it is probably not the only source. As the main source of active TF, MP-associated TF is an important contributor for coagulation activation in APL-associated coagulopathy. So, it is MPs released by APL cells that serve as the vehicle to transfer the large amount of TF inside APL cells to plasma to activate coagulation, ultimately causing the occurrence of coagulopathy
The limitations of this study include the relatively small number of cases, which was mainly due to low incidence of the disease and the extreme difficulty in blood collection. In fact, from a statistical perspective, no definitive standard is available regarding the number of cases required for such a study. Too small sample size introduces the risk of producing false-negative results (called type II error in statistics), whereas in this study, only patients with severe hemorrhagic events before treatment were included; what’s more, case-control study method was adopted, both of which can to some extent make up for the shortage of insufficient sample size. Many positive results were obtained from this study that proved the effectiveness of this design strategy.
Conclusions
MP-TF activity played a key role in coagulation activation in APL-associated coagulopathy before and during induction therapy. The circulating MP-TF that mainly originated from APL cells/partially differentiated APL cells was the main source of active TF in plasma. So, it was MPs released by APL cells/partially differentiated APL cells that served as the vehicle to transfer the large amount of TF inside cells to plasma to activate coagulation, ultimately causing the occurrence of coagulopathy.
References
Zhao W, Wang H, Wang X, Wu F, Guo W, Qu B, Shen Z, Wang Z (2001) Effects of all-trans-retinoic acid and arsenic trioxide on the hemostatic disturbance associated with acute promyelocytic leukemia. Thromb Res 102(3):197–204. https://doi.org/10.1016/s0049-3848(01)00233-x
Kwaan HC, Weiss I, Tallman MS (2019) The role of abnormal hemostasis and fibrinolysis in morbidity and mortality of acute promyelocytic leukemia. Semin Thromb Hemost 45:612–621. https://doi.org/10.1055/s-0039-1693478
Sanz MA, Montesinos P (2020) Advances in the management of coagulopathy in acute promyelocytic leukemia. Thromb Res 191(Suppl 1):S63–S67. https://doi.org/10.1016/S0049-3848(20)30399-6
Mantha S, Tallman MS, Soff GA (2016) What’s new in the pathogenesis of the coagulopathy in acute promyelocytic leukemia? Curr Opin Hematol 23(2):121–126. https://doi.org/10.1097/MOH.0000000000000221
David S, Mathews V (2018) Mechanisms and management of coagulopathy in acute promyelocytic leukemia. Thromb Res 164(Suppl 1):S82–S88. https://doi.org/10.1016/j.thromres.2018.01.041
Kwaan HC, Cull EH (2014) The coagulopathy in acute promyelocytic leukaemia--what have we learned in the past twenty years. Best Pract Res Clin Haematol 27(1):11–18. https://doi.org/10.1016/j.beha.2014.04.005
Koyama T, Hirosawa S, Kawamata N, Tohda S, Aoki N (2007) All-trans retinoic acid upregulates thrombomodulin and downregulates tissue-factor expression in acute promyelocytic leukemia cells: distinct expression of thrombomodulin and tissue factor in human leukemic cells. Blood 84(9):3001–3009
Tallman MS, Abutalib SA, Altman JK (2007) The double hazard of thrombophilia and bleeding in acute promyelocytic leukemia. Semin Thromb Hemost 33(4):330–338. https://doi.org/10.1055/s-2007-976168
Oudijk EJ, Nieuwenhuis HK, Bos R, Fijnheer R (2000) Elastase mediated fibrinolysis in acute promyelocytic leukemia. Thromb Haemost 83(6):906–908
Stein E, McMahon B, Kwaan H, Altman JK, Frankfurt O, Tallman MS (2009) The coagulopathy of acute promyelocytic leukaemia revisited. Best Pract Res Clin Haematol 22(1):153–163. https://doi.org/10.1016/j.beha.2008.12.007
Breen KA, Grimwade D, Hunt BJ (2012) The pathogenesis and management of the coagulopathy of acute promyelocytic leukaemia. Br J Haematol 156(1):24–36. https://doi.org/10.1111/j.1365-2141.2011.08922.x
Falanga A (2017) Predicting APL lethal bleeding in the ATRA era. Blood 129(13):1739–1740. https://doi.org/10.1182/blood-2017-02-763490
Cao M, Li T, He Z, Wang L, Yang X, Kou Y, Zou L, Dong X, Novakovic VA, Bi Y, Kou J, Yu B, Fang S, Wang J, Zhou J, Shi J (2017) Promyelocytic extracellular chromatin exacerbates coagulation and fibrinolysis in acute promyelocytic leukemia. Blood 129(13):1855–1864. https://doi.org/10.1182/blood-2016-09-739334
Lavallee VP, Chagraoui J, MacRae T, Marquis M, Bonnefoy A, Krosl J, Lemieux S, Marinier A, Pabst C, Rivard GE, Hebert J, Sauvageau G (2018) Transcriptomic landscape of acute promyelocytic leukemia reveals aberrant surface expression of the platelet aggregation agonist podoplanin. Leukemia 32(6):1349–1357. https://doi.org/10.1038/s41375-018-0069-1
Heilmann MG, Chardon E, Sultan C, Josso F (2010) The procoagulant factor of leukaemic promyelocytes: demonstration of immunologic cross reactivity with human brain tissue factor. Br J Haematol 30(2):151–158. https://doi.org/10.1111/j.1365-2141.1975.tb00529.x
Tanaka M, Yamanishi H (1993) The expression of tissue factor antigen and activity on the surface of leukemic cells. Leuk Res 17(2):103–111. https://doi.org/10.1016/0145-2126(93)90054-o
Stefano VD, Teofili L, Sica S, Mastrangelo S, Leone G (1995) Effect of all-trans retinoic acid on procoagulant and fibrinolytic activities of cultured blast cells from patients with acute promyelocytic leukemia. Blood 86(9):3535–3541
Kwaan HC, Rego EM (2010) Role of microparticles in the hemostatic dysfunction in acute promyelocytic leukemia. Semin Thromb Hemost 36(08):917–924. https://doi.org/10.1055/s-0030-1267045
Gheldof D, Mullier F, Bailly N, Devalet B, Dogné J-M, Chatelain B, Chatelain C (2014) Microparticle bearing tissue factor: a link between promyelocytic cells and hypercoagulable state. Thromb Res 133(3):433–439. https://doi.org/10.1016/j.thromres.2013.11.008
Ma G, Liu F, Lv L, Gao Y, Su Y (2013) Increased promyelocytic-derived microparticles: a novel potential factor for coagulopathy in acute promyelocytic leukemia. Ann Hematol 92(5):645–652. https://doi.org/10.1007/s00277-013-1676-6
Fogarty PF, Tarantino MD, Brainsky A, Grotzinger KM (2012) Selective validation of the WHO Bleeding Scale in patients with chronic immune thrombocytopenia. Curr Med Res Opin 28(1):79–87. https://doi.org/10.1185/03007995.2011.644849
Thaler J, Koppensteiner R, Pabinger I, Ay C, Gremmel T (2014) Microparticle-associated tissue factor activity in patients with acute unprovoked deep vein thrombosis and during the course of one year. Thromb Res 134(5):1093–1096. https://doi.org/10.1016/j.thromres.2014.07.041
Wang J, Weiss I, Svoboda K, Kwaan HC (2001) Thrombogenic role of cells undergoing apoptosis. Br J Haematol 115(2):382–391. https://doi.org/10.1046/j.1365-2141.2001.03095.x
Acknowledgements
We would like to thank Y.L. for her help in laser scanning confocal microscopy assay.
Funding
This work was supported by the National Natural Science Foundation of China (No. 81270589), Natural Science Foundation of Heilongjiang Province (No. H2017032), The Fundamental Research Funds for the Provincial Universities (No. 2019-KYYWF-0371), and Excellent youth project of the Fourth Affiliated Hospital of Harbin Medical University (No. HYDSYYXQN202013).
Author information
Authors and Affiliations
Contributions
Y.Z., H.Z., J.S., B.J., W.H., and J.Z. were involved in designing and/or conduct of the research; H.Z., J.S., F.C., and H.L. acquired the data; Y.Z., H.Z., and J.S. analyzed the data; and all authors interpreted the data, drafted the manuscript and/or revised it critically, and approved the final draft.
Corresponding author
Ethics declarations
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional committee and with the Helsinki Declaration.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(XLSX 20 kb)
Rights and permissions
About this article
Cite this article
Zhao, H., Sun, J., Yan, L. et al. Tissue factor–bearing microparticles are a link between acute promyelocytic leukemia cells and coagulation activation: a human subject study. Ann Hematol 100, 1473–1483 (2021). https://doi.org/10.1007/s00277-021-04533-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-021-04533-9