Abstract
Mantle cell lymphoma (MCL) is aggressive with poor prognosis. Due to t(11;14)(q13;q32), cyclin D1 is overexpressed. The in vitro activities of arsenic trioxide (As2O3) in MCL were investigated. In MCL lines Jeko-1 and Granta-519, As2O3 induced dose-dependent and time-dependent increases in apoptosis accompanied by cyclin D1 suppression. Downregulation of cyclin D1 resulted in decreased retinoblastoma protein phosphorylation, which led to repressed G1 progression to S/G2 phases. As2O3 did not affect cyclin D1 gene transcription. Instead, As2O3 activated glycogen synthase kinase-3beta (by tyrosine-216 phosphorylation) and IkappaB kinase alpha/beta (by serine-176/180 phosphorylation), both of which phosphorylated cyclin D1 at threonine-286, leading to its poly-ubiquitination and degradation in the proteasome. These observations were recapitulated partly in primary MCL samples obtained from patients refractory to conventional treatment. Our findings suggested that As2O3 might be clinically useful in MCL.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Mantle cell lymphoma (MCL) is a well-defined B-cell lymphoma in the World Health Organization classification [1] and accounts for 3–10 % of all non-Hodgkin lymphomas [2]. Practically all cases possess the translocation t(11;14)(q13;q32) [1], which juxtaposes the immunoglobulin heavy chain joining region on chromosome 14 to the CYCLIN D1 (CCND1) gene on chromosome 11 [3]. The molecular consequence is placement of CCND1 under the control of the immunoglobulin heavy chain gene enhancer [4], leading to cyclin D1 overexpression.
Cyclin D1 assembles with its catalytic partners cyclin-dependent kinase 4 (CDK4) and CDK6 to form an active holoenzyme complex, which phosphorylates the retinoblastoma (Rb) protein [5]. Phosphorylated Rb releases E2F transcription factors from inhibition, enabling E2Fs to coordinately regulate genes necessary for DNA replication and, hence, progression into the S phase [6]. Therefore, cyclin D1 overexpression consequent on t(11;14) leads to enhanced G1/S transition, a crucial step contributing to cellular proliferation and transformation.
CCND1 transcription is carefully regulated throughout the cell cycle [7]. Cyclin D1 level declines during the S phase, which has been attributed to its increased proteasomal degradation [8]. The proteasomal degradation of cyclin D1 is positively regulated by phosphorylation at threonine-286, which is mediated by glycogen synthase kinase-3beta (GSK-3β) [9, 10]. GSK-3β-induced threonine-286 phosphorylation also promotes cyclin D1 binding to a nuclear exportin CRM1, hence increasing its nuclear export [11]. Recently, it has been shown that threonine-286 phosphorylation can also be mediated by IkappaB kinase alpha (IKKα) [12], which thereby controls the subcellular localization and turnover of cyclin D1 [12]. These mechanisms ensure that cyclin D1 levels are well controlled.
Arsenic trioxide (As2O3) is a standard treatment for acute promyelocytic leukemia (APL) [13]. The myriad of molecular mechanisms underlying the efficacy of As2O3 in APL suggests that the drug might also be effective in other malignancies [14]. Preliminary clinical evidence indicated that As2O3 might be effective in MCL. A patient with concomitant therapy-related APL and MCL was reported to show a complete response of both diseases after oral As2O3 treatment [15]. Furthermore, in a clinical trial of intravenous As2O3 and ascorbic acid in 18 patients with refractory lymphomas, only 1 patient responded, and the patient had MCL [16].
In this report, we investigated the in vitro activities of As2O3 on MCL cell lines and primary patient specimens.
Materials and methods
Cell lines
The MCL lines Jeko-1 and Granta-519 (ACC 553 and ACC 342; German Collection of Microorganisms and Cell Cultures, Braunschweig, Germany) were cultured in RPMI 1640 with 20 % fetal bovine serum (FBS) and DMEM with 10 % FBS, respectively.
Primary human samples
Peripheral blood was obtained with informed consent from patients who were refractory to conventional chemotherapy, with the development of MCL in the leukemic phase. Mononuclear cells were collected by Ficoll–Paque density centrifugation, washed, and resuspended in culture medium for experimental use.
Reagents and antibodies
Reagents and antibodies used included cell culture reagents, TRIzol, SuperScript III One-Step Reverse Transcription Polymerase Chain Reaction (RT-PCR) Systems, and anti-ubiquitin antiserum (Life Technologies, Carlsbad, CA, USA); kinase inhibitors and their inactive analogues (Merck, Darmstadt, Germany); antiserum to phospho-GSK-3β (tyrosine-216) and protein G agarose (Millipore, Billerica, MA, USA); mouse monoclonal antibodies to ubiquitin, clone FK1, and clone FK2 (Biomol, Plymouth Meeting, PA, USA); antisera to cyclin D1, phospho-cyclin D1 (threonine-286), GSK-3β, IKKα/β, phospho-IKKα/β (serine-176/180), Rb, phospho-Rb (serine-795), caspase-3, and β-actin (Cell Signaling Technology, Beverly, MA, USA); ECL Kit and Ficoll–Paque Plus (GE Healthcare, Little Chalfont, UK); cell proliferation kit I (MTT) (Roche Diagnostics, Basel, Switzerland); annexin V-FITC Kit and DNA-Prep Reagents Kit (Beckman Coulter, Fullerton, CA, USA).
MTT, apoptosis assay, and cell cycle analysis
Cell viability before and after As2O3 treatment was assessed by MTT assay (Roche) according to standard methods. To study As2O3-induced apoptosis, annexin V-positive propidium iodide (PI)-negative cells were enumerated by standard flow cytometric protocols (Beckman Coulter). For cell cycle analysis, As2O3-treated cells were lysed by DNA-Prep LPR and stained with DNA-Prep Stain (Beckman Coulter) before flow cytometric analysis.
Semiquantitative RT-PCR for CCND1
RNA was extracted from control or As2O3-treated cells with TRIzol, and cDNA was synthesized (from 1 μg RNA) with a 40-cycle PCR (SuperScript III One-Step RT-PCR), using the CCND1 primers 5′-CTG GCC ATG AAC TAC CTG GA-3′ (forward) and 5′-GTC ACA CTT GAT CAC TCT GG-3′ (reverse). Cycling conditions were 15 s at 94 °C (first cycle, 2 min), 30 s at 58 °C, and 1 min at 68 °C (last cycle, 5 min). For internal control, GAPDH was also amplified (forward primer: 5′-AAC GGA TTT GGC CGT ATT GG-3′; reverse primer: 5′-CTT CCC GTT CAG CTC TGG G-3′).
Western blotting analysis
Control or As2O3-treated cells (1 × 106 cells/ml) were lysed (50 mM Tris–HCl, 100 mM NaCl, 5 mM EDTA, 40 mM NaP2O7, pH 7.5, 1 % Triton X-100, 4 μg/ml aprotinin, 1 mM dithiothreitol, 200 μM Na3VO4, 0.7 μg/ml pepstatin, 100 μM phenylmethylsulfonyl fluoride, and 2 μg/ml leupeptin). Clarified lysates were resolved on 12 % SDS-polyacrylamide gels, transferred to nitrocellulose membranes, blocked with 5 % nonfat milk, incubated with the appropriate primary antibodies and horseradish peroxidase-conjugated secondary antisera, visualized by chemiluminescence with the ECL Kit, and quantified by densitometry (ChemiDoc XRS + System; Bio-Rad Laboratories, Hercules, CA, USA).
Co-immunoprecipitation assays
Lysates from control or As2O3-treated cells were treated with the appropriate precipitating antibodies (4 μg/sample) or nonimmune sera at 4 °C for 1 h, followed by incubation with 30 μl of protein G agarose (50 % slurry) at 4 °C for 2 h. Immunoprecipitates were washed, boiled (5 min), and analyzed by Western blotting.
Results
As2O3 induced dose-dependent and time-dependent apoptosis in MCL cell lines
As2O3 induced dose-dependent cytotoxicity in Jeko-1 and Granta-519 cells (Fig. 1a) by a significant induction of apoptosis (Fig. 1b). Western blot analysis showed that caspase-3 activation was involved in As2O3-induced apoptosis (Fig. 1c), appearing first at 4 h after treatment.
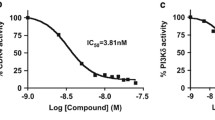
As2O3 inhibited the proliferation of MCL cells by inducing apoptosis and dose-dependent and time-dependent downregulation of cyclin D1. a Jeko-1 and Granta-519 cells (2 × 104 in 100 μl) were cultured in As2O3 for 72 h. There was a concentration-dependent decrease in viability. *P < 0.05, cell viability was significantly decreased as compared with baseline (triplicate experiments, one-way analysis of variance [ANOVA] with Dunnett's posttests). b As2O3 induced apoptosis in MCL. Jeko-1 cells (1 × 106 cells/ml) were treated in As2O3 (4 μM, 37 °C, 24 h) and resuspended in 500 μl buffer containing annexin V-FITC and PI for 20 min on ice before flow cytometric analysis. # P < 0.05, annexin V-positive PI-negative cells increased from a mean of 8.5 % in the control to 56.1 % in As2O3-treated groups (triplicate experiments, one-way ANOVA with Dunnett's posttests). Similar results were also obtained in Granta-519 cells (data not shown). c As2O3 activated caspase-3. Jeko-1 and Granta-519 cells (1 × 106 cells/ml) were treated with As2O3 (4 μM) for various durations. Cell lysates were immunoblotted with anti-caspase-3 or anti-β-actin antibodies. Caspase-3 activation (cleavage of caspase-3 from full-length 35 kDa into smaller fragments of 17 and 19 kDa) in both cell lines occurred after 4 h of As2O3 treatment. Expression of β-actin was unchanged. Representative Western blot of triplicate experiments was shown, with two other sets giving similar results. d Jeko-1 and Granta-519 cells (1 × 106 cells/ml) were treated with As2O3 for 8 h. Cell lysates were immunoblotted with anti-cyclin D1 or anti-β-actin antibodies. There was a dose-dependent downregulation of cyclin D1, which first became significant at 2 μM of As2O3. Representative Western blot and densitometric measurements of triplicate experiments were shown (*P < 0.05, one-way ANOVA with Dunnett's posttests). There was no change in β-actin. e Time-dependent downregulation of cyclin D1 by As2O3 (4 μM), which first became significant after 2 h. Representative Western blot and densitometric measurements of triplicate experiments were shown (*P < 0.05, one-way ANOVA with Dunnett's posttests)
As2O3 downregulated cyclin D1 in MCL cell lines and primary patient samples
As2O3 induced a dose-dependent and time-dependent decrease in cyclin D1 in both Jeko-1 and Granta-519 cells (Fig. 1d, e), first detectable at 0.5 to 1 h, becoming significant at 2 h, and almost complete at 8–12 h (Fig. 1e).
As2O3 induced posttranscriptional downregulation of cyclin D1
RT-PCR showed that CCND1 gene transcription was unaffected by As2O3 treatment, suggesting that the decrease in cyclin D1 levels was posttranscriptional (Fig. 2a).
As2O3 did not affect CCND1 gene expression in MCL cells, but regulated cyclin D1 degradation via GSK-3β and IKKα/β. a Cells were treated with different concentrations of As2O3 as indicated at 37 °C for 8 h. No change in CCND1 gene transcription was observed with As2O3 treatment, as shown by semiquantitative RT-PCR. Representative gels from one of three experiments shown; two other sets yielded similar results. b Jeko-1 cells (1 × 106 cells/ml) were treated with 4 μM As2O3 for 2 h. Cell lysates were immunoblotted with anti-phospho-cyclin D1 (Thr-286), p-Thr-286, or anti-cyclin D1 antibodies. As2O3 induced a significant increase in cyclin D1 Thr-286 phosphorylation. Representative Western blot and densitometric analysis of triplicate experiments were shown (C control; *P < 0.05, one-way ANOVA with Dunnett's posttests). c Cell lysates were immunoblotted with anti-phospho-GSK-3β (Tyr-216), p-Try-216, or anti-GSK-3β antibodies. As2O3 (4 μM, 2 h) also induced a significant increase in GSK-3β activation (phosphorylation). Representative Western blot and densitometric analysis of triplicate experiments were shown (C control; *P < 0.05, one-way ANOVA with Dunnett's posttests). d Prior to As2O3 treatment (4 μM, 8 h), Jeko-1 cells were preincubated with the GSK-3β inhibitor, 6-bromoindirubin-3′-oxime (BIO; 10 μM, 30 min). The downregulation of cyclin D1 induced by As2O3 was significantly reduced by inhibition of GSK-3β. Representative Western blot and densitometric analysis of triplicate experiments were shown (*P < 0.05, one-way ANOVA with Dunnett's posttests). e Jeko-1 cells (1 × 106 cells/ml) were treated with As2O3 (4 μM, 2 h). Cell lysates were immunoblotted with anti-phospho-IKKα/β (Ser-176/180), pSer-176/180, or anti-IKKα/β antibodies. As2O3 treatment resulted in a significant activation (phosphorylation) of IKKα/β. Representative Western blot and densitometric analysis of triplicate experiments were shown (C control; *P < 0.05, one-way ANOVA with Dunnett's posttests). f Prior to As2O3 treatment (4 μM, 8 h), Jeko-1 cells were preincubated with the IKKα/β inhibitor BMS-345541 (BMS; 10 μM, 30 min). Cell lysates were immunoblotted with anti-cyclin D1 or β-actin antibodies. Inhibition of IKKα/β significantly alleviated As2O3-induced cyclin D1 downregulation. Representative Western blot and densitometric analysis of triplicate experiments (*P < 0.05, one-way ANOVA with Dunnett's posttests). g Immunoprecipitation experiments of cell lysates from Jeko-1 cells treated with As2O3 (4 μM, 2 h). Immunoprecipitates (IP) with anti-IKKα/β antibody followed by immunoblotting (IB) showed increased cyclin D1 binding after As2O3 treatment. Conversely, immunoprecipitates with anti-cyclin D1 antibody showed increased IKKα/β binding. Representative Western blot of triplicate experiments was shown, with two other sets giving similar results
As2O3-induced cyclin D1 downregulation was related to GSK-3β activation
In Jeko-1 cells, As2O3 significantly increased cyclin D1 phosphorylation at threonine-286, a prerequisite for cyclin D1 degradation (Fig. 2b). Cyclin D1 phosphorylation is mediated by GSK-3β, which itself requires prior activation by tyrosine-216 phosphorylation. Accordingly, As2O3 in fact significantly increased GSK-3β tyrosine-216 phosphorylation, which paralleled the timing and magnitude of cyclin D1 threonine-286 phosphorylation (Fig. 2c). The GSK-3β inhibitor, 6-bromoindirubin-3′-oxime, successfully prevented As2O3-induced cyclin D1 downregulation (Fig. 2d). Because the diluent for 6-bromoindirubin-3′-oxime (dimethyl sulfoxide [DMSO]) was mildly toxic to Jeko-1 cells, its action on ameliorating As2O3-induced cytotoxicity could not be studied. These observations indicated that As2O3 downregulated cyclin D1 posttranscriptionally, apparently by increasing its degradation through GSK-3β.
As2O3-induced cyclin D1 downregulation was also dependent on IKKα/β
As2O3 significantly increased IKKα/β serine-176/180 phosphorylation, which was required for IKKα/β activation (Fig. 2e). Pretreatment with the IKKα/β inhibitor BMS-345541 significantly prevented As2O3-induced cyclin D1 downregulation, suggesting that IKKα/β was a molecular mediator of As2O3 (Fig. 2f). After As2O3 treatment, co-immunoprecipitation with an anti-IKKα/β antibody showed increased cyclin D1 binding to IKKα/β. Similarly, when cyclin D1 was immunoprecipitated, IKKα/β was also confirmed to co-immunoprecipitate (Fig. 2g). These results indicated that As2O3 activated IKKα/β, which bound cyclin D1, thus participating in its downregulation.
As2O3 promoted cyclin D1 ubiquitination
To study if As2O3-induced cyclin D1 downregulation was mediated via ubiquitination, immunoprecipitation of As2O3-treated Jeko-1 cell lysates with an anti-cyclin D1 antibody showed a time-dependent increase in bound ubiquitin, first detectable at 0.5 h and progressively increasing to up to 2 h (Fig. 3a). Immunoprecipitation with an anti-ubiquitin antibody also showed a time-dependent increase in bound cyclin D1, peaking at 2 h (Fig. 3a). These results showed that As2O3 activated GSK-3β and IKKα/β, leading to cyclin D1 threonine-286 phosphorylation and its subsequent ubiquitination. After immunoprecipitation with an anti-cyclin D1 antibody, immunoblotting with FK1 that recognized poly-ubiquitin moieties [17] and FK2 that recognized both poly-ubiquitin and mono-ubiquitin moieties [17] showed that As2O3 significantly increased ubiquitin binding to cyclin D1 (Fig. 3b). The results clearly indicated that As2O3 induced poly-ubiquitination of cyclin D1.
As2O3 induced ubiquitination of cyclin D1, leading to its degradation in the proteasome. a Jeko-1 cells (1 × 106 cells/ml) were treated with 4 μM As2O3 for different durations as shown. Cell lysates were immunoprecipitated (IP) and immunoblotted (IB) with antibodies as indicated. Lysates immunoprecipitated with anti-cyclin D1 and immunoblotted with anti-ubiquitin showed that As2O3 induced a time-dependent increase in binding of ubiquitin to cyclin D1. Conversely, when the lysates were immunoprecipitated with an anti-ubiquitin antibody and immunoblotted for cyclin D1, As2O3 was also found to induce a time-dependent increase in cyclin D1 binding to ubiquitin. The results of the densitometric analysis (of the major bands) in triplicate experiments were shown next to a representative immunoblot (*P < 0.05, one-way ANOVA with Dunnett's posttests). Note that in the crude lysates, cyclin D1 could be detected to be downregulated at 2 h. Images of the Western blot (with band size ranging from 25 to 45 kDa, representing cyclin D1 attached to varying copies of ubiquitin) were compressed in height for better fitting in the figure. b Lysates from Jeko-1 cells treated with As2O3 (4 μM, 2 h) immunoprecipitated with an anti-cyclin D1 antibody, followed by immunoblotting with appropriate antibodies. As2O3 treatment led to a significant increase in cyclin D1 ubiquitination as shown by the FK1 antibody, which detected poly-ubiquitin moieties. Similarly, an increase in cyclin D1 ubiquitination was observed with the FK2 antibody, which detected both mono-ubiquitin and poly-ubiquitin moieties. The apparent increase in band density might be due to additional mono-ubiquitination of cyclin D1, although owing to the lack of an antibody that recognized only mono-ubiquitin moieties this could not be further verified. Representative Western blot of triplicate experiments was shown, with the other sets showing similar results. c Jeko-1 cells (1 × 106 cells/ml) treated with As2O3 (4 μM, 8 h) with or without prior treatment for 30 min with the proteasome inhibitors MG132 (30 μM), bortezomib (Bort, 10 μg/ml), and lactacystin (Lact, 10 μM). Cell lysates were immunoblotted with anti-cyclin D1 or anti-β-actin antibody. Proteasomal inhibition resulted in significant alleviation of the As2O3-induced cyclin D1 degradation. Representative Western blot analysis and densitometric analysis of triplicate experiments (*P < 0.05, one-way ANOVA with Dunnett's posttests). However, whether the prevention of As2O3-induced cyclin D1 degradation by proteasomal inhibitors might rescue the cells from As2O3 cytotoxicity could not be tested because all the proteasomal inhibitors (MG132, bortezomib, and lactacystin) were themselves cytotoxic to Jeko-1 and Granta cells on prolonged incubation (data not shown). d Treatment with the lysosomal inhibitor ammonium chloride (NH4Cl) (2.5 mM) did not result in any change in As2O3-induced downregulation of cyclin D1. Representative Western blot analysis and densitometric analysis of triplicate experiments (# P = not significant, one-way ANOVA with Dunnett's posttests)
As2O3 induced cyclin D1 degradation in proteasomes but not lysosomes
To show that cyclin D1 ubiquitination resulted in its degradation, Jeko-1 cells were preincubated with the 26S and 20S proteasome inhibitors MG132 (30 μM), bortezomib (10 μg/ml), and lactacystin (10 μM) before As2O3 treatment. Proteasomal inhibition significantly attenuated As2O3-induced cyclin D1 downregulation (Fig. 3c). On the other hand, preincubation with the lysosomal inhibitor ammonium chloride (NH4Cl) had no effect (Fig. 3d). The results confirmed that As2O3 downregulated cyclin D1 by promoting its poly-ubiquitination, hence targeting it to proteasomal degradation.
As2O3-induced downregulation of cyclin D1 resulted in suppression of Rb phosphorylation
As2O3 suppressed Rb phosphorylation, first detectable at 2 h, which was at least 1 h later than As2O3-induced cyclin D1 downregulation (Fig. 4a). Total Rb remained unchanged, indicating that As2O3 affected the activation rather than the stability of Rb. Remarkably, suppression of Rb phosphorylation followed a time course similar to that of cyclin D1 downregulation (Fig. 1d, e). Finally, cell cycle analysis showed that As2O3 induced a significant increase in the apoptotic population and a significant decrease in the S/G2 population (Fig. 4b). Collectively, As2O3-induced downregulation of cyclin D1 preceded and resulted in the suppression of Rb phosphorylation, leading to a block in G1 progression to S and G2 phases.
As2O3 treatment led to decreased Rb phosphorylation and hence suppression of G1 progression to S/G2 phases. a Jeko-1 and Granta-519 cells were treated with As2O3 (4 μM). Cell lysates were immunoblotted with anti-phospho-Rb-Ser-795, pRb (Ser-795), or anti-Rb antibodies. There was a time-dependent downregulation of phosphorylated Rb, with no change in total Rb. Downregulation of phosphorylated Rb first became significant 4 h after treatment. Representative Western blot and densitometric analysis of triplicate experiments were shown (*P < 0.05, one-way ANOVA with Dunnett's posttests). b Cell cycle analysis by flow cytometry with control (0.1 % DMSO) or As2O3 treatment (4 μM, 8 h). Cells (1 × 106 cells/ml) were cultured in As2O3 for 8 h, resuspended in ice-cold phosphate-buffered saline, lysed by DNA-Prep LPR, and stained with DNA-Prep Stain for 20 min on ice before flow cytometric analysis. Results from a representative experiment were shown. Dotted line indicated the raw data, while the filled tracing represented modeling by the ModFit LT software (Verity Software House). As2O3 induced a significant increase in sub-G1 (apoptotic) population (control = 8.5 ± 0.3 % versus As2O3 = 16.2 ± 0.8 %, Dunnett's posttests, P < 0.05) and a significant decrease in the S/G2 population (S phase, control = 4.2 ± 0.4 % versus As2O3 = 2.7 ± 0.2 %, Dunnett's posttests, P < 0.05; G2 phase, control = 17.2 ± 1.1 % versus As2O3 = 5.5 ± 0.4 %, Dunnett's posttests, P < 0.05) (triplicate experiments)
The mechanistic actions of As2O3 on cell lines were recapitulated in primary MCL samples
Eight primary MCL patient samples were treated with As2O3. A significant increase in apoptosis was observed, as shown by flow cytometric analysis of annexin V and PI (Fig. 5a) and cell cycle analysis (Fig. 5b). The increase in apoptosis was mediated by caspase-3 activation (Fig. 5c). Finally, significant downregulation of cyclin D1 was also observed after As2O3 treatment (Fig. 5d), following a time course that was almost identical to those seen in Jeko and Granta cell lines (Fig. 1d, e).
The mechanistic actions of As2O3 were recapitulated in primary MCL samples. a Eight primary MCL patient samples were treated with As2O3 (4 μM, 24 h). A significant increase in apoptotic cells (asterisks annexin V-positive, PI-negative) were seen. The fold increase in apoptosis was obtained by comparing As2O3-treated and 0.1 % DMSO-treated (control) cells (one-way ANOVA with Dunnett's posttests, P < 0.05). b Cell cycle analysis by flow cytometry with control (0.1 % DMSO) or As2O3 treatment (4 μM, 8 h). Results from a representative experiment were shown. As2O3 induced a significant increase in sub-G1 cells (arrow). The results of primary MCL cells from eight patients were summarized in the right graph, showing a significant increase in sub-G1 fraction after As2O3 treatment (one-way ANOVA with Dunnett's posttests, P < 0.05). c As2O3 mediated caspase-3 activation in primary MCL cells. Primary MCL cells from patients (1 × 106 cells/ml) were treated with As2O3 (4 μM). As2O3-induced caspase-3 activation occurred after 4 h. Expression of β-actin was unchanged. Representative Western blot of triplicate experiments was shown, with two other sets giving similar results. d Primary MCL cells from patients (1 × 106 cells/ml) were treated with As2O3 (4 μM). As2O3 induced a progressive time-dependent downregulation of cyclin D1, which again was first significant after 2 h. Representative Western blot and densitometric measurements of triplicate experiments were shown (*P < 0.05, one-way ANOVA with Dunnett's posttests)
Discussion
In this study, we provided in vitro evidence of response of MCL to As2O3. There are several novel observations. We showed that As2O3 induced apoptosis in MCL cell lines and primary patient samples. As2O3 induced a dose-dependent and time-dependent suppression of cyclin D1, which restored Rb to a hypophosphorylated state, resulting in a blockade of G1 progression into the S/G2 phases. The time course of As2O3-induced changes was also consistent with this sequence of changes. As2O3-induced cyclin D1 suppression was first evident at 0.5–1 h, becoming significant at 2 h. Activation (suppression of phosphorylation) of Rb was first evident at 2 h and became significant at 4 h, which was also the time when caspase-3 activation was first observable.
We then showed that CCND1 transcription was unaffected by As2O3 treatment. In MCL cells, CCND1 is under the transcriptional control of the immunoglobulin heavy chain gene enhancer, which is not known to be affected by As2O3. Furthermore, under physiologic conditions, cyclin D1 levels during the cell cycle are controlled via alteration in stability and not changes in the transcription of cyclin D1 [7]. Finally, cyclin D1 levels were decreased as early as 0.5 h after As2O3 treatment, suggesting that protein degradation rather than decreased gene transcription was involved.
Cyclin D1 turnover is regulated by threonine-286 phosphorylation, a process mediated by GSK-3β [8–11]. GSK-3β is itself tightly regulated. Mitogens inactivate GSK-3β by a pathway involving Ras, phosphatidylinositol 3-kinase (PI3K), and protein kinase B/Akt [18]. Ras activates PI3K, which in turn activates Akt. Akt inactivates GSK-3β by phosphorylating it at serine residue 9 [19]. This removes the inhibition of GSK-3β on cyclin D1, allowing cyclin D1 to accumulate and thus activate cell cycling.
On the other hand, GSK-3β can be activated by phosphorylation at tyrosine-216 in the kinase domain [20]. The mechanisms controlling GSK-3β tyrosine-216 phosphorylation are largely undefined. GSK-3β might autophosphorylate. The tyrosine kinases Fyn [21], Csk [22], and Pyk2 [23] have been implicated in tyrosine-216 phosphorylation. Therefore, our findings were novel in showing that As2O3 might also increase tyrosine-216 phosphorylation. Interestingly, arsenic might not be the first example of a cation that regulates GSK-3β phosphorylation, as calcium had also been reported to enhance GSK-3β phosphorylation, via activation of the calcium-sensitive kinase Pyk2 [24]. Whether As2O3 acts through a similar mechanism will have to be investigated. In any case, the end result of As2O3-mediated increase in GSK-3β tyrosine-216 phosphorylation is an increase in cyclin D1 threonine-286 phosphorylation, a key step in its degradation. Again, the time course of As2O3-enhanced GSK-3β and thus cyclin D1 phosphorylation paralleled that of As2O3-induced cyclin D1 downregulation.
Another recently defined cyclin D1 regulation mechanism is the IKK system [12]. The IKK complex is the major regulatory component in the nuclear factor kappa-B (NF-κB) pathway. It comprises the catalytic subunits IKKα and IKKβ and a regulatory subunit IKKγ/NEMO [25]. Interestingly, IKKα has been shown to phosphorylate cyclin D1 at threonine-286, the same site targeted by GSK-3β [12]. IKKα requires activation by phosphorylation at serine-176, before participating in the regulation of NF-κB by phosphorylation of IκB [26]. IKKα serine-176 phosphorylation is mediated by NF-κB inducing kinase (NIK) [27]. Hence, our finding of As2O3-induced phosphorylation of IKKα/β is another important original observation, which may help to define the interaction of IKK and cyclin D1 in cell cycle control. Notably, As2O3 mediated an increase in the physical interaction between IKKα/β and cyclin D1, as shown by co-immunoprecipitation experiments. Finally, an IKKα/β specific inhibitor, BMS, alleviated As2O3-induced cyclin D1 downregulation. Taken together, these results indicated that IKKα/β was also a co-effector of As2O3. How As2O3 increases IKKα/β phosphorylation is unclear. However, NIK is activated by multiple stimuli, including tumor necrosis factor and interleukin-1 [27]. The potential interaction of As2O3 with these signaling molecules requires future studies.
We further showed that As2O3-mediated cyclin D1 threonine-286 phosphorylation increased its ubiquitination. The time course of cyclin D1 ubiquitination was commensurate with the timing of the biochemical events induced by As2O3. After As2O3 treatment, cyclin D1 ubiquitination was first detected at 30 min, coinciding with the observed decrease in cyclin D1 protein. Moreover, the demonstration of a specific chain of molecular events preceding cyclin D1 downregulation, and the absence of decreases in other proteins on Western blot analysis indicated that As2O3-mediated cyclin D1 degradation was not due to a nonspecific process of protein destruction.
Cyclin D1 is a cytosolic and nuclear protein. Degradation of this category of proteins is mediated via poly-ubiquitination, which targets proteins to the proteasomes [28]. Accordingly, we showed significant increases in poly-ubiquitination of cyclin D1 upon As2O3 treatment. Moreover, inhibition of the proteasome successfully prevented As2O3-induced cyclin D1 downregulation. On the other hand, inhibition of lysosomes, the site of degradation of mono-ubiquitinated proteins [29], did not interfere with As2O3-induced cyclin D1 downregulation. Although, in the immunoprecipitation experiments, As2O3-induced mono-ubiquitination could not be entirely excluded, the inability of lysosomal inhibition to attenuate cyclin D1 suppression argued against significant mono-ubiquitination of cyclin D1. Furthermore, mono-ubiquitination affects predominantly membrane-bound proteins [29] and is, therefore, unlikely to be involved in As2O3-induced decrease of cyclin D1. Hence, these results indicated that As2O3 downregulated cyclin D1 by promoting its proteasomal degradation (Fig. 6).
Our study provided evidence that As2O3 downregulated cyclin D1 at the protein level. Interestingly, in a recent study, MCL cell lines were also shown to have downregulation of cyclin D1 protein when treated with As2O3, although the molecular mechanism was not provided [30]. However, it is unlikely that the actions of As2O3 in downregulating cyclin D1 are specific to MCL. More likely, it is the overexpression of cyclin D1 in MCL that makes it sensitive to As2O3. These results also imply that As2O3 might be effective in other neoplasms that overexpress cyclin D1, a proposition that warrants further investigations. The capability of As2O3 in augmenting proteasomal degradation of cyclin D1 is reminiscent of its action on another fusion oncoprotein PML-RARA in APL. As2O3 binds directly to cysteine residues in the zinc finger domain of the PML protein [31], thereby enhancing the conjugation of an ubiquitin-related peptide SUMO-1 to the PML-RARA protein [32]. This directs PML-RARA to nuclear bodies, which are nuclear matrix domains containing 11S proteasome constituents recruited by As2O3 treatment. In this way, As2O3 triggers proteasome-dependent degradation of SUMO-conjugated PML-RARA [31, 32]. Therefore, As2O3 may act in conjunction with components of the proteasomal system to degrade target proteins. Findings of the current study corroborate with this proposition.
Some of these findings were recapitulated in primary MCL samples. Owing to limitations of cell number and in vitro growth capabilities of primary samples, we were unable to validate all the observations from cell lines. However, induction of apoptosis and downregulation of cyclin D1 could be demonstrated. Importantly, these primary samples were obtained from patients who were refractory to conventional chemotherapy, suggesting that As2O3 might be useful in the clinical salvage of these patients.
In conclusion, As2O3 induced significant in vitro suppression of MCL cells, both from established lines and primary patient samples. The concentrations of As2O3 were within the range achievable when As2O3 was used to treat patients with APL [33]. Furthermore, prolonged use of As2O3 has shown remarkable safety, and the advent of oral As2O3 has solved many of the problems associated with intravenous As2O3, particularly in obviating cardiac arrhythmias [34]. These in vitro observations should be validated clinically.
References
Swerdlow SH, Campo E, Seto M, Müller-Hermelink HK (2008) Mantle cell lymphoma. In: Swerdlow SH, Campo E, Harris NL, Jaffe ES, Pileri SA, Stein H, Thiele J, Vardiman JW (eds) WHO classification of tumours of haematopoietic and lymphoid tissues. International Agency for Research on Cancer, Lyon, pp 229–232
The Non-Hodgkin's Lymphoma Classification Project (1997) A clinical evaluation of the International Lymphoma Study Group classification of non-Hodgkin's lymphoma. Blood 89(11):3909–3918
Tsujimoto Y, Yunis J, Onorato-Showe L, Erikson J, Nowell PC, Croce CM (1984) Molecular cloning of the chromosomal breakpoint of B-cell lymphomas and leukemias with the t(11;14) chromosome translocation. Science 224(4656):1403–1406
Tsujimoto Y, Jaffe E, Cossman J, Gorham J, Nowell PC, Croce CM (1985) Clustering of breakpoints on chromosome 11 in human B-cell neoplasms with the t(11;14) chromosome translocation. Nature 315(6017):340–343
Sherr CJ (1996) Cancer cell cycles. Science 274(5293):1672–1677
Pérez-Galán P, Dreyling M, Wiestner A (2011) Mantle cell lymphoma: biology, pathogenesis, and the molecular basis of treatment in the genomic era. Blood 117(1):26–38
Guo Y, Stacey DW, Hitomi M (2002) Post-transcriptional regulation of cyclin D1 expression during G2 phase. Oncogene 21(49):7545–7556
Guo Y, Yang K, Harwalkar J, Nye JM, Mason DR, Garrett MD, Hitomi M, Stacey DW (2005) Phosphorylation of cyclin D1 at Thr 286 during S phase leads to its proteasomal degradation and allows efficient DNA synthesis. Oncogene 24(16):2599–2612
Diehl JA, Zindy F, Sherr CJ (1997) Inhibition of cyclin D1 phosphorylation on threonine-286 prevents its rapid degradation via the ubiquitin-proteasome pathway. Genes Dev 11(8):957–972
Diehl JA, Cheng M, Roussel MF, Sherr CJ (1998) Glycogen synthase kinase-3beta regulates cyclin D1 proteolysis and subcellular localization. Genes Dev 12(22):3499–3511
Alt JR, Cleveland JL, Hannink M, Diehl JA (2000) Phosphorylation-dependent regulation of cyclin D1 nuclear export and cyclin D1-dependent cellular transformation. Genes Dev 14(24):3102–3114
Kwak YT, Li R, Becerra CR, Tripathy D, Frenkel EP, Verma UN (2005) IkappaB kinase alpha regulates subcellular distribution and turnover of cyclin D1 by phosphorylation. J Biol Chem 280(40):33945–33952
Tallman MS, Altman JK (2009) How I treat acute promyelocytic leukemia. Blood 114(25):5126–5135
Chen SJ, Zhou GB, Zhang XW, Mao JH, de Thé H, Chen Z (2011) From an old remedy to a magic bullet: molecular mechanisms underlying the therapeutic effects of arsenic in fighting leukemia. Blood 117(24):6425–6437
Au WY, Ma SK, Chung LP, Chim CS, Kwong YL (2002) Two cases of therapy-related acute promyelocytic leukemia (t-APL) after mantle cell lymphoma and gestational trophoblastic disease. Ann Hematol 81(11):659–661
Chang JE, Voorhees PM, Kolesar JM, Ahuja HG, Sanchez FA, Rodriguez GA, Kim K, Werndli J, Bailey HH, Kahl BS (2009) Phase II study of arsenic trioxide and ascorbic acid for relapsed or refractory lymphoid malignancies: a Wisconsin Oncology Network study. Hematol Oncol 27(1):11–16
Fujimuro M, Yokosawa H (2005) Production of antipolyubiquitin monoclonal antibodies and their use for characterization and isolation of polyubiquitinated proteins. Methods Enzymol 399:75–86
Kauffmann-Zeh A, Rodriguez-Viciana P, Ulrich E, Gilbert C, Coffer P, Downward J, Evan G (1997) Suppression of c-Myc-induced apoptosis by Ras signalling through PI(3)K and PKB. Nature 385(6616):544–548
Cross DA, Alessi DR, Cohen P, Andjelkovich M, Hemmings BA (1995) Inhibition of glycogen synthase kinase-3 by insulin mediated by protein kinase B. Nature 378(6559):785–789
Hughes K, Nikolakaki E, Plyte SE, Totty NF, Woodgett JR (1993) Modulation of the glycogen synthase kinase-3 family by tyrosine phosphorylation. EMBO J 12(2):803–808
Lesort M, Jope RS, Johnson GV (1999) Insulin transiently increases tau phosphorylation: involvement of glycogen synthase kinase-3beta and Fyn tyrosine kinase. J Neurochem 72(2):576–584
Fan G, Ballou LM, Lin RZ (2003) Phospholipase C-independent activation of glycogen synthase kinase-3beta and C-terminal Src kinase by Galphaq. J Biol Chem 278(52):52432–52436
Sayas CL, Ariaens A, Ponsioen B, Moolenaar WH (2006) GSK-3 is activated by the tyrosine kinase Pyk2 during LPA1-mediated neurite retraction. Mol Biol Cell 17(4):1834–1844
Hartigan JA, Johnson GV (1999) Transient increases in intracellular calcium result in prolonged site-selective increases in Tau phosphorylation through a glycogen synthase kinase 3beta-dependent pathway. J Biol Chem 274(30):21395–21401
Karin M, Greten FR (2005) NF-kappaB: linking inflammation and immunity to cancer development and progression. Nat Rev Immunol 5(10):749–759
Ling L, Cao Z, Goeddel DV (1998) NF-kappaB-inducing kinase activates IKK-alpha by phosphorylation of Ser-176. Proc Natl Acad Sci U S A 95(7):3792–3797
Malinin NL, Boldin MP, Kovalenko AV, Wallach D (1997) MAP3K-related kinase involved in NF-kappaB induction by TNF, CD95 and IL-1. Nature 385(6616):540–544
Ciechanover A (1998) The ubiquitin–proteasome pathway: on protein death and cell life. EMBO J 17(24):7151–7160
Hicke L (2001) Protein regulation by monoubiquitin. Nat Rev Mol Cell Biol 2(3):195–201
Jung HJ, Chen Z, McCarty N (2012) Synergistic anticancer effects of arsenic trioxide with bortezomib in mantle cell lymphoma. Am J Hematol 87(12):1057–1064
Zhang XW, Yan XJ, Zhou ZR, Yang FF, Wu ZY, Sun HB, Liang WX, Song AX, Lallemand-Breitenbach V, Jeanne M, Zhang QY, Yang HY, Huang QH, Zhou GB, Tong JH, Zhang Y, Wu JH, Hu HY, de Thé H, Chen SJ, Chen Z (2010) Arsenic trioxide controls the fate of the PML-RARalpha oncoprotein by directly binding PML. Science 328(5975):240–243
Lallemand-Breitenbach V, Zhu J, Puvion F, Koken M, Honore N, Doubeikovsky A, Duprez E, Pandolfi PP, Puvion E, Freemont P, de The H (2001) Role of promyelocytic leukemia (PML) sumolation in nuclear body formation, 11S proteasome recruitment, and As2O3-induced PML or PML/retinoic acid receptor alpha degradation. J Exp Med 193(12):1361–1371
Au WY, Tam S, Fong BM, Kwong YL (2008) Determinants of cerebrospinal fluid arsenic concentration in patients with acute promyelocytic leukemia on oral arsenic trioxide therapy. Blood 112(9):3587–3590
Au WY, Kumana CR, Lee HK, Lin SY, Liu H, Yeung DY, Lau JS, Kwong YL (2011) Oral arsenic trioxide-based maintenance regimens for first complete remission of acute promyelocytic leukemia: a 10-year follow-up study. Blood 118(25):6535–6543
Acknowledgments
This study was supported in part by the Ruby & Minoo N. Master Charity Fund. The authors thank Alice Cheung for the technical assistance. Dr. Wing-Yan Au obtained the patient samples, and Prof. Gopesh Srivastava provided the cell lines.
Conflict of interest
The University of Hong Kong holds patents from the USA and Japan for the use of oral arsenic trioxide in the treatment of leukemias. The authors are employees of the University of Hong Kong.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lo, R.K.H., Kwong, YL. Arsenic trioxide suppressed mantle cell lymphoma by downregulation of cyclin D1. Ann Hematol 93, 255–265 (2014). https://doi.org/10.1007/s00277-013-1866-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-013-1866-2