Abstract
The prolonged life span of chronic lymphocytic leukemia (CLL) cells in vivo is assumed to depend on the surrounding microenvironment since this biologic feature is lost in vitro. We studied here the molecular interactions between CLL cells and their surrounding stroma to identify factors that help CLL cells to resist apoptosis. Sorted CLL cells from 21 patients were cultured in vitro on allogenous, normal bone marrow stromal cells (BMSCs) in the presence/absence of CD40 ligand or in culture medium alone. Surface and mRNA expression of interaction molecules, cytokine production, and apoptosis rate was measured by flow cytometric, real-time PCR and standard immunologic assays. The interaction between CLL cells and BMSCs rescued CLL cells from apoptosis. BMSCs co-cultured with CLL cells showed a strong increase in IL-8 and IL-6 secretion and up-regulated the expression of ICAM-1 and CD40 mRNA. The mRNA expression of CXCL12 and VCAM1 remained unchanged. In turn, CLL cells in interaction with BMSCs significantly up-regulated the expression of CD18 and CD49d that are ligands for the critical adhesion molecules on BMSCs. As a validation of the in vitro data, we found a significant higher expression of CD49d on CLL cells in bone marrow aspirates compared to peripheral blood CLL cells in patient samples. Up-regulation of adhesion molecules and their ligands in CLL–BMSCs interaction along with the increased cytokine production of BMSCs indicate a strong effect of CLL cells on BMSCs in favor of their apoptosis resistance.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Chronic lymphocytic leukemia (CLL) is characterized by the accumulation of monoclonal CD5+ B cells [1]. The majority of CLL cells are nondividing, and it has been suggested that the resistance to apoptosis could be responsible for the accumulation of CLL cells in vivo [2]. Despite the longevity in vivo, the majority of CLL cells die in vitro during a short-term culture in medium [3]. This suggests that the survival of CLL cells is attributed to humoral and cellular factors capable of protecting CLL cells from apoptosis. Direct contact with bone marrow-derived stromal cells (BMSCs) enhances the survival of CLL cells in the absence of exogenous factors [4]. This interaction of CLL cells and BMSCs is mediated by the adhesion molecules very late antigen 4 (VLA-4) and lymphocyte function-associated antigen 1 (LFA-1) and their ligand's vascular cellular adhesion molecule 1 (VCAM-1 [CD106]) and intercellular adhesion molecule (ICAM-1 [CD54]), respectively [4]. In addition, BMSCs in culture also secrete a number of cytokines and chemokines such as IL-1β, IL-6, IL-8, stromal cell-derived factor-1 (SDF-1, CXCL12), and basic fibroblast growth factor (bFGF) that can also support CLL cell survival [5–8].
It has been suggested that CLL cells are able to manipulate their microenvironment. CLL cells are capable of secreting VEGF and other angiogenic factors that induce marrow vascularity in order to provide adequate blood supply for tumor growth [9, 10]. It has also been demonstrated that CLL cells co-cultured with CLL-derived stromal cells (marrow stromal elements, MSE) dramatically increase the secretion of bFGF, compared to MSE or CLL cells cultured alone [11]. In drug development, the new promising agents as thalidomide and its derivate lenalidomide are also based on the inhibition of the beneficial effects of the microenvironment on CLL cells [12, 13].
Proliferating CLL cells occur in so-called proliferation centers or pseudo-follicles (PC) [14]. PC are composed of CD40 ligand (CD40L) expressing activated T cells, proliferating CLL cells, and stromal cells [15]. Stromal cells have been shown to express the B cell associated surface receptor CD40 [16]; therefore, we suppose a direct molecular interaction between activated T cells, stromal cells, and proliferating CLL cells in PC.
In this study, we investigated to which extent CLL cells are able to influence their microenvironment, especially in PC. For this purpose, we used our established in vitro PC model [17], wherein the presence of the T cell-derived CD40L sorted, circulating CLL cells were cultured on allogenous bone marrow-derived stromal cells. Apart from the known anti-apoptotic effect of BMSCs on CLL cells, we could show that CLL cells manipulate their BMSC microenvironment by inducing the secretion of vital cytokines and up-regulate the expression of adhesion molecules in BMSCs to further facilitate their own survival. For an even better interaction with stromal cells, CLL cells also increase the expression of adhesion molecule ligands, which we could also confirm in ex vivo patient samples.
Design and methods
Patients
The ethics committee of the University of Regensburg approved this study, which included 21 B-CLL patients (7 women and 14 men) with a median age of 65 (39 to 84) years. All patients and BMSC donors gave their informed consent. Diagnosis was based on standard clinical immunophenotyping and cytology. At the time point of cell separation, the patients were untreated or had not received any treatment in the previous 3 months. Table 1 summarizes the main clinical data of the patients.
Preparation of BM stromal cell cultures
Primary human BMSC cultures were established as described previously [4]. Briefly, bone marrow aspirates, exclusively from untreated patients without detectable abnormal cells, were applied from routine diagnostic specimens. BMMNC (6–8 × 105) per well were plated on 6-well plates (Falcon, BD Biosciences) in 1 ml Dulbecco modified Eagle medium (DMEM; Biochrom AG), supplemented with 20% heat-inactivated FCS (Biochrom AG), 100 U/ml penicillin (PAN Biotech GmbH), and 100 μg/ml streptomycin (PAN Biotech GmbH) at 37°C and 5% CO2. After 1 week, the non-adherent cells were removed by complete replacement of medium. Adherent cells were further cultured until reaching a confluent layer, the culture medium was replaced twice a week. Confluent cultures, achieved after a minimum of 4 weeks, were split once or twice. The confluent monolayers contained approximately 1–2 × 105 stromal cells per well with similar maturation stages when used for co-culture experiments or direct analysis.
Immunphenotyping of stromal cells
Stromal cells were detached from the 6-well plates by treatment with 37°C 0.04% EDTA in phosphate-buffered saline (PBS; PAA Laboratories GmbH). The cells were washed and suspended in PBS at a concentration of 5 × 105 cells/100 μl and incubated with conjugated monoclonal antibodies in the recommended concentration of the manufacturer's data sheet. Cells were washed and suspended in 0.5 ml PBS and analyzed on LSR II flow-cytometer (BD Biosciences).
Measurement of cytokines in the supernatant of co-cultures
Cytokines were measured in culture supernatants by using the Beadlyte Human Multi-Cytokine Detection System 3 (Upstate Biotechnology), which enables the parallel detection of IL-1β, IL-2, IL-4, IL-6, IL-8, IL-10, IL-12, TNF-α, IFN-γ, and GM-CSF with a sensitivity of 0.7 pg/ml for each cytokine. For cytokine, concentrations over the cut-off samples were diluted accordingly. The analysis was carried out according to the manufacturer's guideline. Results were read on a Luminex® 100™ instrument.
Separation procedure of CLL cells
Peripheral blood mononuclear cells (PBMC) of patients with B-CLL were freshly isolated by centrifugation through Ficoll-Hypaque density gradient, followed by staining with monoclonal antibodies for FACS analysis: fluorescein isothiocyanate (FITC)-labeled anti-glycophorin A (DAKO Inc.), phycoerytrin (PE)-labeled anti-CD14 (BD Bioscience) + anti-CD56 (Beckman Coulter), and allophycocyanin (APC)-labeled anti-CD3 (BD Biosciences). The unstained cells in the lymphoid gate were sorted by a FACSAria Cell Sorter (BD Biosciences) using PBS W/O Ca2+/Mg2+ as sheath fluid. The sorted CLL cell populations had a purity of more than 98%, as proven subsequently by direct immunofluorescence staining with anti-CD19-APC (BD Biosciences) antibody in each case using a FACSCanto Flow Cytometer (BD Biosciences).
Immunphenotyping of CLL cells
Peripheral blood and bone marrow aspirates from seven patients with B-CLL were compared by staining the samples with monoclonal antibodies for FACS analysis: FITC-labeled anti-CD3, PE-labeled anti-CD18 or CD49d, and PECy5-labeled anti-CD19. After red blood cell lysis, samples were washed and analyzed with a FACSCan Flow Cytometer (BD Biosciences).
Culture conditions for CLL cells
Sorted CLL cells were cultured at a concentration of 106 cells/0.5 ml on stromal cells in the presence/absence of 1 μg/ml soluble CD40 Ligand (CD40L) (PeproTech EC) or in culture medium alone. In single CLL culture DMEM supplemented with 10% FCS was applied, other culture conditions were as described previously. The cells were harvested after 84 h. After harvest, the CLL cell contamination on BMSCs was determined by measuring contaminating CD19 mRNA expression. In typical cases, it was 3 log lower compared to CLL cells.
Flow cytometric analysis of apoptosis
Sorted CLL cells before and after culture were washed with cold PBS and resuspended in 100 μl of annexin-binding buffer (BD Biosciences) containing 1 μg/ml propidium iodide (Sigma Aldrich) and 5 μl of FITC-conjugated annexin V (BD Biosciences). After 15 min incubation period, 400 μl of annexin-binding buffer was added, and the cells were analyzed on a LSR II flow-cytometer using FACSDiva software (BD Biosciences). Viable cells were PI- and annexin V-negative.
Calculation of cell survival in vitro
Cultured CLL cells were counted in a Casy Cell Counter Model DT (electronic pulse area analysis). The living population was corrected by subtracting the annexin V positive fraction from the absolute cell count. We set the number of pre-culture living (annexin V/PI negative) cells to 100%. The ratio between the corrected living cell count before and after culture resulted in the survival rate of the CLL cells.
Immunhistochemical staining of vimentin and CD68
Immunohistochemistry for vimentin and CD68 was performed on formalin-fixed BMSCs specimens according to the manufacturers' data sheets. After high-temperature antigen retrieval, the wells were incubated with vimentin or CD68 antibodies (Dako GmbH, Hamburg, Germany) for 30 min. The antigens were detected with the streptavidin–biotin complex method (sABC) (Ventana, France) and visualized in brown with DAB (3, 3 diaminobenzidine tetrahydrochloride) (Ventana), whereas nuclei were counterstained with hematoxylin (Merck, Darmstadt, Germany).
Gene expression analysis
BMSCs were removed by a cell scraper and dissolved in RLT buffer (Qiagen Inc.) for mRNA isolation with QIA-Amp mini kit (QIAGEN) according to the manufacturer's instructions. RNA purity and integrity were assessed using an Agilent 2100 bioanalyzer (Agilent Technologies), and cDNA synthesis was performed using ImProm-II Reverse Transcriptase System (Promega) according to the manufacturer's recommendations. Gene expression analysis with TaqMAN gene expression assays (AssayOnDemand, Applied Biosystems) were carried out in a HT-7900 real time PCR machine (Applied Biosystems). Cycling conditions matched the manufacturer's specifications. Results were analyzed with the SDS2.2 software (ABI)/Microsoft Excel with the deltadelta-Ct method using a general calibrator RNA. To evaluate the gene expression of stromal cells that were in co-culture with B-CLL cells, CLL cells were separated after co-culture from BMSCs, and the mRNA expression of BMSCs and CLL cells were determined separately. Pure BMSC expression was calculated by subtracting expression of contaminating CLL cells from the total expression measured. This was achieved by calculating the proportion and expression strength of contaminating RNA for each gene. Proportion was calculated by the expression ratio of the CD19 gene in contaminated stromal cells and in pure B-CLL cells after co-culture.
Statistical analysis
Statistical analysis was performed with SPSS, version 17.0. Graphs denote box plots or bar graphs. Comparisons of groups of data were performed using the two-tailed t test, and statistical significance was considered at p values ≤0.05.
Results
Establishment of allogenous bone marrow stromal cell culture
Following mononuclear cell separation from aspirates of non-pathological bone marrows after 3–5 days of culture adherent, spindle-like, and round cells with attached lymphoid structures appeared. The adherent cells showed extensions, and aligning cells started to form a network (Fig. 1a) with the simultaneous appearance of double nuclei that is also characteristic for stromal cells (Fig. 1b). During the first 2–3 weeks of culture, all the lymphoid structures detached. The adherent cells started to proliferate in foci, forming complicated nodular structures (Fig. 1c). We could observe a variation in the proliferation potential of BMSCs depending on the age of the donors. BMSCs' yields from bone marrow MNCs (BMMNC) of younger donors were higher (Fig. 1e). On average, after 6 weeks (4–10 weeks) of culture, the cells tended to senescence, lost their spindle-like form, became large and round, and formed a confluent monolayer (Fig. 1d).
In vitro development of bone marrow stromal cells (BMSCs). a One-week-old BMSC culture with adherent spindle-like stromal cell progenitors with attached and free lymphoid cells. b Adherent, large stromal cells have doubled nucleus and long extensions, which bind surviving lymphocytes. c Proliferating stromal cells sometimes form nodules when growing in colonies as a sign of matrix mineralization. d Monolayer of mature bone marrow stromal cells in co-culture with CLL cells, which appear as bright spots. e Efficiency of bone marrow stromal cell (BMSC) cultivation shows inverse association with the patients' age. The ratio of the freshly isolated bone marrow mononuclear cells (BMMNCs) and BMSCs gained is illustrated
Characterization of stromal cells
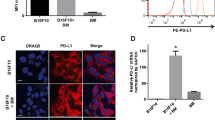
BMSC cultures were analyzed for antigen and mRNA expression and cytokine secretion. BMSCs in culture expressed the mesenchymal tissue-specific subunit of cytoskeletal elements vimentin at a high level, whereas the monocyte and tissue macrophage antigen CD68 could not be detected by immunohistochemisty (Suppl. Fig. 1). The absence of the CD45 mRNA expression in BMSCs, a feature characteristic for stromal cells [18], also proved their non-hematopoietic origin (data not shown), whereas the mRNA expression of the adhesion molecules VCAM-1 and ICAM-1 was at very high levels along with the mRNA expression of the cytokines IL-6, IL-8, and the chemokine CXCL12 (Suppl. Fig. 1b). The mRNA expression of CD40, IL-1β, and TNF-α was detectable, but to a lower extent (Suppl. Fig. 1b). We confirmed the mRNA expression by immunophenotyping showing a considerable expression of the VCAM-1, ICAM-1, and CD40 antigens on the surface of cultured BMSCs (Suppl. Fig. 1c). Multiplex bead assay of the culture supernatants confirmed the secretion of the cytokines IL-6, IL-8, IL-1β, and TNF-α accordingly to the observed mRNA expression (Suppl. Fig. 1d).
BMSCs protected CLL cells from spontaneous apoptosis
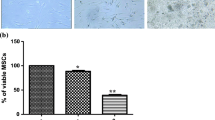
We evaluated the survival of CLL cells co-cultured with BMSCs or in medium alone after 84 h. BMSCs significantly reduced spontaneous apoptosis of CLL cells raising the average survival from 20.5% to 49.5% (Fig. 2). The presence of the T cell-derived soluble CD40-ligand had no beneficial effect on the survival of CLL cells in co-culture (Fig. 2). In this context, we show that the primary effect on CLL survival in PC is mediated by the interaction between CLL cells and the surrounding stroma, and we found no further CD40L dependent anti-apoptotic effect.
Survival of CLL cells under different culture conditions. BMSCs prevented significantly in vitro the spontaneous apoptosis of CLL cells. White columns: survival of CLL cells in medium, gray columns: in medium with CD40L, dark gray columns: on BMSCs, black columns: on BMSCs with CD40L. Results for survival proportion (percent) are the mean ± percentiles of 21 independent experiments, respectively. Student's paired t test; *p < 0.05, **p < 0.01
CLL cells induced ICAM1 expression and cytokine production of BMSCs
To evaluate the potential to which extent CLL cells are able to modify the surrounding stroma in order to further facilitate their own survival, we analyzed the mRNA expression of interaction molecules and the cytokine secretion of BMSCs in the presence/absence of CLL cells.
We found that CLL cells had a considerable effect on BMSCs in co-culture. In the presence of CLL cells, BMSCs significantly up-regulated the mRNA expression of ICAM-1 and CD40, whereas the expression of VCAM-1 and CXCL12 remained unchanged. The presence of CD40L did not further influence the expression of the co-receptors on BMSCs (Fig. 3b). We could detect a slight down-regulation in the expression of CXCL12, but this difference failed to reach statistical significance (Fig. 3b).
The changes of in vitro cytokine production and gene expression under different culture conditions. a Secretion of each measured cytokine was increased in co-culture of BMSCs with CLL cells. Additional CD40L, however, raised moderately the secretion of IL-1β and IL-8. Cytokine production of BMSC (white boxes), in co-culture with CLL cells (gray boxes) and in co-cultures with CLL cells and CD40L (dark gray boxes). b In co-culture with CLL cells, BMSCs up-regulated significantly the mRNA expression of ICAM1 and CD40. IL-6, IL-1β, and TNF-α were also elevated. Additional CD40L did not exert any significant effect on the mRNA expression of the investigated genes. mRNA expression of BMSC in medium (white boxes), in co-culture with CLL cells (gray boxes), in co-culture with CLL cells and CD40L (dark gray columns). c CLL cells expressed significantly more mRNA of TNF-α cultured on BMSCs. Results for each mRNA and cytokine are the mean ± percentiles of at least five independent experiments. Student's paired t test; *p < 0.05, **p < 0.01
The presence of CLL cells on BMSCs significantly influenced the cytokine secretion. We detected an increase in the production of IL-1β, IL-8, and TNF-α in the co-culture supernatant (Fig. 3a). The secretion of IL-6 was also strongly elevated, but this difference did not reach statistical significance (p = 0.079). The presence of CD40L slightly but not significantly increased the secretion of IL-8 and IL-1β in the co-culture (Fig. 3a). To evaluate the origin of the secreted cytokines, we determined their mRNA expression in BMSCs and CLL cells. BMSCs had a remarkable mRNA expression of IL-1β, IL-6, and IL-8 (Fig. 3c). In CLL cells, the expression of IL-1β and IL-6 was marginal, and IL-8 was weakly expressed (data not shown). In contrast, CLL cells showed a considerably higher expression of TNF-α than BMSCs (Fig. 3b, c). Based on these findings, we suggest that the elevated concentration of IL-6, IL-8, and IL-1β seen in the co-culture is secreted by the BMSCs, and the increased TNF-α levels originate from the CLL cells.
CLL cells up-regulate the ligands for adhesion molecules in co-culture with BMSCs
On the surface of CLL cells, VLA-4 and LFA-1 are ligands for the adhesion molecules VCAM-1 and ICAM-1 expressed on stroma cells. To investigate the effect of CLL–BMSC interaction on the expression of VLA-4 and LFA-1, CLL cells were stained for surface CD49d and CD18, parts of the VLA-4 and LFA-1 ligand complexes, respectively. Comparing the relative fluorescence intensities measured by flow cytometry, CLL cell in co-culture with BMSCs significantly up-regulated the expression of CD49d and CD18 compared to peripheral blood CLL cells (Fig. 4a). The presence of CD40L in the co-culture further increased the expression of CD18, but left CD49d unchanged (Fig. 4a).
a Antigen expression on CLL cells in vitro. CLL cells strongly up-regulated the expression of adhesion antigens in co-culture with BMSCs. White boxes: antigen expressions before culture, gray boxes: after co-culture with BMSCs, dark gray boxes: after co-culture with BMSCs with CD40L. b The ratio of CD49d expressing CLL cells was significantly higher in bone marrow than in peripheral blood. White boxes: antigen expressions in peripheral blood; dark gray boxes: in bone marrow. Results for relative fluorescence intensities (RFI) are the mean ± percentiles of 15–18 in vitro and 7 independent experiments, respectively. Student's paired t test; *p < 0.05, **p < 0.001. c Comparison of CD49d expression on CLL cells from bone marrow and peripheral blood. Gray line: FI in peripheral blood; black line: FI in bone marrow
Bone marrow microenvironment induces the CD49d expression on CLL cells in vivo
In order to further prove the stimulating effect of the BMSC–CLL interaction on CLL cells, we compared, in patient samples, the expression of CD49d and CD18 on CLL cells taken from bone marrow and peripheral blood. Three CLL samples with nearly 100% CD49d or CD18 expression in the peripheral blood were excluded. In all investigated cases, the normalized CD49d expression was higher in the bone marrow than in peripheral blood (p < 0.05), which confirms the in vitro findings (Fig. 4b, c). In Fig. 4c, two typical CD49d expression patterns are presented. The expression of CD18, however, was comparable on the bone marrow-derived and peripheral blood CLL cells (Fig. 4b).
Discussion
CLL cells infiltrate the bone marrow from the earliest stage of disease, indicating that the bone marrow microenvironment facilitates disease progression. The presence of bone marrow-derived stromal feeder cells is pivotal for the survival of CLL cells in vitro [19]. As we described previously, the stromal cells sustain apoptosis resistance of primary CLL cells, and the range of survival depends on characteristics of the CLL cells [17]. Additionally, bone marrow stroma has been shown to protect CLL cells from drug-induced apoptosis that may play the major role in treatment failures [11].
In this experimental setup, we analyzed to which extent CLL cells are able to manipulate their stromal microenvironment in favor of their apoptosis resistance. Direct contact between CLL cells and BMSCs is critical for their apoptosis protection. Blocking this interaction between adhesion molecules and their ligands with monoclonal antibodies or by the insertion of a microporous membrane results in increased apoptosis of the CLL cells [11, 20]. Here, we show that CLL cells influence their interaction with BMSCs in order to intensify the adhesion in two ways: (1) CLL cells induce a strong up-regulation of the anti-apoptotic adhesion molecule ICAM-1 on BMSCs; (2) CLL cells up-regulate the adhesion molecule ligands (CD18 and CD49d) on their own surface. We could also show, in patient samples, that CLL cells directly taken from the bone marrow have a significantly higher expression of CD49d than the circulating CLL cells in peripheral blood. These results indicate that CLL cells are able to change their characteristics depending on the surrounding microenvironment. Our data are coincident with previous findings that show up-regulation of CD49d on CLL cells by stromal cells, which we present investigating a larger patient collective [21]. In addition, the significance of CD49d expression in CLL was recently confirmed as an independent predictor of OS [22]. The up-regulation of CD18 seen in vitro could not be confirmed ex vivo, which is probably due to the complex regulation of the CD18 expression, e.g., by T cell-derived cytokines [23–25].
Besides, the direct contact with BMSCs cytokines, such as TNF-α, CXCL12, IL-1β, IL-4, IL-6, IL-8, and IL-10 are also indicated to be involved in the activation, growth, and apoptosis resistance of CLL cells [26, 27]. Chemokines as CXCL12 induce a high-affinity conformation change of integrins on leukocytes that is required for the firm adhesion to endothelial and stromal cells [28, 29]. Elevated serum levels of TNF-α, IL-6, IL-8, and IL-10 are associated with increased mortality in CLL [26, 30–34]. The role of inflammatory cytokines in CLL cell survival is also supported by genome-wide association studies, finding significant relations between mortality and single nucleotide polymorphisms in the region of cytokine coding genes [26, 35]. Studies analyzing mRNA expression of cytokines indicate that circulating CLL express genes for TNF-α, IL-1β, IL-6, and IL-8 [36–38]. To our knowledge, however, a detailed analysis of cytokine crosstalk between CLL cells and BMSCs has till now not been presented. We show here that the secretion of the primary activating cytokine TNF-α is induced by co-culturing CLL cells and BMSCs, and the main source are the CLL cells. The other primary cytokine, IL-1β, was marginally detectable but its secretion increased also strongly in the co-culture. TNF-α acts as an autocrine and paracrine growth factor on CLL cells, and it also stimulates BMSCs to secrete cytokines as, for example, IL-8 [39, 40]. Additionally, significantly higher TNF-α concentration was observed recently in CLL cells of the bone marrow compared to those from peripheral blood, which also emphasizes the different behavior of CLL cells in the presence of stroma cells [32]. IL-6 and IL-8 are known activatory survival cytokines, and we could demonstrate that the presence of CLL cells induce robust secretion of IL-6 and IL-8 by BMSCs. IL-8 secretion of BMSCs is likely to be induced by TNF-α secreted by the CLL cells, whereas the secretion of IL-6 is probably triggered by direct adhesion, similarly as by multiple myeloma cells [40, 41]. Despite the increased level of IL-8 in the supernatant, the mRNA expression was not induced either in BMSCs or in CLL cells, concomitantly with previous findings, which reported constitutive mRNA expression by active secretion [36]. In clinical trials, the plasma levels of inflammatory cytokines as IL-6 and angiogenic factors as IL-8 showed a tight association with the response to lenalidomide justifying their importance in the pathogenesis of CLL [13]. Recent findings also indicate the potential of novel therapeutic strategies targeting the IL-8-dependent pathway [42]. These results suggest that CLL cells may act in a paracrine and in an autocrine manner in the stromal microenvironment in order to enhance their own survival.
B lymphocytes and dendritic cells can bind activated T cells through CD40–CD154 (CD40L). In the current experimental setup, CD40L did not exert any additional effect on the survival of CLL cells in co-culture with BMSCs. The missing anti-apoptotic effect of CD40L can be explained with the lack of a direct effect on CLL cells and stimulating effect on BMSCs; hence, neither the mRNA of adhesion molecules nor the secretion of cytokines was up-regulated. T cells, however, are able to activate CLL cells through complex interactions, mediated by a series of interacting molecules (CD58–CD2, CD27–CD70, CD11a–CD54) and T cell-derived cytokines, such as IL-2 [43]. An immunohistochemical study highlighted that bone marrow stromal elements expressed CD40 in conjunction with B cell lymphomas, which suggests a direct interaction between T cells and stromal cells [16]. We found that CLL cells induced CD40 expression on BMSCs and therefore may enhance the interaction between BMSCs and T lymphocytes. When CD40L engages CD40 on dendritic cells, it stimulates the expression of B7 molecule and the secretion of cytokines that activate T cells [44].
In conclusion, our results demonstrate a crosstalk between CLL cells and BMSCs in which CLL cells are able to influence the stromal microenvironment by inducing the expression of adhesion molecules and increasing the secretion of vital cytokines to facilitate apoptosis resistance. CLL cells simultaneously up-regulate adhesion molecule ligands on their own surface to further enhance the interaction with BMSCs. These data give rationales for the interruption of stroma–CLL cells interaction in drug therapy and may explain the successful application of thalidomide and its derivative lenalidomide even in refractory CLL cases [12, 13].
References
Kay NE, Hamblin TJ, Jelinek DF, Dewald GW, Byrd JC, Farag S et al (2002) Chronic lymphocytic leukemia. Hematology Am Soc Hematol Educ Program 193–213
Kitada S, Andersen J, Akar S, Zapata JM, Takayama S, Krajewski S et al (1998) Expression of apoptosis-regulating proteins in chronic lymphocytic leukemia: correlations with in vitro and in vivo chemoresponses. Blood 91(9):3379–3389
Collins RJ, Verschuer LA, Harmon BV, Prentice RL, Pope JH, Kerr JF (1989) Spontaneous programmed death (apoptosis) of B-chronic lymphocytic leukaemia cells following their culture in vitro. Br J Haematol 71(3):343–350
Lagneaux L, Delforge A, Bron D, de Bruyn C, Stryckmans P (1998) Chronic lymphocytic leukemic B cells but not normal B cells are rescued from apoptosis by contact with normal bone marrow stromal cells. Blood 91(7):2387–2396
Jewell AP, Lydyard PM, Worman CP, Giles FJ, Goldstone AH (1995) Growth factors can protect B-chronic lymphocytic leukaemia cells against programmed cell death without stimulating proliferation. Leuk Lymphoma 18:159–162
Reittie JE, Yong KL, Panayiotidis P, Hoffbrand AV (1996) Interleukin-6 inhibits apoptosis and tumour necrosis factor induced proliferation of B-chronic lymphocytic leukaemia. Leuk Lymphoma 22:83–90
Schröttner P, Leick M, Burger M (2010) The role of chemokines in B-cell chronic lymphocytic leukemia cells: pathophysiological aspects and clinical impact. Ann Hematol 89(5):437–446
König A, Menzel T, Lynen S, Wrazel L, Rosén A, Al-Katib A, Raveche E, Gabrilove JL (1997) Basic fibroblast growth factor (bFGF) upregulates the expression of bcl-2 in B cell chronic lymphocytic leukemia cell lines resulting in delaying apoptosis. Leukemia 11(2):258–265
Kay NE, Bone ND, Tschumper RC, Howell KH, Geyer SM, Dewald GW, Hanson CA, Jelinek DF (2002) B-CLL cells are capable of synthesis and secretion of both pro- and anti-angiogenic molecules. Leukemia 16(5):911–919
Molica S, Vacca A, Ribatti D, Cuneo A, Cavazzini F, Levato D et al (2002) Prognostic value of enhanced bone marrow angiogenesis in early B-cell chronic lymphocytic leukemia. Blood 100(9):3344–3351
Kay NE, Shanafelt TD, Strege AK, Lee YK, Bone ND, Raza A (2007) Bone biopsy derived marrow stromal elements rescue chronic lymphocytic leukemia B-cells from spontaneous and drug induced cell death and facilitates an “angiogenic switch”. Leuk Res 31(7):899–906
Chanan-Khan A, Miller KC, Takeshita K, Koryzna A, Donohue K, Bernstein ZP et al (2005) Results of a phase 1 clinical trial of thalidomide in combination with fludarabine as initial therapy for patients with treatment-requiring chronic lymphocytic leukemia (CLL). Blood 106(10):3348–3352
Ferrajoli A, Lee BN, Schlette EJ, O'Brien SM, Gao H, Wen S et al (2008) Lenalidomide induces complete and partial remissions in patients with relapsed and refractory chronic lymphocytic leukemia. Blood 111(11):5291–5297
Schmid C, Isaacson PG (1994) Proliferation centres in B-cell malignant lymphoma, lymphocytic (B-CLL): an immunophenotypic study. Histopathology 24(5):445–451
Ghia P, Strola G, Granziero L, Geuna M, Guida G, Sallusto F et al (2002) Chronic lymphocytic leukemia B cells are endowed with the capacity to attract CD4+, CD40L+ T cells by producing CCL22. Eur J Immunol 32(5):1403–1413
Vega F, Medeiros LJ, Lang WH, Mansoor A, Bueso-Ramos C, Jones D (2002) The stromal composition of malignant lymphoid aggregates in bone marrow: variations in architecture and phenotype in different B-cell tumours. Br J Haematol 117(3):569–576
Plander M, Seegers S, Ugocsai P, Diermeier-Daucher S, Iványi J, Schmitz G, Hofstädter F, Schwarz S, Orsó E, Knüchel R, Brockhoff G (2009) Different proliferative and survival capacity of CLL-cells in a newly established in vitro model for pseudofollicles. Leukemia 23(11):2118–2128
Haniffa MA, Collin MP, Buckley CD, Dazzi F (2009) Mesenchymal stem cells: the fibroblasts' new clothes? Haematologica 94:258–263
Panayiotidis P, Jones D, Ganeshaguru K, Foroni L, Hoffbrand AV (1996) Human bone marrow stromal cells prevent apoptosis and support the survival of chronic lymphocytic leukaemia cells in vitro. Br J Haematol 92(1):97–103
Lagneaux L, Delforge A, De Bruyn C, Bernier M, Bron D (1999) Adhesion to bone marrow stroma inhibits apoptosis of chronic lymphocytic leukemia cells. Leuk Lymphoma 35(5–6):445–453
Burger JA, Burger M, Kipps TJ (1999) Chronic lymphocytic leukemia B cells express functional CXCR4 chemokine receptors that mediate spontaneous migration beneath bone marrow stromal cells. Blood 94(11):3658–3667
Shanafelt TD, Geyer SM, Bone ND, Tschumper RC, Witzig TE, Nowakowski GS et al (2008) CD49d expression is an independent predictor of overall survival in patients with chronic lymphocytic leukemia: a prognostic parameter with therapeutic potential. Br J Haematol 140(5):537–546
Weber KS, Klickstein LB, Weber C (1999) Specific activation of leukocyte beta2 integrins lymphocyte function-associated antigen-1 and Mac-1 by chemokines mediated by distinct pathways via the alpha subunit cytoplasmic domains. Mol Biol Cell 10(4):861–873
Röpke C, Gladstone P, Nielsen M, Borregaard N, Ledbetter JA, Svejgaard A, Odum N (1996) Apoptosis following interleukin-2 withdrawal from T cells: evidence for a regulatory role of CD18 (beta 2-integrin) molecules. Tissue Antigens 48(2):127–135
Wagner C, Hänsch GM, Stegmaier S, Denefleh B, Hug F, Schoels M (2001) The complement receptor 3, CR3 (CD11b/CD18), on T lymphocytes: activation-dependent up-regulation and regulatory function. Eur J Immunol 31(4):1173–1180
Hulkkonen J, Vilpo J, Vilpo L, Koski T, Hurme M (2000) Interleukin-1 beta, interleukin-1 receptor antagonist and interleukin-6 plasma levels and cytokine gene polymorphisms in chronic lymphocytic leukemia: correlation with prognostic parameters. Haematologica 85(6):600–606
Meinhardt G, Wendtner CM, Hallek M (1999) Molecular pathogenesis of chronic lymphocytic leukemia: factors and signaling pathways regulating cell growth and survival. J Mol Med 77(2):282–293, Review
Springer TA (1994) Traffic signals for lymphocyte recirculation and leukocyte emigration: the multistep paradigm. Cell 76(2):301–314
Burger JA, Kipps TJ (2006) CXCR4: a key receptor in the crosstalk between tumor cells and their microenvironment. Blood 107(5):1761–1767
Fayad L, Keating MJ, Reuben JM, O'Brien S, Lee BN, Lerner S, Kurzrock R (2001) Interleukin-6 and interleukin-10 levels in chronic lymphocytic leukemia: correlation with phenotypic characteristics and outcome. Blood 97(1):256–263
Jewell AP, Worman CP, Giles FJ, Goldstone AH (1997) Serum levels of TNF, IL-6 and sCD23 correlate with changes in lymphocyte count in patients with B-cell chronic lymphocytic leukaemia receiving interferon-alpha therapy. Leuk Lymphoma 24(3–4):327–333
Bojarska-Junak A, Hus I, Szczepanek EW, Dmoszyńska A, Roliński J (2008) Peripheral blood and bone marrow TNF and TNF receptors in early and advanced stages of B-CLL in correlation with ZAP-70 protein and CD38 antigen. Leuk Res 32(2):225–233
Wierda WG, Johnson MM, Do KA, Manshouri T, Dey A, O’Brien S et al (2003) Plasma interleukin 8 level predicts for survival in chronic lymphocytic leukaemia. Br J Haematol 120(3):452–456
Kara IO, Sahin B, Gunesacar R (2007) Expression of soluble CD27 and interleukins-8 and -10 in B-cell chronic lymphocytic leukemia: correlation with disease stage and prognosis. Adv Ther 24(1):29–40
Ennas MG, Moore PS, Zucca M, Angelucci E, Cabras MG, Melis M et al (2008) Interleukin-1B (IL1B) and interleukin-6 (IL6) gene polymorphisms are associated with risk of chronic lymphocytic leukaemia. Hematol Oncol 26(2):98–103
di Celle PF, Carbone A, Marchis D, Zhou D, Sozzani S, Zupo S, Pini M, Mantovani A, Foa R (1994) Cytokine gene expression in B-cell chronic lymphocytic leukemia: evidence of constitutive interleukin-8 (IL-8) mRNA expression and secretion of biologically active IL-8 protein. Blood 84(1):220–228
Zheng Z, Venkatapathy S, Rao G, Harrington CA (2002) Expression profiling of B cell chronic lymphocytic leukemia suggests deficient CD1-mediated immunity, polarized cytokine response, altered adhesion and increased intracellular protein transport and processing of leukemic cells. Leukemia 16(12):2429–2437
Stratowa C, Löffler G, Lichter P, Stilgenbauer S, Haberl P, Schweifer N, Döhner H, Wilgenbus KK (2001) CDNA microarray gene expression analysis of B-cell chronic lymphocytic leukemia proposes potential new prognostic markers involved in lymphocyte trafficking. Int J Cancer 91(4):474–480
Cordingley FT, Bianchi A, Hoffbrand AV, Reittie JE, Heslop HE, Vyakarnam A, Turner M, Meager A, Brenner MK (1988) Tumour necrosis factor as an autocrine tumour growth factor for chronic B-cell malignancies. Lancet 1(8592):969–971
Lisignoli G, Toneguzzi S, Pozzi C, Piacentini A, Grassi F, Ferruzzi A, Gualtieri G, Facchini A (1999) Chemokine expression by subchondral bone marrow stromal cells isolated from osteoarthritis (OA) and rheumatoid arthritis (RA) patients. Clin Exp Immunol 116(2):371–378
Chauhan D, Uchiyama H, Akbarali Y, Urashima M, Yamamoto K, Libermann TA, Anderson KC (1996) Multiple myeloma cell adhesion-induced interleukin-6 expression in bone marrow stromal cells involves activation of NF-kappa B. Blood 87(3):1104–1112
Binsky I, Haran M, Starlets D, Gore Y, Lantner F, Harpaz N et al (2007) IL-8 secreted in a macrophage migration-inhibitory factor- and CD74-dependent manner regulates B cell chronic lymphocytic leukemia survival. Proc Natl Acad Sci USA 104(33):13408–13413
Tretter T, Schuler M, Schneller F, Brass U, Esswein M, Aman MJ, Huber C, Peschel C (1998) Direct cellular interaction with activated CD4 T cells overcomes hyporesponsiveness of B-cell chronic lymphocytic leukemia in vitro. Cell Immunol 189(1):41–50
Abbas AK, Lichtman AH (2005) Cellular and molecular immunology, 5th edn. Elsevier Saunders, Philadelphia, PA, USA, p 173
Acknowledgements
We would like to thank Prof. Kreuser, Department of Oncology and Hematology, Barmherzige Brüder Hospital, Regensburg for providing the patient samples. We thank Birgit Wilhelm and Harry Isslinger for their excellent technical assistance.
Funding
This work was supported by grants from the the Catholic Academic Exchange Service (KAAD), the Bavarian Research Foundation (BFS), the German Research Foundation SFB Transregio-13 Project, the Fraunhofer Project Group Regensburg and the LipidomicNet (FP7-HEALTH 2007-2.1.1.6-202272) project.
Author information
Authors and Affiliations
Corresponding author
Additional information
Márk Plander and Peter Ugocsai contributed equally to the manuscript.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplemental Fig. 1
Characterization of BMSCs. a Immunohistochemistry of BMCSs is positive for vimentin, but not for CD68 b mRNA expression in stromal cells. Bar graphs indicate high expression of VCAM-1, CXCL12, ICAM1, IL-6, and IL-8 and less, but detectable IL-1β, CD40, TNF-α. c Surface expression of antigens on stromal cells; mAb (black line), isotype control (broken line). d Secreted cytokines in supernatant. IL-6 and IL-8 is actively secreted, IL-1β and TNF-α to a lesser extent. Results for each mRNA expression and cytokine concentration are presented as mean ± percentiles of at least five independent experiments (PDF 130 kb)
Rights and permissions
About this article
Cite this article
Plander, M., Ugocsai, P., Seegers, S. et al. Chronic lymphocytic leukemia cells induce anti-apoptotic effects of bone marrow stroma. Ann Hematol 90, 1381–1390 (2011). https://doi.org/10.1007/s00277-011-1218-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-011-1218-z