Abstract
We studied the serum phosphorus (P) level of 110 patients with multiple myeloma (MM) (age range 42–83 years, median 62 years) and evaluated the relationship between that and other prognostic factors. Serum P level significantly correlated with the prognostic factors that are relevant to renal dysfunction: serum creatinine (P<0.00000001), serum β2-microglobulin (P=0.00000088), serum uric acid (P=0.0000014), and corrected serum calcium (cCa P=0.000067). Although it also correlated with the percentage of plasma cells in bone marrow nucleated cells (BMPC%) and the hemoglobin (Hb) and leukocyte counts, the significance was less than for the other four prognostic factors. Serum creatinine, BMPC%, leukocyte count, serum uric acid, bone lesions, β2-microglobulin, and serum cCa were all significantly higher and Hb significantly was lower in the MM patients with hyperphosphatemia (serum P>3.8 mg/dl). The survival time was significantly shorter in these patients (P=0.000087). Multivariate analysis (Cox’s proportional hazards regression model) showed that the serum P level is a significant negative prognostic factor in MM patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Phosphorus (P) is one of the most abundant constituents of tissues, and approximately 85% of the total amount of P in the normal adult is in the skeleton [1]. Most of the P in the plasma is present as inorganic orthophosphate and only about 12% is bound to protein. In multiple myeloma (MM), hyperphosphatemia may result either from inadequate clearance during severe renal failure or from osteolytic bone destruction.
There are several case reports of MM in which pseudohyperphosphatemia caused by hypergammaglobulinemia had been found [2, 3]. In those patients, there was a correlation between the serum level of P and myeloma protein (M-protein), and the pseudohyperphosphatemia resulted from an increase in optic density caused by interference between the M-protein and the molybdic reagent used to determine P in serum [4–8].
The prognostic significance of the serum P level in MM has not been evaluated. In the present study, we measured the serum inorganic phosphorus (iP) level by a method that is not based on the reaction between ammonium molybdate and inorganic phosphorus and also examined the prognostic significance of the baseline serum P levels.
Materials and methods
Patients and treatment
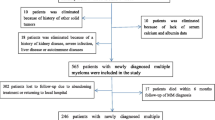
The study group was comprised of 110 patients with MM who underwent treatment in hospital between 1988 and 2003 [57 males, 53 females; median age 63 years (range 42–83)]. The diagnosis of MM was based on the diagnostic criteria of the Leukemia–Myeloma Taskforce (NCI 1973, [9]). The types of MM were IgG type in 62 patients (IgGκ in 45 and IgGλ in 17), IgA type in 32 (IgAκ in 21 and IgAλ in 11), Bence–Jones (BJ) type in 14 (BJκ in 11 and BJλ in three), and IgDκ in one patient. One patient had a non-secretory myeloma (BJλ). The clinical stage of the disease, according to Durie and Salmon’s criteria [10], was stage IA in five, stage IIA in 28, stage IIB in one, stage IIIA in 58, and stage IIIB in 18.
The survival time from the initiation of therapy was known in 97 cases and was used for the evaluation of the significance of prognostic factors. The initial chemotherapy regimen in 49 patients was VCAP [11], comprising of vincristine (2 mg/person, intravenously, day 1), cyclophosphamide (100 mg/m2/day, orally, days 1–4), adriamycin (25 mg/m2/day, intravenously, day 1), and prednisolone (60 mg/m2/day, orally, days 1–4); VCAP with interferon-α (IFN-α) in 21; VCAP/MVMP [MCNU (ranimustine), vincristine, melphalan and prednisolone] chemotherapy (alternating VCAP and MVMP regimens) in 13; and VCAP/MVMP chemotherapy plus IFN-α in nine. The MVMP regimen comprises MCNU (30 mg/m2, intravenous infusion, day 1), vincristine (2 mg, intravenously, day 1), melphalan (4 mg/m2/day, orally, days 1–4), and prednisolone (60 mg/m2/day, orally, days 1–4). The VCMP, VCP, and MP regimens were used in one patient each [VCMP regimen: vincristine (2 mg/person, intravenously, day 1), cyclophosphamide (100 mg/m2/day, orally, days 1–4), melphalan (4 mg/m2/day, orally, days 1–4), and prednisolone (60 mg/m2/day, orally, days 1–4); MP regimen: melphalan (4 mg/m2/day, orally, days 1–4), and prednisolone (60 mg/m2/day, orally, days 1–4)]. No patients underwent stem cell transplantation.
Blood chemistry
The serum P level at the time of diagnosis of MM was evaluated for its prognostic importance, and other clinical parameters determined as significant prognostic factors by univariate analysis (log-rank method) [12] [i.e., corrected serum calcium (serum cCa), serum creatinine, serum uric acid, serum albumin, total cholesterol, serum lactate dehydrogenase (serum LDH), serum β2-microglobulin, percentage of plasma cells in bone marrow nucleated cells (BMPC%), hemoglobin (Hb), leukocyte count, serum immunoglobulin M (IgM), grade of bone lesions (Durie–Salmon scale) [10], and age (years)] were evaluated for their prognostic importance.
The iP level was measured by IatroLQ IP diagnostic kit (Mitsubishi Chemistry Iatron, Tokyo) because it uses purine nucleoside phosphorylase, xanthine peroxidase, and peroxidase in an enzymatic method so is not based on the reaction between ammonium molybdate and iP. The normal level of serum iP measured in a Hitachi autoanalyzer by this method ranges between 2.5 and 3.8 mg/dl.
The serum concentration of Ca was corrected using serum albumin according to the formula of Payne et al. [13]:
The grade of bone lesion was evaluated by the Durie–Salmon scale [10]. Correlations between the serum P level and other prognostic factors were examined by Pearson’s correlation test. The relationship between the serum levels of P and M-protein (serum IgG concentration in IgG type MM patients and serum IgA concentration in IgA type MM patients) was also evaluated.
The difference in the average of the laboratory data between the patients with MM complicated by hyperphosphatemia (serum P >3.8 mg/dl) at first hospitalization and those without hyperphosphatemia was evaluated by Student’s t test, and the median survival time was calculated by Kaplan–Meier’s method [14]. The significance of difference of the survival curves was estimated by log-rank test [12].
Multivariate analysis to define independent prognostic factors used Cox’s proportional hazards regression model [15].
Results
Of the 110 patients with MM, 36 (32.7%) had hyperphosphatemia (serum P >3.8 mg/dl) and 12 (11%) had a serum P level greater than 5 mg/dl. One patient had profound hypophosphatemia (serum P 1.1 mg/dl), hypercalcemia, moderately increased serum Ig (6,621 mg/dl of IgGκ) and positive urine Bence–Jones protein, but the serum creatinine level was almost normal (1.1 mg/dl).
According to Pearson’s correlation test, the serum P level significantly correlated with the prognostic factors related to renal dysfunction; that is, serum creatinine (r=0.636, P<0.00000001), serum β2-microglobulin (r=0.545, P=0.00000088), serum uric acid (r=0.429, P=0.0000014), and serum cCa (r=0.356, P=0.000067) (Table 1). Although it also correlated with BMPC% (P=0.0011), Hb (P=0.0028), and the leukocyte count (P=0.0032), these correlations were less than for the other four prognostic factors. Serum P did not correlate with age, albumin, serum LDH, or total cholesterol.
Because of the concern that high M-protein levels might result in pseudohyperphosphatemia, we investigated whether there was any relationship between the M-protein and serum P levels. No significant correlation between the serum P levels and serum IgG levels in IgG-type MM patients or with the serum IgA levels in IgA type MM patients was observed.
The difference in the average of the laboratory data between the MM patients complicated with hyperphosphatemia (serum P ≥3.8 mg/dl) at first hospitalization and those without hyperphosphatemia (serum P <3.8 mg/dl) was examined (Table 2). The average of serum creatinine in the hyperphosphatemic group (2.08±1.99 mg/dl) was significantly higher than that in the non-hyperphosphatemic group (1.04±0.692 mg/dl) (P=0.00012). Furthermore, the BMPC% (P=0.0038), leukocyte count (P=0.0061), serum uric acid (P=0.0068), bone lesions (P=0.011), serum β2-microglobulin (P=0.017), Hb (P=0.031), and serum cCa (P=0.037) were also significantly different between the two groups.
As to the prognostic significance of the serum P level, the survival time was significantly shorter in MM patients with hyperphosphatemia (median survival 26 months) than in those without (92 months) (P=0.000432) (Fig. 1, Table 3). Of the other prognostic factors, BMPC% (P=0.000515), serum cCa (P=0.000775), serum β2-microglobulin (P=0.00298), serum LDH (P=0.00445), Hb (P=0.00520), age (P=0.00619), and serum creatinine (P=0.00671) were significant prognostic factors for MM. CRP (P=0.0129), IgM (P=0.0240), serum uric acid (P=0.0272), total cholesterol (P=0.0312), urine BJ-protein (P=0.0438), and albumin (P=0.0485) were slightly significant prognostic factors (Table 3). Overall, the serum P level was the most significant of the prognostic factors we examined by univariate analysis.
Multivariate analysis using BMPC%, serum cCa, serum P, serum β2-microglobulin, serum LDH, Hb, age, creatinine, CRP, IgM, serum uric acid, total cholesterol, urine BJ-protein, and albumin revealed that age (χ 2=16.46, P=0.0000496) was the most significant factor, followed by serum cCa level (χ 2=14.04, P=0.000179), serum P level (χ 2=6.552, P=0.0105), and percentage of plasma cells in bone marrow (χ 2=6.080, P=0.0136) (Table 4).
Discussion
Hyperphosphatemia is caused by decreased filtration by the kidney, hyperparathyroidism, hyperthyroidism, increased loading of P, anti-acid drug, diet, and acute destruction of any tissue. There are no symptoms related directly to hyperphosphatemia, unless high levels are maintained for long periods. The serum P level significantly correlates with serum creatinine (P<0.00000001), serum β2-microglobulin (P=0.00000088), serum uric acid (P=0.0000014), and serum cCa (P=0.000067), and these prognostic factors may be strongly influenced by disturbed renal function. The serum creatinine level increases with renal dysfunction, and an increase in the serum levels of β2-microglobulin and uric acid is related to both renal dysfunction and the volume of the myeloma. Serum cCa may be influenced by renal dysfunction and bone lesions, and serum P level also correlates with BMPC%, Hb, and bone lesions, which are factors that may also reflect the volume of tumor. However, in the present study, the correlations between serum P level and the three latter prognostic factors were less than with the four prognostic factors that are related to renal dysfunction. The patients with hyperphosphatemia also had higher values for serum creatinine, serum uric acid, serum cCa level and BMPC% than those without hyperphosphatemia, as well as having anemia and thrombocytopenia. Therefore, the serum P level is influenced mainly not only by renal dysfunction but also by the grade of tumor burden and disease progression.
Several cases of MM with hyperphosphatemia have been reported, but in most those cases, it was spurious.[4, 6, 7, 16–18] Busse et al. [4] reported two cases of IgG type MM complicated with pseudohyperphosphatemia, which was caused by interference of the monoclonal gammaglobulins with the phosphomolybdate colorimetric assay. Subsequent ultrafiltration of the serum samples resulted in normalization of the P values. Oren et al. [7] reported that in three patients with MM and pseudohyperphosphatemia, there was a correlation between the serum P level and the amount of M-protein and that pseudohyperphosphatemia resulted from an increase in optic density caused by interference between the M-protein and the molybdic reagent used to determine P in serum. In all cases, the M-protein was IgG. The mechanism underlying this spurious result may be turbidity in the reaction mixture caused by acid precipitation of the monoclonal IgG protein in the new generation of simplified kits or in some automated systems. Another explanation is possible binding of a large amount of P by the M-protein [2, 3]. Spurious hyperphosphatemia might be considered in newly diagnosed MM patients with increased serum P level but normal renal function and minimal skeletal disease. Most of the present patients with hyperphosphatemia had increased serum creatinine, hypercalcemia, and an advanced stage of MM, which suggests that most of the cases of hyperphosphatemia in these patients were induced by renal failure or lytic bone lesions.
One of the MM patients had profound hypophosphatemia, hypercalcemia, moderately increased serum immunoglobulin level, subnormal serum creatinine, and positive Bence–Jones protein. Several cases of spurious hypophosphatemia caused by the presence of M-protein have been reported [19–23]. Dash et al. [21] reported profound hypophosphatemia and isolated hypersphosphaturia, and Engle and Wallis [23] reported renal tubular defects when there is Fanconi’s syndrome in MM. The mechanism of tubular dysfunction is unknown but may be related to the deposition of monoclonal light chains as crystalline inclusions within proximal tubular cells [24].
A number of prognostic factors for MM have been found and several prognostic systems have been proposed since 1973. Among the prognostic factors identified are bone lesion scale [10], monoclonal protein [10, 25], serum cCa [10, 25, 26], hemoglobin [10, 25, 26, 29, 30], serum creatinine [10, 25, 26, 29, 30], performance state [27, 29], albumin [27, 28, 31–33], blood urea nitrogen [28], BMPC% [26], paraprotein index [29], platelet count [30], Durie–Salmon clinical stage [30], lytic bone lesions [30], age [30], serum β2-microglobulin [31–33], morphology of the myeloma cells [31], and serum LDH. However, to date, the prognostic significance of the serum P level in MM has not been previously reported and, in the present study population, it was a significant negative prognostic factor.
References
Holick MF, Krane SM, Potts JT (1987) Phosphorus, disorders of bone and mineral metabolism. In: Braunwald E, Isselbacher KJ, Petersdorf RG, Wilson JD, Martin JB, Fauci AS (eds) Harrison’s principles of internal medicine, 11th edn. McGraw-Hill, New York, pp 1859–1860
Pettersson T, Hortling L, Teppo AM, Toetterman KJ, Fyhrquist F (1987) Phosphate binding by a myeloma protein. Acta Med Scand 222:89–91
Mandry JM, Posner MR, Tucci JR, Eil C (1991) Hyperphosphatemia in multiple myeloma due to a phosphate-binding immunoglobulin. Cancer 68:1092–1094
Busse JC, Gelhard MA, Byrenes JJ, Hellman R, Vaamonde CA (1987) Pseudohyperphosphatemia and dysproteinemia. Arch Intern Med 147:2045–2046
Sonnenblick M, Eylath U, Brisk R, Eldad C, Hershko C (1986) Paraprotein interference with colorimetry of phosphate in serum of some patients with multiple myeloma. Clin Chem 32:1537–1539
Adler SG, Laidlaw SA, Lubran MM, Kopple JD (1988) Hyperglobulinemia may spuriously elevate measured serum inorganic phosphate levels. Am J Kidney Dis 11:260–263
Oren S, Feldman A, Turkot S, Lugassy G (1994) Hyperphosphatemia in multiple myeloma. Ann Hematol 69:41–43
Marcu CB, Hotchkiss M (2004) Pseudohyperphosphatemia in a patient with multiple myeloma. Conn Med 68:71–77
Chronic Leukemia–Myeloma Taskforce, National Cancer Institute (1973) Proposed guidelines for protocol studies 11. Plasma cell myeloma. Cancer Chemother Rep 3 4:145–158
Durie BGM, Salmon SE (1975) A clinical staging system for multiple myeloma. Cancer 36:842–854
Alexanian R, Salmon S, Bonnet J, Gehan E, Haut A, Weick J (1977) Combination therapy for multiple myeloma. Cancer 40:2765–2771
Peto, R, Pike MC, Armitage P, Breslow NE, Cox DR, Howard SV, Mantel N, McPherson K, Peto J, Smith PG (1977) Design and analysis of randomized clinical trials requiring prolonged observation of each patient II: analysis and examples. Br J Cancer 35:l–39
Payne RB, Little AJ, Williams RB, Milner JR (1973) Interpretation of serum calcium in patients with abnormal proteins. BMJ 4:643–646
Kaplan EL, Meier P (1958) Nonparametric estimation from incomplete observations. J Am Stat Assoc 53:457–481
Cox DR (1972) Regression models and life tables. J R Stat Soc 34:187–196
Weinberg J, Adler AJ (1989) Spurious hyperphosphatemia in patients with dysglobulinemia. Miner Electrolyte Metab 15:185–186
McCloskey EV, Galloway J, Morgan MA, Kanis JA (1989) Pseudohyperphosphatemia in multiple myeloma. BMJ 299:1381–1382
Barutcuoglu B, Parildar Z, Mutaf I, Habif S, Bayindir O (2003) Spuriously elevated inorganic phosphate level in a multiple myeloma patient. Clin Lab Haematol 25:271–274
Loghman-Adham M, Walton D, Iverius PH, Deiss A, Knight JA, Cheung AK (1997) Spurious hypophosphatemia in a patient with multiple myeloma. Am J Kidney Dis 30:571–575
Caras JA (1997) Spurious hypophosphatemia associated with multiple myeloma. Endocr Pract 3:135–136
Dash T, Parker MG, Lafayettw RA (1997) Profound hypophosphatemia and isolated hyperphosphaturia in two case of multiple myeloma. Am J Kidney Dis 29:445–448
Weisbord SD, Chaudhuri A, Blauth K, DeRubertis FR (2003) Monoclonal gammopathy and spurious hypophosphatemia. Am J Med Sci 325:98–100
Engle RL Jr, Wallis LA (1957) Multiple myeloma and the adult Fanconi syndrome. Am J Med 22:5–18
Smithline N, Kassirer JP, Cohen JJ (1976) Light-chain nephropathy: renal tubular dysfunction associated with light-chain proteinuria. N Engl J Med 294:71–74
Alexanian R, Balgerzak S, Bonnet JD, Gehan EA, Haut A, Hewlett JS, Monto RW (1975) Prognostic factors in multiple myeloma. Cancer 36:1192–1201
Merlini G, Waldenström JG, Jayakar SD (1980) A new improved clinical staging system for multiple myeloma based on analysis of 123 treated patients. Blood 55:1011–1019
Medical Research Council (1973) Report on the first myelomatosis trial. Part 1. Analysis of presenting features of prognostic importance. Br J Haematol 24:123–139
Bladé J, Rozman C, Cervantes F, Reverter J-C, Montserat E (1989) A new prognostic system for multiple myeloma based on easily available parameters. Br J Haematol 172:507–511
San Miguel JF, Sànchez J, Gonzalez M (1989) Prognostic factors and classification in multiple myeloma. Br J Haematol 59:113–118
Cavo M, Galieni P, Zuffa E, Baccarani M, Gobbi M, Tura S (1989) Prognostic variables and clinical staging in multiple myeloma. Blood 74:1774–1780
Murakami H, Kawada T, Saitoh T, Uchiumi H, Moridaira K, Matsushima T, Tsukamoto N, Tamura J, Morita K, Sawamura M, Karasawa M, Miyawaki S, Shinonome S, Shimano S, Sato S, Ogawara H, Tsuchiya J (1999) A staging system for multiple myeloma based on the morphology of myeloma cells. Eur J Haematol 62:63–67
Jacobson JL, Hussein MA, Barlogie B, Durie BGM, Crowley JJ (2003) A new staging system for multiple myeloma patients based on the Southwest Oncology Group (SWOG) experience. Br J Haematol 122:441–450
Durie BMG, Kyle RA, Belch A, Bensinger W, Bladé J, Boccadoro M, Child JA, Comenzo R, Djulbegovic B, Fantl D, Gahrton G, Harousseau JL, Mehta J, Morales AR, Morgan G, Nouel A, Oken M, Poweles R, Singhal DS, Sirohi B, Sonnenveld P, Tricot G, Ness BV (2003) Myeloma management guidelines: a consensus report from the scientific advisors of the International Myeloma Foundation. Hematol J 4:379–398
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Umeda, M., Okuda, S., Izumi, H. et al. Prognostic significance of the serum phosphorus level and its relationship with other prognostic factors in multiple myeloma. Ann Hematol 85, 469–473 (2006). https://doi.org/10.1007/s00277-006-0095-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-006-0095-3