Abstract
Uterine leiomyomata, or fibroids, although benign, cause debilitating symptoms in many women. Symptoms are often nonspecific and may be the presenting complaint in a number of other conditions. Furthermore, because the presence of fibroids may be coincident with other symptomatic conditions that result in similar complaints, there may be diagnostic difficulty and consequent difficulty in planning therapeutic strategy. Uterine artery embolization (UAE) is a safe and effective treatment for symptomatic fibroids and is increasingly being performed. Magnetic resonance imaging (MRI) evaluation before and after treatment is routine practice with the potential to significantly alter management in up to a fifth of patients. It is well recognized that significant incidental findings may be demonstrated during imaging investigations, and in particular that abnormalities that are not directly related to the clinical question may be overlooked. Radiologists evaluating pre-UAE MRI studies must be aware of the MRI appearances of gynecological pathologies that may cause similar symptoms or that may affect the success or complication rates of UAE, and they must also be wary of “satisfaction of search,” reviewing imaging thoroughly so that relevant other pathologies are not missed. We demonstrate the appearances of coincidental pathologies found on pre-UAE MRI, with the potential to change patient management.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Uterine leiomyomata, or fibroids, although benign, cause debilitating symptoms in many women. They are the commonest tumor of the female reproductive system [1], occurring in at least 30% of women. Many options are now available for treatment of symptomatic fibroids. These include hormonal therapies (increasingly the Mirena coil), surgical approaches (hysterectomy, myomectomy, laparoscopic uterine artery occlusion), magnetic resonance imaging (MRI)-guided focused ultrasound, and uterine artery embolization (UAE) [2].
UAE is an increasingly popular choice. This is a safe, cost-effective alternative to hysterectomy, allowing uterine preservation [3]. UAE induces infarction of leiomyomata, with resolution of symptoms resulting from necrosis, degeneration and size reduction [4]. NICE guidance endorses the use of UAE as an alternative to hysterectomy or myomectomy for women with symptomatic fibroids measuring >3 cm who wish to retain fertility or who wish to avoid surgery [5].
Although many patients with fibroids are asymptomatic [6], up to 50% experience symptoms including abnormal bleeding, pain, pressure symptoms, dyspareunia, infertility, constipation, and urinary frequency. These symptoms are nonspecific and may be the manifesting complaint in a number of other conditions. Because fibroids may be coincident with other symptomatic conditions with similar complaints, there may be diagnostic difficulty. Symptomatic gynecological conditions most frequently overlooked include endometriosis, adenomyosis, pelvic congestion, and other tubal or ovarian pathologies [7]. In addition, nongynecological pathology may be relevant to the presentation.
With these diagnostic challenges in mind, MRI is performed before UAE in order to confirm the diagnosis and document uterine size, and to establish the number, size, and location of the fibroids—factors that may have an impact on patient suitability for UAE. There has been debate within the literature regarding factors that may influence outcome, including size and location of fibroids. MRI allows accurate assessment of size and position, including identification of a large submucous component or pedunculated subserous location. Both features appear to be associated with an increased risk of complications after UAE [8–10]. There have been concerns about safety and efficacy of UAE in the treatment of bulky fibroid disease, but an increasing number of follow-up studies demonstrate safe and successful treatment of patients with large (>10 cm) solitary fibroids and patients with multiple fibroids resulting in large uterine volume [11, 12].
MRI findings can change the management plan in approximately 20% of patients, allowing assessment for any secondary or alternative diagnoses such as adenomyosis or endometriosis that may influence the likelihood of successful response to treatment [13]. This information allows the patient to be counselled fully—for example, while patients may still opt for UAE with a diagnosis of adenomyosis, they will need to be made aware of the greater potential for clinical failure [13]. Similarly, on the basis of the known increased risk of infections developing in postsurgical patients who develop postoperative hematoma [14], there is a perception and concern that patients with endometriosis may be at increased risk of infection. Although this has not yet been substantiated by a review of the literature, at our institution, patients with endometriosis are counseled regarding the possibility of increased risk of infection.
It is also well recognized that significant incidental findings may be demonstrated during imaging investigations [15, 16], and in particular that abnormalities that are not directly related to the clinical question may be overlooked [17].
In our institution, standard T1 and T2 sagittal and axial sequences are performed. Where there it diagnostic difficulty, a second opinion may be sought from a gynecological radiologist before the patient consultation. A fat saturation sequence may be performed in addition to the standard sequences when blood or fat containing pathology is suspected after initial image review.
Contrast-enhanced MRI may provide additional information, with contrast-enhanced sequences used in many centers to evaluate the degree of fibroid enhancement as a predictor of response to treatment, but this not performed routinely in our institution as a result of time and cost pressures.
Magnetic resonance angiography (MRA) may be useful in the demonstration of ovarian artery supply to fibroids, which is a cause of treatment failure after UAE. Ovarian artery supply to uterine fibroids may be present in up to 8% [18]. Ovarian to uterine artery anastomosis can be classified at angiography into three groups [18]. In class 1 anastomoses, the ovarian artery anastomoses with the uterine artery proximal to the supply to the fibroid through the tubo-ovarian segment. These patients are unlikely to experience treatment failure as a result of the collateral supply because the embolization occurs distal to the anastomosis, although there is a risk of refluxing embolic material toward the ovary when tubal flow is low. In patients with type 2 collateral supply, the ovarian artery supplies the fibroid directly without prior anastomosis with the uterine artery; this cohort is at risk from incomplete infarction with UAE only. Patients with type 3 anastomoses demonstrate ovarian supply from the uterine artery, with flow toward the ovary from the tubal artery. These patients are at increased risk of ovarian failure and menopause after UAE. Visibility, size, and extension of the ovarian artery in the pelvis may be MRA markers for collateral supply, and in the study of Kroencke et al. [19], MRA had a reported sensitivity of 100% and specificity of 77% for depicting ovarian artery supply. This may be helpful in restricting subsequent aortography to those patients with a high suspicion of ovarian supply.
MRI is often also performed after treatment to assess response. There is evidence to suggest a correlation between percentage infarction and clinical outcome [20], with a higher chance of recurrent symptoms if significant enhancement persists. This may be particularly relevant in younger patients. At present in our institution, after UAE, patients are seen by the interventional radiologist for clinical and MRI assessment (using standard T1- and T2-weighted sequences) at 3 months and 1 year after the procedure, although we are moving to clinical assessment at 3 months and clinical and MRI assessments at 1 year. We reserve contrast-enhanced studies for those with treatment failure, which in our institution is <5% of the last 100 patients, with decisions regarding the need for further intervention being based on clinical success (symptoms) rather than technical success (based on extent of or lack of persisting enhancement).
With regard to postprocedural imaging, it is also important to note that imaging soon after UAE can be difficult to interpret. For example, the presence of gas may be normal after UAE and does not necessarily indicate infection.
Here we discuss and demonstrate examples of common pathologies that are of clinical importance because they may manifest in a similar way to fibroids, and that may be found coincidentally at pre-UAE MRI. We stress the importance of evaluating the entire study to avoid overlooking important coexistent or alternative pathology.
Gynecological Pathology
Endometriosis
Endometriosis is the presence of ectopic functional endometrial tissue, with the imaging findings occurring as a result of cyclical bleeding in the ectopic deposits. The most common site for endometriotic deposits are the ovaries, resulting in endometriomata, but implants may occur at any site within the pelvis; indeed, anywhere in the body may be affected. Endometriosis is seen in approximately 10% of the female population (with a considerably higher rate being seen in infertile women), affecting women of reproductive age [7]. Symptoms include dysmenorrhea, abnormal bleeding, and dyspareunia and may therefore overlap with symptoms resulting from fibroids. The classic MRI findings are the result of the presence of blood products and result in cystic masses that return high T1 and low T2 signal (known as shading, which may be seen as a layering phenomenon or throughout the cyst) [21], but appearances are variable, and as a result of the presence of blood products of varying ages, a combination of signal intensities may be seen. A fat saturation sequence is required when ovarian masses are of high T1 signal intensity to exclude teratoma. Endometriomata typically return hyperintense signal after fat saturation, as opposed to the signal loss seen in teratodermoid. The recurrent hemorrhage may result in pelvic adhesions and scarring with tethered appearances, also appreciable at MRI.
Endometriosis is important to identify in pre-UAE patients because there may be an increased risk of infection. In our institution, an increased risk of 1–5% is quoted.
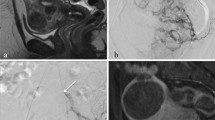
Figure 1 demonstrates shading and hyperintensity after fat saturation within a coincidental endometrioma detected at pre-UAE MRI.
A Sagittal T2-weighted pre-UAE image demonstrates dominant fibroid (F) within an enlarged uterus. An abnormal area of multiloculated low signal (arrow) is present posterior to the uterus. B Corresponding sagittal T1-weighted image demonstrates high signal within the lesion (arrow). C Axial T1-weighted image of the corresponding multiloculated cyst (arrow); high T1 and low T2 signal is known as shading. Also note interface vessels between fibroid and surrounding myometrium. D Axial T1 fat-saturated image demonstrating hyperintensity (arrow), confirming the presence of blood products
Adenomyosis
Adenomyosis is due to migration of endometrial glandular tissue from the endometrium into the myometrium. This results in smooth muscle hyperplasia around the glandular deposits. This is another common condition with hysterectomy specimens demonstrating evidence of adenomyosis in 5–70% [7]. Again, the common manifesting symptoms—pressure symptoms, dysmenorrhea, and menorrhagia—overlap with those commonly seen in patients with fibroids. The MRI finding, as a result of migration of endometrial glands and smooth muscle hyperplasia, is thickening of the low T2 signal uterine junctional zone. This may contain small foci of high T2 or T1 signal, representing cystic glandular dilation or hemorrhage, respectively. A uterine junctional zone measurement of ≥12 mm is diagnostic [7]. Figure 2 demonstrates the typical appearances.
Adenomyosis may be diffuse or focal, depending on the distribution of ectopic glands. When focal, there may be difficulty distinguishing between sub mucous fibroids and focal adenomyosis. The presence of multiple high T2 foci within adenomyosis may help make the distinction, although degenerating fibroids may also contain areas of high T2 or T1 signal. Another distinguishing feature is that fibroids are usually well defined, whereas in adenomyosis, the interface with myometrium is ill defined [22, 23]. In addition, prominent interface vessels at the margin of the mass in the uterus, which appear as signal void structures, may also aid the distinction; they are seen in association with fibroids but not in adenomyosis [6, 24]. Figures 3 and 4 illustrate the difficulties in distinguishing between focal adenomyosis and fibroids.
A Sagittal T2-weighted pre-UAE image demonstrates dominant fibroid (F) within enlarged uterus. B In the same patient, at the fundus, appearance suggests a thickened junctional zone, raising the question of additional adenomyosis (arrowheads). C Axial image before UAE confirms thickening of junctional zone posteriorly, but the lobulated outline anteriorly and possible interface vessel (arrowhead) raised the possibility of a fibroid as an alternative to focal adenomyosis. D Post-UAE T2-weighted image confirms mixed pathologies with a reduction in fibroid size, while the fundal abnormality containing multiple high T2 foci, representing adenomyosis, is more conspicuous
A Sagittal T2-weighted pre-UAE image demonstrates small posterior wall fibroid (arrow). Anteriorly, the ill-defined low signal (arrowheads) suggests adenomyosis. B Axial image with thickened junctional zone suggests adenomyosis, but the possible interface vessel would be more in keeping with fibroids. C Post-UAE T2-weighted sagittal image demonstrates the abnormality is smaller and well defined, and more in keeping with a fibroid
Although UAE may be useful in treating either condition, the success rate is lower for adenomyosis than for fibroids, and the distinction is important so that the patient may be counseled appropriately. In our institution a success rate for UAE of 50% for adenomyosis compared to 80–90% for fibroids is quoted.
Ovarian Cysts
Most of the ovarian cysts found in the premenopausal UAE population will be functional cysts. On the basis of the low risk of malignancy and the high prevalence of physiologic cysts in this group, as a general recommendation, simple cysts <2.5 cm in size usually do not require follow-up [25].
Malignancy more commonly occurs in the 50–70-year age group but may occur at any age. Ovarian cancer in the premenopausal population (i.e., those likely to be undergoing UAE) is rare, with an incidence in the region of 1–10,000 to 1–15,000. It is often asymptomatic at an early stage and may be an incidental finding. Simple, small (2–5 cm) unilateral, unilocular cysts have a very low risk of malignancy, and these can be usually be managed conservatively with followup ultrasound, providing the Ca-125 is normal [26]. Many of these cysts will resolve [25].
Previously undiagnosed larger (>5 cm) or complex cysts (cysts containing nonfatty solid elements, particularly thick or nodular septations, papillary projections, or mural nodularity), whether in a pre- or post-menopausal patient, require further evaluation with serum Ca-125 and clinical assessment by a gynecologist. These imaging features may represent malignant ovarian disease [27]. The combination of serum Ca-125, ultrasound imaging features, and menopausal status can be used to calculate an accurate risk of malignancy index [28]. After the incidental initial imaging detection of a complex cyst, the aim should be to direct the case to an multi-disciplinary team (MDT) specializing in ovarian cancer [29].
Figure 5 demonstrates an ovarian cyst with a papillary mural nodule, detected as an incidental finding in addition to the fibroid. This patient had presented with menorrhagia and underwent surgery, which confirmed the diagnosis of fibroid uterus and a serous cystadenoma with, in this case, a benign papillary projection. However, papillary projections occur with greater frequency in borderline or malignant tumors [27].
Figure 6 demonstrate another incidental discovery. The abnormality is not appreciated on the same images as the fibroid, highlighting the need for careful assessment of the whole study. This left ovarian cyst contains multiple septations. These are thin and smooth, and less likely to indicate malignancy than thickened or nodular septations. However, cystadenomas are usually unilocular whereas malignant cysts are often multilocular [27]. The patient’s Ca-125 was normal, and in this case subsequent follow-up ultrasound demonstrated resolution of the cyst.
Nongynecological Pathology
Vascular Pathology
The presence of dilated veins within the pelvis may indicate a wide variety of pathologies, including proximal venous stenoses or occlusion and portal hypertension, or they may be due to increased flow resulting from presence of tumor or vascular malformation. Arteriovenous malformations are distinguished from pelvic varices by the masslike appearance and rapid enhancement of the former. Recognition of pelvic varices is important in improving the diagnosis of a variety of pelvic and systemic conditions [30], but importantly, secondary varices are rarely associated with pelvic pain.
In contrast, in the presence of chronic pelvic pain, and thus in those patients with symptoms that overlap those of fibroid symptomatology, the presence of pelvic varices raises the possibility of pelvic congestion syndrome. Pelvic congestion syndrome is thought to be an underdiagnosed cause of chronic pelvic pain in premenopausal women. The etiology is not well understood. The incidence of the condition is uncertain, but in a study of healthy female kidney donors, an incompetent ovarian vein was found to have a prevalence of 10%. The authors of this study suggested that up to 77% of such patient could benefit from embolization or ligation [31]. There are no agreed-upon diagnostic criteria for diagnosis of varices with cross-sectional imaging, but an ovarian vein diameter of 8 mm has been suggested [32]. Varices usually demonstrate signal loss on T1-weighted images but may show variable or high signal rather than signal void on T2-weighted sequences, presumably due to slow flow. With MRA techniques, flow within varices is isointense with flow in normal vessels. Newer magnetic resonance venography techniques may be more sensitive than standard T2-weighted sequences [33]. Ovarian vein embolization may be used for treatment of this condition.
Spinal Pathology
Patients with fibroids may experience back pain. Lumbar degenerative changes affecting the lumbosacral vertebrae or intervertebral discs are also extremely common and may be demonstrated coincidentally. Up to 80% of adults experience back pain at some point, and symptoms associated with degenerative disc disease typically affects the 30–50-year age group. The origin of pain in patients with degenerative and associated changes within the lumbar spine is complex [34] and beyond the scope of this article, but it clearly presents potential for diagnostic dilemma. This highlights the need for accurate clinical and radiological evaluation and a combined clinicoradiologic approach to management. Figure 7 demonstrates pre- and post-UAE appearances at MRI in a patient who has vertebral body fusion at L4–L5 level. The patient experienced symptomatic relief after UAE, although the spinal changes have clearly progressed radiologically.
A Pre-UAE MRI demonstrates multiple fibroids and vertebral body fusion at L4–L5 level (arrow). B After UAE, the spinal disease has progressed radiologically, with new high T2 signal changes at the L5–S1 level (arrows). C In another patient, pre-UAE MRI demonstrates multiple fibroids within a retroverted uterus with coexistent disc disease at L5–S1 level (arrow)
Because coincidental disc pathology is common, consideration should be given to this area as a potential cause of persisting back pain in patients who have demonstrated a reduction in fibroid size after UAE but have persisting symptoms, as demonstrated in Fig. 7C, although the high incidence of disc bulge or protrusions reported in asymptomatic patients (52 and 27% respectively) [35] is a reminder of the need for a multidisciplinary approach in determining the origin of pain in such patients.
Bowel-Related Pathology
Colorectal malignancy is the second most common cause of cancer mortality in the developed world, with age-standardized incidence rates in women of 40 per 100,000 for bowel cancer overall, and approximately 20 per 100,000 women for rectal cancer. It may be asymptomatic at early stages.
MRI is well established for local staging of rectal cancer. Tumors in this area are most commonly ulcerating lesions with raised rolled edges, and they most commonly grow circumferentially, resulting in annular stenosis [36]. Tumors of the rectum and rectosigmoid colon may be demonstrated coincidentally at pre-UAE MRI (Fig. 8), even without dedicated preparation or modified sequencing, allowing earlier referral for treatment and potential for improved outcome.
Inflammatory bowel disease may also present with pelvic pain that could be mistakenly attributed to the presence of fibroids. Features of Crohn disease are more clearly seen with dedicated fast breath hold sequences and with good bowel distension but may be suspected as an additional incidental finding on careful inspection of standard sequences.
Urinary Tract Pathology
Urinary retention and ureteric obstruction due to the presence of fibroids are both well recognized, although incidence rates are difficult to cite, with occurrences described in case series rather than populations. Urinary retention as a complication of fibroids usually present acutely to an obstetric team and thus would not be expected as a common incidental finding before UAE, but ureteric obstruction may be found coincidentally, and assessment for this complication, either unilaterally or bilaterally, should be routine. In one cases series of 10 patients with obstructive nephropathy due to fibroids who underwent UAE, the obstruction was the result of a large posterior wall fibroid causing ureteric obstruction at the pelvic brim in all cases; the authors concluded that UAE was a safe and effective in treating patient with obstructive nephropathy due to fibroids [37]. Figure 9 illustrates bilateral ureteric obstruction due to presence of large fibroid and anomalous right ovarian vein supply.
Conclusion
UAE is a safe and effective treatment for symptomatic fibroids and is increasingly performed. MRI evaluation before and after treatment is routine practice, with the potential to significantly alter management in up to a fifth of patients [13], and is useful for patient selection, procedure planning, and follow-up [38]. This article, illustrated using pre-UAE images from our institution, highlights the important features and appearances of pathologies that may mimic or coexist with fibroid symptomatology, and as such have the potential to change patient management.
References
Okolo S (2008) Incidence, aetiology and epidemiology of uterine fibroids. Best Pract Res Obstet Gynaecol 22:288–571
Levy BS (2008) Modern management of uterine fibroids. Acta Obstet Gynecol Scand 87:812–823
Hirst A, Dutton S, Wu O et al (2008) A multi-centre retrospective cohort study comparing the efficacy, safety and cost-effectiveness of hysterectomy and uterine artery embolisation for the treatment of symptomatic uterine fibroids. The HOPEFUL study. Health Technol Assess 12:1–248
Kroncke TJ (2008) Imaging before and after uterine artery embolization. Radiologe 48:639–648
Watkinson A, Nicholson A (2007) Uterine artery embolisation to treat symptomatic uterine fibroids. BMJ 335:720–722
Gupta S, Jose J, Manyonda I (2008) Clinical presentation of fibroids. Best Pract Res Obstet Gynaecol 22:615–626
Kuligowska E, Deeds L, Lu K (2005) Pelvic pain: overlooked and underdiagnosed gynaecologic conditions. Radiographics 25:3–20
Toor SS, Tan KT, Simons ME et al (2008) Clinical failure after uterine artery embolization: evaluation of patient and MR imaging characteristics. J Vasc Interv Radiol 19:662–667
Verma SK, Bergin D, Gonsalves CF et al (2008) Submucosal fibroids becoming endocavitory following uterine artery embolization: risk assessment by MRI. AJR Am J Roentgenol 190:1220–1226
Spielmann A, Keogh C, Forster BB et al (2006) Comparison of MRI and sonography in the preliminary evaluation for fibroid embolization. AJR Am J Roentgenol 187:1499–1504
Firouznia K, Ghanaati H, Sanaati M et al (2008) Uterine artery embolization in 101 cases of uterine fibroids: do size, location and number of fibroids affect therapeutic success and complications? Cardiovasc Intervent Radiol 31:521–526
Parthipun AA, Taylor J, Manyonda I, Belli AM (2010) Does size really matter? analysis of the effect of large fibroids and uterine volumes on complication rates of uterine artery embolisation. Cardiovasc Intervent Radiol 33:955–959
Omary RE, Vasireddy S, Chrisman HB et al (2002) The effect of pelvic MR imaging on the diagnosis and treatment of women with presumed symptomatic uterine fibroids. J Vasc Interv Radiol 13:1149–1153
Lee ES, Santilli SM, Olson MM, Kuskowski MA, Lee JT (2000) Wound infection after infrainguinal bypass operations: multivariate analysis of putative risk factors. Surg Infect 1:257–263
Indes JE, Lipsitz EC, Veith FJ et al (2008) Incidence and significance of nonaneurysmal-related computed tomography scan findings in patients undergoing endovascular aortic repair. J Vasc Surg 48:286–290
Herfarth HH, Grunert M, Klebl F et al (2009) Frequency and nature of incidental extra-enteric lesions found on magnetic resonance enterography (MRE) in patients with inflammatory bowel disease. PloS One 4:e4863
McCreadie G, Oliver TB (2009) Eight CT lessons that we learned the hard way: an analysis of radiological error and discrepancy with particular emphasis on CT. Clin Radiol 64:491–499
Razavi MK, Wolanske KA, Hwang GL et al (2002) Angiographic classification of ovarian to uterine artery anastomoses: initial observations in uterine fibroid embolization. Radiology 224:707–712
Kroencke TJ, Sceurig C, Kluner C et al (2006) Uterine fibroids: contrast enhanced MR angiography to predict ovarian artery supply—initial experience. Radiology 241:181–189
Kroencke TJ, Scheurig C, Poellinger A et al (2010) Uterine artery embolization for leiomyomas: percentage of infarction predicts clinical outcome. Radiology 255:834–841
Glastonbury CM (2002) The shading sign. Radiology 224:199–201
Togashi K, Nishimura K, Fujisawa I et al (1988) Adenomyosis: diagnosis with MR imaging. Radiology 166:111–114
Togashi K, Ozasa H, Konishi I et al (1989) Enlarged uterus: differentiation between adenomyosis and leiomyoma with MR imaging. Radiology 171:531–534
Mark AS, Hricak H, Heinrichs LW et al (1987) Adenomyosis and leiomyomas: differential diagnosis with MR imaging. Radiology 163:527
Stany P, Maxwell GL, Scott Rose G (2010) Clinical decision making using ovarian cancer risk assessment. AJR Am J Roentgenol 194:337–342
RCOG guideline 34. Available at: http://www.rcog.org.uk/womens-health/clinical-guidance/ovarian-cysts-postmenopausal-women-green-top-34. Accessed June 2010
Jeong YY, Outwater EK, Kang HK (2000) Imaging evaluation of ovarian masses. Radiographics 20:1445–1470
Jacobs I, Oram D, Fairbanks J et al (1990) A risk of malignancy index incorporating CA125, ultrasound and menopausal status for the accurate preoperative diagnosis of ovarian cancer. Br J Obstet Gynaecol 97:922–929
Spencer JA (2005) A multidisciplinary approach to ovarian cancer at diagnosis. Br J Radiol 78(Spec No. 2):S94–S102
Umeola S, Koyama T, Togashi K et al (2004) Vascular dilation in the pelvis: identification with CT and MR imaging. Radiographics 24:193–208
Belenky A, Bartal G, Atar E et al (2002) Ovarian varices in healthy female kidney donors: incidence, morbidity and clinical outcome. AJR Am J Roentgenol 179:625–627
Coakley FV, Varghese SL, Hricak H (1999) CT and MRI of pelvic varices in women. JCAT 23:429–434
Dick EA, Burnett C, Anstee A et al (2010) Time-resolved imaging of contrast kinetics 3D magnetic resonance venography with pelvic congestion syndrome. Br J Radiol 83:882–887
Mirsadraee S, Tuite D, Nicholson A (2008) Uterine artery embolisation for ureteric obstruction secondary to fibroids. Cardiovasc Intervent Radiol 31:1094–1099
Modic MT, Ross JS (2007) Lumbar degenerative disk disease. Radiology 245:43–61
Jensen MC, Brant-Zawadzki MN, Obuchowski N et al (1994) Magnetic resonance imaging of the lumbar spine in people without back pain. N Engl J Med 331:69–73
Taylor FGM, Swift RI, Blomqvisy L, Brown G (2008) A systematic approach to the interpretation of preoperative staging MRI for rectal cancer. AJR Am J Roentgenol 191:1827–1835
Kirby JM, Burrows D, Haider E et al (2010) Utility of MRI before and after uterine fibroid embolization: why to do it and what to look for. Cardiovasc Intervent Radiol [Epub ahead of print]
Conflict of interest
No conflict of interest to declare.
Author information
Authors and Affiliations
Corresponding author
Additional information
Rights and permissions
About this article
Cite this article
Williams, P.L., Coote, J.M. & Watkinson, A.F. Pre–Uterine Artery Embolization MRI: Beyond Fibroids. Cardiovasc Intervent Radiol 34, 1143–1150 (2011). https://doi.org/10.1007/s00270-011-0124-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-011-0124-z