Abstract
Background
When performing cholecystectomy after gastrectomy, we often encounter problems, such as adhesions, nutritional insufficiency, and bowel reconstruction. The purpose of this study was to identify the factors related to surgical outcome of these associated procedures, with emphasis on the use of a laparoscopic approach.
Methods
We retrospectively analyzed data from 58 patients who had a history of cholecystectomy after gastrectomy. Differences between subgroups with respect to operation time, length of postoperative hospital stay, and complications were analyzed. To identify the factors related with outcomes of cholecystectomy after gastrectomy, we performed multivariable analysis with the following variables: common bile duct (CBD) exploration, laparoscopic surgery, gender, acute cholecystitis, history of stomach cancer, age, body mass index, period of surgery, and interval between cholecystectomy and gastrectomy.
Results
We found one case (2.9%) of open conversion. The CBD exploration was the most significant independent factor (adjusted odds ratio (OR), 45.15; 95% confidence interval (CI), 4.53–450.55) related to longer operation time. Acute cholecystitis also was a significant independent factor (adjusted OR, 14.66; 95% CI, 1.46–147.4). The laparoscopic approach was not related to operation time but was related to a shorter hospital stay (adjusted OR, 0.057; 95% CI, 0.004–0.74). Acute cholecystitis was independently related to the occurrence of complications (adjusted OR, 27.68; 95% CI, 1.15–666.24); however, CBD exploration and laparoscopic surgery were not. A lower BMI also was an independent predictor of the occurrence of complications (adjusted OR, 0.41; 95% CI, 0.2–0.87).
Conclusions
The laparoscopic approach is feasible for cholecystectomy after gastrectomy, even in cases with CBD stones or acute cholecystitis. This approach does not appear to increase operation time or complication rate and was shown to decrease the length of postoperative hospital stay.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The incidence of cholelithiasis has been reported to be high in gastrectomy patients [1–3]. A vagotomized gallbladder or altered response to and secretion of cholecystokinin have been suggested as underlying pathophysiologies [4–6]. There is some debate about the appropriate management of these conditions, and some authors have suggested performing prophylactic cholecystectomy for these patients [7–9]. However, the incidence of a future need for cholecystectomy after upper gastrointestinal surgery has been reported to be as low as 1–7% in some prospective studies [2, 3, 10–12]. Moreover, laparoscopic cholecystectomy has been safely performed in patients with previous upper abdominal surgery [13–16]. For these reasons, prophylactic cholecystectomy during a gastrectomy procedure is generally not recommended [17, 18].
Although the need for cholecystectomy after gastrectomy is rare, the patient for whom it is indicated frequently suffers from unique problems. First, there may be significant adhesion around Calot’s triangle, especially when lymph node dissection has been performed for stomach cancer. Second, chronic nutritional insufficiency induced by a previous gastrectomy decreases intra-abdominal fat, which may improve surgical accessibility but also may affect the recovery of a patient after the surgery [19]. Third, intestinal reconstruction after gastrectomy may interfere with access to the common bile duct (CBD) via endoscopic retrograde cholangiopancreaticography (ERCP) [20]. A few groups have reported outcomes of laparoscopic cholecystectomy after gastrectomy [15, 16, 21, 22]. However, factors that may increase operation time, length of hospital stay, or complication rates of cholecystectomy after gastrectomy have not yet been reported. The purpose of this study was to identify factors related to surgical difficulties and outcome using multivariable analyses.
Patients and methods
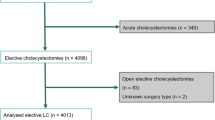
Among the 2,401 patients who underwent a cholecystectomy at Kyung Hee University Medical Center between January 2000 and July 2010, 58 patients (2.4%) who had a history of a previous gastrectomy were included in this study. The median follow-up period time was 59 (range 2–180) months. Characteristics of our study group are summarized in Table 1. Twenty-four patients underwent open cholecystectomy (OC), and 34 patients underwent laparoscopic cholecystectomy (LC). The mean age of our study participants was 61.5 ± 10.2 years, and we had twice as many male patients (n = 40, 69%) as female patients (n = 18, 31%). As with other gastrectomy subjects, body mass index (BMI) was lower than normal (21.2 ± 2.7 kg/m2). The mean interval between gastrectomy and cholecystectomy was 11.2 ± 9.1 years. The most common indication of gastrectomy was stomach cancer (40 patients, 69%), whereas others included benign diseases, such as peptic ulcer disease. Total gastrectomy had been performed on 19 patients (32.8%), and the Billroth II operation was more common (n = 27, 46.6%) than was the Billroth I operation (n = 11, 19%) among partial gastrectomy patients.
The effects of various factors may be related to the period in which the operation was performed. To further analyze this relationship, we divided our study period into the period before 2006, and the period after 2006 based on the fact that laparoscopic cholecystectomies and laparoscopic common bile duct explorations were more frequently performed in the later period (15.4 vs. 93.8%; P < 0.001, and 22.2 vs. 87.5%; P = 0.015, respectively).
Overall, laparoscopic surgical procedures were performed for 34 patients (58.6%), 1 of whom underwent open conversion due to dense adhesions around Calot’s triangle. Acute cholecystitis was present in 33 patients (56.9%) and acute cholangitis was present in 20 (34.5%). Previous percutaneous transhepatic biliary drainage (PTBD) had been performed in three patients (5.2%), and six (10.3%) had undergone previous percutaneous transhepatic gallbladder drainage (PTGBD). To clear CBD stones, ERCP was attempted before cholecystectomy in eight patients (13.8%), but was successful in only one. We performed surgical CBD exploration in 17 patients (29.3%), including 9 cases (15.5%) of laparoscopic CBD exploration. When laparoscopic CBD exploration was indicated, choledochotomy and choledochoscopic investigation and stone removal followed by T-tube placement were performed. Duct clearance was successful in all patients who underwent surgical CBD exploration, and no residual or recurrent stones were identified after the procedure.
Mean operation time was 151.7 ± 79.8 min, and patients resumed a soft diet in 3.1 ± 2.5 days. Patients remained in the hospital for 7.6 ± 7.2 days. Complications were identified in 11 patients (19%), with the most common being intraoperative bowel injury during adhesiolysis. We postulated that operation time represented technical difficulty during the surgical procedure, duration of hospital stay represented patient comfort, and complication rate represented the risks associated with the operation. We designated these three variables as dependent variables, and we conducted analyses to identify factors that would predict technical difficulty, patient discomfort, and complications of the operation. For multivariable analyses, all clinically important variables were analyzed; however, apparently related variables were carefully merged to avoid multicollinearity. We performed multivariable analysis by using following variables: CBD exploration, laparoscopic surgery, gender, acute cholecystitis, history of stomach cancer, age, BMI, period in which the cholecystectomy was performed, and the interval between gastrectomy and cholecystectomy.
Continuous variables were summarized with means and standard deviations, for which frequencies and percentages were used for categorical variables. Student’s t test and the χ2 test were used to compare various demographic, clinical, and laboratory variables to the three dependent variables of operation time, hospital stay, and the presence of complications. Mean values of operation time (152 min) and hospital stay (7.6 days) were used to divide the patients into subgroups (Table 2). Multivariable logistic regression analysis was conducted to identify independent factors that would predict the three dependent variables. The results are presented as adjusted odds ratios (ORs) and 95% confidence intervals (CIs) for each of the three dependent variables. All statistical analyses were conducted by using SPSS® 13.0 (SPSS, Inc., Chicago, IL), and P < 0.05 was considered statistically significant.
Results
To overview the basic data, we subdivided the patients into OC group and LC group (Table 1). The male patients were more dominant in OC group (P = 0.002). However, age, body mass index, ASA score, indications of gastrectomy, and type of gastrectomy procedures were not significantly different between OC patients and LC patients. Among the laboratory data, alanine aminotransferase (ALT) was significantly higher in LC patients. Indications of cholecystectomy were not significantly different, and preoperative and intraoperative management of gallstones, namely PTBD, PTGBD, ERCP, and CBD exploration were not significantly different between groups. LC patients showed earlier diet resumption (P < 0.001) and shorter hospital stay (P = 0.009) and lower incidence of complications (P = 0.038).
Subgroup analyses were performed according to operation time, length of postoperative hospital stay, and the presence of complications (Table 2). We first divided the patients into two groups according to the operation time of cholecystectomy: those with a “short” operation time (mean operation time ≤152 min; n = 34) and those with a “long” operation time (>152 min; n = 24). We found that diet resumption and discharge from the hospital were delayed in the long operation time group (4.2 vs. 2.3 days and 10.8 vs. 5.2 days, respectively; P < 0.05), whereas gender, BMI, and the interval between gastrectomy and cholecystectomy were not significantly related to operation time. Acute cholecystitis and acute cholangitis were more frequently combined in the long operation time group (79.2 vs. 41.2% and 54.2 vs. 20.6%, respectively; P < 0.05). CBD exploration was more frequently performed in the long operation time group (62.5 vs. 5.9%; P < 0.05); however, laparoscopic surgery was not significantly related to a long operation time.
We also divided the patients into two groups according to the length of postoperative hospital stay: those with a “short” stay (≤mean value of 7.6 days; n = 39) and those with a “long” stay (>7.6 days, n = 19). We found that operation time, BMI, and the interval between gastrectomy and cholecystectomy were not significantly related to length of postoperative hospital stay. Diet resumption occurred earlier in the short hospital stay group and the complication rate was higher in the long hospital stay group (2.0 vs. 5.3 days and 5.1% vs. 47.4%, respectively; P < 0.05). Patients who underwent surgery during the later period (post-2006) were more commonly in the short hospital stay group (29.2 vs. 26.3%; P < 0.05). The presence of acute inflammatory pathology, namely acute cholecystitis or acute cholangitis, was not significantly related to the duration of hospital stay. Likewise, CBD exploration, a factor that significantly increased operation time, was not an important factor in predicting the duration of hospital stay. Patients who underwent laparoscopic surgery, however, were more frequently in the short hospital stay group (76.9 vs. 21.1%; P < 0.05).
Eleven patients experienced intraoperative or postoperative complications (19%). We found that diet resumption and discharge from the hospital were delayed in this complications group (2.5 vs. 5.8 days and 5.4 vs. 16.7 days, respectively; P < 0.05), and patients who experienced complications had a lower BMI (21.5 vs. 19.7 kg/m2; P < 0.05). In addition, the interval between gastrectomy and cholecystectomy was shorter in the complications group (12.5 vs. 5.8 years; P < 0.05), which also included a greater number of acute cholecystitis patients (48.9 vs. 90.9%; P < 0.05), although the occurrence of acute cholangitis was not affected. CBD exploration did not increase the likelihood of complications, and laparoscopic surgery was performed less frequently on members of the complications group (66 vs. 27.3%; P < 0.05).
We conducted multivariable analyses to identify independent predictors of longer operation time, longer hospital stay, and increased complications (Table 3). For operation time, the need for CBD exploration was the most significant factor (adjusted OR, 45.15; 95% CI, 4.53–450.55), followed by the presence of acute cholecystitis (adjusted OR, 14.66; 95% CI, 1.46–147.4). A laparoscopic approach, however, was not a significant factor related to operation time. Moreover, a laparoscopic approach was the only factor related to the duration of hospital stay, significantly decreasing the duration of hospital stay (adjusted OR, 0.057; 95% CI, 0.004–0.74). Acute cholecystitis was independently related to the occurrence of complications (adjusted OR, 27.68; 95% CI, 1.15–666.24), and a lower BMI also was an independent predictor of complications (adjusted OR, 0.41; 95% CI, 0.2–0.87). Neither the period during which the cholecystectomy was performed nor the interval between gastrectomy and cholecystectomy was shown to be independently associated with any of the above variables.
Discussion
In 2008, 16,448 gastrectomies were performed in the Republic of Korea, compared with 38,039 cholecystectomies [23]. When cholecystectomy is indicated for a patient with a history of gastrectomy, we can perform either an open or laparoscopic approach; if there are CBD stones, they can be treated by preoperative ERCP or intraoperative CBD explorations. We tried to find the better approach for these patients.
The usefulness of laparoscopic CBD exploration in general patients without history of gastrectomy has been reported, with success rates in the range of 93.3–100% [24–26]. As a result, a single-stage approach without attempting ERCP has been suggested [27, 28]. Moreover, previous gastrectomy has been reported as a reason for failed endoscopic extraction using ERCP [20]. Among the 20 patients diagnosed as combined CBD stones, two spontaneously passed the CBD stones. ERCP was attempted in eight subjects, but successful CBD clearance was achieved in only one patient. Among the eight patients, the previous stomach surgeries were total gastrectomy in three cases and Billroth-II operation in four cases. This higher incidence of complex bowel reconstruction may explain the low success rate of duct clearance by ERCP. Meanwhile, ERCP is not a benign procedure; complications, such as bleeding, pancreatitis, duodenal perforation, and papillotomy stenosis, are not uncommon [28, 29]. One of our patients also experienced small-bowel perforation during the ERCP procedure. One report states that laparoscopic CBD exploration is a feasible approach for postgastrectomy patients [30]. In our series, no recurrent stones were identified after operative CBD exploration during the follow-up period; however, two subjects showed CBD stricture and underwent ballooning and stent insertion, respectively. Our results also suggest the advantage of a single-stage approach for the management of CBD stones after gastrectomy, and we now believe that laparoscopic exploration should be the initial approach for gastrectomy patients with CBD stones.
Laparoscopic cholecystectomy has been suggested as a feasible approach for acute cholecystitis [31, 32], and it was our preferred method, especially during the later period of our study. Combined acute cholecystitis may increase the incidence of complications [33] and may worsen the anatomical orientation that has already been disturbed by previous gastrectomy. The proportion of patients with acute cholecystitis (56.9%) was higher than normal in our study population. We postulated that cholelithiasis patients with a history of gastrectomy were managed more conservatively, and the proportion of more critical patients who could not avoid cholecystectomy, such as subjects with CBD stones or acute cholecystitis, might have been increased in this group. As we expected, two factors—CBD exploration and acute cholecystitis—resulted in increased operation time, which represented technical difficulties. Preoperative ALT level was higher in the noncomplication group than in the complication group (Table 2). Meanwhile, preoperative ALT level was significantly higher in the laparoscopic surgery group than in the open surgery group (Table 1). As the complication rate was lower in laparoscopic surgery group than in open surgery group, ALT level in patients without complication might be paradoxically higher.
Acute cholecystitis was an independent predictor of complications, but CBD exploration was not. The results of this study showed that a laparoscopic approach did not increase operation time and significantly decreased the length of hospital stay. We also found that lower BMI was an independent predictor of complications. This may be a unique feature in this population, and more data are necessary to reveal the underlying mechanisms, such as chronic nutritional insufficiency. The most common complication was the bowel injury, which occurred both in open (2 cases) and laparoscopic (3 cases) approaches. Among three laparoscopic cases, one patient underwent open conversion, and two were managed by laparoscopic repair of the injury. Of note, one patient who underwent laparoscopic repair of the bowel injury developed enterocutaneous fistula, which was cured by conservative management. It has been reported that the type of incision used in previous abdominal surgery is related to the outcome of laparoscopic cholecystectomy [21]. We infer that gastrectomy via minimally invasive surgery may improve outcomes in future reoperations for cholecystectomies. The mean interval between gastrectomy and cholecystectomy was 11.2 years in our series. In Korea, the laparoscopic gastrectomy was not widely accepted until a few years ago. Although only one of our study subjects underwent laparoscopy-assisted distal gastrectomy, we think that the role of minimal invasive surgery in gastrectomy will increase in the near future as laparoscopy-assisted distal gastrectomy gains popularity for the treatment of early gastric cancer [34].
In summary, cholecystectomy after gastrectomy requires a longer operation time in patients who need CBD exploration and in patients with acute cholecystitis. The presence of acute cholecystitis and a lower BMI may increase the rate of complications. A laparoscopic approach is feasible and does not increase operation time or complication rates and decreases the length of hospital stay after surgery. Laparoscopy is a feasible initial approach for cholecystectomy after gastrectomy even in the presence of common bile duct stones or acute cholecystitis.
References
Hauters P, De de Roden A, Pourbaix A (1988) Cholelithiasis: a serious complication after total gastrectomy. Br J Surg 75:899–900
Lorusso D, Misciagna G, Noviello M, Tarantino S (1988) Cholelithiasis after Billroth II gastric resection. Surgery 103:579–583
Rehnberg O, Haglund U (1985) Gallstone disease following antrectomy and gastroduodenostomy with or without vagotomy. Ann Surg 201(3):315–318
Hopman W, Jansen J, Lamers C (1984) Plasma cholecystokinin response to oral fat in patients with Billroth I and Billroth II gastrectomy. Ann Surg 199:276–280
Inoue K, Fuchigami A, Hosotani R et al (1987) Release of cholecystokinin and gallbladder contraction before and after gastrectomy. Ann Surg 205:27–32
Yi S, Ohta T, Tsuchida A et al (2007) Surgical anatomy of innervation of the gallbladder in humans and Suncus murinus with special reference to morphological understanding of gallstone formation after gastrectomy. World J Gastroenterol 13:2066–2071
Fobi M, Lee H, Igwe D et al (2002) Prophylactic cholecystectomy with gastric bypass operation: incidence of gallbladder disease. Obes Surg 12:350–353
Nougou A, Suter M (2008) Almost routine prophylactic cholecystectomy during laparoscopic gastric bypass is safe. Obes Surg 18:535–539
Farsi M, Bernini M, Bencini L et al (2009) The CHOLEGAS study: multicentric randomized, blinded, controlled trial of gastrectomy plus prophylactic cholecystectomy versus gastrectomy only, in adults submitted to gastric cancer surgery with curative intent. Trials 10:32
Inoue K, Fuchigami A, Higashide S et al (1992) Gallbladder sludge and stone formation in relation to contractile function after gastrectomy. A prospective study. Ann Surg 215:19–26
Tsunoda K, Shirai Y, Wakai T et al (2004) Increased risk of cholelithiasis after esophagectomy. J Hepato-Biliary-Pan 11:319–323
Tachibana M, Kinugasa S, Yoshimura H et al (2003) Acute cholecystitis and cholelithiasis developed after esophagectomy. Can J Gastroenterol 17:175–178
Bae YS, Lee SM, Kim JH et al (2009) Laparoscopic cholecystectomy in patients with a history of upper abdominal surgery. J Korean Soc Endosc Laparosc Surg 12:108–112
Karayiannakis A, Polychronidis A, Perente S et al (2004) Laparoscopic cholecystectomy in patients with previous upper or lower abdominal surgery. Surg Endosc 18:97–101
Kwon A (2001) Laparoscopic cholecystectomy and choledocholithotomy in patients with a previous gastrectomy. J Am Coll Surgeons 193:614–619
Sasaki A, Nakajima J, Nitta H et al (2008) Laparoscopic cholecystectomy in patients with a history of gastrectomy. Surg Today 38:790–794
Gillen S, Michalski C, Schuster T et al (2010) Simultaneous/incidental cholecystectomy during gastric/esophageal resection: systematic analysis of risks and benefits. World J Surg 34:1008–1014. doi:10.1007/s00268-010-0444-1
Quesada B, Kohan G, Roff H et al (2010) Management of gallstones and gallbladder disease in patients undergoing gastric bypass. World J Gastroenterol 16:2075–2079
Poitou Bernert C, Ciangura C, Coupaye M et al (2007) Nutritional deficiency after gastric bypass: diagnosis, prevention and treatment. Diabetes Metab 33:13–24
Karaliotas C, Sgourakis G, Goumas C et al (2008) Laparoscopic common bile duct exploration after failed endoscopic stone extraction. Surg Endosc 22:1826–1831
Ercan M, Bostanci EB, Ulas M et al (2009) Effects of previous abdominal surgery incision type on complications and conversion rate in laparoscopic cholecystectomy. Surg Laparosc Endosc Percutan Tech 19:373–378
Fraser SA, Sigman H (2009) Conversion in laparoscopic cholecystectomy after gastric resection: a 15-year review. Can J Surg 52:463–466
Data from the national health insurance corporation. Available at: http://www.nhic.or.kr. Accessed 1 Dec 2010
Berthou J, Drouard F, Charbonneau P, Moussalier K (1998) Evaluation of laparoscopic management of common bile duct stones in 220 patients. Surg Endosc 12:16–22
Gigot J, Navez B, Etienne J et al (1997) A stratified intraoperative surgical strategy is mandatory during laparoscopic common bile duct exploration for common bile duct stones: lessons and limits from an initial experience of 92 patients. Surg Endosc 11:722–728
Tinoco R, Tinoco A, El-Kadre L et al (2008) Laparoscopic common bile duct exploration. Ann Surg 247:674–679
Rhodes M, Sussman L, Cohen L, Lewis M (1998) Randomised trial of laparoscopic exploration of common bile duct versus postoperative endoscopic retrograde cholangiography for common bile duct stones. Lancet 351:159–161
Moore KB, Adrales GL, Mastrangelo MJ Jr (2004) Laparoscopic common bile duct exploration. Curr Surg 61:294–296
Phillips E, Liberman M, Carroll B et al (1995) Bile duct stones in the laparoscopic era: is preoperative sphincterotomy necessary? Arch Surg 130:880–886
Tang C, Tsui K, Yang G et al (2008) Laparoscopic exploration of common bile duct in post-gastrectomy patients. Hepato-Gastroenterol 55:846–849
Gurusamy K, Samraj K, Gluud C et al (2010) Meta analysis of randomized controlled trials on the safety and effectiveness of early versus delayed laparoscopic cholecystectomy for acute cholecystitis. Br J Surg 97:141–150
Wiseman J, Sharuk M, Singla A et al (2010) Surgical management of acute cholecystitis at a tertiary care center in the modern era. Arch Surg 145:439–444
Jatzko G, Lisborg P, Pertl A, Stettner H (1995) Multivariate comparison of complications after laparoscopic cholecystectomy and open cholecystectomy. Ann Surg 221(4):381–386
Kim H, Hyung W, Cho G et al (2010) Morbidity and mortality of laparoscopic gastrectomy versus open gastrectomy for gastric cancer: an interim report-a phase iii multicenter, prospective, randomized trial (KLASS Trial). Ann Surg 251(3):417–420
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kim, J., Cho, J.N., Joo, S.H. et al. Multivariable Analysis of Cholecystectomy after Gastrectomy: Laparoscopy is a Feasible Initial Approach even in the Presence of Common Bile Duct Stones or Acute Cholecystitis. World J Surg 36, 638–644 (2012). https://doi.org/10.1007/s00268-012-1429-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-012-1429-z