Abstract
Background
Patients with adhesive small intestine obstruction (ASIO) are difficult to evaluate and to manage and their treatment is still controversial. The diagnostic and therapeutic role of water-soluble contrast medium (Gastrografin) in ASIO is still debated. This study was designed to determine the therapeutic role of Gastrografin in patients with ASIO.
Methods
The study was a multicenter, prospective, randomized, controlled investigation. The primary end points were the evaluation of the operative rate reduction and shortening the hospital stay after the use of Gastrografin. A total of 76 patients were randomized into two groups: the control group received traditional treatment (TT), whereas the study group (GG) received in addition a Gastrografin meal and follow-through study immediately. Patients with Gastrografin in the colon within 36 hours were considered to be partially obstructed and submitted to nonoperative management. If after 36 hours, the Gastrografin had not entered the colon, the subjects were submitted to laparotomy.
Results
No significant differences were found in age, sex, intravenous administration of prokinetics, incidence and characteristics of the previous procedures in surgical history of the patients, previous episodes of ASIO and surgery for adhesiolysis, or duration of symptoms before admission. In the GG group obstruction resolved subsequently in 31 of 38 cases (81.5%) after a mean time of 6.4 hours. The remaining seven patients were submitted to surgery, and one of them needed bowel resection for strangulation. In the control group, 21 patients were not submitted to surgery (55%), whereas 17 showed persistent untreatable obstruction and required laparotomy: 2 of them underwent bowel resection for strangulation. The difference in the operative rate between the two treatment groups reached statistical significance (p = 0.013). The time from the hospital admission for obstruction to resolution of symptoms was significantly lower in the GG group (6.4 vs. 43 hours; p < 0.01). The length of hospital stay revealed a significant reduction in the GG group (4.7 vs. 7.8 days; p < 0.05). This reduction was more evident in the subset of patients who did not require surgery (3 vs. 5.1 days; p < 0.01). No GG-related complications or significant differences in major complications and the relapse rate were found (relapse rate, 34.2% after a mean time to relapse of 6.3 months in the GG group vs. 42.1% after 7.6 months in the TT; p = not significant).
Conclusions
Data showed that the use of Gastrografin in ASIO is safe and reduces the operative rate and the time to resolution of obstruction, as well as the hospital stay.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Adhesive small intestine obstruction (ASIO) is an important cause of hospital admission and its treatment is still controversial. Emergency surgery is mandatory when strangulation or complete obstruction occur [1]. Nonoperative conservative management is indicated in the case of partial obstruction [2]. The reported operative rate for ASIO ranges from 27% to 42% [3].
The role of Gastrografin, the most widely used water-soluble contrast medium in ASIO, has been assessed recently with regard to diagnostic and therapeutic value [4]. The mechanism by which Gastrografin works is not yet well known. Gastrografin, ionic bitter-flavored mixture of sodium diatrizoate and meglumine diatrizoate, having osmolarity of 1900 mOsm/L, approximately six times more than extracellular fluid, promotes shifting of fluids into the bowel lumen and increases the pressure gradient across obstructive sites. Furthermore, because Gastrografin dilutes the bowel content, it facilitates its passage and decreases edema of the intestine wall facilitating motility. Contrary to barium, Gastrografin is safe even if intestinal perforation and peritoneal spread occurs [5–7].
A great diagnostic benefit of Gastrografin for evaluating the indication for surgical intervention and the timing of surgery in completely obstructed patients without peritonism has been reported [8, 9]. Chen et al. [5] demonstrated that 96% of patients with ASIO in whom Gastrografin failed to reach the colon within 24 hours required surgery.
Moreover, it has been proposed a therapeutic value because Gastrografin reduces the operative rate and the length of hospital stay. However, this topic is still debated [5], because some authors did not find any therapeutic advantage [10, 11]. This study (Gastrografin use in Small Bowel Obstruction Caused by Adherences, GUSBOCA Trial) was designed to determine the therapeutic role of Gastrografin in patients with ASIO without strangulation and peritonism.
Materials and methods
The GUSBOCA Trial is a multicenter, prospective, randomized, controlled study, which was performed in the Departments of Emergency Surgery of S. Orsola-Malpighi (Bologna) and Modena University Hospital (Italy), with the participation of three treating surgeons (FC, LA, MG). The study conformed to good clinical practice guidelines and followed the recommendations of the Declaration of Helsinki. The protocol was approved on September 9, 2003 by the S. Orsola-Malpighi University Hospital’s Ethical Review Board.
Patients
Eligible patients to be enrolled and randomized were ASA I-III adult patients with history of single or multiple previous abdominal surgical procedures, clinical and radiological evidence of ASIO, without signs of strangulation and peritonism. Informed consent was obtained from all patients. The patients were free to withdraw at anytime.
Emergency surgical procedure was performed in patients with the suspicion of strangulation and those patients were excluded from randomization. Other exclusion criteria were: actual presence or high suspicion of intra-abdominal malignancy (clinical history less than 2 years of previous surgery for intra-abdominal cancer or radiologically/endoscopically suspected intra-abdominal cancer or histologically proven cancer), suspicion or history of peritoneal carcinomatosis, active inflammatory bowel disease, positive history of abdominal radiotherapy, and obstructed hernias. Patients with intraoperative findings of diseases other than ASIO have been included in the study according to the intention-to-treat analysis.
Procedures
The randomization was obtained through computer-generated schedule, and its result was sealed in 76 envelopes. If the patient fulfilled the inclusion criteria, the responsible surgeon opened randomly an envelope and, accordingly to the protocol, the patient was asked to sign informed consent.
Preoperative data collected included patient demographics, comorbidities, duration of symptoms before admission to the hospital, and a detailed history of previous episodes of obstruction and surgical procedures. The number and type of previous operations was recorded, as well as the incidence of previous episodes of ASIO and the previous operative rate in these episodes.
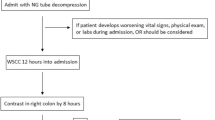
In the control group (TT: Traditional Treatment), the patients have been treated by traditional conservative treatment for ASIO, consisting in nil per os diet, nasogastric tube (NGT) decompression, and intravenous fluid resuscitation. Prokinetics drugs (neostigmine 1 mg daily plus metoclopramide 30 mg daily) were administered upon clinical discretion of the treating surgeon and its use was recorded. The patients were evaluated at 36 hours for presence of clinical and radiological signs of mechanical obstruction (not passing stools nor flatus, NGT output higher than 20 ml per hour on average, persistence of abdominal distension, radiological evidence of air-fluid levels in the small bowel without air in the colonic sections). Those patients with the above-listed clinical and radiological findings consistent with complete mechanical obstruction were submitted to laparotomy. The others who showed radiological improvement after 36 hours and early clinical relief of intestinal obstruction were fed and eventually discharged if tolerating oral diet. Finally those patients showing only clinical and radiological improvement continued the conservative treatment and received clinical and radiological reevaluation at 72 hours. If they showed persistent or worsening signs of obstruction, laparotomy was performed. Otherwise they were fed and discharged after tolerating solid food diet.
The study group (GG: Gastrografin Group) received, beyond the traditional conservative treatment mentioned, a Gastrografin meal with a follow-through study immediately. Gastrografin solution (150 ml of Gastrografin diluted with 50 ml of water) was given through NGT and the transit of contrast was studied by serial (36 and 72 hours) abdomen X-rays. If the contrast did not reach the colon after 36 hours, the subjects were submitted to laparotomy. Whereas those patients showing Gastrografin in the colon after 36 hours, if already clinically relieved of intestinal obstruction, were fed and eventually discharged if tolerating oral diet. Patients not yet relieved of obstruction with contrast in colon within 36 hours were considered to be partially obstructed and continued conservative therapy. Those patients continuing conservative treatment with no improvement after 72 hours from Gastrografin administration, clinical signs, and radiological findings of persisting mechanical obstruction were submitted to surgery. The other patients showing a later clinical improvement within 72 hours were fed and discharged.
The discharge criteria were the achievement of total resolution of intestinal obstruction, defined as complete resolution of clinical and radiological signs and symptoms, with tolerance to solid food diet.
The primary end points were: the operative rate in ASIO patients, the time to resolution of ASIO (in hours, calculated from the hospital admission to resolution of intestinal obstruction), and the length of hospital stay. Secondary end points were: incidence of major and minor complications of treatments in comparison and ASIO recurrences.
Because complications from the use of Gastrografin and allergic reactions are rare [12–14], the onset of any complication related to treatments used in the study or to ASIO was recorded intraoperatively, postoperatively, at discharge, and at 7 days, 1 month, 6 months, and 1 year of follow-up. The recurrences of episodes of ASIO and their operative rate also were eventually recorded at follow-up. A minimum follow-up period of 1 year was achieved for all 76 patients and updated every 6 months until November 2006.
Statistical analysis
Using EpiINFO 2000 (Center for Disease Control and Prevention), a sample size of 38 patients for each group (76 patients for the whole study) has been calculated to reach a confidence level of 95% with power of 80%, supposing a failure rate for conservative nonoperative therapy without administering Gastrografin of approximately 40%, as reported [3], and a reduction in the operative rate of 30% with the use of Gastrografin. SPSS 11.5 software was used for the statistical analysis (SPSS, Inc., Chicago, IL).
Analysis of data was by intention-to-treat. Data are expressed as numbers (%) and means (SD). The results were analyzed by using the χ2 test and Fisher’s exact test, as appropriate, for proportions in case of discrete data. For means of continuous numerical data, we used the independent samples t test and Mann–Whitney test, respectively, for data normally and nonnormally distributed. The data were previously tested for normality by the Kolmogorov-Smirnov test. Kaplan–Meier curves were used for relapse free survival period analysis and its comparative significance has been tested by using log-rank (Mantel Cox) test. p < 0.05 was considered statistically significant.
Results
During the study period from September 2003 to November 2006, 147 obstructed patients were assessed for eligibility, and 65 were excluded. Six patients presented signs of strangulation or peritonism at admission and were immediately submitted to emergency laparotomy. Figure 1 shows a flow diagram of the study conform to the CONSORT statement guidelines.
A total of 76 patients were enrolled and randomized. The mean age of the patients with ASIO was 65.7 (median, 70 (range 22–85)) years (Table 1). Forty-nine (64.5%) patients underwent multiple previous abdominal surgical procedures, whereas 27 (35.5%) presented history of only one surgical operation. The types of previous operation are reported in Table 2.
Thirty-eight patients were randomized to undergo GG meal and follow-through study and 38 patients to traditional treatment only. The two groups’ arms of the study were well matched and homogenous with respect to patient’s baseline characteristics (Table 1).
A significantly lower operative rate was observed in the GG group compared with the TT group. In the GG group, obstruction resolved subsequently in 31 cases (81.5%) after a mean time of 6.5 hours. After 36 hours from administration of GG, the radiological findings revealed complete mechanical obstruction in 13% of the patients and these 5 patients were submitted to laparotomy (1 of them required bowel resection for strangulation), whereas 33 (87%) patients showed a partial obstruction. After 72 hours of continuation of conservative treatment, only 2 of these 33 patients (6%) showed persistent radiological and clinical signs of obstruction and were taken to the operating room (Table 3).
In the control group after 36 hours of conservative treatment and observation, 11 of 38 patients needed surgical intervention because of the presence of clinical and radiological signs of complete mechanical obstruction; 2 of them suffered bowel strangulation and underwent bowel resection. On the other hand, 27 patients were not submitted to surgery and continued conservative treatment, and 21 of them did not require a delayed laparotomy after 72 hours. The remaining 6 of 27 patients who continued traditional conservative treatment up to 72 hours presented untreatable clinically and radiologically persistent obstruction requiring laparotomy. None of them required bowel resection. The difference in the overall operative rate between the two treatment groups (18.5% in the GG vs. 45% in TT group) reached statistical significance (p = 0.013; Table 3).
The time from the hospital admission for obstruction to resolution of symptoms was significantly lower among patients of GG group (6.4 vs. 43 hours; p < 0.01). Thus, the length of hospital stay revealed a marked reduction (4.67 days in GG group vs. 7.8 days in TT group; p < 0.05). This reduction was even higher compared with the length of hospital stay of the subgroups of those patients not submitted to surgery (3 vs. 5.13 days; p < 0.01; Fig. 2). Therefore, Gastrografin seemed to significantly shorten the duration of obstruction and subsequently the hospital stay. No GG-related complications were found. No allergic reactions or aspiration pneumonia were observed. No significant differences were observed in the incidence of major or minor complications between the two groups. Only three patients vomited after administration of GG, and it seemed to be a negative prognostic factor (2 of them were submitted to surgery; Table 4). The patients were followed up for a mean period of 19.5 months with no statistically significant difference in the relapse rate or hazard (Table 4; Fig. 3). The operative rate of the patients presenting relapses, the mean time to relapse, and the relapse-free survival period (24.6 months in GG submitted group vs. 20.1 in TT group) were not significantly different in the two groups (Table 4).
Discussion
Several studies with different designs investigated during the last years the diagnostic role of water-soluble contrast medium and focused on its therapeutic value in ASIO, producing controversial results (Table 5). One of the prominent problems in current studies on the use of water-soluble contrast in ASIO is the lack of uniform design, including patient population, study protocols, characteristics, and volume of contrast used.
Contrasted imaging may be helpful in patients with suspected intestinal obstruction, clarifying the presence of obstruction when the plain abdominal films and clinical findings are equivocal, whether the obstruction is partial or complete and possibly identifying its cause [26]. The use of barium may give precise mucosal detail and clearly delineate the anatomy, but is burdened with potential severe complications (peritonitis and aspiration). The water-soluble hyperosmotic solution is a safer alternative, with potential therapeutic value because of its ability to draw fluid into the bowel lumen, thus increasing the pressure gradient across the obstruction site and stimulating motility. Furthermore, it decreases intestinal wall edema, and its wetting agent facilitates the passage of bowel content. Level II data suggest that this effect may speed the return of bowel function and decrease the length of hospital stay of patients undergoing nonoperative management for partial small-bowel obstruction [27].
In 1994, Assalia reported significant reduction of the mean time for passing stools (6.2 vs. 23.3 hours; p < 0.01) and hospital stay (2.2 vs. 4.4 days; p < 0.01) associated with the use of hyperosmolar water-soluble contrast. No significant reductions in operative rate (10% vs. 21%; p = not significant (ns)) or Gastrografin-related complications were observed [6].
Feigin did not find any advantage in terms of reduction of operative rate, resolution of symptoms, and hospital stay [10]. Chen demonstrated that the presence of contrast (Urografin) in the colon within the first 24 hours predicts a successfully nonoperative treatment with a specificity of 100%, sensitivity of 98%, and accuracy of 99% [5, 28]. No significant differences were observed in a further study in the incidence of nonoperative resolution (31/48 vs. 35/50 patients; p = ns) and hospital stay between contrast and control group [9].
Given these previous controversial results, a prospective randomized trial from Choi was designed to assess the therapeutic value of Gastrografin in the management of ASIO after unsuccessful conservative treatment. The use of Gastrografin significantly reduced the need for surgery by 74%, in the absence of significant complications. The overall hospital stay was similar in both groups (10 days) [4]. However, this study does not really investigate the therapeutic role of Gastrografin, rather focusing its diagnostic value in predicting the need for surgery. These authors do not clarify the controversy of whether water-soluble oral contrast has additional therapeutic effects [20].
In a further randomized study, no significant differences in the operative rate, incidence of bowel strangulation requiring resection, and readmission rate were found between the two groups. Instead the overall hospital stay was significantly shorter in the Gastrografin group (4.1 vs. 8.5 days; p < 0.01) compared with control, as well as in both subgroups of patients who responded to conservative treatment or those surgically treated [11].
Burge et al. [24] randomized 45 patients with ASIO to receive Gastrografin or placebo in double-blind model. Patients did not undergo any further radiological investigation, and if they required subsequent radiological investigation or surgical intervention they were excluded. The patients who received Gastrografin experienced complete resolution of obstruction significantly earlier than placebo group (12 vs. 21 hours; p < 0.01) with shorter hospital stay (3 vs. 4 days; p < 0.05) [24]. The criticism is that patients who needed further radiological investigation or immediate surgery because of worsening of the clinical conditions were excluded. It represents a bias, including only the less severe cases presenting uneventful clinical course. Furthermore, the exclusion of patients needing surgery does not allow analysis of the operative rate. Finally, the decision not to perform further radiological investigations after administration of contrast/placebo and assessing the patients with only individual clinical judgment could delay surgery, which is potentially harmful and ethically questionable. One patient submitted later to surgery, for each group, died, but the death was not amenable to contrast administration.
Kapoor conducted a prospective study administering Gastrografin to patients who failed to improve after 48 hours of conservative treatment, noticing relief of obstruction in 22 of 24 patients [25]. This study suffers strong limitations due to the absence of a control arm and the inclusion criteria (only patients with partial obstruction).
In the meta-analysis from Abbas, the appearance of water-soluble contrast in the colon within 24 hours from its administration predicts the resolution of obstruction with a sensitivity of 97% and specificity of 96%. Furthermore, water-soluble contrast agent did not reduce the need for surgical intervention (p = ns) but reduces the length of hospital stay for patients who did not require surgery compared with placebo (p < 0.01) [29, 30].
Our trial, compared with the previous studies, demonstrates not only a shorter time to resolution of obstruction and shorter hospital stay period, but also a significant reduction of the operative rate in ASIO patients who received Gastrografin compared with those who underwent conservative treatment alone.
Conclusions
The use of Gastrografin in carefully selected ASIO patients is safe and reduces the operative rate, the time needed to resolution of obstruction and, as a result, the hospital stay, without influencing the adverse effects or recurrences incidence. Further randomized trials can confirm the therapeutic effect of hyperosmolar gastrointestinal water-soluble contrast agent.
References
Playforth RH, Holloway JB, Griffen WO Jr (1970) Mechanical small bowel obstruction: a plea for earlier surgical intervention. Ann Surg 171:783–788
Seror D, Feigin E, Szold A, Allweis TM, Carmon M, Nissan S, Freund HR (1993) How conservatively can postoperative small bowel obstruction be treated? Am J Surg 165:121–126
Matter I, Khalemsky L, Abrahamson J, Nash E, Sabo E, Eldar S (1997) Does the index operation influence the course and outcome of adhesive intestinal obstruction? Eur J Surg 163:767–772
Choi HK, Chu KW, Law WL (2002) Therapeutic value of Gastrografin in adhesive small bowel obstruction after unsuccessful conservative treatment: a prospective randomized trial. Ann Surg 236:1–6
Chen SC, Lin FY, Lee PH, Yu SC, Wang SM, Chang KJ (1998) Water-soluble contrast study predicts the need for early surgery in adhesive small bowel obstruction. Br J Surg 85:1692–1694
Assalia A, Schein M, Kopelman D, Hirshberg A, Hashmonai M (1994) Therapeutic effect of oral Gastrografin in adhesive, partial small-bowel obstruction: a prospective randomized trial. Surgery 115:433–437
Stordahl A, Laerum F, Gjolberg T, Enge I (1988) Water-soluble contrast media in radiography of small bowel obstruction. Comparison of ionic and non-ionic contrast media. Acta Radiol 29:53–56
Blackmon S, Lucius C, Wilson JP, Duncan T, Wilson R, Mason EM, Ramshaw B (2000) The use of water-soluble contrast in evaluating clinically equivocal small bowel obstruction. Am Surg 66:238–244
Fevang BT, Jensen D, Fevang J, Sondenaa K, Ovrebo K, Rokke O, Gislasson H, Svanes K, Viste A (2000) Upper gastrointestinal contrast study in the management of small bowel obstruction: a prospective randomised study. Eur J Surg 166:39–43
Feigin E, Seror D, Szold A, Carmon M, Allweis TM, Nissan A, Gross E, Vromen A, Freund R (1996) Water-soluble contrast material has no therapeutic effect on postoperative small-bowel obstruction: results of a prospective, randomized clinical trial. Am J Surg 171:227–229
Biondo S, Pares D, Mora L, Marti Rague J, Kreisler E, Jaurrieta E (2003) Randomized clinical study of Gastrografin administration in patients with adhesive small bowel obstruction. Br J Surg 90:542–546
Skucas J (1997) Anaphylactoid reactions with gastrointestinal contrast media. AJR Am J Roentgenol 168:962–964
Ridley LJ (1998) Allergic reactions to oral iodinated contrast agents: reactions to oral contrast. Australas Radiol 42:114–117
Trulzsch DV, Penmetsa A, Karim A, Evans DA (1992) Gastrografin-induced aspiration pneumonia: a lethal complication of computed tomography. South Med J 85:1255–1256
Stordahl A, Laerum F, Giolberg T, Enge I (1988) Water-soluble contrast media in radiography of small bowel obstruction. Comparison of ionic and non-ionic contrast media. Acta Radiol 29:53–56
Joyce WP, Delaney PV, Gorey TF, Fitzpatrick JM (1992) The value of water-soluble contrast radiology in the management of acute small bowel obstruction. Ann R Coll Surg Engl 74:422–425
Chung CC, Meng WC, Yu SC, Leung KL, Lau WY, Li AK (1996) A prospective study on the use of water-soluble contrast follow-through radiology in the management of small bowel obstruction. ANZ J Surg 66:598–601
Blackmon S, Lucius C, Wilson JP, Duncan T, Wilson R, Mason EM, Ramshaw B (2000) The use of water-soluble contrast in evaluating clinically equivocal small bowel obstruction. Am Surg 66:238–242
Onoue S, Katoh T, Shibata Y, Matsuo K, Suzuki M, Chigira H (2002) The value of contrast radiology for postoperative adhesive small bowel obstruction. Hepatogastroenterology 49:1576–1578
Choi HK, Law WL, Chu KW (2005) Value of Gastrografin in adhesive small bowel obstruction after unsuccessful conservative treatment: a prospective evaluation. World J Gastroenterol 11:3742–3745
Brochwicz-Lewinski MJ, Paterson-Brown S, Murchison JT (2003) Small bowel obstruction: the water-soluble follow-through revisited. Clin Radiol 58:393–397
Roadley G, Cranshaw I, Young M, Hill AG (2004) Role of Gastrografin in assigning patients to a non-operative course in adhesive small bowel obstruction. ANZ J Surg 74:830–832
Yagci G, Kaymakcioglu N, Can MF, Peker Y, Cetiner S, Tufan T (2005) Comparison of Urografin versus standard therapy in postoperative small bowel obstruction. J Invest Surg 18:315–320
Burge J, Abbas SM, Roadley G, Donald J, Connolly A, Bissett IP, Hill AG (2005) Randomized controlled trial of Gastrografin in adhesive small bowel obstruction. ANZ J Surg 75:672–674
Kapoor S, Jain G, Sewkani A, Sharma S, Patel K, Varshney S (2006) Prospective evaluation of oral Gastrografin in postoperative small bowel obstruction. J Surg Res 131:256–260
Practice management guidelines for small bowel obstruction (2007) Eastern Association for the Surgery of Trauma Practice Parameter Workgroup for Management of Small Bowel Obstruction. Available at: http://www.east.org
Thompson JS (2002) Contrast radiography and intestinal obstruction. Ann Surg 236:7–8
Chen SC, Chang KJ, Lee PH, Wang SM, Chen KM, Lin FY (1999) Oral Urografin in postoperative small bowel obstruction. World J Surg 23:1051–1054
Abbas S, Bisset IP, Parry BR (2005) Oral water-soluble contrast for the management of adhesive small bowel obstruction. Cochrane Database Syst Rev 25:1
Abbas S, Bisset IP, Parry BR (2007) Meta-analysis of oral water-soluble contrast agent in the management of adhesive small bowel obstruction. Br J Surg 94:404–411
Acknowledgments
Supported by the Department of Surgical and Anaesthesiological Sciences, University of Bologna, Sant’Orsola-Malpighi Hospital, Via Massarenti 9, 40138, Bologna, Italy. The authors thank all the patients who participated in this trial and all the physicians and nurses whose work made the trial possible.
Author’s Contribution and Acknowledgments
Conception and Design of the Study: F. Catena, L. Ansaloni
Direction of the Clinical Trial: F. Catena
Provision of study materials or patients: F. Catena, L. Ansaloni, M. Gavioli, M. Valentino
Collection and Assembly of Data: F. Catena, L. Ansaloni, S. Di Saverio
Data Analysis and Interpretation: F. Catena, L. Ansaloni, S. Di Saverio
Manuscript Writing: S. Di Saverio, F. Catena, L. Ansaloni
Final Approval of Manuscript: S. Di Saverio, F. Catena, L. Ansaloni, M. Gavioli, M. Valentino, A.D. Pinna
Author information
Authors and Affiliations
Corresponding author
Additional information
ClinicalTrials.gov IDentifier: NCT00601809.
This paper has been selected for and presented in the Lloyd M. Nyhus Prize session, Best Free Papers in gastrointestinal surgery, during the 2007 International Surgical Week conference in Montreal, Canada and it has been awarded by a jury of internationally recognized experts with the 2nd Prize for the Best ISS/SIC Free Paper presentation.
Rights and permissions
About this article
Cite this article
Di Saverio, S., Catena, F., Ansaloni, L. et al. Water-Soluble Contrast Medium (Gastrografin) Value in Adhesive Small Intestine Obstruction (Asio): A Prospective, Randomized, Controlled, Clinical Trial. World J Surg 32, 2293–2304 (2008). https://doi.org/10.1007/s00268-008-9694-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-008-9694-6