Abstract
Pancreatic necrosectomy remains an important treatment modality for the management of infected pancreatic necrosis but is associated with significant mortality. The aim of this study was to identify factors associated with mortality following pancreatic necrosectomy. Patients who underwent pancreatic necrosectomy from January 1995 to December 2004 were reviewed. The association between admission, preoperative and postoperative variables, and mortality was assessed using logistic regression analysis. A total of 1248 patients presented with acute pancreatitis, of whom 94 (7.5%) underwent pancreatic necrosectomy (51 men, 43 women). The preoperative median Acute Physiology, Age, and Chronic Health Evaluation (APACHE II) score was 9 (range 2–19). The median cumulative organ dysfunction score was 2 (0–9) preoperatively and 4 (1–11) postoperatively. In all, 23 patients (24.5%) died. Those who died were older than the survivors; the ages (median and range) were 69 years (40–80 years) versus 52 years (19–79 years) (p < 0.05). They also had higher admission APACHE II scores (median and range): 14 (12–19) versus 9 (2–22) (p < 0.001). There were significant associations between preoperative (p < 0.01) and postoperative (p < 0.01) Marshall scores and mortality following pancreatic necrosectomy. The presence of the systemic inflammatory response syndrome (SIRS) during the first 48 hours (p < 0.01) and the time between presentation and necrosectomy (p < 0.01) were independent predictors of survival. Pancreatic necrosectomy is associated with higher mortality in patients with increased APACHE II scores, early persistent SIRS, and unresolved multiorgan dysfunction. Necrosectomy is associated with poorer outcome when performed within 2 weeks of presentation.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Acute pancreatitis is a potentially serious condition with an overall mortality of 5% to 10% [1]. Mortality from acute pancreatitis has a bimodal distribution: There is a significant proportion of deaths arising as a result of multiorgan dysfunction during the first week of presentation [2, 3] and a later group of deaths occurring as a result of infected pancreatic necrosis [3]. Multiorgan dysfunction is a prominent feature of acute pancreatitis in the latter group of patients [4–9]. Sterile pancreatic necrosis is often treated conservatively [3], whereas infected pancreatic necrosis and peripancreatic abscess formation is an indication for surgery [3]. Surgery for pancreatic necrosis has traditionally been associated with significant mortality [4–9] and a high morbidity rate [10]. A variety of factors, such as age [5], early surgery [5, 11], severity of organ dysfunction [6, 12], extent of pancreatic necrosis [13], and the presence of fungal sepsis [14], have been associated with increased mortality following pancreatic necrosectomy.
The aim of this study was to identify preoperative and postoperative factors associated with mortality following pancreatic necrosectomy in a contemporary population of patients with delayed sepsis associated with necrotizing pancreatitis that could be identified preoperatively.
Methods
Patients who underwent pancreatic necrosectomy following presentation with acute pancreatitis from January 1995 to December 2004 were identified from a prospectively collected Lothian Surgical Audit (LSA) database [15]. Data from the database were supplemented by retrospective chart review and cross-referenced against the hospital laboratory databases. For each patient with acute pancreatitis, age, sex, highest preoperative serum C-reactive protein (CRP) level, and the presence of persistent systemic inflammatory response syndrome (SIRS) during the first 48 hours of presentation were recorded [16]. The Glasgow Severity Score was calculated at 48 hours and the Acute Physiology and Chronic Health Evaluation (APACHE II) scores were calculated on admission, preoperatively, and on the first postoperative day.
Organ dysfunction scores were calculated using the criteria proposed by Marshall et al. [17]. In this study the hepatic score was excluded to avoid the possibility of confounding effects due to biliary obstruction. Organ dysfunction was defined as a Marshall score of ≥2 for each organ system [17]. If this score increased or organ dysfunction (Marshall score of ≥2) developed in a new organ system, the patient was considered to have deteriorating multiorgan dysfunction syndrome (MODS) [17]. The cumulative Marshall organ dysfunction scores were calculated as the sum of the organ dysfunction scores for each of the four organ systems [17]. Marshall scores were calculated immediately preoperatively, and the highest postoperative score was recorded.
A baseline contrast-enhanced computed tomography (CT) scan was performed routinely in all patients with severe or suspected severe pancreatitis within 6 to 10 days of admission. The CT scan was repeated if there was evidence of progressive sepsis or multiorgan dysfunction despite supportive therapy or soon after transfer for patients who were tertiary referrals. The indication for surgical intervention was the presence of persistent sepsis associated with CT scan evidence of significant pancreatic necrosis and/or the presence of pancreatic abscess [18]. All patients were treated with broad-spectrum antibiotics, which included a second- or third-generation cephalosporin and metronidazole or pipercillin and tazobactam. In addition, patients with evidence of methicillin-resistant Staphylococcus aureus (MRSA) received intravenous vancomycin, and all patients who had fungal sepsis received appropriate intravenous antifungal therapy.
The operative technique employed has been described elsewhere [5, 19]. A bilateral transverse subcostal incision was used in most cases. Access to the lesser sac was obtained through the gastrocolic omentum or the transverse mesocolon. Blunt pancreatic and peripancreatic necrosectomy was performed using a mixture of hydrostatic dissection with warm normal saline and gentle digital dissection. Right and left paracolic gutters were mobilized only if there was CT evidence of abscess or collections in these sites and no formal pancreatic excision was performed [5]. In patients with suspected gallstone pancreatitis, cholecystectomy and intraoperative cholangiography was performed when technically possible. At the end of the procedure two large-bore Silastic drains were placed in the lesser sac, and in most patients a feeding jejunostomy or gastrostomy was fashioned. Recently, a small proportion of patients underwent minimally invasive retroperitoneal pancreatic necrosectomy (MIRP) using the previously described methodology [20].
Statistical analysis
Statistical analysis was performed using Statistical Package for Social Sciences (SPSS) version 12 (SPSS, Chicago, IL, USA) software. To avoid distributional assumptions, values were stated as the median and range, and nonparametric statistical tests (χ2, Mann-Whitney, Kruskall-Wallis tests) were used. Stepwise logistic regression analysis was used to identify preoperative predictors of mortality following pancreatic necrosectomy. The diagnostic odds ratio was determined for each predictor at the optimal cutoff levels, which were derived using receiver operator characteristic analysis (preoperative APACHE II score ≥8, SIRS on admission, Glasgow Severity Score ≥4, surgery within 14 days of presentation, preoperative serum CRP ≥150 mmol/L). Similarly, stepwise logistic regression analysis was used to identify postoperative predictors of mortality.
Results
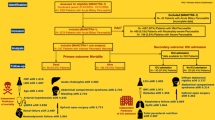
A total of 1248 consecutive patients presented with acute pancreatitis, of whom 307 (24.5%) developed severe acute pancreatitis. The etiology of the acute pancreatitis was gallstones in 579 patients (46.4%), alcohol-related in 386 patients (31%), postendoscopic retrograde cholangiopancreatography in 35 patients (2.8%), and other causes in 51 patients (4.1%); 197 patients (15.7%) presented with idiopathic pancreatitis.
The overall mortality during the index admission was 7.9% (98/1248). In total, 233 (18.9%) had evidence of significant pancreatic necrosis on contrast-enhanced CT scans: 73 of them were treated nonoperatively for sterile pancreatic necrosis; 21 were treated palliatively due to advanced age, severe co-morbidity or previously diagnosed metastatic carcinoma; and 45 died as a result of progressive MODS during the first 2 weeks of presentation without surgical intervention.
Altogether, 94 patients (7.5%) (51 men, 43 women) with a median age of 54 years (range 21–80 years) underwent pancreatic necrosectomy. The median time between presentation and surgery was 31 days (range 5–69 days). Open pancreatic necrosectomy was performed in 87 patients (92.5%), and 7 patients (7.5%) underwent MIRP. A total of 36 patients (38.3%) were tertiary referrals. The median APACHE II score on admission was 13 (range 5–22). Altogether, 61 patients (65%) who underwent pancreatic necrosectomy had SIRS during the first 48 hours after admission.
The median preoperative CRP level was 260 mmol/L (range 26–451 mmol/L). The median preoperative APACHE II score was 9 (range 2–19), which was significantly lower than the median postoperative APACHE II score (11.5; range 2–22) (p = 0.012). The median cumulative Marshall organ dysfunction score was 2 (range 0–9) preoperatively and 4 (range 1–11) postoperatively (p = 0.032). A close correlation was observed between the preoperative APACHE II scores and the cumulative Marshall scores (r 2 = 0.34, p < 0.01).
A total of 29 patients underwent more than one procedure. Table 1 describes the indications for and types of reoperative procedures. Nine patients (9.6%) developed postoperative pancreatic fistulas, and 3 (3.2%) developed enterocutaneous fistulas. The median hospital stay was 43 days (range 12–194 days).
Altogether, 23 patients (24.5%) died. Those who died were older than those who survived (median age and range): 69 years (40–80 years) vs. 52 years (19–79 years) (p = 0.042). The patients who did not survive had higher admission APACHE II scores (median and range): 12 (7–19) vs. 7 (2–13) (p = 0.008) (Fig. 1) and a higher incidence of persistent SIRS during the first 48-hours of presentation [21 patients (91.3%) vs. 40 patients (56.5%); χ2 = 9.32, p = 0.01].
Box and whisker plot comparing the Acute Physiology, Age, and Chronic Health Evaluation (APACHE) II scores on admission between patients who survived (n = 71) and patients who died (n = 23). The thick black lines represent median values, boxes represent the interquartile range, whiskers represent the outliers, and the individual dots are extreme values
Patients who died had higher preoperative APACHE II scores [median and range: 14 (12–19) vs. 10 (2–23); p < 0.001] (Fig. 2) and higher preoperative serum C-reactive protein (CRP) levels [median and range: 350 mmol/L (112–451 mmol/L) vs. 243 mmol/L (26–440 mmol/L); p < 0.05] than survivors. They also had a higher preoperative cumulative Marshall organ dysfunction score [median and range: 5 (3–9) vs. 2 (0–6); p = 0.007] (Fig. 3) than the survivors. Pancreatic necrosectomy within 2 weeks of presentation was associated with significantly higher mortality than surgery after 2 weeks (p < 0.01) (Fig. 4).
Box and whisker plot comparing the preoperative cumulative Marshall multiorgan dysfunction scores between patients who survived (n = 71) and patients who died (n = 23). The thick black lines represent median values, boxes represent the interquartile range, whiskers represent the outliers, and the individual dots are extreme values
Patients who died had significantly higher postoperative APACHE II scores [median 15 (range 7–22)] compared with patients who survived [median 10 (range 5–16)] (p = 0.002). Similarly postoperative cumulative Marshall scores were significantly higher in patients who died [median 8 (range 5–11)] compared with those who survived [median 2 (range 1–5)] (p < 0.001).
Logistic regression analysis revealed that admission APACHE II scores (p = 0.026), persistent SIRS during the first 48 hours (p < 0.01), and time between presentation and necrosectomy (p < 0.01) were independent preoperative predictors of mortality (Table 2), and postoperative APACHE II scores (p = 0.022) and postoperative deterioration in MODS (p = 0.03) were independent postoperative predictors of mortality (Table 3).
Among the 71 survivors, 38 patients (53.5%) developed chronic pancreatic exocrine insufficiency requiring long-term pancreatic enzyme replacement, 25 patients (35.2%) developed diabetes, 14 patients (19.7%) suffered chronic abdominal pain, 3 patients developed biliary strictures, and 2 developed pancreatic duct strictures requiring surgical intervention. Two patients had chronic pancreatic collections that did not resolve following endoscopic or percutaneous therapy; one of these patients required open cystogastrostomy, and the other was treated successfully by distal pancreatectomy.
Discussion
Without necrosectomy the mortality rate from infected pancreatic necrosis approaches 100% [5]. Pancreatic necrosectomy remains the treatment of choice for infected pancreatic necrosis [5–11]. However, it is associated with considerable perioperative morbidity and mortality and a prolonged hospital stay, utilizing considerable resources [5].
Pancreatic necrosectomy is still associated with significant mortality. In this study almost one-fourth of the patients who underwent pancreatic necrosectomy died during the postoperative period. Wide variations exist in the reported mortality following pancreatic necrosectomy, with mortality rates ranging from 7.7% to 43.0% [5–11, 21]. This relates in part to the variation in patient population. Although lower mortality rates have been reported by some authors [21], the results of this study compare favorably with similar series originating from the United Kingdom and other northern European populations in whom pancreatitis tends to affect older patients with more significant co-morbidity [5, 22–25]. Undoubtedly, the variation in mortality among series is also related to the variation in indications for and timing of surgical intervention that have evolved over the last decade.
In this study, preoperative organ dysfunction scores and APACHE II scores were significantly higher in patients who died following pancreatic necrosectomy. The severity of preoperative MODS correlated with high admission and preoperative APACHE II scores. The association between APACHE II scores on admission and mortality is an indication of the severity of the organ dysfunction caused by the disease process, and the preoperative APACHE II score is an indication of the degree of unresolved MODS prior to necrosectomy [5]. Both Rattner et al. [7] and Connor et al. [5] have reported higher admission and preoperative APACHE II scores in patients who do not survive pancreatic necrosectomy. In addition, Connor et al. observed that APACHE II scores and patients’ age were the only two independent predictors of survival following pancreatic necrosectomy [5].
Postoperative organ dysfunction has also been shown to be an independent risk factor for mortality. Buter et al. reported a close correlation between the development of persistent MODS and death from acute pancreatitis [26]. The temporal relation between early MODS and the development of pancreatic necrosis remains an area of interest, as the trend in managing sterile pancreatic necrosis is toward conservative treatment, irrespective of the extent of pancreatic necrosis. Isenman and coworkers reported that although the extent of sterile pancreatic necrosis is an independent predictor of distant organ failure a high incidence of organ failure occurred in the presence of infected necrosis irrespective of the extent of pancreatic necrosis [22].
In this study, a close association between the persistence of SIRS during the first 48 hours of admission and death following surgery for infected pancreatic necrosis was observed. This is despite the fact that the presence and severity of sepsis are built into prognostic scoring systems such as APACHE II. Early persistent SIRS has been found to correlate closely with the severity of MODS and death from acute pancreatitis [27].
The timing of surgery was found to have a major impact on survival from pancreatic necrosectomy, with early surgery being associated with increased risk of death. This has also been observed by previous authors [5, 23–25, 28]. A randomized controlled trial comparing pancreatic necrosectomy during the first 12 days following admission with surgery delayed beyond 12 days revealed significantly higher mortality in the early surgery group [28]. A recent observational study by Runzi et al. found that in patients with infected pancreatic necrosis it is possible to avoid or delay surgery with prophylactic use of antibiotic therapy without compromising the prognosis or outcome [29].
The recent advent of MIRP is a promising development in the management of infected pancreatic necrosis. In the present study, because of the small number of patients who underwent MIRP, it was not possible to draw any meaningful comparisons with the open pancreatic necrosectomy group. Connor et al. reported that MIRP was associated with less utilization of intensive trauma unit care and improved survival compared to open surgery [5]. However, MIRP is associated with an increased number of procedures and longer inpatient stay compared with open necrosectomy [5, 20]. The outcome following MIRP compared to open pancreatic necrosectomy remains to be examined by a multicenter randomized controlled trial [5], although the initial experience with MIRP is promising [5, 20, 30, 31].
In this study, a significant proportion of patients who survived surgery for pancreatic necrosis developed delayed complications, such as diabetes, pancreatic fistulas, and pancreatic exocrine insufficiency. There is increasing recognition that the incidence of long-term, pancreatic exocrine insufficiency in patients who develop necrotizing pancreatitis may be higher than what has been reported in the literature [5]. Bozkurt et al. reported that 12 months after recovery from pancreatic necrosectomy only 16% of the patients showed a normal pancreatic response, and 84% still had pancreatic insufficiency of variable severity [32]. Recent work by Symersky et al. suggests that after recovery from acute pancreatitis long-term exocrine insufficiency was common even among patients with mild acute pancreatitis [33].
Conclusions
Surgery for infected pancreatic necrosis is associated with significant morbidity and mortality but may be life-saving. Pancreatic necrosectomy is associated with higher mortality rates among patients with high APACHE II scores and those with unresolved multiorgan dysfunction. This study also highlights the association between the systemic inflammatory response early in the natural history of acute pancreatitis and subsequent mortality in this cohort of patients.
Efforts to reduce the mortality among patients requiring surgery for infected pancreatic necrosis should focus on intensive multidisciplinary supportive measures to optimize organ function so operative intervention can be delayed to at least the third week in the course of the illness if possible.
References
Triester SL, Kowdley KV (2002) Prognostic factors in acute pancreatitis. J Clin Gastroenterol 34:167–176
Mitchell RM, Byrne MF, Baillie J (2003) Pancreatitis. Lancet 361:1447–1455
Werner J, Feuerbach S, Uhl W, et al. (2005) Management of acute pancreatitis: from surgery to interventional intensive care. Gut 54:426–436
Isenmann R, Rau B, Beger HG (2001) Early severe acute pancreatitis: characteristics of a new subgroup. Pancreas 22:274–278
Connor S, Ghaneh P, Raraty M, et al. (2003) Increasing age and APACHE II scores are the main determinants of outcome from pancreatic necrosectomy. Br J Surg 90:1542–1548
Beattie GC, Mason J, Swan D, et al. (2002) Outcome of necrosectomy in acute pancreatitis: the case for continued vigilance. Scand J Gastroenterol 37:1449–1453
Rattner DW, Legermate DA, Lee MJ, et al. (1992) Early surgical debridement of symptomatic pancreatic necrosis is beneficial irrespective of infection. Am J Surg 163:105–109
Oleynikov D, Cook C, Sellers B, et al. (1998) Decreased mortality from necrotizing pancreatitis. Am J Surg 176:648–653
Karimgani I, Porter KA, Langevin RE, et al. (1992) Prognostic factors in sterile pancreatic necrosis. Gastroenterology 103:1636–1640
Connor S, Alexakis N, Raraty MG, et al. (2005) Early and late complications after pancreatic necrosectomy. Surgery 137:499–505
Kivilaakso E, Fraki O, Nikki P, et al. (1981) Resection of the pancreas for fulminant pancreatitis. Surg Gynecol Obstet 152:493–498
Le Mee J, Paye F, Sauvanet A, et al. (2001) Incidence and reversibility of organ failure in the course of sterile or infected necrotizing pancreatitis. Arch Surg 136:1386–1390
Beger HG, Bittner R, Block S, et al. (1986) Bacterial contamination of pancreatic necrosis: a prospective clinical study. Gastroenterology 91:433–438
Connor S, Alexakis N, Neal T, et al. (2004) Fungal infection but not type of bacterial infection is associated with a high mortality in primary and secondary infected pancreatic necrosis. Dig Surg 21:297–304
Aitken RJ, Nixon SJ, Ruckley CV (1997) Lothian surgical audit: a 15-year experience of improvement in surgical practice through regional computerised audit. Lancet 350:800–804
Bone RC (1996) Immunologic dissonance: a continuing evolution in our understanding of the systemic inflammatory response syndrome and multiple organ dysfunction syndrome (MODS). Ann Intern Med 125:680–687
Marshall JC, Cook DJ, Christou NV, et al. (1995) Multiple organ dysfunction score: a reliable descriptor of a complex clinical outcome. Crit Care Med 23:1638–1652
Uhl W, Warshaw A, Imrie C, et al. (2002) IAP guidelines for the surgical management of acute pancreatitis. Pancreatology 2:565–573
Beger HG, Buchler M, Bittner R, et al. (1988) Necrosectomy and postoperative local lavage in necrotizing pancreatitis. Br J Surg 75:207–212
Connor S, Ghaneh P, Raraty M, et al. (2003) Minimally invasive retroperitoneal pancreatic necrosectomy. Dig Surg 20:270–277
Farkas G, Marton J, Mandi Y, et al. (2006) Surgical management and complex treatment of infected pancreatic necrosis: 18-year experience at a single center. J Gastrointest Surg 10:278–285
Isenmann R, Rau B, Beger HG (1999) Bacterial infection and extent of necrosis are determinants of organ failure in patients with acute necrotizing pancreatitis. Br J Surg 86:1020–1024
Hungness ES, Robb BW, Seeskin C, et al. (2002) Early debridement for necrotizing pancreatitis: is it worthwhile? J Am Coll Surg 194:740–744
Hartwig W, Maksan SM, Foitzik T, et al. (2002) Reduction in mortality with delayed surgical therapy of severe pancreatitis. J Gastrointest Surg 6:481–487
Tzovaras G, Parks RW, Diamond T, et al. (2004) Early and long-term results of surgery for severe necrotising pancreatitis. Dig Surg 21:41–46
Buter A, Imrie CW, Carter CR, et al. (2002) Dynamic nature of early organ dysfunction determines outcome in acute pancreatitis. Br J Surg 89:298–302
Mofidi R, Duff MD, Wigmore SJ, et al. (2006) Association between early systemic inflammatory response syndrome, severity of multiorgan dysfunction and death in acute pancreatitis. Br J Surg 93:738–744
Mier J, Leon E, Castillo A, et al. (1997) Early versus late necrosectomy in severe necrotizing pancreatitis. Am J Surg 173:71–75
Runzi M, Niebel W, Goebell H, et al. (2005) Severe acute pancreatitis: nonsurgical treatment of infected necroses. Pancreas 30:195–199
Carter CR, McKay CJ, Imrie CW (2000) Percutaneous necrosectomy and sinus tract endoscopy in the management of infected pancreatic necrosis: an initial experience. Ann Surg 232:175–180
Risse O, Auguste T, Delannoy P, et al. (2004) Percutaneous video-assisted necrosectomy for infected pancreatic necrosis. Gastroenterol Clin Biol 28:868–871
Bozkurt T, Maroske D, Adler G (1995) Exocrine pancreatic function after recovery from necrotizing pancreatitis. Hepatogastroenterology 42:55–58
Symersky T, van Hoorn B, Masclee AA (2006) The outcome of a long-term follow-up of pancreatic function after recovery from acute pancreatitis. J Pancreas 7:447–453
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was presented at the 39th annual congress of the European Pancreatic Club, Graz, Austria, July 2005.
Rights and permissions
About this article
Cite this article
Mofidi, R., Lee, A.C., Madhavan, K.K. et al. Prognostic Factors in Patients Undergoing Surgery for Severe Necrotizing Pancreatitis. World J Surg 31, 2002–2007 (2007). https://doi.org/10.1007/s00268-007-9164-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-007-9164-6