Abstract
Background
This study investigated the effects of lipofilling on both the functional and the aesthetic aspects of breast reconstruction.
Methods
Sixty-one consecutive patients with irradiated reconstructed breasts (62 breasts) were offered free fat transfer to enhance the results and correct the defects. Twenty patients were enrolled (active branch) and underwent multiple sessions of lipofilling, while the others were considered controls. The fat was harvested by syringe and processed by saline washing only (no centrifugation). Three months after the last session the functional outcome was evaluated using the LENT-SOMA scoring system and the aesthetic outcome was evaluated using a visual 5-point scale.
Results
A significant improvement in all the LENT-SOMA scores after free fat grafting was observed; the scores after treatment were all significantly lower than those before it and were also significantly lower than those of untreated breasts. These results also were confirmed by comparing homogeneous subgroups of breasts with similar LENT-SOMA ranks before treatment. Similarly, the cosmetic outcomes were significantly enhanced after serial lipofilling. The four cases in the active branch with severe flap thinning resolved with no implant exposure (mean follow-up = 17.6 months), while implant exposure occurred in the two cases with the same problem in the control group. In one case, a Baker 3-4 capsular contracture was downgraded to Baker 1 after only one session of lipofilling. No complications occurred in the treated cases.
Conclusion
Free fat transfer is a safe and reliable technique in improving the outcomes of irradiated reconstructed breasts with implants.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Radiotherapy can significantly raise the risk of flap failure, implant exposure, infections, and capsular contracture in prosthetic breast reconstructions. The final aesthetic results can also be compromised due to hypodermic liponecrosis. However, the need for radiotherapy is not always predictable when choosing a reconstructive procedure, and in some cases an autologous reconstruction is not feasible. Recent studies have begun to challenge the dogma of the relative contraindication of radiotherapy after prosthetic reconstruction. On the other hand, many studies have discussed the role of free fat grafts in tissue regeneration [1]. The present study investigates the usefulness of serial fat grafting in irradiated prosthetic breast reconstructions.
Materials and Methods
From January 2006 to January 2008, 62 irradiated breasts in 61 patients (one bilateral case) were reconstructed with prostheses after mastectomy for carcinoma. The patients were then offered autologous free fat transplant and 20 of them were enrolled. Forty-two breasts (group 1, control) received standard treatment only and the remaining 20 breasts underwent serial free fat grafts (group 2, active branch).
Wet infiltration (0.5% lidocaine + epinephrine, 1:200,000 in saline solution) was performed using a 10-cc syringe. The autologous fat was then harvested from the abdomen, the hips, or the trochanteric area using a 3-mm cannula (1-hole, bullet tip) and a 10-cc syringe. The fat was then gently washed and decanted with saline. There was no centrifugation. Using the same syringes used for harvesting and a 14G needle, the graft was implanted into parallel tunnels on multiple layers in the depressed areas, with minimal overcorrection (10-15%), under the scars, and in the areas covered by dystrophic skin. Fat implantation was repeated after a minimum of 20 days until the result was stable or the patient was satisfied.
The functional results were evaluated before fat transplant (T0) and about 3 months after the last session of lipografting (T1) using the LENT-SOMA scoring system. The aesthetic results were evaluated using a 5-point scale (5 = very good, 4 = good, 3 = acceptable, 2 = poor, 1 = very poor) at T0 and at T1. The measures are expressed as mean ± standard deviation (SD). The data were analyzed using the unpaired Student’s t test (for interval variables) and the Wilcoxon two sample test (for ordinal variables).
The present study conformed to the World Medical Association Declaration of Helsinki (June 1964) and subsequent amendments.
Results
The mean age of the patients was 49.1 ± 9.4 years (49.4 ± 9.6 years for group 1 and 48.3 ± 9.1 years for group 2, p = 0.342). All patients presented mild to severe superficial irregularities and different degrees of skin dystrophy. Six breasts showed a severe flap thinning (two in group 1 and four in group 2). Two reconstructions developed capsular contracture (one in group 1 and one in group 2). The LENT-SOMA scores of the breasts in group 1 were comparable to those in group 2 at T0 (Table 1).
The fat grafts were harvested from the hips (57%), the abdomen (30%), or the trochanteric area (12%). The mean number of sessions performed on each reconstructed breast was 3.4 ± 1.9 (range = 1–7 sessions) with an average volume of 24.5 ± 10.8 cc of autologous fat injected in each session (range = 8–50 cc). The average interval between two sessions was 75.9 ± 61.3 days (range = 22–263 days).
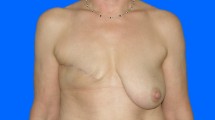
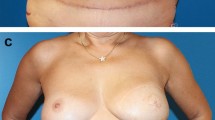
All the objective criteria of the LENT-SOMA scoring system significantly improved in group 2 after serial lipografting (Table 1, T0 vs. T1). The improvement was significant for both the flaps with no or mild effects (score 0 or 1), except for breast edema, and the flaps with moderate or severe effects (scores 2-3 or 4 when applicable) as shown in Table 2. Superficial irregularities completely resolved in 11 cases and significantly improved in the remaining 9 cases (Figs. 1 and 2).
Implant exposure requiring prosthesis removal occurred in the two cases of the severely thinned flaps in group 1. On the other hand, all four thinned flaps in group 2 improved after fat transfer (Fig. 3) and there was no implant exposure after a mean follow-up of 17.6 ± 6.7 months (p = 0.066667).
The Baker 3-4 capsular contracture in group 2 surprisingly was downgraded to Baker 1 after only one fat transfer session and no contracture relapse was observed after 20.3 months (Fig. 4).
The average aesthetic outcome (3.1 ± 1.6) of the reconstructions in group 1 was similar to that in group 2 at T0 (2.7 ± 0.8, p ≤ 0.1827). The mean aesthetic result in group 2 was significantly improved at T1 (4.3 ± 0.6) vs. at T0 (2.7 ± 0.8, p ≤ 0.0004778). The average aesthetic result was significantly worse in group 1 (3.1 ± 1.6) than in group 2 at T1 (4.3 ± 0.6, p ≤ 0.03167). There were no significant complications.
Discussion
The need for radiotherapy is generally considered a relative contraindication for prosthetic breast reconstruction, although some works recently have challenged this dogma [2]. On the other hand, a number of studies recently demonstrated the reliability [3, 4], long-term stability [5], and safety [6, 7] of autologous free fat transplantation in breast reconstruction. In some studies, lipofilling was applied to irradiated breast reconstructions [1]. These works pointed out the regenerative property of autologous fat that is linked to the adipose tissue-derived stem cells (ADSC). The loss of regenerative cells is thought to be the main reason for the late effects of radiotherapy and ADSC are supposed to be able to partially restore the microvascular pattern (neovessel formation) and improve hydration [1]. The great advantage of free fat transfer is its low invasiveness and low morbidity.
In our study, a relatively small volume of fat was implanted in multiple sessions. The main reason for this is that in general fibrosis makes it difficult to leave space for larger volumes of fat. Also, in our series there was no need for great volume replacements.
We preferred syringe aspiration with no tumescent technique to try to better preserve the adipocytes. No centrifugation was performed for the same reason. The fat was processed only by gentle washing with saline to eliminate blood and debris.
Comparisons of functional outcome were made using the LENT-SOMA scoring system, which is considered the most effective validated tool to analyze the late effects of radiotherapy [8]. A visual 5-points scale was used to evaluate aesthetic outcomes. The present study showed that there was a significant improvement in all the objective criteria of the LENT-SOMA scoring system after free fat grafting. In particular, the scores after treatment (group 2 T1) were all significantly lower than before it (group 2 T0). Also, even though the active branch and the controls had similar degrees of late effects of radiotherapy before lipofilling, the scores after treatment in group 2 (T1) were significantly lower than in group 1. These results were confirmed by comparing homogeneous subgroups of breasts with similar LENT-SOMA ranks before treatment. In particular, a significant improvement was recorded among breasts that showed no or mild effects of radiotherapy (excluding only breast edema). This may confirm a radical change in the skin ultrastructure after free fat transplant.
Similarly, the cosmetic outcomes were significantly enhanced after serial lipofilling. This mainly stems from the resolution of superficial irregularities, reduction of fibrosis related deformities, and scar improvement.
Although not statistically significant, probably because of the sample size, none of the breasts with severe flap thinning before treatment showed implant exposure after serial free fat transplantation, while the two thinned flaps in group 1 were reconstruction failures. Free fat grafts may thus play a possible role in salvaging reconstruction and in preventing implant exposures.
Another interesting result was the evident downgrading in capsular contracture observed in one case after only one fat transfer session. Some studies have shown that the mean concentration of collagen is two times higher in irradiated skin than in nonirradiated skin thus leading to fibrosis [9, 10]. Fibroblast-like cells were proven to be the most common cell type in the contracted capsules along with inflammatory cells [11]. One study has suggested that ADSCs can promote dermal fibroblast proliferation by paracrine activation through secretory factors [12]. The same study demonstrated that the concentrations of type I collagen and fibronectin induced by ADSC were found to be at least 1000-fold higher than those of several growth factors. For that reason, it is difficult to explain how free fat grafts can improve both fibrosis and capsular contracture. Maybe a regulatory activity mediated by the secretion of cytokines should be hypothesized. Further studies are necessary to better understand this behavior.
No complications occurred in the present series. One must be careful not to puncture the implant, particularly when an extremely thin flap is being treated. In such cases, the implant should be protected by gently squeezing it away from the thinned area. In our opinion, autologous free fat transplantation should be offered to the patient when performing reconstruction with implants in irradiated breasts.
Conclusion
The present study confirms that free fat grafts can greatly improve both functional and aesthetic results and reduce the incidence of complications. Free fat transplantation contributes strongly to challenging the dogma of the relative contraindication of prosthetic reconstruction in irradiated breasts.
References
Rigotti G, Marchi A, Galiè M, Baroni G, Benati D, Krampera M, Pasini A, Sbarbati A (2007) Clinical treatment of radiotherapy tissue damage by lipoaspirate transplant: a healing process mediated by adipose-derived adult stem cells. Plast Reconstr Surg 119:1409–1422
Percec I, Bucky LP (2008) Successful prosthetic breast reconstruction after radiation therapy. Ann Plast Surg 60:527–531
Missana MC, Laurent I, Barreau L, Balleyguier C (2007) Autologous fat transfer in reconstructive breast surgery: indications, technique and results. Eur J Surg Oncol 33:685–690
Spear SL, Wilson HB, Lockwood MD (2005) Fat injection to correct contour deformities in the reconstructed breast. Plast Reconstr Surg 116:1300–1305
Zheng DN, Li QF, Lei H, Zheng SW, Xie YZ, Xu QH, Yun X, Pu LL (2008) Autologous fat grafting to the breast for cosmetic enhancement: experience in 66 patients with long-term follow up. J Plast Reconstr Aesthet Surg 61:792–798
Amar O, Bruant-Rodier C, Lehmann S, Bollecker V, Wilk A (2008) Fat tissue transplant: restoration of the mammary volume after conservative treatment of breast cancers, clinical and radiological considerations. Ann Chir Plast Esthet 53:169–177
Gosset J, Guerin N, Toussoun G, Delaporte T, Delay E (2008) Radiological evaluation after lipomodelling for correction of breast conservative treatment sequelae. Ann Chir Plast Esthet 53:178–189
Hoeller U, Tribius S, Kuhlmey A, Grader K, Fehlauer F, Alberti W (2003) Increasing the rate of late toxicity by changing the score? A comparison of RTOG/EORTC and LENT/SOMA scores. Int J Radiat Oncol Biol Phys 55:1013–1018
Autio P, Saarto T, Tenhunen M, Elomaa I, Risteli J, Lahtinen T (1998) Demonstration of increased collagen synthesis in irradiated human skin in vivo. Br J Cancer 77:2331–2335
Riekki R, Parikka M, Jukkola A, Salo T, Risteli J, Oikarinen A (2002) Increased expression of collagen types I and III in human skin as a consequence of radiotherapy. Arch Dermatol Res 294:178–184
Prantl L, Pöppl N, Horvat N, Heine N, Eisenmann-Klein M (2005) Serologic and histologic findings in patients with capsular contracture after breast augmentation with smooth silicone gel implants: is serum hyaluronan a potential predictor? Aesthetic Plast Surg 29:510–518
Won-Serk K, Byung-Soon P, Jong-Hyuk S, Jun-Mo Y, Seok-Beom P, Sahng-June K, Jeong-Soo P (2007) Wound healing effect of adipose-derived stem cells: a critical role of secretory factors on human dermal fibroblasts. J Dermatol Sci 48:15–24
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Panettiere, P., Marchetti, L. & Accorsi, D. The Serial Free Fat Transfer in Irradiated Prosthetic Breast Reconstructions. Aesth Plast Surg 33, 695–700 (2009). https://doi.org/10.1007/s00266-009-9366-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-009-9366-4