Abstract
Background
Most patients with blepharoptosis prefer to undergo a double eyelid operation and a ptosis repair simultaneously to achieve the optimal cosmetic and functional result. However, it is difficult to achieve symmetry in patients with blepharoptosis.
Methods
Surgery was performed on the levator aponeurosis or frontalis muscle to correct blepharoptosis while double eyelid surgery was simultaneously performed to correct blephroptosis in 264 patients over the past 15 years. This report describes 39 representative cases of unilateral congenital blepharoptosis and 30 representative cases of bilateral congenital blepharoptosis. In cases of unilateral ptosis with good or fair levator function, a levator resection or plication was performed, and the position of the lid margin was adjusted to 1 to 2 mm below the upper limbus. Cases of severe unilateral blepharoptosis were corrected by frontalis muscle flap, orbicularis oculi muscle flap, or frontalis myofacial flap, and the height of the double eyelid was created to be 1 to 2 mm less than the height on the normal side. The position of the lid margin was adjusted to the level of the superior limbus, and the height of the lid crease of the ptotic eye was determined to be according to that on the nonptotic side. For bilateral ptosis patients with equal levator function, the height of the double eyelid was designed symmetrically. Bilateral blepharoptosis patients with unequal levator muscle function should have the double eyelids on both sides created the same as in normal cases, and they must be grafted in proportion to the severity of the blepharoptosis. If the results are unpredictable, the two-stage operation should be performed.
Results
Only 30% of the eyelids in this study were perfectly symmetric after the blepharoptosis operation, with 70% asymmetric. These 70% showed good symmetry immediately after surgery, but asymmetry occurred 6 months after the operation.
Conclusion
In blepharoptosis surgery, different techniques for double eyelids must be applied according to the method of ptosis correction used. Usually, the height of the double eyelid on the ptotic side should be a little less than the normal double eyelid height on the nonptotic side. However, it is difficult to achieve symmetric double eyelids in blepharoptosis patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
For correction of blepharoptosis, most adult patients desire surgery not only for aesthetic reasons, but also for correction of problems such as visual disturbance. They tend to want double eyelid construction to be performed simultaneously with the blepharoptosis correction so that their heavy and unsightly eyelid will appear light and soft.
To achieve satisfactory aesthetic results, it is crucial not only to correct the blepharoptosis, but also to make the double eyelids symmetric with each other. However, if the levator palpebrae muscle function of a blepharoptosis patient is not the same on both sides, double eyelid constructions frequently result in asymmetric eye shapes that are not aesthetically pleasing. Thus, if the height of the double eyelid on the ptotic side is identical to that on the nonptotic side, double eyelid surgery will cause the ptotic side to appear larger than the nonptotic side when the patient looks straight ahead because the function of the levator palpebrae superioris muscle on the ptotic side will be weaker than the muscle function on the other side. In fact, Melaine H. Erb and others have reported that 17% of blepharoptosis patients will experience more than a 1-mm decrease in contralateral eyelid height [1]. Therefore, it is difficult to create lasting symmetric height in double eyelids.
To achieve this symmetry, the double eyelid on the lesion side must be created the same as on the contralateral normal side so that the two eyes appear identical in form. We report the results of combining blepharoptosis surgery with double eyelid construction for 39 patients with congenital unilateral blepharoptosis and 30 patients with bilateral blepharoptosis from among the blepharoptosis patients treated in our department over the past 15 years.
Materials and Methods
Between January 1990 to December 2004, among 264 patients who underwent simultaneous surgeries for double eyelid construction and correction of congenital blepharoptosis, 69 patients (99 lids) who could participate in a postoperative follow-up study were chosen as the subjects for this research. The results of combining the blepharoptsis surgery with double eyelid construction were investigated by evaluation of issues such as the methods of blepharoptosis correction and double eyelid construction, the height of the postoperative palpebral fissures, the height and symmetry of the double eyelids, the surgical complications, and the satisfaction of both the patients and the doctors involved (Table 1).
Of the 69 subjects (48 males and 21 females) chosen, 39 were unilateral and 30 were bilateral cases. The bilateral cases included 12 cases in which the levator muscle function of both upper eyelids was identical. The patients’ ages ranged from 2 to 40 years (average, 18.9 years).
Preoperative Evaluation
Before the operation, the severity of the patient’s blepharoptosis was determined, and the levator function was measured. Also, ophthalmic evaluations such as the existence of Bell’s phenomenon, the Marcus Gunn phenomenon, ambliopia, and strabismus were examined.
It is important to know the extent of the levator function and the patient’s vision status. Opened eye can develop after ptosis surgery, leading to symptoms of dry eye. Because of this, preoperative evaluation of eye tearing, by history and by Schirmer’s test, is important [2].
In this study, the function of the levator muscle, the most crucial criteria for choosing the operation method, was evaluated by measuring the functional capacity of this muscle using Berke’s method. The levator function was measured from the difference in the heights of upper lid margins with the patient looking lowest and highest after the surgeon pressed the eyebrows to stop the function of the frontalis muscle [3].
After the levator muscle function was measured, the results were classified as excellent (≥13 mm), good (8–12 mm), fair (5–7 mm), or poor (≤4 mm). As a result, 30 of the 99 upper eyelids considered in this study were classified as fair and 69 as poor. In the 30 cases of bilateral blepharoptosis, only 18 upper eyelids had fair levator palpebrae muscle function, compared with 12 in the 39 unilateral cases. Numerous cases were classified as having poor levator palpebrae muscle function.
Operation Procedure
Double eyelid construction differs according to the blepharoptosis surgery method used. The method using frontalis muscle function was applied for poor levator function, and levator resection was used for fair levator function.
In cases of levator muscle resection or plication, double eyelids were formed by direct fixation of the dermis to the superior tarsal plate.
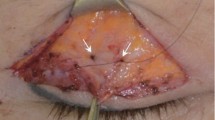
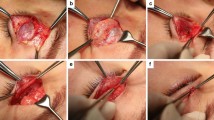
In cases of frontalis muscle flaps, orbicularis oculi muscle flaps, or frontalis myofacial flaps, double eyelids were reconstructed by fixing the palpebral dermis onto the frontalis flap, which was fixed to the superior portion of the tarsal plate (Fig. 1). In cases of unilateral blepharoptosis with fair levator function, the method involved levator resection or placation, with the height of the double eyelid created 1 to 3 mm lower than on the normal side.
Procedure for formation of a double eyelid on the muscle flap. Above left: The muscle flap is fixed to the tarsus by 5-0 nylon suture. Above right: The end portion of the muscle flap is sutured to the palpebral dermis of the lower skin flap with 7-0 nylon to construct the double eyelid. Below left: The lower skin flap is fixed to the muscle flap. Below right: Skin closure with 7-0 nylon
In cases of bilateral blepharoptosis that had identical levator function on both sides, the height of both double eyelids were designed identically, but 1 mm lower than in normal patients. When the frontalis muscle transfer method was used for cases of poor levator function, the height of the double eyelid was created 2 to 4 mm lower than on the normal side. If results were unpredictable, the two-stage operation was performed [3–5].
Blepharoptosis surgery was performed initially, with double eyelid construction performed on the opposite side after about 6 months. The postoperative care included removal of sutures on day 3 or 5 after surgery, followed by administration of ointment and artificial tears. Eye patches were worn during sleep to prevent exposure keratitis and infections for 3 to 6 months after the surgery.
Results
The postoperative follow-up period ranged from 3 to 49 months (average, 24 months). The result was classified according to the criteria of Souther [7] and Jordan and Anderson [8]. The evaluation criteria of Souther [7] and Jordan and Anderson [8] specified the height of the superior palpebral margin of both sides at primary gaze, the height of the double eyelids, symmetry of the eyes, and the satisfaction of both the patients and the doctors. If the height of both lid margins and the height of both double eyelids were symmetric, or if the difference between the heights of the upper lid margins was less than 1 mm, the results were classified as “good.” If the difference between the heights of the upper lid margins was 2 mm or more, the results were classified as “poor.” All other results were considered “satisfactory.” As a result of the surgery, 45 (65%) patients were classified as good, 18 (26%) patients as satisfactory, and 6 (9%) patients as poor.
The results were evaluated not only according to the degree of blepharoptosis, but also according to the degree of double eyelid asymmetry. The height of the double eyelids 6 months after the surgery was symmetric and averaged 5 mm in 27 patients (39%). However, in 42 patients (61%), a difference of 1 to 4 mm (average, 1.5 mm) was found. The height of the upper lid margin (the height of the palpebral fissure) was symmetric in only 21 patients (30%), and 48 patients (70%) showed a difference of 0.5 to 3 mm (average, 1.2 mm) (Table 1).
We analyzed by the opearative method. Among the levator resection cases, 50% were considered “good,” 40% “satisfactory,” and 10% “poor.” The method using frontalis muscle function resulted in 30 (83.3%) of 36 surgeries rated as “good,” 8.3% rated as “satisfactory,” and 8.3% rated as “poor.”
The complications included 6 cases of overcorrection, 12 cases of undercorrection, 2 cases of inclusion cyst, and 2 cases of exposure keratitis. Surgery was performed again for three cases of overcorrection and eight cases of undercorrection.
Figures 2 to 4 show both eyes before and after the double eyelid construction for a case of unilateral blepharoptosis. Figure 2 shows a patient with right blepharoptosis corrected using levator resection, with the double eyelid construction achieved at the same time. Figure 3 shows also a patient with right blepharoptosis who underwent levator resection. The two-stage operation was performed after ptosis correction on the right side, with the double eyelid construction performed on the left side 5 months later. Figure 4 shows a case of unilateral blepharoptosis. The blepharoptosis was corrected using the frontalis muscle transfer method on the left side. The double eyelid construction involved fixation of the palpebral dermis to four to five parts of the frontalis fascia flap [4] by nonabsorbable buried sutures, with supratarsal fixation used to construct the double eyelid on the right side.
A 6-year-old boy with unilateral moderate bleparoptosis on the right side. Levator function is 5 mm on the right side. Above: Preoperative view. Middle: Immediate postoperative view showing the levator resection with a double eyelid operation using the Fernandez technique [6]. Below: Postoperative view 1 year after double eyelid operation using the Sayoc [9] technique on the left side 5 months after ptosis correction on right side. The postoperative view shows a mild degree of ptosis on the right side due to relapse
A 48-year-old man with asymmetric unilateral severe bleparoptosis of the left side. Levator function is 2.5 mm on the left side. Left: Preoperative view. Right: Postoperative view 6 months after the frontalis myofascial flap on the left side and supratarsal fixation to construct the double eyelid on right side
Figure 5 shows a case of asymmetric bilateral blepharoptosis corrected using the levator resection method, in which the double eyelid construction was achieved. Figure 6 shows the result of revision for correction of undercorrection, and Fig. 7 shows the result of correction for overcorrection.
Discussion
When patients with blepharoptosis undergo double eyelid construction, the palpebral fissures become wider and can create a more pleasing eye shape. Especially for Asian patients, it is very important to perform double eyelid surgery simultaneously with blepharoptosis correction. However, in many cases, the double eyelid becomes shallow, asymmetric, and unsatisfactory postoperatively.
Several factors determine the size of the double eyelids when operations for blepharoptosis correction and double eyelid construction are performed simultaneously. First, at the fixation of the levator or frontalis muscle to the tarsal plate, the size of the double eyelids may differ according to whether they are fixed on the superior margin or on the middle portion of the tarsal plate. Second, the size also may be affected by the amount of skin excision.
Additionally, the location of the levator or frontalis muscle fixation may affect the size of the double eyelid. A final consideration is that the size may be affected by whether a portion of the tarsus is excised during surgery or not [10]. The higher the fixation level on the tarsus, the greater the amount of excised skin, the higher the level of the palpebral dermis fixed on the levator aponeurosis or the frontalis, and the higher the double eyelid can be made.
Regardless whether the case is unilateral or bilateral, when levator muscle function is not identical on both sides, the double eyelid on the ptotic side can be loose with a high fold. Therefore, the ptotic side must be made smaller and lower in position than the nonptotic side [11]. However, it is controversial how much smaller is ideal, and articles on this issue are rarely seen. We found that the double eyelid height increased with blepharoptosis in proportion to severity.
Generally, the standard double eyelid height for Asians is 6 to 8 mm and usually does not exceed 10 mm. In our experience, the height of the double eyelid has increased postoperatively according to the preoperative degree of ptosis. The postoperative height of the double eyelid in cases of severe ptosis has become higher than in mild ptosis cases. The cause may be more relapse or recurrence in severe ptosis. In mild ptosis, relapse or recurrence of ptosis has been uncommon, and drooping of the eyelid or widening of the double fold also has been uncommon.
In the current study, only 30% of the patients experienced perfect symmetry after the blepharoptosis operation, and 70% of the patients were asymmetric. The latter patients showed good symmetry immediately after the surgery, but as time passed, the functions of the frontalis and levator muscles weakened, causing asymmetry to occur. These cases thus require a slight overcorrection to avoid this postoperative result. On the other hand, the double eyelid construction performed during blepharoptosis surgery results in a loss of double eyelid height or the creation of asymmetric eyelids because the functions of the frontalis and levator muscles are weakened. In 60% of these cases, postoperative asymmetry occurred.
The study shows that good results were achieved for 50% of the patients by the levator resection method and 83.8% by the frontalis muscle transfer method. It is unusual that the frontalis muscle transfer for poor levator function had better results than the levator resection for fair levator function. The reason for the better results with the frontalis muscle transfer than with the levator resection in our series was that the authors had a better technique for the frontalis transfers than for the levator resections. The cases in which the levator palpebrae muscle or aponeurosis was surgically treated resulted in more natural looking double eyelids. The direction of the double eyelid creases were better physiologically compared with the frontalis muscle flap cases. Therefore, the levator resection method has traditionally been considered to achieve better double eyelid construction postoperative results than the method using frontalis muscle function.
However the results of this study show unusual findings. Thus, on a case-by-case basis, considering the diverse factors that determine the height and shape of double eyelids, the surgical method for creating double eyelids is more important than the type of blepharoptosis operation method chosen. The attached part of the levator palpebrae muscle, or frontalis muscle, the amount of skin excision, the location and method of adhesion, and the amount of tarsus excision must be controlled to create a symmetric fold. If this symmetry is too difficult to predict, a double eyelid should first be created on the blepharoptosis side. Then, after 6 months to 1 year, a double eyelid can be formed for the opposite side.
There are several methods for creating double eyelids. Different techniques for double eyelids must be applied according to the type of ptosis correction method chosen. There also are two options. The one is simultaneous correction. The other is delayed construction of the double eyelid on the nonptotic side.
Conclusion
We studied 69 blepharoptosis patients who underwent ptosis correction and double eyelid construction. In cases of severe unilateral blepharoptosis corrected using the frontalis muscle function, the double eyelid should be created lower on the side with blepharoptosis than on the normal side. This can be achieved by a different design and fixation of the new double fold on the ptotic side and trimming of the skin above the fold line on the ptotic side. In cases of bilateral blepharoptosis, the double eyelid on the side of the weaker levator palpebrae muscle function must be created lower. In cases of moderate blepharoptosis, it should be a little lower than the normal double eyelid height on the nonptotic side. If the results are unpredictable, a two-stage operation, in which blepharoptosis surgery is performed first and double eyelid construction on the nonptotic side is performed after a 6-month wait, may be an option to ensure postoperative symmetry.
References
Ben Simon GJ, Lee S, Schwarcz RM, McCann JD, Goldberg RA (2005) External levator advancement vs Muller’s muscle-conjunctival resection for correction of upper eyelid involutional ptosis. Am J Ophthalmol 140:426
Carraway JH (2003) Combining blepharoplasty with upper eyelid ptosis correction. Aesth Surg 23:59
Park DH, Lee SJ, Song CH (2005) Recurrence of blepharoptosis after a superiorly based muscle flap: Treatment by frontalis muscle advancement. Plast Reconstr Surg 116:1954
Park DH, Ahn KY, Han DG, Baik BS (1998) Blepharoptosis repair by selective use of superiorly based muscle flap. Plast Reconstr Surg 101:592
Park DH, Choi SS (2002) Correction of recurrent blepharoptosis using an orbicularis oculi muscle flap and a frontalis musculofascial flap. Ann Plast Surg 49:604
Fernandez LR (1960) Double eyelid operation in the Oriental in Hawaii. Plast Reconstr Surg 25:257
Souther SG (1974) The Fasanella-Servat operation for ptosis of the upper eyelid. Plast Reconstr Surg 53:123
Jordan DR, Anderson RL (1990) The aponeurotic approach to congenital ptosis. Opthalmic Surg 21:237
Sayoc BT (1974) Surgery of the Oriental eyelid. Clin Plast Surg 1:157
Mustardè JC (1982) A pragmatic approach to ptosis correction. Adv Ophthal Plast Reconstr Surg 1:69
Thornton WR (1994) Combined approach of ptosis and blepharoplasty surgery. Facial Plast Surg 10:177
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Park, D.H., Kim, C.W. & Shim, J.S. Strategies for Simultaneous Double Eyelid Blepharoplasty in Asian Patients With Congenital Blepharoptosis. Aesth Plast Surg 32, 66–71 (2008). https://doi.org/10.1007/s00266-007-9050-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-007-9050-5