Abstract
Background
The CTDR is a technique that treats cervical disc degenerative disease. Initial shorter-term studies showed good clinical and radiological results.
Purpose
To assess the clinical and radiological results of Bryan cervical disc replacement (Medtronic Sofamor Danek Inc., Memphis, TN) at 15-year follow-up.
Results
This prospective study included 20 patients who underwent 22 CTDR, comprising a single-level procedure in 14 patients and two-level procedures in six patients. The mean follow-up period was 15.5 years. The mean age at the intervention was 46.2 years (range: 26–65 years). Two patients needed re-operation for recurrence of symptoms. According to Odom’s criteria, 80.0% (16 of 20 patients) had excellent outcomes, VAS for neck pain was 2.6 (0–10), for shoulder/arm pain it was 1.8 (0–7), and NDI at the final follow up was 14.9. The SF-12 PCS was 46.1, and SF-12 MCS was 51.9. Mobility was maintained in 15 of the 22 (68.2%) operated segments, range of motion (ROM) of prostheses were 9° ± 3.9° (range 4–15°). The prostheses were positioned in kyphosis in 14 of 22 levels (63.6%). There was a positive correlation between the kyphosis of the prosthesis and the occurrence of heterotopic ossification (HO), and their grade (ρ = 0.36, CI 95%[−0.68; 0.07]). HO had developed at 12 of the 22 levels (54.5%) and upper adjacent segment degeneration in 11 of 18 of patients (64.7%). All these results were not significantly different to outcomes at 8 years follow-up.
Conclusion
In a cohort of 20 patients with 15-year clinical and radiological follow-up, the Bryan CTDR has demonstrated a sustained clinical improvement and implant mobility over time, despite a moderate progression of degenerative processes at the prosthetic and adjacent levels.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The first cervical total disc replacement (CTDR) occurred in 1962 (Fernstrom) [1]. The clinical expansion came with V. Bryan who developed a device bearing his name [2].
The European multicentric trial of the Bryan cervical disc prosthesis (Medtronic Sofamor Danek Inc., Memphis, TN) began in 2000. It proved similar improvement of neurological symptoms and signs with the anterior cervical discectomy and fusion (ACDF), but with preservation of cervical range of motion [3].
In previous studies of the Bryan prosthesis, follow up has shown that clinical outcomes are preserved over time, with preservation of mobility [4,5,6,7].
ACDF remains the gold standard for treating patients with cervical degenerative disease but invariably induces adjacent segment degeneration (until 92% at five years) [8] with potential adjacent segment disease [9, 10].
Adjacent segment degeneration has been demonstrated with CTDR on recent long term follow-up of up to ten years [11, 12]. Outcomes beyond that are unknown.
The aim of this study was to assess the clinical and radiological outcomes in a series of patients who underwent one or bi-level CTDR using a Bryan cervical disc prosthesis at 15 year follow-up.
Patients and methods
This single center prospective study included patients who underwent a CTDR with a Bryan disc prosthesis (Medtronic Sofamor Danek Inc., Memphis, TN) from July 2000 to July 2001 in the University Hospital of Bordeaux, by a single surgeon. This was a part of the European prospective multicentre study whose initial follow-up was previously published [3,4,5].
Patient inclusion criteria were cervical disc herniation or spondylosis with radiculopathy that had not responded to conservative treatment for at least six weeks. Exclusion criteria were previous cervical spine surgery, only axial neck pain without neuralgia, significant cervical deformity or spondylosis, ossification of the posterior longitudinal ligament, active infection, or second cervical surgery due to prosthesis device.
Clinical evaluation
Patients were reviewed routinely at regular intervals post-operatively, and data was obtained at 15 years after the surgical procedure, including function scores and physical (including neurological) examination.
The clinical evaluation includes the modified version of Odom’s criteria [13] which categorize outcomes as follows: (1) “excellent”, all pre-operative symptoms relieved, able to carry out daily occupations without impairment; (2) “good”, minimum persistence of pre-operative symptoms, ability to carry out daily occupations without significant interference; (3) “fair”, relief of some pre-operative symptoms, but physical activities significantly limited; and (4) “poor”, symptoms unchanged or worse.
The Visual Analogic Scale pain (VAS) was used to assess neck pain and shoulder/arm pain.
The Neck Disability Index (NDI) was used for the evaluation of neurological outcomes in patients with radiculopathy. Quality of life scores, which have been validated in spine pathologies included the SF-12, comprising physical (SF-12 PCS) and mental state (SF-12 MCS) [14].
The neurological evaluation included sensory and motor functions of upper and lower limbs.
Radiological evaluation
Radiological assessment consisted of static and dynamic flexion-extension lateral radiographs.
Range of motion (ROM) at eight year follow-up and 15 year follow-up was measured on dynamic images using the White’s method [15], measured by the angle between straight lines drawn along the inferior endplate of the upper vertebral body and superior endplate of the lower vertebra. A flexion-extension angle less than 2° defined fusion, as defined previously. Only one degree of motion was studied: the flexion-extension plane as previously established.
Device orientation was assessed on static radiographs. The neutral position was defined when the endplates were parallel, the kyphotic orientation when the angle between the two previous described lines were open on the posterior and report with a negative value, the lordotic orientation were described when the angle is open on anterior and report with a positive value.
Also, we evaluated the degenerative process at the adjacent and prosthetic levels. Concerning the prosthetic levels, the evaluation of heterotopic ossification (HO) was determined using the Mehren classification [16, 17] which categorizes as follows: grade 0: no HO; grade 1: anterior to the vertebral body not involving the disc space; grade 2: HO present within the disc space, with or without loss of ROM; grade 3: Bridging bone, but ROM >2°; grade 4: complete fusion and no mobility.
The adjacent segments (overlying and underlying) were analyzed on lateral radiographs, as follows: (1) new anterior or enlarging osteophyte formation; (2) narrowing of the disc space by >30%; (3) calcification of the anterior longitudinal ligament [12, 18, 19].
Statistical analysis
Descriptive statistics included mean values, standard deviation and range. Results were compared with those obtained at eight years follow up. Statistical analysis was conducting using Student’s paired t-test and Pearson correlation test (SPSS version 15.0 Software, SPSS Inc., USA). A p value of less than 0.05 was considered statistically significant.
Results
From the 21 patients at the eight year follow up, 18 patients had completed 15-year follow-up, and were included in this study. Unfortunately, one patient was excluded for lost to follow up. Two patients underwent re-operation for recurrence of neuralgia symptoms, and required removal of the prosthesis and instrumented cervical fusion (flow chart, Fig. 1). We included theses patients for the clinical analysis, but not for the radiological because they did not complete the 15-year follow-up.
From a total of 22 CTDR, a single-level procedure was performed in 14 patients, and two-levels procedures in four patients, ten men and eight women, mean age at intervention 46.2 years (range: 26–65 years). The mean follow-up period was 15.5 years. The cervical arthroplasty was implanted at the C4-C5 level in two cases, the C5-C6 level in 11 cases, the C6-C7 level in nine cases.
Clinical outcomes
Clinical evaluation
According to Odom’s criteria, 80.0% (16 of 20 patients) had an excellent outcome (all pre-operative symptoms relieved, able to carry out daily occupations without impairment). All patients with a single level arthroplasty had excellent outcomes. There is no statistically significant difference with the eight year follow-up (95.2%) (p > 0.05).
The VAS neck was: 5.5 (3–10) at baseline, 1.7 (0–8) at eight years, 2.6 (0–10) at 15 years. The VAS arm was: 5.8 (3–10) at baseline, 1.5 (0–8) at 8 years, 1.8 (0–7) at 15 years.
The NDI score was: 40.6 (22–68) at baseline, 12.9 (0–58) at eight years, 14.9 (0–44) at 15 years.
The SF-12 PCS was: 37.2 (23.9–53.8) at baseline, 47.3 at eight years (34.9–56.1), 46.1 (24.3–56.6) at 15 years. The SF-12 MCS was: 45.7 (33.3–62.1) at baseline, 52.6 (35.9–61.1) at eight years, and 51.9 (35.4–60.8) at 15 years.
The statistical analysis revealed no significant differences between the eight years and the 15 years follow up (p > 0.05) for all these results. The significant difference was maintained with the baseline follow up (p < 0.05) for all these parameters.
After clinical inspection, none of the patients had neurological symptoms associated with cervical pathologies.
Radiographic evaluation
Mobility was maintained in 15 of the 22 (68.2%) operated segments (Fig. 2). Functional prostheses (i.e., mobility >2° on lateral radiographic view) demonstrated ROM of 9° ± 3.9° (range 4–15°), versus 10.6° ± 4.5 (range 3.3–20.6), p > 0.05. Including the fused prostheses (ROM < 2°), ROM of all prostheses was 6.5° ± 4.1° (range 0–14°) versus 8.4° ± 5.8° (range 0–20.6°) at eight year follow up, p = 0.08. On differentiating between a HO group (15 levels) ROM was 2.9°, and a non-HO group (8 levels) ROM was 12.2°.
Sagittal plane analysis revealed that in neutral position, prostheses were positioned in kyphosis in 14 of 22 levels (63.6%), with a mean angle of −2.1°(−1° to −14°). There is a positive correlation between the position of the prosthesis in the sagittal plane (kyphosis) and the occurrence of HO and its grade (ρ = 0.36, CI 95%[−0.68; 0.07]). The kyphosis angulation was more important with grade 3 and 4.
At 15 years follow-up, 12 of the 22 levels (54.5%) had developed HO (grade 0–4) and 11 of the 22 levels (50%) were grade 3 or 4, which is statistically not significant (p > 0.05). We have presented a small series with a low statistical power, so our two groups (one and bi-level CTDR) could not be compared.However, it seemed that HO occurred more frequently in bi-level group (6/8 levels, i.e., 75%), than in one-level group (6/14 levels, i.e., 42.8%).
Upper adjacent segment degeneration was found in 64.7% of patients with new anterior or enlarging osteophyte formation (grade 1). At the inferior segment, 56.3% of patients did not develop any signs of disc degradation (Fig. 3). It was not possible to evaluate the underlying level (C7-T1) in one patient due to shoulder projection.
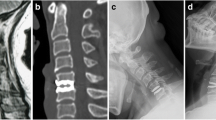
Bi-levels cervical total disc replacement (C4-C5, C5-C6), at one year (3a), at two years (3b), at height years (3c), at 15 years (3d). Adjacent level disease at lower level appeared and progressed (with no clinical symptoms), and heterotopic ossification. a No signs of HO or adjacent segment disease. b Adjacent segment disease at the lower intervertebral disc, and grade 4 HO at the C6-C7 level. c Adjacent segment disease with bone growth, osteophyte formation, and loss of intervertebral space (C6C7). d Bone bridging at the bi-levels with no mobility preserving
Adverse events and reoperation
No patient reported recurrent neurologic symptoms due to adjacent segment disease. Two of 20 (10%) patients required surgery for cervical foraminal stenosis due to HO at the prosthetic level. The two patients had two levels of prostheses C5-C6, C6-C7.
For one patient, neuralgia occurred at the both levels, for the other at the inferior level C6-C7. An anterior prosthetic removal was performed with insertion of a cervical cage to obtain fusion. The first patient had this procedure at two levels, the second at the C6-C7 level, while the C5-C6 prosthesis was left in place.
The second operation for the first patient occurred at 14 years from the initial operation, for the second at 12 years, with complete resolution of symptoms.
Discussion
Our results should be interpreted cautiously. The results of our study are not generalized to all patients because we reported results from a monocentric and a single surgeon. The small size of our cohort was the most important lack of our study, with a low statistical power. However,, this is the first prospective 15 years follow-up study of the Bryan prosthesis (Medtronic Sofamor Danek Inc., Memphis, TN), since the inception of this study as part of the European multicentre cohort initiated in 2000 [3,4,5]. Results were compared to those obtained at eight years follow-up [11]. After 15 years, the clinical results are excellent (80% excellent results). Odom’s criteria are not sensitive to change, however, as they are divided in four, which could explain the good clinical auto-evaluation by patient. They remain a valid clinical outcome tool [3,4,5, 11, 12]. The other functional scores confirmed this trend: VAS neck and arm/shoulder (2.6 and 1.8 respectively) and NDI (14.9). Although these results tended to decrease compared to eight year follow up, it was not statistically different to those obtained at eight year follow-up. Symptoms of an aging population (mean of 62.5 years old) may explain this. Mechanical age-related diseases had emerged during follow-up. Indeed, five patients had shoulder disorders including tendinopathy, which may have interfered with clinical scores results.
Two patients in the cohort (10%) needed re-operation for foraminal stenosis due to HO at a prosthetic level. Signs included recurrence of neuralgia and HO grades 2 and 4. Presumptively, the degenerative process continued until it caused nerve root symptoms. Symptoms resolved after a foraminal decompression and anterior cervical fusion. Other authors faced similar complications after CTDR and proposed a foraminal decompression by an anterior or posterior approach without removing the implant with good results [12, 20]. They were excluded from the 15 years results because they were not carrying a disc prosthesis at the 15 years follow up. Several authors had ever described other causes of implant removal for subsidence, migration of prosthesis, or soft disc herniation at operated level. However, with these two cases, we first reported recurrence of symptoms due to spondylosis process at the operated level. These have shown a failure of the device, but these events occurred after 12 and 14 years follow up, that is the most important recoil for these prostheses that we have found in the literature. So we have reported a large rate of re-intervention (10%), with our small cohort of 20 patients, but it occurred after a long period of implantation of the prostheses.
The radiological analysis showed that the device was still functional after 15 years. ROM in the lateral view were a mean of 9° ± 3.9° per level, much greater than the 2° guide to minimum functional mobility of a cervical prosthetic implant. There was a reduction in mean ROM compared to eight years follow up (8.4°), but not statistically significant. This ROM is substantially higher when compared to that of Zhao et al. at ten years (4.7°) [12]. The decrease in ROM could be related to the high rate of HO formation (54.5% in our series), where 50% of the prosthetic levels had grade 3 or 4 HO. It should to be noted that the initial cases were performed before the use of non-steroid anti-inflammatory drugs.
A trend seemed to show a higher rate of HO observed in multilevel (75%) versus in single level (42.8%) segments which is consistent with the others [17]. In the bi-level group, we could not determine whether HO dominated the lower or upper segment due to the small number of patients. In total, at 15 years follow-up, 54.5% of prosthetic levels developed HO, which is less than Zhao et al. [12], who found 69% of HO at ten years, while Walraevens et al. reported 39% HO at 8 years [21]. The occurrence of HO is not fully understood, and has been attributed in part to the bone milling process and to surgical-retractor-induced muscle damage to the longus coli [22], which may explain why in this series bi-level procedures had a higher incidence of HO. Preliminary studies have found as risk factors of HO, age, male gender, and even the type of device used [22, 23]. These different results of HO incidence depending on the authors, could be explained by a center effect, and raise the issue of generalization of this data.
Perhaps implant positioning in the sagittal plane could explain the HO in part, a point suggested in previous studies [17]. Indeed, there is a positive correlation between the kyphosis at the prosthesis level, and the apparition of HO and its grade. The previous series at eight years demonstrated that the six fused prostheses were positioned in a mean of 7.4° kyphosis [11].
The kyphosis of the disc operated after an arthroplasty by BRYAN has already been evoked in the literature many times [24, 25]. The laying technique (asymetric endplate milling, lack of anterior column support) [26] could explain this phenomenon. Xu et al. showed that by modifying it, the kyphosis of the implant favorably decreased [27]. The studies agree that the overall cervical lordosis is preserved, and that the functional results are maintained despite a prosthetic disc in kyphosis [24, 25].
The goal of CTDR compared to ACDF is to preserve adjacent disc levels from degradation and premature aging, preserving normal spinal motion following anterior discectomy. This series demonstrated significant amounts of adjacent segment degeneration, but there was no clinical consequence. Especially, the occurrence of ASD could be the natural evolution of spondylosis and not only due to the presence of a device [28, 29]. Recently, MRI demonstrated a better sensibility to evaluate the ASD than X-ray radiographies [30, 31]. A prospective study could be based on MRI to diagnose ASD before the CTDR surgery, and evaluate their occurrence or increase.
Sasso et al. found that at ten-years follow up, CTDR compares favorably with ACDF (9% v 32% reoperation) [32], according to Hilibrandt et al. [10] which estimated near 25% as the reoperation rate for ASD at ten years with ACDF. However, this series compares ACDF using anterior plates, knowing that if the distance between the edge of the plate and the disc is less than two millimeters, a rapid deterioration of the disc often occurs. To specifically compare the role of maintaining mobility to preserve the adjacent disc to fusion, this procedure should use a complete intradiscal device (fixed stand alone cage for example).
Conclusion
Although, we observed a moderate progression of degenerative process at prosthetic and adjacent levels, and a 10% rate of recurrence of the symptoms at the operated level requiring a re-intervention after a very long term follow-up we believe that these results are encouraging and confirm the ability of the Bryan cervical arthroplasty to maintain mobility and good clinical outcome over an extended follow up period.
References
Fernström U (1966) Arthroplasty with intercorporal endoprothesis in herniated disc and in painful disc. Acta Chir Scand Suppl 357:154–159
Bryan VE (2002) Cervical motion segment replacement. Eur Spine J 11(Suppl 2):S92–S97. https://doi.org/10.1007/s00586-002-0437-3
Goffin J, Casey A, Kehr P et al (2002) Preliminary clinical experience with the Bryan cervical disc prosthesis. Neurosurgery 51:840–845 discussion 845-847
Goffin J, Van Calenbergh F, van Loon J et al (2003) Intermediate follow-up after treatment of degenerative disc disease with the Bryan cervical disc prosthesis: single-level and bi-level. Spine 28:2673–2678. https://doi.org/10.1097/01.BRS.0000099392.90849.AA
Goffin J, van Loon J, Van Calenbergh F, Lipscomb B (2010) A clinical analysis of 4- and 6-year follow-up results after cervical disc replacement surgery using the Bryan cervical disc prosthesis. J Neurosurg Spine 12:261–269. https://doi.org/10.3171/2009.9.SPINE09129
Heidecke V, Burkert W, Brucke M, Rainov NG (2008) Intervertebral disc replacement for cervical degenerative disease--clinical results and functional outcome at two years in patients implanted with the Bryan cervical disc prosthesis. Acta Neurochir 150:453–459; discussion 459. https://doi.org/10.1007/s00701-008-1552-7
Yang S, Wu X, Hu Y et al (2008) Early and intermediate follow-up results after treatment of degenerative disc disease with the Bryan cervical disc prosthesis: single- and multiple-level. Spine 33:E371–E377. https://doi.org/10.1097/BRS.0b013e31817343a6
Goffin J, Geusens E, Vantomme N et al (2004) Long-term follow-up after interbody fusion of the cervical spine. J Spinal Disord Tech 17:79–85
Baba H, Furusawa N, Imura S et al (1993) Late radiographic findings after anterior cervical fusion for spondylotic myeloradiculopathy. Spine 18:2167–2173
Hilibrand AS, Carlson GD, Palumbo MA et al (1999) Radiculopathy and myelopathy at segments adjacent to the site of a previous anterior cervical arthrodesis. J Bone Joint Surg Am 81:519–528
Quan GMY, Vital J-M, Hansen S, Pointillart V (2011) Eight-year clinical and radiological follow-up of the Bryan cervical disc arthroplasty. Spine 36:639–646. https://doi.org/10.1097/BRS.0b013e3181dc9b51
Zhao Y, Zhang Y, Sun Y et al (2016) Application of cervical arthroplasty with Bryan cervical disc: 10-year follow-up results in China. Spine 41:111–115. https://doi.org/10.1097/BRS.0000000000001145
Odom GL, Finney W, Woodhall B (1958) Cervical disk lesions. J Am Med Assoc 166:23–28
Ware J, Kosinski M, Keller SD (1996) A 12-item short-form health survey: construction of scales and preliminary tests of reliability and validity. Med Care 34:220–233
White AA, Panjabi MM (1978) The basic kinematics of the human spine. A review of past and current knowledge. Spine 3:12–20
McAfee PC, Cunningham BW, Devine J et al (2003) Classification of heterotopic ossification (HO) in artificial disk replacement. J Spinal Disord Tech 16:384–389
Mehren C, Suchomel P, Grochulla F et al (2006) Heterotopic ossification in total cervical artificial disc replacement. Spine 31:2802–2806. https://doi.org/10.1097/01.brs.0000245852.70594.d5
Robertson JT, Papadopoulos SM, Traynelis VC (2005) Assessment of adjacent-segment disease in patients treated with cervical fusion or arthroplasty: a prospective 2-year study. J Neurosurg Spine 3:417–423. https://doi.org/10.3171/spi.2005.3.6.0417
Kim SW, Limson MA, Kim S-B et al (2009) Comparison of radiographic changes after ACDF versus Bryan disc arthroplasty in single and bi-level cases. Eur Spine J 18:218–231. https://doi.org/10.1007/s00586-008-0854-z
Wenger M, Markwalder T-M (2014) Posterior decompression salvages Bryan total disc arthroplasty in post-operatively recurrent uncoforaminal stenosis. J Clin Neurosci Off J Neurosurg Soc Australas 21:741–744. https://doi.org/10.1016/j.jocn.2013.07.016
Walraevens J, Demaerel P, Suetens P et al (2010) Longitudinal prospective long-term radiographic follow-up after treatment of single-level cervical disk disease with the Bryan cervical disc. Neurosurgery 67:679–687; discussion 687. https://doi.org/10.1227/01.NEU.0000377039.89725.F3
Leung C, Casey AT, Goffin J et al (2005) Clinical significance of heterotopic ossification in cervical disc replacement: a prospective multicenter clinical trial. Neurosurgery 57:759–763 discussion 759-763
Yi S, Shin DA, Kim KN et al (2013) The predisposing factors for the heterotopic ossification after cervical artificial disc replacement. Spine J Off J North Am Spine Soc 13:1048–1054. https://doi.org/10.1016/j.spinee.2013.02.036
Kim SW, Shin JH, Arbatin JJ et al (2008) Effects of a cervical disc prosthesis on maintaining sagittal alignment of the functional spinal unit and overall sagittal balance of the cervical spine. Eur Spine J 17:20–29. https://doi.org/10.1007/s00586-007-0459-y
Sasso RC, Metcalf NH, Hipp JA et al (2011) Sagittal alignment after Bryan cervical arthroplasty. Spine 36:991–996. https://doi.org/10.1097/BRS.0b013e3182076d70
Fong SY, DuPlessis SJ, Casha S, Hurlbert RJ (2006) Design limitations of Bryan disc arthroplasty. Spine J Off J North Am Spine Soc 6:233–241. https://doi.org/10.1016/j.spinee.2006.01.007
Xu J-X, Zhang Y-Z, Shen Y, Ding W-Y (2009) Effect of modified techniques in Bryan cervical disc arthroplasty. Spine 34:1012–1017. https://doi.org/10.1097/BRS.0b013e31819c4a5b
Song K-J, Choi B-W, Jeon T-S et al (2011) Adjacent segment degenerative disease: is it due to disease progression or a fusion-associated phenomenon? Comparison between segments adjacent to the fused and non-fused segments. Eur Spine J 20:1940–1945. https://doi.org/10.1007/s00586-011-1864-9
Park JY, Kim KH, Kuh SU et al (2013) What are the associative factors of adjacent segment degeneration after anterior cervical spine surgery? Comparative study between anterior cervical fusion and arthroplasty with 5-year follow-up MRI and CT. Eur Spine J 22:1078–1089. https://doi.org/10.1007/s00586-012-2613-4
Antosh IJ, DeVine JG, Carpenter CT et al (2010) Magnetic resonance imaging evaluation of adjacent segments after cervical disc arthroplasty: magnet strength and its effect on image quality. Clinical article. J Neurosurg Spine 13:722–726. https://doi.org/10.3171/2010.5.SPINE09721
Neal CJ, Rosner MK, Kuklo TR (2005) Magnetic resonance imaging evaluation of adjacent segments after disc arthroplasty. J Neurosurg Spine 3:342–347. https://doi.org/10.3171/spi.2005.3.5.0342
Sasso WR, Smucker JD, Sasso MP, Sasso RC (2016) Long-term clinical outcomes of cervical disc Arthroplasty: a prospective, randomized, controlled trial. Spine 42:209-216. https://doi.org/10.1097/BRS.0000000000001746
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Pointillart, V., Castelain, JE., Coudert, P. et al. Outcomes of the Bryan cervical disc replacement: fifteen year follow-up. International Orthopaedics (SICOT) 42, 851–857 (2018). https://doi.org/10.1007/s00264-017-3745-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-017-3745-2