Abstract
Purpose
To review available approaches and fixation methods for posterolateral fracture fragment (PLF) in tibial plateau fracture, and to propose an algorithm to treat various types of plateau fractures which all involve the PLF.
Methods
This article reviews multiple surgical approaches for PLF and suggests an algorithm for suitable approach and fixation method according to PLF with combined plateau fracture.
Results
The modified anterolateral approach is a suitable single approach for fractures with a PLF combined with an anterolateral plateau fracture and for isolated posterolateral fracture fragments. For a multicolumn tibia plateau fracture involving the lateral, medial and posterior columns, dual approaches (modified anterolateral and posteromedial approach) can be used to access the entire plateau area.
Conclusions
When considering approaches of this complex fracture pattern, one must consider local soft tissue condition, plateau fracture morphology, associated injuries, and fixation options. After review of multiple approaches described in the literature for PLF fixation, we can suggest an algorithm for the approach and fixation to treat tibial plateau fractures with posterolateral fracture fragments.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
A posterolateral fracture fragment (PLF) in tibial plateau fractures is defined as any separate posterolateral quadrant-based articular fracture fragment, with extension of the fracture line to the posterolateral cortex [1]. Posterolateral corner shearing tibial plateau fractures are less commonly seen, with incidence from 7 to 15%. A recent study has demonstrated a 44% incidence of the PLF, with 36% occurring in AO/OTA type B plateau fractures and 54% in AO/OTA type C [1,2,3].
Good long-term outcomes when treating tibia plateau fractures are associated with an anatomic articular reduction and stable fixation [4, 5]. Failure to stabilize these PLF fragments are associated with knee instability during flexion [6]. Anatomic reduction of the posterolateral fracture fragment can be achieved through either an indirect method using an anterolateral approach or a direct reduction using one of the various posterior approaches. Indirect reduction methods are more commonly associated with articular mal-reductions. Articular mal-reductions were present in up to 20% in cases when using a less invasive and unilateral fixed-angle stabilization system [2, 7, 8]. While the anterolateral approach is the most commonly used approach for lateral tibia plateau fractures, direct visualization of PLF is often inadequate [9]. With suboptimal visualization, an anatomical reduction and stable fixation of the PLF fragment is more challenging.
Various approaches for direct visualization and fixation of PLF are described in the literature. Posterior approaches include both direct posterior and posterolateral. Some authors have used a fibular osteotomy with a posterolateral approach for exposure, while others have described an approach without the fibular osteotomy [10,11,12,13,14,15]. While both approaches provide direct access for reduction and fixation of the PLF fragment, care must be taken with these approaches due to their proximity and required exposure of neurovascular structures. There is a higher risk of injury to the common peroneal nerve, popliteal vessels, and bifurcating vessels. Luo et al. [16] has described a posteromedial approach in treating medial column and posterior column fractures. They accessed the PLF using an inverted L-shaped incision over posterior medial aspect of the knee. The recently described modified anterolateral approach provides access through a single approach to reduce and stabilize the PLF while simultaneously treating the anterolateral plateau fracture [17].
Despite the availability of multiple approaches to the posterolateral plateau, a definitive treatment guideline and algorithm is currently lacking. When choosing an approach or combination of approaches, one must consider the condition of soft tissues, the entire plateau fracture morphology including the PLF fragment, and available fixation options. There is no consensus or standard guidelines when choosing an approach for this PLF fracture pattern. To help address this problem, we reviewed multiple approaches described in the literature for the fixation of the PLF. In this review, we propose an algorithm to treat these various types of plateau fractures which all involve the PLF fragment. We describe guidelines for approach selection and surgical techniques.
Morphological evaluation of the PLF
The morphological characteristics of posterolateral tibial plateau fractures has not been widely described in the literature. Recently, a few papers have helped to describe this fragment. Xiang et al. [1] determined the posterolateral articular fragment has a relatively small articular surface area, with the average size of the fragment relative to the surface area of the plateau being 14.3% ± 6.3% (range, 8-32%). The average major articular fracture angle of the posterolateral fracture fragment plane was 23° ± 24° (range, 62° to −43°), which implied a coronal fracture line. The average height of the fragment was 29 mm (range, 18-42 mm; 90th percentile = 38 mm). Average sagittal angle was 77° (range, 58-97°).
Sohn et al. [3] reported the average posterior cortical height was 31.12 mm (range, 10.84–63.93 mm), and the average sagittal fracture angle was 78.48 degrees (range, 41.69–105.12 degrees). The mean articular surface area was 522.18 mm2 (14.5%) of the total tibial articular surface. The mean posterior horizontal distance was 22.93 mm (range, 4.1-49.95 mm) and the lateral anteroposterior distance (LAPD) averaged 10.22 mm (range, −11.18 to 31.17 mm). The LAPD can be helpful when determining the best fixation strategy for the posterolateral fragment. In sum, the fracture patterns in the posterolateral quadrant are usually depression or split-depression type patterns. The fragments are usually conical in shape with a relatively small articular surface area.
Recent computed tomography (CT)-based morphological study also reported the combined quadrant of plateau with PLF according to the three column theory. They revealed that PLF can be presented as, isolated PLF in 7 cases, combined with anterolateral quadrant in 19 cases, posteromedial quadrant in two cases and bicolumnar involvement (AM, AM + AL, AM + PM) in eight cases among 36 PLF [1].
Biomechanical considerations in fixation of PLF
A recent literature review of loading mechanics concluded that biomechanically, the posterolateral buttress plate is the strongest fixation method for the posterolateral shearing tibial plateau fracture [18]. However, it remains controversial that a lateral locking plate can provide sufficient stability to the PLF. In this construct, the proximal locking screws are parallel to the coronal fracture line; therefore, single locking screws are less likely to gain adequate purchase into the PLF and the fixation may fail in this area [18]. Even with locking screws, front-to-back screws are at a mechanical disadvantage with cantilever loading.
Rafting screws, along with an appropriately placed buttress plate, can usually provide the stability needed to maintain the reduction. However, conventional anterolateral periarticular plates do not usually have screws that support a posterior articular fragment. Anterior plating is not strong enough to withstand the axial loading force and the traditional use of lag screws from anterior to posterior was at high risk of failure [19].
Sassoon et al. [20] examined the amount of the lateral tibial plateau which remains unsupported after insertion of the most common anterolateral periarticular plates. The average anterior to posterior depth of the lateral tibial plateau was 38 mm, but the average distance from the posterior-most rafting screw to the posterior tibial plateau border was 16 mm, resulting in approximately 42% of the lateral plateau unsupported by an anterolaterally based rafting screws. This study confirmed that even if posterior articular reduction can be obtained through a standard anterolateral approach, posteriorly placed implants are likely necessary to support the reduction. A variety of plating options have been described, including a one-third tubular plate, 2.7-mm variable-angled locking compression plate, T-plate, 3.5-mm recon plate, and posteromedial specific peri-articular plates [10, 13, 17, 21, 22].
Approaches for posterolateral fracture fragment
The best approach for treating PLF in tibial plateau fractures remains controversial. The optimal approach should provide maximum visualization with access for fracture reduction with rigid fixation, all while causing minimal insult to the surrounding structures. Current available approaches for PLF fragment fixation as described in the literature include: the posterior approach, the posterolateral approach with and without a fibular osteotomy, the posteromedial approach, and the modified anterolateral approach.
Posterior approach
Bhattacharyya et al. [13] described open reduction and internal fixation through a posterior approach to the knee. They used a mid-line S-shaped incision over the popliteal fossa. The medial head of the gastrocnemius was divided, leaving a stump for repair. The medial head was retracted laterally, protecting the neurovascular bundle, exposing back of the knee. The origins of the popliteus and soleus were then elevated from the posteromedial aspect of tibia from medial to lateral. The entire posterior aspect of the tibia was exposed without talking down the lateral head of the gastrocnemius. Using this approach, the posteromedial and posterolateral fragments can be exposed simultaneously.
Posterolateral approach with/without fibular osteotomy
The posterolateral approach, originally described by Lobenhoffer et al. [23], can be utilized with or without a fibular osteotomy. Lobenhoffer et al. developed an extensive lateral approach with fibular osteotomy for posterolateral fractures. This allows posterior retraction of the segment proximal to the osteotomy or even rotation of the fibular head upward, thus exposing the posterolateral plateau, and the lateral and posterior flare of the proximal tibia. Yu et al. [11] has described a new approach with osteotomy of fibular head to access posterolateral aspect of tibial plateau. Tscherne et al. [24] and Solomon et al. [25] demonstrated extensile approach for posterolateral plateau with osteotomy of the fibular neck. While providing nice exposure to the posterolateral plateau, these approaches with fibular osteotomy are always associated with increased risk of peroneal nerve palsy.
Tao et al. [15] introduced a modified posterolateral approach for posterolateral shearing tibial plateau fractures, in which an modified L-shaped incision was made to expose the posterior aspect of the lateral plateau through the intervals along the medial gastrocnemius, lateral gastrocnemius, popliteus and soleus without the need for an osteotomy, tenotomy, or division of muscles. However, with this approach, the common peroneal nerve has to be dissected out and carefully protected. The inferolateral genicular branch of popliteal artery was easily injured with this approach. Distal extension of this dissection should be restricted to no further than five centimeters from the joint line to avoid injury to the bifurcating vessels of the anterior tibial artery [26].
Carlson et al. [10] has described a case series of patients with posterior bicondylar tibial plateau fractures treated by direct fracture exposure and fixation through dual incisions: a posteromedial incision, followed by a posterolateral incision. He used a gentle S-shaped curvilinear incision in the posteromedial aspect of the knee and posterolaterally over the biceps femoris muscle. Using these approaches, both posteromedial and posterolateral fragments can be exposed separately, sequentially or simultaneously as the fracture morphology dictates.
Frosch et al. [12] presented a posterolateral approach with the patient positioned in a lateral position. In this approach, a lateral arthrotomy was used for visualizing the joint surface and a posterolateral approach was utilized for the fracture reduction and plate fixation. Both of these could be achieved through one posterolateral skin incision. This can be very helpful in more complex fracture patterns that involve the lateral or anterolateral parts of the tibia plateau.
The posterolateral approach offers the distinct advantages of being able to not only visualize and manipulate a posterolateral fracture fragment but also to apply posteriorly based implants for definitive fixation. However, a downside to this approach is for fractures that involve the anterior aspect of the lateral plateau. These fractures cannot be directly addressed through this approach. Moreover, assessment of reduction in the posterolateral corner can be technically demanding via a limited surgical field with a surgeon-unfriendly prone or lateral position. This limits the use of a posterolateral approach to the rare, isolated posterolateral coronal shear fracture. Further disadvantages of the posterolateral approach include the risk to the inferolateral geniculate artery, the anterior tibial artery, and the common peroneal nerve. Posterior plating can be difficult with distinctive inclination of the posterior surface of the proximal tibia and relatively deep surgical field.
Posteromedial approach addressing the posterolateral fracture fragment
Luo et al. [16] described a computed tomography based “three column fixation” concept and a “floating position” with an inverted L-shaped posterior approach and anterolateral approach. A posterior inverted L-shaped incision was used to address posterior and medial column fractures. The incision begins at the center of popliteal fossa parallel to Langer’s lines superiorly and medially, than turns distally from the medial corner of the popliteal fossa. Full thickness fascial flaps were elevated, avoiding injury to sural nerve and short saphenous vein. Medial head of gastrocnemius was retracted laterally. All the dissection was performed beneath popliteal muscle to protect the neurovascular bundle. The popliteal and soleus muscle origin were elevated laterally from the proximal medial aspect of tibia. The entire posterior aspect of tibia can be visualized. This is all performed without incising the medial head of the gastrocnemius. Both the posteromedial and posterolateral plateau can be addressed through this approach. However, any anterolateral tibial plateau fracture needs to be addressed through an additional anterolateral approach.
Modified anterolateral approach (or extended anterolateral approach)
The senior authors have also described a modified anterolateral approach to reduce and stabilize the PLF through the space between the fibular collateral ligament (FCL) and the posterolateral plateau rim [17]. We have aptly named this the ‘Para-FCL space’. We set up the patient in the supine position on an ordinary operation table. At first, we put the knee joint in modest flexion with a bump underneath the knee joint. A 10- to 15 cm-long curvilinear incision was made centered over the Gerdy’s tubercle. After the skin incision, subcutaneous dissection was made about 2 cm along the skin incision so that the ITB (iliotibial band) and crural fascia covering the anterior compartment muscles are exposed clearly. Then a fascial incision was made same as the skin incision. The ITB was split in the middle along the direction of the fibers and sharply elevated from Gerdy’s tubercle anteriorly and posteriorly. Then the fascial incision was extended down to the crural fascia leaving a 5-mm anterior fascial flap from the tibial crest for repair. This fascial dissection creates anterior and posterior flaps made of ITB and crural fascia in continuity respectively. The dissection was extended posteriorly by taking down the extensor muscles from the lateral surface of the lateral plateau to the point right in front of the FCL. By this point, we flexed the knee joint further up to 90 degrees to relax the FCL and also the common peroneal nerve. Then, a Sane retractor is placed to the inferior part of the FCL to retract the FCL posterolaterally. Then the interval between the FCL and the posterolateral surface of the lateral plateau (Para-FCL space) was developed by dissecting loose soft tissues from the posterolateral plateau (Fig. 1). Most of the time the popliteus tendon insertion onto the lateral epicondyle is not visible because the thick fascial covering is not incised and explored. It is critical to keep the dissection around the plateau below the joint line so as not to injure the popliteus tendon, which runs obliquely under the femoral origin of the FCL. Once the Para-FCL space is cleared up, the meniscotibial ligament is incised from the tibial attachment in order to gain access to the articular surface. By this point, we should be able to place a Hohmann retractor to the posterior surface of posterolateral corner of the lateral plateau (Fig. 2). We place a Schanz screw to the lateral epicondyle parallel to the joint line on the AP view. Another Schanz screw is placed to the lateral side of the tibial shaft to install a femoral distractor. The knee joint can be distracted with the knee in 90 degrees of flexion. For getting AP fluoroscopic images we pivot the knee joint around the femoral Schanz screw to extend the knee joint up to 30 degrees of flexion. This modification was the posterolateral extension to the classical anterolateral approach. We may call this an ‘extended anterolateral approach’.
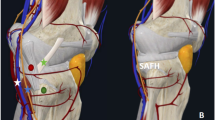
The para-fibular collateral ligament (Para-FCL) space in modified anterolateral approach. a The Para-FCL space (yellow-shaded space) is located between fibular collateral ligament (FCL) and lateral rim of the tibial plateau (AP view). b At the posterolateral corner, popliteal tendon (marked by asterisk) runs in an inferomedial to superolateral direction. The dissection should be performed anterior to popliteus (oblique lateral view)
Modified anterolateral approach in cadaveric dissection. a Dissection of the Para-FCL space (white arrowheads indicate the FCL). b After the coronary ligament was incised, the entire lateral plateau (which contains posterolateral corner) is exposed. c A Hohmann retractor can be placed anterior to FCL. A pointed reduction clamp can be placed to control the posterolateral fracture fragment
Authors’ preferred surgical approach and fixation technique for management of PLF
Standard AP, lateral, and oblique proximal tibia radiographs and CT scans with 3D reconstruction are obtained pre-operatively to assist in identifying fracture morphology and pre-operatively plan. Patients with compartment syndrome are treated with knee spanning external fixation and four-compartment fasciotomy using a single or dual incisions in an emergent nature if required. Patients with bicolumnar plateau fracture patterns, compromised skin, and vascular injuries are also temporized in a knee-spanning external fixator. CT scans are obtained after the application for the external fixator. Patients are taken for definitive fixation once skin conditions are optimized for a surgical incision.
The approach is ultimately chosen after consideration of the fracture morphology of the PLF fragment, the condition of the soft tissues, the possible involvement of other parts of the plateau, and the available fixation options. The PLF fragment is usually seen in combination with another area of the plateau fractured, as we have described. We can further divide the PLF fragment into four types based upon the associated tibial plateau fracture. The preferred surgical approach and fixation options are described according to each type. The types are as follows and classified by AO-OTA classification [27]:
-
1.
Isolated PLF [41-B 1.1 (4), B 2.2(4), B 3.1(2)]
-
2.
PLF with associated anterolateral plateau fracture (41-B 3.1)
-
3.
PLF with posterior shearing fracture (41-B1)
-
4.
PLF with a bicolumnar plateau fracture (41-C 3.1, 3.2, 3.3); posteromedial buttressing is mandatory due to the small posteromedial fragment
Isolated PLF
Isolated PLF can be treated with a single posterolateral approach or a modified anterolateral approach. The posterolateral approach offers the distinct advantage of being able to not only visualize and manipulate a posterolateral fracture fragment but also apply posteriorly based implants for definitive fixation. However, fractures that involve the anterior aspect of the plateau cannot be directly addressed through this approach. The peroneal nerve, inferolateral genicular artery and anterior tibial artery have to be protected as previously described. Through this approach, the PLF can be visualized and manipulated after an arthrotomy. The distal extent of exposure in this approach is restricted to no greater than 5 cm from the joint because the anterior tibial vascular bundle enters the anterior compartment at this point distal to joint line (46.3 ± 9.0 mm; range, 27–62). The lateral tibial metaphysis has a posterior inclination angle of about 45° and the posterolateral split fracture segment is usually less than 4 cm in cortical length. For fixation using this approach, we recommend using a short buttress plate while being cautious of the anterior tibial artery bifurcation [26, 28] (Fig. 3).
Isolated posterolateral tibial plateau depression fracture. A 35-year-old man was injured by a fall. a, b Three-dimensional reconstructions demonstrating an isolated right-knee posterolateral tibial plateau depression. c The patient was operated on using a direct posterolateral approach in the lateral position with direct visualization of the fracture fragment. The PLF was buttressed using a 3.5-mm locking T-plate (white arrowheads indicate the common peroneal nerve). d Post-operative radiograph demonstrating an anatomic reduction
The direct posterolateral approach requires a deep dissection to gain access to the PLF. In this approach, caution is taken around the inferolateral genicular artery and common peroneal nerve as previously described. Some surgeons may feel uncomfortable when accessing and manipulating the PLF fragment through this deep and limited surgical field. In contrast to the direct posterolateral approach, the modified anterolateral approach provides a safer corridor around the rim of the lateral tibial plateau medial to the fibular collateral ligament. Direct access to a posterolateral fragment is possible, and fracture reduction can be done under direct visualization. The relative simplicity of this approach, ease of positioning, and decreased likelihood of iatrogenic injury to neurovascular structures are other potential advantages.
Through this approach, the displaced PLF could be reduced by collinear clamp or pointed reduction clamp through the Para-FCL space. Although it is difficult to place a buttress plate directly with the modified anterolateral approach, the recently described rim plating technique provides adequate support to PLFs with wrapping up of the fragment and multiple rafting screws through the variable angled screw holes [17] (Fig. 4). Detailed rim-plating fixation techniques using a 2.7-mm variable angle (VA) plate will be described in the next section.
A 55-year-old woman had sustained an injury due to a fall. a Three-dimensional CT reconstructions (articular view and posterior view) shows a depressed PLF with inferomedial displacement and an incomplete split with anterolateal depression. Although there was an incomplete split of anterolateral plateau, the main component that needs to be buttressed was located predominantly at the posterolateral corner, we categorized this fracture as an isolated PLF treated with rim plating through the modified anterolateral approach. A modified anterolateral approach was utilized and rim plating was performed. b Postoperative 3D CT reconstuctions (articular view and posterior view) demonstrates reduction of the displaced PLF with rim plate fixation. The small depressed articular surface could be elevated easily by anterolateral cortical window with impacted bone graft and other substitute. The incomplete split of anterolateral plateau with cortical window can also be protected with a simple anterolateral buttress plate using a three-hole 3.5-mm T-plate
PLF with associated anterolateral plateau fracture
A combined dual posterolateral and anterolateral approach can be utilized for PLF with associated anterolateral plateau fractures. The advantage of these combined approaches is their utility in directly accessing entire lateral tibial plateau simultaneously addressing both anterolateral and posterolateral fragments. This combined approach method also has all of the disadvantages of the direct posterolateral approach (Fig. 5).
Our preferred approach for PLF with associated anterolateral fracture is a modified anterolateral approach. The advantages of this modified anterolateral approach include: (1) exposure of the entire articular surface of the lateral plateau, (2) reduction of articular surface under direct vision, (3) no need for peroneal nerve dissection and exposure, (4) the surgery can be performed in the familiar supine position, and (5) if needed, removal of hardware can be performed with standard approaches with little risk to vital structures.
Surgical technique of the rim-plating fixation technique
After completing the approach to the PLF using modified anterolateral approach (as previously described), the entire lateral plateau articular surface can be exposed. The depressed articular surface is then elevated through either a small rectangular cortical window that is made at the metaphyseal area of anterolateral surface of proximal tibia or through the fracture window between lateral plateau and anterior rim. It is elevated with a small impactor or tamp with bone graft or bone graft substitute.
The elevated anterolateral articular surface is then stabilized temporarily with K-wires. The lateral plateau fracture gap is then reduced with a pointed reduction clamp. The displaced PLF is then reduced with a pointed reduction clamp or collinear clamp and then temporarily stabilized with K-wires in an anterior to posterior direction to prevent blocking the positioning of rim plate (Fig. 6).
A 59-year-old man sustained a lateral tibial plateau fracture after a fall from 3 metres height. a Three-dimensional CT reconstructions (AP, posterior, and articular views) show an anterolateral split depression fracture with a posterolateral fracture fragment. b The depressed anterolateral articular fragment was elevated with graft material through the fracture window of the anterolateral split fracture fragment. c The fracture window was closed and reduced with a small pointed reduction clamp. The PLF was reduced with large pointed reduction clamp through the Para-FCL space. d The PLF was fixed with provisional K-wires
For the choice of rim plate, we usually use a 2.7-mm variable-angle locking compression plate (VA LCP) plate from the VA foot set (DePuy Synthes, West Chester, PA, USA). This is then contoured appropriately with VA LCP bending pliers, while avoiding VA hole deformation. The plate is contoured according to the shape of the rim of the lateral plateau. A 2.7-mm cloverleaf-head plate was usually used to support the PLF. The wider portion of plate was positioned posterior to PLF to wrap up the fragment. Then the head of the rim plate was compressed against the PLF using a collinear clamp. Then the anterior most screw hole is filled with a cortical screw to bring the plate down to bone over the lateral surface of the plateau. One or two additional screws are placed through the rim plate while the collinear clamp was maintained. Then the collinear clamp was released. Screws are placed as far posteriorly as possible through the plate usually just anterior to the fibular collateral ligament. Trajectories of the screws are aimed to ensure rafting under the main area of depression.
Sometimes we will place two screws through one combination hole to maximize the fixation because the longest 2.7-mm screw is 60 mm. A locking screw is placed first, followed by the cortical screw. Due to the contour of rim plate, there is a high amount of screw traffic and drill bits can be easily broken. To avoid broken drill bits, we use 2.0-mm K-wires to drill and slightly tilt the trajectories, alternating between slightly cranial and caudal inclinations.
After completing the rim plating, a 3.5-mm anatomically precontoured locking plate is placed at anterolateral surface of tibial plateau to buttress the anterolateral fragment (Fig. 7).
a, b The rim plate was contoured and advanced along the rim of posterolateral plateau. Using the collinear clamp, the head of the plate and the PLF were compressed to the anterior rim of the plateau. Using a 2.0 K-wire as a drill bit, a conventional 2.7-mm screw was inserted to make the plate contoured with the lateral rim while holding the collinear clamp. c Postoperative 3D CT scans demonstrate the anterolateral plateau fracture buttressed with a 3.5-mm precontoured plate and PLF stabilized with a rim plate. d Axial CT scan demonstrates the trajectory of the screws which purchasing the PLF from the rim plate
PLF with posterior shearing fracture
Carlson et al. [10] originally reported a posterior dual approach for a posterior shearing plateau fracture. But most surgeons tend to use a posteromedial approach only because posterolateral corner can be easily accessible and buttressed with this approach. We recommend the posteromedial approach for PLF with a posteromedial plateau fracture as described by Luo et al. [16]. This approach provides better exposure for more substantial posteromedial tibial plateau fractures and can be used to gain access to the posterolateral tibial plateau with retraction of the medial gastrocnemius laterally and elevation of popliteus and soleus off the posterior tibia. Special caution must be given when placing the Hohmann retractor at the lateral border of tibia due to the arterial bifurcation. Through this approach, placement of buttress plating is possible to each posterior column separately. For a posteromedial fragment, the buttress plate is usually placed in a longitudinal direction, while for the posterolateral fragment the plate is usually orientated obliquely.
PLF with a bicolumnar plateau fracture; posteromedial buttressing is mandatory due to small posteromedial fragment
Most multicolumn plateau injuries need separate incisions for gaining access to each column. Several factors must be considered when selecting an approach. Fracture morphology, surgical skill set, patient positioning requirements, and the condition of the soft tissues are all factors to consider when choosing an approach. For these fracture patterns, we prefer to use a dual modified anterolateral approach and a posteromedial approach with the contralateral limb in the lithothomy position. The classic posteromedial approach with prone positioning has limitations requiring the changing patient position to perform an anterolateral approach. To overcome this obstacle, we position the patient supine with contralateral limb in lithotomy position. Both the posteromedial and anterolateral approaches can be performed simultaneously using this position without changing the position of the patient in between two approaches. For the posteromedial approach, the surgeon occupies a position between two legs, while anterolateral approach can be performed sitting at a lateral aspect of the patient’s leg. This positioning reduces intraoperative time and prevents complications associated with prone positioning.
Through the modified anterolateral approach, we can access the anterolateral and posterolateral aspect of the plateau. The posteromedial aspect of the plateau can be accessed from the posteromedial approach. As described by Luo et al. [16], the anteromedial aspect of the tibial plateau can also be accessed by utilizing the interval between the pes anserinus and medial collateral ligament (MCL). Fixation for the PLF can be buttress plating through the posteromedial approach or rim plating through modified anterolateral approach, depending on the fracture morphology of PLF and the comminution at the metaphysis of the posterolateral corner. When the medial extent of the PLF is located far enough medially to reach from posteromedially and the metaphyseal beak is enough for a posterior buttress plate, we use a 3.5-mm T-plate (Fig. 8). In cases where the medial fracture margin ends at the posterolateral corner or metaphyseal beak is small, we preferred fixation with a rim plate (Fig. 9).
PLF with a bicolumnar tibial plateau fracture. This can be a multicolumn injury involving the medial, posterolateral and anterolateral plateau. A 69-year-old woman injured by a fall. a The patient had an anterolateral split and depression fracture, a medial plateau fracture, and a posterolateral fracture fragment which demonstrated enough metaphyseal beak for posterior buttress. b Both posteromedial and anterolateral approach can be simultaneously utilized without changing the position of patient. Posteromedial and posterolateral buttressing was done using posteromedial approach using two 3.5-mm T-plates (white arrowhead indicates buttress plate for PLF). The anterolateral fragment was reduced and fixed using anterolateral approach using 5.0-mm precontoured locking plate. c Complete radiological union was observed at 12 weeks following surgery
A 53-year-old man sustained a left-knee injury in a fall down some stairs. a Three-dimensional CT reconstructions (AP, posterior, and articular views) after knee spanning external fixation shows a complex plateau fracture with an anterior fragment, a lateral split fragment, central depression, a medial fragment, and a displaced PLF. The PLF has a small metaphyseal beak with comminution of the posterior cortex (red arrowhead). b The medial plateau was buttressed through the posteromedial approach. The depressed central articular was elevated with impacted bone graft. The displaced PLF was fixed with a rim plate and the anterolateral split fragment was fixed with an anterolateral plate. PLF was wrapped with rim plate and fixed with two screws (one screw through the plate and one screw from outside the plate)
Discussion
A PLF can be addressed through any of the direct posterior or posterolateral approaches previously mentioned. The modified anterolateral approach also provides good access to this fragment. We prefer a modified anterolateral approach over the direct posterior and posterolateral approaches for several reasons. The posterior and posterolateral approaches allow reduction and fixation of a posterolateral fragment under direct visualization with posterior buttress plating. This buttress plating provides stable fixation and allows early knee motion [12, 29]. However, there are many limitations associated with the direct posterior and posterolateral approaches. A direct midline posterior incision has a deep field and visualization can be difficult. This situation is further complicated by presence of a complex fracture pattern involving the lateral and anterolateral tibial plateau. Another potential downfall from the direct posterior and posterolateral approaches is the proximity of the required exposure of the common peroneal nerve and the close proximity of the popliteal vessels.
Chang et al. [30] also reported the anterolateral supra-fibular head approach for posterolateral tibial plateau fractures. They also developed space between the FCL and the lateral condyle of tibia. The posterolateral fracture fragment was fixed successfully at least two screws from a laterally based implant. In contrast to this technique, the above described rim plating technique not only provides screw purchase into the PLF but also contributes a posterior buttress effect on the fragment, which only strengthens fragment fixation.
We designed the rim plate to hold the PLF, which tends to be displaced posteriorly. It is not real buttressing plating but it could be wrap the fragment along the posterior rim of plateau (named a “hugging plate”). With a collinear clamp used for rigid maneuver reduction throughout the fixation procedure, the rim plate functions to maintain the PLF reduction. Most recent biomechanical analysis compared different type of fixation to PLF. They compared anterolateral lag screws (anterior to posterior direction), screw fixation through an anteromedial plate, screw fixation through a lateral locking plate and a posterolateral buttress plate which were available for PLF fixation. But there was no direct comparison with rim plating [18]. A biomechanical study about rim plating is needed in the near future.
Though there were not many reports, clinical evidence of rim plating was reported. Horizontal belt plate as a rim plating could be applied to complex tibial plateau fracture and showed relevant clinical outcome [30, 31]. We have also reported the good clinical outcomes of rim plating. A total of seven cases were enrolled in that study. There was no loss of reduction and no complications which were related with this procedure. All cases healed in 3 months after operation. Functional outcomes were excellent in four cases, good in one case and fair in one case [17].
In deciding the approach in the treatment of tibial plateau fractures, consideration must be given to the fracture fragment morphology, the available implants, the condition of the soft tissues around the proximal tibia, and the experience of the surgeon. Many alternative approaches for PLF management have been described in the literature. The PLF is usually combined with other additional fractures in the tibial plateau.
In this review, we divide the PLF into four types based upon the presence of injury to other parts of the plateau. We provide guidelines to help determine approach and fixation options. In our experience, the modified anterolateral approach is the most suitable single approach for fractures with a combined posterolateral fracture fragment with an anterolateral plateau fracture and for isolated or predominantly posterolateral fracture fragments. For a multicolumn tibia plateau fracture involving the lateral, medial and posterior columns, dual approaches are needed. In this instance, we prefer a posteromedial and modified anterolateral approach using the lithotomy position for the contralateral lower extremity. This is a versatile position, where both the posteromedial and modified anterolateral approaches can be performed simultaneously without the need for changing patient positioning. The posterolateral fragment can be simultaneously managed through both incisions. In addition, an anteromedial fragment can also be addressed utilizing the interval between pes anserinus and MCL (Fig. 10).
References
Xiang G, Zhi-Jun P, Qiang Z, Hang L (2013) Morphological characteristics of posterolateral articular fragments in tibial plateau fractures. Orthopedics 36(10):e1256–e1261. doi:10.3928/01477447-20130920-16
Partenheimer A, Gosling T, Muller M, Schirmer C, Kaab M, Matschke S, Ryf C, Renner N, Wiebking U, Krettek C (2007) Management of bicondylar fractures of the tibial plateau with unilateral fixed-angle plate fixation. Unfallchirurg 110(8):675–683. doi:10.1007/s00113-007-1271-1
Sohn HS, Yoon YC, Cho JW, Cho WT, Oh CW, Oh JK (2015) Incidence and fracture morphology of posterolateral fragments in lateral and bicondylar tibial plateau fractures. J Orthop Trauma 29(2):91–97
Houben PF, van der Linden ES, van den Wildenberg FA, Stapert JW (1997) Functional and radiological outcome after intra-articular tibial plateau fractures. Injury 28(7):459–462
Singleton N, Sahakian V, Muir D (2017) Outcome after tibial plateau fracture: how important is restoration of articular congruity? J Orthop Trauma 31(3):158–163
Waldrop JI, Macey TI, Trettin JC, Bourgeois WR, Hughston JC (1988) Fractures of the posterolateral tibial plateau. Am J Sports Med 16(5):492–498
Cole PA, Zlowodzki M, Kregor PJ (2004) Treatment of proximal tibia fractures using the less invasive stabilization system—surgical experience and early clinical results in 77 fractures. J Orthop Trauma 18(8):528–535. doi:10.1097/00005131-200409000-00008
Manidakis N, Dosani A, Dimitriou R, Stengel D, Matthews S, Giannoudis P (2010) Tibial plateau fractures: functional outcome and incidence of osteoarthritis in 125 cases. Int Orthop 34(4):565–570. doi:10.1007/s00264-009-0790-5
Solomon LB, Stevenson AW, Lee YC, Baird RP, Howie DW (2013) Posterolateral and anterolateral approaches to unicondylar posterolateral tibial plateau fractures: a comparative study. Injury 44(11):1561–1568. doi:10.1016/j.injury.2013.04.024
Carlson DA (2005) Posterior bicondylar tibial plateau fractures. J Orthop Trauma 19(2):73–78
Yu BQ, Han KW, Zhan C, Zhang CC, Ma H, Su JC (2010) Fibular head osteotomy: a new approach for the treatment of lateral or posterolateral tibial plateau fractures. Knee 17(5):313–318. doi:10.1016/j.knee.2010.01.002
Frosch KH, Balcarek P, Walde T, Sturmer KM (2010) A new posterolateral approach without fibula osteotomy for the treatment of tibial plateau fractures. J Orthop Trauma 24(8):515–520. doi:10.1097/BOT.0b013e3181e5e17d
Bhattacharyya T, McCarty LP 3rd, Harris MB, Morrison SM, Wixted JJ, Vrahas MS, Smith RM (2005) The posterior shearing tibial plateau fracture: treatment and results via a posterior approach. J Orthop Trauma 19(5):305–310
Trickey EL (1968) Rupture of the posterior cruciate ligament of the knee. J Bone Joint Surg (Br) 50(2):334–341
Tao J, Hang DH, Wang QG, Gao W, Zhu LB, Wu XF, Gao KD (2008) The posterolateral shearing tibial plateau fracture: treatment and results via a modified posterolateral approach. Knee 15(6):473–479. doi:10.1016/j.knee.2008.07.004
Luo CF, Sun H, Zhang B, Zeng BF (2010) Three-column fixation for complex tibial plateau fractures. J Orthop Trauma 24(11):683–692. doi:10.1097/BOT.0b013e3181d436f3
Cho JW, Samal P, Jeon YS, Oh CW, Oh JK (2016) Rim plating of Posterolateral fracture fragments (PLFs) through a modified anterolateral approach in tibial plateau fractures. J Orthop Trauma 30(11):e362–e368. doi:10.1097/BOT.0000000000000638
Zhang W, Luo CF, Putnis S, Sun H, Zeng ZM, Zeng BF (2012) Biomechanical analysis of four different fixations for the posterolateral shearing tibial plateau fracture. Knee 19(2):94–98. doi:10.1016/j.knee.2011.02.004
Papagelopoulos PJ, Partsinevelos AA, Themistocleous GS, Mavrogenis AF, Korres DS, Soucacos PN (2006) Complications after tibia plateau fracture surgery. Injury 37(6):475–484. doi:10.1016/j.injury.2005.06.035
Sassoon AA, Torchia ME, Cross WW, Cass JR, Sems SA (2014) Fibular shaft allograft support of posterior joint depression in tibial plateau fractures. J Orthop Trauma 28(7):e169–e175. doi:10.1097/bot.0000000000000020
Chen HW, Zhou SH, Liu GD, Zhao X, Pan J, Ou S, Fei J (2015) An extended anterolateral approach for posterolateral tibial plateau fractures. Knee Surg Sports Traumatol Arthrosc 23(12):3750–3755. doi:10.1007/s00167-014-3304-y
Bermudez CA, Ziran BH, Barrette-Grischow MK (2008) Use of horizontal rafting plates for posterior elements of complex tibial plateau fractures: description and case reports. J Trauma 65(5):1162–1167. doi:10.1097/01.ta.0000222943.45563.b5
Lobenhoffer P, Gerich T, Bertram T, Lattermann C, Pohlemann T, Tscheme H (1997) Particular posteromedial and posterolateral approaches for the treatment of tibial head fractures. Unfallchirurg 100(12):957–967
Tscherne H, Lobenhoffer P (1993) Tibial plateau fractures. Management and expected results. Clin Orthop Relat Res (292):87–100
Solomon LB, Stevenson AW, Baird RP, Pohl AP (2010) Posterolateral transfibular approach to tibial plateau fractures: technique, results, and rationale. J Orthop Trauma 24(8):505–514. doi:10.1097/BOT.0b013e3181ccba4b
Sun H, Luo C-F, Yang G, Shi H-P, Zeng B-F (2013) Anatomical evaluation of the modified posterolateral approach for posterolateral tibial plateau fracture. Eur J Orthop Surg Traumatol 23(7):809–818
Marsh J, Slongo TF, Agel J, Broderick JS, Creevey W, DeCoster TA, Prokuski L, Sirkin MS, Ziran B, Henley B (2007) Fracture and dislocation classification compendium-2007: Orthopaedic trauma association classification, database and outcomes committee. J Orthop Trauma 21(10):S1–S6
Heidari N, Lidder S, Grechenig W, Tesch NP, Weinberg AM (2013) The risk of injury to the anterior tibial artery in the posterolateral approach to the tibia plateau: a cadaver study. J Orthop Trauma 27(4):221–225
Chang S-M, Zheng H-P, Li H-F, Jia Y-W, Huang Y-G, Wang X, Yu G-R (2009) Treatment of isolated posterior coronal fracture of the lateral tibial plateau through posterolateral approach for direct exposure and buttress plate fixation. Arch Orthop Trauma Surg 129(7):955–962
Hu S-J, Chang S-M, Zhang Y-Q, Ma Z, Du S-C, Zhang K (2016) The anterolateral supra-fibular-head approach for plating posterolateral tibial plateau fractures: a novel surgical technique. Injury 47(2):502–507
Pires RES, Giordano V, dos Santos JK, Labronici PJ, de Andrade MAP, de Toledo Lourenço PRB (2015) Expanding indications of the horizontal belt plate: a technical note. Injury 46(10):2059–2063
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Funding
There is no funding source.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Cho, JW., Kim, J., Cho, WT. et al. Approaches and fixation of the posterolateral fracture fragment in tibial plateau fractures: a review with an emphasis on rim plating via modified anterolateral approach. International Orthopaedics (SICOT) 41, 1887–1897 (2017). https://doi.org/10.1007/s00264-017-3563-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-017-3563-6