Abstract
Introduction
Variations in glenoid morphology among patients of different gender, body habitus, and ethnicity have been of interest for surgeons. Understanding these anatomical variations is a critical step in restoring normal glenohumeral structure during shoulder reconstruction surgery.
Methods
Retrospective review of 108 patient shoulder CT scans was performed and glenoid version, AP diameter and height were measured. Statistical multiple regression models were used to investigate the ability of gender and ethnicity to predict glenoid AP diameter, height, and version independently of patient weight and height.
Results
The mean glenoid AP diameter was 24.7 ± 3.5, the mean glenoid height was 31.7 ± 3.7, and the mean glenoid version was 0.05 ± 9.05. According to our regression models, males would be expected to exhibit 8.4° more glenoid retroversion than females (p = 0.003) and have 2.9 mm larger glenoid height compared to females (p = 0.002). The predicted male glenoid AP diameter was 3.4 mm higher than that in females (p < 0.001). Hispanics demonstrated 6.4° more glenoid anteversion compared to African-Americans (p = 0.04). Asians exhibited 4.1 mm smaller glenoid AP diameters than African-Americans (p = 0.002). An increase of 25 kg in patient weight resulted in 1 mm increase in AP diameter (p = 0.01).
Conclusions
Gender is the strongest independent predictor of glenoid size and version. Males exhibited a larger size and more retroverted glenoid. Patient height was found to be predictive of glenoid size only in patients of the same gender. Although variations in glenoid size and version are observed among ethnicities, larger sample size ethnic groups will be necessary to explore the precise relations. Surgeons should consider gender and ethnic variations in the pre-operative planning and surgical restoration of the native glenohumeral relationship.
Level of Evidence: Anatomic Study
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Numerous studies have evaluated glenoid morphology using CT scans and found variations amongst men and women, shoulder dominance, and activity level. For instance, it is known that males typically have a more retroverted glenoid compared to females [1–4]. Although most patients have a neutral to slightly retroverted glenoid, large variations are seen and should be accounted for accordingly [5]. Some studies found a positive correlation between glenoid surface area and patient height and gender, but it is unclear which patient parameters (gender and height) were most predictive of the variance in glenoid diameters and how the variance was affected [6].
Churchill et al. examined the glenoid version and size in more than 170 human cadavers of different ethnicity and gender [7]. Although, they found no significant difference in glenoid size between patients of African-American ethnicity and white patients, a significant difference in glenoid height and width was observed between genders [7]. Glenoid version was found to be significantly different in specimens of various ethnicity, but the authors failed to find a difference between genders of the same ethnicity [7]. Furthermore, they did not investigate the impact of body habitus, specifically body height and weight, in the variation of glenoid version and size.
The purpose of this study is to evaluate how glenoid version, anteroposterior (AP) diameter, and height vary based on patient demographics, specifically gender, ethnicity, weight, height, and laterality. Furthermore, gender and ethnicity characteristics were examined independently of height and weight to limit confounding effects. A secondary aim of the study was to identify the strongest predictors of glenoid AP diameter, height, and version within this patient cohort.
Understanding glenoid anatomical variations between genders and patients of different ethnicity will help surgeons set individual goals for every patient in restoring the native glenohumeral anatomy. These variations could also be taken into account in designing patient specific implants.
Materials and methods
Basic science study; anatomic study
The study was approved by the University of Illinois at Chicago Institutional Review Board, protocol #2012–0195.
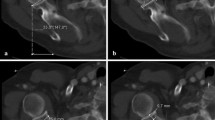
An IRB approved retrospective collection and review of shoulder computerized tomographic (CT) studies was performed. One hundred and eight consecutive CT scans were reviewed and analyzed. Scans were excluded if the patient was skeletally immature, had a congenital limb abnormality, had a history of previous orthopaedic surgery on the shoulder studied, or if they had a history of trauma or fracture on the studied shoulder. The glenoid version, AP diameter and glenoid height were examined with the conventional measuring method, described by Friedman [2]. The AP diameter was measured on the axial cut with the greatest glenoid diameter (Fig. 1). The glenoid height was measured on the coronal cut with the greatest superoinferior diameter (Fig. 2). To find the glenoid version, the middle portion of the glenoid cavity was approximated using the first axial cut inferior to the coracoid and was verified using a coronal cut. In non arthritic glenoids, the midglenoid version has been found to be a good estimate of the version found using a sphere model [8]. A line (X) was drawn from midpoint of glenoid fossa to the medial end of the scapula (Fig. 3). A second perpendicular line (Y) to line (X) was defined as neutral glenoid version. Line (Z) was drawn from anterior and posterior margins of the glenoid face. The angle between (Y) and (Z) was determined to be the glenoid version measurement. If the posterior margin of line (Z) was medial to line (Y) then this was determined to be retroversion and recorded as negative. If vice-versa, then this was determined to be anteversion of the glenoid cavity and was recorded as positive.
Patient data including age, height, weight, BMI, and ethnicity were recorded and used for comparative analysis. Hierarchical multiple regression models were created to assess the ability of gender, ethnicity, patient height, and weight to predict variance in glenoid AP diameter, glenoid height, and glenoid version. Scans were excluded from the regression if any demographic data was missing leading to a sample size of 96 patients. Two predictors were entered in the first step of the hierarchical multiple regression: patient height and weight. Gender and ethnicity were added in the second step of the regression models. African-Americans and females were used as reference groups. No violation of the assumptions of normality (Shapiro-Wilk test), linearity (correlation coefficients), multicolinearity (tolerance and Variance Inflation Factor), and homoscedasticity (graphical boxplot and Levene’s test) were observed. Independent-sample t-test was used to compare continuous and categorical data. All calculations were performed with SPSS Version 22.0 (IBM Corp., Armonk, NY, USA). The significance level was set at 0.05 for all analyses.
Results
In total, 108 patients were identified and included in this study. There were 53 males and 55 females with an average age of 50.8 ± 19.4 years. The mean patient height was 168 ± 12 cm. The mean patient weight was 80.4 ± 19.8 kg and the mean patient BMI was 28.6 ± 6.7. There were 53 (49.1 %) left shoulders and 55 (50.9 %) right shoulders included in the study. Due to patient data missing from the electronic medical records, 96 patients were used in the regression models. The mean glenoid AP diameter was 24.7 ± 3.5 mm and the mean glenoid height was 31.7 ± 3.7 mm. The mean glenoid version was 0.05 ± 9.1°. Detailed descriptive statistics information for all variables is provided in Table 1.
The regression model examining the relationship between the predictors (patient height, weight, gender, and ethnicity) and AP glenoid diameter was significant (p < 0.001). Height and weight in step 1 of the model explained 28.1 % of the variance in glenoid AP diameter with both height and weight being significant predictors (p < 0.001 and p = 0.01 respectively). Using the standardized beta coefficients, calculations for our dataset were made: an increase in patient weight of 24.31 kg (53.6 lbs.) and an increase in patient height of 9.6 cm (3.8 in. resulted in 1 mm increase in glenoid AP diameter according to the first step of our model. The introduction of gender and ethnicity in step 2 explained an additional 15.9 % in the variance of glenoid AP diameter. After the addition of gender and ethnicity as independent variables, height did not show to be a significant predictor of glenoid AP diameter anymore (p = 0.7). The correlation of patient weight and glenoid AP diameter also slightly changed such that an increase of 25.34 kg (55.9 lbs) in weight resulted in 1 mm increase in AP diameter (p = 0.01). Unstandardized B coefficients were used for interpretation of the relationship between gender and ethnicity, and AP glenoid diameter variables. The predicted male AP diameter was 3.4 mm larger than in females (p < 0.001). Patients of Asian ethnicity exhibited 4.1 mm smaller glenoid AP diameters than African-American patients (p = 0.002).
In step 1 of the second regression modeling the variance in glenoid height, patient height, and weight were introduced explaining 23.1 % of the variance (p < 0.001). Only patient height was a significant predictor where an increase in height by 7.4 cm (2.9 in) resulted in a 1 mm increase in glenoid height. After entry of patient gender and ethnicity in step 2, the total variance in glenoid height explained by the model was 33.7 % and gender appeared to be the significant predictor of glenoid height. Males had 2.9 mm larger glenoid height compared to females (p = 0.002).
Step 1 of the third model trying to investigate the ability of height and weight to predict degree of glenoid version was not significant (p = 0.33). After introducing the ethnicity and gender variables in step 2, the regression model explained 12.6 % of the variance in glenoid version (p = 0.04) where males were shown to have 8.4° more glenoid retroversion than females (p = 0.003). The Hispanic cohort demonstrated 6.4° of additional glenoid anteversion compared to African-Americans (p = 0.04). No side-to-side variance in glenoid version was observed in the study (p = 0.89).
Predicted values for glenoid AP diameter, height, and version stratified by gender and plotted against patient height are shown in Figs. 4, 5, and 6.
Discussion
The non-constrained anatomy of the glenohumeral joint creates a highly flexible articulation with a large arc of motion [9]. Understanding native anatomy is essential for maximizing function and minimizing complications during reconstructive surgery. This study focused on understanding the size and orientation of a normal glenoid cavity and how these parameters correlate with patient height, weight, gender, and ethnicity. This information is valuable during the pre-operative evaluation for a total shoulder arthroplasty because non-anatomic placement of the glenoid component can lead to increased rates of instability, clinical, and radiographic loosening [6, 10].
This particular study demonstrated that the average human glenoid version was approximately 0.05° (2.65 ± 9.01° for females and −1.65 ± 9° for males). Previous studies substantiated this finding, citing the average glenoid version to be close to −1° [3, 9]. Severe deviation from this can both be adaptive in high demand shoulders, or anatomic in different sexes and can also result in glenohumeral instability [3, 9]. Our findings are within the previously studied ranges.
This study identified gender as a significant independent predictor of glenoid version, which confirms the results of previous studies [3, 11, 12]. However, none of these studies controlled for patient height and weight. In addition, the results of our analysis showed ethnicity to be an independent factor determining glenoid version and AP diameter. However, because our glenoid version regression model explained very low percent (12.6 %) of the variance in the dependent variable, readers ought to interpret glenoid version predictors with caution. Larger sample size ethnic groups will be necessary to explore the precise relationship with glenoid version. Furthermore, variables such as humeral version, humeral neck-shaft angle, humeral head thickness, and radius of curvature may play a role in explaining more of the variance in glenoid version. Churchill et al. found a difference in glenoid version but did not report variance in glenoid size when comparing African-American and white patients [7].
Although patient height and weight correlated well with patient glenoid diameters, they had no significant prediction capacity for glenoid version. Female patients on average had a glenoid that was in slight anteversion while males had a retroverted glenoid. This may be related to activity level as higher demand shoulders tend to be in a higher degree of retroversion [3]. Certain past studies have failed to report this difference; however, the majority of these did not study pre-morbid shoulder anatomy [2, 7].
We found a significant difference in glenoid AP diameter between African-American and Asian populations after controlling for patient height. Our findings are based on a sample of five Asian patient CT measurements. They may not be predictive for other datasets and larger sample ethnic groups may be needed for obtaining narrower confidence intervals for the predicted values. A larger sample size ethnic groups study may be necessary to identify differences in glenoid version among other ethnicities. Interestingly, Edelson found wide variations amongst different ethnicities in humeral version, however, they did not evaluate glenoid version in their cadaveric study [13].
Gender appeared to be the strongest predictor of glenoid AP diameter and glenoid height. Even though, our male and female cohorts had a significant mismatch in patient height, males being 18.8 cm taller than females on average, the regression model provides correlation between gender and the dependent variables while keeping patient height constant.
Understanding differences in glenoid anatomy could help surgeons optimize planning and subsequent procedures, and also facilitate proper TSA instrumentation selection. Our data suggest women have a native glenoid that is slightly smaller and anteverted while men have a larger retroverted glenoid. Surgeons should be aware of this variance, regardless of the height and the weight of the patient. Other studies have examined the variances in glenoid surface area and humeral head size among patients of different age [14]. Bockmann et al. showed that older patients tend to have larger humeral heads and increased glenoid surface areas compared with younger patients [14]. The comparison was done in nonarthritic shoulders to minimize the possibility of osteophites being the cause for increased measurements in the older group. Interestingly, the authors did not find any age difference in terms of glenoid version in a study of 210 patient CT-scans [14].
In our multi-ethnic society, it does appear that surgeons need to take racial data into consideration when determining not only glenoid version and size, but also humeral head version [13]. Correction of pathologic glenoid anatomy during TSA has been proven to improve glenohumeral biomechanics and lead to better patient outcomes [5, 15]. Studies have shown that failure to correct excessive glenoid retroversion at the time of TSA leads to increased glenoid component shear stress and possible failure [5, 15]. Modern prosthetic designs and surgical techniques should be used in restoration of the native shoulder anatomy and function to avoid posterior displacement of the glenohumeral contact point and thus prevent early glenoid loosening and implant failure [10, 16]. Evaluation of the glenohumeral anatomy/pathoanatomy is also very important in other reconstructive procedures about the shoulder such as the ream and run procedure [17]. Unlike for TSA cases, experienced surgeons tend to rely mostly on standardized anteroposterior and true axillary radiographs for pre-operative shoulder assessment of ream and run procedure candidates [17]. This is mostly true for cases with less complicated pre-operative glenoid pathoanatomy (no excessive posterior glenoid erosion, double concavity, and posterior humeral head subluxation). Complicated cases will still necessitate a more comprehensive image of native glenoid anatomy that a CT scan study has to offer.
There are several limitations of this study. First, while CT scans were used to measure the glenoid, it may not be optimal for pre-operative planning due to exposure to ionizing radiation and the added cost [12]. MRI allows for characterization of soft tissue, but it is limited in the ability to accurately quantify bone loss when present [12]. Second, 3D-CT reconstruction was reported by several studies to be a more accurate method of measuring glenoid version, which is not available in the present study [1, 18]. However, the Friedman method was found to have excellent test-retest and inter-observer reliability with intraclass correlation coefficients of more than 0.95 [19]. Other methods similar to the Friedman method of glenoid version measurement, which correlate very well with Friedman’s method and were also shown to be reproducible, are described in the literature [20, 21]. They use a 2D CT axial cut of the shoulder as the conventional method, but are less subjective to error coming from the variation in scapular concavity, because their axes (to the medial end of the glenoid endostal vault) are much shorter than the axis of the scapula (to the medial scapular border) [20, 21]. However, these methods tend to slightly exaggerate glenoid retroversion compared with Friedman’s method.
Another limitation of the study is that the indication for CT was not recorded. However, any patients with shoulder bony pathology including arthritis were excluded to limit any anatomy divergent from a normal population. Furthermore, we did not record hand dominance, which may affect glenoid version in active patients [3, 11]. Lastly, we restricted the number of independent variables used in our regression models based on the sample size. We had not performed an a priori power analysis and even though the post hoc power analysis showed an achieved power of 0.999, 0.997, and 0.966 (glenoid AP diameter, glenoid height and version, respectively) we consider that larger sample size ethnic groups will be necessary to explore the precise multicultural relationship. Some authors recommend a sample size of 50 + 8 m (m = number of independent variables used in the regression) and other advocate having a minimum of ten participants per predictor variable [22, 23]. Our models had a sample size of around 13 participants per predictor variable, which is considered to be on the lower border of the appropriate sample size for the number of independent variables used in the regression. The regression models for the glenoid AP diameter and height explained a fair amount of the variability of the dependent variables and demonstrated a good fit for our data. The regression model for the glenoid version explained a very low percent of the variability and interpretation of the results should be with caution. Ideally, other glenohumeral measurements should be included in future models to achieve better explanation of the variance in glenoid version data.
This study demonstrates that patient gender and ethnicity should be considered irrespectively of patient weight and height when attempting to recreate native anatomy during TSA. By understanding the dimensions of a non-pathologic shoulder, procedures such as TSA can be better tailored to fit the patients’ anatomy and potentially lead to a reduction in glenoid loosening and implant failure.
Conclusion
Gender is the strongest independent predictor of glenoid size and version. Males exhibit a larger size and more retroverted glenoid than females. Patient height was found to be predictive of glenoid size only in patients of the same gender. Although variations in glenoid size and version are observed among ethnicities, larger sample size ethnic groups will be necessary to explore the precise relations. Surgeons should consider gender and ethnic variations in the pre-operative planning and surgical restoration of the native glenohumeral relationship.
References
Budge MD, Lewis GS, Schaefer E, Coquia S, Flemming DJ, Armstrong AD (2011) Comparison of standard two-dimensional and three-dimensional corrected glenoid version measurements. J Shoulder Elb Surg 20(4):577–583
Friedman RJ, Hawthorne KB, Genez BM (1992) The use of computerized tomography in the measurement of glenoid version. J Bone Joint Surg Am 74(7):1032–1037
Matsumura N, Ogawa K, Kobayashi S, Oki S, Watanabe A, Ikegami H, Toyama Y (2014) Morphologic features of humeral head and glenoid version in the normal glenohumeral joint. J Shoulder Elb Surg 23(11):1724–1730
Sabesan VJ, Callanan M, Youderian A, Iannotti JP (2014) 3D CT assessment of the relationship between humeral head alignment and glenoid retroversion in glenohumeral osteoarthritis. J Bone Joint Surg Am 96(8):e64
Iannotti JP, Weiner S, Rodriguez E, Subhas N, Patterson TE, Jun BJ, Ricchetti ET (2015) Three-dimensional imaging and templating improve glenoid implant positioning. J Bone Joint Surg Am 97(8):651–658
Brems J (1993) The glenoid component in total shoulder arthroplasty. J Shoulder Elb Surg 2(1):47–54
Brems J, Churchill RS, Kotschi H (2001) Glenoid size, inclination, and version: an anatomic study. J Shoulder Elb Surg 10(4):327–332
Lewis GS, Armstrong AD (2011) Glenoid spherical orientation and version. J Shoulder Elb Surg 20(1):3–11
Hohmann E, Tetsworth K (2015) Glenoid version and inclination are risk factors for anterior shoulder dislocation. J Shoulder Elb Surg 24(8):1268–1273
Powell K, Kwon YW, Yum JK, Brems JJ, Iannotti JP (2005) Use of three-dimensional computed tomography for the analysis of the glenoid anatomy. J Shoulder Elb Surg 14(1):85–90
De Wilde LF, Berghs BM, VandeVyver F, Schepens A, Verdonk RC (2003) Glenohumeral relationship in the transverse plane of the body. J Shoulder Elb Surg 12(3):260–267
Lenart BA, Freedman R, Van Thiel GS, Dhawan A, McGill KC, Basu S, Meyer JR, Provencher CM, Cole BJ, Romeo AA, Verma NN (2014) Magnetic resonance imaging evaluation of normal glenoid length and width: an anatomic study. Arthroscopy 30(8):915–920
Edelson G (1999) Variations in the retroversion of the humeral head. J Shoulder Elb Surg 8(2):142–145
Bockmann B, Soschynski S, Lechler P, Ruchholtz S, Debus F, Schwarting T, Frink M (2016) Age-dependent variation of glenohumeral anatomy: a radiological study. Int Orthop 40(1):87–93
Ricchetti ET, Hendel MD, Collins DN, Iannotti JP (2013) Is premorbid glenoid anatomy altered in patients with glenohumeral osteoarthritis? Clin Orthop Relat Res 471(9):2932–2939
Farron A, Terrier A, Buchler P (2006) Risks of loosening of a prosthetic glenoid implanted in retroversion. J Shoulder Elb Surg 15(4):521–526
Matsen FA 3rd (2015) The ream and run: not for every patient, every surgeon or every problem. Int Orthop 39(2):255–261
Hoenecke HR Jr, Hermida JC, Flores-Hernandez C, D’Lima DD (2010) Accuracy of CT-based measurements of glenoid version for total shoulder arthroplasty. J Shoulder Elb Surg 19(2):166–171
Rouleau DM, Kidder JF, Pons-Villanueva J, Dynamidis S, Defranco M, Walch G (2010) Glenoid version: how to measure it? Validity of different methods in two-dimensional computed tomography scans. J Shoulder Elb Surg 19(8):1230–1237
Andrin J, Macaron C, Pottecher P, Martz P, Baulot E, Trouilloud P, Viard B (2016) Determination of a new computed tomography method for measuring the glenoid version and comparing with a reference method. Radio-anatomical and retrospective study. Int Orthop 40(3):525–529
Poon PC, Ting FS (2012) A 2-dimensional glenoid vault method for measuring glenoid version on computed tomography. J Shoulder Elb Surg 21(3):329–335
Green S (1991) How many subjects does It take to do a regression analysis. Multivar Behav Res 26(3):499–510
Morgan B, Voorhis CRWV (2007) Understanding power and rules of thumb for determining sample sizes. Tutor Quant Methods Psychol 3(2):43–50
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Statement for human rights
The study was approved by the University of Illinois at Chicago IRB. The IRB protocol number is: #2012–0195
Ethical approval
For this type of study formal consent is not required
Funding
No external funding was provided for this study.
Rights and permissions
About this article
Cite this article
Piponov, H.I., Savin, D., Shah, N. et al. Glenoid version and size: does gender, ethnicity, or body size play a role?. International Orthopaedics (SICOT) 40, 2347–2353 (2016). https://doi.org/10.1007/s00264-016-3201-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-016-3201-8