Abstract
Purpose
We used the Optetrak Condylar Constrained (CCK) implant, a modular and constrained knee implant as replacement for a failed primary arthroplasty, to assess the survivorship, the complications, the clinical, radiological, and functional situation, and the quality of life of those patients in whom a CCK had been implanted in recent years in order to find predictive pre-operative conditions of survival and clinical outcomes.
Methods
We performed a retrospective study of 125 CCK implanted between 1999 and 2005. The mean follow-up was nine years (range, seven to 13). Mean age was 73.6 years. A total of 78 % of the revised TKA were cemented and 66 % were CR. We assessed the pre-operative, the operative and the postoperative conditions studying the medical files of all the patients. In order to study the functional and clinical situation we used the Hospital for Special Surgery (HSS) score and the Knee Society score (KSS), both clinical and functional. We analysed all the X-rays using the Knee Society Roentgenographic evaluation. The quality of life was studied using the Oxford knee score (OKS).
Results
The mean results of the KSS clinical and the KSS functional were 68.24 and 63.85, respectively. There were not any conditions associated with poor results of the knees (p > 0.05). The global survival at 24 months was 92.7 %, at 60 months 87.8 % and at 96 months it was 87.8 %. There were some conditions associated with poor survival of the knees, e.g. patients were younger than 70 years old, rheumatic diseases, kidney faliure, tibial tuberosity osteotomy, PS primary arthroplasty, revision before five years and septic loosening.
Conclusions
Based on these results there are some pre-operative factors that change the survival of the total knee replacement revision.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Revision total knee arthroplasty (TKAR) is a common procedure, of which 38,000 were performed in 2003 in the United States [1], which is projected to increase six times to 268,000 by 2030 [1]. In a meta-analysis of 42 TKAR studies comparing 1,515 patients, the author published a long-term global survival rate of 79 % [2]. These TKAR survivals can have a significant impact on patient satisfaction, medical costs, and health care use. A better understanding of predictive factors for TKAR survival can inform patients and surgeons and help us target modifiable risk factors to improve TKAR outcomes [3].
Very few studies assessing survival after TKAR have been published. As reported above, pre-operative conditions are not associated with postoperative survival after TKAR [4]. Other TKAR studies report as predictors of survival, the age, sex, time after primary arthroplasty, cemented implants [2] and rheumatoid arthritis [5]. Thus, very few published studies have examined predictors after TKAR. Most studies had small sample sizes and therefore limited power to examine predictors of survival [6–10].
This study aimed to evaluate and compare the CCK implanted as replacement of a failed primary total knee arthroplasty and to assess the survivorship, the complications, the clinical, radiological, and functional situation, and the quality of life of those patients in whom a CCK revision total knee arthroplasty had been implanted in the past in order to study if there is any pre-operative condition that changes the outcomes and survival of the revision arthroplasties.
Patients and methods
Study design
We performed a retrospective observational study of patients who underwent a total knee replacement revision.
Inclusion criteria were:
-
Aseptic loosening of a primary total knee arthroplasty
-
Optetrak Condilar Constrained implant
-
Patients able to understand instructions and follow a rehabilitation treatment
Exclusion criteria were:
-
Septic loosening of a primary total knee replacement
-
Aseptic loosening of a primary unicondilar knee arthroplasty
-
Aseptic loosening of a primary femoro-patelar knee arthroplasty
-
Second knee replacement
-
Revision of an unstable arthroplasty because of a periprothesic fracture
-
Terminal illness
Study group
One hundred twenty-five Optetrak Condilar Constrained (CCK) implants were placed in 117 patients between 1999 and 2005. Of these, 40 were excluded for the following reasons: ten patients died from causes unrelated to the arthroplasty, 15 presented a septic loosening of their primary arthroplasty, six of them presented a femoro-patelar knee arthroplasty, three patients received their second knee replacement, two were terminal patients that received surgery to treat their illness and four of them received surgery to treat an unstable arthroplasty after periprosthetic fracture.
Surgical technique
Patients were operated by a group of surgeons with different levels of experience. The majority of the patients underwent surgery under spinal anaesthesia while 24.7 % received general anaesthesia.
After removing the primary implants all the patients received a condilar constrained total knee arthroplasty, Optetrak CCK. The revision was performed through a longitudinal anterior incision done following the previous approach. The femoral and tibial cuts were done using an endo-medullary guide. Metal supplements were used if the bone loss was significant. Some patients required a lateral retinacular release or a tibial tuberosity osteotomy to treat intra-operative femoro-patellar instability.
Clinical assessment
Variables included age, sex, medical pathologies, ASA risk (American Society of Anesthesiology) [11, 12], type of anaesthesia, side of the knee, primary arthroplasty conditions, experience of the surgeon, intra-operative and postoperative complications, time to discharge, survival and mean follow-up.
At the end of follow-up each patient was contacted for a radiographic and clinical assessment conducted by three independent surgeons who had not taken part in the surgery (RL, BR and AU).
In the pre-operative radiographic projections applied (anteroposterior and lateral), the presence of deformity, primary arthroplasty angles (femoro-tibial, alfa femoral, beta tibial, sagittal femoral and sagittal tibial angles) were assessed. In the postoperative revision arthroplasty angles (femoro-tibial, alfa femoral, beta tibial, sagital femoral and sagital tibial angle) and evolution of the tibial osteotomy were studied [13].
At the end of the follow-up, a survey on all patients was conducted in order to assess their clinical and functional status and their health related quality of life. The Knee Society score (KSS) evaluated both clinical and functional parts [14, 15], and for the Oxford knee score (OKS) the Health Related Quality of Life (HRQoL) questionnaire was completed by the patient [15, 16].
Statistical analysis
Qualitative variables are presented with their frequency distribution and percentage. Quantitative variables were summarized with mean and standard deviation (mean ± SD). Quantitative variables showing a skewed distribution were summarized with median and interquartile range (IQR). We evaluated the association between qualitative variables with chi-square test or Fisher exact test. A comparison of continuous variables that show a normal distribution was performed by analysis of variance (ANOVA). Multiple comparisons were performed between groups using the Bonferroni test. For variables with skewed distribution the Kruskal-Wallis non-parametric test was used. We evaluated the survival of the TKAR using the Kaplan Meier curves. In order to study if there is any variable that changes their survival a univariable study was done. Kaplan-Meier curves were compared using Cox models and adjusted Hazard ratios were performed. Finally, a Cox multivariable model was done using those factors that had a p < 0.05 and were clinically relevant. For all tests a value of significance of 5 % was accepted. Processing and data analysis was performed using SPSS 15.0.
Results
Demographics
The mean age of the patients was 73.66 ± 6.6. The gender distribution (F/M) was 77.6 %/33.4 %. The most frequently affected knee was the right in 51.8 %. The 73.6 % of our patients suffered cardiovascular diseases and 20.5 % presented diabetes mellitus. The 14.5 % was obese (BMI > 40). The distribution of patients regarding their anaesthetic risk was 0 % ASA I, 51.2 % ASA II, 45.1 % ASA III and 3.7 % ASA IV (Table 1).
Perioperative characteristics
The anaesthesia was spinal in 75.3 %. A total of 78 % of the revised TKA were cemented and 66 % were CR. The revision was done after more than five years following the primary TKA in 59 % of the patients. The revision was performed by three groups of surgeons according to their experience: consultants (34.1 %), high skilled surgeons (60 %) and middle grade surgeons (5.9 %). Mean operative time in minutes was 194.48 ± 39.38. The mean hospital stay was 20.9 ± 3.53 days. Of the postoperative incidents including swelling, haematoma, celullitis, and superficial skin infection, 14.5 % were solved with medical treatment.
There was a 7.2 % rate of complications that required surgery including deep infection, skin necrosis, tibial osteotomy fracture and quadriceps rupture.
Clinical outcomes
The mean follow-up was 87.47 ± 19.3 months. While the mean clinical KSS was 63.85 ± 20.71, the mean functional KSS was 68.24 ± 24.95. In the analysis of each of the items on the KSS, the mean range of motion was 97.49° ± 18.19°. Regarding active flexion, the mean range of motion was 99.23° ± 15.76°. The mean extension lag measured was 2.09 °± 7.67°. A total of 97.3 % had a stable knee in the frontal plane and 89.3 % in the sagittal plane; 50.5 % of our patients never or occasionally had pain while 29.7 % referred to mild pain. Also, 48.6 % of our patients were able to walk without limitations and 32.4 % could walk at least for 30 minutes. A total of 89.7 % of our patients were able to use stairs, but only 29.7 % of them did not need help to walk (Table 2).
The KSS was excellent or good in 72.9 % of our revisions. We did not find correlations between pre-operative conditions and postoperative results.
The perceived HRQoL of patients measured by Oxford knee score was 36.61 ± 7.88. The patients with the worst HRQoL before surgery improved more than the others. We did not find pre-operative factors associated with a better HRQoL after surgery. All but one question of this score improved after surgery. Neither before nor after revision were the patients able to kneel down and get up again afterwards.
Mean total KSS and the HRQoL according to OKS were correlated, obtaining a positive but weak correlation coefficient (r = 0.79, p < 0.005) between them, and this correlation was statistically significant. Patients who scored highest on the KSS, also perceived a higher HRQoL.
Survival
Global and aseptic survivals were distinguished three times during follow-up (at 24, 60 and 96 months). While the global survival (failure for any cause) at 24 months was 92.7 %, it was 87.8 % at 60 months and at 96 months it was 85.8 %. The survival excluding infections was 96.1 %, at 24 months, 93.4 % at 60 months and 91.4 % at 96 months.
There were some conditions associated with poor survival of the TKRA. The univariate analysis showed the worst survival if:
-
1.
Patients were younger than 70 years (p0,04), rheumatic diseases (p0.05) or kidney faliure (p0.05)
-
2.
Tibial tuberosity osteotomy (p0.001)
-
3.
PS primary arthroplasty (p0.03)
-
4.
Replacement done before five years (p0.05)
-
5.
Septic failure (p0.01)
When multivariate analysis was done all variables lost their statistical significance (p > 0.05) except PS primary arthroplasty (p 0.03) and tibial tuberosity osteotomy (p0.002).
Radiographic analysis
The mean femoro-tibial angle changed from pre-operative 1.75 to 7.02 at the end of follow-up. Both alfa-femoral and beta-tibial were similar before and after surgery. Significant differences between both sagittal–femoral and sagittal–tibial were noted (Table 3).
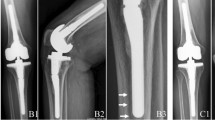
Tibial osteotomy was performed in 30 patients. Consolidation was achieved in 22 developing a non-union in eight patients (Fig. 1).
Complications
We found a total of 23 major complications in 17 patients (29 % of the sample); three patients presented pain and stiffness (3.6 %). There were eight patients with non-union of the tibial osteotomy (9.4 %), seven of them presenting extensor mechanism failure (8.2 %). Six of these patients were operated to repair their extensor mechanism. There was one case of shaft femoral periprosthesic fracture that required osteosynthesis with plates and screws (1.2 %).
Septic loosening was found in six cases (7.4 %), and five patients (6.6 %) presented aseptic failure.
Discussion
In relation to the demographic characteristics of our study population, the average age of our sample is higher than in other studies [2–4, 6, 8–10, 17–22]. Our patients have an average age of 73.6 years and nearly 85 % of them are older than 68 years.
In regards to the pre-operative medical condition, our patients had similar characteristics to patients treated in other centres. A total of 19 % of our patients had morbid obesity (BMI > 40), which is a percentage similar to published series [23–31]. Also, 18 % of our patients had diabetes mellitus, and 9.3 % were rheumatic patients. Assessing surgical risk, using the classification of the American Society of Anesthesiologists (ASA), 48.8 % of our patients were classified as ASA III and ASA IV, similar to published series using this scale [3].
The original arthroplasty was cemented in 78 % of our cases, 66 % were cruciate retaining and the replacement was done after more than five years in 62 % of the cases, all in the same range as other series [4, 6, 8, 9, 21, 22, 32].
According to the literature, our outcomes are very similar to those published [9, 18, 20, 22, 23]. While our mean clinical KSS was 63.85 ± 20.71, our mean functional KSS was 68.24 ± 24.95. Some published replacement series with PS implants obtained worst outcomes: a KSS-C of 68 and a KSS-F of 56 [22] or KSSC of 57 and KSSF 76 [23]. Other authors published better results: a KSSC of 77 and a KSSF of 49 [20] or KSSC of 88.5 and KSSF of 72.4 [9]. Saleh studied a mix replacement series with PS and CR implants that obtained a global KSS of 66.2 [18]. We did not find positive predictive factors as many authors published no clinical outcome predictors [33–35]. However, Singh found an association between poorer functional outcomes and female patients, aged 80 and obese [3].
While our short-term global survival (24 months) was 92.7 %, Sheng in his meta-analysis published a 95 % global survival at two years [19]. According to the literature, our medium-term aseptic survival (60 months) was 93.4 %, similar to reviewed series, e.g. 87.4 % aseptic survival at five years [36], 89 % at five years [19], 92 % at five years [37], and 100 % at seven years [9].
The long-term global survival (96 months) of our revision arthroplasties was 86.6 %, somewhat better than that found in the literature, e.g. 83 % global survival at eight years [4], 82 % at 12 years [38], and 79 % overall survival at ten years [19].
Regarding the overall loosening rate the univariate study showed that global survival was lower in patients younger than 70 years (p0,04), with rheumatoid arthritis (p 0.05), kidney faliure (p 0.04), tibial tubercle osteotomy (p 0.001), PS primary arthroplasty (p 0.03), primary replacement done before five years (p0.05), and septic loosening (p 0,01). When multivariate analysis was done all variables lost their statistical significance (p > 0.05) except PS primary arthroplasty (p 0.03) and tibial tuberosity osteotomy (p 0.002).
Regarding published predictors in replacement survival studies, we have similar conclusions [4, 5, 19, 39]. On one hand, Hass in his 1995 series didn’t find association between long-term survival of their arthroplasties and pre-operative conditions, the original diagnosis or the characteristics of polyethylene [4]. On the other hand, Sheng’s series of 2006 replacement aseptic survival reports that the univariate analysis found statistically significant longer survival in patients older than 70 years (p < 0.005), women (p0.07), primary replacements over five years (p < 0.00015), cemented implants (p < 0.05) and those with bone grafts (p0.05); in the multivariate analysis only age retained its statistical evidence (p < 0.005) [19]. Similar conclusions were published when rheumatologic diseases (rheumatoid arthritis) were related with decreased survival (p < 0.001) [5]. Other authors found decreased replacement survival associated with rheumatoid arthritis patients, due to increased infection rate [39].
Our complication rate was 29 % and the incidence of a new revision was 13.6 %, both in the range published in the literature (26.3 % complications and 12.9 replacement [19], 30 % complications and 7.2 % replacement [40], 13 % complications and 8 % replacement [4], 9 % complications [41] and 18.3 % replacement [42]). The rate of complications requiring reoperation is even lower than that published by some authors (49 % global loosening [19], 31 % septic loosening [38] and 20 % septic loosening [43]). However, our patients tend to suffer more septic loosening than mechanical loosening.
Studying our statistically significant survival predictive conditions and our reoperations, the septic loosening is our worst problem. Infection is associated with chronic diseases like rheumatoid arthritis and kidney failure. Septic failure usually occurred before five years after the primary arthroplasty.
A significant number of tibial tuberosity osteotomy developed a non-union, and weakness or a defect on the anterior proximal tibia with the corresponding higher risk of aseptic failure.
The higher frequency of PS TKA failure in this series is related to the use of this type of knee in most cases in our institution.
Limitations of our study include the retrospective nature, the non-randomization of the process, and the number of patients recruited. Strengths of the study include a minimum of seven years of follow-up and the detailed functional and radiological assessment of all the cases included.
Conclusions
The HRQoL, the survival, the clinical and functional outcomes measured with the KSS of the CCK as revision knee arthroplasty are overall good or very good. We found a positive correlation between a higher KSS score and a higher OKS result.
In regards to the predictive pre-operative conditions study we found that global survival was lower in patients that were younger than 70 years, had rheumatologic illness, kidney faliure, tibial osteotomy, replacement done before five years and septic loosening. The multivariate analysis done shows that patients with a PS primary arthroplasty and tibial osteotomy have lower global survival.
References
Kurtz S, Ong K, Lau E, Mowat F, Halpern M (2007) Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am 89(4):780–785
Sheng P, Lehto M, Kataja M, Halonen P, Moilanen T (2004) Patient outcome following revision total knee arthroplasty: a meta-analysis. Int Orthop 28:78–81
Singh JA, O’Byrne MM, Harmsen WS, Lewallen DG (2010) Predictors of moderate-severe functional limitation 2 and 5 years after revision total knee arthroplasty. J Arthroplast 25(7):1091–1095
Haas SB, Insall JN, Montgomery W, Windsor RE (1995) Revision total knee arthroplasty with use of modular components with stems inserted without cement. J Bone Joint Surg Am 77:1700–1707
Rand JA, Trousdale RT, Ilstrup DM, Harmsen WS (2003) Factors affecting the durability of primary total knee prostheses. J Bone Joint Surg Am 85-A:259–265
Gandhi R, Tsvetkov D, Davey JR, Mahomed NN (2009) Survival and clinical function of cemented and uncemented prostheses in total knee replacement: a meta-analysis. J Bone Joint Surg Br 91(7):889–895
Barrack RL, Engh G, Rorabeck C, Sawhney J, Woolfrey M (2000) Patient satisfaction and outcome after septic versus aseptic revision total knee arthroplasty. J Arthroplasty 15(8):990–993
Wang CJ, Hsieh MC, Huang TW (2004) Clinical outcome and patient satisfaction in aseptic and septic revision total knee arthroplasty. Knee 11:45–49
Lee JK, Kim SJ, Choi CH, Chung HK (2012) Revision total knee arthroplasty using a constrained condylar knee prosthesis in conjunction with a posterior stabilized articular polyethylene. J Arthroplasty 28(4):566–569
Hwang et al (2010) Revision total knee arthroplasty with various prosthesis designs. Clin Orthop Surg 2(2):112–120
Dripps RD, Lamont A, Eckenhoff JE (1961) The role of anesthesia in surgical mortality. JAMA 178:261–266
Weaver F, Hynes D, Hopkinson W et al (2003) Preoperative risks and outcomes of hip and knee arthroplasty in the Veterans Health Administration. J Arthroplasty 18:693–701
Frederick C, Ewald MD (1989) The knee society total knee arthroplasty roentgenographic evaluation and scoring system. Clin Orthop 248:9–12
Insall JN, Dorr LD, Scott WN (1989) Rationale of the Knee Society clinical rating system. Clin Orthop Relat Res 248:13–14
Asif S, Choon DSK (2005) Midterm results of cemented Press Fit Condylar Sigma total knee arthroplasty system. J Orthop Surg 13(3):280–284
Dawson J, Fitzpatrick R, Murray D, Carr A (1998) Questionnaire on the perceptions of patients about total knee replacement. J Bone Joint Surg Br 80(1):63–69
Saleh KJ, Dykes DC, Tweedie RL, Heck DA (2002) Functional outcome after total knee arthroplasty revision: a metaanalysis. J Arthroplasty 17:967–977
Saleh KJ, Hoeffel DP, Kassim, Burstein C (2003) Complications after revision total knee arthroplasty. J Bone Joint Surg Am 85-A(Supplement 1):72–75
Sheng PY, Konttinen L, Lehto M, Ogino D, Jamsen E, Nevalainen J, Pajamaki J, Halonen P, Konttinen YT (2006) Revision total knee arthroplasty: 1990 through 2002. A review of the Finnish arthroplasty registry. J Bone Joint Surg Am 88(7):1425–1430
Incavo S, Wild J, Coughlin M et al (2007) Early revision for component malrotation in total knee arthroplasty. Clin Orthop Relat Res 8:458–464
Mulhall KJ, Ghomrawi HM, Scully S et al (2006) Current etiologies and modes of faliure in total knee arthroplasty revision. Clin Orthop 446:45–50
Van den Broek CM, Van Hellemondt, Jacobs, Wymenga (2006) Step-cut tibial tubercle osteotomy for access in revision total knee replacement. Knee 13:430–434
Sternheim A, Lochab J, Drexler M, Kuzyk P, Safir O, Gross A, Backstein D (2012) The benefit of revision knee arthroplasty for component malrotation after primary total knee replacement. Int Orthop 36(12):2473–2478
Kane RL, Saleh KJ, Wilt TJ, Bershadsky B, Cross WW 3rd, MacDonald RM, Rutks I (2003) Total knee replacement. Summary, Evidence Report/Technology Assessment: Number 86. AHRQ Publication Number 04-E006-1. Agency for Healthcare Research and Quality, Rockville
Kane RL, Saleh KJ, Wilt TJ, Bershadsky B (2005) The functional outcomes of total knee arthroplasty. J Bone Joint Surg Am 87(8):1719–1724
Robinson RP (2005) Five-year follow-up of primary Optetrak Posterior Stabilized total knee arthroplasties in osteoarthritis. J Arthroplasty 20(7):927–931
García-Crespo R, Marco F, Moro LE, Ariza G, Luque R, López-Durán L (2011) Midterm results of optetrak posterior-stabilized total knee system after 7 to 12 years in a University Hospital. J Arthroplasty 26(8):1326–1332
Thelu CE, Pasquier G, Maynou C, Migaud H (2012) Poor results of the Optetrak™ cemented posterior stabilized knee prosthesis after a mean 25-month follow-up: analysis of 110 prostheses. Orthop Traumatol Surg Res 98(4):413–420
Anderson JA, Baldini A, MacDonald JH, Pellicc PM, Sculco T (2006) Primary constrained condylar knee arthroplasty without stem extensions for the valgus knee. Clin Orthop Relat Res 442:199–203
Abbas D, Gunn RS (2006) Medium-term results of the scorpio total knee replacement. Knee 13:307–311
Nakama GY, Peccin MS, Almeida GJ, Lira Neto Ode A, Queiroz AA, Navarro RD (2012) Cemented, cementless or hybrid fixation options in total knee arthroplasty for osteoarthritis and other non-traumatic diseases. Cochrane Database Syst Rev 17:10, CD006193
Fehring TK, Odum S, Griffin WL, Mason JB, Nadaud M (2001) Early failures in total knee arthroplasty. Clin Orthop 392:315–318
Deehan DJ, Murray JD, Birdsall PD et al (2006) Quality of life after knee revision arthroplasty. Acta Orthop 77:761
Pun SY, Ries MD (2008) Effect of gender and preoperative diagnosis on results of revision total knee arthroplasty. Clin Orthop Relat Res 466:2701–2707
Fehring TK, Odum S, Griffin WL et al (2005) Outcome comparison of partial and full component revision TKA. Clin Orthop Relat Res 440:131–142
Ong KL, Lau E, Suggs J, Kurtz SM, Manley MT (2010) Risk of subsequent revision after primary and revision total joint arthroplasty. Clin Orthop Relat Res 468:3070–3076
Meijer MF, Reininga IH, Boerboom AL, Stevens M, Bulstra SK (2013) Poorer survival after a primary implant during revision total knee arthroplasty. Int Orthop 37(3):415–419
Suárez J, Griffin W, Springer B, Fehring T, Mason JB, Odum S (2008) Why do revision knee arthroplasties fail? J Arthroplasty 23(suppl 1):99–103
Jamsen E, Huhtala H, Puolakka T, Moilanen T (2009) Risk factors for infection alter knee arthroplasty: a register-based analysis of 43,149 cases. J Bone Joint Surg Am 91(1):38–47
Callaghan JJ, Insall JN, Greenwald AS, Dennos DA, Komistek AD, Murray DW et al (2000) Mobile-bearing knee replacement. Concepts and results. J Bone Joint Surg Am 82:1020–1041
Kim YH, Kim JS (2009) Revision total knee arthroplasty with use of a constrained condylar knee prosthesis. J Bone Joint Surg Am 91(6):1440–1447
Mortazavi SM, Molligan J, Austin MS, Purtill JJ, Hozack WJ, Parvizi J (2011) Failure following revision total knee arthroplasty: infection is the major cause. Int Orthop 35(8):1157–1164
Sierra RJ, Cooney WPIV, Pagnano MW, Trousdale RT, Rand JA (2004) Reoperations after 3200 revision TKAs: rates, etiology, and lessons learned. Clin Orthop Relat Res 425:200–206
Disclosure statement
All authors confirm they have not received any financial payments or other benefits from any commercial entity related to the subject of this article. No outside funding or grants assisted this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Luque, R., Rizo, B., Urda, A. et al. Predictive factors for failure after total knee replacement revision. International Orthopaedics (SICOT) 38, 429–435 (2014). https://doi.org/10.1007/s00264-013-2268-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-013-2268-8