Abstract
Purpose
Hallux valgus is a complex deformity of the first metatarsophalangeal joint, with varus angulation of the first metatarsal, valgus deviation of the great toe and lateral displacement of the sesamoids and the extensor tendons. The aim of the surgery is to achieve correction of the varus deviation of the 1st metatarsal which is considered by some as the primary intrinsic predisposing factor to hallux valgus deformity.
Methods
We retrospectively reviewed 85 patients (107 feet) who underwent an opening wedge osteotomy of the 1st metatarsal for correction of moderate to severe hallux valgus and metatarsus primus varus. A medially applied anatomic pre-contoured locking plate was used for fixation of the osteotomy.
Results
The mean IMA was decreased from 15.8 (range 12–22) degrees to 7.8 (range 0–12) degrees. The mean pre-operative HVA was 39 (range 21–52) degrees and the mean postoperative HVA was 11.8 (6–19) degrees. The pre-operative AOFAS score was 52 (SD 3.1) and the postoperative score was 85 (SD 5.2).
Conclusion
The proximal opening wedge metatarsal osteotomy is a safe, effective and reproducible technique for correction of moderate to severe hallux valgus deformity. The use of a locking plate provides enough control at the fragments, enhancing healing of osteotomy and maintenance of the correction even with a violated proximal lateral cortex.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Hallux valgus (HV) is a complex deformity of the first metatarsophalangeal joint (MTP), with varus angulation of the first metatarsal, valgus deviation of the great toe and lateral displacement of the sesamoids and the extensor tendons [1].
The aim of the surgery is to achieve correction of the varus deviation of the 1st metatarsal (metatarsus primus varus—MPV), which is considered by some as the primary intrinsic predisposing factor to HV deformity [2]. Selection of the proper procedure is critical to achieve an adequate result and durable correction of the deformity. Numerous surgical procedures have been described for correction of HV. The choice of procedure depends mainly on the severity, location and nature of the pathology [3]. It is widely accepted that treatment of moderate to severe hallux valgus deformity (hallux valgus angle >20°, I–II intermetatarsal angle >13°) usually necessitates use of a proximal metatarsal osteotomy or a metatarsocuneiform arthrodesis combined with a distal soft tissue procedure [4–6].
Different types of proximal metatarsal osteotomies have been used over the last decades including proximal crescentic osteotomy [7], proximal chevron osteotomy [8, 9], scarf osteotomy [10, 11], Ludloff osteotomy [12], Mau osteotomy [13], modified Mau [14], lateral closing wedge basal osteotomy [15] and medial opening wedge basal osteotomy [16].
The latter technique was historically seldom used due to lengthening of the 1st metatarsal, resulting in tightening of the soft tissues of the 1st MTP joint and predisposing to jamming of the joint and subsequent arthritis [17]. Over the subsequent years, proximal opening wedge osteotomy of the 1st metatarsal has become more popular and an effective technique for the correction of moderate to severe hallux valgus deformity.
The aim of this study was to present the mid-term results of the proximal opening wedge metatarsal osteotomy with the use of plate fixation. To our knowledge, this case series has the longest follow up of a significant number of patients treated for hallux valgus deformity with the basal opening wedge metatarsal osteotomy fixed with a locking plate.
Materials and methods
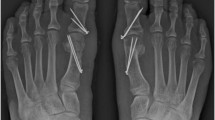
Between 2006 and 2011, an opening wedge osteotomy of the 1st metatarsal with distal lateral soft tissue release and medial bunionectomy was performed for 107 feet, in 85 patients, for correction of moderate to severe hallux valgus and metatarsus primus varus (Figs. 1 and 2). Additional procedures were performed to address deformities of the lesser toes, e.g. Weil osteotomy or PIP joint fusion in 64 feet, and to correct additional deformities of the great toe, e.g. Akin osteotomy in 37 feet and Reverdin distal metatarsal osteotomy in 18 feet. Twenty-three patients (28 feet) were males and 62 patients (79 feet) females. Sixty-one feet were right and 46 were left. The mean age was 56 (range 19–76) years. The mean age of males was 55 (range 32–72) years and the mean age of female patients was 48 (range 19–76) years. The mean follow up was four (two to 5.5) years.
All operated feet had dorsoplantar and lateral weight bearing radiographs performed pre-operatively and postoperatively at six weeks, three months, one year and at the last followup.
We evaluated the following criteria: hallux valgus angle (HVA), first intermetatarsal angle (I–II IMA), distal metatarsal articulation angle (DMAA), length of the 1st metatarsal, 1st MTP joint congruency and radiographic union.
All patients were clinically examined and graded by the AOFAS score, the VAS FA score and the FFI score pre-operatively and at three months followup [18–20]. Total MTP joint range of motion (dorsiflexion plus plantarflexion) was measured with a hand-held goniometer by the treating surgeon preoperatively and at three months postoperatively.
Clinical union was considered when pain-free, solid, non-mobile union was achieved. Cross-bridging on two orthogonal radiographs, interpreted by two surgeons (DG, IB), was considered as radiological union (Fig. 3). In cases that radiological union was in doubt, CT scan was performed to confirm the union. More than five degrees of HVA increase in a postoperative radiograph was considered a recurrence.
Analysis of variance was performed with the Wilcoxon signed rank null hypothesis test and statistical significance was defined at the 5 % (p < 0.05) level.
All cases were performed under general anaesthesia and ankle block, with a thigh tourniquet on after administration of 1.5 g Cefuroxime. A medial midline incision was carried from the metatarsocuneiform (MTC) joint proximally to the base of the 1st phalanx distally. Longitudinal capsulotomy of the 1st MTP joint and excision of medial bunion was performed subsequently. An osteotomy of the base of 1st metatarsal was made perpendicular to the shaft with direction from dorsomedial to plantarlateral and about 1.5 cm distal to the proximal articular surface of the metatarsal. Care was taken not to penetrate the plantarlateral cortex. The osteotomy was carefully teased open with an osteotome and the appropriate wedge plate with a central spacer ranging from 2 mm to 7 mm (Darco Bow II 2.7 mm locking plate, Wright medical technology, Arlington, TN) was used (Fig. 4). The desired correction was an I–II IMA of approximately 6–8°. Fluoroscopy was used to determine the correction of deformity. Bone graft taken from the medial bunion was used to fill the gap of the osteotomy in every case.
Lateral capsular release of the 1st MTP joint and adductor hallucis tenotomy were performed through a dorsal incision in the first web space. The medial capsule of the 1st MTP joint was then repaired with absorbable sutures.
The postoperative rehabilitation protocol included no cast immobilization, elevation of the foot for one week, immediate passive mobilization of the 1st MTP joint, and heel weight bearing mobilization in a stiff-soled shoe for four weeks, which was discontinued at six weeks.
Results
The mean IMA was decreased from 15.8 (range 12–22) degrees preoperatively to 7.8 (range 2–12) degrees postoperatively. This angle remained constant from the time of union to the last follow-up. The mean pre-operative HVA was 39 (range 21–52) degrees, and the mean postoperative HVA was 11.8 (6–19) degrees. The mean HVA at the last follow-up was 12.7 (range 6–30) degrees. The mean lengthening of the 1st metatarsal was 1.2 mm (range 0.6–2.5 mm). The range of motion of the 1st MTP joint was decreased from a mean of 73.3° preoperatively to 66.9° at three months postoperatively.
The preoperative AOFAS score was 52 (SD 3.1) and the postoperative score was 85 (SD 5.2). The median FFI score was preoperatively 73 (SD 6.3) and postoperatively 19 (SD 4.6) and the VAS FA was 55 (SD 6.8) and 82 (SD 8.1), respectively.
The osteotomy was fixed using a 3-mm, 4-mm, 5-mm or 6-mm spacer plate. The 5-mm-spacer plate was used in 55 cases. The average correction of IMA achieved was 2.6° per 1-mm spacer used. Table 1 demonstrates the spacer sizes used and the corresponding amount of correction. Union was achieved at an average of 6.5 weeks and confirmed clinically and radiologically.
Complications of the proximal open wedge metatarsal osteotomy are summarized in Table 2. Two patients with delayed union (1.8 %) were managed with partial weight bearing mobilization in a walking boot for six weeks. In both cases, union was achieved uneventfully. We encountered two cases (1.8 %) with recurrence of hallux valgus deformity. The first one was complicated with non-union of the proximal metatarsal osteotomy. Revision of the metatarsal osteotomy using bone graft and additional arthrodesis of the 1st MTP joint achieved complete union at both sites seven weeks post revision surgery. The second patient had an asymptomatic recurrence of hallux valgus deformity with complete union of the metatarsal osteotomy. He declined any further surgical intervention. Other complications were superficial infection in three cases (2.8 %) treated with oral antibiotics and four patients (3.7 %) with symptomatic hardware associated in one of them with numbness of the incision site. All four patients required removal of metalwork after complete union of the osteotomy with satisfactory results.
Discussion
Osteotomy of the proximal metatarsal in combination with a distal soft tissue procedure is performed for the correction of moderate to severe hallux valgus [7, 21]. It is recommended for correction of HVA greater than 20° and I–II IMA greater than 15° [2].
Proximal metatarsal opening wedge osteotomy has been historically used to correct metatarsus primus varus, using either bone graft alone to maintain the correction of deformity [16] or different fixation devices such as K-wires, staples, screws and mini external fixators [22–25]. The use of a plate with a spacer is a more recent technique which offers a stable fixation that maintains intraoperative correction with an accelerated postoperative recovery [26, 27].
In this study, we reported a significant decrease in I–II IMA of a median value of 8° (p < 0.05) and in HVA of a median value of 17.2° (p < 0.05). These results compare favourable with the results of previous studies with the use of a similar wedge plate [21, 27–30]. Overall a correction of 2.6° per mm spacer size was obtained. In the literature, the average correction in the transverse plane reported ranges from 1.5° per mm to 3° per mm [21, 26].
The primary advantage of a proximal opening wedge osteotomy compared with a closing wedge osteotomy is the preservation of metatarsal length, thereby decreasing the risk for development of transfer metatarsalgia [31]. On the other hand, the lengthening created with the opening wedge results in tightening of the soft tissues about the 1st MTP joint and predisposing the joint to recurrence of hallux valgus deformity, jamming and subsequent arthritis [17]. In our study the mean lengthening of the 1st metatarsal was 1.2 mm, in comparison with lengthening of 2–2.3 mm reported in other studies [30, 32]. Although statistically significant, the lengthening of the first metatarsal did not clinically affect the good outcome of the procedure. The range of motion of the 1st MTP joint decreased postoperatively for a mean value of 6.4° which was clinically and statistically insignificant and did not diminish the overall satisfaction of patients. Similar results are reported in the literature [26].
We encountered one case of non-union of osteotomy and recurrence of hallux valgus deformity. We revised the proximal metatarsal osteotomy with bone graft and we also proceeded with an arthrodesis of the 1st MTP joint. The osteotomy united uneventfully and the patient was satisfied with the final outcome. A second case of recurrence of hallux valgus deformity was probably due to inadequate lateral capsular release and adductor tenotomy and poor quality of the medial capsule repair. The patient declined any further surgical intervention.
The most common postoperative complication was associated with the plate. Four plates caused irritation to skin. All four plates were applied at the medial side of the metatarsal as performed routinely during the early period using this technique [21, 33]. Since we changed our practice, applying the plate more dorsomedially at the proximal metatarsal, no further cases of metalwork-related symptoms have been seen [26]. No cases of loss of correction or failure of metalwork were noted. Even in the few cases that the lateral cortex of the 1st metatarsal with the power saw was violated, the locking plate offered a very rigid fixation. Additionally the spacer on the plate acted as a pillar holding the wedge at the desired width. The use of bone graft was purely for its osteoconductive properties rather its structural function.
The statistically significant increase of the AOFAS score (p < 0.05) corresponds to the successful clinical outcome of this surgical procedure. Both VAS FA and FFI scores improved statistically significantly (p < 0.05), reflecting the dramatic improvement with regard to pain and function. Similar results were reported in other studies using the same method with similar implants [26, 28, 30].
As with all observational studies, this study contains methological limitations that may have influenced the validity of our conclusions. There is also the difficulty of assuming clinical significance based on statistical significance in the setting of a retrospective study such as this.
In conclusion, the proximal opening wedge metatarsal osteotomy is a safe, effective and reproducible technique for correction of moderate to severe hallux valgus deformity with metatarsus primus varus. The use of a locking plate provides enough control of the fragments, enhancing healing of osteotomy and maintenance of the correction even with a violated proximal lateral cortex. The results of this study support the use of the locking wedge plate for correcting moderate to severe hallux valgus deformities with metatarsus primus varus; however, prospective randomized trials are needed to evaluate long-term results.
References
Nikolaou V, Korres D, Xypnitos F, Lazarettos J, Lallos S, Sapkas G, Efstathopoulos N (2009) Fixation of Mitchell’s osteotomy with bioabsorbable pins for the treatment of hallux valgus deformity. Int Orthop 33:701–706
Mann R, Coughlin M (1981) Hallux valgus—etiology, anatomy, treatment and surgical considerations. Clin Orthop Relat Res 157:31–41
Reize P, Schanbacher J, Wulker N (2007) K-wire transfixation or distraction following the Keller-Brandes arthroplasty in hallux rigidus and hallux valgus? Int Orthop 31:325–331
Coughlin M, Mann R (2007) Surgery of the foot and ankle, 8th edn. CV Mosby, St Louis, pp 183–362
Chuchpaiwong B (2012) Comparing proximal and distal metatarsal osteotomy for moderate to severe hallux valgus. Int Orthop 36(11):2275–2278
Jawish R, Assoum H, Saliba E (2010) Opening wedge osteotomy of the first cuneiform for the treatment of hallux valgus. Int Orthop 34:361–368
Mann R, Rudicel S, Graves S (1992) Repair of hallux valgus with a distal soft-tissue procedure and proximal metatarsal osteotomy. J Bone Joint Surg Am 74-A:124–129
Sammarco GJ, Brainard BJ, Sammarco VJ (1983) Bunion correction using proximal chevron osteotomy. Foot Ankle 14:8–14
Park CH, Ahn JY, Kim YM, Lee WC (2013) Plate fixation for proximal chevron osteotomy has greater risk for hallux valgus recurrence than Kirschner wire fixation. Int Orthop 37(6):1085–1092
Barouk LS (2005) Scarf osteotomy for hallux valgus correction. Local anatomy, surgical technique, and combination with other forefoot procedures. Foot Ankle Clin 5:525–558
Fuhrmann R, Zollinger-Kies H, Kundert HP (2010) Mid-term results of scarf osteotomy in hallux valgus. Int Orthop 34:981–989
Nyska M, Trnka HJ, Parks B, Myerson M (2003) The Ludloff metatarsal osteotomy: guidelines for optimal correction based on a geometric analysis conducted on a sawbone model. Foot Ankle Int 24(1):34–39
Mau C, Lauber HJ (1926) Die operative Behandlung des Hallux Valgus. Deutsche Zeit Orthop 197:361–377
Sammarco VJ (2007) Surgical strategies; Mau osteotomy for correction of moderate and severe hallux valgus deformity. Foot Ankle Int 28:857–864
Nigro JS, Geger GM, Catanzariti AR (1991) Closing base wedge osteotomy. J Foot Surg 30(5):494–505
Trethowan J (1923) A system of surgery. PB Hoeber, New York, pp 1046–1049
Mothershed RA (2001) Osteotomies of the first metatarsal base. In: Banks AS, Downey MS, Martin DE, Miller SJ (eds) McGlamry’s comprehensive textbook of foot and ankle surgery. Lippincott Williams & Wilkins, Philadelphia
Budiman-Mak E, Conrad KJ, Roach K (1991) The foot function index: a measure of foot pain and disability. J Clin Epidemiol 4:561–570
Kitaoka H, Alexander I, Adelaar R, Nunley J, Myerson M, Sanders M (1994) Clinical rating systems for the ankle-hindfoot, midfoot, hallux and lesser toes. Foot Ankle Int 15(12):349–353
Richter M, Zech S, Geerling J, Frink M, Knobloch K, Krettek C (2006) A new foot and ankle outcome score: questionnaire based, subjective, visual-analogue-scale, validated and computerized. Foot Ankle Surg 12:191–199
Cooper M, Berlet G, Shurnas P, Lee T (2007) Proximal opening-wedge osteotomy of the first metatarsal for correction of hallux valgus. Surg Technol Int 16:215–219
Amarnek D, Juda E, Oloff L, Jacobs A (1986) Opening base wedge osteotomy of the first metatarsal utilizing rigid external fixation. J Foot Surg 25:321–326
Haddad R (1975) Hallux valgus and metatarsus primus varus treated by bunionectomy and proximal metatarsal osteotomy. South Med J 68(6):684–686
Sollito RJ, Hart TJ, Sergi AR (1991) Opening base wedge osteotomy with first metatarsophalangeal joint implantation arthroplasty—a retrospective study. J Foot Surg 30:165–169
Wanivenhaus AH, Feldner-Busztin H (1988) Basal osteotomy of the first metatarsal for the correction of metatarsus primus varus associated with hallux valgus. Foot Ankle 8:337–343
Shurnas P, Watson T, Crislip T (2009) Proximal first metatarsal opening wedge osteotomy with a low profile plate. Foot Ankle Int 30(9):865–872
Wukich D, Roussel A, Dial D (2009) Correction of metatarsus primus varus with an opening wedge plate: a review of 18 procedures. J Foot Ankle Surg 48(4):420–426
Kumar S, Konan S, Oddy M, Madhav R (2012) Basal medial opening wedge first metatarsal osteotomy stabilized with a low profile wedge plate. Acta Orthop Belg 78:362–368
Randhawa S, Pepper D (2009) Radiographic evaluation of hallux valgus treated with opening wedge osteotomy. Foot Ankle Int 30:427–431
Saragas N (2009) Proximal opening-wedge osteotomy of the first metatarsal for hallux valgus using a low profile plate. Foot Ankle Int 30:976–980
Easley ME, Trnka HJ (2007) Current concepts review: hallux valgus part ii: operative treatment. Foot Ankle Int 28:748–758
Watson T, Shurnas P (2008) The proximal opening wedge osteotomy for the correction of hallux valgus deformity. Tech Foot Ankle Surg 7(1):17–24
Smith W, Hyer C, DeCarbo W, Berlet G, Lee T (2009) Opening wedge osteotomies for correction of hallux valgus. A review of wedge plate fixation. Foot Ankle Spec 2(6):277–282
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Badekas, A., Georgiannos, D., Lampridis, V. et al. Proximal opening wedge metatarsal osteotomy for correction of moderate to severe hallux valgus deformity using a locking plate. International Orthopaedics (SICOT) 37, 1765–1770 (2013). https://doi.org/10.1007/s00264-013-2019-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-013-2019-x