Abstract
Purpose
Osteonecrosis of femoral head remains a major complication of femoral neck fractures. It has been postulated that early internal fixation drastically reduces the incidence of osteonecrosis of the femoral head. However, there is a paucity of literature looking at the effect of time delay to internal fixation on the development of this late complication. In this study, we aim to assess the effect of time delay and method of internal fixation on the development of osteonecrosis in those less than 60 years of age.
Methods
We retrospectively analysed 92 patients less than 60 years of age who presented with intracapsular neck of femur fractures that underwent internal fixation between 1999 and 2009.
Results
Of the 92 intracapsular fractures, 50 underwent fixation using cannulated screws, 32 using a dynamic hip screw, and ten using a dynamic hip screw with a derotation screw. In total, 13 patients (14.1 %) developed osteonecrosis of the femoral head, the highest incidence being in the cannulated screw fixation group with an osteonecrosis rate of 24 %. We did not find the time delay to internal fixation to be a significant predictor of the development of osteonecrosis.
Conclusion
Our study demonstrated that the method of internal fixation rather than delay in internal fixation was more predictive of osteonecrosis of the femoral head. We did not find support to the current belief that early surgical fixation of neck of femur fractures reduces the risk of osteonecrosis in patients less than 60 years.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Fractures of the neck of femur (#NOF) can be described as the current ‘orthopaedic epidemic’ as they constitute the majority of acute admissions to orthopaedic ward [1]. Osteonecrosis of femoral head (ONFH) and non-union are the two most common complications of intracapsular #NOF following internal fixation, but other potential complications include neurovascular compromise in the distal leg, shortening, varus or valgus deformity, post-traumatic osteoarthritis, malrotation deformity, wound infection, and deep vein thrombosis, amongst others [2]. ONFH is usually a late complication after surgical repair of #NOF and thus these patients must be followed up for a considerable period of time to fully ascertain the results of a particular approach.
The usual management of #NOF in elderly patients is hemi-arthroplasty or total hip arthroplasty [3]. Multiple trials and reviews have supported the use of arthroplasty in these situations over internal fixation, as it is associated with improved functional outcomes and a lower rate of re-operation [4, 5]. In contrast, there is much less evidence to support any treatment method in the management of patients under the age of 60 years where these fractures are considerably less common [6, 7]. Since this patient group is younger, it is imperative to retain as much bone as possible; thus, hip replacements are a last resort [8], especially given their increased activity levels [9]. Furthermore, there appears to be an increased incidence of complications after #NOF in this demographic, especially ONFH and non-union are reported to be as high as 45 % and 35 %, respectively [6, 10, 11].
Currently, there are conflicting views in the literature regarding the optimal time to internal fixation. For instance, Jain et al. (2002) concluded that postoperative complications were more prevalent with fixation after 12 h from injury [12], whilst Karaeminogullari et al. (2004) found no association between time to fixation and ONFH [13]. In this study, we aim to address these inconsistencies by analysing the effect of time delay to fixation on ONFH in a hip fracture cohort of patients less than 60 years. We also look at the influence of different methods of internal fixation—cannulated cancellous screw (CS), dynamic hip screw (DHS) or dynamic hip screw with a derotation screw (DHS+DS).
Methods
The databases of two hospitals in Southeast England were used for retrospective analysis. One hundred and seven patients under the age of 60 years presenting with intracapsular #NOF between 1999 and 2009 were identified. Of these, five patients were treated with total hip replacement and three with bipolar hemiarthroplasty. These patients were excluded from the data. No follow-up data was available for seven patients, so these patients were also excluded from the data. Therefore, 92 patients under the age of 60 with #NOF were included.
Mechanisms of injury ranged from high-energy trauma, such as road traffic accidents, falls from significant heights to low-energy injuries, such as mechanical falls (Table 1). Smoking history was noted.
The majority of patients had a pre-fracture ASA score of less than three [14] and mobility score greater than five [15]. Their age ranged from 11 to 59, with a mean of 44.7 (median age, 50 years).
Garden’s classification [16] of #NOF was used to divide patients into undisplaced (Garden I or II) and displaced (Garden III and IV) intracapsular fracture groups; there were 24 and 68 patients, respectively, in the two groups. This is an important distinction when considering frequency of ONFH [1] since displaced fractures pose a greater risk to the vascular supply of the femur [17].
To accurately assess time to fixation, the time of initial injury, time of presentation and time of fixation were all recorded. Time to fixation was then used to further sub-divide patients into the following groups: less than or equal to six h, six–12 h, 12–18 h, 18–24 h, 24–48 h, and more than 48 h (see Table 2).
Ninety-two patients with intracapsular fractures underwent fixation with either dynamic hip screws (DHS), cannulated screws (CS), or dynamic hip screw with a derotation screw (DHS+DS) (Table 1). There were no technical problems reported during any of these procedures. Three patients experienced early postoperative complications, namely, one pulmonary embolism and two superficial wound infections that resolved within the duration of the patient’s hospital stay.
The mean follow-up period was two years, within which the incidence of long-term complications was documented. ONFH was diagnosed both clinically and radiologically. Time to fixation and method of fixation were correlated to the occurrence of ONFH using the Statistical Package for the Social Sciences (SPSS®), and a binary logistic regression model was applied to evaluate the predictive value of the categorical variables of time and method of fixation on ONFH rates.
Results
Of the 92 patients who had intracapsular #NOF, 32 had internal fixation with a dynamic hip screw (DHS), 50 with cannulated screws (CS) and ten patients had DHS+DS (Table 1).
In total, 13 patients (14.1 %) developed ONFH: two with undisplaced fractures (8.3 % of all undisplaced fractures) and 11 with displaced fractures (16.2 % of all displaced fractures).
The incidence ONFH did not rise significantly past the six h mark (Fig. 1), and there was no significant difference in ONFH rates according to time to fixation (p = 0.999).
In contrast, we found that method of fixation was more predictive of ONFH risk. More specifically, 24 % of all patients undergoing cannulated screw fixation developed ONFH, compared with 3 % of all patients undergoing DHS and 0 % undergoing DHS+DS (p = 0.012) (Table 3).
When analysing the rates of ONFH according to both the Gardner classification and type of fixation, we found that there was no significant difference in the development of ONFH according to the method of fixation for undisplaced #NOF (Gardner I and II) (Table 4). However, we did find a significantly higher rate of ONFH in the CS group for displaced fracture (29.4 %) compared to both DHS or DHS+DS (4 % and 0 % respectively) (p = 0.012).
Discussion
Osteonecrosis of the head of the femur (ONFH) is a serious and unpredictable complication which can occur after displaced intracapsular #NOF due to disturbed blood supply of the femoral head. It is also thought that ONFH is more likely to occur in #NOF with delayed time to surgical fixation. Its incidence in patients less than 60 years is noted to vary from 16 % to 86 % [6, 10, 11, 18, 19]. Younger patients have a higher prevalence of femoral head osteonecrosis and non-union [11, 19]. It is imperative to anticipate the occurrence of ONFH as it can lead to femoral head collapse and osteoarthritis which often necessitates further surgeries.
The femoral head has an inherently vulnerable blood supply due to its natural course [2]. It is fed by a variety of vessels, mainly branches of the medial and lateral femoral circumflex arteries that branch off the femoral profunda artery that is in turn fed by the common femoral artery. These circumflex arteries encircle the femoral head in the trochanteric area and branch off into retinacular vessels that pass proximally toward the head in three segments: small anterior, posteroinferior and posterosuperior retinacular arteries. Additionally, the round ligament of the femur carries arterial supply to the anterosuperior femoral head distally from the acetabular branch of the obturator artery [20]. Lastly, the medullary cavity carries nutrient vessels constituting another arterial blood supply to the femoral head. Although numerous, this arterial supply to the femoral head is intrinsically precarious, thus leaving this area susceptible to vascular compromise in the face of trauma. More specifically, the terminal arteries are intracapsular and can be easily disturbed with #NOF, their manipulation and changes in intracapsular pressure [21].
It is widely accepted that anatomical reduction and stable internal fixation of #NOF reduces the risk of ONFH and is therefore the goal of therapy. However, there is paucity of evidence-based literature indicating the most favourable time to fixation that minimizes ONFH rates post-fixation. Therefore, there are numerous alternative management algorithms which have been published for use internationally [8, 22, 23]. Each of these algorithms holds subtle differences, but consider similar factors when determining type of fixation, including patient age (both chronological and physiological bone age), activity levels, comorbidities and fracture patterns. For instance, Kuner et al. (1995) reported a significant advantage in fracture outcome with intervention within 24 h of injury [24], whilst Braun et al. (1991) went a step further and demonstrated that operating within six h improved functional outcome and ONFH rates [18].
In light of these different approaches to the management of #NOF, our multi-centred study endeavours to assess the evidence behind prompt surgical fixation. We retrospectively analysed patients’ outcomes from #NOF sustained in a variety of incidents ranging from low to high energy trauma. These patients had either DHS, CS or both fixations inserted at varying time points post-injury.
Time to fixation
Analysing ONFH occurrence in our 92 patients, we could not identify a significant pattern between increasing time to fixation and ONFH rates, and hence was not a valid predictor of ONFH following internal fixation. This inconsistency across the various time groups is illustrated in Fig. 1, and in our study no linear relationship was found between ONFH rate and increasing time to fixation.
In support of this finding, Karaeminogullari et al. (2004) had similar results when studying ONFH and non-union rates in patients whose fractures were fixed before or after the 12 h mark from injury [13]. Before 12 h, ONFH and non-union rates were 12.5 % and 25 %, versus 14 % and 27 % after 12 h (not statistically significant). In addition, Haidukewych et al. (2004) found no difference in osteonecrosis rates for surgical intervention before and after 24 h (25 % and 20 % respectively) [10]. Upadhyay et al. (2004) also found no discrepancy in ONFH or mal-union rates in patients even after 48 h [19], further endorsing our findings.
Method of fixation
Stability of surgical fixation and quality of union are two major predictors of ONFH. Current literature demonstrates the controversy over optimum fixation method regarding #NOF of young adults. For instance, Zhou et al. (2007) demonstrated that cannulated screws reduced the risk of ONFH as well as improved fracture union rates [25]. Ly and Swiontkowski (2009) favoured three cannulated screws as definite treatment; however, they also raise the issue of capsulotomy and its role in these types of fractures [26]. On the other hand, Kuner et al. (1995) showed that DHS devices promised the best outcomes [24].
Detailed analysis of our data revealed that type of fixation may in fact play a vital role in rates of ONFH. Internal fixation with DHS had an ONFH rate of 3 %. This is in contrast to CS which had an ONFH rate of 24 %. Thus, in support of Kuner et al. (1995), our study found DHS to be a superior method of fixation to CS [24].
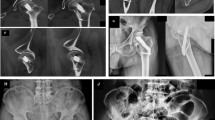
Our results suggest that management with DHS alone, or in combination with derotation screw, is associated with significantly lower rates of ONFH in those under 60 years of age compared to CS fixation, regardless of time to fixation. Figure 2 shows a clear tendency for ONFH to develop in patients with displaced #NOF treated by CS. The significantly lower ONFH risk seen with DHS and DHS+DS in our study provides strong support for the use of DHS or DHS+DS over other methods of fixation in the management of displaced #NOF in young patients. We did not find that the method of fixation for undisplaced #NOF had any significant influence on ONFH rates.
In further support of our data, Bonnaire and Weber (2002) as well as Baitner et al. (1999) have shown that DHS with derotation screw fixation gives superior stabilisation of #NOF which ultimately reduces ONFH rates, based on biomechanical study of cadaveric femurs with basicervical fractures [27, 28]. Furthermore, Chen et al. (2008) and Hrubina et al (2010) have shown similar promising results with DHS fixation in basicervical and pertrochanteric #NOF [29, 30].
Limitations
Our study has several limitations. First, despite the large period of data analysis (ten years), only 92 patients were included in data analysis. It was a retrospective study that relied on outpatient clinic follow up; no follow-up data was available for seven patients (and hence these were not included in the study). In relation to the method of fixation, there was not enough information available from data collection to provide reference to the type of DHS (e.g. amount of holes, angle) or number of cannulated screws used. Nor was there enough to comment on intraoperative placement of prosthesis (e.g. technical success of placement of DHS / CS) and whether this had any implication on osteonecrosis rates.
Conclusion
Our study suggests time to internal fixation of intracapsular #NOF is less important in the prevention of ONFH than was initially thought. Patients treated more than 48 h post-fracture showed no increased incidence of ONFH.
Internal fixation of displaced #NOF using cannulated screws was found to be associated with a significantly increased incidence of ONFH compared with DHS and DHS+DS. Our results suggest that the use of DHS or DHS+DS in stabilising displaced intracapsular #NOF is a safe and effective method in patients less than 60 years.
References
Wood PR, Mahoney PF, Cooper J (2009) Trauma and orthopedic surgery in clinical practice. 1st edition. [online] Springer. Available from: http://www.jbjs.org.uk/media/22213/focuson_intracapsular.pdf. Accessed 5 Feb 2011
Kregor PJ (1996) The effect of femoral neck fractures on femoral blood flow. Orthopedics 19(12):1031–1036
Kannan A, Kancherla R, McMahon S, Hawdon G, Soral A, Malhotra R (2012) Arthroplasty options in femoral-neck fracture: answers from the national registries. Int Orthop 36(1):1–8
Lu-yao GL, Keller RB, Littenberg B, Wennberg JE (1994) Outcomes after displaced fractures of the femoral neck: a meta-analysis of one hundred and six published reports. J Bone Joint Surg Am 76-A:15–25
Parker MJ, Gurusamy K (2006) Internal fixation versus arthroplasty for intracapsular proximal femoral fractures in adults. Cochrane Database Syst Rev (4):CD001708
Protzman RR, Burkhalter WE (1976) Femoral neck fractures in young adults. J Bone Joint Surg Am 58:689–695
Robinson CM, Court-Brown CM, McQueen MM, Christie J (1995) Hip fractures in adults younger than 50 years of age. Epidemiology and results. Clin Orthop Relat Res 312:238–246
Cuckler JM, Tamarapalli JR (1994) An algorithm for the management of femoral neck fractures. Orthopedics 17(9):789–792
Chandler HP, Reineck FT, Wixson RL, McCarthy JC (1981) Total hip replacement in patients younger than thirty years old. A five-year follow-up study. J Bone Joint Surg Am 63:1426–1434
Haidukewych GJ, Rothwell WS, Jacofsky DJ, Torchia ME, Berry DJ (2004) Operative treatment of femoral neck fractures in patients between the ages of fifteen and fifty years. J Bone Joint Surg Am 86:1711–1716
Swiontkowski MF, Winquist RA, Hansen ST (1984) Fractures of the femoral neck in patients between the ages of twelve and forty-nine years. J Bone Joint Surg Am 66:837–846
Jain R, Koo M, Kreder HJ, Schemitsch EH, Davey JR, Mahomed NN (2002) Comparison of early and delayed fixation of subcapital hip fractures in patients sixty years of age or less. J Bone Joint Surg Am 84:1605–1612
Karaeminogullari O, Demirors H, Atabek M, Tuncay C, Tandogan R, Ozalay M (2004) Avascular necrosis and non-union after osteosynthesis of femoral neck fractures: effect of fracture displacement and time to surgery. Adv Ther 21(5):335–342
Muller ME, Nazarian S, Koch P, Schatzker J (1994) The AO classification of long bone fractures, first edn. Springer, Berlin, American Society of Anaesthesiologists. New classification of physical status. Anaesthesiology 1963;24:111
Parker MJ, Palmer CR (1993) A new mobility score for predicting mortality after hip fracture. J Bone Joint Surg Br 75-B:797–798
Garden RS (1964) Stability and union in subcapital fractures of the femur. J Bone Joint Surg Br 46-B:630–647
Mao YJ, Wei J, Zhou L, Wang MY, Su JG (2005) Related factor analysis of avascular necrosis of the femoral head after internal fixation with cannulated screws in femoral neck fractures. Zhonghua Yi Xue Za Zhi 85(46):3256–3259
Braun W, Rüter A, Wiedemann M, Kissing F (1991) Femoral head preserving therapy in medial femoral neck fractures. A clinical study of the effects of treatment method on the outcome. Unfallchirurg 94(6):325–330
Upadhyaya A, Jain P, Mishra P, Maini L, Gautum VK, Dhaon BK (2004) Delayed internal fixation of fractures of the neck of femur in young adults. A prospective, randomised study comparing closed and open reduction. J Bone Joint Surg 86(7):1035–1040
Howe WW Jr, Lacey T, Schwartz RP (1950) A study of the gross anatomy fo the femoral head in adult man. J Bone Joint Surg Br 32:856–866
Arnoldi CC, Linderholm H (1977) Fracture of the femoral neck. II. Relative importance of primary vasculature damage and surgical procedure for the development of necrosis of the femoral head. Clin Orthop Relat Res 129:217–222
Bhandari M, Devereaux PJ, Tornetta P 3rd et al (2005) Operative management of displaced fractures in elderly patients. An international survey. J Bone Joint Surg Am 87:2122–2130
Shah A, Eissler J, Radomisli T (2002) Algorithms for the treatment of femoral neck fractures. Clin Orthop Relat Res 399:28–34
Kuner EH, Lorz W, Bonnaire F (1995) Femoral neck fractures in adults: joint sparing operations. I. Results of an AO collective study with 328 patients. Unfallchirurg 98(5):251–258
Zhou L, Tan J, Xu B (2007) Treatment of femoral neck fracture with cannulated screw fixation in young adults. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi 21(3):275–277
Ly TV, Swiontkowski MF (2009) Treatment of femoral neck fractures in young adults. Instr Course Lect 58:69–81
Bonnaire FA, Weber AT (2003) Analysis of fracture gap changes, dynamic and static stability of different osteosynthetic procedures in the femoral neck. Injury 33(Suppl 3):C24–C32
Baitner AC, Maurer SG, Hickey DG, Jazrawi LM, Kummer FJ, Jamal J, Goldman S, Koval KJ (1999) Vertical shear fractures of the femoral. A biomechanical study. Clin Orthop Relat Res 367:300–305
Chen CY, Chiu FY, Chen CM, Huang CK, Chen WM, Chen TH (2008) Surgical treatment of basicervical fractures of femur—a prospective evaluation of 269 patients. J Trauma 64(2):427–429
Hrubina M, Skoták M, Běhounek J (2010) Complications of dynamic hip screw treatment for proximal femoral fractures. Acta Chir Orthop Traumatol Cech 77(5):395–401
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Razik, F., Alexopoulos, AS., El-Osta, B. et al. Time to internal fixation of femoral neck fractures in patients under sixty years—does this matter in the development of osteonecrosis of femoral head?. International Orthopaedics (SICOT) 36, 2127–2132 (2012). https://doi.org/10.1007/s00264-012-1619-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-012-1619-1