Abstract
Purpose
The aim of this study was to compare the results of a new technique for low, multidirectional locked nailing with closed reduction and minimally invasive plating in the treatment of distal tibial metadiaphyseal fractures.
Methods
Forty-six matched patients were divided according to age, gender, Injury Severity Score, and fracture pattern into group A (expert tibial nailing) and group B (minimally invasive plating). Then, the patients were followed up, and the clinical and radiographic results were retrospectively analysed.
Results
The mean followed-up was 24.7 ± 2.7 months in group A and 25.8 ± 2.8 months in group B. No patient had nonunion, shortening, hardware breakdown, or deep-seated infection. Patients in group A had a significantly shorter mean operating time, hospital stay, full weight-bearing time and union time (76 ± 16.6 vs. 90 ± 20.3 minutes, p = 0.000; 5.8 ± 2.1 vs. 8.9 ± 3.1 days, p = 0.000; 9.0 ± 1.4 vs. 11.1 ± 1.7 weeks, p = 0.000; and 21.3 ± 3.5 vs. 23.1 ± 3.6 weeks, p = 0.047, respectively). Three patients in group A and one patient in group B presented with malalignment (p = 0.608). The mean Olerud-Molander Ankle score was 89.0 ± 7.1 in group A and 87.6 ± 8.4 in group B (p = 0.478).
Conclusions
Distal tibia metadiaphyseal fractures may be treated successfully with low, multidirectional locked nails or plates. However, low, multidirectional locked nailing may represent a superior surgical option, since it offers advantages in terms of mean operating time, hospital stay, full weight-bearing time and union time.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Distal tibial metadiaphyseal fractures are a common consequence of road traffic accidents, falling injuries and other high-energy trauma and usually involve a severe soft-tissue injury. These fractures generally require surgical management, such as reduction and internal or external fixation. Surgical treatment for distal tibial metadiaphyseal fractures is still a challenge because extensive soft-tissue injuries often disrupt the vascular supply to the fracture site and increase the risk of infection and delayed union or nonunion [1]. A variety of treatments may be used, including intramedullary (IM) nailing, plating and external fixation [2–7]. However, surgical treatment for distal tibial metadiaphyseal fractures remains controversial. Which internal fixation method should be chosen and which is better: intramedullary (IM) nailing or plating? We hypothesized that superior results may be achieved when distal tibial metadiaphyseal fractures are treated with intramedullary (IM) nails. This approach protects the soft tissue that envelops the fracture site.
In the past, plate fixation achieved an acceptable degree of reduction and rigid fixation. The technique was used widely, but it usually required relatively extensive wound exposure and soft-tissue dissection. These factors increase the risk of infection and nonunion, especially for fractures with a severe soft-tissue injury or open fractures. In recent years, closed reduction and minimally invasive plating have provided superior options for treating these fractures. At the same time, locked intramedullary nailing has been widely accepted as a satisfactory treatment of tibial fracture. However, in patients with distal tibial fractures, there is a risk that the fracture will propagate into the ankle or that the nail will fail because of inadequate fixation of the small distal fragment [8]. The construction of IM nails has improved greatly. The indications for their use have been extended to fractures closer to distal segments [9–11]. In recent years, shortened IM nailing, in which the distal tip of a standard IM tibial nail is cut by 1 cm, has been developed and used to treat distal tibial fractures [12–14]. The Expert Tibial Nail (ETN, Synthes) is a new kind of low, multidirectional locked tibial intramedullary nail; its interlocking system (Fig. 1) was developed to attain increased angular stability and to enhance the axial and lateral stability of fracture fragments. Because of the increased stability attained by the nail fixing of proximal or distal tibial fractures, the indications for use of the nail were expanded. The nail currently represents an effective approach to the treatment of complex tibial fractures such as distal tibial metadiaphyseal fractures [15]. In this control-matched study, we compared the two surgical procedures—nailing and plating—in the treatment of distal tibial metadiaphyseal fractures.
Patients and methods
This study was undertaken at the Department of Orthopaedic Surgery at West China Hospital, Sichuan University. It was approved by the research administration departments and ethical committees of West China Hospital, Sichuan University.
The criteria for inclusion in this study were (1) distal tibial metadiaphyseal fractures, (2) closed or Gustilo grade-I or grade-II open fractures, (3) skeletally mature adult patients and (4) early failure of conservative treatment. Patients with earlier fractures of distal metadiaphyseal tibia on the same side, proximal intra-articular or distal intra-articular fractures or pathological fractures of the tibia were excluded.
Using the database and the medical records (between September 2007 and October 2009), 23 patients treated with low, multidirectional locked nailing (Expert Tibial Nail, Synthes) were matched to 23 patients treated with closed reduction and minimally invasive plating on the basis of gender, age (±3 years), Injury Severity Score, and fracture pattern (AO classification). These patients were treated with the new low, multidirectional locking nails (group A) or locking compression plates (group B). Trauma radiographs were used to determine the location and AO classification of the fractures in the patients selected.
Fibula fractures were fixed if the ankle joint was affected. In group A, all patients were managed with closed nailing, and the nail was inserted after reaming if necessary. The static locking mode was used in all patients; at least two proximal and three distal locking screws were implanted. In the closed reduction and minimally invasive plating group (group B), all 23 patients were treated with the anatomically contoured locking compression plates (LCP) and screws. All operations were performed by a senior attending surgeon with the assistance of residents. In general, patients were followed up for two weeks after the operation and every four to six weeks thereafter.
In both groups, cefazolin 2000 mg was used as a prophylactic antibiotic 30 minutes before the operation and once postoperatively. The patient was encouraged to perform ankle range-of-motion exercises after the operation. Partial weight bearing on the affected leg was permitted after three weeks. Patients were followed-up clinically and radiographically at six-week intervals until bony union was achieved. Union was defined clinically as the ability to walk without aid or pain, and radiographically showing a solid bridging callus or obliteration of the fracture line. Delayed union was defined as a lack of radiographic union by week 24. Radiological assessment was performed using anteroposterior and lateral views. We recorded the degree of postoperative angulation at the fracture site; malunion was defined as more than 5° of angular deformity in any plane or as shortening by 1 cm or more in length. In addition, functional results were scored using the Olerud-Molander Ankle Score (OMAS) [16]. An OMAS score of more than 91 points was considered excellent; 61–90 points, good; 31–60 points, fair; and less than 30, poor. Removal of the hardware was suggested at one year after radiological and clinical union in all patients. Twenty-one patients in group A and 19 patients in group B underwent an implant removal before the final follow-up.
Statistical analysis
The two groups were compared with respect to age, sex, AO fracture type, classification of open fractures (Gustilo-Anderson classification) [17], operating time, bony union time, incidence of wound complications, angulation of the fracture, and the Olerud-Molander ankle score. An independent statistician, who was not directly involved with the study, performed the statistical analysis. The parameters were compared between groups. A paired-sample t test was used for the interval data (age, operating time, length of hospital stay, weeks to full weight-bearing, bony union time, and postoperative angulation). The Fisher two-sided exact test was used to compare rates of infection, malalignment, anterior knee pain and functional outcome. The statistical analysis was performed using the Statistical Package for Social Science (SPSS version 16.0; SPSS). The chosen level of significance was p < 0.05.
Results
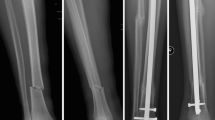
The pre-operative characteristics of both groups are shown in Table 1. Thirty-four patients had associated fibular fractures, and 30 patients had been fixed because of the involvement of the ankle joint. In these 30 patients, fibular fractures were first reduced and fixed with the plate and screws. In the nailing group, two patients with open injury were treated by external fixation, which was performed as part of an emergency operation. Internal fixation was performed after the external fixations were removed. In the plate-fixation group, three patients were treated with plate fixation after the external fixation had been removed. All fractures in both the nailing group and in the closed reduction and minimally invasive plating group healed without the need for secondary procedures. Figure 2 shows a patient treated using the new intramedullary nail system, while Fig. 3 presents a patient treated using a system comprising a locked plate and screws.
Table 2 summarizes the follow-up data for both groups. The mean postoperative angulation in the coronal plane (varus/valgus) was 2.4 ± 2.2 (range, 0–9°) in group A and 2.0 ± 1.6 (range, 0 –6°) in group B (p = 0.480, group A vs. group B). In the sagittal plane, the mean extent of postoperative ante-/recurvatum was 1.7 ± 1.6 (range, 0 –7) in group A and 1.4 ± 1.3 (range, 0– 4) in group B (p = 0.383, group A vs. group B). Table 2 also shows the functional results evaluated according to the OMAS in both groups. In the analysis with the Fisher two-sided exact test, no significant difference was found between the groups. However, five patients in group A reported occasional anterior knee pain and discomfort on kneeling, and two patients did not experience complete relief of their symptoms after the removal of the nail. Only one patient complained of anterior knee pain in group B. The pain disappeared upon the administration of Celecoxib 200 mg/day for three weeks.
Discussion
All patients in both groups regained full weight-bearing capacity and returned to normal domestic activities. The new low, multidirectional locked nail technique demonstrated showed advantages in terms of the operation time, hospital stay, early full weight-bearing and bony union.
In recent years, the indications for use of the intramedullary nail system were expanded to include the treatment of a wide spectrum of tibial fractures [9, 18]. This new low, multidirectional locked intramedullary system involves multiple locking options in different planes at the proximal and distal ends. The system has an angular stability locking system that enhances the axial and lateral stability of the fracture fragments [19]. Because of this modified design, the new system has advantages over the traditional tibial intramedullary nail in dealing with both proximal and distal tibial fractures. A biomechanical study showed that the addition of two proximal oblique screws (Fig. 1) significantly enhanced the stability of the intramedullary fixation construct compared with the original approach to fixation, which involved the use of two transverse screws fixation (Fig. 1). In terms of varus–valgus and flexion–extension, the appendage of oblique screws increased the angular stability [20]. In addition, there are four advanced distal locking options in this new tibial intramedullary nail (Fig. 1). The set-up involved one oblique locking option placed very distally, which allowed for optimized bone purchase and prevented damage to the soft tissue, as well as two mediolateral (ML) locking options and one anteroposterior (AP) locking option for better stabilization of the distal fragment. These design modifications ensure that angular stability is retained and angle-stable locking reflects a potential to maintain fixation stability of distal tibia fractures [20]. All of these design modifications allow for better fixation of metaphyseal tibial segments through multiple interlocking holes in close proximity to either end of the nail. The use of multidirectional interlocking screws ensures that alignment can be maintained and that stability can be preserved despite a short proximal or distal tibial segment. The present study showed similar results for the mean degree of postoperative angulation in both groups (p = 0.480 in the coronal plane and p = 0.383 in the sagittal plane). In a comparison of the incidence of malunion (>5°), no statistically significant difference was found between the groups. This finding may indicate that most angulations with this new intramedullary nail were acceptable and that they had a significant advantage in maintaining alignment compared with traditional intramedullary nails [2].
Delayed union and nonunions are important issues in the clinical treatment of tibial fractures. In the literature, the rate of delayed unions among tibial fractures treated with intramedullary nails ranges from 0 to 11% for closed fractures and from 9% to 47% for open fractures. Published reports show that non-union occurs in 0% to 8% of the closed fractures and 3% to 17% of the open fractures [21–24]. In recent years, intramedullary nailing has become widely accepted as the operative treatment of choice for distal tibial diaphyseal fractures [25, 26]. Tyllianakis et al. reviewed 73 patients with distal tibial fractures treated with reamed nailing and reported union in 96% of the patients. In the present study, there were no nonunions, malunions or hardware failures, and all patients achieved satisfactory or excellent results. The fixation of distal tibial fractures with this new nail system or anatomically contoured locking compression plate in association with use of the Minimally Invasive Plate Osteosynthesis (MIPO) technique is associated with high union rates and offers a significant benefit in protecting the soft tissue enveloping the fracture site. Therefore, as a result of using closed reduction and MIPO technique, although 17 open fractures were included in the present study, only one patient in the nailing group and three patients in the plating group exhibited a superficial infection. However, in a related prospective, randomized clinical trial (64 patients), a superficial infection was observed in patients treated with closed intramedullary nailing as well as in those treated with open reduction internal fixation (one patient vs. six patients, p = 0.03) [4].
Weight-bearing exercise is essential for building and maintaining healthy bones. In the present study, when patients begin weight-bearing activities, fracture pattern, fracture localization, the condition of the soft tissue and the quality of the bone should be taken into account. Partial weight bearing (sole contact or up to 15 kg) is the primary way in which the fractured leg is loaded. The increase in load is determined according to the fracture pattern and localization, the condition of the soft tissue, bone quality as well as the absence or presence of load-induced pain.
A greater number of days in the hospital imposes higher healthcare costs and economic burdens to society. In the present study, patients in group A had a significantly shorter length of hospital stay compared with those in group B (p < 0.05), which would result in reduced healthcare costs. Patients in both groups have achieved satisfactory functional results. Notably, anterior knee pain after nailing the tibia should not be ignored. The occurrence of anterior knee pain is frequently associated with tibial intramedullary nailing with an incidence reported to be between 32% and 57% [27–30]. In the present study, five patients experienced some degree of chronic knee pain. More patients in the group treated with nailing had difficulty kneeling, but only one patient in the plate-fixation group experienced these symptoms. Dogra, Ruiz, and Marsh reviewed 83 patients with isolated fractures of the tibial diaphysis treated primarily with closed, reamed intramedullary nailing. Twenty-nine patients experienced pain around the knee when resting. The cause of this symptom is still unclear. Some authors suggested contributing factors including an increased level of activity, nail prominence above the proximal tibial cortex, a meniscal tear, an unrecognized articular injury, increased contact pressure at the patellofemoral articulation, damage to the infrapatellar nerve, and surgically induced scar formation. Knee pain is often an indication for nail removal, but evidence suggests that this is not always beneficial [31].
The control-matched design of this study has certain limitations. Selection bias was not avoided, as the surgeon decided which operative treatment to perform. Some of the bias was eliminated by matching the patients. To maintain a sufficient number of patients, matching considered only gender, age, AO classification, and Injury Severity Score.
Although this study is limited by the number of patients and the retrospective design, our results suggest that both treatment methods can achieve satisfactory functional outcomes in patients with distal tibial metadiaphyseal fractures. Low, multidirectional locked nailing may be considered a better surgical option as it offers advantages in terms of mean operating time, hospital stay, full weight-bearing time and union time.
References
Blick SS, Brumback RJ, Lakatos R et al (1989) Early bone grafting of high-energy tibial fractures. Clin Orthop Relat Res 240:21–41
Newman SD, Mauffrey CP, Krikler S (2010) Distal metadiaphyseal tibial fractures. Injury 41(7):693–702
Jukka R, Flinkkilä T, Pekka H (2007) Two-ring hybrid external fixation of distal tibial fractures: A review of 47 cases. J Trauma 62(1):174–183
Im GI, Tae SK (2005) Distal metaphyseal fractures of tibia: a prospective randomized trial of closed reduction and intramedullary nail versus open reduction and plate and screws fixation. J Trauma 59(5):1219–1223
Zelle BA, Bhandari M, Espiritu M et al (2006) Treatment of distal tibia fractures without articular involvement: a systematic review of 1125 fractures. J Orthop Trauma 20(1):76–79
Ronga M, Shanmugam C, Longo UG et al (2009) Minimally invasive osteosynthesis of distal tibial fractures using locking plates. Orthop Clin North Am 40(4):499–504
Bedi A, Le TT, Karunakar MA (2006) Surgical treatment of nonarticular distal tibia fractures. J Am Acad Orthop Surg 14(7):406–416
Trafton PG (1992) Tibial shaft fracture. In: Browner BD, Jupiter JB, Levine AM, Trafton PG (eds) Skeletal trauma. W.B. Saunders, Philadelphia, pp 1771–1871
Nork SE, Barei DP, Schildhauer TA et al (2006) Intramedullary nailing of proximal quarter tibial fractures. J Orthop Trauma 20(8):523–528
Megas P, Zouboulis P, Papadopoulos AX, Karageorgos A, Lambiris E (2003) Distal tibial fractures and non-unions treated with shortened intramedullary nail. Int Orthop 27(6):348–351
Nork SE, Schwartz AK, Agel J et al (2005) Intramedullary nailing of distal metaphyseal tibial fractures. J Bone Joint Surg Am 87(6):1213–1221
Yang S-W, Tzeng H-M, Chou Yi-Jiun et al (2006) Treatment of distal tibial metaphyseal fractures: Plating versus shortened intramedullary nailing. Injury 37(6):531–535
Dogra AS, Ruiz AL, Thompson NS et al (2000) Dia-metaphyseal distal tibial fractures: treatment with a shortened intramedullary nail: a review of 15 cases. Injury 31:799–804
Gorczyca JT, McKale J, Pugh K et al (2002) Modified tibial nails for treating distal tibia fractures. J Orthop Trauma 16:18–22
Hansen M, El Attal R, Blum J et al (2009) Intramedullary nailing of the tibia with the expert tibia nail. Oper Orthop Traumatol 21(6):620–635
Olerud C, Molander H (1984) A scoring scale for symptom evaluation after ankle fracture. Arch Orthop Trauma Surg 103:190–194
Gustilo RB, Anderson JT (1976) The prevention of infection in treatment of 1000 and 25 open fractures of long bones—retrospective and prospective analysis. J Bone Joint Surg Am 58(4):453–458
Kuhn S, Hansen M, Rommers PM (2008) Extending the indication of intra medullary nailing of tibial fractures. Eur J Trauma Emerg Surg 75(2):77–87
Ibrahimi AE, Shimi M, Daoudi A et al (2009) Intramedullary nailing in the management of distal tibial fractures. Current Orthopaedic Practice 20(3):300–303
Gueorguiev B, Ockert B, Schwieger K, Wahnert D, Lawson-Smith M, Windolf M, Stoffel K (2011) Angular stability potentially permits fewer locking screws compared with conventional locking in intramedullary nailed distal tibia fractures: a biomechanical study. J Orthop Trauma 25(6):340–346
Bonatus T, Olson SA, Lee S et al (1997) Nonreamed locking intramedullary nailing for open fractures of the tibia. Clin Orthop Relat Res 339:58–64
Gaebler C, Stanzl-Tschegg S, Heinze G et al (1999) Fatigue strength of locking screws and prototypes used in small-diameter tibial nails: a biomechanical study. J Trauma 47:379–384
Singer RW, Kellam JF (1995) Open tibial diaphyseal fractures. Results of unreamed locked intramedullary nailing. Clin Orthop Relat Res 315:114–118
Wiss DA, Stetson WB (1995) Unstable fractures of the tibia treated with a reamed intramedullary interlocking nail. Clin Orthop Relat Res 315:56–63
Busse JW, Morton E, Lacchetti C et al (2008) Current management of tibial shaft fractures: a survey of 450 Canadian orthopedic trauma surgeons. Acta Orthop 79(5):689–694
Kakar S, Tornetta P 3rd (2007) Open fractures of the tibia treated by immediate intramedullary tibial nail insertion without reaming: a prospective study. J Orthop Trauma 21(3):153–157
Young H, Topliss C (2007) Complications associated with the use of a titanium tibial nail. Injury 38:223–226
Court-Brown CM, Christie J, McQueen MM (1990) Closed intramedullary tibial nailing. Its use in closed and type I open fractures. J Bone Joint Surg Br 72(4):605–611
Keating JF, O’Brien PI, Blachut PA et al (1997) Reamed interlocking intramedullary nailing of open fractures of the tibia. Clin Orthop 338:182–191
Gaebler C, Berger U, Schandelmaier P et al (2001) Rates and odds ratios for complications in closed and open tibial fractures treated with unreamed, small diameter tibial nails: a multicenter analysis of 467 cases. J Object Technol 15:415–423
Boerger TO, Patel G, Murphy JP (1999) Is routine removal of intramedullary nails justified? Injury 30:79–81
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Li, Y., Liu, L., Tang, X. et al. Comparison of low, multidirectional locked nailing and plating in the treatment of distal tibial metadiaphyseal fractures. International Orthopaedics (SICOT) 36, 1457–1462 (2012). https://doi.org/10.1007/s00264-012-1494-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-012-1494-9