Abstract
Clinical tumor remissions after adoptive T-cell therapy are frequently not durable due to limited survival and homing of transfused tumor-reactive T cells, what can be mainly attributed to the long-term culture necessary for in vitro expansion. Here, we introduce an approach allowing the reliable in vitro generation of leukemia-reactive cytotoxic T lymphocytes (CTLs) from naive CD8+ T cells of healthy donors, leading to high cell numbers within a relatively short culture period. The protocol includes the stimulation of purified CD45RA+ CD8+ T cells with primary acute myeloid leukemia blasts of patient origin in HLA-class I-matched allogeneic mixed lymphocyte-leukemia cultures. The procedure allowed the isolation of a large diversity of HLA-A/-B/-C-restricted leukemia-reactive CTL clones and oligoclonal lines. CTLs showed reactivity to either leukemia blasts exclusively, or to leukemia blasts as well as patient-derived B lymphoblastoid-cell lines (LCLs). In contrast, LCLs of donor origin were not lysed. This reactivity pattern suggested that CTLs recognized leukemia-associated antigens or hematopoietic minor histocompatibility antigens. Consistent with this hypothesis, most CTLs did not react with patient-derived fibroblasts. The efficiency of the protocol could be further increased by addition of interleukin-21 during primary in vitro stimulation. Most importantly, leukemia-reactive CTLs retained the expression of early T-cell differentiation markers CD27, CD28, CD62L and CD127 for several weeks during culture. The effective in vitro expansion of leukemia-reactive CD8+ CTLs from naive CD45RA+ precursors of healthy donors can accelerate the molecular definition of candidate leukemia antigens and might be of potential use for the development of adoptive CTL therapy in leukemia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In leukemia patients the curative immune response after allogeneic hematopoietic stem-cell transplantation (HSCT) and donor lymphocyte infusion (DLI) mainly relies on leukemia-eliminating T cells that develop from adoptively transferred donor peripheral blood mononuclear cells (PBMCs) in vivo [1, 2]. Although this graft-versus-leukemia (GvL) effect is impressive and a frequently observed clinical event, it is strongly associated with unwanted and often deleterious graft-versus-host (GvH) reactivity against non-hematopoietic recipient tissues [3]. Current strategies to separate the GvL from GvH effects include the adoptive transfer of leukemia-reactive T-cell lines and clones isolated from PBMCs of healthy donors by primary in vitro stimulation [4]. Unfortunately, the precursor frequency of leukemia-reactive T cells is very low in healthy individuals. Amplifying these cells to numbers sufficient for adoptive immunotherapy still requires extensive in vitro expansion over several weeks. However, long-term culture of antigen-specific T cells is accompanied by terminal differentiation and functional exhaustion due to replicative senescence. There is strong evidence from animal models and clinical studies that T cells with such a late-stage phenotype fail to persist upon adoptive transfer in vivo [5–7].
Considering the fundamental limitations of long-term cultured T-cell populations, we proposed to set-up a novel in vitro protocol allowing the reliable production of leukemia-reactive CD8+ T cells with an early differentiation phenotype during a preferably short culture period. As a source of T cells, we chose CD45RA+ naive precursors from healthy donors because of their superior capability to maintain cell division function compared to memory and effector T cells [8]. We stimulated these naive CD8+ T cells with HLA-class I-matched primary acute myeloid leukemia (AML) blasts using an allogeneic mini-mixed lymphocyte-leukemia culture (mini-MLLC) approach [9]. The protocol includes IL-12 to facilitate priming of naive T cells against leukemia antigens and to substitute Th1 help. While IL-12 is replaced on day 14 of culture by IL-2, the homeostatic proliferation cytokines IL-7 and IL-15 are used throughout the culture. In the current study, we have added the common gamma chain receptor cytokine IL-21 to this protocol because it appears to promote the development of antigen-specific T cells predominantly from naive T cells [10]. We demonstrate herein in eight different AML patient/donor pairs that naive CD45RA+ CD8+ T cells of healthy donors regularly contained numerous precursors of cytolytic T lymphocyte (CTL) clones recognizing primary AML blasts in association with various HLA-A/-B/-C alleles. The addition of IL-21 to the protocol substantially increased the efficacy in generating these CTLs in vitro. CTLs not only showed strong interferon-γ (IFN-γ) secretion and cytolytic activity, but also maintained a robust growth pattern and the expression of early T-cell differentiation markers for several weeks.
Materials and methods
Donors and patients
The study was approved by the local ethics committee. Informed consent was obtained from participants in accordance with the Declaration of Helsinki. Patients were diagnosed with M1 (MZ529), M4 (MZ169, MZ580, MZ728, MZ987), and M5 (MZ201, MZ653) subtype AML according to the French-American-British Cooperative Group (FAB) classification. All patients except two (MZ169, M728) had white blood cell count exceeding 105 per μL at primary diagnosis, consistent with unfavorable disease prognosis [11]. Further adverse prognostic factors were refractory leukemia after induction chemotherapy (MZ201, MZ728) and FLT3-ITD mutation (MZ529, MZ580, MZ987). Patients MZ201, MZ653, and MZ728 died from treatment-refractory AML within few months. Patients MZ529, MZ580, and MZ987 were transplanted from HLA-matched unrelated donors, but died within 1 year because of leukemia relapse. Patient MZ169 remained disease-free until today. High-resolution HLA typing was performed according to standard procedures.
Primary cells and cell lines
PBMCs and primary AML blasts were isolated by Ficoll separation from buffycoats of healthy donors or from leukapheresis products and peripheral blood samples of patients at primary diagnosis, respectively. Epstein–Barr virus (EBV)-transformed B lymphoblastoid-cell lines (LCLs) and phytohemagglutinin (PHA)-activated T-cell blasts were generated by standard in vitro protocols. Monocytes were isolated from PBMCs using CD14-Microbeads (Miltenyi Biotec, Bergisch-Gladbach, Germany). Primary fibroblasts were isolated and expanded from bone marrow aspirates of AML patients in vitro as described [12]. The non-hematopoietic and stromal origin was regularly confirmed by the surface phenotype CD45−, CD33−, CD14−, CD90+, and D7-Fib+ in flow cytometry [12]. Fibroblasts regularly expressed strong levels of HLA-class I. Pretreatment of fibroblasts with 500 IU/mL IFN-γ before use did not lead to increased recognition by CTLs.
Isolation of naive CD8+ T cells
Naive CD8+ T cells were isolated from PBMCs using the Naive CD8 + T-Cell Isolation Kit (Miltenyi Biotec). Briefly, non-naive T cells and NK cells were first depleted on LD columns using a cocktail of biotin-conjugated antibodies against CD45RO, CD56, CD57, and CD244. Naive CD8+ T cells were then selected using CD8-Microbeads and MS or LS columns, respectively. Total CD8+ T cells were isolated from PBMCs by CD8 Microbeads with a purity of >95% (Miltenyi Biotec).
Mini-mixed lymphocyte-leukemia cultures
Mini-MLLCs were started in 96-well plates in AIM-V culture medium (GIBCO-BRL, Grand Island, NY, USA) supplemented with 10% human serum [9]. Responder cells were CD45RA+ naive CD8+ T cells or entire CD8+ T cells (each 104 per well) isolated from healthy donors as described above. Stimulators were allogeneic primary AML blasts (104 per well) pre-cultured overnight and irradiated with 35–60 Gy. Irradiated CD8-negative or non-naive T cells (104 per well) of the same donor were used as feeders. Medium was supplemented with 5 ng/mL IL-7, 1 ng/mL IL-12, and 5 ng/mL IL-15 (all R&D Systems, Wiesbaden, Germany). To analyze the impact of IL-21 in side-by-side MLLCs, the cytokine was added at 10–30 ng/mL (Biomol, Hamburg, Germany) or omitted, respectively. Mini-MLLC responders were weekly restimulated with irradiated AML blasts. IL-12 was replaced by IL-2 (50–250 IU/mL; Chiron, Emeryville, CA, USA) on d14. Growing mini-cultures were expanded in 24-well plates using 106 responders and 106 irradiated AML blasts per well. Set-up of mini-MLLCs including functional and phenotypic characterization of responding cultures is illustrated in supplementary Figure 1. Depending on available T-cell numbers, we initiated 0.5–2 96-well plates per experimental condition.
IFN-γ ELISpot assay
IFN-γ enzyme-linked immunosorbent spot (ELISpot) assays were performed over 20 h as described [13]. T cells were seeded at 1 × 104 to 2 × 104 per well and target cells at 5 × 104 per well. To analyze HLA-class I-restricted reactivity of CTLs, the following murine monoclonal antibodies (mAbs) were added at saturating concentration: W6/32, an anti-HLA class I IgG2a, PA2.1, an anti-HLA-A2 IgG1, GAP-A3, an anti-HLA-A3 IgG2a, B1.23.2, an anti-HLA-B and -C IgG2a, SFR8-B6, an anti-HLA-Bw6 and -C IgG2b, and L243, an anti-HLA-DR IgG2a [13]. To investigate reactivity of AML-reactive CTLs to known leukemia-associated antigens (LAA) and minor histocompatibility antigens (mHag), HLA-A*02:01-restricted CTLs were tested against A*02:01-expressing target cells T2 and K562-A*02:01 loaded with 10 μg/mL of the following peptides: WT1 p126–134 (RMFPNAPYL), Proteinase-3 PR1 p169–177 (VLQELNVTV), PRAME p100–108 (VLDGLDVLL), HA-1 p166–174 (VLHDDLLEA). Spots were counted by a computer-assisted image analyzer (KS-ELISpot 4.9; Zeiss, Jena, Germany). Results represent mean ± standard deviation (SD) of duplicates. Data were statistically analyzed with the Wilcoxon signed-rank test.
51Chromium-release assay
Target cells (1 × 106) were incubated for 2 h with 100 μCi of Na 512 CrO4 (Perkin Elmer, Rodgau, Germany) and 50 μL fetal calf serum. After washing, labeled targets were plated at 1.5 × 103 per well in conical 96-well plates. T cells were added at indicated effector-to-target (E:T) ratios. After incubation over 5 h at 37°C, supernatant was measured in a Packard Cobra gamma counter (Perkin Elmer). Percent specific lysis was calculated using the following equation: % specific lysis = 100 × (experimental release − spontaneous release)/(maximum release − spontaneous release). Data are mean ± SD of duplicates.
Flow cytometry analysis
Cells were stained with FITC-, PE-, APC-, PerCP-, PE-Cy5-, or Horizon V450-conjugated mAbs (Immunotech/Beckman Coulter, Marseille, France; BD Biosciences, Heidelberg, Germany; R&D Systems, Wiesbaden, Germany; Miltenyi Biotec). T-cell receptor (TCR) Vβ chains were determined using fluorescein-labeled mAbs recognizing 24 different Vβ families (IOTest BetaMark Kit, Immunotech/Beckman Coulter). Analysis was performed on a BD FACSCanto II flow cytometer. Software was BD FACSDiva™ and EXPO32™ for re-analysis. To evaluate expression level of distinct markers, the relative fluorescence intensity was calculated from median fluorescence intensity (MFI) values of relevant stainings divided by MFI values of the respective IgG isotype control stainings. Flow cytometric analyses of apoptotic and dead cells in T-cell cultures were performed with Annexin-V and 7-AAD stainings, respectively (BD Biosciences). Statistical data analysis was conducted with SPSS-15.0 software. Mann–Whitney U test was performed when appropriate.
Results
Reliable generation of leukemia-reactive CD8+ T cells from naive CD45RA+ precursors and favorable influence of IL-21
We initially compared the naive CD8+ T-cell subset with entire unseparated CD8+ T cells as a source for generating leukemia-reactive CTLs from healthy donors in vitro. Both cell populations were isolated from PBMCs by immunomagnetic beads. In phenotypic analysis, naive CD8+ T cells expressed CD45RA, CCR7, CD62L(high/low+), CD27, CD28, CD127, CXCR4, and were negative or low positive for CD45RO, CD57 and CD95 (supplementary Fig. 2). Naive and total CD8+ T cells were both stimulated in 96-well mini-MLLCs with primary AML blasts. Donors and AML patients were selected on the basis of complete HLA-class I match in donor-versus-patient direction at high resolution (Table 1). Cultures were supplemented with IL-7, IL-12 (until d14), IL-15, and IL-2 (from d14 on). To investigate the influence of IL-21, half of cultures were started with this cytokine. After two to three weekly AML stimulations, aliquots of all responder populations were used to screen for leukemia reactivity by split-well IFN-γ ELISpot assay. In three out of three AML patient/donor pairs significantly higher numbers of leukemia-reactive T cells were observed in cultures initiated with naive CD8+ T cells compared to unseparated CD8+ T cells (P = 0.043; Fig. 1a). Additional mini-MLLC experiments in one related and six unrelated patient/donor pairs confirmed that naive CD45RA+ T cells were a very reliable source for producing leukemia-reactive CD8+ T cells, and that the efficiency of the procedure could be further increased by IL-21 (Fig. 1b). Overall, this cytokine resulted in 1.1–3.3-fold (mean 1.8-fold) higher numbers of AML-reactive CD8+ T-cell populations compared to untreated cultures [P = 0.042, n = 5 (10 ng/mL IL-21); P = 0.028, n = 7 (30 ng/mL IL-21)].
IL-21 promotes the generation of AML-reactive CD8+ T cells from naive CD45RA+ precursors. a Numbers of AML-reactive cultures per 96 replicate wells obtained with purified CD45RA+ CD8+ T cells or unseparated CD8+ T cells in three AML patient/donor pairs with full HLA-class I match. Allogeneic mini-MLLCs were initiated with (10 or 30 ng/mL) or without IL-21, respectively, and were analyzed 5 days after the second (d14) or third (d21) antigen-specific restimulation for reactivity to primary AML blasts in split-well IFN-γ ELISpot assay. Wells considered as “positive” for AML recognition had ≥5-fold higher spot numbers compared to background level (i.e. spontaneous IFN-γ production). b Numbers of AML-reactive mini-cultures per 96 replicate wells generated from naive CD45RA+ CD8+ T cells from seven HLA-class I-matched AML patient/donor pairs
Functional properties of AML-reactive CTLs
A total of 257 CD8+ T-cell populations with strong AML reactivity in the screening assay were transferred into 48-/24-well plates and were expanded by weekly AML stimulations. More than half of them (i.e. 150) showed HLA-class I-restricted leukemia reactivity as well as sustained in vitro expansion over several weeks (data not shown). Interestingly, a higher fraction of such robust cultures was isolated from plates treated with IL-21 (110 of 165; 67%) versus those without IL-21 (40 of 92; 43.5%). Comprehensive analyses of several functional properties (i.e. HLA-restriction element, cross-reactivity to other patient-derived target cells and third-party target cells expressing shared HLA alleles, cytolytic activity, TCR Vβ usage) were performed with 26 individual CD8+ T-cell populations selected from 6 different AML patient/donor pairs, in which sufficient amounts of AML blasts were available.
All CD8+ T-cell populations showed significant reactivity in IFN-γ ELISpot and cytotoxicity assays to either AML blasts only or AML blasts and patient-derived LCLs. Representative examples are described in Figs. 2 and 3. None of CTLs were reactive to donor-derived LCLs and natural killer target K562, suggesting that CTLs may recognize LAA or recipient mHag as target structures. A single CTL with reactivity to patient AML (and not LCL) showed also minor recognition of monocytes, suggesting a myeloid-associated antigen overexpressed in AML as target (Table 2). Several CTLs reactive to patient’s AML and LCL also recognized PHA-activated T-cell blasts of patient origin, consistent with potential reactivity to recipient mHag with hematopoiesis-restricted expression. Of 26 CTLs totally analyzed, 8 showed significant cross-reactivity to patient’s stromal fibroblasts, suggesting that these CTLs may recognize recipient mHag broadly expressed in hematopoietic and non-hematopoietic cells. Interestingly, three CTLs were isolated that recognized B-LCL but not T-cell blasts from the same patient, potentially indicating antigens with low or absent expression in the T-cell lineage [14, 15]. Nineteen CTLs cross-reacted with a median number of 4 (range 1–18) third-party primary myeloid leukemias that expressed HLA-class I alleles shared with patient’s AML. Donor’s PBMCs were recognized by a single CTL only (Table 2). In addition to IFN-γ production, CTLs secreted TNF-α upon AML stimulation, as determined by ELISA in nine CTLs from six patient/donor pairs (data not shown).
HLA-class I restriction, cross-reactivity, in vitro expansion, and TCR Vβ chains of AML-reactive CD8+ T-cell populations. Shown are three representative CTL clones from three different AML patient/donor pairs. a CTL 2D8 (MZ201-AML/Don.168) recognizing exclusively patient’s AML blasts, b CTL 5H11 (MZ580-AML/Don.931) reacting to patient’s AML blasts as well as patient-derived lymphocytes, c CTL 7H1 (MZ529-AML/Don.730) recognizing patient’s hematopoietic as well as non-hematopoietic cells. Left panel cross-reactivity patterns to patient’s hematopoietic cells and stromal fibroblasts as well as donor’s hematopoietic cells and the natural killer cell-target K562 determined by IFN-γ ELISpot assay. Note that anti-HLA-class I mAb W6/32 inhibited recognition of AML blasts. Cross-reactivity to fibroblasts, PHA-activated T-cell blasts, and donor PBMCs was defined as significant if values were >10% of AML reactivity. Middle panel mini-MLLCs were initiated with 104 naive CD45RA+ CD8+ T cells and were stimulated once a week with irradiated AML blasts. Numbers of expanding cells were weekly determined as soon as cell counting was feasible (mostly d28–d35). Right panel flow cytometric characterization of the TCR Vβ chain used by the CTLs that grew out of mini-MLLCs. CTL was defined as monoclonal if >90% of cells expressed a single TCR Vβ chain. *CTL 5H11 cross-reacts with AML blasts from patient MZ946. Because bone marrow aspirate from patient MZ580 (whose AML cells were used for stimulation) was not available, stromal fibroblasts isolated from patient MZ946 were used
IL-21 does not impact on cytolytic activity of AML-reactive CTLs. CD8+ T-cell populations were restimulated with AML blasts over 2 weeks in the presence (gray 10 ng/mL, black 30 ng/mL) or absence (white) of IL-21, and were subsequently tested in 5 h 51Chromium-release assays for cytolytic activity against patient’s AML cells, patient-derived LCL cells, donor-derived LCL cells, and K562 cells. a CTL 2D8 (MZ201-AML/Donor168) originally generated with IL-21 and recognizing AML blasts. b CTL 7H1 (MZ529-AML/Donor730) originally generated with IL-21 and recognizing AML blasts as well as patient-derived LCL cells. c CTL 1E3 (MZ653-AML/Donor069) originally generated without IL-21 and recognizing AML blasts. d CTL 2E8 (MZ529-AML/Donor730) originally generated without IL-21 and recognizing AML blasts as well as patient-derived LCL cells. Cytokines were not added to the assay medium
By using mAbs that cover allele-specific or shared HLA epitopes, and by cross-reactivity tests on leukemia blasts expressing HLA alleles matched with the original AML stimulator cells, HLA-A01, -A02, -B13, -B15, -B57, -C03, -C06, or -C07 were identified as potential restriction elements for CTLs (Table 2). This information allowed us to screen 7 HLA-A*02:01-restricted CTLs for recognition of known A*02:01-binding peptide epitopes encoded by LAA WT-1, Proteinase-3, PRAME, and mHag HA-1. However, none of them showed reactivity to these epitopes (data not shown).
In order to analyze the clonality of CTLs, we performed flow cytometric stainings of TCR Vβ chains. Of 26 CTLs analyzed, 14 (i.e. 54%) expressed a single TCR Vβ chain suggesting monoclonality (Fig. 2; Table 2). Eight (i.e. 31%) CTLs showed expression of two to three different TCR Vβ chains. Furthermore, the approach was unable to detect the major TCR Vβ chains in 4 CTLs (Table 2). By weekly in vitro stimulations with AML blasts and cytokines, CTLs could be easily expanded to cell numbers exceeding 108 within few weeks (Fig. 2).
Influence of IL-21 on AML reactivity and expansion rate of long-term cultured CTLs
Most AML-reactive CTLs retained IFN-γ production and cytolytic activity for at least 10 weeks of culture. In order to investigate the impact of IL-21 on these effector functions, CTLs generated in the presence of IL-21 were restimulated at later culture periods (>d42) in medium supplemented with or without IL-21 for at least 2 weeks. They were subsequently tested in 51Chromium-release assays. Overall, in vitro presence or absence of IL-21 did not induce clear differences in CTL-mediated cytolysis of AML cells. Representative examples out of 12 CTLs analyzed are shown in Fig. 3a, b. Only a single CTL-mediated stronger lysis against AML if pre-cultured in IL-21-containing medium (not shown). Also, when analyzing anti-AML CTLs that had been generated without IL-21, the secondary use of this cytokine at later culture periods was unable to further enhance cytolytic activity; four of five CTLs analyzed demonstrated no significant difference in cytotoxicity (representative examples shown in Fig. 3c, d). A single CTL generated without IL-21 lysed target cells stronger when IL-21 was added at later culture periods preceding the cytotoxicity assay (data not shown). We obtained similar results if IFN-γ ELISpot instead of 51Chromium-release were used as read-out assay.
Significantly lower numbers of AML-reactive CTLs were isolated from mini-MLLCs started without IL-21 compared to those with IL-21 during primary in vitro stimulation (Fig. 1). However, single AML-reactive CTLs generated without IL-21 (e.g. 2E8 and 1E3) could be expanded to comparably high cell numbers than IL-21-exposed CTLs. Hence, we analyzed the impact of IL-21 on the growth rate of AML-reactive CTLs in more detail. At the earliest time point when cell counting of each mini-culture was feasible (d28), we determined higher total cell numbers in IL-21-treated cultures (median 2.6 × 106; range 0.25–3.54 × 106) compared to cultures started without IL-21 (median 1.3 × 106; range 0.3–3.15 × 106, P = 0.036). To analyze if IL-21 improved the viability of T cells, mini-cultures (37–38 cultures each for +/− IL-21) were randomly selected on d21–d28 in two patient/donor pairs and were stained with Annexin-V and 7-AAD, respectively. We detected a modest decrease in the percentage of apoptotic and dead CD8+ T cells in IL-21-treated mini-cultures [Annexin-V: 7.7 vs. 4.0%, P = 0.037; 7-AAD: 6.1 vs. 3.7%, P = 0.081 (data not shown)].
To also analyze the effect of IL-21 on proliferation during long-term culture, frozen aliqouts of CTLs from later culture periods (d35–d70) were thawed and restimulated over 2–3 weeks with AML cells in the presence or absence of IL-21. Weekly determination of growth factors did not reveal a clear impact of IL-21 on T-cell expansion. Briefly, 6 of 14 CTLs that had been generated in the presence of IL-21 grew better at later culture periods if IL-21 was applied. Each four CTLs, however, showed lower or unaltered growth rates in these experiments. Four of five CTLs that were originally cultured without IL-21 demonstrated better growth at later culture periods if IL-21 was added (data not shown). However, the IL-21 effect on these CTLs could not be confirmed in a substantial proportion of control experiments. We concluded that IL-21 did not have a consistent influence on the expansion of AML-reactive CTLs during late culture periods.
AML-reactive CTLs display markers of an early differentiation phenotype
We next analyzed 49 AML-reactive CTLs for surface expression of several markers of differentiation (CD45RA, CD45RO, CD27, CD28, CD95, CD57), homing (CD62L, CCR7, CXCR4) and responsiveness to cytokines (CD127). CTLs were derived from seven patient/donor pairs and were tested between day 21 and 91 of culture in two series of experiments: early stainings from day 21 to 42 during primary culture as well as stainings at later culture periods (>d56) in CTLs generated in the presence or absence of IL-21. In general, we observed that CTLs regularly expressed the markers CD45RO, CD45RA, CD27, CD57, CD95, and CXCR4 at intermediate to high levels during the whole observation period. The homing molecule CD62L and the chemokine receptor CCR7, necessary for trafficking of CTLs to lymphatic organs, were expressed at intermediate to low levels until day 28–35, although we still detected CD62L expression on single CTLs up to day 70. The IL-7 receptor alpha chain (CD127) and the costimulatory molecule CD28 were consistently observed until day 49 to 56, respectively. Representative data of a single CD45RA+-derived anti-AML CTL are shown in Fig. 4a.
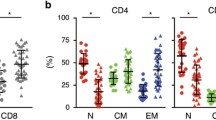
CD45RA+-derived leukemia-reactive CTLs retain markers of an early differentiation phenotype, which is further promoted by IL-21. a Flow cytometric characterization of CTL clone 4B2 (MZ653-AML/Donor069) at d35 of culture. Shown are the stainings for several T-cell differentiation markers (black lines) and the respective isotype control (gray shadings), as well as the co-stainings for CD8 and TCR Vβ 11. b Box plots showing the median expression level for CD28, CD127, CD45RO, CD45RA, CD62L, and CXCR4 on 5–11 CTLs per group (without/with IL-21) in three AML patient/donor pairs analyzed at d35 of culture. Expression level is shown as relative fluorescence intensity calculated from the median fluorescence intensity (MFI) value of the relevant staining divided by the MFI value of the respective IgG isotype control staining. All control stainings had absolute MFI values in the range 0.2–0.8 depending on the used fluorochrome, analyzed with EXPO32™ software. P values were calculated with the Mann–Whitney U test
Further comparisons of CTLs isolated in three AML patient/donor pairs with or without IL-21 and analyzed from day 21 to 42 revealed that CD45RO was clearly lower expressed (P < 0.02 at d35 and d42) on IL-21-treated CTLs, consistent with concomitant higher expression of CD45RA (Fig. 4b). CD62L showed increased expression from day 28 to 35 on CTLs generated with IL-21. The chemokine receptor CXCR4 was detectable at low to intermediate level until day 70 on several CTLs, but from day 35 to 42 with higher intensity (P < 0.03) on AML-reactive CTLs generated without IL-21. In addition, we measured stronger CD28 expression (P < 0.05) on CTLs with IL-21 from day 21 to 35. This also applied to CD127, which was detectable until day 49, with higher expression between day 28 and 42 on IL-21-exposed CTLs (P < 0.04 at d28; data not shown). In contrast, we did not find an enhancing effect of IL-21 on the expression levels of CD27, CCR7, CD57, and CD95 during the entire observation period (data not shown). The data set of CD markers on isolated naive CD8+ T-cell subsets and related AML-reactive CTL populations generated with IL-21 in three patient/donor pairs is shown in supplementary Table 1.
In summary, we have shown that AML-reactive CTLs generated from naive CD45RA+ CD8+ T cells of healthy donors express CD27, CD28, CD127, and CD62L for at least 4–5 weeks after primary in vitro stimulation. The expression of several of these “early” phenotypic markers is further promoted by the addition of IL-21 to the cultures.
Discussion
Clinical tumor remissions following adoptive immunotherapy with in vitro expanded tumor- and leukemia-reactive T-cell lines and clones are frequently not durable and may occur as mixed responses only at certain sites [16–18]. Among other reasons, these observations can be explained by insufficient persistence and homing of adoptively transferred T cells, which have reached a terminal differentiation state during in vitro expansion over several weeks. One potential strategy to overcome this limitation is to improve the efficiency of in vitro protocols allowing more leukemia-reactive T-cell precursors to grow during the primary stimulation phase. This may help to reduce the number of cell cycles of each single precursor and should translate into improved immune functions upon adoptive transfer in vivo. Here, we introduce a very reliable and efficient method for the generation of leukemia-reactive CTLs from naive CD45RA+ CD8+ T lymphocytes of healthy donors during a comparably short culture period. The approach allows the in vitro expansion of a large diversity of HLA-class I-restricted CTLs with an early differentiation phenotype and sustained effector functions toward AML blasts.
The set-up of allogeneic MLLCs with naive CD8+ T cells as responders has two major advantages: first, it reduces the likelihood that leukemia-reactive CTLs rapidly enter a status of terminal differentiation that is accompanied by functional exhaustion and cell death. The superiority of early differentiated (naive/central memory) CD8+ T-cell subsets in mediating antitumor and antiviral immunity after adoptive transfer has been impressively demonstrated in murine and primate models [6, 19, 20]. These observations may be explained with less-shortened chromosome telomeres in the naive subset (i.e. less cell division cycles) of less-differentiated T cells that have not yet reached replicative senescence, correlating with persistence after adoptive transfer [8, 21, 22]. Second, the precursor frequency of leukemia-reactive CTLs in PBMCs of healthy individuals is very low [23]. Due to the high diversity of their TCR repertoire, naive CD8+ T cells contain the majority of tumor-reactive CTL precursors in healthy individuals [24–26]. The latter point was confirmed herein for leukemia-reactive CTLs by detecting more precursors in naive CD45RA+ compared to entire CD8+ T cells. Thus, by the use of naive CD45RA+ CD8+ T cells in combination with limiting-dilution conditions and no IL-2 during the primary stimulation phase, we promote the expansion of leukemia-reactive CTLs, and we avoid the overgrowth with competing specificities, for example virus-reactive memory T cells.
As stimulator cells in allogeneic MLLCs we used leukemia blasts previously isolated from peripheral blood of AML patients. This assures the in vitro stimulation of donor T cells against hematopoietic mHag as well as LAA presented by recipient AML cells. Cross-reactivity data shown herein indicate that both of these proposed CTL specificities are most likely expanded by our approach. In contrast to other groups [18, 27], we did not use non-malignant mononuclear cells or dendritic cells of patient origin as stimulator cells, because it would restrict in vitro reactivity exclusively to hematopoietic mHag. This difference in stimulation conditions may be an important point, since the contribution of both antigen categories (i.e. hematopoietic mHag and LAA) to the induction of effective GVL responses in vivo is still not fully understood [28]. We also observed that one-third of leukemia-reactive CTLs cross-reacted with stromal fibroblasts. This suggested recognition of antigens ubiquitously expressed by hematopoietic and non-hematopoietic recipient cells [15]. If such CTLs would be adoptively transferred into patients, they might induce serious GvH reactivity and therefore should be excluded from any therapeutic approach. However, additional work including the molecular definition of CTL antigens and adoptive CTL transfer experiments in AML-engrafted immunodeficient mice [9] are required before CTLs generated by the described approach appear safe enough to be investigated in pilot clinical trials. Clinical testing would then definitely demonstrate if such CTLs are capable of mediating sufficient GvL effects in the absence of GvHD in vivo.
Another beneficial component of our protocol appears to be the cytokine combination used during primary stimulation. The common gamma chain cytokines IL-7 and IL-15 are essential for the survival and homeostasis of naive and memory T cells [29–32]. Furthermore, IL-15 has been shown to favor the in vitro generation of leukemia-reactive CD8+ central memory T cells [33]. IL-12 is necessary as “third signal” for efficient priming of naive CD8+ precursors [34]. While we already described this favorable cytokine combination in our previous study [9], the current addition of IL-21 clearly improved the efficacy in generating leukemia-reactive CTLs. This was demonstrated in eight different AML patient/donor pairs with remarkable consistency. Our observation with leukemia-reactive CTL clones is in accordance with earlier reports showing that IL-21 promotes the priming of naive CD8+ T cells and enhances anti-tumor effects of antigen-specific CTLs [10, 35–38].
We confirmed previous data from Li et al. [10] showing that the beneficial effect of IL-21 on the production of antigen-specific CTLs can partly be attributed to decreased apoptosis and increased survival of T cells in IL-21-treated cultures. Consistent with the authors, however, we consider antigen-specific CTL proliferation enhanced by IL-21 as the primary cytokine effect. Although IL-21 clearly improved the yield of AML-reactive CTLs during the first weeks of MLLCs, it did not increase antigen-dependent proliferation and effector functions during later culture periods. This is not necessarily inconsistent with other reports showing a synergistic positive effect of IL-15 and IL-21 on proliferation and effector functions of tumor-specific CTL at early time points of culture [39, 40]. First, our approach also included IL-7 (throughout the culture) and IL-2 (from d14 on), which might have enhanced the expansion and effector functions of CTLs to a level where the synergism of IL-15 and IL-21 is hard to detect. Beside different cytokine settings, previous studies also differed in several other important parameters (e.g. CTL bulk cultures, stimulation with specific peptides, time point of testing) from our work, making direct comparisons of findings very difficult. Again, testing leukemia-reactive CTLs (+/− IL-21) in suitable immunodeficient animal models would be helpful to finally determine the biological relevance of CTLs as well as the impact of IL-21 on CTL effector function in vivo.
After adoptive transfer into patients, leukemia-reactive CTLs should survive and expand in vivo, migrate to end organs and exert strong effector functions. It is widely assumed that these important properties are mediated by cytokine receptors (e.g. CD127), homing molecules (e.g. CD62L), chemokine receptors (e.g. CCR7, CXCR4), and costimulatory molecules (CD27, CD28) [8, 41, 42]. Herein we show that several of these “early” (naive/central memory) differentiation markers were expressed by CD45RA+-derived CTLs over multiple weeks of in vitro culture. In addition, CTL clones generated in presence of IL-21 demonstrated stronger expression of CD28, CD127, CD62L, and CD45RA along with decreased expression of CD45RO leading to a more “early” phenotype, which might promote the survival and homing of T cells. These findings are consistent with previous reports demonstrating the expression of central memory markers on antigen-specific T-cell lines primed in the presence of IL-21 [10, 38, 43–45]. In contrast to CD62L, we did not observe the regular expression of CCR7 beyond 5 weeks of culture. Furthermore, although the chemokine receptor CXCR4 was found at lower expression level on IL-21-treated CTLs, all of them expressed this marker. Expression of CXCR4 has been suggested to allow for the migration of T cells into the bone marrow [46]. Thus CXCR4+ CD62L+ CTLs should be able to home in lymphoid tissues and reach leukemia-infiltrated marrow sites.
In summary, leukemia-reactive CTLs generated from the naive CD45RA+ compartment could be promising candidates for cellular immunotherapy because of their relatively early differentiation phenotype and strong capability of cell expansion, what might translate into improved functions in vivo. We also showed that the addition of IL-21 to the protocol enabled more precursors to develop into potent leukemia-reactive CTLs, presumably by its beneficial effects on cell survival and antigen-specific proliferation during the first weeks of cultures. The cytokine also strengthened the early stage phenotype. Nevertheless, further preclinical work is required before such CTLs appear safe enough to be investigated in pilot clinical trials. The herein described allo-MLLC approach with in vitro “programmed” naive CTL precursors of healthy donors independent of a HSCT setting is a valuable alternative to the conventional method of isolating in vivo primed donor CTLs out of patients after transplantation [18, 47]. This would make leukemia-reactive CTLs already available at the time point of HSCT, when residual leukemia disease is minimal and the chances for complete leukemia eradication are high. Although the translation of the entire approach into a good manufacturing practice protocol is challenging, the use of certain components (e.g. naive CD8+ T cells, cytokine combination) might improve other methods to generate tumor antigen-specific T cells for clinical application. Furthermore, leukemia-reactive CTLs effectively expanded by this in vitro protocol can be used as screening populations to define candidate LAA and mHag for antigen-specific immunotherapy.
Abbreviations
- AML:
-
Acute myeloid leukemia
- CTL:
-
Cytotoxic T lymphocyte
- DLI:
-
Donor lymphocyte infusion
- EBV:
-
Epstein–Barr virus
- FAB:
-
French-American-British
- GvH:
-
Graft-versus-host
- GvL:
-
Graft-versus-leukemia
- HLA:
-
Human leukocyte antigen
- HSCT:
-
Hematopoietic stem-cell transplantation
- LAA:
-
Leukemia-associated antigen
- LCL B:
-
Lymphoblastoid-cell line
- mAb:
-
Monoclonal antibody
- mHag:
-
Minor histocompatibility antigen
- MLLC:
-
Mixed lymphocyte-leukemia culture
- PBMC:
-
Peripheral blood mononuclear cell
- SIB:
-
Sibling donor
- TCR:
-
T-cell receptor
References
Kolb HJ (2008) Graft-versus-leukemia effects of transplantation and donor lymphocytes. Blood 112:4371–4383
Falkenburg JHF, Heslop HE, Barrett AJ (2008) T cell therapy in allogeneic stem cell transplantation. Biol Blood Marrow Transplant 14:136–141
Barrett AJ (2008) Understanding and harnessing the graft-versus-leukaemia effect. Br J Haematol 142:877–888
Bleakley M, Riddell SR (2004) Molecules and mechanisms of the graft-versus-leukaemia effect. Nat Rev Cancer 4:371–380
Gattinoni L, Klebanoff CA, Palmer DC, Wrzesinski C, Kerstann K, Yu Z, Finkelstein SE, Theoret MR, Rosenberg SA, Restifo NP (2005) Acquisition of full effector function in vitro paradoxically impairs the in vivo antitumor efficacy of adoptively transferred CD8+ T cells. J Clin Invest 115:1616–1626
Klebanoff CA, Gattinoni L, Torabi-Parizi P, Kerstann K, Cardones AR, Finkelstein SE, Palmer DC, Antony PA, Hwang ST, Rosenberg SA et al (2005) Central memory self/tumor-reactive CD8+ T cells confer superior antitumor immunity compared with effector memory T cells. Proc Natl Acad Sci USA 102:9571–9576
Berger C, Turtle CJ, Jensen MC, Riddell SR (2009) Adoptive transfer of virus-specific and tumor-specific T cell immunity. Curr Opin Immunol 21:224–232
Klebanoff CA, Gattinoni L, Restifo NP (2006) CD8+ T-cell memory in tumor immunology and immunotherapy. Immunol Rev 211:214–224
Distler E, Wölfel C, Köhler S, Nonn M, Kaus N, Schnürer E, Meyer RG, Wehler TC, Huber C, Wölfel T, Hartwig UF, Herr W (2008) Acute myeloid leukemia (AML)-reactive cytotoxic T lymphocyte clones rapidly expanded from CD8+ CD62L(high)+ T cells of healthy donors prevent AML engraftment in NOD/SCID IL2Rγnull mice. Exp Hematol 36:451–463
Li Y, Bleakley M, Yee C (2005) IL-21 influences the frequency, phenotype, and affinity of the antigen-specific CD8 T cell response. J Immunol 175:2261–2269
Delmer A, Marie JP, Thevenin D, Cadiou M, Viguie F, Zittoun R (1989) Multivariate analysis of prognostic factors in acute myeloid leukemia: value of clonogenic leukemic cell properties. J Clin Oncol 7:738–746
Nonn M, Herr W, Khan S, Todorova M, Link I, Thies J, Distler E, Kaltwasser M, Hoffmann J, Huber C, Hartwig UF (2008) Selective depletion of alloreactive T lymphocytes using patient-derived nonhematopoietic stimulator cells in allograft engineering. Transplantation 86:1427–1435
Dörrschuck A, Schmidt A, Schnürer E, Glückmann M, Albrecht C, Wölfel C, Lennerz V, Lifke A, Di Natale C, Ranieri E, Gesualdo L, Huber C, Karas M, Wölfel T, Herr W (2004) CD8+ cytotoxic T lymphocytes isolated from allogeneic healthy donors recognize HLA class Ia/Ib-associated renal carcinoma antigens with ubiquitous or restricted tissue expression. Blood 104:2591–2599
Dolstra H, Fredrix H, Maas F, Couline PG, Brasseur F, Mensink E, Adema GJ, De Witte TM, Figdor CG, Van de Wiel-van Kemenade E (1999) A human minor histocompatibility antigen specific for B cell acute lymphoblastic leukemia. J Exp Med 189:301–308
Feng X, Hui KM, Younes HM, Brickner AG (2008) Targeting minor histocompatibility antigens in graft versus tumor or graft versus leukemia responses. Trends Immunol 29:624–632
Huang J, Khong HT, Dudley ME, El-Gamil M, Li YF, Rosenberg SA, Robbins PF (2005) Survival, persistence, and progressive differentiation of adoptively transferred tumor-reactive T cells is associated with tumor regression. J Immunother 28:258–267
Robbins PF, Dudley ME, Wunderlich J, El-Gamil M, Li YF, Zhou J, Huang J, Powell DR Jr, Rosenberg SA (2004) Cutting edge: persistence of transferred lymphocyte clonotypes correlates with cancer regression in patients receiving cell transfer therapy. J Immunol 173:7125–7130
Warren EH, Fujii N, Akatsuka Y, Chaney CN, Mito JK, Loeb KR, Gooley TA, Brown ML, Koo KK, Rosinski KV et al (2010) Therapy of relapsed leukemia after allogeneic hematopoietic cell transplantation with T cells specific for minor histocompatibility antigens. Blood 115:3869–3878
Berger C, Jensen MC, Lansdorp PM, Gough M, Elliott C, Riddell SR (2008) Adoptive transfer of effector CD8+ T cells derived from central memory cells establishes persistent T cell memory in primates. J Clin Invest 118:294–305
Hinrichs CS, Borman ZA, Cassard L, Gattinoni L, Spolski R, Yu Z, Sanchez-Perez L, Muranski P, Kern SJ, Logun C et al (2009) Adoptively transferred effector cells derived from naive rather than central memory CD8+ T cells mediate superior antitumor immunity. Proc Natl Acad Sci USA 106:17469–17474
Zhou J, Shen X, Huang J, Hodes RJ, Rosenberg SA, Robbins PF (2005) Telomere length of transferred lymphocytes correlates with in vivo persistence and tumor regression in melanoma patients receiving cell transfer therapy. J Immunol 175:7046–7052
Shen X, Zhou J, Hathcock KS, Robbins P, Powell DJ Jr, Rosenberg SA, Hodes RJ (2007) Persistence of tumor infiltrating lymphocytes in adoptive immunotherapy correlates with telomere length. J Immunother 30:123–129
Smit WM, Rijnbeek M, van Bergen CA, Willemze R, Falkenburg JH (1998) Generation of leukemia-reactive cytotoxic T lymphocytes from HLA-identical donors of patients with chronic myeloid leukemia using modifications of a limiting dilution assay. Bone Marrow Transplant 21:553–560
Goldrath AW, Bevan MJ (1999) Selecting and maintaining a diverse T-cell repertoire. Nature 402:255–262
Pittet MJ, Valmori D, Dunbar PR, Speiser DE, Liénard D, Lejeune F, Fleischhauer K, Cerundolo V, Cerottini JC, Romero P (1999) High frequencies of naive Melan-A/MART-1-specific CD8(+) T cells in a large proportion of human histocompatibility leukocyte antigen (HLA)-A2 individuals. J Exp Med 190:705–715
Kausche S, Wehler T, Schnürer E, Lennerz V, Brenner W, Melchior S, Gröne M, Nonn M, Strand S, Meyer R, Ranieri E, Huber C, Falk CS, Herr W (2006) Superior antitumor in vitro responses of allogeneic matched sibling compared with autologous patient CD8+ T cells. Cancer Res 66:11447–11454
Bleakley M, Otterud BE, Richardt JL, Mollerup AD, Hudecek M, Nishida T, Chaney CN, Warren EH, Leppert MF, Riddell SR (2010) Leukemia-associated minor histocompatibility antigen discovery using T cell clones isolated by in vitro stimulation of naive CD8+ T cells. Blood 115:4923–4933
Rezvani K, Barrett AJ (2008) Characterizing and optimizing immune responses to leukaemia antigens after allogeneic stem cell transplantation. Best Pract Res Clin Haematol 21:437–453
Schluns KS, Kieper WC, Jameson SC, Lefrancois L (2000) Interleukin-7 mediates the homeostasis of naive and memory CD8 T cells in vivo. Nat Immunol 1:426–432
Berard M, Brandt K, Bulfone-Paus S, Tough DF (2003) IL-15 promotes the survival of naive and memory phenotype CD8+ T cells. J Immunol 170:5018–5026
Surh CD, Sprent J (2008) Homeostasis of naive and memory T cells. Immunity 29:848–862
Rochman Y, Spolski R, Leonard WJ (2009) New insights into the regulation of T cells by γc family cytokines. Nat Rev Immunol 9:480–490
Daudt L, Maccario R, Locatelli F, Turin I, Silla L, Montini E, Percivalle E, Giugliani R, Avanzini MA, Moretta A, Montagna D (2008) Interleukin-15 favors the expansion of central memory CD8+ T cells in ex vivo generated, antileukemia human cytotoxic T lymphocyte lines. J Immunother 31:385–393
Mescher MF, Curtsinger JM, Agarwal P, Casey KA, Gerner M, Hammerbeck CD, Popescu F, Xiao Z (2006) Signals required for programming effector and memory development by CD8+ T cells. Immunol Rev 211:81–92
Parrish-Novak J, Dillon SR, Nelson A, Hammond A, Sprecher C, Gross JA, Johnston J, Madden K, Xu W, West J et al (2000) Interleukin 21 and its receptor are involved in NK cell expansion and regulation of lymphocyte function. Nature 408:57–63
Casey KA, Mescher MF (2007) IL-21 promotes differentiation of naive CD8 T cells to a unique effector phenotype. J Immunol 178:7640–7648
Zeng R, Spolski R, Finkelstein SE, Oh S, Kovanen PE, Hinrichs CS, Pise-Masison CA, Radonovich MF, Brady JN, Restifo NP, Berzofsky JA, Leonard WJ (2005) Synergy of IL-21 and IL-15 in regulating CD8+ T cell expansion and function. J Exp Med 201:139–148
Kaka AS, Shaffer DR, Hartmeier R, Leen AM, Lu A, Bear A, Rooney CM, Foster AE (2009) Genetic modification of T cells with IL-21 enhances antigen presentation and generation of central memory tumor-specific cytotoxic T-lymphocytes. J Immunother 32:726–736
Pouw N, Treffers-Westerlaken E, Kraan J, Wittink F, ten Hagen T, Verweij J, Debets R (2010) Combination of IL-21 and IL-15 enhances tumour-specific cytotoxicity and cytokine production of TCR-transduced primary T cells. Cancer Immunol Immunother 59:921–931
Huarte E, Fisher J, Turk JM, Mellinger D, Foster C, Wolf B, Meehan KR, Fadul CE, Ernstoff MS (2009) Ex vivo expansion of tumor specific lymphocytes with IL-15 and IL-21 for adoptive immunotherapy in melanoma. Cancer Lett 285:80–88
Hinrichs CS, Gattinoni L, Restifo NP (2006) Programming CD8+ T cells for effective immunotherapy. Curr Opin Immunol 18:363–370
Powell DJ Jr, Dudley ME, Robbins PF, Rosenberg SA (2005) Transition of late-stage effector T cells to CD27+ CD28+ tumor-reactive effector memory T cells in humans after adoptive cell transfer therapy. Blood 105:241–250
Hinrichs CS, Spolski R, Paulos CM, Gattinoni L, Kerstann KW, Palmer DC, Klebanoff CA, Rosenberg SA, Leonard WJ, Restifo NP (2008) IL-2 and IL-21 confer opposing differentiation programs to CD8+ T cells for adoptive immunotherapy. Blood 111:5326–5333
Ansén S, Butler MO, Berezovskaya A, Murray AP, Stevenson K, Nadler LM, Hirano N (2008) Dissociation of its opposing immunologic effects is critical for the optimization of antitumor CD8+ T-cell responses induced by interleukin 21. Clin Cancer Res 14:6125–6136
Alves NL, Arosa FA, van Lier RA (2005) IL-21 sustains CD28 expression on IL-15-activated human naive CD8 T cells. J Immunol 175:755–762
Mora JR, von Andrian UH (2006) T-cell homing specificity and plasticity: new concepts and future challenges. Trends Immunol 27:235–243
Kloosterboer FM, van Luxemburg-Heijs SA, van Soest RA, Barbui AM, van Egmond HM, Strijbosch MP, Kester MG, Marijt WA, Goulmy E, Willemze R, Falkenburg JH (2004) Direct cloning of leukemia-reactive T cells from patients treated with donor lymphocyte infusion shows a relative dominance of hematopoiesis-restricted minor histocompatibility antigen HA-1 and HA-2 specific T cells. Leukemia 18:798–808
Acknowledgments
We thank Dr. Eva Wagner and Dr. Roland Conradi from Mainz for coordinating leukemia and lymphocyte sampling. We are grateful to Elke Schnürer for her excellent technical assistance. We also thank Dr. Holger Voss and Prof. Dr. Thomas Wölfel, Mainz, for providing LAA and mHag peptides. This work was supported by grant KFO183-TP5 of the Deutsche Forschungsgemeinschaft (DFG) to W.H.
Author information
Authors and Affiliations
Corresponding author
Additional information
W. Herr and E. Distler share senior authorship.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Albrecht, J., Frey, M., Teschner, D. et al. IL-21-treated naive CD45RA+ CD8+ T cells represent a reliable source for producing leukemia-reactive cytotoxic T lymphocytes with high proliferative potential and early differentiation phenotype. Cancer Immunol Immunother 60, 235–248 (2011). https://doi.org/10.1007/s00262-010-0936-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-010-0936-8