Abstract
The purpose of this study was to clarify whether HLA-DR expression of colorectal tumour cells or the CD4+/CD8+ ratio of the tumour infiltrating lymphocytes is significantly associated with the prognosis of colorectal cancer. Using flow cytometry, we studied the tumour cell expression of the HLA class II in 70 enzymatically dissociated colorectal cancers and the phenotype of tumour infiltrating lymphocytes (TILs) in 41 cases. There was no trend in 5-year survival between three levels (low, medium, high) of HLA-DR expression on the tumour cells. Patients with low CD4+/CD8+ ratios had a better clinical course, with significantly higher 5-year survival, p=0.046, independent of the Dukes stage and age. Our results have implications for tumour immunology; colorectal cancer cells might be a target for cytotoxic T-lymphocytes, however the tumour cells are not able to initiate an immune response. Stimulation of the immune system could possible be obtained using dendritic cells cultured in vitro and loaded with tumour antigens.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Malignant transformation of cells occurs through the accumulation of mutations in specific classes of genes [16]. Most mutations give rise to abnormal proteins, resulting in abnormal or lost function of proteins. Provided adequate stimulation, a change in amino acid sequence of a protein can be recognised by and stimulate the immune system. All nuclear cells are capable of presenting peptides via HLA class I molecules to the effector arm of the cellular immune system (CD8+ lymphocytes), but are unable to initiate an immune response which is initiated by functional antigen-presenting cells (APCs). In these cells, peptides are bound to HLA class II molecules and presented on the surface. Together with the co-stimulatory molecules on the APC, the peptide/HLA class II complex will stimulate the immune response (CD4+ lymphocytes).
Several attempts have been made to study the immune response to colorectal cancers. Pronounced lymphocytic infiltration in colorectal cancer has been shown to be an important prognostic parameter [5, 13]. Since then it has been shown that infiltration of cytotoxic T-cells (CD8+), contributes to a better survival of patients [11, 21]. High expression of HLA class II molecules has been associated with an improved prognosis in two studies [1, 15] while one other study did not confirm this [19].
We have previously developed a multiparameter flow cytometric measurement system to characterise cancer cells from colorectal tumours [6]. Using flow cytometry we examined both the expression of HLA class II on colorectal cancer cells and the phenotype of the infiltrating lymphocytes [7, 8]. In relation to these findings the objective of the present study was to clarify whether HLA-DR expression of tumour cells or the CD4+/CD8+ ratio of the tumour infiltrating lymphocytes was significantly associated with prognosis.
Materials and methods
Patients and tissue samples
Tumour tissue was obtained from 70 patients with a colorectal adenocarcinoma, all undergoing surgery in 1995 or 1996 at either Odense University Hospital or at Svendborg Hospital. Histopathological examination and staging of the tumours were performed on routine fixed and paraffin-embedded sections stained with haematoxylin and eosin. All carcinomas were staged according to Dukes and Bussey [9] as modified by Turnbull et al. (stage D, meaning distant metastasis or unresectable tumours because of parietal invasion) [24]. Further intensity of lymphoid infiltration (pronounced or modest) and tumour growth pattern (expansive or infiltrative) were evaluated as described by Jass et al. [13]. No cases received adjuvant radiation or chemotherapy. All patients were followed until death or for 5 years. For the present study, a sample of viable non-necrotic tumour tissue was taken from the tumour edge immediately after removal. All tumours were analysed for expression of HLA-DR at tumour cells, while in 41 tumours the CD4+/CD8+ ratio of the tumour infiltrating lymphocytes was analysed (Table 1). The study protocol was approved the Scientific Ethical Committee, Denmark.
Flow cytometry of the dissociated tumour tissue
Preparation of single cell suspensions from the solid tumours and the characterisation of the cell suspensions by multiparameter flow cytometry were evaluated as described previously [7, 8]. In brief, the tumour tissue was cut into small pieces with a pair of scissors, followed by incubation with the enzymes (collagenase, deoxyribonuclease and hyaluronidase) and preparation in a rotating chamber at 37°C. After 1 h, the cell suspension was filtered, and washed twice. Remaining tumour tissue was dissociated for another hour. The cell suspensions were pooled, and cryopreserved.
On the day of use the cells were thawed and counted. Viable cells were distributed in Falcon tubes (approx. 106 cells per tube) and centrifuged. The pellet was resuspended in the antibody suspension and incubated for 30 min in the dark at room temperature. The cell suspension was washed once more before being used in the FACScan (Becton Dickinson) and cell acquisition was carried out within 1 h. The data were obtained and analysed using the CellQuest (Becton Dickinson) software.
Tumour cells were analysed using a fluorescein isothiocyanate (FITC) labelled mAb to EP4 (an epithelial cell surface marker, Ber-EP4, Dako, Glostrup, Denmark) and a R-phycoerythrin (RPE) labelled mAb to HLA-DR (L243, Becton Dickinson, Amsterdam, CA). Tumour infiltrating lymphocytes were analysed with a FITC labelled mAb to CD8 (DK25, Dako), a RPE labelled mAb to CD4 (MT310, Dako) and a RPE-Cy5 R-phycoerythrin-cyanin labelled mAb to CD3 (UCHT1 Dako). Appropriate isotype controls were used to estimate background fluorescence and calibrite beads (Becton Dickinson) were used as an external standard. Electronic compensation was calibrated with a cell suspension labelled with 1) FITC-conjugated anti-CD8, RPE conjugated anti-CD4 and RPE-Cy5 conjugated anti-CD3, 2) FITC-conjugated anti-HLA-ABC (W6/32, Dako) and 3) RPE-conjugated anti-HLA-ABC (W6/32, Dako).
In the analyses, two dot-plots were made, one combining mAb to EP4 and HLA-DR and another (gating on the lymphocytes) combining mAb to CD4 and CD8.
Statistical evaluation
Reproducibility was studied calculating the kappa-value, i.e. 1.00 when agreement is perfect and zero when there is no agreement. To investigate if mean levels of the CD4+/CD8+ ratio differed from the Duke classification, an analysis of variance was performed. Survival curves based on all deaths, were computed by the Kaplan-Meier method and cumulative survival probability was calculated at 5 years stratified according to HLA-DR expression of tumour cells and CD4+/CD8+ ratio of the tumour infiltrating lymphocytes, in this case without any corrections. To investigate the influence of the CD4+/CD8+ ratio on mortality, controlling for the Dukes classification, age and sex, we used the model M given by:
where Dukes' A will be our group of reference, i.e., the relative risk is 1 for this group. In order to obtain relative risks, coefficients of variables in model M were estimated by the Cox regression method. The Cox proportional hazard assumption was tested by standard methods and was not found to be violated. Also, no variables in the model show interaction with risk-time. Afterwards sex was omitted from further analysis since the survival curves for male and females were not significantly distinct (log rank test, p=0.76) and also played no role on mortality in the Cox regression.
Results
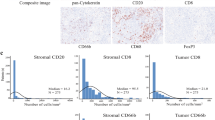
The dissociated cell suspension contained a mixture of tumour cells, lymphocytes, erythrocytes and fibroblasts. An average of 32% of the cells were EP4+ (range 3–60%). Gating on the EP4+ cells we estimated the number of tumour cells expressing HLA-DR. HLA-DR was expressed very heterogeneously both among tumours and within tumours. In 24 tumours less than 25% tumour cells expressed HLA-DR (low), in 22 tumours between 25 and 40% tumour cells expressed HLA-DR (medium), while in 24 tumours more than 40% of the tumour cells expressed HLA-DR (high). In the forward/side scatter gate, 60% of the TILs were CD3+. Among these CD4+ TILs were predominant—the median CD4+/CD8+ ratio was 2.2, range 0.8–6.8 (mean 2.5, standard deviation 1.27, N=41). The variable could be assumed to be normal distributed (probit plot not shown). There was a good agreement between two flow cytometric estimations on different days, kappa value=0.79.
There was no trend in 5-year survival between the three levels (low, medium, high) of HLA-DR expression on the tumour cells—HLA-DR low had a 5-year survival of 38% (9 out of 24), HLA-DR medium a 5-year survival of 55% (12 out of 22) and HLA-DR high tumours a 5-year survival of 17% (4 out of 24), see Fig. 1.
There was no difference in mean levels of CD4+/CD8+ ratios across Dukes' stages A, B, C and D (p=0.87). Patients with low CD4+/CD8+ ratios (>2.0) had a better clinical course, with a higher 5-year survival, 61% (11/18) versus 22% (5/23), see Fig. 2. In the Cox regression method the CD4+/CD8+ ratio was a substantial and significant predictor of mortality, even when correcting for Dukes classification and age (p=0.046). As expected the Dukes classification had high relative risks, while the influence of age was smaller, see Table 2.
The CD4+/CD8+ ratio was associated with intensity of lymphoid infiltration, but the data sample was to small to show any possible significance, see Table 3. There was no association between the CD4+/CD8+ ratio and tumour localisation or growth pattern, while the CD4+/CD8+ ratio was inversely associated with tumour differentiation (data not shown).
Discussion
The infiltration of CD4+ and CD8+ lymphocytes in colorectal cancer and the adjacent normal colon has been investigated in a few papers [2, 4, 18]. These authors found that the CD8+ lymphocytes were predominant in the intraepithelium of the colonic mucosa, however, in colorectal cancer the CD4+ lymphocytes were more frequent. These studies have not investigated the infiltration of CD4+ or CD8+ lymphocytes and survival.
The main finding in this paper is a significant inverse relationship between survival and the CD4+/CD8+ ratio of tumour infiltration lymphocytes. For several years it has been known that pronounced lymphocytic infiltration in colorectal cancer is an important prognostic parameter [5, 13], but until recently it has not been possible to demonstrate that predominance in the infiltrate of either one or the other T-cell subpopulation is consistently related to a better prognosis or survival [12, 17, 22]. However, using immunohistochemistry, two papers have now demonstrated that infiltration of CD8+ T cells within tumours contributes to a better survival [11, 21]. Our results are in agreement with this conclusion. Previously, it has been reported that colorectal cancer cells have down-regulated or even lost the expression of HLA class I molecules [10, 14, 19, 20], and this has been interpreted as a mechanism of tumour escape from the immune system [3]. All these data have been obtained by immunohistochemical analysis. Since then we have shown that flow cytometry is more sensitive, and that tumours previously described as HLA class I negative by immunohistochemistry were found to express HLA class I using flow cytometry [6]. We found that HLA class I was expressed on all tumour cells in 60 of the tumours, and reduced in 10, but importantly we never observed a total loss of HLA class I on all tumour cells in any tumour [7]. Our data indicate that via the HLA class I molecules the tumour cells are capable of presenting tumour peptides to the effector arm of the cellular immune system (CD8+ lymphocytes) and, if the CD8+ lymphocytes are present (low CD4+/CD8+ ratio), this is associated to a better prognosis, especially if there is a pronounced lymphoid infiltration.
Here we also describe that high expression of HLA-DR on tumour cells is not associated with a good prognosis and is rated the opposite. There does not seem to be consensus in the literature on this subject: in two studies, the expression of HLA class II on colorectal cancer cells has been related to a good prognosis [1, 15], while another study did not confirm this [19]. Previously we have described lack of CD80 expression on the tumour cells [7]. In the absence of the co-stimulatory signals delivered by CD80 and CD86, the interaction between HLA class II positive tumour cells and lymphocytes should give rise to anergy [23]. It is therefore possible that when tumour cells express HLA class II but not CD80, CD4+ lymphocytes are anergised rather than being stimulated and this might therefore correlate with a poor prognosis. This seems to fit with our data since very high expression of HLA-DR is actually associated with a poor prognosis.
Our results have implications for tumour immunology; colorectal cancer cells in general express HLA class I antigens on the surface and these might be targets for cytotoxic T-lymphocytes. However, the tumour cells are probably not able to initiate an immune response since expression of HLA class II does not seem to be related to prognosis and finally co-stimulatory molecules are not expressed. Since the immune response appears to be inadequate, stimulation of the immune system could possible be obtained using dendritic cells cultured in vitro and stimulated/loaded with tumour antigens. Such studies are currently ongoing.
References
Andersen SN, Rognum TO, Lund E, Meling GI, Hauge S (1993) Strong HLA-DR expression in large bowel carcinomas is associated with good prognosis. Br J Cancer 68:80
Banner BF, Savas L, Baker S, Woda BA (1993) Characterization of the inflammatory cell populations in normal colon and colonic carcinomas. Virchows Arch B Cell Pathol Incl Mol Pathol 64:213
Bodmer WF, Browning MJ, Krausa P, Rowan A, Bicknell DC, Bodmer JG (1993) Tumor escape from immune response by variation in HLA expression and other mechanisms. Ann N Y Acad Sci 690:42
Csiba A, Whitwell HL, Moore M (1984) Distribution of histocompatibility and leucocyte differentiation antigens in normal human colon and in benign and malignant colonic neoplasms. Br J Cancer 50:699
Di Giorgio A, Botti C, Tocchi A, Mingazzini P, Flammia M (1992) The influence of tumor lymphocytic infiltration on long term survival of surgically treated colorectal cancer patients. Int Surg 77:256
Diederichsen ACP, Hansen TP, Nielsen O, Fenger C, Jensenius JC, Christensen PB, Kristensen T, Zeuthen J (1998) A comparison of flow cytometry and immunohistochemistry in human colorectal cancers. APMIS 106:562
Diederichsen ACP, Stenholm ACO, Kronborg O, Fenger C, Jensenius JC, Zeuthen J, Christensen PB, Kristensen T (1998) Flow cytometric investigation of immune-response-related surface molecules on human colorectal cancers. Int J Cancer (Pred Oncol) 79:283
Diederichsen ACP, Zeuthen J, Christensen PB, Kristensen T (1999) Characterisation of tumour infiltrating lymphocytes and correlations with immunological surface molecules in colorectal cancer. Eur J Cancer 35:721
Dukes CE, Bussey HJR (1958) The spread of rectal cancer and its effect on prognosis. Br J Cancer 12:309
Garrido F, Cabrera T, Lopez Nevot MA, Ruiz Cabello F (1995) HLA class I antigens in human tumors. Adv Cancer Res 67:155
Guidoboni M, Gafa R, Viel A et al. (2001) Microsatellite instability and high content of activated cytotoxic lymphocytes identify colon cancer patients with a favorable prognosis. Am J Pathol 159:297
Hÿkansson L, Adell G, Boeryd B, Sjÿgren F, Sjÿdahl R (1997) Infiltration of mononuclear inflammatory cells into primary colorectal carcinomas: an immunohistological analysis. Br J Cancer 75:374
Jass JR, Love SB, Northover JM (1987) A new prognostic classification of rectal cancer. Lancet 1:1303
Kaklamanis L, Gatter KC, Hill AB, Mortensen N, Harris AL, Krausa P, McMichael A, Bodmer JG, Bodmer WF (1992) Loss of HLA class-I alleles, heavy chains and beta 2-microglobulin in colorectal cancer. Int J Cancer 51:379
Lazaris AC, Theodoropoulos GE, Davaris PS, Panoussopoulos D, Nakopoulou L, Kittas C, Golematis BC (1995) Heat shock protein 70 and HLA-DR molecules tissue expression. Prognostic implications in colorectal cancer. Dis Colon Rectum 38:739
Lengauer C, Kinzler WK, Vogelstein B (1997) Genetic instability in colorectal cancers. Nature 386:623
Matsuda M, Petersson M, Lenkei R, Taupin JL, Magnusson I, Mellstedt H, Anderson P, Kiessling R (1995) Alterations in the signal-transducing molecules of T cells and NK cells in colorectal tumor-infiltrating, gut mucosal and peripheral lymphocytes: correlation with the stage of the disease. Int J Cancer 61:765
Matsuda S, Yamane T, Hamaji M (1998) CD4 and TCR alphabeta-positive T lymphocytes predominantly infiltrated into well-moderately differentiated colon adenocarcinoma tissues. Jpn J Clin Oncol 28:97
Möller P, Momburg F, Koretz K, Moldenhauer G, Herfarth C, Otto HF, Hammerling GJ, Schlag P (1991) Influence of major histocompatibility complex class I and II antigens on survival in colorectal carcinoma. Cancer Res 51:729
Moore M, Ghosh AK, Jones DJ (1989) MHC status of primary human colorectal carcinoma: biological significance and implications for host immune recognition. Acta Chir Scand Suppl 549:17
Naito Y, Saito K, Shiiba K, Ohuchi A, Saigenji K, Nagura H, Ohtani H (1998) CD8+ T cells infiltrated within cancer cell nests as a prognostic factor in human colorectal cancer. Cancer Res 58:3491
Østenstad B, Lea T, Schlichting E, Harboe M (1994) Human colorectal tumour infiltrating lymphocytes express activation markers and the CD45RO molecule, showing a primed population of lymphocytes in the tumour area. Gut 35:382
Schwartz RH (1990) A cell culture model for T lymphocyte clonal anergy. Science 248:1349
Turnbull RB Jr, Kyle K, Watson FR, Spratt J (1967) Cancer of the colon: the influence of the no-touch isolation technic on survival rates. Ann Surg 166:420
Acknowledgements
The authors thank Mrs. K. Kejling for excellent technical assistance. We also thank the Department of Clinical Immunology, Odense University Hospital, for use of laboratory facilities. This work was supported by the Danish Cancer Society, The P Carl Petersen Foundation, University of Southern Denmark, the Danish Medical Association Research Fund, Lunds Foundation, The Novo Nordisk Foundation and Skovgaards Foundation, Denmark.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Diederichsen, A.C.P., v. B. Hjelmborg, J., Christensen, P.B. et al. Prognostic value of the CD4+/CD8+ ratio of tumour infiltrating lymphocytes in colorectal cancer and HLA-DR expression on tumour cells. Cancer Immunol Immunother 52, 423–428 (2003). https://doi.org/10.1007/s00262-003-0388-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-003-0388-5