Abstract
Purpose
To investigate the value of contrast-enhanced ultrasonography (CEUS) in the differential diagnosis of malignant and benign focal gallbladder diseases confined to the gallbladder wall.
Methods
From July 2006 to May 2016, 88 patients (mean age 48.8 years; age range 18–77 years) were enrolled. All patients had focal gallbladder lesions confined to the gallbladder wall according to CEUS examination. The conventional ultrasound and CEUS characteristics of the lesions were evaluated, and diagnostic performance was evaluated via receiver-operating characteristic (ROC) analysis.
Results
Multiple logistic regression analysis showed that three characteristics, an irregular shape, branched intralesional vessels and hypo-enhancement in the late phase, were features indicating a malignant gallbladder disease (all P < 0.05). When combining any two of these three features, diagnostic specificity improved from 51.5%–77.3% to 92.4% (P < 0.05 for all), and the area under the ROC (AUROC) curve improved from 0.735–0.874 to 0.917, without a significant loss of sensitivity.
Conclusions
CEUS features have greater specificity than those from conventional US for the differentiation of benign and malignant gallbladder diseases confined to the gallbladder wall, without a loss of sensitivity.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Contrast-enhanced ultrasonography (CEUS) has been used for the diagnosis of gallbladder and bile duct diseases and is considered a valuable complement to conventional US [1,2,3,4,5,6]. Preliminary clinical studies have indicated that CEUS shows good diagnostic performance in differentiating malignant from benign tumors in gallbladder disease, and CEUS has been developed as a highly sensitive and accurate diagnostic technique in clinical settings [3,4,5,6,7]. Some CEUS features, such as branched intralesional blood vessels, washout of the contrast agent within 35–60 s and destruction of gallbladder wall integrity [3, 4, 7,8,9,10], seem to be useful clues for differentiating between malignant and benign gallbladder diseases. Among these characteristics, destruction of gallbladder wall integrity shows the best diagnostic performance [4, 7, 11]. However, approximately 20% of gallbladder carcinomas may not destroy the gallbladder wall, which makes a differential diagnosis both challenging and critical [12]. To the best of our knowledge, no studies have evaluated diagnostic performance for gallbladder disease confined to the gallbladder wall. We hypothesized that the use of CEUS features, either alone or in combination with conventional B-mode US features, would improve the accuracy of assessing whether a lesion is malignant, thus improving patient management. The purpose of our study was to retrospectively evaluate the diagnostic performance of CEUS in the differentiation of malignant and benign gallbladder diseases confined to the gallbladder wall.
Materials and methods
Patients
This retrospective study was approved by the research ethics board of our institution, and the need for informed consent was waived. From July 2006 to May 2016, 642 consecutive patients who had suspicious gallbladder tumors were referred for CEUS at our institution. The inclusion criteria were as follows: (a) stationary, focal lesions that protruded into the gallbladder lumen, (b) no infiltration of the gallbladder wall or adjacent liver parenchyma, and (c) confirmed by pathological results after surgery. Patients who showed typical US findings of gallbladder stones, sludge, debris, and small polypoid lesions (≤0.5 cm in diameter), those with a recent coronary syndrome, or those who were pregnant, lactating, or <18 year or >80 year old were excluded from this study. Patients in whom CEUS showed non-enhancement in the three phases that was confirmed to be biliary sludge were also excluded. Of these 642 patients, 554 patients were excluded due to the following reasons: (1) 227 patients did not undergo surgery and did not have pathological results; (2) 92 patients had diffuse thickening of gallbladder wall and without focal lesions; (3) 43 patients had biliary sludge; (4) 192 patients had infiltration of the gallbladder wall and/or invasion of the adjacent liver parenchyma. Finally, 88 patients with gallbladder-confined tumors, which were confirmed by pathological results, were included in this study. Distant diseases, such as lymph node, peritoneal, or liver metastases, were not detected on US imaging in these 88 patients.
The patients included 41 men and 47 women, with a mean age of 48.8 ± 14.5 years (range 18–77 years). In 65 (73.9%) patients, a single lesion was found, whereas in the remaining 23 (26.1%) patients, multiple lesions were detected. In the patients with multiple lesions, generally the largest lesion on US was selected for analysis; however, if the largest lesion was inconspicuous on US, the most conspicuous of the remaining lesions was selected for analysis. Pathological examination revealed 23 cholesterol polyps, 29 adenomas (13 with atypical hyperplasia), 14 adenomyomas, and 22 adenocarcinomas.
Conventional US and CEUS examination
Two US machines were used in this study, depending on the availability of the machine. One machine was an Acuson Sequoia 512 system (Siemens Medical Solutions, Mountain View, Calif.), and the other was an Aplio XV system (Toshiba Medical Systems, Tokyo, Japan). A 4V1 vector transducer with a frequency range of 1–4 MHz was used with the Acuson Sequoia 512 scanner, and a 375BT convex transducer with a frequency range of 1.9–6.0 MHz was used with the Aplio XV scanner. A low mechanical index (MI) contrast-specific imaging mode of contrast pulse sequencing (CPS; MI range 0.15–0.21) was used in the Acuson Sequoia 512 scanner, and contrast harmonic imaging (CHI; MI range 0.08–0.10) was used in the Aplio XV. The contrast agent used in this study was SonoVue (Bracco, Milan, Italy).
Conventional US and CEUS were performed by radiologists with more than five years of experience with liver US and at least two years of experience with CEUS. US examinations were performed according to the following standardized protocol, which was assessed at a consensus meeting prior to the study. Each patient fasted for at least 8 h before the US examination. Initially, the entire gallbladder and adjacent liver parenchyma were thoroughly examined using conventional gray-scale US, and the target lesions were identified. The position, size, shape, echogenicity, and lesion number were evaluated. Color Doppler ultrasound was used to evaluate blood flow in the lesion. After activating the contrast-specific imaging mode, a bolus injection of 2.4 mL of SonoVue was administered intravenously via an antecubital vein, followed immediately by a 5-mL saline flush. A timer was started at the beginning of contrast agent administration, and the lesion was observed continuously for at least 3 min. Another bolus was administered at least 20 min after the first bolus if the initial enhancement was missed or if the target lesion was changed. The gallbladder lesion enhancement process was classified into early (10–30 s after contrast injection) and late phases (31–180 s after contrast injection) because the blood supply of the gallbladder is entirely arterial [13]. Baseline US images and those from the entire early and late phases were stored digitally on the hard disk of the imaging system and were transferred to a personal computer for subsequent analysis.
Image analysis
The images from conventional US and CEUS were analyzed according to the consensus of two experienced investigators (M.X.L. and W.W.) who had more than 8 years US and CEUS experience. These investigators were not involved in the US and CEUS examinations and were unaware of the clinical histories, histopathological results and other imaging findings of the patients. The two investigators initially read the images independently; if there was any disagreement, the images were re-reviewed, and a determination was reached by consensus.
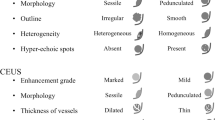
Patient demographic data, including age and gender, were collected. The following conventional US features of the gallbladder lesions were documented: diameter, number, echogenicity relative to the gallbladder wall (hyperechoic, isoechoic, hypoechoic, or mixed), shape (regular or irregular) (Fig. 1), and features of the base of the lesion (<1/2 the diameter of the tumor or >1/2 the diameter of the tumor). Color Doppler imaging was then used to assess the vascularity of the lesion, which was classified as abundant, scarce, or none.
Gallbladder lesion shape. A A 47-year-old woman referred for medical examination in our hospital. Conventional US showed an irregular gallbladder lesion (arrows). The pathologic diagnosis was gallbladder adenocarcinoma. B A 40-year-old woman had occasional epigastric pain. Conventional US showed a regular lesion in the gallbladder (arrows). The pathologic diagnosis was cholesterol polyps
On CEUS images, intralesional vascularity during the early phase was categorized as dotted (when the artery was short and speckled), linear (when the artery was continuous and had no branches) or branched (when the artery was branched) (Fig. 2). The degree of enhancement of the lesion was determined in reference to that of the adjacent liver parenchyma at the same depth and was categorized as non-, hypo-, iso-, or hyper-enhancement. The greatest enhancement of the lesion was considered if different enhancement levels were present, and enhancement patterns were divided into homogeneous and heterogeneous enhancement. Homogeneous enhancement indicated that all components of the lesion were enhanced to the same extent, and heterogeneous enhancement indicated that variable enhancement patterns were seen in different components of the lesion. Gallbladder wall integrity beneath the lesion was depicted using conventional US and CEUS. Gallbladder wall visualization was categorized as distinct or indistinct. Wall destruction or intactness was defined according to whether the outer layer of the gallbladder wall was incomplete or continuous. The time at which contrast agent appeared in the lesion and the times at which “iso-enhancement” and “hypo-enhancement” were first noticed by the observers were recorded.
Intralesional blood vessels in gallbladder lesions on CEUS (arrows). A A 20-year-old man had occasional epigastric pain. The CEUS image shows dotted blood vessels (arrowheads). The pathologic diagnosis was cholesterol polyps. B A 58-year-old woman was referred for medical examination, and the gallbladder lesion was found by chance. The CEUS image shows linear blood vessels in the lesion (arrowheads). The pathologic diagnosis was adenoma. C A 58-year-old man with a gallbladder lesion found by physical examination and who received further inspection at our institution. The CEUS image shows branched blood vessels in the lesion (arrowheads). The pathologic diagnosis was adenocarcinoma
Statistical analysis
Continuous data are expressed as the mean ± standard deviation. Independent t tests was applied to evaluate the differences between benign and malignant gallbladder diseases in terms of patient age, the size of the lesion, the time of initial enhancement of the lesion, and the washout time in the lesion. Chi-squared tests were applied to evaluate the differences between benign and malignant gallbladder diseases in terms of echogenicity, intralesional vascularity on conventional US, and the extent and pattern of enhancement on CEUS. A two-tailed P value <0.05 was considered statistically significant. Multiple logistic regression analyses were performed to select the independent variables from the patients’ features, as well as the US and CEUS features that were associated with the dependent variable. The independent variables are listed in Table 1. A forward stepwise selection method was used. The independent variables with P values <0.05 in the multiple logistic regression analyses were selected for the ROC curve analysis. Sensitivity, specificity, positive predictive value (PPV), negative predictive value (NPV), accuracy and the AUROC were calculated. Differences in sensitivity, specificity, and accuracy were compared using the McNemar test. Differences in the AUCs were assessed using the method described by Hanley and Mc-Neil [14]. Statistical analyses were performed with the SPSS 19.0 software package (SPSS, Chicago, IL.)
Results
The mean age of the patients with gallbladder carcinoma (56.3 years; range 34–75 years) was significantly different from the mean age of patients with benign gallbladder disease (45.8 years; age 18–77 years) (P = 0.031; Table 1). There were no significant differences between malignant and benign gallbladder diseases regarding patient gender (P = 0.064; Table 1).
Conventional US characteristics
The mean diameter of gallbladder adenomas was 3.4 ± 1.4 cm (range 1.3–7.5 cm), while the mean diameter of benign gallbladder diseases was 2.2 ± 0.9 cm (range 0.4–6.0 cm; P < 0.001; Table 1). The features of an irregular type and lesions with a base >1/2 of the lesion diameter were more commonly found in malignant gallbladder diseases (P < 0.001; Table 1). There were significant differences in lesions regarding intralesional flow signals on color Doppler imaging between malignant and benign gallbladder diseases (P < 0.001; Table 1).
CEUS features
During the early phase, intralesional blood vessels were more often branched or linear in malignant gallbladder diseases, whereas they were more frequently dotted in benign diseases (P < 0.001; Table 1). There were no significant differences between malignant and benign gallbladder diseases in the enhancement pattern and enhancement extent of lesions during the early phase (all P > 0.05; Table 1). However, during the late phase, the enhancement extent of almost half lesions appeared as iso-enhancement in benign gallbladder diseases (47.0%, 31/66) (Fig. 3) and most lesions showed hypo-enhancement in malignant gallbladder diseases (95.5%, 21/22) (Fig. 4). Contrast arrival time, time to iso-enhancement, and time to hypo-enhancement, however, showed no significant differences between the two groups (Table 1).
Images from a 58-year-old man with gallbladder adenocarcinoma. A US exhibited a hypoechoic lesion sized 4.8 cm in diameter (arrow). B In the early phase of CEUS (23 s), the gallbladder lesion (arrow) showed homogeneous hyper-enhancement. Branched blood vessels in the lesion were detected (arrowheads). C The lesion (arrow) showed hypo-enhancement at 87 s after contrast agent injection and showed continuous hypo-enhancement during the late phase
Multivariate analysis of US and CEUS characteristics
All independent variables that were significantly different (as shown in Table 1) were submitted to multiple logistic regression analyses. The results show that an irregular shape (OR 18.56), branched intralesional vessels (OR 0.007) and hypo-enhancement in the late phase (OR: 0.003) were associated with a malignant gallbladder disease (all P < 0.05; Table 2).
Diagnostic performance
Because the features of an irregular shape, branched intralesional vessels on CEUS, and hypo-enhancement in the late phase had the highest association with malignant tumors, they were selected to assess diagnostic performance. Combining the significant features of US and CEUS, we developed a set of diagnostic criteria, which included the combination of any two features, to predict the malignancy of gallbladder-confined tumors. The specificity of the combinational diagnostic criteria was 92.4% (61 of 66), which was significantly higher than the specificity of any single feature (P < 0.05 for all; Table 3). There were no changes in sensitivity (P > 0.05 for all; Table 3). The AUROC of the combinational diagnostic criteria was higher than the AUROC of shape or extent of enhancement in late phase (0.917 vs. 0.788 and 0.735, respectively, both P < 0.05; Table 3; Fig. 5).
Discussion
Clinical stage is one of the main prognostic factors for gallbladder carcinoma [15, 16]. Patients with a disease at a localized stage have much higher survival rates (TNM Stages I and II have a five-year survival rate of 91% and 85%, respectively) than those with regional or distant metastasis (Stages III and IV, 40% and 19%, respectively) [17]. Therefore, the early diagnosis and treatment of gallbladder carcinoma are crucial and significant. Previous studies have shown that once the lesion destroys the gallbladder wall beneath the lesion or even infiltrates the adjacent liver tissue, the specificity of using CEUS in diagnosing malignancy reaches 93%–100% [4, 7, 11, 18]. However, for a lesion where the gallbladder wall is intact, making a differential diagnosis is still difficult. In trying to address this situation, our study found that combinations of US and CEUS features were useful to radiologists when differentiating gallbladder-confined carcinoma from a benign gallbladder disease.
In the present study, combination of US and CEUS features of gallbladder masses significantly improved the specificity of diagnoses without a loss of sensitivity. When combining any two of the three conditions (shape on US; intralesional vessels and extent of enhancement in the late phase on CEUS), the specificity improved from 51.5%–77.3% to 92.4%, and the AUROC reached 0.917. Meanwhile, diagnostic sensitivity remained at 90%. CEUS has been suggested to be helpful in identifying malignant lesions from gallbladder masses confined to the gallbladder wall. In many previous studies, an improvement in diagnostic performances occurred when adding CEUS to increase the specificity in discriminating malignant from benign lesions [7, 19].
In this study, we found that the US and CEUS features which could be used to distinguish malignant from benign masses were an irregular shape, branched intralesional vessels and hypo-enhancement in the late phase. In contrast, benign gallbladder diseases, such as cholesterol polyps, mostly had a regular shape, dotted intralesional vessels and iso-enhancement in the late phase. The morphology of benign gallbladder lesions, such as cholesterol polyps, is mostly regular in shape, but malignant lesions generally have an irregular shape. This characteristic is similar to tumors in other organs [18]. This view is supported by our study. Our research shows that branched intralesional vessels on CEUS were an indicator of malignancy. Similar to malignancies in other organs, most gallbladder carcinomas are hyper-vascular. Aggressive tumor cells form channels that may function as blood vessels to transport oxygen and nutrients [20]. Therefore, we can observe more branched vessels in malignant gallbladder diseases on CEUS imaging. Some previous literature [3, 21,22,23] has also proposed that branched intralesional vessels on CEUS are possible characteristics of gallbladder malignancy. Therefore, intralesional vessels play an important role in making differential diagnosis of benign and malignant gallbladder diseases.
In the present study, malignant gallbladder lesions showed hyper-enhancement in the early phase that then faded to hypo-enhancement in the late phase, which is similar to hepatocellular carcinoma. However, we did not find a discrepancy in the washout times of the contrast agent from the time of administration between gallbladder carcinomas (59.7 ± 33.7 s) and benign diseases (70.7 ± 32.9 s; P = 0.233). Our previous study [7] reported that rapid wash-out of the contrast agent within 35 s after administration may be a key predictor of malignant gallbladder diseases. This discrepancy between the studies may be explained by the differences in the patient populations, such as clinical stage and tumor size. In the present study, we only included patients with gallbladder carcinoma without destruction of the gallbladder wall, which can be classified as early-stage gallbladder carcinoma.
It should be specifically mentioned that adenomas are regarded as pre-malignant and should be managed with cholecystectomy, while polyps and adenomyomas can be treated conservatively and followed up with serial US. In our study, 29 cases involved adenomas, and most of them showed a regular shape (72.4%, 21/29), dotted intralesional vessels (75.9%, 22/29), and hypo-enhancement in the late phase (55.1%, 16/29). Further study is needed to distinguish adenomas from other benign gallbladder lesions.
Our study had several limitations. First, our comparative analysis was retrospective. Our sample size was not large enough to show benefits in some of the subgroup analyses. Second, patients were not strictly asked to hold their breath when they underwent CEUS examination. Respiratory movement would affect the results of a quantitative analysis; therefore, we did not perform a time intensity curve analysis. The observed enhancement pattern on CEUS was a subjective judgment based on visual assessments; however, quantitative analyses of time intensity curves may be helpful in future studies. Third, cholecystitis or an abscess with perforation may also present as an interruption of the gallbladder wall; therefore, discontinuity of the gallbladder wall cannot be considered as the only diagnostic indicator of malignancy in these cases. Fourth, the Aplio XV system obtains low-MI images with harmonic filtering, and, unlike in phase inversion with tissue subtraction, satisfactory background tissue subtraction is not achieved. Therefore, lesion echogenicity relative to the liver may be affected by background liver tissue echogenicity. Fifth, the vascular morphology may appear as linear or dotted depending on whether it is viewed in the long or short axis on two-dimensional CEUS images. This may affect the radiologist’s judgment of the vascular pattern. Three-dimensional CEUS may provide more information to accurately assess intralesional vascularity.
In conclusion, the use of CEUS could improve diagnostic specificity in focal gallbladder tumors confined to the gallbladder wall, without a loss in sensitivity, but further prospective validation is needed.
References
Wang W, Fei Y, Wang F (2016) Meta-analysis of contrast-enhanced ultrasonography for the detection of gallbladder carcinoma. Med Ultrason 18:228–281. doi:10.11152/mu.2013.2066.183.wei
Tang S, Huang L, Wang Y, Wang Y (2015) Contrast-enhanced ultrasonography diagnosis of fundal localized type of gallbladder adenomyomas. BMC Gastroenterol 15:99. doi:10.1186/s12876-015-0326-y
Gerstenmaier JF, Hoang KN, Gibson RN (2016) Contrast-enhanced ultrasound in gallbladder disease: a pictorial review. Abdom Radiol 41:1640–1652. doi:10.1007/s00261-016-0729-4
Liu LN, Xu HX, Lu MD, et al. (2012) Contrast-enhanced ultrasound in the diagnosis of gallbladder diseases: a multi-center experience. PLoS ONE 7:e48371. doi:10.1371/journal.pone.0048371
Badea R, Zaro R, Opincariu I, Chiorean L (2014) Ultrasound in the examination of the gallbladder—a holistic approach: grey scale, Doppler, CEUS, elastography, and 3D. Med Ultrason 16:345–355. doi:10.11152/mu.201.3.2066.164.rbrz
Zheng SG, Xu HX, Liu LN, et al. (2013) Contrast-enhanced ultrasound versus conventional ultrasound in the diagnosis of polypoid lesion of gallbladder: a multi-center study of dynamic microvascularization. Clin Hemorheol Microcirc 55:359–374. doi:10.3233/ch-121651
Xie XH, Xu HX, Xie XY, et al. (2010) Differential diagnosis between benign and malignant gallbladder diseases with real-time contrast-enhanced ultrasound. Eur Radiol 20:239–248. doi:10.1007/s00330-009-1538-8
Xu HX (2009) Contrast-enhanced ultrasound in the biliary system: potential uses and indications. World J Radiol 1:37–44. doi:10.4329/wjr.v1.i1.37
Liu XS, Gu LH, Du J, et al. (2015) Differential diagnosis of polypoid lesions of the gallbladder using contrast-enhanced sonography. J Ultrasound Med 34:1061–1069. doi:10.7863/ultra.34.6.1061
Si Q, Qian XL, Wang F, et al. (2013) Real-time grey scale contrast-enhanced ultrasonography in diagnosis of gallbladder cancer. Ultrasound Med Biol 39:S86
Sun LP, Guo LH, Xu HX, et al. (2015) Value of contrast-enhanced ultrasound in the differential diagnosis between gallbladder adenoma and gallbladder adenoma canceration. Int J Clin Exp Med 8:1115–1121
Kiran RP, Pokala N, Dudrick SJ (2007) Incidence pattern and survival for gallbladder cancer over three decades–an analysis of 10301 patients. Ann Surg Oncol 14:827–832. doi:10.1245/s10434-006-9224-4
Spârchez Z, Radu P (2012) Role of CEUS in the diagnosis of gallbladder disease. Med Ultrason 14:326–330
Hanley JA, McNeil BJ (1983) A method of comparing the areas under receiver operating characteristic curves derived from the same cases. Radiology 148:839–843. doi:10.1148/radiology.148.3.6878708
Lazcano-Ponce EC, Miquel JF, Muñoz N, et al. (2001) Epidemiology and molecular pathology of gallbladder cancer. CA Cancer J Clin 51:349–364. doi:10.3322/canjclin.51.6.349
Gourgiotis S, Kocher HM, Solaini L, et al. (2008) Gallbladder cancer. Am J Surg 196:252–264. doi:10.1016/j.amjsurg.2007.11.011
Tsukada K, Hatakeyama K, Kurosaki I, et al. (1996) Outcome of radical surgery for carcinoma of the gallbladder according to the TNM stage. Surgery 120:816–821. doi:10.1016/S0039-6060(96)80089-4
Yuan HX, Cao JY, Kong WT, et al. (2015) Contrast-enhanced ultrasound in diagnosis of gallbladder adenoma. HBPD Int 14:201–207. doi:10.1016/s1499-3872(15)60351-4
Forner A, Vilana R, Ayuso C, et al. (2008) Diagnosis of hepatic nodules 20 mm or smaller in cirrhosis: prospective validation of the noninvasive diagnostic criteria for hepatocellular carcinoma. Hepatology 47:97–104. doi:10.1002/hep.21966
Bian XW, Chen JH, Jiang XF, et al. (2004) Angiogenesis as an immunopharmacologic target in inflammation and cancer. Int Immunopharmacol 4:1537–1547. doi:10.1016/j.intimp.2004.07.017
Inoue T, Kitano M, Kudo M, et al. (2007) Diagnosis of gallbladder diseases by contrast-enhanced phase-inversion harmonic ultrasonography. Ultrasound Med Biol 33:353–361. doi:10.1016/j.ultrasmedbio.2006.09.003
Numata K, Oka H, Morimoto M, et al. (2007) Differential diagnosis of gallbladder diseases with contrast-enhanced harmonic gray scale ultrasonography. J Ultrasound Med 26:763–774. doi:10.7863/jum.2007.26.6.763
Tsuji S, Sofuni A, Moriyasu F, et al. (2012) Contrast-enhanced ultrasonography in the diagnosis of gallbladder disease. Hepato-Gastroenterology 59:336–340. doi:10.5754/hge11447
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
Science and Technology Planning Project of Guangdong Province, China (2012B031800459). National Natural Science Foundation of China (81601500). Natural Science Foundation of Guangdong Province, China (2016A030310143).
Conflict of interest
All the authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards. For this type of study, formal consent is not required.
Informed consent
A waiver of informed consent was obtained from the institutional review board as this was a retrospective study and all patients underwent CEUS as part of their clinical work-up.
Rights and permissions
About this article
Cite this article
Zhuang, B., Li, W., Wang, W. et al. Contrast-enhanced ultrasonography improves the diagnostic specificity for gallbladder-confined focal tumors. Abdom Radiol 43, 1134–1142 (2018). https://doi.org/10.1007/s00261-017-1268-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-017-1268-3