Abstract
Purpose
To describe the natural history of liver adenomatosis (LA), including complications and changes in lesion size over time.
Materials and methods
Eighteen patients with clinical diagnosis of LA were included. Clinical and biochemical information were collected. The initial and follow-up MR studies were reviewed retrospectively to determine change in lesion size and imaging features.
Results
Seventeen patients were women (94.4%). The mean age of the initial MR study was 37.0 years (18–52 years). The median size of the largest lesion was 6.7 cm (range 3.0–13.5 cm). Intratumoral bleeding was detected on MRI in 9 lesions, in 7 patients (38.8%). The median size for hemorrhagic lesions was 7.6 cm (range 4.1–13.5 cm). During the mean follow-up period of 29.4 (range 4–98) months, 10 patients had stable disease (55.6%), and 8 patients had tumor regression (44.4%). Of 8 patients who were followed without intervention, 3 patients (37.5%) had spontaneous regression. No malignant transformation or lesion progression was occurred.
Conclusion
During an over 2-year follow-up period, the majority of lesions of LA appeared to remain stable or showed tumor regression. Spontaneous tumor regression can be observed in approximately 37% of individuals in the age range of 28–53 years.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Hepatocellular adenoma (HCA) is an uncommon benign neoplasm of the liver, generally occurring in women in their reproductive years taking oral contraceptives (OC). Most HCAs are solitary, but occasionally more than 1 nodule can be seen [1].
Flejou et al. [2] described liver adenomatosis (LA) as a clinical entity distinct from isolated hepatocellular adenoma in 1985. This entity is characterized by the presence of multiple adenomas (arbitrarily, more than 10), otherwise in normal liver parenchyma, and they observed lack of correlation with steroid medication or contraceptives use, and with equal sex distribution. During the past 10 years, great progress has been made concerning HCA and LA is not a specific entity as thought before [3].
HCAs and LA are usually asymptomatic, but large nodules may present with abdominal pain due to hemorrhage or rupture. Another reported complication is malignant transformation. The risk of lesion rupture and malignant transformation has been reported as 21–25% and 4–8%, respectively [1, 4]. The risk of rupture correlates with increasing tumor size and surgical intervention is recommended in any tumor >4 cm. [4].
To our knowledge, little is known about the natural history and maturation course of LA. Although there were a few reports showing regression in tumor size after cessation of OC use [1, 3] and also regression of LA following androgenic progestin therapy withdrawal [5]; however, this has not been a consistent observation and those series usually included both single and multiple HCAs. One series of six patients of LA showed that 43% of smaller tumors continued to grow during follow-up and tumor regression was observed in four patients [6].
The purpose of our study is to describe the natural history of LA, including complications and changes in lesion size and MRI features
Materials and methods
Patients
This retrospective study was approved by our institutional review board, and informed consent was waived.
To accrue patient, we reviewed the databases of the Department of Pathology and Internal medicine, Division of Gastroenterology and Hepatology, from January 1, 2002 to June 30, 2012. Twenty patients with a diagnosis of LA were identified. Patients were only included in the study, if they had at least 2 available MR or CT studies as initial study and follow-up. Two patients were excluded on the basis of having only 1 MR study and no CT or MRI to follow-up. Eighteen patients were thus included in our study. All patients had at least 2 MR studies, as initial and follow-up, except for one patient (subject 9) who had CT at the time of presentation and MR as a follow-up study. The diagnosis of LA was confirmed based on a combination of clinical, imaging studies, and histological evaluation in 14 patients (subjects 1–13 and 18 in Table 1), and by a combination of clinical, characteristic imaging findings and imaging follow-up in four patients (subjects 14–17 in Table 1). Among 4 patients who did not have pathological diagnosis, two patients (subject 16–17 in Table 1) had at least 1 MR study using gadoxetic acid (Eovist, Bayer Healthcare) as a contrast agent with acquisition of a delayed hepatobiliary phase at 20 min after contrast infection, that showed no uptake of contrast agent and had follow-period at 36, 13, and 6 months, another patient with a history of OCs use presented with subcapsular hepatic hemorrhage on initial MR study, and had follow-up period at 12 months (subject 15 in Table 1), the last patient had a 17-year history of OCs use and had follow-up period at 88 months (subject 14 in Table 1).
Clinical and radiological data were retrospectively reviewed and analyzed. The clinical and biochemical information collected included sex, age, steroid medication or oral contraceptive use, clinical presentation, BMI, liver function test. Immunohistochemical analysis was not performed in all patients.
Imaging evaluation
Two radiologists (Saowanee Srirattanapong and Bong Soo Kim) with 5 and 10 years of abdominal MRI experience retrospectively reviewed the studies on a picture archiving and communication system (PACS) workstation in consensus with knowledge of the diagnosis of LA. The following features were evaluated: the number of lesions, the longest dimension of the largest lesion in the axial plane, signal intensity of the lesions on unenhanced T1- and T2-weighted images and contrast enhanced T1-weighted images when compared with that of the surrounding liver parenchyma using a 4-point gray scale (hypointense, isointense, slightly hyperintense, and markedly hyperintense), evidence of lesional hemorrhage as hyperintesity on both T1- and T2-weighted images or evidence of ruptured tumor as perilesional or perihepatic fluid collection or focal areas of low signal intensity on the T2-weighted images that suggested hemosiderin deposition, size of hemorrhagic lesion, presence of liver steatosis and presence of microscopic intralesional fat as observed by signal dropout on opposed phase T1-weighted gradient echo imaging. On T2-weighted images, the signal was considered markedly hyperintense if it was at least as intense as the spleen signal. If hemorrhagic or necrotic component was found in the lesion, only the nonhemorrhagic or non-necrotic tissue of the lesion was taken into account for signal intensity evaluation. On follow-up studies, changes in lesion number, size, and signal intensities were evaluated. If the largest tumor was surgically resected on the follow-up study, then another next largest lesion on the initial study was selected to evaluate change in lesion size.
The criterion for tumor regression was based on the decrease in diameter of the largest lesions between the first imaging study and the last follow-up. Criteria for tumor progression included an increase in diameter of the largest lesion or increase in number of the hepatic lesions. Stable disease was considered when neither tumor progression nor regression criteria were met.
MRI technique
MRI of the abdomen was performed with 1.5-T (Vision, Sonata or Avanto, Siemens Health care, Malvern, PA) and 3.0-T MRI systems (Trio, Siemens Healthcare, Malvern, PA, USA) using a phased-array torso coil. All MR imaging examinations were performed with the following protocol (Table 2): transverse and coronal T1-weighted spoiled gradient-echo (SGE); transverse T1-weighted dual echo in-phase and out-of-phase SGE; T2-weighted sequence that included a fat-suppressed half-Fourier rapid acquisition with relaxation enhancement (HASTE) sequence in the transverse and coronal planes.
Gadobenate dimeglumine (MultiHance, Bracco Diagnostics, Princeton, NJ, USA) at a dose of 0.05 mmol/kg or gadodiamide at a dose of 0.1 mmol/kg (Omniscan, GE Healthcare, Princeton, NJ, USA) or 0.025 mmol/kg of gadoxetate disodium (Gd-EOB-DTPA or Eovist/Primovist, Bayer Health care) were administered IV as a power-injected (Spectris Solaris EP, Medrad, Pittsburg, PA, USA) bolus at 2 mL/s in all patients followed by a bolus of 20 mL of saline flush. Gadobenate dimeglumine has replaced gadodiamide in all gadolinium-enhanced MR studies of patients beginning in June 2007.
For the contrast enhanced series, phase-encoding steps were acquired with sequential ordering, and the center of k space was in the range of 8–10 s from the start point of the acquisitions. The method of contrast enhanced imaging changed during the course of the study. For the past 2 years after 2010, after acquisition of unenhanced MR images, timing for the contrast-enhanced hepatic arterial dominant phase used bolus-tracking technique (CARE Bolus software; Siemens Medical Solutions) with the following approach: the contrast agent was monitored by the technologist as it traveled through the vascular system. After the visual enhancement of contrast in the descending aorta, patients were instructed to suspend breathing for 8-s and the liver was imaged thereafter. In prior years, an empiric timing method was employed with the data acquisition initiated 18 s after the start of contrast administration. The second pass was obtained 45–90 s postcontrast administration early hepatic venous phase. The third pass was the interstitial phase, which was obtained from 100 to 180 s following contrast injection. The duration of the entire study was 10 years; as a consequence contrast-enhanced GRE sequence had different slice thickness through this study period. Earlier data had thicker section acquisition on older systems (8 mm for 2D-GRE and 3 mm for the 3D-GRE). In the study using Gd-EOB-DTPA, an additional data acquisition at 20 min after injection of the contrast medium was obtained.
Results
Eighteen patients, 17 women, with a mean age at diagnosis of 37.0 years (age range, 18–52 years) were included in the study. None had a history of chronic liver disease. 15/17 women (88.2%) had a history of OC use, with 12 having data available regarding the duration of OC usage (mean 14.8 years, range of duration 8–35 years). The mean BMI at diagnosis was 32.2 kg/m2 (range 23.6–52.7 kg/m2). The majority of patients (12/18 patients, 66.7%) were obese (BMI > 30 kg/m2). The clinical manifestations of LA observed were asymptomatic (10/18 patients, 55.5%), chronic abdominal pain (4/18 patients, 27.7%) and acute abdominal pain (3/18 patients, 16.5%). LFTs had abnormal elevation of AST/ALT and/or ALP in 10 patients (55.5%). AFP levels were available in 15 cases and were normal in all of these patients (Table 1).
The detailed MRI findings in 18 patients with LA are summarized in Table 3. The number of lesions per patient was greater than 10 the majority of patients, only two patients had less than 5 lesions (subject 17 and 18). The median size of the largest lesion was 6.7 cm (range 3.0–13.5 cm). Tumoral hemorrhage was detected on MRI in 9 lesions in 7 patients (38.8%). One patient had tumoral hemorrhage with subcapsular hepatic hematoma. The median size for hemorrhagic lesions was 7.6 cm (range 4.1–13.5 cm). Hepatic steatosis was noted in 13 patients (72.2%), and the presence of MR-detected microscopic intralesional fat was noted in lesion in 5 patients (27.8%).
Most of the lesions were isointensity on T1-weighted images (83%). On T2-weighted images, 55% of lesions were slightly hyperintensity, 39% were isointensity, and 6% were hypointense compared to liver parenchyma. On the arterial phase, 94% appeared hyperintense. On portal venous phase, 67% were hyperintensity and 33% were isointensity. On the interstitial phase, 44% remained hyperintense, 50% showed isointensity, and only one patient showed hypointensity compared to adjacent liver parenchyma.
Management and follow-up
All patients (15/17), who were taking OC at presentation, discontinued their use. Eight patients underwent MR follow-up without intervention. Among these 8 patients, one patient (subject 15) had one lesion with intralesional hemorrhage and subcapsular hematoma. During hospitalization (6 days) the patient required narcotic medication for pain control and remained hemodynamically stable, not requiring blood transfusions. At 12-month follow-up period, the lesions showed a combination of stability and decrease in size. In subject 1, the largest tumor (8.0 cm), was considered for resection, but at laparoscopy the multiplicity and diffuse liver involvement obviated resection. At 31-month follow-up period, the lesions remained stable. In subject 7, resection of the largest lesion (13.1 cm) was also considered, but the patient preferred to undergo follow-up with reevaluate after stopping OC. At 33-month follow-up period, the lesion decreased to 8.2 cm. In subject 11, the largest tumor (5 cm) evidenced minimal intratumoral hemorrhage. The patient was asymptomatic and opted to wait and undergo imaging re-evaluation. Following cessation of OC use, the largest lesion decreased to 3.1 cm at 12-month follow-up. In subject 12, the largest tumor was 5.3 cm; this individual continued her follow-up care at another hospital for a number of and eventually returned to our center and at 98-month follow-up, the tumors remain stable.
Nine patients underwent surgical resection of a lesion greater than 4 cm in diameter, with 6/9 of these patients having evidence of tumoral hemorrhage. Transcatheter arterial embolization (TAE) was performed in two patients. One of two patients (subject 3) underwent TAE 2 years after resection of the largest tumor in the left lobe, but a large lesion, >4 cm, was left behind in right hepatic lobe. The other patient (subject 4) underwent TAE alone, due to the high risk of surgery.
Over the mean follow-up period of 29.4 (4–98) months, 10 patients had stable disease (55.6%), and 8 patients had tumor regression (44.4%). All 8 of these latter patients were imaged 10–72 months after the initial MRI. There was no development of tumor bleeding or rupture, malignant transformation, or death during the follow-up period. Among patients with lesion regression: one patient had TAE after surgical resection and showed significant decrease in size of the remaining lesions at 72 months follow-up (subject 3); one patient had undergone TAE and showed substantial lesion necrosis with decrease in size of the lesion at 10 months follow-up (subject 4); two patients had significantly decreased tumor size of the remaining lesions, after surgical resection of the largest lesion at 12 and 19 months follow-up (subject 5 and 10); and four patients had spontaneous regression, without any surgical intervention, at 32, 4, 12, and 12 months follow-up at age 28, 51, 53, and 41 years old (subject 7, 9, 11, and 15). Of eight patients who were followed without intervention: three patients (37.5%) had spontaneous regression, and five patients (62.5%) had stable disease. No cases of lesion progression or malignant transformation were observed.
The signal intensity features and enhancement pattern of all lesions did not show any substantial change except for post TAE in one patient, which showed significantly decreased tumor enhancement associated with necrosis.
Discussion
HCAs usually arise in women associated with OCs use, while in men it is often associated with use of anabolic steroids. Most often these lesions present as a solitary hypervascular mass; occasionally they present as multiple lesions and uncommonly they may present with hemorrhage and/or rupture, and rarely they may be associated with malignant degeneration [7]. On initial radiologic work up, it may be difficult to differentiate these lesions from other hypervascular masses.
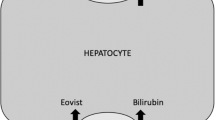
In a patient without underlying liver disease or known primary tumor, HCAs and focal nodular hyperplasia (FNH) must be considered in the differential diagnosis of hypervascular masses. Gadobenate dimeglumine and Gadoxetic acid disodium both show hepatocellular uptake, which is useful to distinguish FNHs (which show uptake) and HCAs (which do not). There does not appear to be differences between solitary HCAs and LA, such that lesions in LA also do not show uptake. Uptake of these agents is dependent on specific the level of membrane transporter expression, present for FNH and absent for HCA, which accounts for their differentiation at hepatocellular phase imaging [8].
The different molecular pathways that contribute to tumor development has recently been described and led to a new classification of HCAs into at least 3 subtypes [9]: HCAs associated with HNF1A gene (also known as transcription factor-1 gene), HCAs associated with β-cantenin gene, and inflammatory HCAs. HCAs without any of above mentioned genotypic marker were considered unclassified subtype [10, 11]. Each HCA subtype is potentially associated with different risk factors [12]. HCAs associated with β-cantenin gene have a higher risk of malignant transformation [3, 10].
A series by Laumonier et al. [12] observed that there were two MR imaging features of HCAs, that were either closely associated with HNF1A or with inflammatory HCAs. They described that for the diagnosis of HCA associated with HNF1A, the positive predictive value of homogeneous signal dropout on chemical shift images was 100%, the negative predictive value was 94.7%, the sensitivity was 86.7% and specificity was 100%. For the diagnosis of inflammatory HCAs, marked hyperintensity on T2-weighted sequences, associated with delayed persistent enhancement, had a positive predictive value of 88.5%, a negative predictive value of 84%, sensitivity of 85.2%, and specificity of 87.5%. Therefore, HCAs that either HNF1A associated subtype or inflammatory subtype were associated with specific MRI patterns related to diffuse fat content or sinusoidal dilatation, respectively. Furthermore, a recent study by Ronot et al. [13] reported a high specificity of MRI findings for the diagnosis of telangiectatic/inflammatory and steatotic HCAs that were 88.9% and 100%, respectively. They demonstrated that radiologists correctly classified HCAs in 85%, the interobserver kappa correlation coefficient was 0.86; whereas routine histological analysis led to a 76.6% correct classification, which improved to 81.6% when immunophenotypical characteristics were available. Immunohistochemical analysis was not performed in our study, thus we cannot evaluate our sensitivity and specificity of these features.
In our study, we measured the largest lesion of each patient as a reference for study; however, the overall lesions in each patient also had been stable or decreased size as well, and no increased size of the tumor was seen. We observed that over a mean of more than 2-year follow-up period, the lesions in many of our patients (10/18, 56%) appeared to remain stable; however, overall tumor regression was observed in 8/18 patients (44%) who either had partial resection or no intervention. Spontaneous regression in patients without any intervention was observed in 3/8 patients (37.5%), who were aged 28–53 years. Dokmak et al. [1] found that 4% of 45 patients (age 37–59) with single and multiple HCAs had regression or disappearance of HCAs after a follow-up period of 130 months, whereas increased tumor size was seen in 9 (8%) patients. These latter were a younger cohort of subjects (age 19–49). The difference in percentage of spontaneous regression compared to our series may be due to the small number of patients in both series, and perhaps differences in patient selection. One study by Bioulac-Sage et al. [3] showed that the majority of HCAs (usually small in size) in patient who were taken off OCs remained stable and in general did not grow, but disappeared in a small percentage of cases. They observed that inflammatory HCAs may disappear more rapidly than other types (Figs. 1, 2, 3, 4).
An 18-year-old male with history of moderate mental retardation who was found to have elevated liver function tests. A Axial T2-weighted image shows two circumscribed slightly hyperintense lesions in the posterior right lobe. B Arterial phase post contrast image shows diffuse enhancement of these two hepatic lesions with fading on C interstitial phase image. A percutaneous core biopsy of the anterior lesion was performed and proven to be adenoma. He subsequently underwent TAE of the right hepatic masses. Follow-up MR study was performed 3 months after TAE. D Axial T2-weighted image shows necrotic change of the anterior mass which is T2 hyperintense and shows lack of contrast enhancement on post contrast E arterial phase, and F interstitial phase images. The more posterior mass remains enhanced on the arterial phase and fades on later phase. This case demonstrates LA in a young male with tumor necrosis and decreased size 3 months post TAE.
A 25-year-old woman with a 10-year history of oral contraceptive use who presented with mild elevated alkaline phosphatase level. A Coronal and B axial T2-weighted images with fat suppression show a bulging contour of left hepatic lobe due to large masses which are heterogeneous and mildly T2 hyperintense. C–F MRI follow-up, 32 months later, after discontinued OC use. C Coronal and D axial T2-weighted images show substantial decrease in size of masses in the left lobe and caudate lobe and decreased bulging contour of the left hepatic lobe. E Axial post-contrast arterial phase image shows enhancement of the masses in the left lobe, caudate lobe, and also small lesion in the right lobe. F Axial T1-weighted interstitial phase image shows fading of the enhancing masses to isointensity. This case demonstrates spontaneous decreased size of tumors after a 32-month follow-up, without any intervention.
A 29-year-old woman with an 8-year history of oral contraceptive use. Multiple hepatic lesions were incidentally discovered when she underwent work up for hypertension. A Coronal and B, C axial T2-weighted images show multiple circumscribed hyperintense masses in the liver. D, E Post-contrast arterial phase images show intense enhancement of the masses with persistent enhancement in the later phase. F The large mass in left hepatic lobe was subsequently resected and proven to be an adenoma. The patient underwent TAE of the right hepatic lesions 2 years after surgery. G–J MRI performed 22 months after TAE. G, H Post-Gd-EOB arterial phase images show diffuse enhancement and decreased size of the large lesion in the posterior right lobe. Note an additional two well defined enhancing lesions in the remaining left lobe. I, J Delayed 20 min post-Gd-EOB images show no uptake of Gd-EOB within the large lesion in right hepatic lobe and smaller lesions in the remaining left lobe. This case demonstrates decreased tumor size after resection of a dominant mass followed by TAE after a 72-month follow-up.
A 40-year-old woman presented with acute right upper quadrant pain. She had an 18-year history of oral contraceptive use. A, B Axial T1-weighted images with fat suppression show evidence of hyperintense subcapsular hematoma along the lateral aspect of the right lobe. A large mass of heterogeneous mild T1-hyperintensity is noted abutting the subcapsular hematoma. C Post-contrast-arterial phase images show homogeneous enhancement of the lesion and persistent enhancement on the portal phase (D). E–G MRI study performed 12 months later after conservative treatment. E, F Axial gradient in-phase and out-of-phase images show evidence of hepatic steatosis with multiple lesions in the liver. G Axial T1-weighted post contrast image shows complete resolution of subcapsular hematoma and decreased size of enhancing mass in the posterior right lobe. Note that additional multiple small enhancing lesions in the right lobe. This case shows the resolution of a subcapsular hematoma with decreased size of tumor after conservative treatment at 12-month follow-up.
To our knowledge, the oldest reported individual with LA was a 66-year-old female who also had 3 years of OC use [14]. Very few patients with LA have been described after the age of 50. In our series, only 2 women were older than 50 years, and the oldest woman was aged 52–53 over the period of investigation. The majority of reported patients, including those in our series, had received OCs. Although our small series was insufficient to derive a conclusion, our suspicion, combining our findings with that in the literature, is that the great majority of LAs substantially resolve commencing by the mid-50’s. Additional complicating factors would include the age and duration of OC and other hormonal agent usage. Resolution of LA lesions may reflect the combination that endogenous sex hormones substantially decrease following menopause, and OC use would also be absent from the mid 40’s onward. Unfortunately, no study has reported on the menstrual status or had a sufficient long follow-up period, extending from prior to and following menopause to confirm our suspicion. Future studies with longer follow-up times are needed to address this.
HCA is a multifactorial disease [3]. Several factors have been proposed regarding the potential causes and associations with this tumor. The relationship between HCAs and obesity has been studied. One study has [15] reported 55% of 60 patients diagnosed with HCAs were obese and tumor progression was more frequently observed in obese patients. Moreover, 3 of the 15 obese patients had no progression in liver lesions after they lost ≥5% body weight, whereas 5/12 (42%) obese patients who did not achieve at least 5% weight reduction had progression of HCAs during follow-up. In our study, a comparable number, 66%, were obese. Based on these findings, it would seem prudent to request of obese patients with LA or HCAs, that they lose weight in addition to discontinue OCs use.
In a case control study between the association of HCAs and liver steatosis [16], investigators found that the prevalence of liver steatosis was significantly higher in patients with hepatic adenomas (58%) than in control subjects (29%). In addition, liver steatosis has been more commonly described in patients with multiple hepatic adenomas (82%) than in those with a single hepatic adenoma (38%). In our series, 63.2% of patients had hepatic steatosis, supporting the concept of the association between hepatic steatosis and LA.
Evidence of rupture or hemorrhage of HCAs was found in 25% of individuals in one prior study, and the risk of rupture or hemorrhage correlated with increased tumor size and recent hormone use [4]. Our data showed evidence of hemorrhage into and HCA in 38.8% of subjects. The smallest hemorrhagic HCA was 4.1 cm in diameter. Due to the risk of hemorrhage, it may be reasonable to consider surgical removal of lesions greater than 4 cm [4]. Among the seven patients in our series who had hemorrhagic lesions, 6 patients underwent partial hepatic resection of 8 hemorrhagic lesions, and 1 patient underwent conservative management.
A recent report has described a therapeutic effect using selective TAE on nonhemorrhagic HCAs [17]. After TAE, the majority of the stroma of the adenomas showed necrotic change, without showing an increase in tumor size or evidence of hemorrhage and rupture, during the follow-up period. They suggested that TAE is an effective treatment for hypervascular HCAs to prevent hemorrhage and rupture, when it is difficult to perform hepatectomy. In our study, two patients, with non-hemorrhagic HCAs >4 cm, underwent TAE. One of two patients underwent TAE 2 years after resection of another large tumor, and in this patient after a 72-month follow-up period multiple residual lesions exhibited decrease in size of lesions. The other patient underwent TAE alone, due to the high risk of surgery, and showed tumor necrosis with decrease in tumor size after a 10-month follow-up.
Risk of malignant transformation of HCAs has been reported in about 4%–8% of patients [1, 4, 18]. It has also been suggested that HCAs associated with β-catenin gene, patients with a history of androgen or anabolic steroid intake [1], and patients of male gender [1, 3] carry a higher risk of malignant transformation. Lesion size has also been reported as a risk factor for malignant transformation [4]. In our series, no evidence of malignant transformation was observed, we also looked at all patients who underwent histologic evaluation in the Pathology Department over the same 10-year period and no patient with HCA was shown to develop malignant transformation. It should be noted that this is reporting only on a single institution database. There was also only one male in our series. This patient had Gilbert’s syndrome and no underlying exogenous androgen steroids as the predisposing factor. Gilbert’s syndrome is a benign unconjugated hyperbilirubinemia that occurs in the absence of hemolysis or structural liver disease [19]. It is clinically inconsequential entity that requires neither treatment nor long-term medical attention [20], and has never been reported to be associated with HCA.
Limitations of our study include the retrospective design, the few numbers of patients, as referenced above. The rarity of the entity accounts for the few number of patients. The inclusion of patients with no histological confirmation may have introduced some uncertainty of diagnosis; however, lesion appearance and rate of lesion size change were consistent with subjects who did have histologic confirmation. Another major limitation of our study was the short duration of follow-up for our patients and that none were imaged well into their 50’s. This would have provided direct evidence of our assumption that LA resolves progressively at this age. Immunohistochemical analysis was also not performed in our study, which may have provided interesting insight into the underlying types of adenoma associated with LA.
In conclusion, our study showed that over an approximately 2-year follow-up period, in the majority of patients with LA, the lesions remained stable or showed tumor regression. Spontaneous tumor regression in patients without any intervention is not uncommon and can be observed in about 37% of individuals.
References
Dokmak S, Paradis V, Vilgrain V, et al. (2009) A single-center surgical experience of 122 patients with single and multiple hepatocellular adenomas. Gastroenterology 137:1698–1705
Flejou J, Barge J, Menu Y, et al. (1985) Liver adenomatosis. An entity distinct from liver adenoma? Gastroenterology 89:1132
Bioulac-Sage P, Laumonier H, Couchy G, et al. (2009) Hepatocellular adenoma management and phenotypic classification: the Bordeaux experience. Hepatology 50:481–489
Deneve JL, Pawlik TM, Cunningham S, et al. (2009) Liver cell adenoma: a multicenter analysis of risk factors for rupture and malignancy. Ann Surg Oncol 16:640–648
Svrcek M, Jeannot E, Arrive L, et al. (2007) Regressive liver adenomatosis following androgenic progestin therapy withdrawal: a case report with a 10-year follow-up and a molecular analysis. Eur J Endocrinol 156:617–621
Vetelainen R, Erdogan D, de Graaf W, et al. (2008) Liver adenomatosis: re-evaluation of aetiology and management. Liver Int 28:499–508
Raman SP, Hruban RH, Fishman EK (2013) Hepatic adenomatosis: spectrum of imaging findings. Abdom Imaging 38(3):474–481
Goodwin MD, Dobson JE, Sirlin CB, Lim BG, Stella DL (2011) Diagnostic challenges and pitfalls in MR imaging with hepatocyte-specific contrast agents. Radiographics 31:1547–1568
Rebouissou S, Bioulac-Sage P, Zucman-Rossi J (2008) Molecular pathogenesis of focal nodular hyperplasia and hepatocellular adenoma. J Hepatol 48:163–170
Zucman-Rossi J, Jeannot E, Nhieu JT, et al. (2006) Genotype–phenotype correlation in hepatocellular adenoma: new classification and relationship with HCC. Hepatology 43:515–524
Bioulac-Sage P, Rebouissou S, Thomas C, et al. (2007) Hepatocellular adenoma subtype classification using molecular markers and immunohistochemistry. Hepatology 46:740–748
Laumonier H, Bioulac-Sage P, Laurent C, et al. (2008) Hepatocellular adenomas: magnetic resonance imaging features as a function of molecular pathological classification. Hepatology 48:808–818
Ronot M, Bahrami S, Calderaro J, et al. (2011) Hepatocellular adenomas: accuracy of magnetic resonance imaging and liver biopsy in subtype classification. Hepatology 53:1182–1191
Grazioli L, Federle MP, Ichikawa T, et al. (2000) Liver adenomatosis: clinical, histopathologic, and imaging findings in 15 patients. Radiology 216:395–402
Bunchorntavakul C, Bahirwani R, Drazek D, et al. (2011) Clinical features and natural history of hepatocellular adenomas: the impact of obesity. Aliment Pharmacol Ther 34:664–674
Furlan A, van der Windt DJ, Nalesnik MA, et al. (2008) Multiple hepatic adenomas associated with liver steatosis at CT and MRI: a case–control study. Am J Roentgenol 191:1430–1435
Kobayashi S, Sakaguchi H, Takatsuka M, et al. (2009) Two cases of hepatocellular adenomatosis treated with transcatheter arterial embolization. Hepatol Int 3:416–420
Stoot JH, Coelen RJ, De Jong MC, Dejong CH (2010) Malignant transformation of hepatocellular adenomas into hepatocellular carcinomas: a systematic review including more than 1600 adenoma cases. HPB 12:509–522
Arita J, Sugawara Y, Hashimoto T, et al. (2003) Liver resection in patients with Gilbert’s syndrome. Surgery 134:835–837
Radu P, Atsmon J (2001) Gilbert’s syndrome—clinical and pharmacological implications. Isr Med Assoc J 3:593–598
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Srirattanapong, S., Angthong, W., Kim, B.S. et al. Liver adenomatosis: serial investigation on MRI. Abdom Imaging 39, 269–282 (2014). https://doi.org/10.1007/s00261-013-0056-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-013-0056-y