Abstract
Aim
To present the gastrointestinal (GI) complications associated with bevacizumab therapy and their findings on abdominal imaging studies.
Methods
A computerized search identified 11 patients with GI complications of bevacizumab therapy on abdominal CT (n = 11) and fluoroscopic GI contrast studies (n = 4) who met our study criteria (including five patients with ovarian cancer, five with colon cancer, and one with cervical cancer). The medical records and imaging studies were reviewed to determine the clinical and radiographic findings in these patients.
Results
All 11 patients had findings of GI perforation on CT, or CT and GI contrast studies. CT revealed a localized extraluminal collection containing gas, fluid, and/or contrast material in eight patients (73%) with focal perforation, and free abdominal air and fluid in three (27%) with free perforation The imaging studies also revealed seven fistulas, including two colovaginal, one rectovaginal, one enterocutaneous, one colocutaneous, one gastrocolic, and one colorectal fistula. Eight (73%) of the 11 patients died within 1 year of the development of GI perforation, and the perforation was felt to be the cause of death in four patients (36%).
Conclusion
Abdominal CT and fluoroscopic GI contrast studies are useful imaging tests for the diagnosis of potentially life-threatening GI perforation as a complication of bevacizumab therapy. When GI perforation is detected on abdominal imaging studies, treatment with bevacizumab should immediately be discontinued.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Vascular endothelial growth factor (VEGF) is a signal protein produced by malignant neoplasms that acts on endothelial cells to induce mitosis and enhance angiogenesis, thereby enabling these tumors to grow faster [1]. Because of its ability to inhibit VEGF-mediated tumor angiogenesis, bevacizumab (Avastin; Genentech), a monoclonal antibody against VEGF, has been advocated for treatment of malignant tumors [2, 3]. This agent was initially approved for treatment of metastatic colon cancer after a phase III clinical trial documented its therapeutic efficacy [4]. Since that time, bevacizumab has been shown to be effective for treatment of a variety of malignancies, including colonic, ovarian, breast, cervical, and small cell lung cancer, when administered in combination with chemotherapy [5–7]. It is also effective as a single agent for the treatment of ovarian cancer. Bevacizumab is administered as an IV infusion in doses of 5–15 mg/kg with a 2- or 3-week interval between treatment cycles.
Unfortunately, bevacizumab therapy may be associated with serious side effects, particularly involving the gastrointestinal (GI) tract. Colovaginal, rectovaginal, colorectal, and colocutaneous fistulas have all been reported in patients receiving this agent for treatment of colonic and ovarian carcinoma [8–10]. Bowel necrosis and perforation have also been reported as potentially life-threatening complications of bevacizumab therapy, leading to intra-abdominal abscesses, peritonitis, sepsis, and death [4, 11–17]. In a review of the literature by Badgwell et al. [13], GI perforation occurred in 25 (1.7%) of 1442 patients treated with bevacizumab. In another study, GI perforation was reported in 8 (4%) of 223 patients with unresected primary tumors treated with bevacizumab [4]. The perforation rate in patients with ovarian cancer has been reported to be as high as 15% [13, 16–19]. The risk of GI perforation may be even higher in patients who have received concomitant radiation therapy [11].
While GI perforation and fistula formation are well-recognized complications of bevacizumab therapy, to the best of our knowledge, this subject has not been adequately addressed in the radiology literature. Nevertheless, it is important for radiologists to be aware of the potentially life-threatening GI side effects of bevacizumab, so treatment with this agent can immediately be stopped and aggressive management instituted when serious GI complications are encountered on CT or fluoroscopic GI contrast studies. The purpose of our investigation is to present the GI complications associated with bevacizumab therapy and the findings on abdominal imaging studies.
Materials and methods
Patient population
A computerized search of the radiology database at our university hospital was performed, using Pathology and Radiology Enterprise Search Tool (PRESTO) to identify patients with abdominal imaging studies who developed GI complications after bevacizumab therapy for malignant tumors during a 5-year period from January 2006 to December 2010. Patients were included in our study only if the dose and duration of bevacizumab therapy were documented in their medical records and clinical follow-up data and abdominal imaging studies were available for review. Eleven patients fulfilled our selection criteria; these 11 patients constituted our study group. All 11 (100%) were women. The mean patient age was 56.7 years (range 40–71 years). All 11 patients (100%) had abdominal CT scans and four (36%) also had GI contrast studies, including two water-soluble contrast enemas, one small bowel follow-through and one fistulogram.
Examination technique
Abdominal CT
The 11 CT scans were performed on multidetector helical CT scanners according to an established protocol. All but one of the 11 patients (91%) received positive oral contrast material (30 mL of Gastrografin [diatrizoate meglumine and diatrizoate sodium solution; Bracco Diagnostics, Inc.] in 1000 mL of water) 30–60 min before the scans. Eight patients (73%) also received 100 mL of iodinated contrast material (iopamidol [Isoview; Bracco Diagnostics]) IV. CT scans were obtained with the patient supine during full inspiration. Axial images were obtained at 5- to 7-mm slice collimations (pitch; 1.3:1; 200–220 mAs) and reconstructed with a soft-tissue algorithm. Coronal and sagittal reformatting of the images was performed at the time of the scan.
Fluoroscopic GI contrast studies
Two water-soluble contrast enemas were performed by administering water-soluble contrast material (diatrizoate meglumine and diatrizoate sodium [Gastroview; Mallinckrodt] diluted 1:1 with water) via a catheter inserted into the rectum and obtaining fluoroscopic spot images of the colon. A fistulogram was performed by administering water-soluble contrast material (Gastroview) via a catheter inserted into an opening on the anterior abdominal wall and obtaining fluoroscopic spot images of the fistula. Finally, a small bowel follow-through was performed by having the patient ingest four 16 oz cups of 60% w/v barium (Entrobar; E-Z-EM) and obtaining spot images of the jejunum and ileum at 30-min intervals. All of the contrast studies were performed with digital fluoroscopy equipment (Sireskop SD; Siemens).
Study design
All of the imaging studies for these 11 patients were reviewed to identify GI complications of bevacizumab therapy. Medical records were also reviewed to determine the dose, duration, and timing of bevacizumab therapy prior to the development of GI complications as well as the clinical presentation, treatment, and subsequent patient course.
Review of images
Abdominal CT scans and fluoroscopic GI contrast studies for these 11 patients were reviewed retrospectively at a computer workstation by a consensus of three GI radiologists. The imaging studies were reviewed to identify GI complications of bevacizumab therapy, including the location and radiographic findings of bowel perforation and fistula formation. In patients with previous GI tract surgery, all enteric anastomoses were carefully assessed for radiologic signs of anastomotic breakdown. The CT scans were also assessed for radiographic signs of bowel wall thickening, intestinal pneumatosis, mesenteric edema, and pneumoperitoneum.
The findings of our retrospective review of the images were compared with the original radiologic reports by one author, and no major discrepancies were found.
Institutional review board approval
Our institutional review board approved all aspects of this retrospective study and did not require informed consent from any patients whose radiographic images or medical records were included in our study. This investigation was also compliant with the Health Insurance Portability and Accountability Act (HIPAA).
Results
Cancer history and treatment
Our study group consisted of 11 patients with malignant tumors who underwent bevacizumab therapy, including five patients (45%) with ovarian cancer, five (45%) with colorectal cancer, and one (9%) with cervical cancer. Four patients (80%) with ovarian cancer had stage IIIC disease and one (20%) had stage IV disease; all five patients (100%) with colorectal cancer had stage IV disease; and one patient with cervical cancer had stage IIIB disease.
All 11 patients (100%) had one or more operations for their primary cancers. Four of the five patients with ovarian cancer underwent a total abdominal hysterectomy and bilateral salpingo-oophorectomy and two of these patients also had a sigmoid resection with tumor debulking and a diverting colostomy. The remaining patient with ovarian cancer underwent a right hemicolectomy and ileal resection with a primary ileocolic anastomosis for metastatic disease involving the bowel. Three of the five patients with colorectal cancer underwent a right hemicolectomy, one had a sigmoid resection, and one had a total colectomy with an end ileostomy. The one patient with cervical cancer underwent a diverting colostomy. Two (18%) of the 11 patients in our study had a history of previous radiation therapy to the pelvis 3 years and 8 months before developing rectosigmoid perforation, respectively.
Ten patients (91%) underwent one or more chemotherapy regimens prior to treatment with bevacizumab, including paclitaxel [Taxol; Bristol-Myers Squibb] with carboplatin [Paraplatin; Bristol-Myers Squibb] (n = 5); FOLFIRI (folinic acid, fluorouracil, and irinotecan [Camptosar; Pfizer]) (n = 2); FOLFOX (folinic acid, fluorouracil, and oxaliplatin [Eloxatin; Sanofi Aventis]) (n = 3); irinotecan (n = 2); oxaliplatin (n = 2); capecitabine [Xeloda; Roche] (n = 1); gemcitabine [Gemzar; Lilly] (n = 1); etoposide [Etopophos; Bristol-Myers Squibb] (n = 1); letrozole [Femara; Novartis Pharmaceuticals] (n = 1); and topotecan [Hycamtin; GlaxoSmithKline] with thalidomide [Thalomid; Celgene Corp] (n = 1). All 11 patients (100%) were receiving concurrent chemotherapy while on treatment with bevacizumab, including cyclophosphamide [cytoxan; Bristol-Myers Squibb] (n = 4); FOLFIRI (n = 2); FOLFOX (n = 2); carboplatin with paclitaxel (n = 2); and capecitabine (n = 1). The mean duration between the most recent cycle of chemotherapy and documentation of GI complications in these 11 patients was 19 days (range 1–90 days), excluding one outlier with a chronic rectovaginal fistula.
Bevacizumab treatment
The dose of bevacizumab for each treatment cycle was 15 mg/kg for three patients (60%) with ovarian cancer and 10 mg/kg for two (40%); 5 mg/kg for all five patients (100%) with colorectal cancer; and 15 mg/kg for the one patient with cervical cancer. The mean number of cycles of bevacizumab therapy these patients had received at the time of clinical presentation was 5.3 (range 1–19 cycles). The mean duration between the most recent treatment cycle with bevacizumab and clinical presentation was 9.6 days (range 1–26 days), excluding the one outlier mentioned previously.
Clinical presentation
All 11 patients underwent abdominal CT or fluoroscopic GI contrast studies for one or more clinical signs or symptoms, including abdominal pain in nine patients (82%), nausea and/or vomiting in five (45%), feculent discharge from the vagina in three (27%), change in bowel habits in three (27%), fever and chills in three (27%), abdominal tenderness, guarding, and rebound in two (18%) (both of these patients were found to have peritonitis), draining cutaneous fistulas from the anterior abdominal wall in two (18%), and vaginal bleeding in one (9%). (One patient with peritonitis did not have peritoneal signs or symptoms.) The mean duration of symptoms at the time of presentation was 5.1 days (range 1–14 days), excluding the one outlier with a chronic rectovaginal fistula who had feculent discharge from the vagina for 20 months before seeking medical treatment.
Radiographic findings
All 11 patients had findings of GI perforation on abdominal CT or fluoroscopic GI contrast studies, with a focal, contained (i.e., sealed-off) perforation in eight patients (73%) (Figs. 1, 2, 3) and free perforation into the peritoneal cavity in three (27%) (Figs. 4, 5). The site of perforation included the rectum in three patients (27%), colon in three (27%) (sigmoid colon in two and transverse colon in one) (Figs. 1, 2, 3), jejunum in two (18%) (Fig. 5), colorectal anastomosis in one (9%), colocolic anastomosis in one (9%) (Fig. 4), and ileocolic anastomosis in one (9%). CT revealed a localized extraluminal collection containing gas, fluid, and/or contrast material at the site of perforation in eight patients with a contained perforation (Fig. 3A). In contrast, CT revealed free intraperitoneal air and fluid in the three patients with free perforation into the peritoneal cavity (Figs. 4, 5). CT also revealed bowel wall thickening at or near the site of perforation in nine (82%) of the 11 patients with perforation (Fig. 3A, 5) and intramural pneumatosis in two (18%).
67-Year-old woman with colon cancer who presented with feculent vaginal discharge due to development of colovaginal fistula after four cycles of bevacizumab. This patient previously underwent sigmoid resection, total abdominal hysterectomy, and bilateral salpingo-oophorectomy. A Oral-enhanced sagittal CT scan shows soft-tissue density (large white arrows) caused by metastatic tumor in the pouch of Douglas. Also note gas in fistula (small black arrow) extending from colon (large black arrow) to vagina (small white arrows). B Left lateral spot image from water-soluble contrast enema 4 weeks later shows narrowing of colorectal anastomosis (small white arrow) with focal extravasation of contrast material from colon proximal to anastomosis into contained extraluminal collection (large white arrows) that communicates anteriorly with vagina (large black arrows) via fistula (small black arrows).
63-Year-old woman with ovarian cancer who presented with feculent vaginal discharge due to development of colovaginal fistula after three cycles of bevacizumab. She previously underwent total abdominal hysterectomy, bilateral salpingo-oophorectomy, and diverting colostomy. Left posterior oblique spot image from water-soluble contrast enema shows irregular narrowing of rectosigmoid colon (small white arrow) due to encasement by metastatic tumor. There is also focal extravasation of contrast material from sigmoid colon into a contained extraluminal collection (large white arrows) that communicates inferiorly with vagina (black arrows). (Residual contrast material is present in bladder from previous CT.)
64-Year-old woman with ovarian cancer who presented with abdominal pain and draining anterior abdominal wall wound due to development of colocutaneous and gastrocolic fistulas after one cycle of bevacizumab. She previously underwent total abdominal hysterectomy, bilateral salpingo-oophorectomy, and small bowel and sigmoid resections. A Oral-enhanced axial CT scan shows irregular thickening (large white arrows) of transverse colon with gas and contrast material in a contained extraluminal collection anteriorly (small white arrows). Gas is also seen entering track (small black arrow) that communicates with gas-filled collection (large black arrow) in anterior abdominal wall. B Injection of anterior abdominal wound 2 weeks later shows water-soluble contrast material filling a grossly irregular transverse colon (small white arrows) with focal extravasation of contrast material into two contained extraluminal collections (large white arrows) abutting inferior aspect of transverse colon. Also note contrast material entering thin track (small black arrows) that extends superiorly from transverse colon into stomach. (Large black arrow denotes contrast material in balloon of percutaneous gastrostomy tube.)
59-Year-old woman with ovarian cancer who presented with fever, chills, and abdominal pain due to perforation of descending colon at site of anastomosis and peritonitis after six cycles of bevacizumab. She previously underwent total abdominal hysterectomy, bilateral salpingo-oophorectomy, and partial left colectomy. IV- and oral-enhanced axial CT scan shows extensive pneumoperitoneum (small black arrows) secondary to free perforation from left colon at site of colocolic anastomosis, denoted by staple line (small white arrow). Note gas and stool in left colon (large black arrows) with extraluminal fluid laterally and posteriorly (large white arrows) near site of perforation.
45-Year-old woman with colon cancer who presented with fever, chills, and abdominal pain due to perforation of small bowel and peritonitis after 14 cycles of bevacizumab. She previously underwent right hemicolectomy with ileocolic anastomosis. IV- and oral-enhanced axial CT scan shows pneumoperitoneum (white arrows) in anterior abdomen. Also note thickening of wall (black arrows) in several loops of small bowel and engorgement of adjacent mesentery. This patient was found to have jejunal necrosis and perforation at laparotomy later that day.
Bowel perforation was associated with a total of seven fistulas in four patients, including two colovaginal, one rectovaginal, one enterocutaneous, one colocutaneous, one gastrocolic, and one colorectal fistula. All but one of the fistulas was manifested on CT by extraluminal air, fluid, and/or contrast material within the fistulous track (Figs. 1A, 3A). The one fistula (a colovaginal fistula) not detected on CT was visualized on a water-soluble contrast enema.
In two patients with colovaginal fistulas, water-soluble contrast enemas revealed focal breakdown of the rectosigmoid colon, with water-soluble contrast material entering a contained extraluminal collection in the pelvis that also communicated with the vagina (Figs. 1B, 2). In one patient with a colocutaneous fistula, a fistulogram revealed water-soluble contrast material entering the transverse colon via the fistula, with a markedly irregular colonic wall and contained extraluminal collections that communicated with the lumen of the transverse colon (Fig. 3B). Water-soluble contrast material was also seen entering the stomach via a gastrocolic fistula (Fig. 3B). In a final patient, a small bowel follow-through showed focal extravasation of barium from a loop of jejunum into a fistulous track that communicated with the anterior abdominal wall, indicating the presence of an enterocutaneous fistula.
Treatment and patient course
Four patients (including the three with free perforation and peritonitis) (36%) underwent emergent laparotomies with lysis of adhesions, a segmental left colonic resection, and a transverse loop colostomy in one; a segmental jejunal resection in one; a partial colectomy with a diverting colostomy and creation of a blind-ending Hartmann pouch in one; and fulguration of an enterocutaneous fistula in one. The remaining seven patients (64%) with bowel perforation underwent conservative medical management because of the long half life of bevacizumab (~20 days) and the greater risks of surgery in these patients secondary to impaired wound and anastomotic healing for 28 days post dosing with bevacizumab.
Eight patients (73%) died within 1 year of the development of GI perforation; the perforation itself was felt to be the cause of death in four patients (36%) and progression of tumor in the remaining four (36%). Two patients (18%) were still alive 1 year after presentation and one (9%) was still alive 3 years after presentation.
Discussion
Despite its effectiveness in the treatment of malignant tumors, bevacizumab is associated with a variety of serious complications. Like other angiogenesis inhibitors, bevacizumab may cause hypertension and proteinuria [4]. Patients receiving this agent are also at increased risk for arterial thromboembolic events [20, 21], which can be catastrophic. These patients may also have substantially delayed wound healing [22]. Patients who receive bevacizumab in combination with radiation to the thorax are predisposed to the development of tracheoesophageal fistulas [23, 24], whereas patients who receive bevacizumab for colonic and ovarian carcinomas are at increased risk for developing a variety of GI fistulas, particularly colovaginal or rectovaginal fistulas, even in the absence of radiation therapy [8–10].
GI perforation is a well-documented and potentially life-threatening complication of bevacizumab therapy [11–19], which, to the best our knowledge, has not been adequately addressed in the radiology literature. In our study, 8 (73%) of 11 patients with bevacizumab-related GI perforation died within 1 year, and GI perforation was thought to be the cause of death in four patients (36%). The devastating consequences of GI perforation in this clinical setting were recognized in a recent meta-analysis of 12, 294 patients treated with bevacizumab, in which the mortality rate from GI perforation was 21.7% [16].
As in our study, GI perforation and fistula formation have typically developed in patients receiving bevacizumab infusions in doses of 5 mg/kg for colonic carcinoma and 10–15 mg/kg for ovarian carcinoma [14, 15, 17]. With the exception of one patient who developed a chronic rectovaginal fistula, all of the patients in our study had signs and symptoms of GI perforation within 1–26 days of their most recent dose of bevacizumab, and the mean duration between the last treatment dose and clinical presentation was 9.6 days. In the review of the literature by Badgwell et al. [13], GI perforation occurred within 2–49 days of treatment with bevacizumab. This complication therefore can develop as early as 1–2 days after the last treatment dose. Others have found that GI perforation almost always develops within the first 6 months after treatment with bevacizumab [25]. Similarly, fistula formation has been reported to develop as early as 2–5 weeks after bevacizumab therapy for rectal cancer [26]. It therefore is important to recognize that GI perforation or fistula formation can occur within days to weeks of bevacizumab therapy, so these devastating complications may develop rapidly after treatment with this agent.
In our study, CT revealed gas, fluid, and/or contrast material in contained extraluminal collections or fistulas in eight (73%) of the 11 patients with GI perforation after bevacizumab therapy (Fig. 3A). The remaining three patients (27%) developed free perforation with air and fluid in the peritoneal cavity and peritonitis, a life-threatening condition (Figs. 4, 5). Three (27%) of the perforations occurred at the site of a bowel anastomosis (Fig. 4), so enteric anastomoses may be particularly vulnerable to the deleterious effects of bevacizumab. Whatever the site of breakdown, it is important to be aware of the association between treatment with bevacizumab and the development of GI perforation or fistulas, so treatment with this agent can immediately be discontinued.
CT revealed focal bowel wall thickening in close proximity to the site of perforation in nine (82%) of the 11 patients (100%) with GI perforation (Figs. 3A, 5) and intramural pneumatosis in two (18%). These findings were most likely secondary to varying degrees of bowel ischemia and necrosis at or near the site of perforation. Localized bowel wall thickening and pneumatosis therefore may be an early indicator on CT of an increased risk for impending bowel perforation in patients treated with bevacizumab.
Four patients (36%) who were treated with bevacizumab also developed a variety of fistulas, including colovaginal, rectovaginal, enterocutaneous, colocutaneous, gastrocolic, and colorectal fistulas that were visualized on CT or fluoroscopic contrast studies (Figs. 1, 2, 3). These fistulas may be acute or chronic, persisting for as long as a year or more, as in one of our patients with a long-standing rectovaginal fistula. The development of GI fistulas in patients who have been treated for ovarian or colonic carcinoma therefore should prompt the radiologist to inquire about a prior history of bevacizumab therapy.
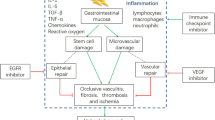
The etiology of GI perforation in patients treated with bevacizumab is uncertain. It has been suggested that inhibition of tumor angiogenesis not only may cause tumor necrosis, but also necrosis and perforation of the adjacent bowel [27, 28]. Bevacizumab therapy may also lead to arterial microthromboembolic phenomena with associated ischemia and perforation [29]. Alternatively, it has been postulated that bevacizumab may cause GI ulceration as a precursor to localized perforation [30]. Finally, VEGF is thought to play a role in repairing injured GI mucosa [27, 28], so inhibition of VEGF by bevacizumab may render injured bowel more susceptible to perforation.
Two (18%) of the 11 patients in our study had a history of previous radiation therapy to the pelvis before developing a rectosigmoid perforation. As suggested by others, treatment with bevacizumab therefore could potentiate radiation-induced bowel injury, causing these patients to be at even greater risk for GI perforation [11].
Our investigation has the inherent limitations of a retrospective study, including selection bias and interpretation bias, though there were no major discrepancies between our retrospective image review and the original radiology reports. Also, all of the patients in our study group were women, possibly because of sample bias related to the small size of our study group and the high frequency of malignant gynecologic tumors, which were present in 6 (55%) of our 11 patients.
In conclusion, it is important for radiologists to be aware of the association between bevacizumab therapy and the development of potentially life-threatening GI perforation. Abdominal CT and fluoroscopic GI contrast studies are useful imaging tests for showing focal or free GI perforation as well as associated fistula formation. When GI perforation is detected on abdominal imaging studies, treatment with bevacizumab should immediately be discontinued.
References
Horn L, Sandler A (2007) Chemotherapy and antiangiogenic agents in non-small-cell lung cancer. Clin Lung Cancer 8(suppl 2):S68–S73
Ranieri G, Patruno R, Ruggieri E, et al. (2006) Vascular endothelial growth factor (VEGF) as a target of bevacizumab in cancer: from the biology to the clinic [Review]. Curr Med Chem 13:1845–1857
Homsi J, Daud AI (2007) Spectrum of activity and mechanism of action of VEGF/PDGF inhibitors. Cancer Control 14:285–294
Van Cutsem E, Rivera F, Berry S, et al. (2009) Safety and efficacy of first-line bevacizumab with FOLFOX, XELOX, FOLFIRI and fluoropyrimidines in metastatic colorectal cancer: the BEAT study. Ann Oncol 20:1842–1847
Hurwitz H, Fehrenbacher L, Novotny W, et al. (2004) Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N Engl J Med 350:2335–2342
Sandler A, Gray R, Perry MC, et al. (2006) Paclitaxel-carboplatin alone or with bevacizumab for non-small-cell lung cancer. N Engl J Med 355:2542–2550
Miller K, Wang M, Gralow J, et al. (2007) Paclitaxel plus bevacizumab versus paclitaxel alone for metastatic breast cancer. N Engl J Med 357:2666–2676
Sparano JA, Gray R, Giantonio B, et al. (2004) Evaluating antiangiogenesis agents in the clinic: the eastern cooperative oncology group portfolio of clinical trials. Clin Cancer Res 10:1206–1211
Ley EJ, Vukasin P, Kaiser AM, et al. (2007) Delayed rectovaginal fistula: a potential complication of bevacizumab (avastin) [Letter]. Dis Colon Rectum 50:930
Chéreau E, Stefanescu D, Selle F, et al. (2009) Spontaneous rectovaginal fistula during bevacizumab therapy for ovarian cancer: a case report. Am J Obstet Gynecol 200:e15–e16
Gordon MS, Cunningham D (2005) Managing patients treated with bevacizumab combination therapy. Oncology 69(suppl 3):25–33
Garcia AA, Hirte H, Fleming G, et al. (2008) Phase II clinical trial of bevacizumab and low-dose metronomic oral cyclophosphamide in recurrent ovarian cancer: a trial of the California, Chicago, and Princess Margaret Hospital phase II consortia. J Clin Oncol 26:76–82
Badgwell BD, Camp ER, Feig B, et al. (2008) Management of bevacizumab-associated bowel perforation: a case series and review of the literature. Ann Oncol 19:577–582
Vincenzi B, Santini D, Russo A, et al. (2009) Bevacizumab in association with de gramont 5-fluorouracil/folinic acid in patients with oxaliplatin-, irinotecan-, and cetuximab-refractory colorectal cancer: a single-center phase 2 trial. Cancer 115:4849–4856
Monk BJ, Sill MW, Burger RA, et al. (2009) Phase II trial of bevacizumab in the treatment of persistent or recurrent squamous cell carcinoma of the cervix: a gynecologic oncology group study. J Clin Oncol 27:1069–1074
Hapani S, Chu D, Wu S (2009) Risk of gastrointestinal perforation in patients with cancer treated with bevacizumab: a meta-analysis [Review]. Lancet Oncol 10:559–568
Cannistra SA, Matulonis UA, Penson RT, et al. (2007) Phase II study of bevacizumab in patients with platinum-resistant ovarian cancer or peritoneal serous cancer. J Clin Oncol 25:5180–5186
Wright JD, Hagemann A, Rader JS, et al. (2006) Bevacizumab combination therapy in recurrent, platinum-refractory, epithelial ovarian carcinoma: a retrospective analysis. Cancer 107:83–89
Nimeiri HS, Oza AM, Morgan RJ, et al. (2008) Efficacy and safety of bevacizumab plus erlotinib for patients with recurrent ovarian, primary peritoneal, and fallopian tube cancer: a trial of the Chicago, PMH, and California Phase II Consortia. Gynecol Oncol 110:49–55
Skillings JR, Johnson DH, Miller K, et al. (2005) Arterial thromboembolic events (ATEs) in a pooled analysis of 5 randomized, controlled trials (RCTs) of bevacizumab (BV) with chemotherapy. J Clin Oncol 23(suppl 16):3019
Zangari M, Fink LM, Elice F, et al. (2009) Thrombotic events in patients with cancer receiving antiangiogenesis agents. J Clin Oncol 27:4865–4873
Scappaticci F, Fehrenbacher L, Cartwright T, et al. (2005) Surgical wound healing complications in metastatic colorectal cancer patients treated with bevacizumab. J Surg Oncol 91:173–180
Goodgame B, Veeramachaneni N, Patterson A, et al. (2008) Tracheo-esophageal fistula with bevacizumab after mediastinal radiation. J Thorac Oncol 3:1080–1081
Spigel DR, Hainsworth JD, Yardley DA, et al. (2010) Tracheoesophageal fistula formation in patients with lung cancer treated with chemoradiation and bevacizumab. J Clin Oncol 28:43–48
Saif MW, Elfiky A, Salem RR (2007) Gastrointestinal perforation due to bevacizumab in colorectal cancer. Ann Surg Oncol 14:1860–1869
Wolf I, Urban D, Pfeffer R, et al. (2007) High incidence of fistula formation during bevacizumab treatment in rectal cancer patients [Letter]. Acta Oncol 46:550–553
Gressett SM, Shah SR (2009) Intricacies of bevacizumab-induced toxicities and their management. Ann Pharmacother 43:490–501
Tarnawski AS (2005) Cellular and molecular mechanisms of gastrointestinal ulcer healing. Dig Dis Sci 50(suppl 1):S24–S33
Heinzerling JH, Huerta S (2006) Bowel perforation from bevacizumab for the treatment of metastatic colon cancer: incidence, etiology, and management. Curr Surg 63:334–347
Tol J, Cats A, Mol L, et al. (2008) Gastrointestinal ulceration as a possible side effect of bevacizumab which may herald perforation. Invest New Drugs 26:393–397
Acknowledgments
Janos L. Tanyi was supported by Reproductive Scientist Development Program, through NIH Grant #5K12HD00849-23.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Borofsky, S.E., Levine, M.S., Rubesin, S.E. et al. Bevacizumab-induced perforation of the gastrointestinal tract: clinical and radiographic findings in 11 patients. Abdom Imaging 38, 265–272 (2013). https://doi.org/10.1007/s00261-012-9913-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-012-9913-3