Abstract
Leiomyosarcomas of adrenal origin occur infrequently, always present as huge abdominal masses, and are associated with poor prognoses when other organs are invaded. Radiologic images of small adrenal leiomyosarcomas have not been published. This report presents magnetic resonance images of a 3-cm left adrenal leiomyosarcoma from a 49-year-old male. Ten months after adrenalectomy, the patient was alive without tumor recurrence.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Primary adrenal leiomyosarcomas are extremely rare. Only nine patients [1–9] and two autopsies [10] have been reported in the literature. Most of the clinically diagnosed tumors described in these reports were larger than 10 cm in diameter. To our knowledge, images of primary adrenal leiomyosarcomas smaller than 5 cm in diameter have never been described. This report describes a male patient with a 3-cm primary left adrenal leiomyosarcoma and presents magnetic resonance imaging (MRI) of that tumor.
Case report
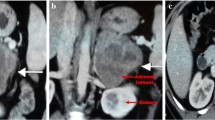
A 49-year-old man had left flank pain for 6 months. Ultrasound revealed a left abdominal mass. MRI (Magnetom Sonata, Siemens Medical Solutions) showed a round, left suprarenal tumor with heterogeneously low intensity on T1-weighted images, high intensity on T2-weighted images, and marginal enhancement after gadolinium diethylenetriamine pentaacetic acid administration (Fig. 1). Neither venous thrombosis nor lymphadenopathy was found. The tumor was subsequently removed by laparoscopic surgery, and histologic examination revealed a leiomyosarcoma of the left adrenal gland. The microscopic appearance was that of a hypercellular tumor with a haphazard arrangement of spindled, oval, or rounded cells intermingled with bizarre tumor cells. After immunohistochemical staining, the tumor was found to be positive for desmin and negative for creatine kinase, myoglobin, S-100, CD34, CD117 (C-kit), and HMB-45. Ten months after surgery, the patient was alive and exhibited no symptoms or evidence of tumor recurrence.
Magnetic resonance images of a 3-cm left adrenal leiomyosarcoma. A T2-weighted, balanced, steady-state, free precession sequence (true fast imaging with steady state free precession [FISP]; repetition time [TR]/echo time [TE]/flip angle [FA] = 4.3 ms/2.1 ms/72 degrees) in coronal section shows a heterogeneous mass in the left suprarenal area. B T1-weighted spoiled gradient echo sequence (two-dimensional fast low-angle shot; TR/TE/FA = 150 ms/1.8 ms/70 degrees) in axial section displays a well-defined hypointense mass on the left adrenal gland. C T2-weighted turbo spin-echo sequence (TR/TE/FA = 2300 ms/94 ms/150 degrees) demonstrates a hyperintense tumor. D After contrast medium administration (gadolinium diethylenetriamine pentaacetic acid), the peripheral portion of the tumor is well enhanced and shows central necrosis.
Discussion
Primary smooth muscle tumors arising from the adrenal glands are rare and are believed to originate from the smooth muscle wall of the central adrenal vein and its branches. In almost all clinically reported cases to date, these tumors are larger than 10 cm in diameter. Patients presenting with such tumors range from 30 to 68 years of age. Females and males are approximately equally affected, and tumors occur in the right and left adrenals to approximately the same extent. With invasive diseases that include venous thrombosis, adjacent organ invasion, and distant metastases, the prognosis is extremely poor. Although tumor responses to radiation and chemotherapy are limited, early radical resection is associated with a better outcome. However, identification of the tumor at an early stage is difficult because symptoms are usually not present and because clinically applicable tumor markers are not currently available.
In the case described in this report, the patient presented with left flank pain. The tumor was therefore identified at a relatively early stage. Few MRI scans of primary adrenal leiomyosarcoma have been reported, and images of smaller (<5 cm) tumors are virtually nonexistent. The MRI evidence for extensive necrosis, in the 3-cm tumor described in this report indicates that such small tumors can be extremely aggressive in nature.
In conclusion, the imaging characteristics of adrenal leiomyosarcomas are indistinguishable from those of adrenal cortical carcinomas and metastatic cancers. However, adrenal cortical carcinomas are usually functional and capable of corticosteroid or sex steroid secretion. An early stage, centrally necrotic, and nonfunctioning adrenal tumor occurring in the absence of a primary malignancy should alert the physician to the possibility that a leiomyosarcoma is present.
References
Kato T, Kato T, Sakamoto S, et al. Primary adrenal leiomyosarcoma with inferior vena cava thrombosis. Int J Clin Oncol 2004;9:189–192
Thamboo TP, Liew LC, Raju GC. Adrenal leiomyosarcoma: a case report and literature review. Pathology 2003;35:47–49
Lujan MG, Hoang MP. Pleomorphic leiomyosarcoma of the adrenal gland. Arch Pathol Lab Med 2003;127:e32–e35
Matsui Y, Fujikawa K, Oka H, et al. Adrenal leiomyosarcoma extending into the right atrium. Int J Urol 2002;9:54–56
Fernandez JM, Huescar AM, Ablanedo P, et al. Primary leiomyosarcoma. A rare tumor of the adrenal gland. Arch Esp Urol 1998;51:1029–1031
Zetler PJ, Filipenko JD, Bilbey JH, Schmidt N. Primary adrenal leiomyosarcoma in a man with acquired immunodeficiency syndrome (AIDS). Further evidence for an increase in smooth muscle tumors related to Epstein-Barr infection in AIDS. Arch Pathol Lab Med 1995;119:1164–1167
Lack EE, Graham CW, Azumi N, et al. Primary leiomyosarcoma of adrenal gland. Case report with immunohistochemical and ultrastructural study. Am J Surg Pathol 1991;15:899–905
Choi SH, Liu K. Leiomyosarcoma of the adrenal gland and its angiographic features: a case report. J Surg Oncol 1981;16:145–148
Nakaishi M, Iseda T, Nishio S, et al. Spontaneous retroperitoneal hemorrhage from an adrenal leiomyosarcoma. Nishinihon J Urol 1999;61:466–467
Boman F, Gultekin H, Dickman PS. Latent Epstein-Barr virus infection demonstrated in low-grade leiomyosarcomas of adults with acquired immunodeficiency syndrome, but not in adjacent Kaposi’s lesion or smooth muscle tumors in immunocompetent patients. Arch Pathol Lab Med 1997;121:834–838
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lee, CW., Tsang, YM. & Liu, KL. Primary adrenal leiomyosarcoma. Abdom Imaging 31, 123–124 (2006). https://doi.org/10.1007/s00261-005-0343-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-005-0343-3