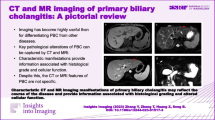
Abstract
Magnetic resonance imaging (MRI) findings of primary biliary cirrhosis (PBC; currently regarded as a vanishing bile duct syndrome) are not established. In this report, we describe our preliminary analysis of the relation between MRI findings and histopathologic staging of PBC and review clinical, morphologic, and MRI findings of PBC especially focusing on the staging of PBC.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Primary biliary cirrhosis (PBC) is a disease in which intrahepatic bile ducts are progressively destroyed [1]. Ahrens et al. defined this disease entity [2]. In the early stages, chronic nonsuppurative destructive cholangitis (CNSDC) occurs in the liver; after the cholestatic processes have progressed, the liver becomes cirrhotic [3]. The etiology of PBC is still unknown. However, immunologic abnormalities seem to contribute to the disease process, including bile duct destruction. Cholestasis follows cytotoxic T-cell attack of the biliary epithelium [4].
In many respects, PBC is similar to the graft-versus-host syndrome, as seen, for instance, after bone marrow transplantation and when the immune system has become sensitized to foreign HLA proteins [1, 5]. Sherlock and Dooley [1] suggested that PBC may be a spontaneous form of chronic liver rejection.
In this article, we review the general information about PBC for radiologists and present our preliminary analysis of the relation between magnetic resonance imaging (MRI) findings and the histopathologic staging of PBC.
Clinical features of PBC
Clinically, 90% of patients are female and usually middle age. The reason for the female predominance is unknown. In most cases, pruritus is the initial symptom, and jaundice appears within 2 to 3 years. Subsequently, hepatosplenomegaly and portal hypertension develop gradually. These cases are called symptomatic PBC.
However, in some cases, the only symptom is abnormal serum hepatobiliary enzyme levels (such as high alkaline phosphatase and γ-glutamyltranspeptidase) discovered during annual health checkups. Such cases are called asymptomatic PBC. The clinical course in the asymptomatic patient with PBC diagnosed early seems much longer (survival rate, ≥least 10 years) [6]. In contrast, those with symptomatic disease and jaundice survive about 7 years [7].
Diagnosis of PBC is based on the histopathologic finding of CNSDC and the presence of serum antimitochondrial antibody.
Ursodeoxycholic acid therapy appears to be effective in delaying or preventing the need for transplantation and improving survival rate. Liver transplantation is the treatment of choice for patients with advanced PBC. However, recurrence of PBC after liver transplantation has been described in up to 15% of patients [8].
Pathology of PBC
Pathologically, PBC is characterized by nonsuppurative inflammation and destruction of the interlobular bile ducts. Rubin et al. first described the histopathologic findings of PBC as CNSDC [3] (Fig. 1). Scheuer classified PBC into four stages based on findings of florid duct lesions (portal hepatitis; stage I), ductular proliferation and periportal hepatitis (stage II), scarring (bridging necrosis and septal fibrosis; stage III), and cirrhosis (stage IV) [9].
Nakanuma et al., by histometric evaluation, found that bile ducts with a lumen smaller than 70 to 80 μm are destroyed in PBC. Extensive destruction of the ducts was seen more frequently in the nonfibrotic stage of PBC than in later stages [10]. Destruction and disappearance of intrahepatic bile ducts in PBC is observed mainly in small bile ducts; however, active inflammation is observed even around larger bile ducts (Figs. 1, 2). These histopathologic changes can be observed as periportal inflammatory change on radiologic imaging.
Histologic staging and MRI findings of PBC
Periportal hyperintensity on T2-weighted MRI
MRI provides high-contrast resolution of soft tissues, and intrahepatic periportal hyperintensity on T2-weighted MR images represents edema, ductular proliferation, dilatation of lymph vessels, and inflammatory cell infiltration of portal tracts [11].
We previously reported that none of four cases with cirrhotic-stage (stage IV) PBC showed positive periportal hyperintensity on T2-weighted MR images [11]. However, our recent analysis showed that periportal hyperintensity on T2 weighted MR images is often observed, especially at earlier stages of PBC (Fig. 3). Periportal hyperintensity is thought to represent the periportal inflammation associated with CNSDC.
In our preliminary analysis, the incidences of the periportal hyperintensity on T2-weighted MRI at each histologic stage of PBC were 100% at stages I and II, 75% at stage III, and 33% at stage IV. This finding was considered to reflect active inflammation in the portal tracts. Therefore, the frequency of periportal hyperintensity may parallel the incidence of CNSDC in the each stage.
In the current study, periportal hyperintensity was seen even in the late stage of PBC (33% of stage IV cases showed this finding in our preliminary analysis). It may be explained by the fact that, even in Scheuer stage III or IV, the florid duct lesions were seen at histopathologic examination [12] (Fig. 2).
Arterial portal shunting on dynamic MRI
In PBC cases, small punctuated or segmental staining is sometimes observed in the early phase of dynamic MRI (Figs. 4, 5). Irreversible, small portal branch occlusions, which are caused by active inflammation in the portal tract (CNSDC), may induce arterial-portal shunting and may be observed as early contrast enhancement on dynamic MRI. Histopathologically, morphologic alteration of peribiliary vascular plexus, a network of capillaries that arises from the hepatic artery surrounding the intrahepatic bile ducts, is observed in early stages of PBC [13, 14, 15]. This event also may be related to intrahepatic microcirculatory disturbance and may cause this MR finding.
A 71-year-old man with PBC, Scheuer histologic stage III. Early phase (30 s) of axial dynamic-contrast enhanced T1-weighted MR image (SPGR;
repetition time/echo time, 165 ms/1.4 ms; flip angle, 90 degrees) demonstrates small punctuated staining on the lateral segment of the left liver lobe (arrow). This pattern indicates small arterial-portal shunting.
A 79-year-old man with PBC, Scheuer histologic stage IV. Early phase (30 s) of axial dynamic contrast-enhanced T1-weighted MR image (SPGR; repetition time/echo time, 165 ms/1.4 ms; flip angle, 90 degrees) depicts a small wedge-shaped stain on the medial segment of the liver (arrow), indicating small arterial-portal shunting.
In our preliminary analysis, the incidences of irregular segmental contrast enhancement on dynamic MRI at each PBC stage were 40% at stage I, 25% at stage II, 50% at stage III, and 67% at stage IV. The incidences of small punctuated staining on dynamic MRI of each stage of PBC were 20% at stage I, 0% at stage II, 25% at stage III, and 33% at stage IV. No significant correlation occurred between the incidence of these findings and the histologic stage of PBC. Because arterial-portal shunting caused by CNSDC is an irreversible event, the incidence of this finding on MRI may not change with the progression of PBC histopathologic stage.
Lymphadenopathy
Outwater et al. reported that lymphadenopathy is a frequent computed tomographic (CT) finding in PBC and that recognition of this association can help prevent misdiagnosis of lymphoma or metastatic disease. Specifically, CT scanning showed that 81% of patients have enlarged nodes in the gastrohepatic ligament and porta hepatis [16]. Enlarged paracardiac (24%) and mesenteric (19%) nodes are also seen [16]. Wenzel et al. also reported that 62% of PBC cases showed lymphadenopathy of the periportal, gastrohepatic ligament, or upper retroperitoneal nodes [17] (Fig. 6).
Regrettably, the relation between the incidence of lymphadenopathy and the histologic staging of PBC has not been investigated.
Portal hypertension and splenomegaly
Portal hypertension is a recognized complication of early histologic stages of PBC [10, 18] (Fig. 7). The reasons are not fully understood. It is thought that CNSDC and granuloma formation in the portal tract may cause obstruction of the intrahepatic portal venous branch and induce intrahepatic presinusoidal portal hypertension [19, 20].
We previously reported that patients with PBC present with significantly more severe splenomegaly in the noncirrhotic histologic stage and that splenomegaly persists thereafter (Fig. 8). Prolonged portal hypertension and other mechanisms, possibly related to immune disarrangement, may be responsible for the prominent splenomegaly in PBC [21].
Outwater et al., after a review of CT images of PBC patients, reported that 76% showed splenomegaly, whereas 43% showed cirrhosis [16].
MRI periportal halo sign
Wenzel et al. reported the occurrence of the MRI “periportal halo” sign, a conspicuous low-intensity signal abnormality centered around portal venous branches on T1- and T2-weighted MR images, in 43% of liver transplant recipients with PBC [17] (Fig. 9). Compared with patients with cirrhosis not caused by PBC, patients with cirrhosis due to PBC had a significantly high incidence of this finding, suggesting that this sign is highly specific for the diagnosis of PBC [17]. We believe this finding may apply to late stage PBC because, in our experience, early stage (stages I and II) PBC cases did not show this MR finding.
Hepatocellular carcinoma
Sherlock and Dooley reported that hepatocellular carcinoma (HCC) is a very rare feature of PBC, perhaps because true nodular cirrhosis develops so late [1]. Recently, Nakanuma et al. reported that about 4% of autopsied PBC cases had coexistent HCC [22]. Wenzel et al. reported 5% of their transplant recipients had HCC [17]. Jones et al. also reported that HCC developed in about 2.4% of PBC cases, all of which were stage III or IV [23].
In these studies, it was difficult to exclude the influence of the hepatitis virus infection, so whether PBC itself has hepatocarcinogenic potential remains unknown (Fig. 10).
A 79-year-old man with PBC, Scheuer histologic stage IV. Axial T2-weighted MR image (single-shot first spin echo; repetition time/echo time, 3500 ms/90 ms) depicts a 2-cm, slightly hyperintense round lesion on the anterior segment of the right liver (arrow). Diagnosis of HCC was confirmed by needle biopsy. A small liver cyst is also observed on this plane (arrowhead).
Nodular regenerative hyperplasia
Nodular regenerative hyperplasia (NRH) is a rare disorder of the liver characterized by the presence of multiple small nodules diffusely scattered in the parenchyma of the liver. The nodule ranges from 1 to 20 mm. The nodule consists of hyperplastic hepatocytes. Nakanuma et al. reported the association of NRH with portal hypertension in patients with early stages of PBC. Of 26 cases of stage I and II PBC, nine showed NRH [24]. However, there are no radiologic reports about the association between NRH and PBC.
Differential diagnosis of PBC
For diagnosis of PBC, radiographic demonstration of a normal biliary tree is usually essential to exclude other possible diagnoses such as hepatic masses, secondary biliary cirrhosis, subacute biliary obstruction, and sclerosing cholangitis [16]. Primary sclerosing cholangitis (PSC) should be excluded because PBC and PSC show chronic cholestatic features clinically. On imaging studies, PSC cases show irregular intra- and/or extrahepatic bile duct dilatation (Fig. 11). Ito et al. reported that the most common finding is intrahepatic bile duct dilatation (77%), followed by intrahepatic bile duct stenosis (64%), extrahepatic bile duct stenosis (50%), and intrahepatic bile duct beading (36%) [25]. In PBC cases, these segmental abnormalities in the major bile ducts are not seen, and the cholangiographic findings are usually normal or diffuse attenuation and narrowing of intrahepatic bile ducts [26] (Fig. 12). In addition, periportal hyperintensity in major portal tracts on T2-weighted image is usually marked and definite with PSC. Hence, it is not difficult to distinguish PSC from PBC by MRI, if the imaging findings show the features typical for PSC.
Conclusion
In this update, we present a preliminary analysis of our MRI findings of PBC and a review of the literature dealing with imaging findings in PBC patients. With improvement in diagnostic methods, the incidence of asymptomatic early stage PBC has increased. Currently, the staging of PBC depends on histopathologic diagnosis. However, the development of a radiologic, noninvasive surrogate staging method is anticipated.
References
S Sherlock J Dooley (1993) Primary biliary cirrhosis S Sherlock J Dooley (Eds) Diseases of the liver and biliary system EditionNumber9 Blackwell Scientific Publications London 236–248
EH Ahrens SuffixJr MA Payne HG Kunkel et al. (1950) ArticleTitlePrimary biliary cirrhosis Medicine (Baltimore) 29 299–364
E Rubin F Schaffner H Popper (1965) ArticleTitlePrimary biliary cirrhosis Am J Pathol 46 387–407 Occurrence Handle14266218 Occurrence Handle1:STN:280:DyaF2M%2FntVOmtg%3D%3D
G Balladini R Mirakian FB Bianchi et al. (1984) ArticleTitleAberrant expression of HLA-DR antigens on bile duct epithelium in primary biliary cirrhosis: relevance to pathogenesis Lancet 2 1009–1013 Occurrence Handle10.1016/S0140-6736(84)91108-5
O Epstein HC Thomas S Sherlock (1980) ArticleTitlePrimary biliary cirrhosis is a “dry gland” syndrome with features of chronic graft-versus-host disease Lancet 1 1166–1168 Occurrence Handle6103987 Occurrence Handle10.1016/S0140-6736(80)91621-9 Occurrence Handle1:STN:280:DyaL3c3gvVKiuw%3D%3D
DR Beswick G Klatskin JL Boyer (1985) ArticleTitleAsymptomatic primary biliary cirrhosis—long term follow-up and natural history Gastroenterology 89 267–271 Occurrence Handle4007417 Occurrence Handle1:STN:280:DyaL2M3jtFykug%3D%3D
S Sherlock (1959) ArticleTitlePrimary biliary cirrhosis (chronic intrahepatic obstructive jaundice) Gastroenterology 37 574–586 Occurrence Handle14445875 Occurrence Handle1:STN:280:DyaF3c7pvVKgsA%3D%3D
KD Lindor ER Dickson (1999) Primary biliary cirrhosis ER Schiff MF Sorrell WC Maddrey (Eds) Disease of the liver EditionNumber8 Lippincott-Raven Philadelphia 679–692
P Scheuer (1967) ArticleTitlePrimary biliary cirrhosis Proc R Soc Med 60 1257–1260 Occurrence Handle6066569 Occurrence Handle1:STN:280:DyaF1c%2FptVOguw%3D%3D
Y Nakanuma G Ohta K Kobayashi et al. (1982) ArticleTitleHistological and histometric examination of the intrahepatic portal vein branches in primary biliary cirrhosis without regenerative nodules Am J Gastroenterol 77 405–413 Occurrence Handle7091126 Occurrence Handle1:STN:280:DyaL383islKguw%3D%3D
O Matsui M Kadoya T Takashima et al. (1989) ArticleTitleIntrahepatic periportal abnormal intensity on MR images: an indication of various hepatobiliary diseases Radiology 171 335–338 Occurrence Handle2704798 Occurrence Handle1:STN:280:DyaL1M3gt1KktQ%3D%3D
J Ludwig ER Dickson GSA McDonald (1978) ArticleTitleStaging of chronic nonsuppurative destructive cholangitis (syndrome of primary biliary cirrhosis) Virchows Arch A Pathol Anat Histopathol 379 103–112 Occurrence Handle10.1007/BF00432479 Occurrence Handle1:STN:280:DyaE1c3ltF2qsg%3D%3D
S Kobayashi Y Nakanuma O Matsui (1994) ArticleTitleIntrahepatic peribiliary vascular plexus in various hepatobiliary diseases: a histological survey Hum Pathol 25 940–946 Occurrence Handle8088771 Occurrence Handle10.1016/0046-8177(94)90016-7 Occurrence Handle1:STN:280:DyaK2cznsV2qtg%3D%3D
K Washington PA Clavien P Killenberg (1997) ArticleTitlePeribiliary vascular plexus in primary sclerosing cholangitis and primary biliary cirrhosis Hum Pathol 28 791–795 Occurrence Handle9224746 Occurrence Handle10.1016/S0046-8177(97)90151-9 Occurrence Handle1:STN:280:DyaK2szmsl2kuw%3D%3D
Y Matsunaga T Terada (1999) ArticleTitlePeribiliary capillary plexus around interlobular bile ducts in various chronic liver diseases: an immunohistochemical and morphometric study Pathol Int 49 869–873 Occurrence Handle10571819 Occurrence Handle10.1046/j.1440-1827.1999.00959.x Occurrence Handle1:STN:280:DC%2BD3c%2FktVSruw%3D%3D
E Outwater MM Kaplan MS Bankoff (1989) ArticleTitleLymphadenopathy in primary biliary cirrhosis: CT observations Radiology 171 731–733 Occurrence Handle2717743 Occurrence Handle1:STN:280:DyaL1M3ktFaisw%3D%3D
JS Wenzel A Donohoe KL Ford SuffixIII et al. (2001) ArticleTitlePrimary biliary cirrhosis: MR imaging findings and description of MR imaging periportal halo sign AJR 176 885–889 Occurrence Handle11264071 Occurrence Handle10.2214/ajr.176.4.1760885 Occurrence Handle1:STN:280:DC%2BD3M3hslahsg%3D%3D
S Sherlock (1982) ArticleTitleNoncirrhotic extrahepatic and intrahepatic portal hypertension Semin Liver Dis 2 202–210 Occurrence Handle6891100 Occurrence Handle10.1055/s-2008-1040708 Occurrence Handle1:STN:280:DyaL3s%2FptlWjsQ%3D%3D
Y Nakanuma G Ohta (1979) ArticleTitlePortal hypertension of patients with primary biliary cirrhosis: its pathogenesis and comparison with other liver disease using histometric methods Acta Hepatol Jpn 20 388–395 Occurrence Handle10.2957/kanzo.20.388
S Arora M Kaplan (1987) ArticleTitlePortal hypertension in early stage primary biliary cirrhosis: a possible explanation Am J Gastroenterol 82 90–91 Occurrence Handle3799588 Occurrence Handle1:STN:280:DyaL2s%2FpslWquw%3D%3D
N Terayama KP Makimoto S Kobayashi et al. (1994) ArticleTitlePathology of the spleen in primary biliary cirrhosis: an autopsy study Pathol Int 44 753–758 Occurrence Handle7834076 Occurrence Handle10.1111/j.1440-1827.1994.tb02922.x Occurrence Handle1:STN:280:DyaK2M7jsFGqtw%3D%3D
Y Nakanuma T Terada K Doishita et al. (1990) ArticleTitleHepatocellular carcinoma in primary biliary cirrhosis: an autopsy study Hepatology 11 1010–1016 Occurrence Handle1694811 Occurrence Handle10.1002/hep.1840110616 Occurrence Handle1:STN:280:DyaK3czgs1yrug%3D%3D
DEJ Jones JV Metcalf JD Collier et al. (1997) ArticleTitleHepatocellular carcinoma in primary biliary cirrhosis and its impact on outcomes Hepatology 26 1138–1142 Occurrence Handle9362353 Occurrence Handle10.1002/hep.510260508 Occurrence Handle1:STN:280:DyaK1c%2Fis1KktA%3D%3D
Y Nakanuma G Ohta (1987) ArticleTitleNodular hyperplasia of the liver in primary biliary cirrhosis of early histological stages Am J Gastroenterol 82 8–10 Occurrence Handle3799585 Occurrence Handle1:STN:280:DyaL2s%2FpslWqtA%3D%3D
K Ito DG Mitchell EK Outwater et al. (1999) ArticleTitlePrimary sclerosing cholangitis: MR imaging features AJR 172 1527–1533 Occurrence Handle10350284 Occurrence Handle10.2214/ajr.172.6.10350284 Occurrence Handle1:STN:280:DyaK1M3nslOrtQ%3D%3D
DA Legge HC Carlson ER Dickson et al. (1971) ArticleTitleCholangiographic findings in cholangiolitic hepatitis: syndrome of primary biliary cirrhosis AJR 113 16–20 Occurrence Handle10.2214/ajr.113.1.16 Occurrence Handle1:STN:280:DyaE38%2FgvV2itQ%3D%3D
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kobayashi, S., Matsui, O., Gabata, T. et al. MRI findings of primary biliary cirrhosis: correlation with Scheuer histologic staging. Abdom Imaging 30, 71–76 (2004). https://doi.org/10.1007/s00261-004-0228-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-004-0228-x