Abstract
Purpose
Overexpression of HER2 receptors is a prognostic and predictive biomarker in breast cancer and a number of other malignancies. Radionuclide molecular imaging of HER2 overexpression may influence patient management making treatment more personalized. Earlier, 111In-DOTA-ZHER2:342-pep2 (ABY-002) Affibody molecule demonstrated excellent imaging of HER2-expressing xenografts in mice shortly after injection. The use of the positron-emitting nuclide 68Ga instead of 111In might increase both the sensitivity of HER2 imaging and accuracy of expression quantification. The goal of this study was to prepare and characterize 68Ga-labelled ABY-002.
Methods
68Ga labelling of ABY-002 was optimized. In vitro cell binding and procession of 68Ga-ABY-002 was evaluated. Biodistribution and tumour targeting of 68Ga-ABY-002 and 111In-ABY-002 was compared in vivo by paired-label experiments.
Results
ABY-002 was incubated with 68Ga at 90°C for 10 min resulting in a radiochemical labelling yield of over 95%. Capacity for specific binding to HER2-expressing cells was retained. In vivo, both 68Ga-ABY-002 and 111In-ABY-002 demonstrated specific targeting of SKOV-3 xenografts and high-contrast imaging. Background radioactivity in blood, lungs, gastrointestinal tract and muscle fell more rapidly for 68Ga-ABY-002 compared with 111In-ABY-002 favouring imaging shortly after injection. For 68Ga-ABY-002, a tumour uptake of 12.4 ± 3.8%ID/g and a tumour to blood ratio of 31 ± 13 were achieved at 2 h post-injection.
Conclusion
68Ga-ABY-002 is easy to label and provides high-contrast imaging within 2 h after injection. This makes it a promising candidate for clinical molecular imaging of HER2 expression in malignant tumours.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Human epidermal growth factor type 2 (HER2, ErbB 2) is a transmembrane tyrosine kinase belonging to the HER (ErbB) family of tyrosine kinase receptors [1]. Signalling of HER2 receptors occurs by several pathways, resulting in cell division, suppression of apoptosis and increasing of cell motility [1]. Interestingly, there is no known ligand to HER2 and this receptor acts by heterodimerization with other members of the HER family [2]. Overexpression of HER2 is associated with malignant transformation of cells and has been detected in a significant fraction of breast, urinary bladder, ovarian, colorectal and prostate cancers [3]. Disruption of HER2 signalling by the monoclonal antibody trastuzumab or the tyrosine kinase inhibitor lapatinib improves survival of patients with metastatic breast cancer. The American Association of Clinical Oncology [4] and European Group on Tumor Markers [5] recommend assessment of HER2 expression in each breast tumour at the time of diagnosis or recurrence in order to select patients who would benefit from anti-HER2 therapy. The clinical potential of detection of HER2 overexpression is not limited to breast cancer. Predictive and/or prognostic values of HER2 overexpression in ovarian [6], lung [7] and prostate [8] carcinomas have been reported. In prostate cancer, high HER2 expression is highly associated with androgen independence [9].
The use of radionuclide molecular imaging might improve diagnostics of HER2 expression in metastatic cancer, adding the clear advantages of being global, minimally invasive, less sensitive to intratumoural heterogeneity of expression and applicable for repeated use enabling quantification of expression changes due to disease progression and/or therapy. It has been stated, for example, that HER2 expression varies with the clinical state of patients with prostate carcinoma and sampling of metastases is required for an accurate HER2 profiling [10]. This is not feasible by biopsy, but is possible using radionuclide imaging. Different targeting agents based on intact monoclonal antibodies, antibody fragments and molecular display-selected peptides have been evaluated for in vivo imaging of HER2 expression (for reviews see [11, 12]). Preclinical data showed that small high-affinity targeting proteins provide the best sensitivity and specificity of HER2 imaging due to rapid tumour targeting and rapid clearance from healthy non-HER2-expressing tissues. Exceptionally high imaging contrast has been obtained using small (7 kDa) targeting proteins called Affibody molecules. Affibody molecules originate from the 58 amino acid scaffold of the Z domain, which was derived from staphylococcal protein A. This three-helix bundle Z protein lacks cysteines and is composed of a single polypeptide subunit capable of rapid folding. The scaffold has been subjected to randomization of 13 surface-exposed residues to generate a library from which high-affinity binders to different targets have been selected by phage display [13]. Preclinical studies demonstrated that derivatives of the HER2-binding Affibody molecule ZHER2:342, which are labelled with single photon emitters 125I (surrogate of 123I), 111In and 99mTc, provide high-contrast imaging of HER2-expressing xenografts in mice within 0.5–1 h after injection [14]. A clear advantage of Affibody molecules is their robustness, which enables the use of harsh labelling conditions, such as elevated temperatures (up to 90°C), broad range of pH or high concentration of reducing agents without affecting binding properties [14].
The use of positron emission tomography (PET) for detection of HER2 expression or assessment of changes in the HER2 level in response to therapy might further extend the diagnostic utility of Affibody molecules. This prompted evaluation of the positron-emitting nuclides 76Br [15], 18F [16, 17], 57Co (surrogate for 55Co) [18] and 124I [19] for labelling of HER2-binding Affibody molecules. These studies confirmed a high potential for combining Affibody-mediated targeting and PET. Particularly, the feasibility of monitoring changes in HER2 expression in murine xenografts in response to anti-HSP90 therapy has been demonstrated [20]. The use of the generator-produced 68Ga (T 1/2 = 1.14 h) is potentially a convenient way to improve the availability of positron-emitting Affibody-based tracers. Previous studies have demonstrated that the short biological half-life of ZHER2:342 is compatible with the physical half-life of 68Ga.
Several 68Ge/68Ga generator systems have been developed (for a recent review, see [21]). The generator based on an TiO2 ion exchanger may be the most suitable for practical use because it permits elution of the daughter nuclide with relatively low molarity (0.1 M) hydrochloric acid [22–24] and because titanium is not toxic. As all chelator-based methods, labelling with 68Ga is sensitive to the presence of metal impurities in the generator eluate and reaction buffers. Cation exchange- [24] and anion exchange- [22, 25] based purification and concentration of 68Ga eluate have been described. However, it was also demonstrated [22, 23, 26] that high yield and reasonably high specific radioactivity of labelled peptides might be obtained by the use of supra-pure eluent and buffer components and the use of eluate fractions with the highest radioactivity concentrations. A further advantage is the simple instrumentation required, enabling implementation by relatively inexperienced personnel. In the current study, we have adopted this labelling method.
A recently published excellent review of radiopharmaceutical chemistry of 68Ga suggests that 1,4,7,10-tetra-azacylododecane-N,N′,N″,N′″-tetraacetic acid (DOTA) is a suitable chelator for 68Ga labelling of peptides [27]. For this reason, a chemically manufactured DOTA derivative of the HER2-binding Affibody molecule ZHER2:342, DOTA-ZHER2:342 (ABY-002), having an apparent dissociation constant (KD) of 65 pM [28], was selected for the present study. Site-specific coupling of DOTA to the N-terminus of ZHER2:342 during peptide synthesis provides a homogeneous conjugate with well-defined chemical and biological properties. Previous studies showed that HER2-expressing xenografts in mice were clearly visualized by clinical gamma camera as early as 1 h after injection of 111In-ABY-002 [28]. This was a strong indication that ABY-002 would be a suitable candidate also for labelling with 68Ga. However, a number of studies on DOTA-conjugated short peptides have demonstrated that exchange of 111In for 68Ga can considerably alter both uptake in normal organs and tumour-targeting properties [29–31]. A further understanding of the influence of various radiometals on biodistribution of Affibody molecules is essential for the design of future Affibody tracers.
The goals of this study were: to establish labelling of ABY-002 with 68Ga, to evaluate cellular processing, biodistribution and tumour-targeting properties of 68Ga-ABY-002 and to compare those with properties of 111In-ABY-002 under uniform conditions provided by co-injection of both tracers.
Materials and methods
Materials
A synthetic ABY-002 (DOTA-ZHER2:342) was supplied by Affibody AB, Bromma, Sweden, in a freeze-dried form. The ABY-002 Affibody molecule was synthesized by standard Fmoc procedure in a single chemical process and characterized as described by Orlova and co-workers [28]. For a site-specific labelling control experiment, a recombinant non-DOTA-containing ZHER2:342 Affibody molecule was provided by Affibody AB. Labelling of ABY-002 with 111In for a comparative biodistribution study was performed as described in [28]. Buffers, such as 0.1 M phosphate-buffered saline (PBS), pH 7.5, and 1.25 M ammonium acetate, pH 4.2, were prepared using common methods from chemicals supplied by Merck (Darmstadt, Germany). High-quality Milli-Q© water (resistance higher than 18 MΩ/cm) was used for preparing solutions. Buffers, which were used for labelling, were purified from metal contamination using Chelex 100 resin (Bio-Rad Laboratories, Richmond, CA, USA). The 68Ge/68Ga generator (50 mCi, Eckert and Ziegler, Berlin, Germany) was eluted with 0.1 M hydrochloric acid (prepared from 30% ultra-pure HCl from Merck). At the time of the experiments, the generator was 20 months old. 111In-indium chloride was purchased from Covidien (Dublin, Ireland). Cells in the in vitro experiments were detached using trypsin-ethylenediaminetetraacetate (EDTA) solution (0.25% trypsin, 0.02% EDTA in buffer, Biochrom AG, Berlin, Germany). Ketalar (ketamine, 50 mg/ml, Pfizer, New York, NY, USA), Rompun (xylazine, 20 mg/ml, Bayer, Leverkusen, Germany) and heparin (5,000 IE/ml, Leo Pharma, Copenhagen, Denmark) were obtained commercially. The radioactivity was measured using an automated gamma counter with 3-inch NaI(Tl) detector (1480 WIZARD, Wallac Oy, Turku, Finland).
Data on cellular uptake were analysed by unpaired, two-tailed t test using GraphPad Prism (version 4.00 for Windows GraphPad Software, San Diego, CA, USA) in order to determine significant differences (p < 0.05). For a dual-isotope animal study, a paired, two-tailed t test was applied.
Analytical methods
High-performance liquid chromatography (HPLC) analysis was performed using a system from Beckman (Fullerton, CA, USA) consisting of a 126 pump, a 166 UV detector and a radiation detector coupled in series. Data acquisition and handling were performed using the Beckman System Gold Nouveau Chromatography Software Package. The column used was a Vydac RP 300 Å HPLC column (Grace Vydac, Columbia, MD, USA) with the dimensions 150 × 4.6 mm, 5-µm particle size. The applied gradient elution had the following parameters: mobile phase A: 10 mM trifluoroacetic acid (TFA) in water; mobile phase B: 70% acetonitrile, 30% H2O, 10 mM TFA; mobile phase flow rate: 1.0 ml/min; the gradient elution profile: 0–2 min isocratic 20% B, 8 min linear gradient 20–90% B, 2 min linear gradient 90–20% B. UV detection was performed at 280 nm. The 68Ga-ABY-002 sample was spiked with non-labelled ABY-002. Retention times (tR) for the UV- and radio-HPLC signals were 7.7 ± 0.02 and 7.80 ± 0.02 min for ABY-002 and 68Ga-ABY-002, respectively. To control the recovery of free 68Ga and 68Ga-ABY-002 from the HPLC system and, in particular, from the Vydac RP HPLC column, the radioactivity of the loaded sample and the fractions collected from the outlet of the HPLC system were measured in a dose calibrator (CAPINTECH CRC-120). The recovery of the free 68Ga injected alone was ∼98%. The radioactivity recovery in the case of 68Ga-ABY-002 was over 91%.
Radio-instant thin-layer chromatography (ITLC) analysis was performed using 150–771 DARK GREEN, Tec-Control Chromatography strips from Biodex Medical Systems (Shirley, NY, USA), eluted with 0.2 M citric acid, pH 2.0. In this system, radiolabelled Affibody molecules remain at the origin, while 68Ga-acetate and 68Ga-EDTA (during EDTA challenge experiment) migrated with the running buffer front. The analytical system was verified using a blank experiment, where no Affibody molecule was added to the reaction mixture. Blank experiments showed that less than 0.5% of radioactivity remained at the application point of ITLC. The identity of 68Ga-ABY-002 was confirmed by a reverse phase HPLC analysis. Sodium dodecyl sulphate polyacrylamide gel electrophoresis (SDS-PAGE), 200 V constant, was performed using NuPAGE 4–12% Bis-Tris Gel (Invitrogen AB, Lidingö, Sweden) in MES buffer (Invitrogen AB, Lidingö, Sweden). Distribution of radioactivity along the ITLC strips and SDS-PAGE gels was measured on a Cyclone™ Storage Phosphor System and analysed using the OptiQuant™ image analysis software (both from Perkin Elmer Sweden AB, Stockholm, Sweden).
Labelling and stability
The generator was pre-eluted 3 h before the labelling. The generator was eluted with 250-µl fractions of 0.1 M HCl. Fraction 4 containing the maximum radioactivity (41 ± 8%) was used for labelling.
To establish the optimum labelling condition, a solution of ABY-002 (50 µg, 7 nmol) in 210 µl 1.25 M ammonium acetate, pH 4.2, was mixed with 230 μl 68Ga-containing eluate. The mixture was incubated at room temperature, 60°C or 90°C. At 5, 10, 15, 20 and 30 min after start of incubation, a small aliquot (0.8 μl) of reaction mixture was taken and analysed by radio-ITLC. The experiments were performed at least in duplicates. For further experiments (stability tests, in vitro and in vivo studies), labelling at 90°C during 10 min was selected.
To verify that 68Ga labelling was DOTA mediated, a control labelling of recombinant ZHER2:342 without DOTA was performed under exactly the same conditions as for 68Ga-ABY-002. The labelling outcome was monitored by reverse phase HPLC analysis. The analyte sample was spiked with ABY-002 used as an authentic reference.
The stability of 68Ga-ABY-002 was demonstrated in two experiments. During the EDTA challenge test, two samples were diluted with 500-fold molar excess of disodium salt of EDTA solution in water, while two control samples were diluted with an equal amount of water. After 4 h of incubation at room temperature, all samples were analysed using radio-ITLC. To evaluate serum stability, two samples of 68Ga-ABY-002 (purity 98.2%) were mixed with murine serum to mimic tracer concentration immediately after injection. A control sample was diluted with an equal volume of PBS. The samples were incubated at 37°C during 60 min. The incubation time was selected based on previous data on biodistribution of Affibody molecules, which showed that more than 95% of Affibody-related radioactivity was cleared from the blood at 1 h after injection. After incubation in serum, the samples were treated with sample buffer (10 min at 70°C) and analysed using SDS-PAGE. To provide a marker for low-molecular weight radioactivity, a sample of 68Ga-acetate was applied next to the analytes on the same gel.
In vitro studies
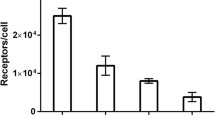
Specificity of the 68Ga-ABY-002 binding to HER2-expressing cells was evaluated using ovarian carcinoma SKOV-3 and prostate carcinoma DU-145 cell lines [purchased from American Type Tissue Culture Collection (ATCC) via LGC Promochem, Borås, Sweden]. SKOV-3 was selected because it has a high level of HER2 expression (1.2 × 106 receptors per cell [32]) and was used in our earlier studies on radiolabelled Affibody molecules. The DU-145 cell line (5 × 104 receptors per cell, A. Orlova, unpublished results) was selected because of our intention to visualize HER2 expression in prostate cancer in future studies. An in vitro specificity test was performed according to the methods describe earlier [33]. Briefly, a solution of 68Ga-ABY-002 (3 ng protein per dish) was added to six Petri dishes (ca. 106 cells in each). For blocking, a 500-fold excess of non-labelled recombinant ZHER2:342 was added 5 min before 68Ga-ABY-002 to saturate the receptors. The cells were incubated during 1 h in a humidified incubator at 37°C. Thereafter, the media was collected, the cells were detached by trypsin-EDTA solution and the radioactivity in cells and media was measured to calculate a percentage of cell-bound radioactivity.
The antigen-binding capacity (ABC) was analysed according to the method described and validated by Wållberg and co-workers [18]. The SKOV-3 cells were scraped from culture flasks and three cell pellets containing 107 cells were formed in Eppendorf tubes by gentle centrifugation. The supernatant was discarded. A solution of 68Ga-ABY-002 in cell culture medium (1 ml, 0.26 pmol) was added to each pellet to provide approximately 100-fold molar access of receptor over conjugate. The cells were gently resuspended and incubated for 1 h at 4°C under gentle shaking. After incubation, cells were pelleted and 0.5 ml of the supernatant was transferred to Eppendorf tubes. The radioactivity of the samples was measured and the ABC was calculated as
A study concerning retention and processing of 68Ga-ABY-002 by SKOV-3 cells was performed according to the method developed and validated by Wållberg and Orlova [33].
The cells were incubated with the labelled compound at 4°C using a 5:1 molar ratio of Affibody molecule to HER2. After 15 min of incubation the labelled compound was removed and the cells were washed three times with ice-cold serum-free medium. Then 1 ml complete medium was added to each cell dish and the cells were further incubated at 37°C, 5% CO2. At predetermined time points (0, 0.5, 1, 2, 3 and 4 h after media changing), the medium from a set of three dishes was collected and the cells were washed three times with ice-cold serum-free medium. The cells were subsequently treated with 0.5 ml 0.2 M glycine buffer with 4 M urea, pH 2.0, for 5 min on ice. The acidic solution was collected and the cells were washed additionally with 0.5 ml glycine buffer, which was collected and pooled with the first fraction before radioactivity was measured. The radioactivity in the acid wash fraction was considered as membrane-bound radioactivity. After addition of 0.5 ml 1 M NaOH, cells were incubated at 37°C for 0.5 h before the alkaline fraction was collected. The cell dishes were washed with an additional 0.5 ml NaOH before the radioactivity in the alkaline fraction was measured. This fraction of radioactivity was considered as internalized.
In vivo studies
The goal of the experiments was comparative evaluation of 68Ga and 111In labels on biodistribution and targeting properties of ABY-002. All animal experiments were planned and performed in accordance with national legislation on laboratory animals’ protection and were approved by the Local Ethics Committee for Animal Research. In order to reduce the number of animals in the experiments, a dual-label approach was used when 68Ga- and 111In-labelled ABY-002 were co-injected in the same mice. Before the animal study, the gamma spectra of 111In and 68Ga were recorded using a gamma spectrometer. A summation peak of 111In overlapped partially with the annihilation peak of 68Ga; however, no indium counts were registered in channels for 540 keV and higher. Radioactivity in these channels was used for measurement of 68Ga radioactivity in biological samples. 111In radioactivity was measured in the energy range from 140 to 510 keV (using both photopeaks and summation peak) at least 24 h after measurement of 68Ga, when all 68Ga radioactivity was decayed.
The mice were euthanized at predetermined time points by an intraperitoneal injection of Ketalar-Rompun solution (20 μl of solution/g body weight: Ketalar, 10 mg/ml; Rompun, 1 mg/ml) followed by heart puncture with a 1-ml syringe rinsed with heparin (5,000 IE/ml). Blood and organ samples: lung, liver, spleen, kidneys, tumour (from xenografted mice), muscle, bone, gastrointestinal tract (with content) and the remaining carcass were collected, weighed and the radioactivity measured as describe above. The standards of injected radioactivity were prepared at the time of injection. The data were corrected for background radiation, gamma spectrometer dead time percentage during each measurement and decay during measurement. The organ uptake values were calculated as percent of injected dose per gram of tissue (%ID/g), except for the gastrointestinal tract and the remaining carcass, which were calculated as %ID per whole sample.
To study the influence of 111In and 68Ga labels on biodistribution of ABY-002, female NMRI mice (18 weeks old, weight 30 ± 3 g) were used. All animals received 4 µg (0.56 nmol) ABY-002 diluted in 100 μl PBS. All animal groups were injected with 10 kBq 111In-DOTA-ZHER2:342 per animal. The 68Ga-ABY-002 radioactivity was adjusted to 58, 110 and 205 kBq per mouse for groups (n = 4 or 3), which should be sacrificed 45 min, 2 h and 3 h after injection, respectively. The mixtures were injected into tail veins. At 45 min, 2 h or 3 h post-injection (p.i.), a group of three or four mice was sacrificed and dissected.
Comparison of tumour targeting was performed in female BALB/c nu/nu mice (15 weeks old, weight 22 ± 2 g) carrying SKOV-3 xenografts. Cells (107 cells per mouse) were implanted subcutaneously on the right hind leg 5 weeks before the experiment. At the time of injection, the average tumour weight was 75 ± 7 mg. The mice were injected with a mixture of 10 kBq 111In-ABY-002 and 58 kBq (45 min time point) or 110 kBq (2 h time point) of 68Ga-ABY-002 in 100 μl PBS. The total amount of ABY-002 was adjusted to 4 µg (0.56 nmol) per animal by non-labelled ABY-002. To check the specificity of xenograft targeting, a group of three mice was subcutaneously pre-injected (neck area) with 500 µg (70 nmol) non-labelled recombinant ZHER2:342 Affibody molecule. The control group was sacrificed at 2 h p.i.
To confirm the capacity of the conjugates to visualize HER2-expressing tumours an in vivo imaging experiment was performed. For this purpose, two SKOV-3 xenograft-bearing mice were co-injected with 1 MBq 111In-ABY-002 and 1.5 MBq 68Ga-ABY-002 (amount of peptide 4 µg). Immediately before imaging, 2 h p.i., the animals were sacrificed by overdosing Ketalar-Rompun. After euthanasia, the urine bladders were excised. The PET imaging of 68Ga-ABY-002 was performed using a clinical scanner, GE Discovery VCT PET/CT, at the department of Nuclear Medicine at Uppsala University Hospital. It was made in 3-D mode with a 30-min image reconstructed in a 256 × 256 matrix with a 30-cm field of view (FOV).
The animal cadavers were frozen immediately after PET imaging. The gamma camera imaging was performed 24 h after PET imaging, after complete decay of 68Ga (21 half-lives).
The imaging experiment was performed using a GE Infinia gamma camera equipped with a medium energy general purpose (MEGP) collimator. Static images (30 min) were obtained with a zoom factor of 3 in a 256 × 256 matrix.
Results
Labelling and stability
The kinetics of 68Ga-ABY-002 formation at different temperatures is presented in Fig. 1. The labelling at room temperature was inefficient. Increasing the reaction temperature to 60°C improved the yield; however, the analytical radiochemical (decay-corrected) yield was only 87 ± 2% (n = 3) after 30 min of incubation. Further temperature increase to 90°C resulted in an increase of the radiochemical yield to 98.6 ± 0.7% (n = 12) within 10 min. For further experiments, the ABY-002 was labelled at 90°C and used without further purification.
The reverse phase radio-HPLC confirmed identity and purity of 68Ga-ABY-002 (Fig. 2). In the control experiments on the 68Ga labelling of recombinant ZHER2:342 without DOTA, no radio-HPLC signal associated with UV-HPLC signal of ZHER2:342 could be detected (data not shown). This result confirms that the 68Ga labelling of ABY-002 is site specific and DOTA mediated.
Stability of 68Ga-ABY-002 was evaluated by a challenge with 500-fold molar excess EDTA and by incubation in murine serum at 37°C. The EDTA challenge demonstrated very high labelling stability. The radiochemical purity of treated samples was 98.7 ± 0.3% (average ± SEM), while the purity of the untreated control was 99.4 ± 0.3%, i.e.,the difference was within the accuracy of the analytical method. 68Ga-ABY-002 was stable in murine serum. SDS-PAGE demonstrated that 94.4 ± 0.9% (average ± SEM) of the radioactivity was associated with 68Ga-ABY-002 after 1 h of incubation at 37°C (Fig. 3). In the control sample, which was incubated at 37°C in PBS, 95.3% of radioactivity was attached to ABY-002.
SDS-PAGE analysis of 68Ga-ABY-002 stability in serum. Distribution of radioactivity along lanes was visualized and quantified using Cyclone™ Storage Phosphor System. 1 68Ga-ABY-002 sample, which was incubated in murine serum at 37°C for 1 h. 2 68Ga-ABY-002 sample, which was incubated in PBS at 37°C for 1 h. 3 68Ga-gallium acetate was used as a marker for low molecular weight compounds
In vitro studies
Binding specificity tests demonstrated that the binding of 68Ga-ABY-002 to living HER2-expressing cells was receptor mediated, because saturation of the receptors by pre-incubation with non-labelled ZHER2:342 significantly decreased the binding of the radiolabelled Affibody molecule (for all studied cell lines, p < 0.0001). The level of cell-associated radioactivity was appreciably lower for non-blocked DU-145 cell line (2.17 ± 0.05%) than for SKOV-3 cell line (39.8 ± 0.9%), reflecting lower expression level of HER2.
The antigen-binding capacity after labelling was retained to a very high extent: 89.4 ± 1.4% of conjugate was bound to SKOV-3 cells after incubation during 1 h at approximately 100-fold receptor excess.
The retention and processing of 68Ga-ABY-002 by HER2-expressing SKOV-3 cells are presented in Fig. 4. The data were similar to data for other ZHER2:342-based radiolabelled conjugates [18, 33]. Cellular retention of radioactivity was high. After a short dissociation phase during the first 30 min, the level of cell-associated radioactivity did not change appreciably between 0.5 (77.7 ± 1.1% of initial level) and 4 h (73.0 ± 0.8%) of incubation. The internalization of the compound was relatively slow, although continuously increasing throughout the experiment. After 4 h of incubation, 12.4 ± 0.5% of the radioactivity was internalized by SKOV-3 cells.
Retention and internalization of 68Ga-ABY-002 by HER2-expressing SKOV-3 cell line. Cells were pre-incubated with 68Ga-ABY-002 on ice, and then the culture medium was changed. Data are presented as an average of three samples with standard deviations; error bars might be not seen because they are smaller than the symbols
In vivo studies
Data concerning biodistribution of 68Ga-ABY-002 and 111In-ABY-002 in normal NMRI mice at 45 min, 2 h and 3 h p.i. are presented in Table 1. Biodistribution of both compounds was characterized by rapid renal clearance from blood. Radioactivity accumulation in the gastrointestinal tract (a measure for hepatobiliary excretion) was low. Renal clearance from the body was accompanied by reabsorption of radioactivity in kidneys. The levels of renal uptake did not differ significantly between conjugates. Interestingly, the radioactivity level of 68Ga-ABY-002 was significantly lower in blood, lung, muscle and bone at all time points after administration compared with the levels seen with 111In-ABY-002. The whole-body clearance rate of 68Ga-ABY-002 was also higher.
Data concerning targeting of HER2-expressing SKOV-3 xenografts in BALB/c nu/nu mice are presented in Tables 2 and 3 and Fig. 5. The data were in good agreement with data for NMRI mice. This experiment also demonstrated a significantly lower level of 68Ga-ABY-002 uptake in blood, lung, spleen and gastrointestinal tract. The tumour uptake at 2 h p.i. was high, 12.4 ± 3.8 and 15.2 ± 4.8%ID/g for 68Ga-ABY-002 and 111In-ABY-002, respectively, and did not differ significantly between the two conjugates. The tumour uptake of both conjugates was dramatically reduced by pre-saturation of HER2 receptors in tumours using non-labelled ZHER2:342 (Fig. 5), confirming the targeting specificity. The tumour to organ ratios were high for all studied organs except kidneys (Table 3) and did not differ significantly between the conjugates.
In vivo binding specificity of 68Ga-ABY-002 (left panel) and 111In-ABY-002 (right panel), 2 h p.i. The total injected ABY-002 dose per mouse was 4 µg (0.56 nmol). The blocked group was subcutaneously pre-injected with an excess amount (500 µg, 70 nmol) of non-labelled ZHER2:342. Results are presented as percentage of injected dose per gram of tissue (%ID/g). Statistical significance in the tumour uptake between the groups, according to Student’s t test gave p < 0.05
PET and gamma camera images of radioactivity distribution 2 h after the i.v. injection of the 111In-ABY-002 and 68Ga-ABY-002 into immunodeficient mice bearing subcutaneous SKOV-3 xenografts confirmed that HER2-expressing tumours could be visualized at this time point (Fig. 6). As predicted from the biodistribution studies, substantial renal retention of radioactivity was visualized for both conjugates. Other organs and tissues were not seen with either conjugate. Rapid clearance of the conjugates provided very low background radioactivity and ensured high imaging contrast.
Imaging of HER2 expression in SKOV-3 xenografts in BALB/c nu/nu mice using PET (panel A) and gamma camera (panel B). The animals were injected with a mixture of 68Ga-ABY-002 and 111In-ABY-002 (totally 4 µg, 0.56 nmol). Animals were sacrificed 2 h p.i. and the PET image was acquired. Gamma camera image was acquired 24 h later, after decay of 68Ga. To facilitate interpretation, animal contours were derived from a digital photograph and superimposed over the PET and gamma camera image. Arrows show tumour (T) and kidneys (K) in one representative animal
Discussion
The results of this study demonstrate that it is possible to label DOTA-containing anti-HER2 Affibody molecule with 68Ga with preserved capacity to specifically target HER2-expressing cells both in vitro and in vivo. Generally, post-elution concentration and purification of 68Ga and the use of microwave-assisted labelling improves a specific radioactivity of 68Ga-labelled peptides [22]. However, high specific radioactivity is not required with 68Ga-ABY-002, because of very high expression of HER2 in malignant tumours and the absence of agonistic activity of the tracer. Preclinical data demonstrated that the uptake of 111In-ABY-002 in SKOV-3 xenografts does not differ significantly in the range of injected mass between 0.1 and 10 µg (14 pmol to 1.4 nmol) per mouse [34]. For this reason, a simple and robust approach, which excludes post-elution treatment of 68Ga [22, 23], was selected. This methodology does not require sophisticated equipment apart from the 68Ga generator and a controlled heating block and enables kit formulation. The amount of radioactivity obtained by fractionation of the generator eluate is lower than may be achieved by pre-concentration. Nevertheless, we believe that the methodology may provide sufficient amount of radioactivity and can be implemented in any radiopharmaceutical laboratory qualified for labelling of 99mTc kits or 111In-Octreoscan. This factor is essential because of an increasing number of satellite PET/CT scanners, which are not co-located with cyclotrons and rely on shipment of 18F-FDG and other tracers from central dispensaries. Production of 68Ga-based tracers would enhance the capacity of such satellite scanners.
Efficient labelling required incubating the reaction mixture at 90°C during 10 min (Fig. 1). However, neither the specificity of HER2 targeting nor the antigen-binding capacity of 68Ga-ABY-002 were compromised. This is in a good agreement with our previous experience with labelling of ABY-002 with 111In at elevated temperatures [28]. In principle, Affibody molecules may be denatured during labelling under the harsh conditions, but they refold rapidly to their initial structure after returning back to physiological conditions [35]. We cannot exclude that some pendant groups (such as e.g. chelators) might interfere with the refolding, but this was obviously not the case with 68Ga-ABY-002. The 10-min-long labelling procedure causes a loss of 10% 68Ga radioactivity due to decay, but we believe that this is acceptable. For comparison, labelling of oxoamine-modified Affibody molecules using 18F-fluorobenzaldehyde provides 13–18% decay-corrected overall yield after about a 100-min-long procedure [17]. In the case of labelling of cysteine-containing Affibody molecules using N-2-(4[18F]fluorobenzamido)ethyl]maleimide ([18F]FBEM), an overall (non-decay-corrected) yield of 6.5% has been reported [16]. For indirect radiobromination using ((4-hydroxyphenyl)ethyl)maleimide (HPEM), an overall yield of ca. 50% has been obtained [15]. All methods for labelling of Affibody molecules with positron-emitting halogens include several steps, which require highly qualified personnel or not yet available automation. It is very likely that development of simple and efficient labelling with 68Ga would facilitate the implementation of Affibody molecules into clinical PET practice. The in vitro test demonstrated high stability of the 68Ga coupling to ABY-002 toward challenges with EDTA and murine serum. This is in agreement with the results of biodistribution studies, which did not reveal any indication of label instability, such as long residence of radioactivity in blood due to transchelation to transferrin, or elevated uptake in liver and spleen due to colloid formation.
The cellular retention of 68Ga-ABY-002 was good (Fig. 4). Unlike many other radiometal-labelled targeting peptides, the retention of radioactivity was mainly due to high affinity binding of the tracer to receptors on the membrane, not due to residualizing properties of 68Ga. The internalization of 68Ga-ABY-002 was slow, amounting to 12.4 ± 0.5% of totally cell-bound radioactivity after 4 h of incubation at 37°C. This is in excellent agreement with the data previously obtained for 111In-ABY-002 [33] and a technetium-labelled cysteine-containing variant of ZHER2:342, 99mTc-ZHER2:2395 [36]. These data suggest that internalization of Affibody molecules is unaffected by labelling methods.
The biodistribution properties were very similar in different mouse strains. Moreover, the data for 111In-ABY-002 were also in agreement with data from an earlier study [28]. Both 68Ga-ABY-002 and 111In-ABY-002 were rapidly cleared from blood by glomerular filtration with subsequent reabsorption in kidneys. In tumour-bearing mice, both conjugates demonstrated high and specific tumour localization. However, clearance of 68Ga-ABY-002 was more efficient from blood, lungs, gastrointestinal tract and muscles in both mouse strains. Earlier studies have shown that the use of different nuclides for the same peptide-chelator conjugate influence biodistribution of melanocyte-stimulating hormone (MSH) [30, 37], somatostatin [29, 38–40], bombesin analogues [31] and arginine-glycine-aspartic acid (RGD) peptides [26]. One of the explanations was the different coordination geometry of nuclides, which causes profound changes in the overall structure of the conjugates [39]. These observations were done with short peptides containing up to ten amino acid residues and with a chelator located close to the binding site of the peptide moiety. Affibody molecules are approximately fourfold larger, and a less pronounced difference between tracers labelled with nuclides was expected on the biological activity, biodistribution and pharmacokinetics. However, the results of this study as well as the comparison of 111In- and 57Co-labelled ZHER2:342 derivatives [18] indicate that biodistribution of even 7-kDa proteins can be influenced by radionuclide selection. This information is important not only for the development of Affibody-based tracers, but also for other scaffold-based imaging agents.
The PET and gamma camera imaging experiment demonstrated a capacity of both 68Ga-ABY-002 and 111In-ABY-002 to image HER2-expressing tumours with a high contrast (Fig. 6). The use of a clinical PET scanner provided a visualization of xenografts in the close proximity (2 cm) to kidneys, indicating that this would be possible also in clinical settings.
Overall, 68Ga-ABY-002 demonstrated excellent targeting properties. Two hours after injection, the tumour to blood ratio was 31 ± 13, which is similar to values for radiofluorinated 18F-FBEM-ZHER2:342 (23 ± 5.5). The tumour to bone ratio was appreciably better for 68Ga-labelled ZHER2:342, which can be associated with different biodistribution of radiocatabolites. The tumour to liver ratios were approximately equal (about 7) for 68Ga-ABY-002 and 18F-FBEM-ZHER2:342. Thus, 68Ga-DOTA-ZHER2:342 was equal or better than the radiofluorinated variant for imaging of HER2 expression in the major metastatic sites. The disadvantage of the residualizing 68Ga label is a high renal retention of the radioactivity. 68Ga-ABY-002 provided better tumour to organ ratios than another putative imaging agent, the 68Ga-labelled DOTA-F(ab′)2 fragment of trastuzumab [41]. The tumour to blood ratio was higher than the corresponding maximum values for full-length antibodies or antibody fragments labelled with positron-emitting nuclides 124I [19, 42], 86Y [43] or 89Zr [44]. Recently, a two-helix variant of Affibody molecules has been developed to reduce the size of a targeting agent [45]. The stabilizing helix 3 has been removed and helices 1 and 2 were cross-linked in order to stabilize the favourable conformation of anti-HER2 Affibody molecule. However, this modification reduced an apparent affinity by nearly two orders of magnitude, to 5 nM. The new protein (designated as MUT-DS) has been conjugated with DOTA, labelled with 68Ga and evaluated in mice bearing SKOV-3 xenografts [46]. 68Ga-DOTA-MUT-DS demonstrated capacity for specific and high-contrast imaging of HER2 in vivo; however, the tumour uptake was threefold lower and the tumour to organ ratio was fourfold lower in comparison with 68Ga-ABY-002 (2 h p.i.). Taken together, our data strongly suggest that the HER2-binding three-helix Affibody molecule is a superior imaging agent for HER2.
The high renal reabsorption is one apparent issue for clinical applications of radiolabelled Affibody molecules. In the case of non-residualizing radiohalogen positron-emitting labels, such as 76Br [15], 18F [16, 17] or 124I [19], the renal reabsorption, internalization and catabolism are associated with rapid washout of radiocatabolites from kidneys. As a result, the radioactivity concentration in kidney at 2–6 h after injection was lower that the radioactivity concentration in tumour xenografts, where internalization and degradation occur slowly. 68Ga is a residualizing label causing high renal retention, similarly to retention of other residualizing radiometal labels on Affibody molecules, such as 111In or 57Co [18, 28]. However, the results of this study show that imaging of tumours in close proximity to the kidneys is possible by a clinical PET camera. The excellent availability of 68Ga makes it an attractive choice. Therefore, alternative strategies for reduction of renal reabsorption are being considered, including the use of Gelofusine, albumin fragments, polyglutamic acids or cationic amino acids [47–50], having demonstrated promising results with other radiolabelled targeting proteins and peptides.
In conclusion, the HER2-binding ABY-002 Affibody molecule was efficiently labelled with 68Ga with preserved binding specificity using a simple and robust procedure. Similarly to 111In-ABY-002, internalization of 68Ga-ABY-002 was slow, but cellular retention was good due to strong binding to HER2. 68Ga-ABY-002 demonstrated high and specific targeting of HER2-expressing xenografts in mice and provided high tumour to organ ratios already 2 h after injection. 68Ga-ABY-002 cleared more rapidly from blood and healthy tissues (except kidneys) than 111In-ABY-002, which is favourable for imaging shortly after injection.
References
Yarden Y, Sliwkowski MX. Untangling the ErbB signalling network. Nat Rev Mol Cell Biol 2001;2:127–37.
Citri A, Yarden Y. EGF-ERBB signalling: towards the systems level. Nat Rev Mol Cell Biol 2006;7:505–16.
Carlsson J. EGFR-family expression and implications for targeted radionuclide therapy. In: Stigbrand T, Carlsson J, Adams G, editors. Targeted radionuclide tumor therapy: biological aspects. New York: Springer; 2008. p. 25–58.
Wolff AC, Hammond ME, Schwartz JN, Hagerty KL, Allred DC, Cote RJ, et al. American Society of Clinical Oncology/College of American Pathologists guideline recommendations for human epidermal growth factor receptor 2 testing in breast cancer. J Clin Oncol 2007;25:118–45.
Molina R, Barak V, van Dalen A, Duffy MJ, Einarsson R, Gion M, et al. Tumor markers in breast cancer-European Group on Tumor Markers recommendations. Tumour Biol 2005;26:281–93.
Verri E, Guglielmini P, Puntoni M, Perdelli L, Papadia A, Lorenzi P, et al. HER2/neu oncoprotein overexpression in epithelial ovarian cancer: evaluation of its prevalence and prognostic significance. Clinical study. Oncology 2005;68:154–61.
Nakamura H, Kawasaki N, Taguchi M, Kabasawa K. Association of HER-2 overexpression with prognosis in nonsmall cell lung carcinoma: a metaanalysis. Cancer 2005;103:1865–73.
Morote J, de Torres I, Caceres C, Vallejo C, Schwartz S Jr, Reventos J. Prognostic value of immunohistochemical expression of the c-erbB-2 oncoprotein in metastasic prostate cancer. Int J Cancer 1999;84:421–5.
Shi Y, Brands FH, Chatterjee S, Feng AC, Groshen S, Schewe J, et al. Her-2/neu expression in prostate cancer: high level of expression associated with exposure to hormone therapy and androgen independent disease. J Urol 2001;166:1514–9.
Carles J, Lloreta J, Salido M, Font A, Suarez M, Baena V, et al. Her-2/neu expression in prostate cancer: a dynamic process? Clin Cancer Res 2004;10:4742–5.
Tolmachev V. Imaging of HER-2 overexpression in tumors for guiding therapy. Curr Pharm Des 2008;14:2999–3019.
Dijkers EC, de Vries EG, Kosterink JG, Brouwers AH, Lub-de Hooge MN. Immunoscintigraphy as potential tool in the clinical evaluation of HER2/neu targeted therapy. Curr Pharm Des 2008;14:3348–62.
Nygren PA. Alternative binding proteins: affibody binding proteins developed from a small three-helix bundle scaffold. FEBS J 2008;275:2668–76.
Orlova A, Feldwisch J, Abrahmsén L, Tolmachev V. Update: affibody molecules for molecular imaging and therapy for cancer. Cancer Biother Radiopharm 2007;22:573–84.
Mume E, Orlova A, Larsson B, Nilsson AS, Nilsson FY, Sjöberg S, et al. Evaluation of ((4-hydroxyphenyl)ethyl)maleimide for site-specific radiobromination of anti-HER2 affibody. Bioconjug Chem 2005;16:1547–55.
Kramer-Marek G, Kiesewetter DO, Martiniova L, Jagoda E, Lee SB, Capala J. [18F]FBEM-Z(HER2:342)-Affibody molecule-a new molecular tracer for in vivo monitoring of HER2 expression by positron emission tomography. Eur J Nucl Med Mol Imaging 2008;35:1008–18.
Cheng Z, De Jesus OP, Namavari M, De A, Levi J, Webster JM, et al. Small-animal PET imaging of human epidermal growth factor receptor type 2 expression with site-specific 18F-labeled protein scaffold molecules. J Nucl Med 2008;49:804–13.
Wållberg H, Ahlgren S, Widström C, Orlova A. Evaluation of the radiocobalt-labeled [MMA-DOTA-Cys61]-Z HER2:2395(-Cys) affibody molecule for targeting of HER2-expressing tumors. Mol Imaging Biol 2010;12:54–62.
Orlova A, Wållberg H, Stone-Elander S, Tolmachev V. On the selection of a tracer for PET imaging of HER2-expressing tumors: direct comparison of a 124I-labeled affibody molecule and trastuzumab in a murine xenograft model. J Nucl Med 2009;50:417–25.
Kramer-Marek G, Kiesewetter DO, Capala J. Changes in HER2 expression in breast cancer xenografts after therapy can be quantified using PET and (18)F-labeled affibody molecules. J Nucl Med 2009;50:1131–9.
Rösch F, Knapp FF. Radionuclide generators. In: Vértes A, Nagy S, Klencsár Z, Rösch F, editors. Handbook of nuclear chemistry. Dordrecht: Kluwer Academic; 2003;4. p. 81–118.
Velikyan I, Beyer GJ, Långström B. Microwave-supported preparation of (68)Ga bioconjugates with high specific radioactivity. Bioconjug Chem 2004;15:554–60.
Breeman WA, de Jong M, de Blois E, Bernard BF, Konijnenberg M, Krenning EP. Radiolabelling DOTA-peptides with 68Ga. Eur J Nucl Med Mol Imaging 2005;32:478–85.
Zhernosekov KP, Filosofov DV, Baum RP, Aschoff P, Bihl H, Razbash AA, et al. Processing of generator-produced 68Ga for medical application. J Nucl Med 2007;48:1741–8.
Meyer GJ, Mäcke H, Schuhmacher J, Knapp WH, Hofmann M. 68Ga-labelled DOTA-derivatised peptide ligands. Eur J Nucl Med Mol Imaging 2004;31:1097–104.
Decristoforo C, Hernandez Gonzalez I, Carlsen J, Rupprich M, Huisman M, Virgolini I, et al. 68Ga- and 111In-labelled DOTA-RGD peptides for imaging of alphavbeta3 integrin expression. Eur J Nucl Med Mol Imaging 2008;35:1507–15.
Maecke HR, André JP. 68Ga-PET radiopharmacy: a generator-based alternative to 18F-radiopharmacy. Ernst Schering Res Found Workshop 2007;62:215–42.
Orlova A, Tolmachev V, Pehrson R, Lindborg M, Tran T, Sandström M, et al. Synthetic affibody molecules: a novel class of affinity ligands for molecular imaging of HER2-expressing malignant tumors. Cancer Res 2007;67:2178–86.
Antunes P, Ginj M, Zhang H, Waser B, Baum RP, Reubi JC, et al. Are radiogallium-labelled DOTA-conjugated somatostatin analogues superior to those labelled with other radiometals? Eur J Nucl Med Mol Imaging 2007;34:982–93.
Froidevaux S, Calame-Christe M, Schuhmacher J, Tanner H, Saffrich R, Henze M, et al. A gallium-labeled DOTA-alpha-melanocyte-stimulating hormone analog for PET imaging of melanoma metastases. J Nucl Med 2004;45:116–23.
Zhang H, Schuhmacher J, Waser B, Wild D, Eisenhut M, Reubi JC, et al. DOTA-PESIN, a DOTA-conjugated bombesin derivative designed for the imaging and targeted radionuclide treatment of bombesin receptor-positive tumours. Eur J Nucl Med Mol Imaging 2007;34:1198–208.
Persson M, Tolmachev V, Andersson K, Gedda L, Sandström M, Carlsson J. [(177)Lu]pertuzumab: experimental studies on targeting of HER-2 positive tumour cells. Eur J Nucl Med Mol Imaging 2005;32:1457–62.
Wållberg H, Orlova A. Slow internalization of anti-HER2 synthetic affibody monomer 111In-DOTA-ZHER2:342-pep2: implications for development of labeled tracers. Cancer Biother Radiopharm 2008;23:435–42.
Orlova A, Wållberg H, Tolmachev V. Optimisation of specific radioactivity of Affibody molecule enables in vivo discrimination between high and low HER2 expression. Eur J Nucl Med Mol Imaging 2008;35 Suppl 2:S187.
Arora P, Oas TG, Myers JK. Fast and faster: a designed variant of the B-domain of protein A folds in 3 microsec. Protein Sci 2004;13:847–53.
Ahlgren S, Wållberg H, Tran TA, Widström C, Hjertman M, Abrahmsén L, et al. Targeting of HER2-expressing tumors with a site-specifically 99mTc-labeled recombinant affibody molecule, ZHER2:2395, with C-terminally engineered cysteine. J Nucl Med 2009;50:781–9.
Wei L, Zhang X, Gallazzi F, Miao Y, Jin X, Brechbiel MW, et al. Melanoma imaging using (111)In-, (86)Y- and (68)Ga-labeled CHX-A''-Re(Arg11)CCMSH. Nucl Med Biol 2009;36:345–54.
de Jong M, Bakker WH, Krenning EP, Breeman WA, van der Pluijm ME, Bernard BF, et al. Yttrium-90 and indium-111 labelling, receptor binding and biodistribution of [DOTA0,d-Phe1,Tyr3]octreotide, a promising somatostatin analogue for radionuclide therapy. Eur J Nucl Med 1997;24:368–71.
Heppeler A, Froidevaux S, Mäcke H, Jermann E, Béhé M, Powell P, et al. Radiometal-labelled macrocyclic chelator-derivatised somatostatin analogue with superb tumour-targeting properties and potential for receptor-mediated internal radiotherapy. Chem Eur J 1999;5:1974–81.
Froidevaux S, Eberle AN, Christe M, Sumanovski L, Heppeler A, Schmitt JS, et al. Neuroendocrine tumor targeting: study of novel gallium-labeled somatostatin radiopeptides in a rat pancreatic tumor model. Int J Cancer 2002;98:930–7.
Smith-Jones PM, Solit DB, Akhurst T, Afroze F, Rosen N, Larson SM. Imaging the pharmacodynamics of HER2 degradation in response to Hsp90 inhibitors. Nat Biotechnol 2004;22:701–6.
Robinson MK, Doss M, Shaller C, Narayanan D, Marks JD, Adler LP, et al. Quantitative immuno-positron emission tomography imaging of HER2-positive tumor xenografts with an iodine-124 labeled anti-HER2 diabody. Cancer Res 2005;65:1471–8.
Garmestani K, Milenic DE, Plascjak PS, Brechbiel MW. A new and convenient method for purification of 86Y using a Sr(II) selective resin and comparison of biodistribution of 86Y and 111In labeled Herceptin. Nucl Med Biol 2002;29:599–606.
Dijkers EC, Kosterink JG, Rademaker AP, Perk LR, van Dongen GA, Bart J, et al. Development and characterization of clinical-grade 89Zr-trastuzumab for HER2/neu immunoPET imaging. J Nucl Med 2009;50:974–81.
Webster JM, Zhang R, Gambhir SS, Cheng Z, Syud FA. Engineered two-helix small proteins for molecular recognition. Chembiochem 2009;10:1293–6.
Ren G, Zhang R, Liu Z, Webster JM, Miao Z, Gambhir SS, et al. A 2-helix small protein labeled with 68Ga for PET imaging of HER2 expression. J Nucl Med 2009;50(9):1492–9.
Melis M, Bijster M, de Visser M, Konijnenberg MW, de Swart J, Rolleman EJ, et al. Dose-response effect of Gelofusine on renal uptake and retention of radiolabelled octreotate in rats with CA20948 tumours. Eur J Nucl Med Mol Imaging 2009 Jul 8. [Epub ahead of print].
Bernard BF, Krenning EP, Breeman WA, Rolleman EJ, Bakker WH, Visser TJ, et al. D-lysine reduction of indium-111 octreotide and yttrium-90 octreotide renal uptake. J Nucl Med 1997;38(12):1929–33.
Vegt E, van Eerd JE, Eek A, Oyen WJ, Wetzels JF, de Jong M, et al. Reducing renal uptake of radiolabeled peptides using albumin fragments. J Nucl Med 2008;49(9):1506–11.
Béhé M, Kluge G, Becker W, Gotthardt M, Behr TM. Use of polyglutamic acids to reduce uptake of radiometal-labeled minigastrin in the kidneys. J Nucl Med 2005;46(6):1012–5.
Acknowledgements
This work was financially supported by the Swedish Cancer Society (Cancerfonden) and the Swedish Research Council (Vetenskapsrådet). UASL, GE Healthcare is acknowledged for the kind permission to access the 68Ge/68Ga generator.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tolmachev, V., Velikyan, I., Sandström, M. et al. A HER2-binding Affibody molecule labelled with 68Ga for PET imaging: direct in vivo comparison with the 111In-labelled analogue. Eur J Nucl Med Mol Imaging 37, 1356–1367 (2010). https://doi.org/10.1007/s00259-009-1367-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-009-1367-7