Abstract
Tuberculosis (TB) remains one of the most menacing infectious diseases, although attenuated Mycobacterium bovis Bacillus Calmette-Guerin (BCG) vaccine has been widely used to protect children against primary TB. There are increasing evidences that rapid growing and dormant Mycobacterium tuberculosis (M. tuberculosis) coexist in vivo after infection. However, BCG vaccine only elicits cell-mediated immune responses to secretory antigens expressed by rapid growing pathogen. BCG vaccine is thus unable to thwart the reactivation of latent tuberculosis infection (LTBI), and its protection wanes over age after neonatal immunization. In order to extend its ability for a durable protection, a novel recombinant BCG (rBCG) strain, named rBCG::XB, was constructed by overexpressing immunodominant multistage antigens of Ag85B and HspX, which are expressed by both rapid replicating and dormant M. tuberculosis. Long-term protective effect and immunogenicity of rBCG::XB were compared with the parental BCG in vaccinated C57BL/6 mice. Our results demonstrated that rBCG::XB provided the stronger and long-lasting protection against M. tuberculosis H37Rv intranasal infection than BCG. The rBCG::XB not only elicited the more durable multistage antigen-specific CD4+Th1-biased immune responses and specific polyfunctional CD4+T cells but also augmented the CD8+ CTL effects against Ag85B in vivo. In particular, higher levels of CD4+ TEM and CD8+ TCM cells, dominated by IL2+ CD4+ and CD8+ TCM cells, were obtained in the spleen of rBCG::XB vaccinated mice. Therefore, our findings indicate that rBCG::XB is a promising candidate to improve the efficacy of BCG.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Since 1974, Mycobacterium bovis Bacillus Calmette-Guérin (BCG) has been integrating into Expanded Programme of Immunization (EPI) as the only licensed vaccine for tuberculosis (TB) (Keja et al. 1988). With high immunization coverage, ranging from 82 to 97 % (Harris et al. 2014), BCG vaccine provides effective protection against primary TB in children (Colditz et al. 1995). However, the protective efficacy of BCG vaccination wanes over age and may last for only 10 to 15 years (Andersen and Doherty 2005; Mangtani et al. 2014). Nowadays, TB remains one of the most menacing infectious diseases with 8.1 million adult cases diagnosed in 2013 (WHO 2014). Approximately one third of the world population are estimated to be on the stage of latent TB infection (LTBIs) and represent a reservoir for adult TB (WHO 2015). Therefore, there is an urgent need to develop a more effective vaccine for the prevention of TB.
During the past decades, great progress has been made in the development of TB vaccine candidates, including recombinant adenovirus or modified Vaccinia Ankara virus (MVA) vectors, subunit proteins, attenuated Mycobacterium tuberculosis or recombinant BCG (rBCG) strains (Kaufmann 2014). However, a novel licensed TB vaccine better than BCG remains elusive in a shorter time. For example, while strengthening the CD4+ Th1-typed response that is considered as a determinant in vaccine-induced protection (Tameris et al. 2014; O’Garra et al. 2013), recombinant MAV expressing Ag85A of M. tuberculosis did not enhance any protection when boosting BCG priming infants in a recent clinical trial (Tameris et al. 2013). The strategy based on rBCG aims to extend the ability of BCG for the longer-term protection and have attracted much more attention in the development of the next generation of TB vaccine (Da et al. 2014). rBCG vaccine not only inherits BCG itself advantages for effective protection against primary infection but also minimizes the affect of novel vaccine on the current immunization strategy. The first attempt rBCG30 supported this notion and provided stronger protection than BCG against M. tuberculosis challenge in different animal models (Horwitz et al. 2006). The rBCG30 was constructed by overexpression of major secretory antigen Ag85B from the Ag85 complex expressed mainly by rapid growing M. tuberculosis during primary phase (D’Souza et al. 2003). However, our recent studies found that T cells from both active TB patients and LTBIs could recognize either secretory antigens or latency antigens expressed largely by M. tuberculosis during latent phase (Wang et al. 2015), indicating the coexistence of both rapid growing and nonreplicating dormant M. tuberculosis strains after infection. The situation is consistent with the theory of modern chemotherapy against TB by combining drugs targeting different status of M. tuberculosis in vivo (Zhang 2007). In contrast, vaccination with BCG mainly confers high IFN-γ response to secretory antigens (Hoft et al. 2008) rather than latency antigens such as HspX (Geluk et al. 2007; Shi et al. 2010), although highly homologous genes encoding latency antigens of M. tuberculosis also present in the genome of BCG. Moreover, the parent BCG strain with the reintroduction of latency antigens, such as HspX (Shi et al. 2010), Rv2659 or Rv1733 (Reece et al. 2011), improved its ability to protect against primary, latent and even post-primary TB infection.
Previously, we developed a novel rBCG ABX by mixing three rBCG strains expressing single antigen, characteristically expressed during both primary stage (Ag85Aand Ag85B) and latency (HspX) of M. tuberculosis. ABX could provide more effective protection than BCG against M. tuberculosis infection in vaccinated mice (Liang et al. 2015). In order to lower the cost of manufacture, a novel rBCG strain overexpressing multistage antigens Ag85B and HspX of M. tuberculosis, namely rBCG::XB, was constructed in this study. The long-term protective efficacy against the challenge with M. tuberculosis and the immunogenicity of rBCG::XB were compared with BCG in vaccinated C57BL/6 mice.
Materials and methods
Construction and identification of recombinant BCG strain rBCG::XB
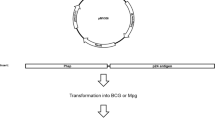
The recombinant plasmid pMXAg85B was constructed by subcloning the gene fragment fbpB from pMAg85B (Wang et al. 2012) into pMHspX (Shi et al. 2010) and confirmed by DNA sequencing and enzyme digestion. Both fbpB and acr genes were expressed under the direction of their putative promoters. The pMXAg85B was amplified in Escherichia coli strain DH5α, followed by the transformation into BCG China strain through electroporation as described previously (Shi et al. 2010). The positive construct rBCG::XB was selected on kanamycin (final concentration of 25 μg/mL)-resistant Middlebrook 7H11 plates (Difco Laboratories, NJ, USA), supplemented with 10 % ADC (Difco Laboratories), 0.5 % glycerol, and 0.05 % Tween80. Culture supernatant and bacterial cell cytosol of rBCG::XB growth in Middlebrook 7H9 medium were prepared and overexpression of HspX and Ag85B protein in rBCG::XB was detected by Western blotting using anti-Ag85B rabbit polyclonal antibodies (1:2000, ab43019, Abcam, Cambridge, UK) or anti-HspX mouse monoclonal antibodies (1:2000, ab64786, Abcam) to develop the immunoblots (Shi et al. 2010). After identification, rBCG::XB strain was deposited in China Center for Type Culture Collection (Preservation number CCTCC M 2014360). To facilitate the assessment during manufacture, relative mRNA levels of Ag85B or HspX expressed in 1 × 106 CFU of rBCG::XB were compared to the parent BCG by using RT-qPCR and the increased fold of gene expression was normalized to the conserved SigA gene and calculated using 2−ΔΔCT method as previously described (Liang et al. 2015).
Mice and immunization
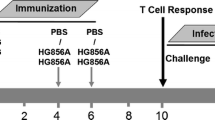
Tongji School Committee on Biosafety and the Committee on the Ethics of Animal Experiments of Tongji Medical College (Wuhan, China) approved the research protocol. Animal experiments were performed in accordance with the guidelines of Chinese Council on Animal Care. Specific pathogen-free, female C57BL/6 (H-2b) mice aged 6 weeks were obtained from the Center for Animal Experiment of Wuhan University (Wuhan, China). Mice were randomly grouped and were bred in separate cages in a biosafety laboratory and fed commercial mouse chow and water ad libitum. Mice were immunized subcutaneously (s.c.) once at the base of the tail with 1 × 106 CFU of rBCG::XB or BCG in a final volume of 100 μl of PBS. The control group was performed with the equal amount of PBS as the same way. Twelve and 32 weeks after immunization, six mice in each group were used for immunological assay. The remains mice in each group were challenged with virulent M. tuberculosis H37Rv strain (American Type Culture Collection 27294) at 12 week after vaccination. Five mice in each group were used for bacterial load in organs and three mice for pathological analysis at 4, 10, and 20 weeks after infection, respectively. All experiments were repeated three times.
Challenge of vaccinated mice with virulent M. tuberculosis H37Rv
At week 12, each vaccinated C57BL/6 mouse was injected via intraperitoneal (i.p.) with 0.96 mg of pentobarbital sodium per 15 g weight. After anesthetized, mice were challenged via intranasal (i.n.) with M. tuberculosis H37Rv. The next day, three mice in the PBS control group were sacrificed in order to confirm infection and to determine actual infectious dose. The whole lung of these mice was removed aseptically, homogenized, and cultured for CFU of M. tuberculosis on Middlebrook 7H11 agar. At 4, 10, and 20 weeks post-infection, eight mice in each group were sacrificed, respectively. Bacterial load in the both lung and spleen (n = 5) and lung histopathology (n = 3) were performed to evaluate the protective efficacy as described previously (Wang et al. 2015).
Antigen-specific antibodies assay
Sera of three mice in each group were collected at 12 and 32 weeks after immunization. Antigen-specific IgG, IgG1, and IgG2a antibodies against recombinant Ag85B or HspX proteins were then determined by ELISA as described previously (Liang et al. 2015). Antibody titers were expressed as reciprocal end point titers and the results are displayed as the mean of log2 antibody titer of three mice in each vaccinated group.
Antigen-specific Th1-typed cytokines secreted by splenocytes
Twelve and 32 weeks after immunization, the levels of Th1-typed cytokines IFN-γ, TNF-α, and IL-2, and Th2-typed cytokine IL-4, secreted by splenocytes from rBCG::XB group incubated with 10 μg/mL of either recombinant HspX, or Ag85B proteins, were determined as previously described (Liang et al. 2015). PPD (10 μg/mL, Statens Serum Institut, Copenhagen, Denmark) was used as a positive control and RPMI1640 medium was performed as a negative control. The results are expressed as the mean ± standard derivation (SD) (pg/mL) pre-group (n = 3).
Intracellular flow cytometry analysis of splenocytes
PPD, recombinant proteins Ag85B, and HspX-specific polyfunctional CD4+ T cell responses were analyzed by multicolour flow cytometry at 12 and 32 weeks as described previously (Liang et al. 2015). Biomarkers including anti-CD3-FITC (clone 17A2, eBioscience, CA, USA), anti-CD4-allophycocyanin-Cy7 (clone GK1.5, BD Pharmingen, CA, USA), anti-IFN-PerCP-Cy5.5 (clone XMG1.2, eBioscience), anti-TNF-PE Cy7 (clone MP6-XT22, BD Pharmingen), and anti-IL-2-allophycocyanin (clone JES6-5H4, eBioscience) mAbs were used. The cytokine profiles of the single cell were assessed by gating on CD4+ T cells, and the absolute numbers of polyfunctional expression of IFN-γ, TNF-α, and IL-2 by CD4+ T cells are shown as mean ± SD per group (n = 3).
Ag85B-specific CTL assay
The CD8 peptide of Ag85B10-18aa YLQVPSPSM-pulsed (10 μg/mL, ChinaPeptides, Shanghai, China) and CFSE-labeled splenocytes were analyzed for in vivo CTL activities of immunized C57BL/6 mice after 12 and 32 weeks as previously described (Liang et al. 2015). The results are expressed as the mean ± SD of three mice per group.
Antigen-specific memory T cell analysis
Twelve and 32 weeks after immunization, splenocytes from different vaccinated C57BL/6 mice were stimulated with CD4 peptides of Ag85B240-260aa FQDAYNAAGGHNAVFNFPPNG, HspX11-30aa PRSLFPEFSELFAAFPSFAG (each 10 μg/mL, ChinaPeptides), and then stained with anti-CD4-PE-Cy7 (clone GK1.5, eBioscience), anti-CD62L-FITC (clone MEL-14, BD Pharmingen), and anti-CD44-APC-Cy7 (clone IM7, BD Pharmingen) mAbs. Alternatively, the CD8 peptide of Ag85B10-18aa was used and then stained with anti-CD8α-PE (clone53-6.7, eBioscience). Intracellular staining was performed with anti-IFN-PerCP-Cy5.5 (clone XMG1.2, eBioscience) and anti-IL-2-allophycocyanin (clone JES6-5H4, eBioscience) mAbs. TCM (central memory T cells, CD62LhiCD44hi) and TEM (effector memory T cells, CD62LloCD44hi) cells were run on a six-colour BD FACSC onto flow cytometer (BD Biosciences) and analyzed with the FlowJo software as previously described (Liang et al. 2015). Data are expressed as the mean ± SD of three mice per group.
Statistical analysis
Student’s t test was used for two-sample comparison, and statistical analysis was performed by the SPSS 17.0 software (SPSS Inc., USA). p < 0.05 was considered statistically significant.
Results
Higher expression levels of multistage antigens Ag85B and HspX from rBCG::XB
Recombinant mycobacterial expression plasmid pMXAg85B was constructed successfully and confirmed by enzyme digestion. The inserted DNA fragments were verified by DNA sequencing. The rBCG::XB was obtained by the transformation of the parent BCG strain with the recombinant plasmid pMXAg85B. Protein overexpression in both culture supernatants and cell lysates of BCG strains were analyzed by Western blotting (Fig. 1a). As expected, low levels of Ag85B (30 kDa) and HspX (16 kDa) proteins were detected from control using wild BCG strain because of endogenous expression. In comparison to BCG, rBCG::XB mainly expressed the much higher concentration of Ag85B protein in both supernatant and lysate and much more HspX protein only in the lysate. Consistent with the results of Western blotting, the increased fold of Ag85B- or HspX-specific mRNAs in rBCG::XB was about 20 times over BCG, respectively (Fig. 1b).
The overexpression of Ag85B and HspX in rBCG::XB. a The overexpression of both Ag85B and HspX in the supernatant and bacterial cytosol was confirmed by Western blotting using anti-Ag85B or anti-HspX antibodies, respectively. b The relative mRNA level of Ag85B and HspX in 1 × 106 CFU of rBCG::XB to the parent BCG was detected by RT-qPCR technology (n = 3). The results are expressed as the mean (±SD) of 2−ΔΔCT
Stronger and longer-lasting protection conferred by rBCG::XB
To investigate protective efficacy of rBCG::XB, mice vaccinated with rBCG::XB and BCG were challenged i.n. with approximately 200 CFU of virulent M. tuberculosis H37Rv at week 12. Four, 10, or 20 weeks post-challenge, bacterial load and lung histopathological changes were assessed. Compared with the control group, bacterial load in both lung and spleen was more significantly and persistently decreased over time in rBCG::XB and BCG vaccinated groups (p < 0.05) (Fig. 2a). Most importantly, rBCG::XB provided the strongest protection in the lung of all groups during the entire experimental period (p < 0.05) and in the spleen only at weeks 4 and 12 after infection (Fig. 2a).
Protective efficacy of rBCG::XB vaccinated C57BL/6 mice. C57BL/6 mice were vaccinated with rBCG::XB, BCG, or PBS, respectively. Twelve weeks later, mice were i.n. challenged with about 200 CFU of virulent M. tuberculosis H37Rv. Four, 10, and 20 weeks post-challenge, the bacterial load in the lung or spleen from each mouse was enumerated, respectively. Results are shown as mean (±SEM) log10 CFU per organs. Four and 20 weeks post-challenge, lung tissue sections were fixed and embedded for HE staining. a Bacterial load per lung and spleen of different groups at different time points (n = 5). b The representative lung histopathology of different groups (scale bar 400 μm). Arrow means granuloma-like pathological change
Four weeks later, the most severe granuloma-like histopathological changes were observed in the lung of PBS control mice. Twenty weeks later, the lung section from PBS control mice still maintained severe interstitial pneumonia and intense inflammation (Fig. 2b). Comparatively, pathological changes were much alleviated in the lung from mice vaccinated with BCG vaccine (Fig. 2b) and several inflammatory foci appeared to form granuloma. Remarkably, alveolar tissue from the mice vaccinated with rBCG::XB appeared to be intact with the lightest lung inflammation over time.
Multistage antigen-specific Th1-biased responses elicited by rBCG::XB
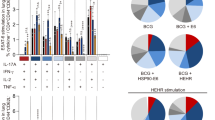
To elucidate immunological mechanisms of better protection provided by rBCG::XB, antigen-specific Th1-type cytokines including TNF-α, IFN-γ, and IL-2, and Th-2 cytokine IL-4 secreted by splenocytes from immunized mice were detected by ELISA at 12 and 32 weeks after immunization. Of three groups, the lowest levels of these Th1-type cytokines were secreted by splenocytes from the PBS control mice, whereas the highest levels of Th1-type cytokines were observed in rBCG::XB group (p < 0.05) (Fig. 3) and also increased significantly over time (p < 0.05) regardless of the stimulus using either PPD, antigens Ag85B, or HspX (Fig. 3). As a representative of Th2-type responses, only detectable level of IL-4 was produced by splenocytes from all groups (data not shown).
Antigen-specific TNF-α, IFN-γ, and IL-2 levels. C57BL/6 mice were vaccinated with rBCG::XB, BCG, or PBS, respectively. Splenocytes (5 × 106) isolated from each immunized C57BL/6 mice after 12 and 32 weeks were stimulated with 10 μg/mL of Ag85B, HspX, PPD, or culture medium for 24 h (IL-2) and 72 h (TNF-α and IFN-γ) at 37 °C, 5 % CO2. Antigen-specific TNF-α, IFN-γ, and IL-2 levels were measured by ELISA. Results are expressed as means ± SD pg/ml of three mice per group. *p < 0.05, 12 vs. 32 weeks; bars represent p < 0.05. This experiment was repeated twice with similar results
In addition, the level of Ag85B-specific antibodies IgG, IgG1, and IgG2a in the rBCG::XB group was higher than that in the BCG group at 12 weeks after immunization (p < 0.05; Fig. 4). Higher level of HspX specific antibodies IgG1 and IgG2a was also elicited in rBCG::XB vaccinated mice (p < 0.05). Ag85B and HspX specific antibodies of BCG group also increased significantly over time (p < 0.05; Fig. 4). At 32 weeks after immunization, only the levels of IgG against Ag85B and IgG2a against Ag85B and HspX of rBCG::XB were higher than that in BCG group (p < 0.05). The ratio of IgG2a:IgG1 was also greater in mice immunized with rBCG::XB comparing to BCG vaccinated mice (Fig. 4). As expected, no antigen specific antibodies were detected in PBS control mice.
Antigen-specific antibodies in sera. C57BL/6 mice were vaccinated with rBCG::XB, BCG, or PBS, respectively. Serum was collected from each mouse from different immunized mice at 12 and 32 weeks after immunization. IgG, IgG1, and IgG2c (replaced with IgG2a during assay) antibodies against recombinant proteins Ag85B and HspX in sera were detected by an ELISA assay. Results are shown as mean (±SEM) log2 endpoint titer and the ratio of IgG2a:IgG1 in different vaccinated mice (n = 3). *p < 0.05 vs.12 weeks; bars represent p < 0.05. This experiment was repeated twice with similar results
Multistage antigen-specific polyfunctional CD4+ T cells induced by rBCG::XB
To screen effective biomarkers associated with enhanced protection mediated by rBCG::XB, polyfunctional CD4+ T cells from vaccinated mice were further examined. Twelve weeks after immunization, absolute numbers of TNF-α+IFN-γ+, single IFN-γ+, or TNF-α+ CD4+T cells were higher in the rBCG::XB group than BCG vaccinated mice in response to PPD or antigens Ag85B and HspX (p < 0.05; Fig. 5). Thirty-two weeks after immunization, higher absolute numbers of PPD and multistage antigen-specific TNF-α+IFN-γ+, single IFN-γ+ or TNF-α+, even TNF-α+ IFN-γ+IL-2+ CD4+T cells were induced in the rBCG::XB group in comparison with the BCG group (p < 0.05; Fig. 5). In addition, rBCG::XB induced higher numbers of mono- and double-CD4+ T cells reacting to specific antigens, such as Ag85B-specific single IL-2+, and Ag85B-specific IFN-γ+IL-2+ CD4+ T cells (p < 0.05) (Fig. 5). Our results indicate that these biomarkers might be key components contributing to the enhanced protection of rBCG::XB, when compared with the BCG vaccine.
Antigen-specific polyfunctional CD4+ T cell responses. C57BL/6 mice were vaccinated with rBCG::XB, BCG, or PBS, respectively. PPD, Ag85B, and HspX antigen-specific polyfunctional CD4+ T cell responses were analyzed by multicolour flow cytometry at 12 and 32 weeks. The cytokine profile of single cell was assessed by gating on CD4+ T cells. Absolute numbers of polyfunctional expression of IFN-γ, TNF-α, and IL-2 by CD4+ T cells are shown as mean ± SD (n = 3) per group. *p < 0.05, 12 vs. 32 weeks; bars represent p < 0.05. This experiment was repeated twice with similar results
Stronger and longer-lasting Ag85B-specific CTL activity induced by rBCG::XB
Twelve and 32 weeks after immunization, the CTL activity of Ag85B-specific CD8+ T cells in both BCG and rBCG::XB vaccinated mice was compared by the CFSE-labeled method in vivo (Fig. 6). Only very low levels of specific killing were obtained in the BCG group during the whole experimental period as reported previously (Liang et al. 2015), while rBCG::XB vaccinated mice increased more significantly the specific killing than BCG vaccine (p < 0.001), and maintained approximately three times higher levels up to 32 weeks (Fig. 6).
In vivo CTL activities and Ag85B peptide-specific memory CD8+ T cells. C57BL/6 mice were vaccinated with rBCG::XB, BCG, or PBS, respectively. Ag85B CD8+ peptide-pulsed CFSE-labeled target cells were analyzed for in vivo CTL activities of immunized C57BL/6 mice (n = 3) after 12 and 32 weeks. a Representative histograms of splenocytes with the right and left peaks showing CFSE-labeled Ag85B peptide-pulsed and unpulsed splenocytes, respectively. b Percentages of cytotoxic activity. The results are expressed as the mean ± SD of three mice per group. Bars represent p < 0.05. This experiment was repeated twice with similar results. c Absolute numbers of Ag85B peptide-specific CD8+ TCM (CD62LhiCD44hi), TEM (CD62LloCD44hi) cells, TCM cells secreting IL-2 and TEM cells secreting IFN-γ are expressed as the mean ± SD of three mice per group. *p < 0.05, 12 vs. 32 weeks; bars represent p < 0.05. This experiment was repeated twice with similar results
Higher levels of memory T cells elicited by rBCG::XB
To elucidate the mechanism of the longer-lasting protection conferred by rBCG::XB, splenic memory CD4+ T cells against peptides of either Ag85B or HspX, or Ag85B CD8 peptide-specific memory CD8+ T cells were identified based on the expression of CD62L and CD44. Of three groups, the highest level of Ag85B-specific memory CD8 + T cells, including TCM and IFN-γ+ TEM cells, was induced in rBCG::XB vaccinated mice at 12 weeks (p < 0.05) (Fig. 6). The highest level of Ag85B-specific TEM CD8 + T cells was provided by BCG vaccinated mice at 12 weeks, which was significantly decreased at 32 weeks (p < 0.05). Thirty-two weeks later, memory CD8+ T cells were also significantly increased in the rBCG::XB group (p < 0.05) with the domination of IL-2+ TCM cells. Especially, higher numbers of TEM, IL-2+ TCM and IFN-γ+ TEM cells were induced in the rBCG::XB group compared to the BCG vaccinated mice (p < 0.05).
Of all groups, the highest number of both multistage antigen-specific TCM and TEM CD4+ T cells was induced in rBCG::XB vaccinated mice (Fig. 7) and many more Ag85B-specific TCM and IFN-γ+ TEM CD4+ T cells were elicited in rBCG::XB than BCG vaccinated mice at 12 weeks (p < 0.05). Thirty-two weeks later, the number of the multistage antigen-specific IFN-γ+ CD4+ TEM cells was increased persistently in both rBCG::XB and BCG groups (p < 0.05) (Fig. 7). However, IL-2+ CD4+ TCM cells responding to both multistage antigens dominated in BCG or rBCG::XB vaccinated mice. Notably, rBCG::XB conferred many more numbers of Ag85B- and HspX-specific IL-2+ TCM cells and Ag85B-specific IFN-γ+ TEM T cells, when compared with the BCG group (p < 0.05).
Antigen-specific memory CD4+ T cells. C57BL/6 mice were vaccinated with rBCG::XB, BCG, or PBS, respectively. The subsets of CD4+ peptides of Ag85B and HspX-specific memory CD4+ T cells in spleens of immunized C57BL/6 mice after 12 and 32 weeks were identified by ICS. Absolute numbers of TCM (CD62LhiCD44hi), TEM (CD62LloCD44hi), TCM cells secreting IL-2 and TEM cells secreting IFN-γ are expressed as the mean ± SD of three mice per group. *p < 0.05, 12 vs. 32 weeks; bars represent p < 0.05. This experiment was repeated twice with similar results
Discussion
Once infected via aerosol, M. tuberculosis is engulfed by macrophages localized in pulmonary alveoli. Primary infection is established when M. tuberculosis grows exponentially in vivo, which could secret some immunodominant antigens such as Ag85 complex (Ag85A, Ag85B, and Ag85C), as observed growth in culture medium in vitro (D’Souza et al. 2003). Gradually, CD4+ Th1-typed responses targeting these secretory antigens are conferred and thus leading to the formation of granuloma at the site of infection of the lung. During this chronic and latency phase, antigens repertoire of M. tuberculosis persisting in the granuloma would change correspondingly because its growing status will transfer from growing replication to dormant state in vivo, with the characteristic up-regulated expression of 48 DosR-regulon genes including HspX (Vasudeva-Rao and McDonough 2008). Dormant M. tuberculosis persisting in the host, as main source of the post-primary infection, could reactivate again and thus resulting in the development of active pulmonary TB in adults. In this study, a novel rBCG strain rBCG::XB was constructed through the overexpression of multistage antigens Ag85B and HspX. The immunogenicity and protective efficacy of rBCG::XB were evaluated and compared with BCG in vaccinated C57BL/6 mice. Our results demonstrated that rBCG::XB could produce a stronger and long-lasting protection against M. tuberculosis challenge than parental BCG, as evidenced by lower bacterial loads in the lung and spleen and less lung pathological changes over time. Our results indicate that rBCG::XB could not only preserve the advantage of BCG to protect against primary TB infection, but also extend and broaden the protection of the current BCG vaccine to better control TB in adults.
CD4+ Th1-typed responses play a decisive role in the protection against M. tuberculosis infection (O’Garra et al. 2013). CD8+ T cells not only compensate the role of CD4+ Th1 response against primary infection by secreting Th1 cytokines, but also participate in the process to thwart the reactivation of latent infection (Woodworth and Behar 2006). In the current study, BCG is a strong inducer of CD4+ Th1 responses to secretory antigen Ag85B rather than latency antigen HspX, as demonstrated by the levels of IFN-γ secreting from splenocytes, which confirmed the previous conclusion (Liang et al. 2015; Shi et al. 2010). In addition, our research also confirmed that BCG vaccination only conferred poor or weak CD8+ CTL effects (Liang et al. 2015). Therefore, the combination of CD4+ Th1 biased responses and the elevated CD8+ CTL effects to the multistage antigens induced by rBCG::XB enhanced the protection of BCG against primary M. tuberculosis infection.
Actual mechanism of the declining protection after BCG vaccination over time remains unclear. BCG increased persistently the number of effector and central memory CD4+ T cells response to the multistage antigens over time, although IFN-γ+ CD4+ TEM cells as well as IL-2+ CD8+ TCM cells had no significant changes in BCG vaccinated mice during the whole experiment period. In contrast, many more numbers of these kinds of memory T cells were induced by rBCG::XB, which might be attributed to the longer-term protection of rBCG::XB than BCG vaccinated mice. TCM cells expressing IL-2, detected in rBCG30 (Hoft et al. 2008) and rBCG△ureC::hly (Vogelzang et al. 2014) vaccinated individuals or mesured in treated TB patients (Adekambi et al. 2012), were dominated in the CD4+ and CD8+ TCM cells induced by rBCG::XB. Together with these data, contrary memory T cells might play an important role for the maintenance of immunological memory following the vaccination or control the reinfection.
In conclusion, our results demonstrated that rBCG::XB co-expressing multistage antigens could induce better and more durable protection against primary M. tuberculosis infection over BCG. Such enhanced protection could be attributed to augmented memory CD4+ and CD8+ T cell responses to the multistage antigen elicited by rBCG::XB. Therefore, our results suggest that rBCG strains expressing immunodominant antigens present at different phases of M. tuberculosis infection could improve the efficacy of BCG for adult TB. The rBCG::XB is thus a promising TB vaccine candidate and warrants further evaluation.
References
Adekambi T, Ibegbu CC, Kalokhe AS, Yu T, Ray SM, Rengarajan J (2012) Distinct effector memory CD4+ T cell signatures in latent Mycobacterium tuberculosis infection, BCG vaccination and clinically resolved tuberculosis. PLoS One 7, e36046
Andersen P, Doherty TM (2005) The success and failure of BCG - implications for a novel tuberculosis vaccine. Nat Rev Microbiol 3:656–662
Colditz GA, Berkey CS, Mosteller F, Brewer TF, Wilson ME, Burdick E, Fineberg HV (1995) The efficacy of bacillus Calmette-Guerin vaccination of newborns and infants in the prevention of tuberculosis: meta-analyses of the published literature. Pediatrics 96:29–35
Da CA, Nogueira SV, Kipnis A, Junqueira-Kipnis AP (2014) Recombinant BCG: innovations on an old vaccine. Scope of BCG strains and strategies to improve long-lasting memory. Front Immunol 5:152
D’Souza S, Rosseels V, Romano M, Tanghe A, Denis O, Jurion F, Castiglione N, Vanonckelen A, Palfliet K, Huygen K (2003) Mapping of murine Th1 helper T-cell epitopes of mycolyl transferases Ag85A, Ag85B, and Ag85C from Mycobacterium tuberculosis. Infect Immun 71:483–493
Geluk A, Lin MY, van Meijgaarden KE, Leyten EM, Franken KL, Ottenhoff TH, Klein MR (2007) T-cell recognition of the HspX protein of Mycobacterium tuberculosis correlates with latent M. tuberculosis infection but not with M. bovis BCG vaccination. Infect Immun 75:2914–2921
Harris JB, Gacic-Dobo M, Eggers R, Brown DW, Sodha SV (2014) Global routine vaccination coverage, 2013. MMWR Morb Mortal Wkly Rep 63:1055–1058
Hoft DF, Blazevic A, Abate G, Hanekom WA, Kaplan G, Soler JH, Weichold F, Geiter L, Sadoff JC, Horwitz MA (2008) A new recombinant bacille Calmette-Guerin vaccine safely induces significantly enhanced tuberculosis-specific immunity in human volunteers. J Infect Dis 198:1491–1501
Horwitz MA, Harth G, Dillon BJ, Maslesa-Galic S (2006) Extraordinarily few organisms of a live recombinant BCG vaccine against tuberculosis induce maximal cell-mediated and protective immunity. Vaccine 24:443–451
Kaufmann SH (2014) Tuberculosis vaccine development at a divide. Curr Opin Pulm Med 20:294–300
Keja K, Chan C, Hayden G, Henderson RH (1988) Expanded programme on immunization. World Health Stat Q 41:59–63
Liang J, Teng X, Yuan X, Zhang Y, Shi C, Yue T, Zhou L, Li J, Fan X (2015) Enhanced and durable protective immune responses induced by a cocktail of recombinant BCG strains expressing antigens of multistage of Mycobacterium tuberculosis. Mol Immunol 66:392–401
Mangtani P, Abubakar I, Ariti C, Beynon R, Pimpin L, Fine PE, Rodrigues LC, Smith PG, Lipman M, Whiting PF, Sterne JA (2014) Protection by BCG vaccine against tuberculosis: a systematic review of randomized controlled trials. Clin Infect Dis 58:470–480
O’Garra A, Redford PS, McNab FW, Bloom CI, Wilkinson RJ, Berry MP (2013) The immune response in tuberculosis. Annu Rev Immunol 31:475–527
Reece ST, Nasser-Eddine A, Dietrich J, Stein M, Zedler U, Schommer-Leitner S, Ottenhoff TH, Andersen P, Kaufmann SH (2011) Improved long-term protection against Mycobacterium tuberculosis Beijing/W in mice after intra-dermal inoculation of recombinant BCG expressing latency associated antigens. Vaccine 29:8740–8744
Shi C, Chen L, Chen Z, Zhang Y, Zhou Z, Lu J, Fu R, Wang C, Fang Z, Fan X (2010) Enhanced protection against tuberculosis by vaccination with recombinant BCG over-expressing HspX protein. Vaccine 28:5237–5244
Tameris M, Geldenhuys H, Luabeya AK, Smit E, Hughes JE, Vermaak S, Hanekom WA, Hatherill M, Mahomed H, McShane H, Scriba TJ (2014) The candidate TB vaccine, MVA85A, induces highly durable Th1 responses. PLoS One 9, e87340
Tameris MD, Hatherill M, Landry BS, Scriba TJ, Snowden MA, Lockhart S, Shea JE, McClain JB, Hussey GD, Hanekom WA, Mahomed H, McShane H (2013) Safety and efficacy of MVA85A, a new tuberculosis vaccine, in infants previously vaccinated with BCG: a randomised, placebo-controlled phase 2b trial. Lancet 381:1021–1028
Vasudeva-Rao HM, McDonough KA (2008) Expression of the Mycobacterium tuberculosis acr-coregulated genes from the DevR (DosR) regulon is controlled by multiple levels of regulation. Infect Immun 76:2478–2489
Vogelzang A, Perdomo C, Zedler U, Kuhlmann S, Hurwitz R, Gengenbacher M, Kaufmann SH (2014) Central memory CD4+ T cells are responsible for the recombinant Bacillus Calmette-Guerin DeltaureC::hly vaccine’s superior protection against tuberculosis. J Infect Dis 210:1928–1937
Wang C, Fu R, Chen Z, Tan K, Chen L, Teng X, Lu J, Shi C, Fan X (2012) Immunogenicity and protective efficacy of a novel recombinant BCG strain overexpressing antigens Ag85A and Ag85B. Clin Dev Immunol 2012:563838
Wang X, Zhang J, Liang J, Zhang Y, Teng X, Yuan X, Fan X (2015) Protection against Mycobacterium tuberculosis infection offered by a new multistage subunit vaccine correlates with increased number of IFN-γ+ IL-2+ CD4+ and IFN-γ+CD8+ T cells. PLoS One 10:e122560
Woodworth JS, Behar SM (2006) Mycobacterium tuberculosis-specific CD8+ T cells and their role in immunity. Crit Rev Immunol 26:317–352
WHO (2014) Global tuberculosis report 2014. World Health Organization Web. http://www.who.int/tb/publications/global_report/en/ (accessed Aug 12, 2015)
WHO (2015) Guidelines on the management of latent tuberculosis infection. World Health Organization Web. http://www.who.int/entity/tb/publications/latent-tuberculosis-infection/en/ (accessed Aug 12, 2015)
Zhang Y (2007) Advances in the treatment of tuberculosis. Clin Pharmacol Ther 82:595–600
Acknowledgments
This study was funded by grants of the National High Technology Research and Development of China (863 program; No.2012AA02A401) and the National Mega-projects of Science Research for the 12th Five-year Plan of China (2012ZX10003008-005).
Ethical statement
Tongji Medical School Committee on Biosafety and the Committee on the Ethics of Animal Experiments of Tongji Medical College (Wuhan, China) approved the research protocol. Animal experiments were performed in accordance with the guidelines of Chinese Council on Animal Care.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Xuefeng Yuan, Xindong Teng and Yukai Jing contributed equally to this work.
Rights and permissions
About this article
Cite this article
Yuan, X., Teng, X., Jing, Y. et al. A live attenuated BCG vaccine overexpressing multistage antigens Ag85B and HspX provides superior protection against Mycobacterium tuberculosis infection. Appl Microbiol Biotechnol 99, 10587–10595 (2015). https://doi.org/10.1007/s00253-015-6962-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00253-015-6962-x