Abstract
Background
Pediatric optic pathway gliomas are typically indolent but have a variable clinical course. Treatment is dictated by symptoms and changes on contrast-enhanced MRI examinations. Gadolinium retention in children has motivated parsimonious use of gadolinium-based contrast agents.
Objectives
To determine surveillance MR factors that motivate changes in tumor-directed therapies and extrapolate cost-efficacy of a non-contrast follow-up protocol.
Materials and methods
Using an imaging database search we identified children with isolated optic pathway gliomas and ≥3 follow-up contrast-enhanced MRIs. We reviewed medical records and imaging for: (1) coincident changes on contrast-enhanced MRI and tumor-directed therapy, (2) demographics and duration of follow-up, (3) motivations for intervention, (4) assessment of gadolinium-based contrast agents’ utility and (5) health care utilization data. We assessed cost impact in terms of relative value unit (RVU) burden.
Results
We included 17 neurofibromatosis type 1 (NF1) and 21 non-NF1 patients who underwent a median 16.9 and 24.3 cumulative contrast-enhanced MR exams over 7.7 years and 8.1 years of follow-up, respectively. Eight children (one with NF1) had intervention based on contrast-enhanced MR findings alone. For these eight, increased tumor size was the only common feature, and it was apparent on non-contrast T2 sequences. For the median patient, a non-contrast follow-up protocol could result in 15.9 (NF1) and 23.3 (non-NF1) fewer gadolinium-based contrast agent administrations, and a 39% lower yearly RVU burden.
Conclusion
Pediatric patients with isolated optic pathway gliomas undergo a large number of routine contrast-enhanced MR follow-up exams. Gadolinium might not be needed for these exams to inform management decisions. Secondary benefits of a non-contrast follow-up protocol include decreased cost and risk to the patient.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Gadolinium-based contrast agents (GBCAs) are employed in approximately 40% of the MRI studies performed in the United States in pediatric patients [1]. Since recognition of the association between GBCA administration and nephrogenic systemic fibrosis prompted avoidance of use in the setting of renal failure, GBCAs have generally been well tolerated in both adults and children [2]. However there has been recent recognition of long-term, dose-dependent gadolinium retention in both children and adults without severe renal dysfunction, including accumulation in the central nervous system (CNS) [2,3,4,5,6], bone [7], skin [8] and iron-overloaded liver [9]. The clinical significance of its accumulation in the human body in the context of normal renal function is unclear. Excluding nephrogenic systemic fibrosis, there have been rare clinical case reports of gadolinium-induced toxicity (all in adults) that include various symptoms [10, 11]. Presently, however, there is no definitive evidence that accumulated gadolinium in children with normal renal function results in clinical pathology. Pre-clinically, multiple gadolinium-associated toxicities have been observed [10]. These data have led to increased caution in the medical community regarding potential unknown long-term clinical consequences that might result from accumulated gadolinium and exploration of imaging protocols designed to limit gadolinium exposure over long-term follow-up [12,13,14,15,16,17].
In the interest of diminishing any risks associated with the administration of GBCAs and avoiding unnecessary costs related to GBCA administration, we examined the routine use of GBCAs at our tertiary pediatric referral center for high-exposure populations such as children undergoing multiple contrast-enhanced MR exams for brain tumor surveillance. Here, we present results from our retrospective study of contrast-enhanced MR exams for follow-up of pediatric patients with optic pathway gliomas.
An optic pathway glioma is most commonly a pilocytic astrocytoma involving any combination of the optic nerve, chiasm, optic tracts and radiations, and it comprises approximately 5% of all childhood tumors [18], most frequently presenting between 2 years and 8 years of age [19]. Up to 30% are associated with neurofibromatosis type 1 (NF1) [20]. The evolution of these tumors is unpredictable and progression can result in permanent vision loss and other neurologic and endocrine symptoms [20,21,22]. Diagnosis is typically made on contrast-enhanced MR prompted by clinical symptoms (e.g., unexplained vision loss, nystagmus, ataxia, proptosis, precocious puberty, absence of pain/inflammatory signs). Biopsy is generally not performed for lesions with classic imaging appearance (optic pathway involvement, solid or mixed solid/cystic, T1-isointense, avidly and heterogeneously T2-hyperintense, with variable contrast enhancement) [21, 23].
Although optic pathway gliomas have approximately 90% overall survival, average progression-free survival is variable, ranging from approximately 40% at 10 years without treatment in NF1-associated cases [20] to 24% at 5 years with treatment in sporadic cases [22]. The general prognosis (less visual impairment at diagnosis, less likely to progress) and typical MR imaging features (e.g., smaller tumor size, decreased cystic components) of NF1-associated optic pathway gliomas versus sporadic optic pathway gliomas might be partly attributable to detection bias [24,25,26,27]. There are no universally accepted policies for MRI-based optic pathway glioma screening in asymptomatic children with NF1; however some authors have advocated for this practice [28], and children with NF1, by nature of their disease and frequent evaluations by multiple clinical specialists, are more likely to undergo baseline diagnostic brain imaging than children without NF1. Once identified, NF1-associated and sporadic optic pathway gliomas are typically followed in a similar fashion, using serial MRI and neuro-opthalmologic examination.
Treatment of optic pathway gliomas is typically directed by a multi-disciplinary team. Upon presentation, “watchful waiting” including observation with serial imaging and neuro-ophthalmologic exams is generally instituted [21]. Tumor-directed therapy is initiated with progression, either based on exam (usually changes in vision), or tumor growth on imaging. Though radiation therapy is generally accepted to be a more definitive treatment, in order to avoid deleterious effects in children, particularly neurodevelopmental/intellectual effects in younger children, chemotherapy is usually attempted as a first-line therapy. Surgical resection is also selectively employed, but the diffuse nature and potential morbidity (e.g., additional vision loss) limit its utility [21].
The imaging modality that is typically employed for follow-up is contrast-enhanced MR of the brain. Although intervals of neuro-ophthalmologic follow-up are generally standardized (every 3 months for the first year, followed by increasing intervals), there is no consensus on the optimal frequency of neuroimaging for follow-up of optic pathway gliomas [29]. Proposed imaging intervals range from 3 months to 24 months and can be influenced by the location of the tumor, the degree of visual impairment, and evidence of tumor progression [29,30,31,32,33].
Given the frequent contrast-enhanced MR monitoring and the excellent overall life expectancy of children with optic pathway gliomas, these children are at higher risk of gadolinium tissue deposition related to repeated GBCA administration and theoretically potential complications associated with gadolinium accumulation. We hypothesized that GBCA administration is not necessary for routine MR surveillance of isolated optic pathway gliomas to direct tumor management, which would obviate the potential risk and cost of repeated GBCA administration. To test this hypothesis we undertook a retrospective review of our institutional experience.
Materials and methods
The study was performed at a tertiary pediatric hospital that is a referral center for pediatric optic pathway gliomas. Following institutional review board approval, we searched radiology reports using an internal electronic database (zVision software, version 1.4.65; Clario Medical Imaging, Seattle, WA) with the key phrase “optic pathway glioma” spanning the dates of June 1, 2002, through Dec. 30, 2016. This yielded 43 patients with optic pathway gliomas who were treated at our institution and had a minimum of 3 contrast-enhanced MR brain examinations on our institutional picture archiving and communication system (PACS) available for review. To minimize the impact of imaging follow-up practices unrelated to optic pathway glioma, we included only isolated optic pathway glioma cases; to this end we excluded four children (all with NF1) who had suspected or pathologically proven additional CNS tumors, as well as one child (also with NF1) with concurrent Moyamoya syndrome. One of five of the investigators (E.M., a fellow; A.L.S., 8 years’ experience; F.A.P., 4 years’ experience; R.S.I., 7 years’ experience; D.W.W.S., 26 years’ experience) reviewed the electronic medical record and available MR brain reports for the 38 children with isolated optic pathway gliomas to identify instances of coincident changes on contrast-enhanced MR and changes in tumor-directed therapies. Specifically, we examined consensus tumor board notes to identify instances of initiation of chemotherapy or clinical-trial medications, surgery or radiation therapy that were attributed at least in part to changes in tumor attributes observed on contrast-enhanced MR exams (this could have included size, composition or enhancement characteristics). We then verified the change in the attributed exam’s report, with review of imaging on PACS. The relevant contrast-enhanced MR exams in all cases were performed at our institution. Per protocol during the study period at our institution post-gadolinium sequences were always obtained immediately following GBCA administration. No specific time-linked cut-off was used for “coincident” changes, only specific attribution of the change in therapy to a change on a specific contrast-enhanced MR exam.
Using the electronic medical record, we also obtained data including age, gender and weight at optic pathway glioma diagnosis, NF1 diagnosis status, insurance carrier, and duration of clinical follow-up for optic pathway gliomas. The latter was defined as the time between diagnosis and the most recent relevant clinical note. We further evaluated tumor board notes (incorporating consensus rationale from multiple subspecialty physicians including ophthalmologists, neuroradiologists and neuro-oncologists) to assess all of the underlying motivations of changes in tumor-directed therapies. This process included review with a pediatric neuro-oncology specialist from the hematology/oncology division (S.L., 9 years’ experience) to determine any influence that optic pathway glioma enhancement characteristics might have had on clinical decisions. In some cases, the electronic medical record identified additional contrast-enhanced MR brain exams performed before PACS inception or at outside institutions that were not present on our institutional PACS; the total number of contrast-enhanced MR brain exams for each patient included these additional outside institutional exams dating to 1990. To establish the denominator of patients with optic pathway gliomas seen clinically at our institution over the same date range with any duration of follow-up, we conducted a separate search of a regional cancer registry inclusive of all children treated or diagnosed by our hematology/oncology department, specifying our institution, International Classification of Diseases for Oncology (ICD-O) histology codes for glioma (9380–9489), and all available site codes involving the optic pathways (C72.30–C72.32).
To preliminarily assess the need for post-gadolinium sequences to identify tumor progression, a subspecialty board-certified neuroradiologist (F.A.P., 4 years’ exerience) conducted a blinded review of the eight cases where contrast-enhanced MR findings alone resulted in a change in tumor-directed therapy. For each case, two exam pairs were compiled. The two exams in each pair were always consecutive, obtained within 1 year of each other, and were performed at our institution. The first pair included the exam and relevant comparison previously identified in tumor board notes where a change in the tumor size had motivated a change in tumor-directed therapy. The second pair was selected from a later time point, when consensus tumor board notes stated that there was no significant difference in tumor size between exams. This second pair served as an internal control for each patient. Magnet field strength at 1.5 tesla (T) or 3 T was not necessarily matched between studies and there was some slight variability in sequence slice thickness and specific sequence parameters in some cases.
All exam pairs were reviewed by F.A.P., who was blinded to the pair type and report contents, and the product of the greatest axial plane whole-tumor perpendicular diameters was calculated for each exam on T1-weighted post-gadolinium, T2-weighted and fluid-attenuated inversion recovery (FLAIR) sequences. Percentage change in cross-product was assessed for each pair. We adapted this method from previous studies assessing changes in optic pathway glioma size on traditional MRI [34,35,36,37], and consensus guidelines for size assessments of low-grade gliomas [38, 39]. We used paired Student’s t-tests to compare the results obtained for measurements made on the different imaging sequences for both the size-change group and the control group. P values of <0.05 were considered statistically significant.
We also performed preliminary cost-efficacy analysis with attention to: (1) imaging exam-related costs, including relative value units (RVUs) for a contrast-enhanced MR brain protocol model versus non-contrast model (eliminating only the post-contrast sequences); (2) per-GBCA-administration patient risks, including incidence of moderate-to-severe allergic-like contrast reaction and cumulative gadolinium deposition. We performed linear regressions between cumulative contrast-enhanced examination burden and clinical follow-up time using the statistical software package R [40]. We used the Healthcare Common Procedure Coding System codes 70551 and 70553 to identify appropriate global RVU values, combining the professional and technical components, for non-contrast (6.43) and contrast-enhanced (10.51) MR brain exams from the Centers for Medicare and Medicaid Services website [41]. To translate RVUs to “generalizable” dollar amounts, we: (1) used published national payment indices for private insurer-to-Medicare of 1.30 [42] and Medicaid-to-Medicare of 0.82 [43], (2) assumed no geographic practice cost index adjustments that are typically applied to RVUs when calculating Medicare payments and (3) used only the 2017 Medicare conversion factor of $35.8887.
Results
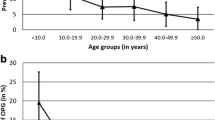
Thirty-eight children with isolated optic pathway gliomas and at least 3 contrast-enhanced MR exams obtained between 2002 and 2016 were identified by imaging-record search within a population of 104 children with optic pathway gliomas who were seen clinically at our institution over the same date range with any duration of follow-up. Select characteristics of the 38 children meeting our search criteria are presented in Table 1. The number of contrast-enhanced MR brain exams performed per year of clinical follow-up for optic pathway gliomas is presented in Fig. 1. On average, children with NF1 had fewer exams per year of clinical follow-up. Linear regression analysis with adjustment for NF1 status and age at diagnosis demonstrated a first-order linear trend between years of clinical follow-up for optic pathway gliomas and the cumulative number of contrast-enhanced MR brain examinations undergone by the child (Fig. 1). Eighteen children were found to have least one instance of change in tumor-directed therapy motivated at least in part by change on MRI. Of these 18 cases, 8 therapy changes were made based on MRI findings alone (i.e. no significant changes were noted in the child’s neuro-ophthalmologic exam/testing or other reported symptoms), and 10 were made in the context of changes occurring both on MRI and in the child’s clinical symptoms. For all 18 cases, increase in tumor size was the only imaging feature that drove therapy decision-making (see Fig. 2 for a representative case). Consensus tumor board notes in the eight cases where MRI findings alone motivated change in management cited only the increase in tumor size as evidence of tumor progression, and most commonly stated “preservation of tenuous remaining vision” as the accompanying clinical rationale for initiation of tumor-directed therapy. Discussion of clinical management of children with optic pathway gliomas and changes in contrast-enhanced MR findings with a neuro-oncology specialist revealed that in all 18 cases, changes in the contrast-enhancement characteristics of the optic pathway gliomas did not influence tumor-directed therapies, impact assessment of treatment response, or alter frequency of follow-up imaging.
Cumulative contrast-enhanced MR brain examination (CEMR) burden for children with isolated optic pathway glioma (OPG). a The mean (dotted line)/median (solid line) and interquartile range (whiskers) of contrast-enhanced MR brain examinations performed per year for clinical follow-up of optic pathway gliomas were: 2.2/2.2 (1.6–2.6) for children with neurofibromatosis type 1 (NF1), 3.1/3.0 (2.3–3.8) for children without NF1, and 2.7/2.6 (1.9–3.4) overall. Comparing the average values across the two subpopulations, the associated P-value was 0.002 (**), with a value of <0.05 considered statistically significant. b A first-order linear trend was demonstrated between years of clinical follow-up for optic pathway gliomas and the cumulative number of contrast-enhanced MR brain examinations the patient underwent. Linear regression (LR) analysis with adjustment for NF1 status and age of diagnosis using robust standard errors generated a slope value of 1.9 (95% confidence interval 1.4–2.5) and an associated P-value of 3 × 10^-9, with a value of <0.05 considered statistically significant
Example case, a 3-year-old boy undergoing routine 3-month interval follow-up of a sporadic isolated optic pathway glioma diagnosed 2 years prior. Axial T1-weighted (a and d), post-contrast (b and e), and non-contrast fluid-attenuated inversion recovery (FLAIR; c and f) images at the level of the midbrain are shown from two consecutive contrast-enhanced MR exams. The contrast-enhanced MR images from baseline (a–c) show stable disease, and ophthalmologic exam revealed stable visual testing abnormalities. The contrast-enhanced MR images from 3 months later (d–f) show an increase in tumor size that is readily apparent on both the axial post-contrast T1 and FLAIR sequences, although visual testing abnormalities/exam remained unchanged. The boy was subsequently started on chemotherapy, with good response, in 2004. To date, he has undergone 50 contrast-enhanced MR brain exams over 14.8 years of surveillance
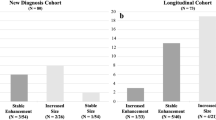
Select patient demographics and MRI exam details from our preliminary blinded review of eight patients (one with NF1 and seven without NF1) with isolated optic pathway gliomas are presented in Table 2 [44]. Percentage changes in tumor size derived from measurements on T2-weighted, FLAIR and T1-weighted post-gadolinium sequences are presented in Fig. 3. For exam pairs where size increase had motivated change in tumor-directed therapy, all size changes based on T2/FLAIR sequence measurements exceeded 25% (range: 28–106%), a commonly employed threshold for assessing meaningful size increase beyond measurement variability on neuroimaging [34, 38]. Size changes based on gadolinium-enhanced sequence measurements showed greater variability, and in two instances were less than 25% (range: 6–133%). For control exam pairs, percentage size changes based on T2/FLAIR sequences (range: −20–11%) and gadolinium-enhanced sequences (range: −12–14%) were similar. Paired t-tests revealed no significant difference between sequences within the tumor-board-defined size-increase group or the control group.
MRI sequence-specific assessments of changes in tumor size on routine follow-up exam pairs from eight children with isolated optic pathway glioma. The “size increase” group included exam pairs identified by consensus tumor board notes where an isolated increase in tumor size on MRI had led to a change in tumor-directed therapy. The “control” group included exam pairs from the same children where no significant change in tumor size was identified. In the “size increase” group, all size change assessments on T2-weighted and FLAIR sequences met a commonly used threshold of 25%, reflecting meaningful size increase. In two instances for measurements made on the post-gadolinium sequence, this threshold was not met. Solid lines represent the mean values for each group. Error bars indicate standard error from the mean. FLAIR fluid-attenuated inversion recovery, +Gd T1-weighted post-gadolinium sequence, T2W T2-weighted
To retrospectively estimate the potential impact of a non-contrast MR surveillance strategy on risk and cost in our cohort, we used the median values for 17 NF1/21 non-NF1 patients with isolated optic pathway glioma of 2.2/3.0 yearly MR brain examinations over 7.7/8.1 years of clinical follow-up to estimate median cumulative MR brain examination totals of 16.9/24.3. For a non-contrast follow-up protocol model, we assumed the patient would receive a single contrast-enhanced MRI at diagnosis and 15.9/23.3 subsequent non-contrast MRI surveillance studies, resulting in 15.9/23.3 fewer GBCA administrations. Assuming a constant moderate-to-severe allergic-like reaction incidence of 18 per 100,000 exams [45], for the median NF1/non-NF1 patient with isolated optic pathway glioma undergoing 16.9/24.3 contrast-enhanced MRIs, the cumulative incidence would be 0.30%/0.44%, versus a non-contrast follow-up protocol where the single diagnostic exam exposure would lead to a cumulative incidence of 0.018% for both patient subpopulations. Yearly and cumulative RVU burdens derived from contrast-enhanced and non-contrast MR follow-up protocol models are depicted in Fig. 4. Employing the assumptions described in the methods section to the commercial insurance coverage distribution in our study population, the 39% reduction in median yearly RVU burden achieved for both the NF1 and non-NF1 patient cohorts with a non-contrast MR follow-up protocol equates to median yearly dollars saved of $383 per NF1 patient and $481 per non-NF1 patient. Over a median 7.7/8.1 years of clinical follow-up, this translates to $2950 and $3897 saved for each NF1 and non-NF1 patient, respectively.
Potential cost impact of a non-contrast MRI follow-up protocol for children with isolated optic pathway glioma. a Mean (dotted line)/median (solid line) and interquartile range (whiskers) for global relative value units (RVUs) generated by MR brain examinations per year of isolated optic pathway glioma follow-up with a contrast-enhanced protocol (+C; 22.7/22.7, 16.8–27.7 for NF1 patients, 32.2/31.5, 23.9–39.7 for non-NF1 patients), versus a non-contrast protocol model (–C; 13.9/13.9, 10.3–16.9 for NF1 patients, 19.7/19.3, 14.6–24.3 for non-NF1 patients). Yearly RVU burden was significantly reduced for both NF1 and non-NF1 patients under the non-contrast model, with associated P-values <0.001 (***), with a value of <0.05 considered statistically significant. b Cumulative RVU burden for optic pathway glioma MR follow-up protocols. Linear regressions fit to contrast-enhanced (+C) and non-contrast enhanced (–C) models for the combined NF1 and non-NF1 patient populations generated slope values and 95% confidence intervals of 23.8 (18.2–29.5) versus 14.6 (11.1–18.0), respectively. The associated P-value was 0.006, with a value of <0.05 considered statistically significant. Note that after 5 years of follow-up the 95% confidence intervals for the best fit lines (shaded areas) no longer overlap
Discussion
The definition of “progression” of optic pathway gliomas on follow-up contrast-enhanced MR has been variably reported to involve an increase in tumor size/extension or a change in the pattern of enhancement [29, 31,32,33, 44, 46,47,48]. Heterogeneity within the literature reflects the lack of consensus imaging assessment criteria for optic pathway gliomas. The Dodge and modified Dodge criteria have been used to qualitatively classify tumors by anatomical distribution because involvement of specific locations has distinct prognostic significance [44, 47, 49, 50]. Quantitative evaluation of most gliomas is typically performed using the Response Assessment in Neuro-Oncology (RANO) criteria [38, 39, 48]. However, no well-accepted guidelines that combine these two criteria exist, and the complex radiologic features of optic pathway gliomas make them difficult to characterize using the RANO criteria. For low-grade gliomas, RANO classification emphasizes size measurements (the product of perpendicular diameters) on the T2/FLAIR sequence for assessment, rather than the size of contrast-enhancing portions (because fibrillary astrocytomas rarely enhance), as well as avoidance of cystic component measurement [38, 39]. However, optic pathway gliomas, primarily pilocytic astrocytomas, often demonstrate heterogeneous foci of enhancement in addition to T2/FLAIR hyperintensity of solid components and their cystic components sometimes contribute to clinically relevant mass effect on adjacent nerve fibers [23]. Such features make the use of RANO guidelines for therapeutic response or surveillance of untreated tumor progression difficult to apply for optic pathway gliomas. Some groups are working toward developing an imaging classification/monitoring system specific to optic pathway gliomas, emphasizing both tumor location and changes in tumor size, with sub-segmentation of tumor components (solid enhancing, solid non-enhancing, and cystic) [51,52,53,54]. The results of our study indicate that changes in optic pathway glioma size, uninfluenced by contrast enhancement characteristics, drive current management decisions that are based solely on follow-up MR imaging. In our preliminary retrospective review, changes in size were reliably apparent on T2/FLAIR sequences because the slow growth and anatomical distribution typical of optic pathway gliomas result in little or no surrounding edema that might obscure tumor borders [23]. Significant peritumoral edema effacing tumor borders has also not been described in MRI follow-up studies of chemo/radiation treatment response for optic pathway gliomas [34, 36, 37].
Our study suggests that routine surveillance MR exams for isolated optic pathway gliomas do not require gadolinium to guide management decisions. Untreated optic pathway gliomas are now recognized to have variable contrast enhancement patterns over time without associated clinical significance [23]. Similar to the experience at our institution, Gaudino et al. [55] observed “spontaneous fluctuations” (random appearance, increase, decrease or disappearance) in conventional MR contrast enhancement foci of optic-hypothalamic pilocytic astrocytomas over 3–7 years of follow-up in patients not receiving tumor-directed therapies. They observed no correlation between enhancement characteristics and clinical symptoms or tumor size (the latter based on largest diameter and orthogonal line, including cystic and solid regions, measured on T2-weighted fast spin-echo sequence). Theoretically, inflammatory reactions/degenerative changes (e.g., those induced by successful treatments) could increase blood–brain barrier permeability, resulting in cyst formation and increased contrast enhancement, but this has not been demonstrated in clinical imaging studies [56, 57]. Studies of reliable means to identify optic pathway glioma treatment response with conventional, clinical MRI are limited and difficult to perform given tumor heterogeneity and the rarity of the disease. There have been mixed results when correlating MRI findings with visual acuity changes in the context of variable study designs and patient populations [34, 36]. However one common feature implicit in the designs of these studies is the minimal value attributed to gadolinium-enhanced sequences as criteria for determining optic pathway glioma response to treatment. A recent study of contrast-enhanced MR-based response assessment for first-line chemotherapy agents in 15 patients with isolated optic pathway glioma revealed a mean decrease in the solid tumor volume (9.7%±23%), and a mean increase in the tumor cystic component (35%±100%), but no significant difference in tumor enhancement [37]. Fisher et al. [34] employed only T2-weighted sequences for imaging-based assessment of optic pathway glioma response to initial chemotherapy treatment in 71 people with NF1. Kelly et al. [36] measured tumor volumes exclusively on T2/FLAIR sequences for imaging-based assessment of optic pathway glioma response to initial therapy with chemotherapy or radiation therapy in 21 patients. In addition, a recent large clinical trial assessing chemotherapy efficacy for treatment of low-grade gliomas, including optic pathway gliomas, relied primarily on measurements from T2-weighted sequences to evaluate treatment response, rather than contrast-enhanced MRI sequences [35]. These studies, combined with the findings in our preliminary patient series, call into question any benefit of GBCA administration in children with isolated optic pathway glioma on routine follow-up exams, particularly given the large number of exams these children typically undergo.
Gadolinium administration can, however, add critical information to the initial diagnostic MR brain/orbits evaluation for a child presenting with visual symptoms, at a time when the differential diagnosis is broad. In addition, at initial diagnosis, contrast-enhanced MR can be helpful in identifying optic pathway gliomas that are more likely to progress. There have been mixed results regarding the prognostic significance of the degree of conventional contrast enhancement at the time of optic pathway glioma diagnosis [58, 59]; however, advanced quantitative techniques (such as dynamic contrast-enhanced imaging) have been shown to more reliably predict subsequent clinical progression [59, 60].
Optic pathway gliomas are the most common central nervous system tumor in NF1 patients; however additional, predominantly benign and indolent CNS tumors are also more common in people with NF1 than in the general population [29, 61, 62]. In one large series (n=104) that included 84 NF1 patients with optic pathway glioma, 20% of all patients had multiple CNS tumors, most commonly a combination of an optic pathway glioma and a low-grade brainstem tumor, equating to approximately 25% of the optic pathway glioma cohort [63]. When all brain tumors are taken into account, previous studies have found contrast administration in the NF1 population to be “useful” and “necessary” in documenting tumor stability [64, 65]. In our own study, additional CNS tumors, either pathologically proven or suspected on imaging, were seen in 4 of 22 cases (18%) of optic pathway glioma in children with NF1 who met the initial search criteria, and in none of the sporadic cases. We excluded non-isolated optic pathway glioma cases from our analysis to avoid confounding influence on neuroimaging frequency and treatment decisions, and our results are only relevant to the majority of NF1 patients with optic pathway glioma who do not have concurrent CNS tumors.
Fisher et al. [34] identified initial chemotherapy treatment rationale from retrospective chart review of 115 people with NF1 treated at 10 referral centers between 1997 and 2007. In their article “tumor enhancement” was identified as an indication for initiation of the first course of chemotherapy treatment for 23 patients, and as a “primary” indication in 16 (note that this study allowed multiple indications to be listed simultaneously as the “primary” indication, with a median of 2 “primary” indications per case). Two critical points should be considered when synthesizing these results with our study. First, Fisher et al. did not distinguish between information derived from diagnostic versus follow-up MRI exams — “tumor enhancement” might be a feature of the initial diagnostic MRI that helped to establish the diagnosis and direct therapy while the differential remained broad, or a change in the enhancement characteristics on follow-up for a known tumor. Second, despite the high degree of variability in rationale for initiating treatment between the participating institutions and the relatively large number of cases analyzed, tumor enhancement characteristics were never cited as an isolated indication for initiation of therapy, only in combination with other imaging and clinical considerations [34]. The only isolated indications for initiation of therapy in the Fisher et al. study were visual acuity loss (n=18) and tumor growth (n=10) [34]. The latter is consistent with the results of our study and has reasonable causal inference in the complex context of medical treatment directives. The variable significance attributed to optic pathway glioma enhancement by the diverse set of clinicians in Fisher et al.’s study might be attributable to evolving practice patterns at the time. The study of Fisher et al. was published 5 months prior to the paper by Gaudino et al. [55] that described variable enhancement characteristics of untreated optic pathway gliomas over time without clinical significance.
In the study by Fisher et al. [34], the authors also mentioned that the non-neoplastic T2-hyperintense white matter foci commonly observed in the brains of people with NF1 might influence tumor size assessments, but thought this to be unlikely when exams were interpreted by subspecialty neuroradiologists using a minimum 25% change as threshold for size increase. In our study, only one of the eight cases of therapy initiated based solely on change in MRI occurred in an NF1 patient with isolated optic pathway glioma — the remaining cases were sporadic optic pathway gliomas. For this single case, optic pathway glioma size increase on follow-up contrast-enhanced MR was readily apparent on T2/FLAIR sequences, was the only change identified, and motivated initiation of chemotherapy. These findings are consistent with the growing body of literature relying on T2-weighted sequences for size assessments at follow-up of both NF1 and non-NF1 optic pathway gliomas [34,35,36,37].
The ability of various GBCAs to release free gadolinium and result in tissue deposition varies but is lowest among macrocyclic agents [66, 67]. A recent survey revealed that 80% of North American pediatric hospitals use macrocyclic gadolinium-based contrast agents [5], and for hospitals who recently switched agents, the most common rationale was concern regarding gadolinium tissue deposition. In the era of macrocyclic GBCAs, some might voice skepticism as to the utility of tailoring tumor follow-up protocols to exclude gadolinium-enhanced sequences. This stems, in part, from the radiology community’s focus on surrogate markers of gadolinium deposition. For example, a recent study by Radbruch et al. [68] demonstrated no significant signal intensity increase in the dentate nucleus on non-contrast MRI in pediatric patients who had previously received up to 23 doses of macrocyclic GBCA (a phenomenon demonstrated in children exposed to linear agents) [68, 69]. Brain deposition with macrocyclic GBCAs has, however, been demonstrated pathologically in adults [7]. Furthermore, deposition is greater than in the brain in some tissues such as bone, where macrocyclic GBCAs have been shown to accumulate in concentrations as much as 23 times higher than in the brain [7]. Some have suggested that gadolinium in the bone matrix could function as a long-term systemic reservoir, slowly releasing gadolinium into the circulation and redistributing it to other organs over a long period of time [6, 16, 70]. Precise estimates of cumulative gadolinium tissue deposition in children are difficult given the incomplete understanding of specific patient and contrast-agent factors that contribute; however, given the known dose-dependence of gadolinium deposition in children [2] and the high number of follow-up contrast-enhanced MR exams children with optic pathway gliomas undergo, implementing a non-contrast MRI follow-up protocol for these children would be expected to result in a substantial reduction in accumulated gadolinium over time. Moreover, the unknown long-term risks of gadolinium deposition accompany the per-dose-risk of allergic-like contrast reaction (likely underestimated in our current study because we limited our analysis to moderate-to-severe reactions that have relatively constant incidence, versus the increasing-per-dose incidence of mild reactions), the per-dose risk of contrast extravasation, and the minor trauma of intravenous administration [71, 72]. In this context, for the purposes of guiding clinical follow-up policy decisions, the risk reduction that a non-contrast MR follow-up protocol provides to the patient is likely best quantified in absolute terms. In our study and proposed non-contrast protocol model, this was a median 15.9 and 23.3 fewer GBCA administrations over 7.7 and 8.1 years of clinical follow-up for NF1 and non-NF1 patients, respectively.
Our relatively simplistic preliminary estimations of cost efficacy are intended to provide a general impression of the impact that implementation of a non-contrast MRI follow-up protocol might have on the value of care provided to the average child with optic pathway glioma. Such considerations are particularly important in the evolving value-focused health care remuneration system [73]. We used the Centers for Medicare and Medicaid Services global RVUs to provide a standardized benchmark for the cost of follow-up MR imaging to the health care system because this method has become the reimbursement basis for Medicaid programs and many commercial payers covering the vast majority of children in the United States [74]. RVUs are robust to between-institution imaging variability and this strengthens the generalizability of our results. Assessing the cost in dollars as well as medical risk per patient examined is only a preliminary step in cost-effectiveness analysis. Assessment of the diagnostic performance and impact of a test requires knowledge of its sensitivity and specificity for a given application [75, 76]. To our knowledge, a large comparative study of non-contrast and contrast-enhanced MRI protocols for assessment of isolated optic pathway gliomas at follow-up has not been published.
Our study had limitations, including being predominantly an exploratory study with pragmatic design. While non-contrast sequences appeared to be independently effective in assessing changes in tumor size on our review of a limited sample of cases, further prospective studies of larger case sets are needed to assess the reliability and overall accuracy of this test versus a contrast-enhanced protocol for isolated optic pathway glioma follow-up. Our data were also derived from a single tertiary pediatric referral center and reviewed by a single group of academic specialists, and local practice bias might have influenced our results. The most pivotal aspect of this work was identifying instances of change in tumor-directed-therapy that were solely motivated by changes observed on contrast-enhanced MR that could be retrospectively examined. For efficiency, we chose to limit our case capture to individuals with isolated optic pathway gliomas and at least three contrast-enhanced MR brain examinations that had been internally interpreted with images available for review in PACS. This criterion helped to identify children with sufficiently large, internally available imaging repositories that could be evaluated against clinical histories. However, while our search method maximized this important aspect of case-specificity for the current study, it diminished the sensitivity of our case capture (e.g., excluding children with imaging predominantly performed at outside institutions). The yield of including these additional children in the current study would likely be low because the proportion of missing imaging data available for internal review would be high, and thus an isolated change in reviewable imaging resulting in changed management would be rare. Even in our enriched series, such instances were found in a minority of cases reviewed (21%). For a powered study of the efficacy of a non-contrast MR protocol for follow-up of isolated optic pathway gliomas, without the requirement of time-linked changes in both reviewable imaging and treatment directives, these additional cases could provide valuable diversity to blinded case review.
Conclusion
Pediatric patients with isolated optic pathway gliomas undergo a large number of routine follow-up MRI exams. Gadolinium might not be needed on these exams to inform tumor management decisions when driven by increasing tumor size on MRI. Given the lack of clinical benefit, and the potential reduction in gadolinium deposition, adverse contrast reactions, and monetary cost to the health care system, it is prudent to reassess gadolinium use in MR imaging follow-up of isolated optic pathway gliomas. Although these are preliminary results from a single center, they are consistent with a growing body of literature from multiple optic pathway glioma referral centers. Further study of larger case sets are needed to ensure reproducibility across a diverse spectrum of disease for both NF1 and non-NF1 patients with optic pathway gliomas.
References
Gale EM, Caravan P, Rao AG et al (2017) Gadolinium-based contrast agents in pediatric magnetic resonance imaging. Pediatr Radiol 47:507–521
McDonald JS, McDonald RJ, Jentoft ME et al (2017) Intracranial gadolinium deposition following gadodiamide-enhanced magnetic resonance imaging in pediatric patients: a case-control study. JAMA Pediatr 171:705–707
Kanda T, Fukusato T, Matsuda M et al (2015) Gadolinium-based contrast agent accumulates in the brain even in subjects without severe renal dysfunction: evaluation of autopsy brain specimens with inductively coupled plasma mass spectroscopy. Radiology 276:228–232
Miller JH, Hu HH, Pokorney A et al (2015) MRI brain signal intensity changes of a child during the course of 35 gadolinium contrast examinations. Pediatrics 136:e1637–e1640
Mithal LB, Patel PS, Mithal D et al (2017) Use of gadolinium-based magnetic resonance imaging contrast agents and awareness of brain gadolinium deposition among pediatric providers in North America. Pediatr Radiol 47:657–664
Roberts DR, Chatterjee AR, Yazdani M et al (2016) Pediatric patients demonstrate progressive T1-weighted hyperintensity in the dentate nucleus following multiple doses of gadolinium-based contrast agent. AJNR Am J Neuroradiol 37:2340–2347
Murata N, Gonzalez-Cuyar LF, Murata K et al (2016) Macrocyclic and other non-group 1 gadolinium contrast agents deposit low levels of gadolinium in brain and bone tissue: preliminary results from 9 patients with normal renal function. Investig Radiol 51:447–453
Roberts DR, Lindhorst SM, Welsh CT et al (2016) High levels of gadolinium deposition in the skin of a patient with normal renal function. Investig Radiol 51:280–289
Maximova N, Gregori M, Zennaro F et al (2016) Hepatic gadolinium deposition and reversibility after contrast agent-enhanced MR imaging of pediatric hematopoietic stem cell transplant recipients. Radiology 281:418–426
Rogosnitzky M, Branch S (2016) Gadolinium-based contrast agent toxicity: a review of known and proposed mechanisms. Biometals 29:365–376
Semelka RC, Ramalho M, AlObaidy M, Ramalho J (2016) Gadolinium in humans: a family of disorders. AJR Am J Roentgenol 207:229–233
U. S. Food and Drug Administration (2017) Drug safety communications. FDA evaluating the risk of brain deposits with repeated use of gadolinium-based contrast agents for magnetic resonance imaging. https://www.fda.gov/downloads/Drugs/DrugSafety/UCM455390.pdf. Accessed 17 April 2017
European Medicines Agency (2017) PRAC concludes assessment of gadolinium agents used in body scans and recommends regulatory actions, including suspension for some marketing authorisations. http://www.ema.europa.eu/docs/en_GB/document_library/Press_release/2017/03/WC500223209.pdf. Accessed 17 April 2017
American College of Radiology (2017) ACR manual on contrast media version 10.3 (78). https://www.acr.org/-/media/ACR/Files/Clinical-Resources/Contrast_Media.pdf. Accessed 12 April 2018
American College of Radiology (2017) News releases: ACR response to the European PRAC recommendations (April 4, 2017). http://www.publicnow.com/view/DA714236788989CE92F38E18EA3CCB6FCC9DFDE3?2017-04-04-17:31:30+01:00-xxx935. Accessed 12 April 2018
Goischke HK (2017) Safety assessment of gadolinium-based contrast agents (GBCAs) requires consideration of long-term adverse effects in all human tissues. Mult Scler J Exp Transl Clin 3:2055217317704450
Gupta A, Al-Dasuqi K, Xia F et al (2017) The use of noncontrast quantitative MRI to detect gadolinium-enhancing multiple sclerosis brain lesions: a systematic review and meta-analysis. AJNR Am J Neuroradiol 38:1317–1322
Heideman RL (1993) Tumors of the central nervous system. In: Pizzo PA, Poplack DG (eds) Principles and practice of pediatric oncology. Lippincott-Raven, Philadelphia, pp 633–681
Ostrom QT, Gittleman H, Fulop J et al (2015) CBTRUS statistical report: primary brain and central nervous system tumors diagnosed in the United States in 2008-2012. Neuro Oncol 17:iv1–iv62
Albers AC, Gutmann DH (2009) Gliomas in patients with neurofibromatosis type 1. Expert Rev Neurother 9:535–539
Recht LD (2017) Optic pathway glioma. In: UpToDate. https://www.uptodate.com/contents/optic-pathway-glioma. Accessed 12 April 2018
Wan MJ, Ullrich NJ, Manley PE et al (2016) Long-term visual outcomes of optic pathway gliomas in pediatric patients without neurofibromatosis type 1. J Neuro Oncol 129:173–178
Gaudino S, Martucci M, Russo R et al (2017) MR imaging of brain pilocytic astrocytoma: beyond the stereotype of benign astrocytoma. Childs Nerv Syst 33:35–54
Hernaiz Driever P, von Hornstein S, Pietsch T et al (2010) Natural history and management of low-grade glioma in NF-1 children. J Neuro Oncol 100:199–207
Kornreich L, Blaser S, Schwarz M et al (2001) Optic pathway glioma: correlation of imaging findings with the presence of neurofibromatosis. AJNR Am J Neuroradiol 22:1963–1969
Kerrison JB (2005) Chapter 38: phacomatoses. In: Miller NR (ed) Walsh & Hoyt's clinical neuro-ophthalmology, 6th edn. Lippincott Williams & Wilkins, Philadelphia, pp 1823–1898
Chateil JF, Soussotte C, Pedespan JM et al (2001) MRI and clinical differences between optic pathway tumours in children with and without neurofibromatosis. Br J Radiol 74:24–31
Prada CE, Hufnagel RB, Hummel TR et al (2015) The use of magnetic resonance imaging screening for optic pathway gliomas in children with neurofibromatosis type 1. J Pediatr 167:851–856
Listernick R, Ferner RE, Liu GT, Gutmann DH (2007) Optic pathway gliomas in neurofibromatosis-1: controversies and recommendations. Ann Neurol 61:189–198
Balcer LJ, Liu GT, Heller G et al (2001) Visual loss in children with neurofibromatosis type 1 and optic pathway gliomas. Relation to tumor location by magnetic resonance imaging. Am J Ophthalmol 131:442–445
Listernick R, Louis DN, Packer RJ, Gutmann DH (1997) Optic pathway gliomas in children with neurofibromatosis 1: consensus statement from the NF1 optic pathway glioma task force. Neuro Oncol 41:143–149
Liu GT (2006) Optic gliomas of the anterior visual pathway. Curr Opin Ophthalmol 17:427–431
Thiagalingam S, Flaherty M, Billson F, North K (2004) Neurofibromatosis type 1 and optic pathway gliomas: follow-up of 54 patients. Ophthalmology 111:568–577
Fisher MJ, Loguidice M, Gutmann DH et al (2012) Visual outcomes in children with neurofibromatosis type 1-associated optic pathway glioma following chemotherapy: a multicenter retrospective analysis. Neuro-Oncology 14:790–797
Ater JL, Zhou T, Holmes E et al (2012) Randomized study of two chemotherapy regimens for treatment of low-grade glioma in young children: a report from the Children's oncology group. J Clin Oncol 30:2641–2647
Kelly JP, Leary S, Khanna P, Weiss AH (2012) Longitudinal measures of visual function, tumor volume, and prediction of visual outcomes after treatment of optic pathway gliomas. Ophthalmology 119:1231–1237
Shofty B, Mauda-Havakuk M, Weizman L et al (2015) The effect of chemotherapy on optic pathway gliomas and their sub-components: a volumetric MR analysis study. Pediatr Blood Cancer 62:1353–1359
van den Bent MJ, Wefel JS, Schiff D et al (2011) Response assessment in neuro-oncology (a report of the RANO group): assessment of outcome in trials of diffuse low-grade gliomas. Lancet Oncol 12:583–593
Wen PY, Chang SM, Van den Bent MJ et al (2017) Response assessment in neuro-oncology clinical trials. J Clin Oncol 35:2439–2449
R Core Team (2016) R: a language and environment for statistical computing. R Foundation for Statistical Computing, Vienna. https://www.R-project.org. Accessed 14 March 2018
Centers for Medicare and Medicaid Services (2017) Searchable Medicare physician fee schedule. http://www.cms.gov/apps/physician-fee-schedule/overview.aspx. Accessed 12 Sept 2017
Clemens J, Gottlieb JD (2017) In the shadow of a giant: Medicare's influence on private physician payments. J Polit Econ 125:1–39
The Henry J. Kaiser Family Foundation (2016) State health facts — Medicaid-to-Medicare fee index (2016). http://www.kff.org/state-category/medicaid-chip/medicaid-physician-fees/. Accessed 15 Sept 2017
Taylor T, Jaspan T, Milano G et al (2008) Radiological classification of optic pathway gliomas: experience of a modified functional classification system. Br J Radiol 81:761–766
Dillman JR, Ellis JH, Cohan RH et al (2007) Frequency and severity of acute allergic-like reactions to gadolinium-containing i.v. contrast media in children and adults. AJR Am J Roentgenol 189:1533–1538
Astrup J (2003) Natural history and clinical management of optic pathway glioma. Br J Neurosurg 17:327–335
Dodge HW Jr, Love JG, Craig WM et al (1958) Gliomas of the optic nerves. AMA Arch Neurol Psychiatry 79:607–621
Wen PY, Macdonald DR, Reardon DA et al (2010) Updated response assessment criteria for high-grade gliomas: response assessment in neuro-oncology working group. J Clin Oncol 28:1963–1972
Pollack IF, Hoffman HJ, Humphreys RP, Becker L (1993) The long-term outcome after surgical treatment of dorsally exophytic brain-stem gliomas. J Neurosurg 78:859–863
Lee AG (2007) Neuroophthalmological management of optic pathway gliomas. Neurosurg Focus 23:E1
Lambron J, Rakotonjanahary J, Loisel D et al (2016) Can we improve accuracy and reliability of MRI interpretation in children with optic pathway glioma? Proposal for a reproducible imaging classification. Neuroradiology 58:197–208
Weizman L, Sira LB, Joskowicz L et al (2014) Semiautomatic segmentation and follow-up of multicomponent low-grade tumors in longitudinal brain MRI studies. Med Phys 41:052303
Weizman L, Ben Sira L, Joskowicz L et al (2012) Automatic segmentation, internal classification, and follow-up of optic pathway gliomas in MRI. Med Image Anal 16:177–188
Shofty B, Weizman L, Joskowicz L et al (2011) MRI internal segmentation of optic pathway gliomas: clinical implementation of a novel algorithm. Childs Nerv Syst 27:1265–1272
Gaudino S, Quaglio F, Schiarelli C et al (2012) Spontaneous modifications of contrast enhancement in childhood non-cerebellar pilocytic astrocytomas. Neuroradiology 54:989–995
Beni-Adani L, Gomori M, Spektor S, Constantini S (2000) Cyst wall enhancement in pilocytic astrocytoma: neoplastic or reactive phenomena. Pediatr Neurosurg 32:234–239
Takeuchi H, Kubota T, Sato K, Arishima H (2004) Ultrastructure of capillary endothelium in pilocytic astrocytomas. Brain Tumor Pathol 21:23–26
Strong JA, Hatten HP Jr, Brown MT et al (1993) Pilocytic astrocytoma: correlation between the initial imaging features and clinical aggressiveness. AJR Am J Roentgenol 161:369–372
Jittapiromsak N, Hou P, Liu HL et al (2017) Prognostic role of conventional and dynamic contrast-enhanced MRI in optic pathway gliomas. J Neuroimaging 27:594–601
Jost SC, Ackerman JW, Garbow JR et al (2008) Diffusion-weighted and dynamic contrast-enhanced imaging as markers of clinical behavior in children with optic pathway glioma. Pediatr Radiol 38:1293–1299
Singhal S, Birch JM, Kerr B et al (2002) Neurofibromatosis type 1 and sporadic optic gliomas. Arch Dis Child 87:65–70
Campian J, Gutmann DH (2017) CNS tumors in neurofibromatosis. J Clin Oncol 35:2378–2385
Guillamo JS, Creange A, Kalifa C et al (2003) Prognostic factors of CNS tumours in neurofibromatosis 1 (NF1): a retrospective study of 104 patients. Brain 126:152–160
Mentzel HJ, Seidel J, Fitzek C et al (2005) Pediatric brain MRI in neurofibromatosis type I. Eur Radiol 15:814–822
Bonawitz C, Castillo M, Chin CT et al (1998) Usefulness of contrast material in MR of patients with neurofibromatosis type 1. AJNR Am J Neuroradiol 19:541–546
Jost G, Lenhard DC, Sieber MA et al (2016) Signal increase on unenhanced T1-weighted images in the rat brain after repeated, extended doses of gadolinium-based contrast agents: comparison of linear and macrocyclic agents. Investig Radiol 51:83–89
Sieber MA, Steger-Hartmann T, Lengsfeld P, Pietsch H (2009) Gadolinium-based contrast agents and NSF: evidence from animal experience. J Magn Reson Imaging 30:1268–1276
Radbruch A, Haase R, Kickingereder P et al (2017) Pediatric brain: no increased signal intensity in the dentate nucleus on unenhanced T1-weighted MR images after consecutive exposure to a macrocyclic gadolinium-based contrast agent. Radiology 283:828–836
Flood TF, Stence NV, Maloney JA, Mirsky DM (2017) Pediatric brain: repeated exposure to linear gadolinium-based contrast material is associated with increased signal intensity at unenhanced T1-weighted MR imaging. Radiology 282:222–228
Abraham JL, Thakral C (2008) Tissue distribution and kinetics of gadolinium and nephrogenic systemic fibrosis. Eur J Radiol 66:200–207
Costello JR, Kalb B, Martin DR (2016) Incidence and risk factors for gadolinium-based contrast agent immediate reactions. Top Magn Reson Imaging 25:257–263
Jung JW, Kang HR, Kim MH et al (2012) Immediate hypersensitivity reaction to gadolinium-based MR contrast media. Radiology 264:414–422
Stecker EC, Schroeder SA (2013) Adding value to relative-value units. N Engl J Med 369:2176–2179
The Henry J. Kaiser Family Foundation (2017) Next steps for CHIP: what is at stake for children? http://files.kff.org/attachment/Fact-Sheet-Next-Steps-for-CHIP-What-is-at-Stake-for-Children. Accessed 14 Sept 2017
Patton DD, Woolfenden JM (1989) A utility-based model for comparing the cost-effectiveness of diagnostic studies. Investig Radiol 24:263–271
Hollingworth W, Jarvik JG (2007) Technology assessment in radiology: putting the evidence in evidence-based radiology. Radiology 244:31–38
Acknowledgment
Dr. Maloney is supported, in part, through a National Institutes of Health, National Research Service Award training grant (grant number 5 T32 DK0072).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Additional information
This article was awarded the John Kirkpatrick Young Investigator Award at the Society for Pediatric Radiology 2017 meeting.
Rights and permissions
About this article
Cite this article
Maloney, E., Stanescu, A.L., Perez, F.A. et al. Surveillance magnetic resonance imaging for isolated optic pathway gliomas: is gadolinium necessary?. Pediatr Radiol 48, 1472–1484 (2018). https://doi.org/10.1007/s00247-018-4154-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-018-4154-4