Abstract
Background
Cuboid fractures are rare, usually occult on initial radiographs and are often underdiagnosed. MRI is more sensitive than radiographs for detecting acute, non-displaced cuboid fractures in adults, but only case reports have described these findings in children.
Objective
To summarize the MR and clinical features of cuboid fractures and compare MR findings with initial and follow-up radiographs in a cohort of children.
Materials and methods
A retrospective search for patients <18 years of age with cuboid fractures was performed during a 10-year period at a large tertiary children’s hospital. Subjects with cuboid fractures reported on MRI and available clinical history were included. MR images were evaluated for fracture location, fracture morphology, percentage of marrow edema in the cuboid, subchondral disruption, and associated tendon or ligamentous injury. Initial and short-term follow-up radiographs were also reviewed when available.
Results
Nineteen children ages 18 months to 17 years (mean: 9.0 years, standard deviation: 4.1 years, 63% boys) were diagnosed with cuboid fractures by MRI. Most cases of cuboid fractures are related to acute trauma (63%) but can be seen as stress fractures (16%). Most fractures (17/19, 89%) were linear in configuration. Fractures were most commonly adjacent to the tarsometatarsal joint (10/19, 52%). The degree of marrow edema was variable. Ligamentous injury was seen in two patients and tendon pathology was seen in one, all adolescents. Initial radiographs (n=10) were negative in 9 cases (90%). All available follow-up radiographs (n=12, obtained 19–42 days after MRI) demonstrated sclerosis in the region of the fracture.
Conclusion
MR-depicted cuboid fractures in children typically occur in isolation. The fractures were most commonly adjacent to the tarsometatarsal joint and linear in morphology. Initial radiographs were usually normal and follow-up radiographs depicted sclerosis at the site of fracture in all available cases.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The cuboid bone, located in the lateral midfoot, serves as a central pillar of the lateral column and is subject to a variety of compressive and shearing forces [1]. Cuboid fractures are rare in both adults and children. When these fractures do occur in children, they often go undiagnosed, as they are frequently occult on radiographs and the history and physical exam in small children is often vague. In a small series describing cuboid fractures in preschool children, 71% were not diagnosed until at least a 2-week follow-up [2]. Although the MR imaging features of pediatric cuboid fractures have not been well described in the literature, MR imaging has been found to be both sensitive and specific for evaluating occult fractures [3].
Much of what is known about imaging pediatric cuboid fractures is limited to case reports and case series. Although there have been a few retrospective studies that have reviewed the clinical and imaging features of cuboid fractures in both adults and children, to our knowledge there are no retrospective or prospective studies describing the MR imaging of cuboid fractures in children. In children, Englaro et al. [4] demonstrated that the cuboid bone was the most common origin of injury in the foot in a large cohort of preschool children undergoing bone scintigraphy for lower extremity pain and gait abnormality. Senaran et al. [2] also studied the clinical and radiographic features of cuboid fracture in 28 pediatric patients demonstrating that fractures were often not detected radiographically until 1–2 weeks after the injury, characterized by sclerosis and callus formation [2, 4]. In adults, the MR features of cuboid fractures have been described in a retrospective review of 10 patients [5].
The purpose of this study is to summarize the MR and clinical features of cuboid fractures and compare MR findings with initial and follow-up radiographs in a cohort of children.
Materials and methods
This is a retrospective study of children with MR-confirmed cuboid fractures at a tertiary children’s hospital during a 10-year period. The institutional review board approved the study protocol and the requirement for patient consent was waived. A search was carried out on imaging studies within our database from September 1, 2006, to September 1, 2016, using Montage® (Montage Healthcare Solutions, Philadelphia, PA) and Illuminate® (Softek Solutions, Prairie Village, KS) software. The electronic medical record for each patient was also reviewed. Search criteria included all patients <18 years old with a foot or ankle MR with final report including the keywords “cuboid” and “fracture,” or “cuboid” and “stress.” The medical record was then reviewed to confirm diagnosis of cuboid fracture either with clinical assessment, follow-up radiographs or both. Patients with nondiagnostic MR images or without diagnostic criteria for cuboid fracture on MR were excluded. None of the patients included in our study had undergone CT or nuclear scintigraphy. The electronic medical record was reviewed for clinical background information including date of injury, laterality, etiology and mechanism of injury, sport or activity involved in, presenting symptoms, treatment and outcome.
The MR imaging was also correlated with available initial and follow-up radiographs of the foot when available. Initial radiographs of the foot were obtained at the time of injury or initial presentation. Follow-up radiographs of the foot were those obtained more than 7 days after injury or initial presentation. All radiographs of the foot included frontal, inverted oblique and lateral projections. MRI studies were obtained with the patient in a supine position. The positioning of the foot was variable during scanning. MRI scanners varied between 1.5- and 3-T machines from various manufacturers. The ankle protocol included a combination of the following parameters: proton density turbo spin echo fat saturated in axial and sagittal planes, T2 turbo spin echo fat saturated in axial and coronal planes, and T1 images in coronal plane. The foot protocol included proton density turbo spin echo fat saturated in short axis, footprint and sagittal planes, short tau inversion recovery (STIR) footprint, and T1 spin echo footprint images.
The radiographs and MR images were reviewed by consensus of two fellowship-trained pediatric radiologists (N.A.C. and D.M.B.) with 7 and 6 years of experience, respectively, along with a pediatric radiology fellow (M.C.O). Both initial and follow-up radiographs were reviewed for linear lucency, subchondral disruption, sclerosis of the cuboid bone; soft-tissue swelling, fracture of additional bones and anatomical variants. On MR, the diagnostic criterion for a cuboid fracture was edema on T2-weighted imaging with a low linear signal on T1-weighted imaging consistent with a fracture line. The cuboid fractures were characterized by fracture location, fracture morphology (linear or stellate), location and percentage of marrow edema in the cuboid, presence of subchondral disruption and associated tendon or ligamentous injury. Given the complex shape of the cuboid, fracture and marrow edema location was determined relative to the nearest joint (tarsometatarsal anteriorly, calcaneocuboid posteriorly, and cuneocuboid or cuboideonavicular medially). Marrow edema and/or hemorrhage was defined as increased signal on T2 images or decreased signal on T1 images. The percentage of edema present was measured subjectively and divided into quartile groups (i.e. 0–25%, 25–50%, etc.). Subchondral disruption was defined as a step-off deformity or displacement of the osseous cortex associated with the fracture. Tendon or ligamentous injury was defined as increased signal within the tendon, tendon sheath or ligament on fluid-sensitive sequences, thickening of the tendon or ligament, or disruption of the fibers in the tendon or ligament.
Results
Nineteen children ages 18 months to 17 years (mean: 9.0 years, standard deviation: 4.1 years), 63% boys, were diagnosed with cuboid fracture by MRI. Two patients were excluded, both of whom had nonspecific edema within the cuboid with absence of a fracture line. One of the patients had a pathological fracture through an enchondroma of the phalanx and the other patient was diagnosed with Freiberg disease.
The right cuboid was involved in 14/19 (74%) of patients. Trauma was the most common etiology (12/19, 63%) of these patients, followed by unknown etiology and repetitive stress injuries. Five of these patients sustained cuboid fractures while playing sports. The sports involved were gymnastics (n=2), dance, track and lacrosse. Limping was the more common presenting symptom in small children, while focal pain and swelling were more common in older children. All MR studies were obtained within 2 months of the initial injury or pain (mean time from injury/pain to MRI was 17 days with a range of 2 to 47 days). Clinical findings are included in Table 1.
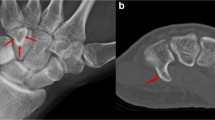
There were 10 cases with initial radiographs available and 14 with follow-up radiographs. None of the initial radiographs demonstrated sclerosis. Follow-up radiographic series included the same projections and were obtained between 11 and 42 days of the initial injury. One follow-up radiograph was obtained prior to the initial MRI. Initial radiographs were negative in 9/10 cases (90%). One case demonstrated a linear lucency corresponding to the cuboid fracture. All available follow-up radiographs (n=14) demonstrated sclerosis in the region of the fracture (Table 2) (Fig. 1).
On MRI, most fractures (17/19, 89%) were linear (Fig. 2) with associated bone marrow edema or hemorrhage. There was significant variability in fracture location and degree of marrow edema. However, a small majority was adjacent to the tarsometatarsal joint (10/19, 52%). Ligamentous injury was seen in two patients, and tendon pathology was seen in one (Fig. 3). All of the patients with tendon or ligament pathology were adolescents. In three patients, there were additional fractures. Two patients had fractures of the base of the metatarsals and the third patient had a fracture of the navicular. No anatomical variants were seen during imaging review. All patients were successfully treated conservatively with lower extremity immobilization and healed in 1–3 months.
MRI of a cuboid fracture in a 13-year-old girl following a fall during gymnastics. Sagittal T1-weighted (a) and sagittal fat-suppressed T2-weighted (b) MR images of the midfoot demonstrate a linear, hypointense fracture line (arrow) without obvious subchondral disruption along the tarsometatarsal joint, as well as marked edema (arrowheads) occupying more than 75% of the volume of the cuboid. To assist with orientation, the calcaneus is marked by an asterisk
MRI of a partial tear of the calcaneocuboid ligament associated with a cuboid fracture in a 17-year-old male lacrosse player with foot pain. Sagittal short tau inversion recovery (STIR) image of the foot demonstrates increased signal within the calcaneocuboid ligament (arrowheads) without full-thickness tear
Discussion
Cuboid fracture is a cause of foot pain and unexplained limping in children that is frequently occult on initial radiographs. Additionally, history and physical exam findings can be ambiguous in small children making the diagnosis of cuboid fracture challenging. In children, cuboid fractures are often occult on initial radiographs but are almost always present on follow-up [2]. Also, bone scintigraphy has been proven useful for the early diagnosis of pediatric cuboid fracture in the setting of negative radiographs [6]. MRI has demonstrated sensitivity in diagnosing acute bone injuries in children and in the cuboid in adults. Sadineni et al. [3] showed that in a cohort of 75 individuals with recent radiographically occult bone injuries within 4 weeks, 16 (21%) were shown to have fractures on MRI and 39 (52%) had bone contusions. Miller et al. [7] further demonstrated the superiority of MRI in demonstrating radiographically occult cuboid fractures. In a cohort of 17 adults with isolated cuboid fracture, 8 were demonstrated on MRI after being occult on radiographs [7].
The cuboid bone is a lesser tarsal bone centered in the lateral column of the midfoot. As the only bone that articulates with both the midtarsal joint and the tarsometatarsal joint, it is responsible for much of the stability in the lateral longitudinal arch of the foot. The bone is pyramidal in shape with six surfaces, three of them articular with a total of five articular facets [8]. The articular surfaces form the calcaneocuboid joint proximally, the cuneocuboid and occasionally the cuboideonavicular joint medially, and the fourth and fifth tarsometatarsal joints distally. There is a deep groove on the anterior plantar surface (i.e. the peroneal sulcus), which contains the peroneus longus tendon. The long plantar ligament inserts on a prominent ridge immediately posterior to the peroneal sulcus [9]. The tibialis posterior tendon (the only muscular attachment on the cuboid) inserts on the cuboid tuberosity along the lateral aspect of the plantar surface. Numerous additional ligaments attach the adjacent bones to the plantar and dorsal surfaces of the cuboid [10]. The plantar fascia provides stability along the plantar surface of the cuboid, and disruption has been associated with stress fracture [11]. These anatomical features lead to a myriad of potential mechanisms of injury that usually require significant energy to produce [12]. Avulsion injuries, though incompletely understood, are likely the result of an inversion injury. Crush injuries typically occur along articular surfaces and are likely the result of compression between adjacent bones. The nutcracker mechanism, first described by Hermel and Gershon-Cohen [13], is a type of crush injury. In this injury, described commonly in horseback riders, the cuboid is compressed between the metatarsals anteriorly and the calcaneus posteriorly, similar to a nutcracker [14, 15]. Comminuted fractures typically result from direct high-impact trauma to the lateral foot.
Hermel and Gershon-Cohen [13] first described the nutcracker mechanism of cuboid fracture in a case series in 1952. Since then, the literature on cuboid fractures has largely been limited to case reports in both adults [8, 16,17,18] and children [19,20,21,22]. In children, Blumberg and Patterson [23] described a case series of four toddlers’ cuboid fractures in 1991, and concluded that delayed radiographs may be sufficient to diagnose cuboid fractures in limping toddlers with witnessed foot injury. Ceroni et al. [15] also reported four cuboid fractures in children injured during horseback riding, providing further evidence for the nutcracker mechanism. In eight cuboid fractures in children younger than 4 years old, Simonian et al. [24] concluded that bone scintigraphy can help lead to an earlier diagnosis in the setting of negative radiographs in a limping child.
There have been several recent studies on the clinical and imaging features of cuboid fractures, although none was specifically designed to describe the MR imaging features of such fractures in children. In a retrospective review of adults, Yu et al. [5] studied the MRI features of isolated cuboid fractures concluding that most adult cuboid fractures are inferolateral (i.e. not associated with a joint) and are most often associated with abnormalities of the plantar fascia or peroneus tendon, and are more common in women 9/10 (90%). Senaran et al. [2] studied the clinical and radiographic characteristics of cuboid fractures in 28 school-aged children. They concluded that cuboid fractures were often occult on initial radiographs but were almost always present on follow-up radiographs obtained between 1 and 4 weeks following the initial injury. Most injuries in this cohort were related to minor trauma (e.g., fall from steps or ankle sprains). All 28 cases healed within 13 weeks with immobilization only. None of the patients in their cohort underwent MRI for diagnosis. They concluded that further imaging with bone scintigraphy or MRI was not necessary as cuboid fracture would eventually be seen on radiography as sclerosis [2]. In a demographically similar cohort of 25 small children, Joo et al. [6] concluded that bone scintigraphy may be useful for the early diagnosis of cuboid fracture in the setting of negative radiographs.
In our study group, there were significantly more males (63%) with cuboid fractures, which is similar to previous pediatric studies by Senaran et al. [2] (61%) and Joo et al. [6] (52%). In the adult populations studied by Miller et al. [7] and Yu et al. [5], women were much more commonly affected, 76% and 90%, respectively. Right-side injuries were more common in our study (74%), which was also similar to results by Senaran et al. [2] (64%), but different than Joo et al. [6] (40%). In prior studies, trauma is the most common etiology and is often related to sports injuries in adolescents, teenagers and adults. In the study by Yu et al. [5], 7/10 (70%) of cuboid fractures in adults were related to sports, mostly in runners (n=5) with one related to dance and one related to gymnastics. Similar to our results, prior studies on children also suggest limp as the most common presentation in toddlers, whereas focal pain and swelling are more common in older children and adults.
When comparing to MR findings in adults, we found that most fractures were linear in configuration in both pediatric (89%) and adult (80%) populations. In contrary to the adult literature, only 16% of pediatric cuboid fractures had associated ligament or tendon pathology whereas 40% of adults had concomitant ligament or tendon pathology [5].
In our patient population, initial radiographs for cuboid fractures were negative. Although follow-up radiographs are not needed to confirm an MR diagnosis of an occult fracture, radiographs obtained 1–5 weeks after the initial injury were positive for sclerosis and callus formation. This was a similar finding in prior studies by Senaran et al. [2] and Miller et al. [7].
There are several limitations to our study. Of most significance, the retrospective nature of the study prevents standardized work-up and patient management. Second, there was a low sample size precluding statistical analysis. Third, this was a single institution study; therefore, our patient population is dependent on the work-up and referral patterns of our orthopedic and sports medicine clinicians. Also, our population may not mirror the population at smaller community hospitals or outpatient clinics. Finally, not all patients had initial and follow-up radiographs available, and the interval between studies was variable, which affects the imaging appearance of fractures.
Conclusion
MR-depicted cuboid fractures in children typically occur in isolation and have a variable pattern of injury. Initial radiographs are usually normal. Although not needed for an MR-confirmed occult fracture, follow-up radiographs were useful for depicting sclerosis at the fracture site. In young children, cuboid fractures are isolated injuries as accompanying ligamentous and tendon injuries were seen in older children.
References
Pierre-Jerome C, Reyes EJ, Moncayo V et al (2012) MRI of the cuboid bone: analysis of changes in diabetic versus non-diabetic patients and their clinical significance. Eur J Radiol 81:2771–2775
Senaran H, Mason D, De Pellegrin M (2006) Cuboid fractures in preschool children. J Pediatr Orthop 26:741–744
Sadineni RT, Pasumarthy A, Bellapa NC, Velicheti S (2015) Imaging patterns in MRI in recent bone injuries following negative or inconclusive plain radiographs. J Clin Diagn Res 9:TC10–TC13
Englaro EE, Gelfand MJ, Paltiel HJ (1992) Bone scintigraphy in preschool children with lower extremity pain of unknown origin. J Nucl Med 33:351–354
Yu SM, Dardani M, Yu JS (2013) MRI of isolated cuboid stress fractures in adults. AJR Am J Roentgenol 201:1325–1330
Joo SY, Jeong C (2015) Stress fracture of tarsal cuboid bone in early childhood. Eur J Orthop Surg Traumatol 25:595–599
Miller TT, Pavlov H, Gupta M et al (2002) Isolated injury of the cuboid bone. Emerg Radiol 9:272–277
Kolker D, Marti CB, Gautier E (2002) Pericuboid fracture-dislocation with cuboid subluxation. Foot Ankle Int 23:163–167
Borrelli J Jr, De S, VanPelt M (2012) Fracture of the cuboid. J Am Acad Orthop Surg 20:472–477
Dodson NB, Dodson EE, Shromoff PJ (2008) Imaging strategies for diagnosing calcaneal and cuboid stress fractures. Clin Podiatr Med Surg 25:183–201 vi
Yu JS, Solmen J (2001) Stress fractures associated with plantar fascia disruption: two case reports involving the cuboid. J Comput Assist Tomogr 25:971–974
Mayr J, Peicha G, Grechenig W et al (2006) Fractures and dislocations of the foot in children. Clin Podiatr Med Surg 23:167–189 ix
Hermel MB, Gershon-Cohen J (1953) The nutcracker fracture of the cuboid by indirect violence. Radiology 60:850–854
Bahel A, Yu JS (2010) Lateral plantar pain: diagnostic considerations. Emerg Radiol 17:291–298
Ceroni D, De Rosa V, De Coulon G, Kaelin A (2007) Cuboid nutcracker fracture due to horseback riding in children: case series and review of the literature. J Pediatr Orthop 27:557–561
Franco M, Albano L, Kacso I et al (2005) An uncommon cause of foot pain: the cuboid insufficiency stress fracture. Joint Bone Spine 72:76–78
Hunter JC, Sangeorzan BJ (1996) A nutcracker fracture: cuboid fracture with an associated avulsion fracture of the tarsal navicular. AJR Am J Roentgenol 166:888
Williams DP, Hanoun A, Hakimi M et al (2009) Talonavicular dislocation with associated cuboid fracture following low-energy trauma. Foot Ankle Surg 15:155–157
Holbein O, Bauer G, Kinzl L (1998) Fracture of the cuboid in children: case report and review of the literature. J Pediatr Orthop 18:466–468
Hsu JC, Chang JH, Wang SJ, Wu SS (2004) The nutcracker fracture of the cuboid in children: a case report. Foot Ankle Int 25:423–425
Nicastro JF, Haupt HA (1984) Probable stress fracture of the cuboid in an infant. A case report. J Bone Joint Surg Am 66:1106–1108
Stalder H, Zanetti M (2000) Stress fracture of the cuboid in an 8-year-old boy: a characteristic magnetic resonance imaging diagnosis. Arch Orthop Trauma Surg 120:233–235
Blumberg K, Patterson RJ (1991) The toddler's cuboid fracture. Radiology 179:93–94
Simonian PT, Vahey JW, Rosenbaum DM et al (1995) Fracture of the cuboid in children. A source of leg symptoms. J Bone Joint Surg (Br) 77:104–106
Acknowledgments
This abstract was presented at the Society for Pediatric Radiology 2017 meeting in Vancouver, British Columbia, Canada.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Rights and permissions
About this article
Cite this article
O’Dell, M.C., Chauvin, N.A., Jaramillo, D. et al. MR imaging features of cuboid fractures in children. Pediatr Radiol 48, 680–685 (2018). https://doi.org/10.1007/s00247-018-4076-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-018-4076-1