Abstract
Background
Our understanding of osseous morphology and pathology of the patellofemoral joint continues to improve with the use of magnetic resonance imaging (MRI), but a paucity of data currently exists in the pediatric population.
Objective
We aim to formulate a reproducible means of quantitative assessment of patellofemoral morphology in children using MRI and to describe morphological changes based on sex and age.
Materials and methods
We identified 414 children presenting between 2002 and 2014 who obtained a knee MRI to evaluate for knee pain or clinically suspected knee pathology. After application of inclusion criteria, 144 “normal” MRIs in 131 children (71 boys, 60 girls) were included in the analysis. The following MRI measurements were recorded: lateral trochlear inclination, trochlear facet asymmetry, trochlear depth, tibial tuberosity-trochlear groove distance, sulcus angle and patellar height ratio. To assess intraobserver reliability, measurements in 30 randomly selected children were repeated. Differences between patient age and sex were assessed using independent t-tests and adjusted regression analysis.
Results
All recorded measurements had strong to very strong inter- and intraobserver reliability: lateral trochlear inclination (0.91/0.82), trochlear facet asymmetry (0.81/0.83), trochlear depth (0.83/0.90), tibial tuberosity-trochlear groove distance (0.97/0.87), sulcus angle (0.84/0.78) and patellar height ratio (0.96/0.83). When age and sex were mutually adjusted, statistically significant differences between males and females were observed in trochlear depth (P = 0.0084) and patellar height ratio (P = 0.0035). However, statistically significant age differences were found on all measurements except for lateral trochlear inclination. As expected, mean measurement values approached adult norms throughout skeletal maturation suggestive of age-dependent patellofemoral maturation.
Conclusion
Our data verify the development of patellofemoral morphology with advancing age. We found that six of the most commonly used patellofemoral measurements in adults can be accurately reproduced regardless of age.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Plain radiographs and computed tomography (CT) are frequently used in the evaluation of anterior knee pain and patellofemoral disorders [1–5]; however, the inability to visualize the surrounding soft tissues and articular surfaces has made magnetic resonance imaging (MRI) an increasingly important diagnostic tool [6–8]. Further supporting the routine use of MRI, recent cadaver and MRI studies have shown that significant variations exist between the bony and cartilaginous contours of the patellofemoral joint [9–11]. This is an important consideration when surgical restoration of patellofemoral anatomy is necessary. As a result, quantitative and qualitative measurements of patellar instability once described on CT and X-ray have now been adapted to MRI [5, 12–15].
Our understanding of osseous morphology and pathology of the patellofemoral joint continues to improve with MRI, but a paucity of data exists in children. With early identification of normal and abnormal patellofemoral anatomy, patient outcomes may be improved. By using MRI-based patellofemoral measurement techniques described in adults, we have two aims: 1) to formulate a reproducible and reliable means of quantitative assessment of patellofemoral morphology in children and 2) to describe morphological features based on age and sex.
Materials and methods
Study population
After approval from our Institutional Review Board, we identified 414 children presenting between 2002 and 2014 who obtained a knee MRI to evaluate for knee pain or clinically suspected knee pathology. All imaging was stored in our Picture Archiving and Communication Systems (PACS) and read by a pediatric-trained radiologist.
Inclusion criteria were: 1) ages 1 through 16, 2) open physis at the distal femur and 3) normal or near-normal MRI findings. Normal MRIs were determined by the lack of structural abnormalities; however, to increase study subjects in the 1- to 4-year-olds, we did include a small number of near-normal radiologic findings that would have little effect on patellofemoral anatomy. These included baker’s cysts, discoid menisci and small effusions. Based on anticipated physeal closure, girls were only included up to age 14, while boys were included up to age 16. To allow for equal age distribution, we randomly selected five knee MRIs for girls and five MRIs for boys to represent each age group with the exception of 1- to 2-year-olds for whom all MRIs were included. Patients were excluded if the knee MRI included any of the following: moderate to severe effusions, cartilaginous defects including cartilage and subchondral edema, patellofemoral abnormalities (e.g., patellar tilt and subluxation, trochlear dysplasia), ligamentous injury, neoplasms, infection, congenital disease, contractures or arthritic changes. Additionally, knees were excluded if MRI obtained showed the knee to be >10 degrees of knee flexion on the sagittal plane.
A total of 144 normal MRIs in 131 children (71 boys, 60 girls) were included in the analysis after meeting criteria. Ten children had bilateral knee MRIs and two had a repeat ipsilateral knee MRI performed at a later age. Multiple MRIs in the same child were included only after criteria were met.
MR protocol
All MR imaging was performed at our institution utilizing a 1.5- to 3.0-T system with a knee coil (GE Signa Excite HD 1.5 T, GE Signa HD XT 3 T, GE Healthcare, Waukesha, WI, and Siemens Skyra 3 T, Siemens Healthcare, Malvern, PA). Children younger than 2 were done using a torso or cardiac coil with 4 or 8 channels. Each patient had routine knee images as per hospital protocol, which involves neutral positioning of knees, typically 0–10 degrees of knee extension. The following sequences were obtained in each patient: axial proton density (PD) fast-spin echo (FSE) with fat saturation, coronal conventional T1-W, coronal FSE T2-W with fat saturation, coronal FSE PD, sagittal FSE PD, and sagittal FSE T2-W with fat saturation.
The axial and sagittal measurements were obtained from T2 or PD sequences for optimal cartilage visualization. Axial slice thickness was between 3 and 5 mm, whereas sagittal slices were 2–4 mm in thickness. An open distal femoral physis was only considered to be present after visualization of a discrete cartilage signal across the entire physis on a fat-suppressed FSE T2- or PD-weighted axial sequence.
MRI measurements
After review of the current literature and collaboration between a pediatric-trained radiologist with 17 years of post-fellowship experience and a pediatric orthopedic surgeon with 13 years of post-fellowship experience, six measurements were selected for analysis. Measurement techniques were based on existing literature and were discussed between authors to ensure uniformity of measurements. Under the guidance of the two senior authors (B.H.A.,K.E.K.), each of our measurements was recorded by a third-year orthopedic resident (A.R.) and a medical school graduate (A.M.). The following MRI measurements were recorded: lateral trochlear inclination (Fig. 1), trochlear facet asymmetry (Fig. 2), trochlear depth (Fig. 3), tibial tuberosity-trochlear groove distance (Fig. 4), sulcus angle (Fig. 5) and patellar height ratio (Fig. 6). To assess intraobserver reliability, measurements in 30 randomly selected patients were repeated. Each author obtained all measurements individually and was blinded to the results of the other. The data were stratified based on age and sex.
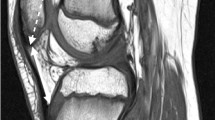
Tibial tuberosity – trochlear groove distance measured in a 6-year-old girl. Superior attachment of patellar tendon at tibial tuberosity is marked (a) and then transposed on our standard axial sequence (b). The distance between the marker (*) and solid white line that is extending through the deep sulcus to the reference line was recorded
All measurements were performed to include cartilaginous landmarks on the patella and distal femur. Five axial measurements were taken at a single sequence where the distal femoral condylar width was the greatest. The sixth measurement, patellar height ratio (i.e., Insall-Salvati Ratio), was assessed on the most midline sagittal sequence by counting all sequences containing the patella and dividing by two. Using this guided criteria, each reviewer independently determined which axial and sagittal sequence would be used to obtain each measurement. The six measurement techniques are outlined in Table 1.
Statistical analysis
Statistical analysis to determine intraobserver and interobserver reliability was performed. Mean values, standard deviation (SD) and 95% confidence intervals (CI) of all six patellofemoral measurements were determined. Sex differences were compared in all patellofemoral measurements using independent t-tests. Regression analyses were performed on all six patellofemoral measurements respectively, with age and sex mutually adjusted in the six regression models. A statistically significant level was set at α = 0.05. All analyses were performed using SAS 9.3 (Cary, NC).
Results
High correlations were observed between two data recorders and test-retest for one data recorder across all six measurements. All these correlations are statistically significant, demonstrating high inter- and intraobserver reliability (Table 2). Table 3 presents total population mean, SD and 95% CI for the six measurements. There were no statistically significant differences between boys and girls on all measurements except for trochlear depth (P = 0.0037).
Table 4 describes the mean values, along with SD, at each individual age across our six measurements. The results from our regression analyses showed that after adjusting for age, two of six measurements showed statistically significant sex differences, including trochlear depth (P = 0.0084) and patellar height ratio (P = 0.0035) (Table 5). However, all six measurements except for lateral trochlear inclination showed statistically significant differences in age after adjusting for sex. Specifically, as age increased, trochlear depth (P < 0.0001), tibial tuberosity-trochlear groove distance (P < 0.0001) and patellar height ratio (P < 0.0001) significantly increased, while trochlear facet asymmetry (P < 0.0001) and sulcus angle (P < 0.0001) significantly decreased, suggesting a gradual trend toward adult values with increasing age.
Discussion
Patellar instability is frequently encountered in children with clinical presentation ranging from mild anterior knee pain to obligatory instability. An incidence of first‐time acute patellar dislocation is seen in 48 of 100,000 children [16]. Routinely observed in the second decade of life, patellar instability is a multifactorial disorder characterized by bony abnormalities or a dysfunction in the static and dynamic soft-tissue stabilizers surrounding the knee [3, 16, 17]. During evaluation, the orthopedist must differentiate between soft-tissue and osseous abnormalities as operative and nonoperative indications may vary.
Dejour et al. [3] first utilized radiographs to generate a reproducible and quantitative means of assessing patellar instability, whereupon four factors were found to be most closely associated with symptomatic patellar instability: trochlear dysplasia, quadriceps dysplasia, patella alta and tibial tuberosity-trochlear groove distance. More recent studies have utilized MRI for diagnostic purposes and its ability to differentiate between bony and cartilaginous surfaces [11]. Using MRI, patellofemoral morphology has been standardized in adults, but normative data in children is lacking [18, 19].
Kim et al. [19] first utilized adult patellofemoral measurements in children to describe age- and sex-related changes throughout skeletal maturation. After children were stratified based on sex and the presence of an open or closed physis, no statistically significant differences were found. However, there were two primary limitations of their study: The majority of their patients was older than 10 years of age with half found to have a closed or closing physis. The lack of children under 10 years of age may unfavorably distribute the open physeal group mean values toward adult or closed physeal values, thus contributing to the lack of statistical significance. In our study, we included children only with an open physis and we distributed equally across all ages. As expected, our total mean values, with the exception of tibial tuberosity-trochlear distance, were most similar to those in the open physeal group.
Our regression analysis further depicts the progression of patellofemoral change that occurs throughout skeletal maturation. The results showed that statistically significant age differences were observed in all six measurements with the exception of lateral trochlear inclination. As age increased, the mean patellofemoral values were more likely to differ from those of younger children and began to approach adult norms [20]. Our data suggest that pediatric patellofemoral measurements should not be compared across all ages, and should be used judiciously, if at all, in the youngest patients. Furthermore, through comparison of our patellofemoral measurements to the closed physeal patients of Kim et al. [19] and to the adult mean values as described by Charles et al. [20], we can appreciate that minimal patellofemoral changes occur after physeal closure as the knee adopts adult morphology. As there is an abundance of adult literature, the study by Charles et al. [20] was selected for comparison due to similar measurement techniques across the six measurements used. As knee maturation progressed, each of our six measurements approached adult values [20].
Lateralization of the tibial tubercle is a well-known risk factor of patellar instability, and can be assessed by measurement of tibial tuberosity-trochlear groove distance [8, 18, 21, 22]. A threshold of 20 mm has traditionally been interpreted as abnormal in adults, but additional studies have shown that normative tibial tuberosity-trochlear groove distance values are subject to considerable variation as patellar instability can be seen in patients with a tibial tuberosity-trochlear groove distance as low as 10–20 mm [3, 8, 21–23]. In the pediatric cohort, Dickens et al. [18] describes tibial tuberosity-trochlear groove distance chronologically from birth into adulthood, and determined that tibial tuberosity-trochlear groove distance can be reliably reproduced in the skeletally immature knee and will reach adult norms as a child enters adolescence. Although we utilized a slightly different measurement technique, our mean of 7.84 mm was similar to Dickens’ mean of 8.6 mm [18]. Similarly, our age-based means steadily increased as described by Dickens [18].
Each of the six measurements had excellent reproducibility regardless of age or sex. During sex-based comparison of mean measurement values, we found that only trochlear depth and patellar height ratio were statistically different. The sex-based differences of trochlear depth have been demonstrated in a few adult studies [24, 25] and are believed to be due to the smaller trochlear height-condylar width ratio in girls [24]. These statistical differences may also be the result of a relatively small number of boys and girls within each age group. Pfirrmann et al. [13] suggests that the most sensitive data would include axial measurements at 3 cm above the joint space, but this technique is not reliably replicated in skeletally immature knees where joint space distances vary considerably and cartilage cannot be reliably seen at the most craniocaudal slice [25, 26]. To account for these discrepancies, we used the axial sequence with the largest femoral condylar width, which could easily be identified in all children, and has been shown to be accurate in previous pediatric studies [19]. Of note, Pfirrmann [13] was able to show statistically significant differences in trochlear depth and trochlear facet asymmetry at 1 to 2 cm above the joint space as well, which would more closely resemble our measurement technique [13].
Our study has several limitations. First, we utilized chronological age, when bone age would be a better predictor of skeletal maturation. Using bone age to calculate age-predicted maturation would perhaps change our mean values and result in statistical significance. However, determination of bone age in a retrospective review is difficult as the majority of patients are without adequate imaging to do so. Furthermore, available orthogonal axial and sagittal sequences within PACS may differ between individuals resulting in variability in reviewer slice selection and, therefore, patellofemoral measurements. This is especially true in the youngest of children where a small knee may have fewer axial and sagittal sequences from which to select. There is also evidence that knee positioning may affect patellofemoral measurements, namely patellar height ratio and tibial tuberosity-trochlear groove distance [12, 27]. Although we could not correct for rotational differences, our institutional protocol utilizes knee flexion angles <10 degrees in the absence of other musculoskeletal deformities. Despite these limitations, we maintained excellent interobserver reliability between recorders. Ultimately, a direct comparison with adult norms will be needed to further evaluate ages at which pediatric data can reliably be interpreted using established adult cutoffs or if new pediatric cutoffs will become necessary.
Conclusion
By establishing normative pediatric data, we may now consider an age-based approach to patellofemoral evaluation. Our data verify the development of patellofemoral morphology with advancing age. We found that six of the most commonly used patellofemoral measurements in adults can be accurately reproduced regardless of age; however, there are statistically significant differences between younger and older children that must be considered. This will act as a foundation for future pediatric studies regarding early morphological changes associated with patellar instability and the effect of early intervention on such knees.
References
Merchant AC, Mercer RL, Jacobsen RH et al (1974) Roentgenographic analysis of patellofemoral congruence. J Bone Joint Surg Am 56:1391–1396
Fucentese SF, Schottle PB, Pfirrmann CW et al (2007) CT changes after trochleoplasty for symptomatic trochlear dysplasia. Knee Surg Sports Traumatol Arthrosc 15:168–174
Dejour H, Walch G, Nove-Josserand L et al (1994) Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc 2:19–26
Brattstroem H (1964) Shape of the intercondylar groove normally and in recurrent dislocation of patella. A clinical and X-ray-anatomical investigation. Acta Orthop Scand Suppl 68:61–148
Insall J, Salvati E (1971) Patella position in the normal knee joint. Radiology 101:101–104
Muellner T, Funovics M, Nikolic A et al (1998) Patellar alignment evaluated by MRI. Acta Orthop Scand 69:489–492
Kujala UM, Osterman K, Kormano M et al (1989) Patellofemoral relationships in recurrent patellar dislocation. J Bone Joint Surg (Br) 71:788–792
Wittstein JR, Bartlett EC, Easterbrook J et al (2006) Magnetic resonance imaging evaluation of patellofemoral malalignment. Arthroscopy 22:643–649
Shih YF, Bull AM, Amis AA (2004) The cartilaginous and osseous geometry of the femoral trochlear groove. Knee Surg Sports Traumatol Arthrosc 12:300–306
Van Huyssteen AL, Hendrix MR, Barnett AJ et al (2006) Cartilage-bone mismatch in the dysplastic trochlea. An MRI study. J Bone Joint Surg (Br) 88:688–691
Staubli HU, Durrenmatt U, Porcellini B et al (1999) Anatomy and surface geometry of the patellofemoral joint in the axial plane. J Bone Joint Surg (Br) 81:452–458
Miller TT, Staron RB, Feldman F (1996) Patellar height on sagittal MR imaging of the knee. AJR Am J Roentgenol 167:339–341
Pfirrmann CW, Zanetti M, Romero J et al (2000) Femoral trochlear dysplasia: MR findings. Radiology 216:858–864
Bernageau J, Goutallier D, Larde D et al (1981) L’obliquitè de la joue externe de la throclee femorale. Encyclop Med Chir 30:39–42
Carrillon Y, Abidi H, Dejour D et al (2000) Patellar instability: assessment on MR images by measuring the lateral trochlear inclination-initial experience. Radiology 216:582–585
Nietosvaara Y, Aalto K, Kallio PE (1994) Acute patellar dislocation in children: incidence and associated osteochondral fractures. J Pediatr Orthop 14:513–515
Colvin AC, West RV (2008) Patellar instability. J Bone Joint Surg Am 90:2751–2762
Dickens AJ, Morrell NT, Doering A et al (2014) Tibial tubercle-trochlear groove distance: defining normal in a pediatric population. J Bone Joint Surg Am 96:318–324
Kim HK, Shiraj S, Anton C et al (2014) The patellofemoral joint: do age and gender affect skeletal maturation of the osseous morphology in children? Pediatr Radiol 44:141–148
Charles MD, Haloman S, Chen L et al (2013) Magnetic resonance imaging–based topographical differences between control and recurrent patellofemoral instability patients. Am J Sports Med 41:374–384
Pandit S, Frampton C, Stoddart J et al (2011) Magnetic resonance imaging assessment of tibial tuberosity-trochlear groove distance: normal values for males and females. Int Orthop 35:1799–1803
Schoettle PB, Zanetti M, Seifert B et al (2006) The tibial tuberosity-trochlear groove distance; a comparative study between CT and MRI scanning. Knee 13:26–31
Alemparte J, Ekdahl M, Burnier L et al (2007) Patellofemoral evaluation with radiographs and computed tomography scans in 60 knees of asymptomatic subjects. Arthroscopy 23:170–177
Biedert RM, Bachmann M (2009) Anterior-posterior trochlear measurements of normal and dysplastic trochlea by axial magnetic resonance imaging. Knee Surg Sports Traumatol Arthrosc 17:1225–1230
Hasler RM, Gal I, Biedert RM (2014) Landmarks of the normal adult human trochlea based on axial MRI measurements: a cross-sectional study. Knee Surg Sports Traumatol Arthrosc 22:2372–2376
Ogden JA (1984) Radiology of postnatal skeletal development. X. Patella and tibial tuberosity. Skeletal Radiol 11:246–257
Yao L, Gai N, Boutin RD (2014) Axial scan orientation and the tibial tubercle-trochlear groove distance: error analysis and correction. AJR Am J Roentgenol 202:1291–1296
Conflicts of interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mundy, A., Ravindra, A., Yang, J. et al. Standardization of patellofemoral morphology in the pediatric knee. Pediatr Radiol 46, 255–262 (2016). https://doi.org/10.1007/s00247-015-3459-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-015-3459-9