Abstract
Initial experience of dual-source dual-energy (DE) lung perfusion CT in children is described. In addition to traditional identification of pulmonary emboli, the assessment of lung perfusion is technically feasible with dual-source DE CT in children with acceptable radiation dose. This article describes how to perform dual-source DE lung perfusion CT in children, including the optimization of intravenous injection method and CT dose parameters. How to produce weighted-average CT images for the assessment of pulmonary emboli and colour-coded perfusion maps for the assessment of regional lung perfusion is also detailed. Lung perfusion status can then be evaluated on perfusion maps by means of either qualitative or quantitative analysis. Potential advantages and disadvantages of this emerging CT technique compared to lung perfusion scintigraphy and cardiac MRI are discussed.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Recently, the prevalence of pulmonary embolism in children was reported to be between 14.0% and 15.5% and is higher than previously reported, as it was derived from a patient population with a high clinical suspicion in tertiary children’s hospitals [1, 2]. Early and accurate diagnosis is critical to prevent detrimental consequences of overlooked or missed pulmonary embolism, such as pulmonary arterial hypertension and right heart failure, although fatal cases are less common in children due to presumed protective mechanisms from thromboembolism [3]. For the diagnosis of pulmonary embolism, various imaging modalities have been used, including ventilation/perfusion scintigraphy, pulmonary CT angiography, MRI and catheter pulmonary angiography. For this diagnostic task, imaging modalities other than pulmonary CT angiography are limited by the following disadvantages: limited availability in urgent situations, long examination time and inferior spatial resolution in scintigraphy and MRI; frequent indeterminate results of scintigraphy; technical difficulty for young children in inhaling the aerosol in ventilation scintigraphy; and invasiveness of catheter pulmonary angiography, particularly for children. On the contrary, pulmonary CT angiography is currently used as the initial examination of choice and is considered the reference standard for the diagnosis of pulmonary embolism in adults, thanks to the introduction of multislice spiral CT technology [4]. A few studies conducted in children also proved the excellent diagnostic performance of pulmonary CT angiography using multislice spiral CT technology for the diagnosis of pulmonary embolism [1, 2].
Since the introduction of dual-source CT, the extraction of a specific material such as iodine, uric acid and xenon, with the DE scan mode and the three-material decomposition, has become technically feasible [5]. DE pulmonary CT angiography enables us to detect perfusion defects in the lung parenchyma in addition to pulmonary emboli [6–12]. This additional identification of lung perfusion defects may be useful for assessing the prognostic implication of pulmonary emboli since the pulmonary haemodynamics may be affected more by small occlusive emboli than by larger non-occlusive ones. Despite the technical improvements of CT, pulmonary CT angiography alone is still limited in detecting emboli in the subsegmental pulmonary artery in 80% of children [1]. Thus, DE pulmonary CT angiography may be helpful in overcoming this limitation. However, the technical feasibility of this emerging imaging technique has not been described in children. This article describes how to perform dual-source DE lung perfusion CT and how to assess the results in children.
Description
The institutional review board approved this study and informed consent was waived because dual-source DE pulmonary CT angiography is used routinely in the evaluation of pulmonary embolism in our hospital. Between December 2007 and October 2009, 14 children (median age, 12 years; range, 1–19 years) who were known to have, or suspected of having, pulmonary thromboembolism underwent dual-source chest CT in DE mode.
Dual-source DE lung perfusion CT
Chest CT was performed with a dual-source CT system (Somatom Definition; Siemens Healthcare, Forchheim, Germany) in DE mode (80 kVp and 140 kVp) in all children. Multislice spiral scan of the whole lung was acquired during inspiratory breath-hold in ten conscious children (71%, 10/14) and during free breathing in four sedated children. Two sets of spiral CT data were acquired with 14 × 1.2-mm collimation, 0.5 pitch, 0.33 s rotation time and a 512 × 512-pixel matrix. The duration of data acquisition and breath-holding is subject to prolongation with DE CT because only the central 14 out of 32 detector rows were used and a low pitch was used to improve image quality. Tube current for the 80 kVp scans was adjusted to four times greater than that for the 140 kVp scans to make the image noise of the CT images from the two kVp levels comparable to each other. CT dose parameters were determined on the basis of our paediatric chest protocol [13]. The volume CT dose index (CTDIvol, mGy) values were, therefore, adapted to the corresponding weight groups: 1.9 for 5.0–9.9 kg, 2.7 for 10.0–19.9 kg, 3.9 for 20.0–39.9 kg, 5.7 for 40.0–59.9 kg and 8.8 for 60.0–69.9 kg. There was a lower limit, 2.72 mGy CTDIvol, for DE scan mode due to a lower limit of 15 mAs in tube current time-product for the 140-kVp tube. Spiral scan was acquired in the caudocranial direction to reduce streak artefacts from undiluted contrast agent in the subclavian vein and superior vena cava.
To avoid less diagnostic or non-diagnostic quality of DE lung perfusion CT, one should optimize (1) the injection protocol to minimize contrast agent-induced beam-hardening artefacts and (2) the scan delay to achieve peak lung parenchymal enhancement. Iodinated contrast agent (Iomeron 400, 400 mg I/ml; Bracco Imaging SpA, Milan, Italy) was intravenously injected with a dual-head power injector via the arm vein at a maximally allowable injection rate (2.0–4.0 ml/s) depending on the placed angiocatheter size (22– to 18-gauge), followed by a saline chaser, 20–40 ml, at the same injection rate. The total volume of contrast agent was adapted to the child’s body weight at 1.0–1.5 ml/kg. To determine the scan delay of CT, a test injection was performed by using 5–10 ml of contrast agent with dynamic single-slice scans at the upper level of the left atrium (Fig. 1). A monitoring delay for the dynamic scans was set to be long, 7–10 s, to minimize radiation dose. Then, the peak enhancement time for the pulmonary vein was used for the scan delay from the beginning of the injection of contrast agent, which was variable, ranging from 13 s to 17 s. The injection time of contrast agent should be carefully selected to take full advantage of the effect of the saline chaser ameliorating streak artefacts due to undiluted contrast agent. Therefore, it was shorter than the scan delay of CT by 3–5 s that might correspond to the arrival time of a bolus to the subclavian vein and superior vena cava from the arm vein.
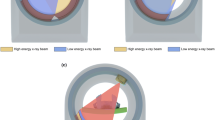
Test injection method to determine optimal scan delay of DE lung perfusion CT. a Dynamic axial CT scan is repeated every 1 s at the upper level of the left atrium, starting the scan 10 s after the intravenous administration of 10 ml of contrast agent at the same injection rate as for the DE CT scan. Then, a round region of interest is placed in the pulmonary artery (1) and pulmonary vein (2), respectively. A small amount of pleural effusion is noted with passive lung atelectasis in both thoraces. b Time-attenuation curve demonstrates dynamic enhancement patterns of the pulmonary vein. The peak enhancement time of the pulmonary artery is not used for the scan delay because it is likely to be too early for the peak enhancement time of the lung parenchyma. The time to peak is 3 s for the pulmonary vein (2). Hence, 13 s, a sum of the scan delay (10 s) of the dynamic axial CT and the time to peak (3 s) for the pulmonary vein, is chosen for the scan delay of subsequent DE CT. PA, pulmonary artery; PV pulmonary vein
CT images were reconstructed with a medium-soft convolution kernel (D30) developed for DE scan at 1.5-mm slice thickness with a 0.7-mm increment. Three sets of weighted-average images, iodine distribution maps and overlay images were generated on a commercially available workstation with the pulmonary blood volume (PBV) application class of Syngo Dual Energy (Siemens Healthcare) (Fig. 2). Weighted-average images were produced from a combination of 70% of 140 kVp images and 30% of 80 kVp images, i.e. a 0.3 weighting factor. As a result, image quality of the weighted-average images is assumed to be similar to that of single-energy 120 kVp images. Based on three-material decomposition of soft tissue, air and iodine [5], colour-coded iodine distribution maps of the lung were reconstructed. In that material decomposition, pulmonary vessels are automatically excluded from the calculation because the attenuation (Hounsfield units, HU) is >−300 HU (the default threshold for maximum value; −960 HU for minimum value). Bronchi also have no value because no iodine is present in bronchi. On the workstation, overlay images were produced mainly from a fusion of 50% of weighted-average images and 50% of colour-coded iodine distribution maps. Axial, coronal and sagittal reformatted images of those three sets were reconstructed for image analysis at 3.0 to 5.0-mm slice thickness depending on the size of the child (Fig. 2). The field of view of iodine distribution map and overlay image were restricted to 26 cm due to the smaller second detector. However, the lungs could be included in their entirety in the limited central field of view in all cases.
Normal appearances on weighted-average image, iodine distribution map and overlay image generated from dual-source DE chest CT in an 11-year-old girl with isolated left pulmonary artery stenosis (Patient 2 in Table 1). a Axial weighted-average CT image at the level of the aortic arch shows normal vascular opacification. Of note, the well-designed intravenous injection protocol results in appropriately diluted iodinated contrast agent in the superior vena cava (arrows), which is attributed to a lack of streak artefacts on the iodine distribution map (b). b Axial iodine distribution map at the same level as (a) shows homogeneous distribution of iodine that is normal. Iodine enhancement in the dependent portion of the right lung is slightly higher than other regions, which is considered a normal gravity-related perfusion gradient. c Axial overlay image at the same level as (a) shows vascular enhancement in the pulmonary artery and iodine distribution in the lung parenchyma simultaneously
Dose-length-product (DLP, mGy∙cm)-based effective dose of CT was estimated by taking age, sex and scanner-specific conversion factors into account according to the following formula:
where E (mSv) is the effective dose, Pf refers to the phantom factor, Cf (mSv/mGy·cm) is the effective dose normalized to the DLP (mGy·cm), sC is the scanner correction factor in head mode (sChead) or body mode (sCbody), aC is the age correction factor and x is a factor required for scanner correction in children [13]. The average effective CT dose was 2.6 mSv, ranging from 1.2 mSv to 5.9 mSv.
Data analysis
Diagnostic image quality
Image quality of DE lung perfusion CT, including the weighted-average image and iodine distribution map, was diagnostic in 13 of 14 children (Fig. 3). In the remaining child, image quality was slightly degraded due to beam-hardening artefacts from metallic instruments used for posterior spinal fixation (Fig. 4). As in single-energy CT, motion artefacts of a free-breathing weighted-average image were not pronounced and were comparable to that of a breath-hold study. On the contrary, motion artefacts were present around the heart and, less extensively, the diaphragm on the iodine distribution map although the extent was limited to the adjacent lung regions only. Iodine values could not be calculated in atelectasis or consolidation because the soft tissue was excluded from material decomposition in the lung PBV application software. Thus, lung perfusion in those lung parenchymal lesions could not be assessed. Registration artefacts potentially resulting from a 90° offset (83 ms) between the two kVp images were not observed on weighted-average images.
Diagnostic image quality of DE lung perfusion CT in a 10-year-old boy with acute chest pain. a Image quality of coronal weighted-average image is diagnostic with high vascular enhancement and no motion artefacts. b Image quality of coronal overlay image is also diagnostic but cardiac pulsation artefacts (red) are shown in the medial portion of both lungs. Slightly decreased iodine enhancement (blue) in the peripheral portion of both lungs is a normal finding, but decreased iodine enhancement in the left upper lobe is associated with lung parenchymal lesions. c Coronal colour-coded image produced by a “lung vessels” analysis tool shows enhanced vessels (light blue) and non-enhancing vessels (red). Nodular areas in red in the left upper lobe were presumed to be infectious lung parenchymal lesions and were completely resolved on follow-up chest radiographs
Fourteen-year-old girl who underwent posterior spinal fixation for scoliosis and was suspected of having pulmonary embolism after surgery. Image quality of axial weighted-average image (a) and iodine distribution map (b) is degraded by beam-hardening artefacts from metallic instruments in the spine. On iodine distribution map (b), iodine enhancement could not be calculated in the atelectasis. Coloured areas in the bronchi and outside the patient are artefacts
Qualitative analysis of lung perfusion
By visual assessment, DE CT demonstrated normal lung perfusion showing homogeneous iodine distribution (Fig. 2), although a slight gradient was present between nondependent and dependent portions and between central and peripheral portions of the lung. Perfusion defects, if they were present, could be easily detected because reduction of iodine enhancement was much greater than the slight geographic gradient in the normal lung (Fig. 5). True perfusion defects should be differentiated from motion artefacts and beam-hardening artefacts. For this discrimination, assessing the location and shape of areas with low iodine enhancement on multiplanar reformatted images seems to be helpful. Regional lung perfusion on the iodine distribution map can be correlated with pulmonary emboli on weighted-average images by means of side-by-side comparison or overlay images. On the other hand, global mild reduction of lung perfusion may not be easy to recognize (Fig. 6).
Six-year-old girl with leukaemia (Patient 3 in Table 1). Dual-source DE contrast-enhanced chest CT was performed to evaluate reduced flow in the left pulmonary artery suspected at echocardiography. a Axial iodine distribution map shows decreased regional iodine-related enhancement in the medial segment of the right middle lobe (arrows). The lesion should be carefully interpreted as to whether the identified perfusion defect is true because paracardiac areas such as the right middle lobe and the lingular division of the left upper lobe are subject to motion and streak artefacts on DE CT. b Right posterior oblique perfusion scintigraphy shows a perfusion defect (arrow) in the right middle lobe that corresponds to the lesion on CT. The lesion was a ventilation/perfusion matched defect indicating a low probability of pulmonary embolism because ventilation scintigraphy (not shown) also showed a defect in the same location
A 13-year-old girl with lymphoma (Patient 4). The girl underwent dual-source DE contrast-enhanced chest CT because pulmonary emboli related to the central venous catheter were detected on the previous chest CT. a Coronal weighted-average CT image with a bone window setting shows a non-occlusive, calcified embolus mimicking a tram track in the central right pulmonary artery. Distal branches of the right pulmonary artery are opacified normally. The severely dilated inferior vena cava (arrows) is noted. b Axial iodine distribution map at the lower thorax demonstrates that the iodine-related enhancement, 35.4 HU, of the right lung is diffusely lower than that, 42.7 HU, of the left lung. c Graph shows the distribution of the measured contrast enhancement on iodine distribution map against the slice position along the z-axis (first slice, lung apex; last slice, diaphragm) of each lung demonstrates a lower level of iodine-related enhancement of the right lung throughout the z-axis. The degree of the measured contrast enhancement drops rapidly near the diaphragm. d Graph shows the distribution of the measured lung area on CT against the slice position along the z-axis (first slice, lung apex; last slice, diaphragm) of each lung demonstrates that the right lung area is largely greater than the left lung area in contrast to a lower level of iodine-related enhancement of the right lung (c). Colour-coded regional blood volume map of the lung (e) and time-intensity curve (f) produced from three-dimensional contrast-enhanced time-resolved MR angiographic data confirmed that the global mild reduction of right lung perfusion depicted with DE lung perfusion CT was true
Quantitative analysis of lung perfusion
Because normal lung parenchymal iodine enhancement on DE CT is substantially influenced by the intravenous injection protocol of contrast agent, including iodine delivery rate and scan delay as well as the haemodynamic condition of the patient, it appears almost impossible to define normal data such as mean, standard deviation, minimal value and maximal value. Regional measurement of iodine enhancement is the most commonly used and relatively easy method of quantitative analysis for the evaluation of regional lung perfusion. It should be noted that the measured value means the degree of iodine enhancement in HU was not affected by tissue density. The measured iodine enhancement on DE CT was lower in the perfusion defects (<35.5 HU) than in the normal lung (41.1–43.0 HU). A time-consuming quantitative method places regions of interest slice-by-slice to include the right lung and left lung separately on DE CT yielding lung parenchymal enhancement and lung volume percentages of the right lung. The measured iodine enhancement and area of the right lung can be plotted against the slice number (Fig. 6). On the plot, a subtle finding of global mild reduction of right lung perfusion due to a non-occlusive embolus in the right branch pulmonary artery could be demonstrated (Fig. 6). Lung perfusion on DE CT may be defined as a product of lung parenchymal enhancement and lung volume. The normal right lung carries approximately 55% of the pulmonary blood flow and volume [14]. This is because the main mass of the heart is slightly deviated toward the left in normal subjects. Perfusion percentages of the right lung on DE CT were not greatly different from those on perfusion scintigraphy and phase-contrast MRI in the small number of children (Table 1).
Two other analysis methods are available: another DE application class for “lung vessels” and an automatic presentation of regional lung perfusion percentages. The tool for “lung vessels” was developed to discriminate non-enhancing subsegmental pulmonary arteries from enhancing ones by using DE iodine extraction data (Fig. 2), which has been regarded as a challenging task on conventional pulmonary CT angiography. From automatic lung segmentation, regional lung perfusion percentages (right lung vs. left lung, upper vs. middle vs. lower lung zones of each lung) similar to those of lung perfusion scintigraphy can be automatically generated. However, clinical validation of these two methods remains to be determined.
Discussion
It is feasible to evaluate regional lung perfusion with dual-source DE lung perfusion CT in children. For the evaluation of regional lung perfusion, both qualitative and quantitative methods are described. Other investigators found good agreement between DE CT and scintigraphy for the assessment of lung perfusion [6]. However, the two imaging modalities were compared qualitatively in the previous study. In a subset of the patient population in this study, the right lung perfusion percentage quantified with DE lung perfusion CT showed small differences from those with perfusion scintigraphy and phase-contrast MRI. On the other hand, standards of reference used in other studies dealing with DE lung perfusion CT were usually subjective: independent third reading of CT [7], CT reading by two radiologists in consensus [8] and pathologic findings [12]. In a study [7], iodine-related enhancement was measured in the lung parenchyma on DE lung perfusion CT. The mean value measured in the normal lung was 56 HU (range 20–79 HU) and in the perfusion defects 18 HU (range 9–19 HU) [7]. In this study, the values were 41.1–43.0 HU in the normal lung and <35.5 HU in the perfusion defects. The threshold distinguishing normal lung from the perfusion defects seems to be quite different between the two studies, approximately 20 HU in the former and approximately 40 HU in the latter. This discrepancy may be attributable to the study population having different types of pulmonary emboli and injection protocol of contrast agent. Unlike contrast-enhanced time-resolved MR angiography, only one scan is acquired for DE lung perfusion CT. Therefore, the use of meticulously optimized injection protocol is critical for the quantitative evaluation of regional lung perfusion. Because the DE CT technique evaluated in this study is vulnerable to beam-hardening artefact, the injection protocol should be tailored not only to minimize streak artefacts from undiluted contrast agent in the central thoracic veins and right cardiac chambers, but also to achieve a high degree of contrast enhancement in the pulmonary arteries and lungs. For the same reason, dual-source DE lung perfusion CT is not recommended for patients with metallic devices in the scan range.
In most adult studies, a bolus tracking method was used to determine the optimal scan delay of DE CT [6–12]. On the contrary, a test injection method was used in this study to increase the chance of achieving peak enhancement of the lung parenchyma, indispensable for DE lung perfusion CT. As used in this study, a weight-adapted injection protocol is generally preferred to a fixed amount of contrast agent in both adults and children, particularly for the quantitative evaluation of iodine enhancement on DE CT. Caudocranial scan direction was used in this study to minimize streak artefacts from undiluted contrast agent in the superior vena cava and subclavian veins as used in most adult studies [6, 7, 9]. A high degree of enhancement of an input vessel, the main pulmonary artery, is also essential. In this study, the attenuation measured in the main pulmonary artery ranged from 251 HU to 432 HU. In general, vascular opacification >250 HU is regarded as appropriate in contrast-enhanced chest CT. The CT densities measured in this study are lower than those (range, 315–594 HU) in an adult study [7], probably due to a difference in the injection rate: the injection rate is much lower (1.0–3.0 ml/s) in children than that in adults (4.0–5.0 ml/s). Basically, greater vascular enhancement is achieved at a higher injection rate. A normalization of measured iodine enhancement, for instance, by using the degree of contrast enhancement in the pulmonary artery as an input function, may be necessary but may not be easy because DE lung perfusion CT is not a multi-phase study but a single-phase study.
For the assessment of lung perfusion, a few noninvasive imaging methods including perfusion scintigraphy [15] and MRI [16, 17] have been used. In the diagnosis of acute pulmonary embolism, ventilation/perfusion single photon emission CT showed higher sensitivity and lower specificity in comparison with multislice pulmonary CT angiography [15]. Because of the low specificity of scintigraphy, indeterminate studies are frequent, up to approximately three-quarters of the adult patients. Another disadvantage of scintigraphy is difficulty in reading the results in patients with congenital heart disease, particularly when right-to-left shunts and high haematocrit levels are present. MRI techniques for evaluating regional lung perfusion have evolved and appear promising, including contrast-enhanced, time-resolved MR angiography [16] and noncontrast MR angiography based on arterial spin labeling techniques [17]. Low spatial resolution is a limitation of both perfusion scintigraphy and MRI. In contrast, CT has inherent merit in evaluating the lung parenchyma due to high tissue-air contrast and high spatial resolution. Thus, associated lung parenchymal lesions can be easily and accurately assessed in patients with known or suspected pulmonary embolism. Before the introduction of DE CT, the evaluation of lung perfusion with CT has been regarded as difficult. Few studies using single-energy CT were performed with dynamic multisection electron beam CT in humans [18] and with conventional CT using a subtraction technique between pre-contrast and contrast-enhanced CT examinations during a single breath-hold in an animal study [19]. However, both are limited by increased radiation exposure to patients and technical difficulties. Several studies in adults have suggested that DE CT has an additional diagnostic value in the diagnosis of pulmonary embolism by providing prognostic significance of pulmonary emboli [6–12]. In a study that correlated DE CT findings with cardiovascular measurements, right cardiac function might be reflected by the extent of lung perfusion but not by the extent of pulmonary emboli [10]. These results underscore the functional significance of lung perfusion defects resulting from small occlusive emboli that are difficult to detect with the current spatial resolution of CT. Another study also showed that perfusion defect score quantified on DE CT had good correlation with right ventricular/left ventricular diameter ratio and CT angiographic obstruction score [11]. The detection of subsegmental pulmonary emboli is more difficult in children than in adults, probably due to the small size of the vessel and the blurring effect of respiratory motion [1]. Therefore, the detection of perfusion defects in addition to pulmonary emboli with DE lung perfusion CT may have greater clinical implications for children than for adults.
Radiation dose of DE lung perfusion CT should be acceptably low in order to become a clinically routine procedure. In this study, the average effective dose of dual-source DE lung perfusion CT was 2.6 mSv, ranging from 1.2 mSv to 5.9 mSv. The CT dose of this study is comparable to that (2–5 mSv) of a paediatric study [2] and lower than that (average, 10.5 mSv; range 2.3–26 mSv) of another paediatric study [1] using single-source, single-energy, multislice pulmonary CT angiography. Radiation dose, ranging from 3.1 mSv to 4.7 mSv, of dual-source DE lung perfusion CT in adults is also dose-neutral.
Dual-source DE lung perfusion CT has several potential limitations. Strictly speaking, iodine enhancement evaluated with DE CT is not true dynamic lung perfusion information because the CT scan is obtained at only a single time point. However, regional lung perfusion status depicted with this CT technique may provide additional clinical value that is not obtained with conventional single-energy CT scan. A small field of view, 26 cm, is one of the limitations of DE scan mode related to the second, smaller detector array. As a result, iodine distribution maps outside the 26-cm field of view could not be evaluated in 68% [8], 72% [9] and 76% [10] of adult patients. This limitation may be less frequent in Asians and children. In fact, there was no such case in this study. Streak artefacts from undiluted contrast agent and beam-hardening artefact from the shoulder and metallic devices (Fig. 3) may make the evaluation difficult. Therefore, single-energy pulmonary CT angiography would be preferred in order to obtain diagnostic image quality when metallic devices are present in the thorax. In addition, motion artefacts from the heart and diaphragm commonly occur in adjacent lung areas on the iodine distribution map. However, the artefacts may be largely differentiated from true perfusion defects on the basis of specific locations and their shape. Longer scan duration of DE CT, for instance, 12 s from 5 s [8], may make breath-holding difficult in children and dyspnoeic adult patients. Some of these limitations, such as the smaller field of view, a relatively low signal-to-noise ratio particularly in large patients, longer scan time and a substantial overlap between the two energy levels, will be overcome by the second-generation dual-source CT system [20]. Future studies such as DE ventilation and perfusion CT in one examination and lobar segmentation of quantitative CT results are expected to further improve not only patient care, but also our insight into the pathophysiology of pulmonary embolism. In fact, xenon ventilation CT was recently validated in the functional evaluation of the lung in healthy volunteers and patients [21, 22].
In conclusion, the evaluation of regional lung perfusion in addition to identification of pulmonary emboli with dual-source DE CT is technically feasible in children with acceptable radiation dose. Thus, this emerging technique is ready for clinical validation.
References
Kritsaneepaiboon S, Lee EY, Zurakowski D et al (2009) MDCT pulmonary angiography evaluation of pulmonary embolism in children. AJR 192:1246–1252
Victoria T, Mong A, Altes T et al (2009) Evaluation of pulmonary embolism in a pediatric population with high clinical suspicion. Pediatr Radiol 39:35–41
Babyn PS, Gahunia HK, Massicotte P (2005) Pulmonary thromboembolism in children. Pediatr Radiol 35:258–274
Remy-Jardin M, Pistolesi M, Goodman LR et al (2007) Management of suspected acute pulmonary embolism in the era of CT angiography: a statement from the Fleischner Society. Radiology 245:315–329
Johnson TR, Krauss B, Sedlmair M et al (2007) Material differentiation by dual energy CT: initial experience. Eur Radiol 17:1510–1517
Thieme SF, Becker CR, Hacker M et al (2008) Dual energy CT for the assessment of lung perfusion—correlation to scintigraphy. Eur J Radiol 68:369–374
Fink C, Johnson TR, Michaely HJ et al (2008) Dual-energy CT angiography of the lung in patients with suspected pulmonary embolism: initial results. Rofo 180:879–883
Pontana F, Faivre JB, Remy-Jardin M et al (2008) Lung perfusion with dual-energy multidetector-row CT (MDCT): feasibility for the evaluation of acute pulmonary embolism in 117 consecutive patients. Acad Radiol 15:1494–1504
Thieme SF, Johnson TR, Lee C et al (2009) Dual-energy CT for the assessment of contrast material distribution in the pulmonary parenchyma. AJR 193:144–149
Zhang LJ, Yang GF, Zhao YE et al (2009) Detection of pulmonary embolism using dual-energy computed tomography and correlation with cardiovascular measurements: a preliminary study. Acta Radiol 50:892–901
Chae EJ, Seo JB, Jang YM et al (2010) Dual-energy CT for assessment of the severity of acute pulmonary embolism: pulmonary perfusion defect score compared with CT angiographic obstruction score and right ventricular/left ventricular diameter ratio. AJR 194:604–610
Zhang LJ, Zhao YE, Wu SY et al (2009) Pulmonary embolism detection with dual-energy CT: experimental study of dual-source CT in rabbits. Radiology 252:61–70
Yang DH, Goo HW (2008) Pediatric 16-slice CT protocols: radiation dose and image quality. J Korean Radiol Soc 59:333–347
Bryan AC, Bentivoglio LG, Beerel F et al (1964) Factors affecting regional distribution of ventilation and perfusion in the lung. J Appl Physiol 19:395–402
Reinartz P, Windberger JE, Schaefer W et al (2004) Tomographic imaging in the diagnosis of pulmonary embolism: a comparison between V/Q lung scintigraphy in SPECT technique and multislice spiral CT. J Nucl Med 45:1501–1508
Goo HW, Yang DH, Park IS et al (2007) Time-resolved three-dimensional contrast-enhanced magnetic resonance angiography in patients who have undergone a Fontan operation or bidirectional cavopulmonary connection: initial experience. J Magn Reson Imaging 25:727–736
Mai VM, Berr SS (1999) MR perfusion imaging of pulmonary parenchyma using pulsed arterial spin labeling techniques: FAIRER and FAIR. J Magn Reson Imaging 9:483–487
Schoepf UJ, Bruening R, Konschitzky H et al (2000) Pulmonary embolism: comprehensive diagnosis by using electron-beam CT for detection of emboli and assessment of pulmonary blood flow. Radiology 217:693–700
Wildberger JE, Klotz E, Ditt H et al (2005) Multislice computed tomography perfusion imaging for visualization of acute pulmonary embolism: animal experience. Eur Radiol 15:1378–1386
Petersilka M, Bruder H, Krauss B et al (2008) Technical principles of dual source CT. Eur J Radiol 68:362–368
Chae EJ, Seo JB, Goo HW et al (2008) Xenon ventilation CT with a dual-energy technique of dual-source CT: initial experience. Radiology 248:615–624
Goo HW, Chae EJ, Seo JB et al (2008) Xenon ventilation CT using a dual-source dual-energy technique: dynamic ventilation abnormality in a child with bronchial atresia. Pediatr Radiol 38:1113–1116
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Goo, H.W. Initial experience of dual-energy lung perfusion CT using a dual-source CT system in children. Pediatr Radiol 40, 1536–1544 (2010). https://doi.org/10.1007/s00247-010-1759-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-010-1759-7