Abstract
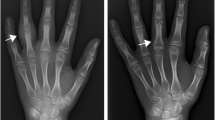
Juvenile idiopathic arthritis (JIA) represents a group of heterogeneous diseases characterized by a chronic inflammatory process primarily targeting the synovial membrane. A persistent synovitis is associated with an increased risk of osteocartilaginous damage.
With the advent of effective structure-modifying treatment for JIA, it may be possible to significantly reduce or even completely prevent structural damage and associated functional disability. The trend towards early suppression of inflammation, in order to prevent erosive disease, shifts the emphasis away from conventional radiographic detectable structural damage to the slightest traces of early joint damage, and drives the need for alternative imaging techniques more sensitive in detecting early signs of disease activity and damage. In this regard MRI and US are playing an increasing role in the evaluation of arthritic joints.
This article will review the key aspects of the current status and recent important advances of imaging techniques available to investigate the child with rheumatic disease, briefly discussing conventional radiography, and particularly focusing on MRI and US. In this era of advancing imaging technology, knowledge of the relative values of available imaging techniques is necessary to optimize the management of children with JIA.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Juvenile idiopathic arthritis (JIA) is the most common chronic rheumatic disease of childhood and an important cause of short-term and long-term disability. Studies in developed countries have reported a prevalence that ranges between 16 and 150 per 100,000 [1]. The affected joints develop synovial proliferation and infiltration by inflammatory cells, with subsequent increased secretion of synovial fluid and pannus formation. Persistent synovial inflammation may ultimately lead to articular cartilage and bone damage that are responsible for most disability in JIA [2, 3]. JIA is not a single disease, but a term that encompasses all forms of arthritis with onset in patients <16 years old, lasting more than 6 weeks and of unknown origin. The term represents, therefore, a diagnosis of exclusion and a wide range of differential diagnoses, many of which have recognisable features on imaging (Table 1) [4].
A number of classification systems have been developed over the years, the most recent being that proposed by the International League of Association for Rheumatology (ILAR) (Table 2) that aims to enable identification of homogeneous groups of children suitable for aetiopathogenetic studies [5].
Imaging in JIA is crucial for diagnosis of the disease, assessing its severity and prognosis, monitoring disease progression and treatment response, and evaluating complications associated with the disease or its therapy. The recent introduction of effective structure-modifying treatments has created new demands on imaging for more sensitive methods of predicting and monitoring treatment effect [6, 7].
This article will review key aspects of the current status and recent important advances in imaging in JIA, briefly discussing conventional radiography, and particularly focusing on MRI and US. The value and limitations of these imaging modalities and an overview of future imaging scenarios in JIA will be also reported.
Advances in radiography
Up to the present day, conventional radiography (CR) has been the mainstay of imaging evaluation in JIA. The main radiological features in JIA are reported in Table 3, together with the advantages and drawbacks of this technique. The recent advances in radiographs in JIA can be summarized into two broad categories: technical advances and advances in the standardization of radiographic methods.
New computed radiography and digital/direct radiography, with electronic display and interpretation, have largely replaced films/screen radiography. Clinical studies in patients with rheumatoid arthritis (RA) have demonstrated that the image quality of computed radiography is at least as good as screen-film; small and early erosions, in fact, can be seen equally well with the digital technique as compared with the conventional film-screen techniques [8, 9]. These results support diffusion of digital technique into clinical practice, with advantages also in image distribution, storage, and cost. Furthermore Ludwig K et al. [10], in a recent experimental study, have clearly demonstrated that a digital flat-panel detector offers a diagnostic performance superior to screen films, even in the detection of very small bone erosions (diameter starting from 0.5 mm, with a depth of 0.5 mm) at clinical exposure settings. According to the authors’ conclusions, using the flat-panel system, the exposure dose can be reduced by 50% to obtain a diagnostic performance comparable with a speed class 200 screen-film.
Modern therapeutic strategies have created a growing need for a reliable radiographic assessment standard for evaluation of the potential value of these drugs in preventing structural joint damage in JIA. Assessment of structural damage is a key outcome endpoint in treatment efficacy studies and is now required by the US Food and Drug administration as a measure of disease progression in clinical trials of potential disease modifying antirheumatic drugs (DMARDs) in patients with RA [11]. The imaging evaluation of articular disorders in children differs from that in adults in several important aspects. Due to the peculiarities of the growing skeleton (the thickness of the articular cartilage varies among joints of children of different ages, ossification is incomplete, the presence of bone growth abnormalities etc.), the radiographic assessment of structural damage in JIA is challenging, and to apply adult-designed radiographic scoring systems to evaluate the progression of JIA may not be feasible.
In recent years there has been a great effort to devise paediatric-targeted radiographic scoring systems (Table 4); some of these measures have undergone a thorough validation process and have proved to be reliable and valid for assessment of radiographic progression in children with JIA. This has led to the suggestion that the time has come to include quantitative measure of radiographic damage in therapeutic trials in JIA, as recently proposed by Ravelli A [12].
The trend towards early suppression of inflammation to prevent erosive disease shifts the emphasis away from conventional radiography-detectable structural damage to early stage manifestations of the disease, such as inflammatory changes in the soft tissues, and drives the need for alternative imaging techniques that are more sensitive in detecting inflammatory processes, as well as the slightest traces of erosive joint damage. In this regard MRI and US are playing an increasing role in the evaluation of arthritic joints.
Advances in MRI
MRI provides multiplanar tomographic imaging with unprecedented soft-tissue contrast and allows assessment of all the joint structures involved in JIA (Table 5).
The knowledge of the pathological processes and clinical issues that have to be adequately imaged in JIA is essential for the choice of the variety of pulse sequences that are available for assessment of different joint components. Choosing the best protocol for a specific indication is crucial in order to maximize cost-effectiveness and optimize diagnostic information of MRI.
In the last decade there has been a great deal of effort by the OMERACT (outcome measures in rheumatology clinical trials) MRI-RA group aiming to quantify the large amount of information produced by MRI, and culminating in the development and validation of a semi-quantitative scoring system for the assessment of inflammatory and damage abnormalities in RA. Consensus MRI definitions of important joint pathologies and a core set of basic MRI sequences were also suggested [13]. Despite the large number of studies available in adults, the experience on the use of MRI in the assessment of JIA is limited. So far pilot MRI grading scores for the assessment of hip and knee disease activity and damage of JIA patients have been proposed [14–16]. However, these scales have not been validated and have been tested on a limited number of patients. The lack of validated MRI scales targeted to children and standardized MRI protocols, together with the heterogeneity in the quality of the methodology used, have strongly affected the results of a recent systematic review of the literature, according to which the quality of reporting of methods in studies on the MRI assessment of JIA is heterogeneous and fair overall [17, 18]. Furthermore, as outlined by the authors, long-term studies on MRI are lacking, therefore it is difficult to make treatment recommendations on MRI findings alone, as the long-term significance of these abnormalities is still unclear.
Notwithstanding and being aware of these limitations, we report below the more recent advances in MRI assessment of pathological findings in JIA and the way how they have changed our view of the disease.
Advances in MR imaging of synovial inflammation
MRI is the most sensitive imaging modality available for the detection of ongoing synovial inflammation, the primary target abnormality in JIA. Contrast-enhanced MRI allows a reliable differentiation of pannus from joint effusion (Figs. 1 and 2), an accurate differentiation of the active destructive hypervascular pannus from the inactive fibrotic pannus, and is able to show persistent synovitis in subclinical patients [14, 19, 20]. Of note in children with oligoarticular JIA, imaging of clinically unaffected joints has suggested that subclinical MRI-observed features of arthritis may predict extension of arthritis [21].
Sagittal MR images of the knee in a 5-year-old girl with JIA. The fat suppressed (FS) T2-weighted fast spin-echo (FSE) sequence (a) and the contrast-enhanced FS T1-weighted sequence (b) show a large rim-enhancing joint effusion with thickened synovial margins, compatible with synovitis. The gadolinium-enhanced T1-W sequence (b) better differentiates fluid (*) and synovium (arrowhead). The radially arrayed enhancement of the articular cartilage of the distal femur epiphysis following gadolinium administration represents prominent penetrating vessels
As the goal of new treatment is to obtain total suppression of joint inflammation to prevent erosive damage, future outcome measures in both clinical trials and clinical practice, should comprise sensitive and robust measures of inflammation. Computerized measurements of synovial volumes (Fig. 3) have been found to be useful for the evaluation of disease activity and responsiveness to treatment, as well as in predicting progressive joint destruction in RA [22–26]. In line with the results of studies in RA, Graham et al. [27] demonstrated the feasibility of MRI synovial volume measurement as an objective, quantitative method to assess disease activity in children with JIA. Synovial volume, obtained using a semi-automated segmentation program from the hands and wrists, correlated well with local clinical signs of inflammation and with the total number of active joints, arguing for the utility of the wrist as a surrogate marker for total burden of synovitis in JIA. Of note Gylys-Morin et al. [28] showed that synovial volume had greater sensitivity (97%) than maximal synovial thickness (77%) in distinguishing clinical synovitis. Finally it has been shown that a decrease in pannus volume and enhancement in the hips and knees of JIA patients, correlated well with favourable clinical outcome [19]. In addition to volume measurement, the technique of dynamic contrast-enhanced MRI (DCE-MRI) provides a quantitative assessment of inflammation based on the analysis of the time course of signal changes following gadolinium injection. The rate of enhancement of the synovial compartment is mainly determined by the local tissue vascularity and by the capillary permeability, both of which are supposed to closely mirror the degree of inflammatory activity. DCE-MRI has been shown to be a sensitive and accurate method for estimating synovitis monitoring response to therapy, as well as for predicting future bone damage in patients with RA [29–34].
Coronal FS gradient-echo (GRE) contrast-enhanced 3-D T1-W sequence of a wrist in a child with JIA. The results of synovial segmentation process for the evaluation of total volume are reported in a single coronal slice, as an example. Computerized measurements of synovial volume may be obtained either by manual (red selection) computer-assisted outlining base on visual analysis of the images (a) or by semiautomatic (green selection) computerizing counting of pixels fulfilling specific criteria (b)
In accordance with the studies performed in adults, Malattia et al. [35] recently demonstrated that DCE-MRI is a reliable and accurate tool for quantifying the degree of synovial inflammation in JIA, especially in patients with wrist arthritis.
Workie et al. [36] have proposed the use pharmacokinetic modelling to quantitatively analyze dynamic synovial enhancement of the knee of children with JIA. Quantification of DCE-MRI data, by means of pharmacokinetic models, aims to calculate absolute measures that are directly related to tissue physiology such as vessel permeability. These absolute measures lend themselves well to longitudinal studies, as confirmed by the same authors in a subsequent study, in which it was shown that quantitative DCE-MRI (based on pharmacokinetic modelling) may be used as an objective follow-up measure of therapeutic efficacy in JIA; of note in the same study, improvement in synovial volume appeared to lag behind dynamic parameters [37].
The use of fully automated voxel-by-voxel analysis of signal intensity versus time curves, extracted from MRI dynamic slices, has been recently demonstrated to overcome the shortcomings of the region-of-interest (ROI) approach (sampling error and inter-user variability) and provide a truly objective overview of the tissue behaviour in the whole imaged area in patients with RA [38]. Through the use of a computer-assisted detection (CAD) programs, dynamic parameters are estimating for each voxel and presented in a form of parametric colour maps, providing an advanced visual aid for assessment of the spread and magnitude of the inflammation in the affected joint.
How has MRI changed our view of JIA?
-
Synovitis is the primary target of the disease
-
Synovitis is coupled with damage
-
Patients in clinical remission may have persistent synovitis
Advances in MR imaging of bone marrow oedema
MRI is the only technique able to visualize bone marrow oedema (BME) (Fig. 4), one of the most intriguing MRI features in inflammatory chronic arthritis. Longitudinal studies, in fact, have demonstrated that BME is a key predictor of erosive joint damage in patients with RA [39, 40]. Recent studies of bone histology from joint replacement specimens in RA revealed that regions of MRI BME contain an inflammatory cellular infiltrate that is in close apposition to activated osteoclasts, implying cross-talk and a possible mechanism to explain the development of erosions [41]. The prognostic value of BME in JIA has not yet been established, even though significant work in the adult field suggests that exploration of this area would be fruitful.
How has MRI changed our view of JIA?
-
Bone erosions and BME are intimately linked from the pathophysiological perspective
-
If the prognostic value of BME would be demonstrated even in JIA, BME should be regarded as a red flag for treating physicians and active management with powerful anti-erosive medications should be considered
Advances in MR imaging of cartilage
Another unique strength of MRI is its ability to directly visualize articular cartilage. Direct imaging of this tissue is more specific than radiographic joint space width and tomography provides greater anatomical coverage of the joint surface than does projection. With the use of dedicated sequences it is possible to accurately assess signs of cartilaginous damage, such as thinning, erosions and deep cartilage loss in JIA patients, and to discriminate different types of cartilage (articular, epiphyseal, and physeal) at distinct stages of development of growing joints (Fig. 5) [19, 42, 43]. The administration of contrast medium was found to be useful for the characterization of cartilage thickness and erosions as well as the pattern of enhancement (peculiar, striated, or linear) of the cartilaginous epiphyses in JIA patients [16, 44, 45]. Newer pulse sequences such as ultra-short TE sequences, driven equilibrium Fourier transform (DEFT) imaging, and steady-state free precession (SSFP) sequences appear promising in the detection of subtle surface irregularities and tiny focal defects of the articular cartilage [46–49]. In addition, sophisticated analysis of 3-D image data can provide articular surface contour mapping, 3-D rendering and volumetric quantification of articular cartilage that can be used to evaluate the progression and response to treatment in patients with chronic arthritis. This technique may be useful for monitoring changes in cartilage volume over time in JIA patients. However further studies are needed in this field in the paediatric population, and measurements correlating normal articular cartilage volume with age have to be developed.
Coronal image of the knee in a healthy 5-year-old boy obtained with a balanced turbo field echo (BTFE) FS sequence for cartilage evaluation. In addition to high image SNR, cartilage imaging demands contrast between cartilage and structures such as synovial fluid and bone. In this example at the distal end of the femur the central ossified epiphysis (*) is of low signal intensity. The epiphysis is surrounded by high-to-intermediate signal intensity growth cartilage. Along the joint margins the articular cartilage is of slightly high signal intensity and can be differentiated from growth cartilage (arrows). Note the good contrast between articular cartilage (arrows) and synovial fluid (arrowheads)
Of particular interest Kight AC et al. [50] recently suggested the role of T2 relaxation time properties in measuring the mobility of cartilage water that is sensitive to the integrity of collagen in the extracellular matrix. The finding of an increased average T2 relaxation time of the distal femoral weight-bearing cartilage in patients with JIA, compared with sex- and age-matched healthy control subjects, suggests that T2 relaxation time maps may reflect cartilage microstructure differences that occur in JIA. Correlations between the transverse relaxation rate and collagen concentrations in the cartilage matrix have been previously demonstrated in a study in engineered cartilage tissue [51]. These specialized T2-mapping sequences, allowing an assessment of the biochemical and biophysical changes in the extracellular cartilage, and providing information about very early cartilage damage (before morphologic changes can be qualitatively detected with conventional imaging methods), represent a powerful method of monitoring disease progression with the long-term potential to guide therapy.
Furthermore, once translational studies on new functional MRI techniques are performed, new insights into the biological pathways of cartilage turnover will improve our understanding of the physiopathogenesis of JIA.
How has MRI changed our view of JIA?
-
Quantitative imaging may potentially provide information beyond morphological changes in articular cartilage, with regard to early cartilage damage
-
Cartilage matrix changes can be detected at stages when damage to the cartilage is still reversible and may be treated
-
Research in the field of composition of the cartilage matrix is driven by the technological developments and may provide pathophysiologic information relevant to disease progression
Advances in MR imaging of bone erosion
Early detection of bone erosions and subchondral changes, and aggressive control of the disease is of outstanding value in decreasing the chance of further disability. Consistent with the results of previous studies in RA patients Malattia C et al. [52] in a pilot multi-imaging study, demonstrated that MRI was the most sensitive imaging modality for detection of bone erosions in the wrist of patients with JIA, revealing more than twice as many erosions as radiography and US [53–57]. The increased accuracy of MRI in detecting erosive changes was much more evident in the group of patients with shorter disease duration. All patients with shortstanding disease showed minor erosive changes revealed by MRI. An early concern that increased sensitivity of MRI may be at the cost of reduced specificity and that MRI erosions were “not real” has now largely been debunked by comparison with the 3-D radiographic technique of CT scanning [58, 59].
Studies on adults with RA have demonstrated the significant prognostic value of MRI detectable structural damage with respect to long-term radiographic erosive damage [57, 60]. The greater sensitivity of MRI to disclose incipient destructive changes could be leveraged to select patients for more aggressive therapy and to monitor treatment response. Predicting prognosis in children with newly diagnosed JIA is of key importance in order to tailor treatment to the risk of disability. However, before using MRI in guiding therapeutic decision, further longitudinal studies are needed to determine the real prognostic value of MRI detectable bone lesions.
Less work has been done looking at computerized measurements of erosion volume on MRI compared with synovial volume; this most likely reflects the difficulties in estimating the proximal bone outline prior to erosion [24]. Computerized software advances should improve automation of the segmentation process.
How has MRI changed our view of JIA?
-
Bone erosion is common in the early course of the disease
-
MRI could be helpful to identify patients at increased risk of developing erosive disease and who will benefit from more aggressive treatment at an early stage
Advances in US
The use of US and colour Doppler continues to increase as resolution of the equipment improves; in fact the visualization of any intra-articular structures is significantly improved by the use of high frequency (12–18 MHz) linear probes.
The severity of joint involvement may be judged sonographically by parameters such as the size of the effusion, synovial thickening, cartilage thinning and bone erosions. Colour and power Doppler facilitate detection of hyperaemia and vascular abnormalities (Table 6) [61]. US can also be used to assess tenosynovitis and to guide joint aspiration or injection.
However, the major limit of US (joint accessibility) limits its applicability in “difficult joints” such as the temporo-mandibular joint (TMJ), sacroiliac joints etc. In a recent report, Muller et al. [62] concluded that US is not able to reliably exclude active TMJ arthritis and that MRI of the TMJs should be performed in children with JIA.
Synovial thickening and effusion
Sonography is more sensitive than plain radiography or clinical examination in the detection of effusion, synovial thickening and synovial cysts [16, 19]. Recent studies in children with JIA have shown that clinical examination may underestimate significant joint inflammation when compared with US, especially in the small joints of the hands and feet [63, 64]. Furthermore inflammatory involvement of the hip, shoulder and elbow is more frequently accurately detected by US compared with clinical examination (Fig. 6).
a Longitudinal US scan over the dorsal aspect of the wrist shows abnormal hypoechoic synovial tissue at the level of the dorsal recess of the intercarpal joint. Colour Doppler gives an indication of the degree of synovial vascularity. b US scan of the peroneal tendons obtained transversely to their long axis at the lateral aspect of the ankle shows hypoechoic thickened tissue (arrows) within the tendon sheath that is indicative of mild tenosynovitis. c Transverse scan over the dorsal aspect of the wrist in a child with JIA shows evidence of a focal discontinuity of the bone surface of the capitate (it is considered an erosion if it is confirmed in two perpendicular planes). d Longitudinal scan of the suprapatellar recess of the knee shows presence of effusion and synovial hypertrophy
The issue of US detectable subclinical synovitis may be particularly relevant in JIA. In the current ILAR classification, children with JIA are defined as having oligoarthritis or polyarthritis on the basis of the number of affected joints. The presence of active disease in a minimum of five joints is necessary for the diagnosis of polyarticular JIA, as well as being a prerequisite for patient inclusion in clinical trials of second-line or biologic agents [6, 65, 66]. Identification of subclinical disease may change patient classification and potentially alert the treating physicians towards more aggressive treatment and close monitoring of the patient.
It is well established that serial US may supplement clinical assessment in monitoring disease activity and in evaluating response to therapy, especially in hip synovitis. Eich et al. [45] in fact, demonstrated that US is a useful tool to assess effusion and pannus after intra-articular steroid injection in a cohort of JIA patients with hip and knee active arthritis. In this regard, colour Doppler provides an indication of the degree of synovial hypertrophy and assessment of its vascularity may be particularly useful (Fig. 6). In addition, resistive indices and fraction of colour pixels have been proposed as quantitative measurements of blood flow [67, 68].
Strunk J et al. [69] in a recent study compared 3-D power Doppler US (3-D PDUS) with contrast-enhanced MRI in their ability to visualize synovial vascularity in inflamed wrists of patients with RA. The analyses of the obtained 3-D images allowed differentiation between intra- and extra-articular blood vessels, as well as quantification of intra-articular blood vessels in a well-defined ROI, providing a new approach for numerical quantification of synovial vascularisation.
The administration of US contrast agent has been shown to further improve the detection and assessment of the vascularity, thanks to the recent availability of real-time contrast-enhanced US imaging and software for quantification of data. The value of this technique in improving diagnosis, staging activity of the disease and monitoring therapy efficacy has been demonstrated in patients with RA [70].
Cartilage thinning and erosions
US allows direct visualization of articular cartilage that is normally seen as a hypoechoic structure with a smooth outline over the bone surfaces. The reliability of the assessment of cartilage thickness with US has been recently demonstrated by Spannow et al. [71] in a cohort of healthy children of different ages. The authors found a good intra- and interobserver agreement both in large and small joints, using ultrasonographic standard scans according to EULAR guidelines. Furthermore Moller et al. [72] have recently demonstrated that the US method of direct visualization and quantification of cartilage in metacarpophalangeal and proximal interphalangeal joints is objective, reliable and valid, and suggested its use for diagnostic purposes in patients with RA. However, further studies aiming to collect more data on the expected normal cartilage thickness in children of different ages are needed in order to provide an accurate assessment of cartilage thinning in JIA.
In line with previous studies in RA, recent studies on JIA confirmed that US is equal or superior to CR in detecting cortical erosions in sonographically accessible areas (Fig. 6), but it is less reliable in detecting intramedullary lesions and those within the centres of larger joints, due to the acoustic shadowing from overlying bones [52, 73, 74].
Tenosynovitis
It is well established that US is sensitive in the detection of the full spectrum of tendon pathology (Fig. 5). In a recent paper Rooney et al. [75] demonstrated the extremely useful role of US in the evaluation of the anatomical basis for clinically detected ankle joint swelling in JIA. Physical examination is, in fact, very difficult in younger children due to the distribution of fat, the lack of prominent anatomical landmarks and poor co-operation, making the distinction between joint synovitis and tenosynovitis difficult. Their findings showed an unexpectedly high degree of tenosynovitis, which was often the only abnormality. This could be important for the diagnosis and therapy of JIA and potentially for classification purposes. In fact, in their conclusions the authors postulate that a substantial number of children may be wrongly classified as having extended oligoarticular or polyarticular disease on the basis of ankle involvement, when they have oligoarticular disease with tenosynovitis. Their findings however, as recently mentioned by McGonagle and Benjamin [76], have also potential implications for a new clinico-immunopathological classification of JIA; the authors argue that US findings could provide a platform for a better anatomical US-based classification of JIA.
In conclusion, US may be a valid method for monitoring synovitis and, in accessible areas, erosive progression, even if more data on reproducibility and sensitivity to change are needed. Furthermore the assessment of joints with US is still limited by the fact that US cannot penetrate bone, by intermachine and inter-reader variability, by lack of consensus on systems for assessment of activity and damage, and by limited testing of the available systems in longitudinal follow-up studies.
How has US changed our view of JIA?
-
US is sensitive in detecting subclinical synovitis
-
US has a potential role in improving JIA classification
-
US is sensitive for assessment of disease activity and damage
-
Expanding role of US in monitoring treatment efficacy should be encouraged
Future prospective in imaging in JIA
New imaging techniques are under evaluation for better and earlier assessment of synovial, cartilaginous or osseous abnormalities. It is, however, in the field of MRI that the most exciting advances are expected with the implementation of diffusion-weighted and perfusion imaging techniques, delayed gadolinium-enhanced cartilage imaging, T2 relaxation time mapping and quantitative computer-assisted tools for MRI analysis. Diffusion-weighted imaging (DWI), by detecting microscopic changes in water mobility, allows an indirect assessment of tissue integrity. This technique is promising for evaluating very early cartilage abnormalities by detecting collagen fibre degradation [77].
Dynamic contrast-enhanced MRI may allow detection of the perfusion imaging of each anatomical compartment of the joint and direct therapeutic scheduling according to enhancement patterns.
Delayed gadolinium-enhanced MR cartilage imaging (dGEMRIC) is a sensitive technique for assessing cartilage proteoglycan content, using the negative charge of the paramagnetic MR contrast agent (Fig. 7). The contrast agent distributes into the cartilage inversely to the fixed charge density of negatively charged glycosaminoglycans (GAG) [77]. Thus, T1 relaxation time, in presence of this contrast agent, is approximately linearly related to the glycosaminoglycan content. dGEMRIC may be used to assess early cartilage injury that occurs before morphologic cartilage damage can be detected by conventional imaging.
T1 mapping as a result of delayed gadolinium enhanced imaging of cartilage (dGEMRIC) for the evaluation of articular cartilage in a mid sagittal plane of a wrist in a patient with JIA: radio-lunate, luno-capitate and capitate-3rd metacarpal base joints. dGEMRIC is a technique that specifically looks at glycosaminoglycans (GAGs). Gd(DTPA)2− can be used to evaluate the fixed charge density of the cartilage which is closely related to the GAG concentration. T1 map reflects the concentration of Gd(DTPA)2− in the cartilage. GAGs are negatively charged and they repel ionic gadolinium. Areas with GAG loss have a higher concentration of gadolinium. When there is a breakdown of GAGs, cartilage loses its negative charge and allows more Gd (DTPA)2− into its matrix with a shorter T1 relaxation time, on the contrary areas with GAG integrity have a lower concentration of gadolinium, and therefore have longer T1
The recent development of 3-T MRI, with its increased signal-to-noise ratio (SNR), gives us the opportunity to obtain clearer images, better resolution and faster scans. Cartilage can be clearly visualized and pathology more easily detected due to increased image quality [78]. To date, both animal and human imaging has also been performed on a whole-body 7-T scanner, with promising results in terms of detailed imaging and functional data. However the road ahead is long and we cannot predict the end of this exciting adventure with higher field strengths.
Conclusion
With the availability of new exciting imaging tools a wide range of morphological, functional and biochemical data will be available. Translational studies will further improve our understanding of the physiopathogenesis of the disease through the integration of radiological findings with clinical, genetic and immunological data. In this context it is crucial that the radiologist and paediatric rheumatologist work in a multidisciplinary team including experts in bio-imaging processing and analysis as a more extensive use of imaging will also depend on computer-assisted diagnostics.
References
Ravelli A, Martini A (2007) Juvenile idiopathic arthritis. Lancet 369:767–778
van Rossum MA, Zwinderman AH, Boers M et al (2003) Radiologic features in juvenile idiopathic arthritis: a first step in the development of a standardized assessment method. Arthritis Rheum 48:507–515
Wallace CA, Levinson JE (1991) Juvenile rheumatoid arthritis: outcome and treatment for the 1990s. Rheum Dis Clin North Am 17:891–905
Miller ML (2002) Use of imaging in the differential diagnosis of rheumatic disease in children. Rheum Dis Clin North Am 28:483–492
Petty RE, Southwood TR, Manners P et al (2004) International League of Associations for Rheumatology classification of juvenile idiopathic arthritis: second revision, Edmonton 2001. J Rheumatol 31:390–392
Lovell DJ, Giannini EH, Reiff A et al (2000) Etanercept in children with polyarticular juvenile rheumatoid arthritis. Pediatric Rheumatology Collaborative Study Group. N Engl J Med 342:763–769
Lovell DJ, Ruperto N, Goodman S et al (2008) Adalimumab with or without methotrexate in juvenile rheumatoid arthritis. N Engl J Med 359:810–820
Swee RG, Gray JE, Beabout JW et al (1997) Screen-film versus computed radiography imaging of the hand: a direct comparison. AJR 168:539–542
van der Jagt EJ, Hofman S, Kraft BM et al (2000) Can we see enough? A comparative study of film-screen vs digital radiographs in small lesions in rheumatoid arthritis. Eur Radiol 10:304–307
Ludwig K, Henschel A, Bernhardt TM et al (2003) Performance of a flat-panel detector in the detection of artificial erosive changes: comparison with conventional screen-film and storage-phosphor radiography. Eur Radiol 13:1316–1323
US Department of Health and Human Services; Food and Drug Administration. Guidance for industry: clinical development programs for drugs, devices, and biological products for the treatment of rheumatoid arthritis. Center for Drug Evaluation and Research, Center for Biologics Evaluation and Research, Center for Devices and Radiologic Health; February 1999. Available at: http://www.fda.gov/cber/gdlns/rheumcln.pdf. Accessed December 3, 2007
Ravelli A (2008) The time has come to include assessment of radiographic progression in juvenile idiopathic arthritis clinical trials. J Rheumatol 35:553–557
Østergaard M, Peterfy C, Conaghan P et al (2003) OMERACT Rheumatoid Arthritis Magnetic Resonance Imaging Studies. Core set of MRI acquisitions, joint pathology definitions, and the OMERACT RA-MRI scoring system. J Rheumatol 30:1385–1386
Nistala K, Babar J, Johnson K et al (2007) Clinical assessment and core outcome variables are poor predictors of hip arthritis diagnosed by MRI in juvenile idiopathic arthritis. Rheumatology 46:699–702
Argyropoulou MI, Fanis SL, Xenakis T et al (2002) The role of MRI in the evaluation of hip joint disease in clinical subtypes of juvenile idiopathic arthritis. Br J Radiol 75:229–233
El-Miedany YM, Housny IH, Mansour HM et al (2001) Ultrasound versus MRI in the evaluation of juvenile idiopathic arthritis of the knee. Joint Bone Spine 68:222–230
Miller E, Roposch A, Uleryk E et al (2009) Juvenile idiopathic arthritis of peripheral joints: quality of reporting of diagnostic accuracy of conventional MRI. Acad Radiol 16:739–757
Miller E, Uleryk E, Doria AS (2009) Evidence-based outcomes of studies addressing diagnostic accuracy of MRI of juvenile idiopathic arthritis. AJR 192:1209–1218
Lamer S, Sebag GH (2000) MRI and ultrasound in children with juvenile chronic arthritis. Eur J Radiol 33:85–93
Brown AK, Quinn MA, Karim Z et al (2006) Presence of significant synovitis in rheumatoid arthritis patients with disease-modifying antirheumatic drug-induced clinical remission: evidence from an imaging study may explain structural progression. Arthritis Rheum 54:3761–3773
Gardner-Medwin JM, Killeen OG, Ryder CA et al (2006) Magnetic resonance imaging identifies features in clinically unaffected knees predicting extension of arthritis in children with monoarthritis. J Rheumatol 33:2337–2343
Cimmino MA, Bountis C, Silvestri E et al (2000) An appraisal of magnetic resonance imaging of the wrist in rheumatoid arthritis. Semin Arthritis Rheum 30:180–195
Sugimoto H, Takeda A, Kano S (1998) Assessment of disease activity in rheumatoid arthritis using magnetic resonance imaging: quantification of pannus volume in the hands. Br J Rheumatol 37:854–861
Bird P, Lassere M, Shnier R et al (2003) Computerized measurement of magnetic resonance imaging erosion volumes in patients with rheumatoid arthritis: a comparison with existing magnetic resonance imaging scoring systems and standard clinical outcome measures. Arthritis Rheum 48:614–624
Zikou AK, Argyropoulou MI, Voulgari PV et al (2006) Magnetic resonance imaging quantification of hand synovitis in patients with rheumatoid arthritis treated with adalimumab. J Rheumatol 33:219–223
Ostergaard M, Hansen M, Stoltenberg M et al (1999) Magnetic resonance imaging-determined synovial membrane volume as a marker of disease activity and a predictor of progressive joint destruction in the wrists of patients with rheumatoid arthritis. Arthritis Rheum 42:918–929
Graham TB, Laor T, Dardzinski BJ (2005) Quantitative magnetic resonance imaging of the hands and wrists of children with juvenile rheumatoid arthritis. J Rheumatol 32:1811–1820
Gylys-Morin VM, Graham TB, Blebea JS et al (2001) Knee in early juvenile rheumatoid arthritis: MR imaging findings. Radiology 220:696–706
Hodgson RJ, O’Connor P, Moots R (2008) MRI of rheumatoid arthritis image quantitation for the assessment of disease activity, progression and response to therapy. Rheumatology 47:13–21
Palosaari K, Vuotila J, Takalo R et al (2004) Contrast-enhanced dynamic and static MRI correlates with quantitative 99mTc-labelled nanocolloid scintigraphy. Study of early rheumatoid arthritis patients. Rheumatology 43:1364–1373
Ostergaard M, Ejbjerg B, Stoltenberg M et al (2001) Quantitative magnetic resonance imaging as marker of synovial membrane regeneration and recurrence of synovitis after arthroscopic knee joint synovectomy: a one year follow up study. Ann Rheum Dis 60:233–236
Tam LS, Griffith JF, Yu AB et al (2007) Rapid improvement in rheumatoid arthritis patients on combination of methotrexate and infliximab: clinical and magnetic resonance imaging evaluation. Clin Rheumatol 26:941–946
Reece RJ, Kraan MC, Radjenovic A et al (2002) Comparative assessment of leflunomide and methotrexate for the treatment of rheumatoid arthritis, by dynamic enhanced magnetic resonance imaging. Arthritis Rheum 46:366–372
Huang J, Stewart N, Crabbe J et al (2000) A 1-year follow-up study of dynamic magnetic resonance imaging in early rheumatoid arthritis reveals synovitis to be increased in shared epitope-positive patients and predictive of erosions at 1 year. Rheumatology 39:407–416
Malattia C, Damasio MB, Basso C et al (2010) Dynamic contrast-enhanced magnetic resonance imaging in the assessment of disease activity in patients with juvenile idiopathic arthritis. Rheumatology 49:178–185
Workie DW, Dardzinski BJ, Graham TB et al (2004) Quantification of dynamic contrast-enhanced MR imaging of the knee in children with juvenile rheumatoid arthritis based on pharmacokinetic modelling. Magn Reson Imaging 22:1201–1210
Workie DW, Graham TB, Laor T et al (2007) Quantitative MR characterization of disease activity in the knee in children with juvenile idiopathic arthritis: a longitudinal pilot study. Pediatr Radiol 37:535–543
Kubassova O, Boesen M, Cimmino MA et al (2009) A computer-aided detection system for rheumatoid arthritis MRI data interpretation and quantification of synovial activity. Eur J Radiol May 1 [Epub ahead of print]
McQueen FM, Benton N, Perry D et al (2003) Bone edema scored on magnetic resonance imaging scans of the dominant carpus at presentation predicts radiographic joint damage of the hands and feet 6 years later in patients with rheumatoid arthritis. Arthritis Rheum 48:1814–1827
Benton N, Stewart N, Crabbe J et al (2004) MRI of the wrist in early rheumatoid arthritis can be used to predict functional outcome at 6 years. Ann Rheum Dis 63:555–561
Dalbeth N, Smith T, Gray S et al (2009) Cellular characterization of magnetic resonance imaging bone oedema in rheumatoid arthritis; implications for pathogenesis of erosive disease. Ann Rheum Dis 68:279–282
Peterfy CG, Genant HK (1996) Emerging applications of magnetic resonance imaging in the evaluation of articular cartilage. Radiol Clin North Am 34:195–213
Doria AS, Babyn PS, Feldman B (2006) A critical appraisal of radiographic scoring systems for assessment of juvenile idiopathic arthritis. Pediatr Radiol 36:759–772
Herve-Somma CM, Sebag GH, Prieur AM et al (1992) Juvenile rheumatoid arthritis of the knee: MR evaluation with Gd-DOTA. Radiology 182:93–98
Eich GF, Halle F, Hodler J et al (1994) Juvenile chronic arthritis: imaging of the knees and hips before and after intraarticular steroid infection. Pediatr Radiol 24:558–563
Hardy PA, Recht MP, Piraino D et al (1996) Optimization of a dual echo in the steady state (DESS) free-precession sequence for imaging cartilage. J Magn Reson Imaging 6:329–335
Ruehm S, Zanetti M, Romero J et al (1998) MRI of patellar articular cartilage: evaluation of an optimized gradient echo sequence (3D-DESS). J Magn Reson Imaging 8:1246–1251
Reeder SB, Wen Z, Yu H et al (2004) Multicoil Dixon chemical species separation with an iterative least-squares estimation method. Magn Reson Med 51:35–45
Duerk JL, Lewin JS, Wendt M et al (1998) Remember true FISP? A high SNR, near 1-second imaging method for T2-like contrast in interventional MRI at .2T. J Magn Reson Imaging 8:203–208
Kight AC, Dardzinski BJ, Laor T et al (2004) Magnetic resonance imaging evaluation of the effects of juvenile rheumatoid arthritis on distal femoral weight-bearing cartilage. Arthritis Rheum 50:901–905
Potter K, Butler JJ, Horton WE et al (2000) Response of engineered cartilage tissue to biochemical agents as studied by proton magnetic resonance microscopy. Arthritis Rheum 43:1580–1590
Malattia C, Damasio MB, Magnaguagno F et al (2008) Magnetic resonance imaging, ultrasonography, and conventional radiography in the assessment of bone erosions in juvenile idiopathic arthritis. Arthritis Rheum 59:1764–1772
Gilkeson G, Polisson R, Sinclair H et al (1988) Early detection of carpal erosions in patients with rheumatoid arthritis: a pilot study of magnetic resonance imaging. J Rheumatol 15:1361–1366
Backhaus M, Kamradt T, Sandrock D et al (1999) Arthritis of the finger joints: a comprehensive approach comparing conventional radiography, scintigraphy, ultrasound, and contrast-enhanced magnetic resonance imaging. Arthritis Rheum 42:1232–1245
McQueen FM, Stewart N, Crabbe J et al (1998) Magnetic resonance imaging of the wrist in early rheumatoid arthritis reveals a high prevalence of erosions at four months after symptom onset. Ann Rheum Dis 57:350–356
Hoving JL, Buchbinder R, Hall S et al (2004) A comparison of magnetic resonance imaging, sonography, and radiography of the hand in patients with early rheumatoid arthritis. J Rheumatol 31:663–675
Østergaard M, Hansen M, Stoltenberg M et al (2003) New radiographic bone erosions in the wrists of patients with rheumatoid arthritis are detectable with magnetic resonance imaging a median of 2 years earlier. Arthritis Rheum 48:2128–2131
Perry D, Stewart N, Benton N et al (2005) Detection of erosions in the rheumatoid hand; a comparative study of multidetector computerized tomography versus magnetic resonance scanning. J Rheumatol 32:256–267
Døhn UM, Ejbjerg BJ, Hasselquist M et al (2007) Rheumatoid arthritis bone erosion volumes on CT and MRI: reliability and correlations with erosion scores on CT, MRI and radiography. Ann Rheum Dis 66:1388–1392
McQueen FM, Benton N, Crabbe J et al (2001) What is the fate of erosions in early rheumatoid arthritis? Tracking individual lesions using x rays and magnetic resonance imaging over the first 2 years of disease. Ann Rheum Dis 60:859–868
Wakefield RJ, Balint PV, Szkudlarek M et al (2005) Musculoskeletal ultrasound including definitions for ultrasonographic pathology. J Rheumatol 32:2485–2487
Muller L, Kellenberger CJ, Cannizzaro E et al (2009) Early diagnosis of temporomandibular joint involvement in juvenile idiopathic arthritis: a pilot study comparing clinical examination and ultrasound to magnetic resonance imaging. Rheumatology 48:680–685
Magni-Manzoni S, Epis O, Ravelli A et al (2009) Comparison of clinical versus ultrasound-determined synovitis in juvenile idiopathic arthritis. Arthritis Rheum 61:1497–1504
Haslam KE, McCann LJ, Wyatt S et al (2010) The detection of subclinical synovitis by ultrasound in oligoarticular juvenile idiopathic arthritis: a pilot study. Rheumatology 49:123–127
Giannini EH, Brewer EJ, Kuzmina N et al (1992) Methotrexate in resistant juvenile rheumatoid arthritis: results of the USA-USSR double-blind, placebo-controlled trial. The Pediatric Rheumatology Collaborative Study group and The Cooperative Children’s Study group. N Engl J Med 326:1043–1049
Ruperto N, Murray KJ, Gerloni V et al (2004) A randomized trial of parenteral methotrexate comparing an intermediate dose with a higher dose in children with juvenile idiopathic arthritis who failed to respond to standard doses of methotrexate. Arthritis Rheum 50:2191–2201
Doria AS, Kiss MH, Lotito AP et al (2001) Juvenile rheumatoid arthritis of the knee: evaluation with contrast enhanced color Doppler ultrasound. Pediatr Radiol 31:524–531
Newman JS, Laing TJ, McCarthy CJ et al (1996) Power Doppler sonography of synovitis: assessment of therapeutic response–preliminary observations. Radiology 198:582–584
Strunk J, Klingenberger P, Strube K et al (2006) Three-dimensional Doppler sonographic vascular imaging in regions with increased MR enhancement in inflamed wrists of patients with rheumatoid arthritis. Joint Bone Spine 73:518–522
Mouterde G, Carotti M, D’Agostino MA (2009) Contrast-enhanced ultrasound in musculoskeletal diseases. J Radiol 90:148–155
Spannow AH, Pfeiffer-Jensen M, Andersen NT et al (2009) Inter- and intraobserver variation of ultrasonographic cartilage thickness assessments in small and large joints in healthy children. Pediatr Rheumatol Online J 7:12
Möller B, Bonel H, Rotzetter M et al (2009) Measuring finger joint cartilage by ultrasound as a promising alternative to conventional radiograph imaging. Arthritis Rheum 61:435–441
Wakefield RJ, O’Connor PJ, Conaghan PG et al (2007) Finger tendon disease in untreated early rheumatoid arthritis: a comparison of ultrasound and magnetic resonance imaging. Arthritis Rheum 57:1158–1164
Buchmann RF, Jaramillo D (2004) Imaging of articular disorders in children. Radiol Clin North Am 42:151–168
Rooney ME, McAllister C, Burns JF (2009) Ankle disease in juvenile idiopathic arthritis: ultrasound findings in clinically swollen ankles. J Rheumatol 36:1725–1729
McGonagle D, Benjamin M (2009) Towards a new clinico-immunopathological classification of juvenile inflammatory arthritis. J Rheumatol 36:1573–1574
Babyn P, Doria AS (2007) Radiologic investigation of rheumatic diseases. Rheum Dis Clin North Am 33:403–440
Chavhan GB, Babyn PS (2009) Pediatric musculoskeletal imaging at 3 Tesla. Semin Musculoskelet Radiol 13:181–195
Pettersson H, Rydholm U (1984) Radiologic classification of knee joint destruction in juvenile chronic arthritis. Pediatr Radiol 14:419–421
Poznanski AK, Hernandez RJ, Guire KE et al (1978) Carpal length in children- a useful measurement in the diagnosis of rheumatoid arthritis and some congenital malformation syndromes. Radiology 129:661–668
Magni-Manzoni S, Rossi F, Pistorio A et al (2003) Prognostic factors for radiographic progression, damage, and disability in juvenile idiopathic arthritis. Arthritis Rheum 52:2865–2872
Doria AS, de Castro CC, Kiss MH et al (2003) Inter- and intrareader variability in the interpretation of two radiographic classification systems in juvenile rheumatoid arthritis. Pediatr Radiol 33:673–681
Van Rossum MA, Boers M, Zwinderman AH (2005) Development of a standardized method of assessment of radiographs and radiographic changes in juvenile idiopathic arthritis: introduction of the Dijkstra composite score. Arthritis Rheum 52:2865–2872
Rossi F, Di Dia F, Galipo O et al (2006) Use of the Sharp and Larsen scoring method in the assessment of radiographic progression in juvenile idiopathic arthritis. Arthritis Rheum 55:717–723
Ravelli A, Ioseliani M, Norambuena X et al (2007) Adapted versions of the Sharp/van der Heijde score are reliable and valid for assessment of radiographic progression in JIA. Arthritis Rheum 56:3087–3095
Bertamino M, Rossi F, Pistorio A et al (2010) Development and initial validation of a radiographic scoring system for the hip in juvenile idiopathic arthritis. J Rheumatol 37:432–439
Remedios D, Martin K, Kaplan G et al (1997) Juvenile chronic arthritis: diagnosis and management of tibio-talar and sub-talar disease. Br J Rheumatol 36:1214–1217
Kuseler A, Pederson TK, Herlin T et al (1998) Contrast enhanced magnetic resonance imaging asa method to diagnose early inflammation changes in the temporomandibular joint in children with juvenile chronic arthritis. J Rheumatol 25:1406–1412
Karmazyn B, Bowyer SL, Schmidt KM et al (2007) US findings of metacarpophalangeal joints in children with idiopathic juvenile arthritis. Pediatr Radiol 37:475–482
Author information
Authors and Affiliations
Corresponding author
Additional information
Drs Damasio and Malattia contributed equally to this article.
Rights and permissions
About this article
Cite this article
Damasio, M.B., Malattia, C., Martini, A. et al. Synovial and inflammatory diseases in childhood: role of new imaging modalities in the assessment of patients with juvenile idiopathic arthritis. Pediatr Radiol 40, 985–998 (2010). https://doi.org/10.1007/s00247-010-1612-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-010-1612-z