Abstract
Background: It has been suggested that increased hepatic and intramuscular fat is associated with insulin resistance, and that increased pancreatic fat is related to impaired insulin secretion. Objective: We postulated that in obese nondiabetic teenagers insulin levels would be directly related to increases in intramuscular and hepatic fat and inversely related to increases in pancreatic fat. Materials and methods: MRI was used to assess the percentage of fat in the liver, muscle and pancreas in 15 healthy Mexican-American girls, 14–17 years old, with body mass indexes (BMIs) ranging from 17.7 kg/m2 to 46 kg/m2. Results: Strong correlations were observed between BMI and fat content in the liver, muscle, and pancreas (r2s between 0.50 and 0.89; P<0.003). Serum insulin levels were closely associated with fat measures in the muscle and liver (r2s=0.63 and 0.29, and P=0.001 and P=0.023, respectively). In contrast to our hypothesis, fat content in the pancreas was also directly related to insulin secretion (r2=0.74; P=0.001). Summary: We conclude that in nondiabetic teenagers, obesity is associated with an increased accumulation of fat in the pancreas without impairment of insulin secretion.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Worldwide, obesity has reached epidemic proportions. More than 30% of children in the United States are overweight or obese, and there is no evidence that the rise in obesity incidence will plateau or decline in the coming years [1, 2]. Insulin resistance commonly occurs in overweight and obese children and is associated with type 2 diabetes, which accounts for a large number of the new-onset cases of diabetes in children [3]. The increasing incidence of type 2 diabetes parallels the increasing occurrence and severity of pediatric obesity [4–6].
In overweight adolescents, excess fat in the muscle cells and hepatocytes interferes with insulin signaling, leading to insulin resistance [7]. As obesity develops, insulin secretion increases parallel to insulin resistance in order to maintain normal glucose homeostasis. Although most people are capable of compensating for insulin resistance by increasing insulin secretion, thus maintaining normal glucose levels, patients predisposed to diabetes fail to compensate adequately for the greater insulin requirements [8]. It has been suggested that the eventual impairment of insulin secretion in subjects with type 2 diabetes is related to an overload of adipose tissue in the pancreas [9, 10]. Indeed, data from experimental animals indicate that the ectopic deposition of lipids in the pancreas is associated with destruction of islet cells and impaired insulin secretion [11, 12].
Whether variations in pancreatic fat accumulation also account for differences in insulin secretion in humans is unknown because of technical difficulties in measuring fat stores in intra-abdominal organs in vivo. Magnetic resonance (MR) spectroscopy has been used to assess lipid content in skeletal muscle and, less frequently, in the liver, but inaccuracies related to motion have limited its use in the pancreas. The availability of novel magnetic resonance imaging (MRI) techniques that can provide noninvasive assessments of pancreatic composition might allow delineation of the phenotypic characteristics of subjects at risk for type 2 diabetes.
In this study, we used an MR technique that was described by Dixon [13] and provides accurate measures of fat content in any tissue to assess which lean tissues stockpile the most fat in lean and obese subjects. We postulated that in nondiabetic teenagers, increasing body mass would be related to increased fat accumulation in the muscle, liver, and pancreas. We also postulated that even though insulin levels in teenagers would be correlated with the percentage of fat in the liver and muscle (because of compensation for insulin resistance), beyond a threshold, pancreatic fat content would be inversely related to insulin levels (because of impaired insulin secretion).
Materials and methods
Experimental subjects
Fifteen nondiabetic, healthy Mexican-American girls, 14–17 years of age, were recruited from a lifestyle intervention program for overweight youth (Kids N Fitness) in the Division of Endocrinology, Diabetes and Metabolism at Children’s Hospital of Los Angeles (CHLA), as well as schools in the area. All obese subjects enrolled in the study had fasting glucose levels and hemoglobin A1c (HbA1c) as part of their participation in the Kids N Fitness program to ensure no presence of type 2 diabetes. Subjects were excluded if they had been diagnosed with any major illness, including pancreatitis, had a condition or had taken medications known to influence body composition, insulin action, or insulin secretion, or if they had a family history of tpe 2 diabetes among first-degree relatives. The investigational protocol was approved by the institutional review board for clinical investigations at CHLA, and informed consent was obtained from all subjects and their parents.
Physical examination
All participants underwent a physical examination by a pediatric endocrinologist to determine their general health and stage of sexual development. Tanner stage of sexual maturity was assessed based on breast development [14]. Only girls in Tanner stage 5 were included in the study. Measurements of total height were obtained to the nearest 0.1 cm using the Harpenden stadiometer (Holtain, Crymmych, Wales), and measurements of weight were obtained to the nearest 0.1 kg using the Scale-Tronix (Scale-Tronix,, Wheaton, Ill., USA). Body mass index (BMI) was calculated as weight in kilograms divided by the square of height in meters.
Biochemical determinations
Blood was drawn and serum levels of fasting glucose, serum insulin, HbA1c and lipid profiles, including triglycerides, low-density lipoprotein (LDL), high-density lipoprotein (HDL), and cholesterol were obtained using validated methods. Fasting glucose levels were measured with an YSI 2300 Stat glucose/lactate analyzer (YSI, Inc., Yellow Springs, Ohio, USA). Serum insulin was determined by RIA [15]. HbA1c was measured by high-pressure liquid chromatography [16] using the fully automated Glycosylated Hemoglobin Analyzer System (Bio-Rad Laboratories, Inc., Richmond, Calif., USA). Total cholesterol, HDL- and LDL-cholesterol and triglycerides were measured as previously described [17].
Three-point Dixon MR imaging
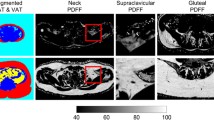
Subjects underwent imaging examinations of the liver, pancreas,and soleus muscle in the supine position with the use of a 1.5 T GE MR unit (GE Medical Systems, Milwaukee, Wis., USA). The soleus muscle was selected because it is prevalently composed of slow-twitch oxidative fibers (fiber type I), which have the greatest insulin sensitivity [18]. After positioning the abdomen in a phased array coil, axial images were acquired from the level of the liver and the pancreas (Fig. 1) using the three-point Dixon sequence (not widely commercially available). Thereafter, the subjects were repositioned, and three-point Dixon images from the right calf (Fig. 2) at the level of the largest circumference were acquired using the knee coil. The entire procedure, including positioning and scanning, was completed within 30 min.
After completion of the automated reconstruction of the three-point Dixon images, the images were transferred to a GE Advantage Workstation for analysis. The signal intensity in the images was calculated with operator-defined regions of interest (ROIs) at the same location in both fat and water images. A total of three ROIs per organ (liver, pancreas, soleus muscle) were acquired and averaged, with care given to placement of the ROIs to avoid confounding anatomy (e.g., large blood vessels). Fat/water ratios were calculated on a pixel-by-pixel basis by dividing the signal intensity calculated from the fat image by the signal intensity calculated from the water image.
The use of decomposing fat and water signals to discriminate between fat and water protons based on their resonant frequency difference was first introduced by Dixon [13]. This method uses two acquisitions with a delay between the radiofrequency (RF) and gradient echoes, such that the phase shift between water and fat is either 0 or radians (in-phase and out-of-phase, respectively). Separate water and fat images can be obtained by adding and subtracting the in-phase and out-of-phase images. This method was subsequently enhanced to accommodate magnetic field (B0) and RF inhomogeneity through the use of a third acquisition, leading to the three-point Dixon method [19, 20]. The resulting sequence produced three registered volumes with the refocusing pulse time shifted to produce phase differences of 0, π, and −π radians. The pulse sequence parameters were: TR/TE=4,000/54 ms, echo train length=10, slice thickness 3 mm, matrix=512×192, NEX=1, and a total scan time 8:48 min. In vitro reproducibility of the quantitative fat fraction measurements in phantom models using this technique has been calculated to be 1.27% [21]; in vivo reproducibility in the liver, muscle, and pancreas was between 2.3% and 4.6% in normal volunteers.
Statistical analysis
Statistical analysis was carried out using STATA for windows (version 8.0, STATA, College Station, Tex., USA). Data are expressed as means±SD. Statistical analyses included the Pearson correlation and linear regression. Comparison of the slopes of the fat content in liver, muscle, and pancreas was made using the difference in the fat content as the dependent variable and either BMI or insulin as the independent variable. Analyses were conducted for all subjects together and for lean and obese teenagers independently. For the purpose of this study, lean subjects were defined as those who had a BMI of <25, and obese subjects as those with a BMI of ≥25.
Results
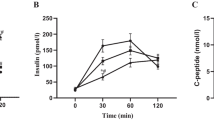
Age, anthropometric and metabolic data, and the percentage volumes of fat in the liver, muscle, and pancreas in all subjects and in lean and obese subgroups are summarized in Table 1. There was a wide range of values for BMI in study subjects, from 17.7 to 46.0. Moderate correlations were found between weight and BMI and serum levels of triglycerides, HDL, and HgA1C (Table 2). Strong correlations were observed between BMI and the liver (R2=0.50), muscle (r2=0.80) and pancreas (r2=0.89) fat contents; the strongest associations were seen with muscle and pancreatic fats (Fig. 3). BMI was also strongly correlated with serum insulin, implying a state of compensated insulin resistance in the obese subjects (Fig. 4). As expected, the levels of serum insulin were closely associated with measures of adiposity in the muscle and the liver. However, in contrast to our hypothesis, serum insulin levels in the teenagers studied were also positively associated with fat content in the pancreas (Fig. 5). Because of the high correlation between adiposity in the pancreas and in the muscle (R2=0.82), it was not possible to determine which variable was more influential in relation to insulin levels; multivariate analyses indicated that when either muscle or pancreatic fat was taken into account, fat content in the other tissues did not enter into the equation.
Lean and obese nondiabetic teenagers had similar values for fasting glucose, HgA1C and cholesterol. In contrast, measures for fasting serum insulin were significantly higher, and those for HDL were significantly lower in obese subjects than in lean subjects. On average, obese teenagers stored 50–150% more fat in the liver, muscle, and pancreas than lean subjects. Significant correlations were present between BMI and measures of fat in the liver, muscle, and pancreas of the obese and lean subgroups; the strongest were seen between BMI and muscle fat content; r2 s=0.59 and 0.69 for lean and obese subgroups, respectively. In obese subjects, strong correlations were seen between values for fasting serum insulin and measures of adiposity in the muscle and the pancreas; r2 s=0.50 and 0.52, respectively.
Discussion
The findings of this study corroborate data indicating that obese subjects have greater intramuscular and hepatic fat and increased insulin resistance, resulting in increased insulin levels. Our results also demonstrated that when compared with normal-weight subjects, obese teenagers had greater fat accumulation in the pancreas. However, in contrast to our hypothesis, the greater proportion of pancreatic fat in the obese nondiabetic subjects studied was associated with increased, not decreased, insulin levels.
We postulated that the ability of the pancreas to maintain a high insulin secretory rate declines with an increasing accumulation of pancreatic fat. This supposition was based on evidence that the clinical onset of type 2 diabetes is preceded by years of insulin resistance and a shorter period of decreased insulin secretion. Although the mechanism for the failure of insulin production has not been well-delineated, it might be related to lipotoxicity of β-cells [22]. Data from in vitro studies suggest that ectopic deposition of lipids in the pancreas is associated with destruction of islet cells and impaired insulin secretion [23]. In addition, studies in obese rats indicate that increases in triglyceride content in β-cells result in β-cell damage [24]. Our hypothesis was also supported by the knowledge that progressive fat replacement in the pancreas of patients with cystic fibrosis (CF) coincides with increasing disruption of islet morphology and β-cell apoptosis; in cases of CF, diabetes is observed in 9% of children, 26% of adolescents, 35% of adults ages 20–29%, and 43% of adults age 30 and older [25, 26]. Lastly, there is increasing evidence from studies in experimental animals that the use of thiazolidinediones (TZDs) leads to decreased islet triglyceride stores [27] and increased islet cell insulin [28, 29]. Several recent trials of diabetes prevention in humans have shown that TZDs preserve β-cell function, and it has been proposed that the mechanism of this effect is a decrease in lipotoxicity in the pancreatic β-cell [22].
There are several possible explanations for our unexpected results. One might be that the degree of pancreatic fat accumulation had not reached a hypothetical threshold, above which insulin secretion deteriorates. Another is the possible high variability in pancreatic fat accumulation among obese teenagers. However, the cohort studied included markedly obese subjects, and there was a strong correlation between pancreatic fat and weight, minimizing the likelihood of the above possibilities. It is more probable that there is variability in genetic susceptibility to lipotoxicity, or the deleterious effect of adipose tissue deposition in the pancreas might require a long time before manifesting in impaired β-cell function. Indeed, it has been estimated that pancreatic β-cell damage is present for more than a decade before diabetes is diagnosed [30]. Thus, there might be a lengthy period in which lipotoxicity-induced β-cell damage is associated with normal β-cell function.
Until recently, studies supporting the concept that lipotoxicity in humans contributes to a decline in β-cell function through increased apoptosis have been limited to extrapolations from observations of experimental animal models. In this study, the three-point Dixon MR technique was used to obtain quantitative measures of hepatic, muscular, and pancreatic fat. Because the number of islets of Langerhans in the pancreas is about two times greater in the tail of the pancreas than in the head, we specifically measured the percentage of fat in the tail [31]. Previously, studies using multiple phantoms with various fat volumes (0–50%) conducted at our institution indicated that measures of fat obtained with the three-point Dixon technique correlated strongly with true fat ratios (r2=0.98; P<0.001) [21].
It should be noted that MR measures of pancreatic fat using the three-point Dixon method are influenced by both the fat content in the islet cells, which is believed to be related to lipotoxicity, and extracellular fat accumulation. Although it is not possible to quantify adipose tissue independently in these two compartments with this technique, studies in experimental animals suggest that, with obesity, the intraislet lipid content increases disproportionately to the extracellular fat [24]. In humans, autopsy studies show that the amount of adipose tissue correlates positively with age and body weight [32] and that, with aging, more fat accumulates in the pancreatic β-cells than in the exocrine pancreas [33, 34]. More recently, studies with I125-labeled LDLs have shown the presence of high-affinity LDL receptors on β-cells, but not on neighboring α-cells [33]. Because with progressive obesity the proportion of fat that accumulates in the intracellular compartment increases, MR measures of total fat using the three-point Dixon technique likely reflect intracellular fat content.
In summary, this study represents the first in vivo measurement of the ratio of pancreatic fat and water in lean and obese subjects. Further studies are needed to establish the degree to which fat accumulation in the pancreas is associated with impaired β-cell function and decreased insulin secretion. The future application of novel MRI techniques to assess noninvasively the composition of the pancreas might eventually be useful in delineating the phenotypic characteristics of subjects at risk for type 2 diabetes.
References
Zimmet PZ (1999) Diabetes epidemiology as a tool to trigger diabetes research and care. Diabetologia 42:499–518
Miller J, Rosenbloom A, Silverstein J (2004) Childhood obesity. J Clin Endocrinol Metab 89:4211–4218
Fagot-Campagna A (2000) Emergence of type 2 diabetes mellitus in children: epidemiological evidence. J Pediatr Endocrinol Metab 13[Suppl 6]:1395–1402
Aye T, Levitsky LL (2003) Type 2 diabetes: an epidemic disease in childhood. Curr Opin Pediatr 15:411–415
Katzmarzyk PT (2002) The Canadian obesity epidemic, 1985–1998. CMAJ 166:1039–1040
Mokdad AH, Serdula MK, Dietz WH, et al (1999) The spread of the obesity epidemic in the United States, 1991–1998. JAMA 282:1519–1522
Schaffer JE (2003) Lipotoxicity: when tissues overeat. Curr Opin Lipidol 14:281–287
Poitout V (2004) Beta-cell lipotoxicity: burning fat into heat? Endocrinology 145:3563–3565
Carpentier A, Mittelman SD, Bergman RN, et al (2000) Prolonged elevation of plasma-free fatty acids impairs pancreatic beta-cell function in obese nondiabetic humans but not in individuals with type 2 diabetes. Diabetes 49:399–408
Lee Y, Hirose H, Ohneda M, et al (1994) Beta-cell lipotoxicity in the pathogenesis of non-insulin-dependent diabetes mellitus of obese rats: impairment in adipocyte-beta-cell relationships. Proc Natl Acad Sci USA 91:10878–10882
McGarry JD (2001) Dysregulation of fatty acid metabolism in the etiology of type 2 diabetes. Diabetes 51:7–18
Unger RH (2002) Lipotoxic diseases. Annu Rev Med 53:319–336
Dixon W (1984) Simple proton spectroscopic imaging. Radiology 153:189–194
Tanner JM (1978) Physical growth and development. In: Forfar JO, Arnell CC (eds) Textbook of Pediatrics. Churchill Livingstone, Edinburgh, pp 249–303
Desbuquois B, Aurbach GD (1971) Use of polyethylene glycol to separate free and antibody-bound peptide hormones in radioimmunoassays. J Clin Endocrinol Metab 33:732–738
Stenman UH, Pesonen K, Ylinen K, et al (1984) Rapid chromatographic quantitation of glycosylated haemoglobins. J Chromatogr 297:327–332
Yki-Jarvinen H, Kauppila M, Kujansuu E, et al (1992) Comparison of insulin regimens in patients with non-insulin-dependent diabetes mellitus. N Engl J Med 327:1426–1433
Perseghin G, Scifo P, De Cobelli F, et al (1999) Intramyocellular triglyceride content is a determinant of in vivo insulin resistance in humans: a 1H-13C nuclear magnetic resonance spectroscopy assessment in offspring of type 2 diabetic parents. Diabetes 48:1600–1606
Glover G, Schneider E (1991) Three-point Dixon technique for true water/fat decomposition with BO inhomogeneity correction. Magn Reson Med 18:371–383
Glover GH (1991) Multipoint Dixon technique for water and fat proton and susceptibility imaging. J Magn Reson Imaging 1:521–530
Guclu CC, Kovanlikaya I, Desai C, et al (2004) Lipid percentage measurements using three-point Dixon method. In: Proceedings of the 12th Annual Meeting of the ISMRM, Kyoto, 497 p
Bell DSH (2004) Management of type 2 diabetes with thiazolidinediones: link between β-cell preservation and durability of response. Endocrinologist 14:293–300
Zhou YP, Ling ZC, Grill VE (1996) Inhibitory effects of fatty acids on glucose-regulated β-cell function: association with increased islet triglyceride stores and altered effect of fatty acid oxidation on glucose metabolism. Metabolism 45:981–986
Unger RH (1995) Lipotoxicity in the pathogenesis of obesity-dependent NIDDM. Genetic and clinical implications. Diabetes 44:863–870
Iannucci A, Mukai K, Johnson D, et al (1984) Endocrine pancreas in cystic fibrosis: an immunohistochemical study. Hum Pathol 15:278–284
Moran A (1999) Cystic fibrosis related diabetes. In: Cystic Fibrosis Worldwide website http://www.cfww.org/pub/newsletter/nl01a/nl01af.htm
Shimabukuro M, Zhou YT, Lee Y, et al (1998) Troglitazone lowers islet fat and restores beta cell function of Zucker diabetic fatty rats. J Biol Chem 273:3547–3550
Lister CA, Moore GBT, Piercy V, et al (1999) Rosiglitazone, but not metformin or glibenclamide, improves glycaemic control and increases islet insulin content. Diabetologia 42:A150
Finegood DT, McArthur MD, Kojwang D, et al (2001) Beta-cell mass dynamics in Zucker diabetic fatty rats. Rosiglitazone prevents the rise in net cell death. Diabetes 50:1021–1029
Group. UKPS (1995) UK Prospective Diabetes Study 16. Overview of 6 years therapy of type 2 diabetes: a progressive disease. Diabetes 44:1249–1258
Netter FH (1970) The CIBA collection of medical illustrations: endocrine system and selected metabolic diseases. CIBA, New York
Schmitz-Moormann P, Pittner PM, Heinze W (1981) Lipomatosis of the pancreas. A morphometrical investigation. Pathol Res Pract 173:45–53
Cnop M, Grupping A, Hoorens A, l et al (2000) Endocytosis of low-density lipoprotein by human pancreatic beta cells and uptake in lipid-storing vesicles, which increase with age. Am J Pathol 156:237–244
Weichselbaum A, Stangl E (1902) Wien Klin Wochenschr 15:969–976
Acknowledgements
The authors would like to express their acknowledgement of and appreciation for the support of General Electric Medical Systems, Milwaukee, Wisconsin, USA.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kovanlikaya, A., Mittelman, S.D., Ward, A. et al. Obesity and fat quantification in lean tissues using three-point Dixon MR imaging. Pediatr Radiol 35, 601–607 (2005). https://doi.org/10.1007/s00247-005-1413-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-005-1413-y